Abstract
The cutaneous manifestation of dengue is a maculopapular blanchable erythema over the body that spares the palms and the soles. We report a case of serologically proven, uncomplicated dengue fever in a lady who developed macular morbilliform erythema with islands of sparing over the plantar regions of the bilateral soles on day 8 of disease. This phenomenon has not yet been reported in dengue literature.
Introduction
Singapore is hyperendemic for dengue, with all four serotypes of dengue existing in the local mosquito population. 1 Dengue can clinically present as a rash, classically described as a morbilliform erythema with islands of white that usually spares the palms and soles. 2 We present a report involving a 63-year-old lady with dengue fever, confirmed with laboratory tests, with a rash developing over the soles of the feet as part of the cutaneous manifestation of dengue. This is the first case report of this clinical sign in dengue.
Case report
The patient was a 63-year-old Chinese female with a past medical history of hyperlipidaemia on diet control and worked as a homemaker. She lived in a region that was having a dengue outbreak on the day of admission to hospital.
She presented to our local hospital with symptoms of fever for three days with postural giddiness, resulting in a fall and sustained trauma to her head and her shoulders. She had no joint or back pain. She had not recently travelled abroad. She had first seen a family physician for a fall and was found to have thrombocytopaenia, with a platelet count of 129×109/L, and was referred to our hospital to rule out dengue with intracranial haemorrhage.
Upon presenting to the emergency department, she was febrile with a core temperature of 38.1°C. A postural blood-pressure measurement was did not reveal any postural hypotension or narrow pulse pressure. Other physical signs found included a 3 cm bruise on her left forehead. She had no hepatomegaly or abdominal tenderness. There were no ascites, and the auscultation of the lungs was clear. There were no abnormal neurological signs. She did not have any rashes, and the tourniquet sign was negative.
A point-of-care screening test kit showed that the patient was dengue NS1 antigen positive and dengue immunoglobulin (Ig)M and IgG negative, and her full blood count showed a platelet count of 67×109/L, with normal haemoglobin and leucocyte values. Her coagulation profile showed an activated partial thromboplasmin time of 33.4 seconds and an international normalised ratio of 0.95. Her liver function tests showed a raised aspartase transaminase value of 163 mmol/L and an alanine transaminase value of 74 mmol/L. A non-contrast computed tomography scan of the brain did not show any intracranial haemorrhage. She was admitted to hospital for monitoring in view of her diagnosis of dengue fever and a fall resulting in a head injury. This was the first episode of dengue in her lifetime, as her IgG was negative.
The patient was monitored on the ward and placed on complete bed rest and on thrombocytopaenia precautions. Her full blood count was checked daily to assess her fitness for discharge. Her platelet trend is shown in Figure 1. She became afebrile on the fourth day of illness. She had been kept on strict bed rest until the eighth day of her illness, until her platelet count improved beyond 40×109/L, and she was subsequently allowed to ambulate freely.

Trend of platelets. Patient was admitted on the third day of illness. The bilateral plantar rash occurred on the eighth day of illness.
On the day 8 of illness, the patient developed a painless, erythematous, macular blanchable erythema involving the bilateral soles up to the ankles, with islands of sparing (Figure 2). The rash was neither pruritic nor painful. There were no other rashes on other parts of the body, including the palms, the face, the torso, the abdomen and the upper limbs. The oral mucosa had no petechiae, and she did not have any stigmata of other conditions known to cause rashes in the soles. The feet were not warm to touch. There was no fever or any other perturbation of her vital signs. There were no joint effusions, no evidence of uveitis, no oral ulcers and no oral petechiae. There was no desquamation of her palms or soles. There was no antecedent history of trauma. She had had no new medication and had not taken any supplements, except for intravenous infusions of Hartman’s solution and per oral omeprazole, which she had taken six years ago without any allergies. She had had no recent sexual activity. Epidemiologically, there were no outbreaks of Zika or Chikungunya in Singapore, and Singapore remains yellow fever free. She had no travel history, and there were no recent tick bites. Her platelet count was 40×109/L in the morning. She was not tested for other mosquito-borne infections, syphilis, or rickettsial infections, and no other blood cultures were taken, as there was no clinical indication to do so.
