Abstract
Severe retroperitoneal haemorrhage after retrograde pyelogram (RPG) is rare and has not been reported in the literature. One of the few indications for performing RPG in end-stage kidneys is evaluation of the upper urinary tract for malignancy. We present a rare case of massive retroperitoneal haemorrhage in a 58-year-old man, with a history of deceased donor kidney transplantation for end-stage kidney disease (ESKD), following bilateral RPG for the evaluation of urothelial cancer. The bleeding was successfully stopped with renal artery angioembolisation. This case demonstrates the importance of exercising extra caution when performing endoscopic procedures in patients with ESKD and keeping the intrarenal pressure as low as possible.
Keywords
Introduction
Retrograde pyelogram (RPG) is a routine diagnostic procedure, performed by the urologist in combination with cystoscopy, to investigate for pathology involving the upper urinary tracts, that is, the ureters and pelvicalyceal systems. Typically, it involves the intraluminal instillation of contrast media under reasonably low syringe pressure and the use of fluoroscopic imaging to look for abnormalities. While it is generally a safe procedure, complications can occur when the principles of practice are not adhered to. One of the rare indications for RPG in end-stage kidney disease (ESKD) is evaluation of the upper tract for urothelial cancer (UC). We report a rare case of massive retroperitoneal haemorrhage following bilateral RPG in end-stage kidneys in a kidney transplant patient with high-risk UC of the bladder.
Case report
We present the case of a 58-year-old man, an ex-smoker with a 20 pack-year history, who had received a deceased donor kidney transplantation 9 years ago for ESKD secondary to chronic glomerulonephritis, after being on haemodialysis for 4 years. His other co-morbidities included multiple strokes, BK viraemia and non-muscle-invasive bladder cancer. His long-term medications included clopidogrel (75 mg daily), prednisolone (5 mg daily) and tacrolimus (6 mg daily). At baseline, his serum creatinine was 75 µmol/L, translating to an estimated glomerular filtration rate (eGFR) of 96 mL/min/1.73 m2 of body surface area.
The patient had been on follow-up for non-invasive (pTa) bladder cancer with high-risk features: high-grade and concurrent carcinoma in situ (CIS). He previously received intravesical treatment with Bacillus Calmette–Guérin (BCG) instillations, having completed the induction and one maintenance cycle. While intravesical BCG is the standard of care for high-risk non-invasive bladder cancer, its efficacy and safety in immunosuppressed patients remain controversial. In his latest surveillance, imaging did not show obvious upper-tract lesions, while urine cytology revealed atypical urothelial cells. Subsequently, a cystoscopic evaluation under general anaesthesia was performed, together with bilateral RPG to rule out upper-tract disease. Clopidogrel was stopped for 7 days prior to the day of procedure. Preoperative evaluation showed a baseline serum haemoglobin (Hb) of 11.3 g/dL and normal coagulation profile. The findings on rigid cystoscopy were unremarkable. An attempt to cannulate the transplant ureter was unsuccessful due to acute angulation of the anastomotic opening. During bilateral RPG of the native kidneys, the ureteral catheter was parked at the distal ureters; mild resistance was encountered during contrast opacification of the ureters and kidneys, requiring additional syringe force to overcome the small-calibre upper urinary tracts. On fluoroscopy, there were no abnormal filling defects. What was thought to be a calyceal diverticulum was seen in the left upper pole. However, this could have been a forniceal rupture, in retrospect. There were fluoroscopic signs of pyelo-venous backflow (Figure 1).