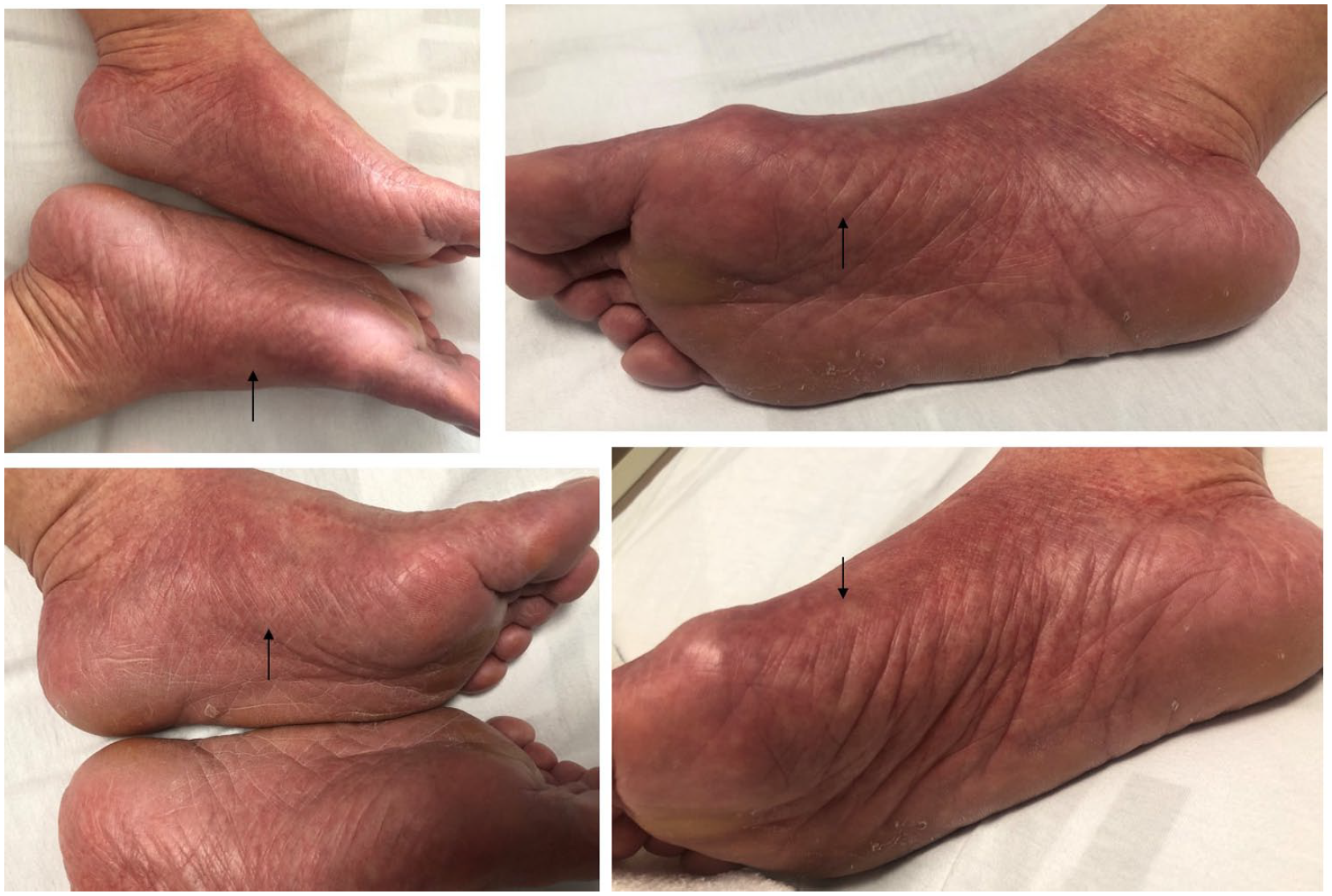
Macular morbilliform erythema seen from day 8 of illness. Notice the islands of sparing (solid arrows).
We had initially thought that she had put on her tight-fitting shoes (Figure 3), but after clarification with the patient, her attending nurses and the physiotherapists who saw her the day before and the day of the rash, she only wore comfortable rubber slippers, and these slippers were not tight fitting. The resolution of her rash is shown one week and four months later in Figure 4.

Footwear worn by the patient. The patient was wearing slippers (solid arrow). Notice that the rash extends beyond the shoe and stops below the ankles (dotted line).