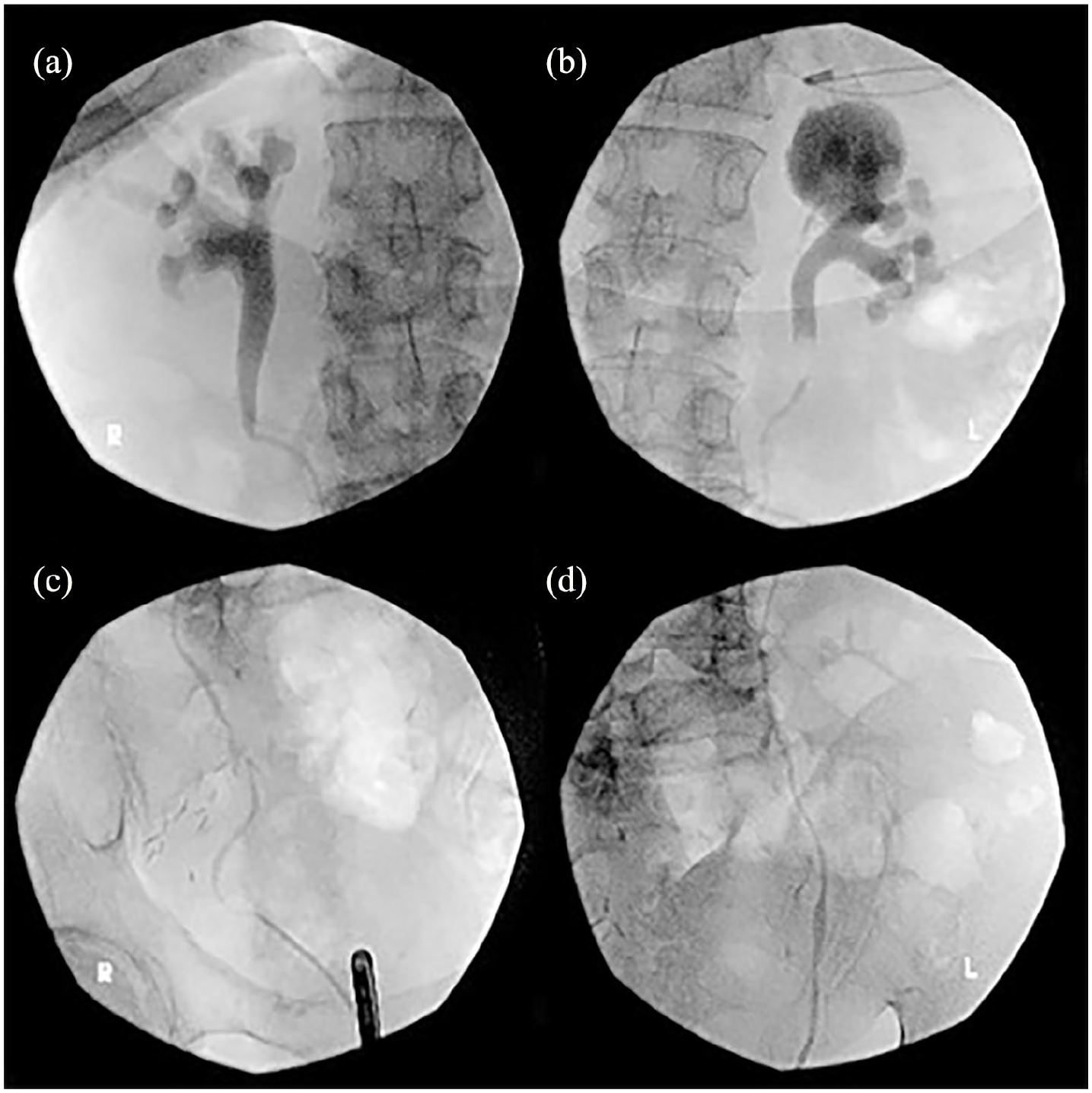
Bilateral retrograde pyelogram (RPG) on fluoroscopy. (a) and (b) Clubbed renal calyces suggestive of high intrapelvic pressure. (b) Ruptured left upper-pole calyceal fornix (black arrowhead) and pyelo-venous backflow (white arrowhead). (c) and (d) Small-calibre ureters in end-stage native kidneys.
In the evening post procedure, the patient had a transient episode of hypotension, prompting admission for further evaluation. Serial checks of serum Hb were stable over 24 hours (10.5–11.0 g/dL). Intravenous antibiotics were started on the suspicion of procedure-related urosepsis based on elevated white blood cell count (44.0×109/L). On post-procedure day 3, the patient complained of left flank pain, with a drop in Hb to 7.9 g/dL, and clinical examination found left abdominal fullness with tenderness. An urgent computed tomography (CT) scan of the abdomen and pelvis revealed an extensive left perinephric haematoma and a smaller one on the right side (Figure 2). The patient was immediately escalated to high-dependency care and given red blood cell transfusions, bringing up his serum Hb to 9.0 g/dL. He remained stable with conservative management until post-procedure day 5, when his left flank pain worsened, and he became tachycardic and hypotensive, with a drop in serum Hb to 6.7 g/dL. An urgent renal artery angioembolisation was arranged with the duty interventional radiologist. Multiple bleeding points were confirmed on left renal artery angiogram, and the left main renal artery was embolised with micro coils and a mixture of Lipiodol (Guerbet, Villepinte, France) and Histoacryl (B. Braun, Melsungen, Germany). One bleeding point in the upper-pole branch of the right renal artery was selectively embolised with micro coils. The patient remained haemodynamically stable thereafter, requiring intermittent blood transfusions to maintain an Hb level of >8 g/dL. On post-embolisation day 6, worsening left flank fullness and ecchymosis triggered a CT angiogram of the abdomen and pelvis, which showed an enlarged left retroperitoneal haematoma without active bleeding. The patient remained clinically stable with conservative management, and did not have any gross haematuria. Throughout his 4-week stay in hospital (also for other medical issues), 11 units of red blood cell transfusions were given in total, together with platelet and plasma products transfusions. He was discharged well, with a serum Hb of 10.6 g/dL and creatinine of 65 µmol/L.
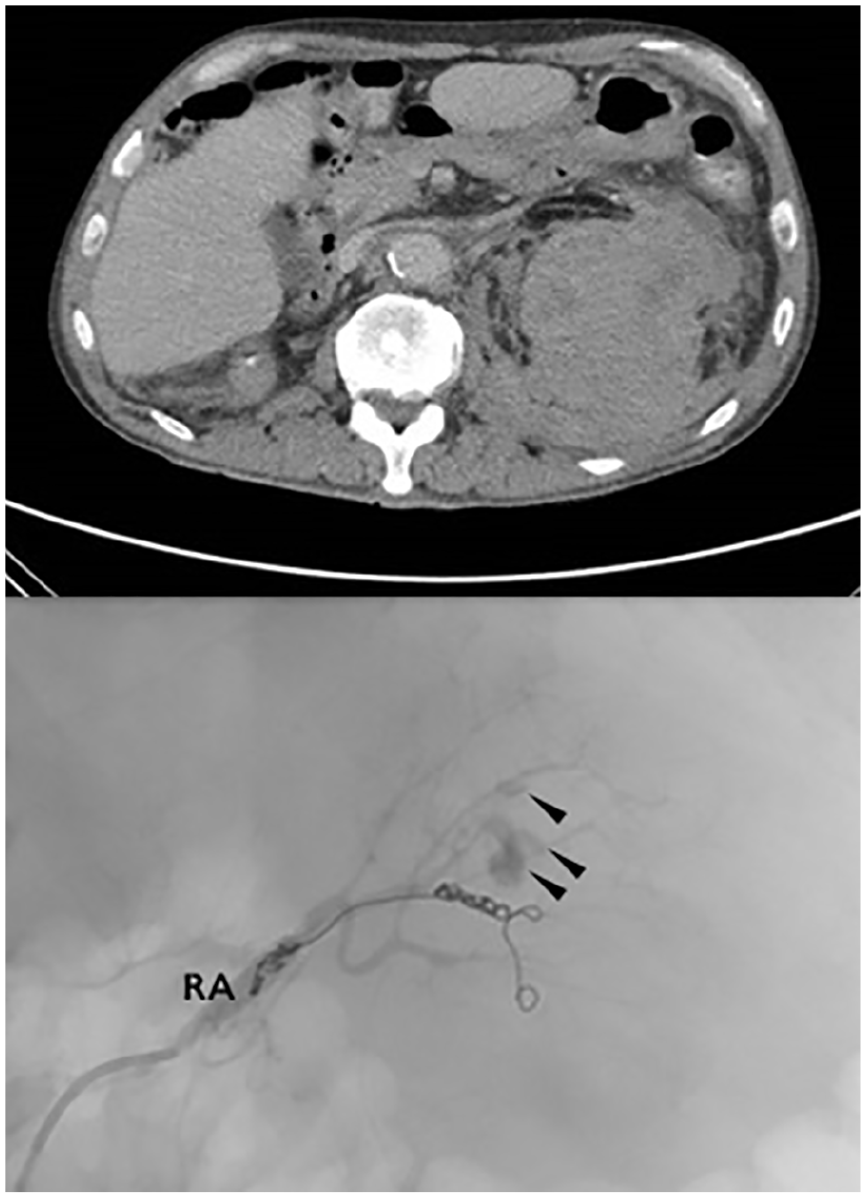
Severe left retroperitoneal bleeding. (a) Axial section of computed tomography scan of the abdomen and pelvis on post-RPG day 3, showing a large left perinephric haematoma, displacing the left kidney anteriorly. (b) Left renal artery angiogram on post-RPG day 5, showing multiple bleeding points (arrowheads) after initial attempt at selective angioembolisation. RA: renal artery.
Discussion
Most reports of retroperitoneal haemorrhage in the literature were spontaneous non-traumatic cases, sometimes termed as Wunderlich syndrome, attributable to various causes, such as ruptured angiomyolipoma, renal-cell carcinoma, cystic kidney diseases and anticoagulation therapy.1–4 Subcapsular and perirenal haematomas have been reported as rare complications of endourological procedures, 5 but retroperitoneal bleeding following RPG has not been described in the literature. This may be due to under-reporting of cases rather than the true incidence.
The aetiology of perirenal haemorrhage after endourological procedures has not been well defined. One likely cause would be guidewire trauma. Bansal et al. proposed that raised intrarenal pressure could lead to forniceal rupture and separation of the capsule from the parenchyma, resulting in haematoma formation. 6 Chronic kidney disease (CKD) was suggested by Kao et al. as a predisposing factor for perirenal haemorrhage, as such kidneys might be structurally weaker and more easily damaged than their healthy counterparts. 7 Other risk factors described in a systematic review included moderate to severe hydronephrosis, thinner renal cortex, presence of urinary tract infection and hypertension. 5 In our patient, the factors that could have contributed to the massive retroperitoneal bleeding included: (a) native ESKD kidneys, which were more fragile and predisposed to bleeding from minor trauma or raised intrarenal pressure during RPG; (b) small-calibre upper urinary tracts, requiring a greater syringe pressure to push the intraluminal contrast up into the kidneys; and (c) use of clopidogrel, although the risk of persistent platelet dysfunction was low after 7 days of discontinuation.
Sporadic reports have documented rare but serious complications of RPG, such as acute renal failure, anaphylactoid reaction to contrast, air embolism and ureteric and renal perforations.8–12 Guidewire trauma was excluded in our case, as it was not used. In our patient, a calyceal fornix might have ruptured. The presence of forniceal clubbing and pyelo-venous backflow suggested high intrarenal pressure from contrast instillation. Pyelo-venous backflow is the reflux of contrast out of the collecting system due to a small forniceal rupture, occurring at high intrapelvic pressures of around 80 mmHg in humans, although animal studies have suggested that it can occur at lower pressures.13,14 In a porcine model, the intrapelvic pressure required to cause intrarenal backflow is lower in hypoxic kidneys. 15 This is relevant, as chronic hypoxia is thought to be the final common pathway leading to ESKD. 16 The shrunken end-stage kidneys would most certainly have changes in their structural integrity, and this can be inferred from ultrasound elastography studies. Leong et al. demonstrated that CKD was associated with stiffer kidneys than healthy controls. 17 In another study, Lin et al. found that a change in renal elasticity was associated with rapid renal deterioration in CKD kidneys. 18 This collective evidence suggests that end-stage kidneys may be at higher risk of injuries, even at relatively low intrapelvic pressures in the case of RPG.
A valuable lesson from this case is that extra care must be taken when performing any interventions on end-stage kidneys. Endoluminal instillation of contrast should be slow and in small volumes under close fluoroscopic imaging guidance in order to avoid over-pressurising the collecting system. If the upper urinary tracts are small in calibre, the ureteral catheter may be advanced gently, over a guidewire, into the renal pelvis so that contrast can be instilled at lower pressures. These principles of safe practice could minimise the risk of contrast extravasation and avoid rupturing the calyceal fornices. The absence of haematuria in our patient was probably due to the anuric native kidneys. Massive retroperitoneal bleeding is rare and can be life threatening. The initial management will require prompt resuscitation, adhering to advanced life-support principles. Conservative management will usually suffice, as bleeding is often self-limited by the perirenal fascia, providing a tamponading effect. Renal artery embolisation should stop any active bleeding. Open nephrectomy is high risk and rarely indicated, being reserved only for cases of intractable bleeding.
In conclusion, massive retroperitoneal haemorrhage following RPG is an uncommon but potentially life-threatening complication. Special precautions must be taken when performing RPG in end-stage kidneys, which are fragile and prone to bleeding, in order to keep the intrarenal pressure as low as possible.
Footnotes
Acknowledgements
None.
Authors’ contributions
X.Y. wrote the first draft of the manuscript. All authors reviewed and edited the manuscript and approved the final version of the manuscript.
Availability of data and materials
Data sharing is not applicable to this article, as no data sets were generated or analysed during the current study.
Ethical approval
Singapore General Hospital does not require ethical approval for reporting individual cases or case series.
Informed consent
Written informed consent was obtained from the patients for their anonymised information to be published in this article
Conflict of interest
The authors declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The authors received no financial support for the research, authorship and/or publication of this article.