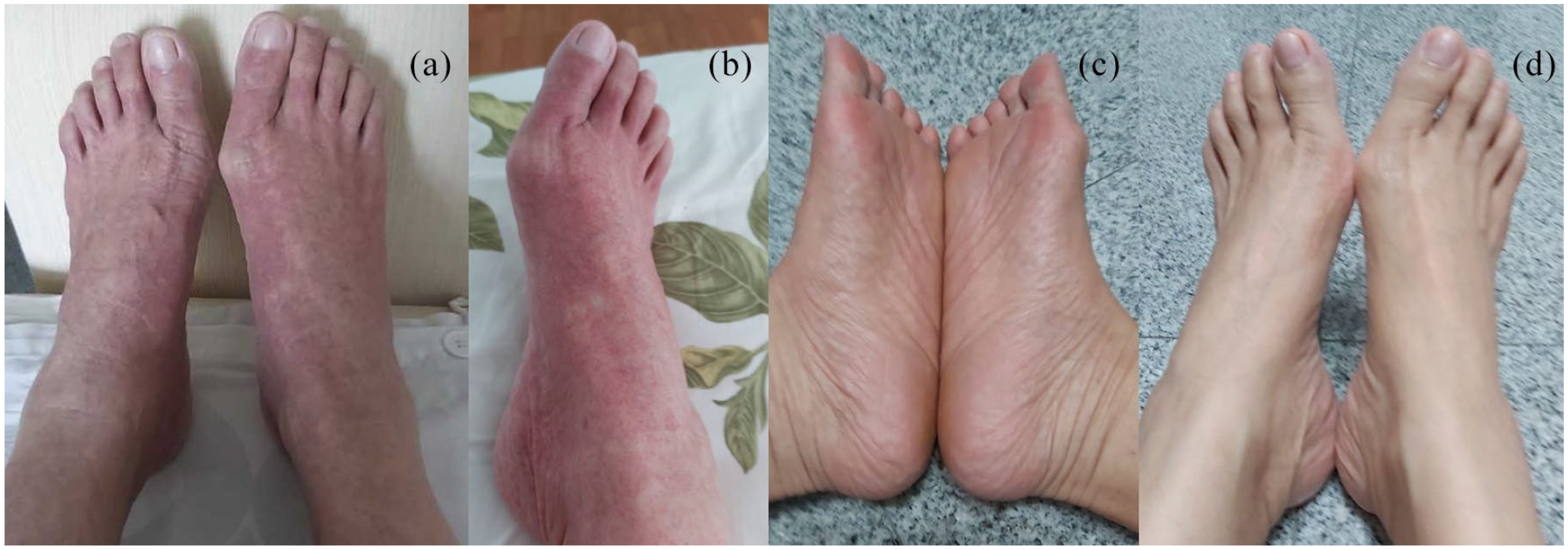
Improvement of rash (a) and (b) one week from discharge, and (c) and (d) four months from discharge with complete resolution.
This erythematous dermatosis improved without new medication, and she had no further inpatient complications. She had no symptoms or signs of dengue haemorrhagic fever and was not suffering from dengue shock syndrome. She was discharged two days later and with a platelet count of 75×109/L on the day of discharge.
Discussion
The specificity and the positive predictive value of the NS1 antigen for dengue has been reported as 100% and has been considered as equivalent to the polymerase chain reaction (PCR) for diagnosis of dengue. 3
Our patient was NS1 antigen positive and dengue serology negative, suggesting that her illness was the first episode of dengue she had in her lifetime and that she was diagnosed early in her illness, as evidenced by a lack of IgM antibodies towards dengue. We did not test the PCR for the specific serotype of dengue in this patient, as it did not influence clinical management.
The typical exanthem of dengue has been estimated to occur in 50–82% of all patients with dengue fever. 2 The rashes of dengue normally manifest three to four days after the onset of the fever. 4 As described in the current literature, this exanthem starts out as a transient flushing erythema before or during the first onset of symptoms followed by a maculopapular or morbilliform eruption which may eventually coalesce and form the characteristic ‘white islands in a sea of red’. 2 This exanthem has been known to spare the palms and the soles, and starts from the dorsum of the hand and feet and spreads to the arms, legs and torso and subsequently persists for days without desquamation. 2 There may be pruritis in 27% of patients. 2 This exanthem is thought to be immune mediated. 2 Cutaneous haemorrhagic manifestations on the skin such as a positive tourniquet sign, petechiae and purpura are more commonly seen in dengue haemorrhagic fever and dengue shock syndrome. 2
The most common involvement of the soles, in the setting of dengue infection, is swelling without erythema. 4 This has been reported in 12–62% of patients. 4 The presence of a rash has not been shown to be related to any increases in mortality or morbidity. 5 There has been one report, in a seven-day-old NS1-positive infant in Thailand, of petechiae and ecchymoses on the palms and soles in the setting of dengue shock syndrome, but this report did not show that the patient had the morbilliform rash of dengue. 6
Not all rashes involve the palms and soles. The differential diagnoses of such unusual rashes raise a limited list of differential diagnoses which have been previously described,7,8 which can be divided into infectious, autoimmune, primary dermatological, oncological, drug and toxin-related causes. Dengue, which is described in this report, in addition to other diseases such as arsenic 9 and mercury 10 poisoning, hand-foot syndrome from chemotherapy, 11 graft-versus-host disease, 12 erythema elevatum diutinum, 13 Mediterranean spotted fever 14 and even allergies to food 15 are now added to this list of differential diagnoses (Table 1). The bacterial and drug-related causes of such rashes are usually those which have potential for severe harm to the patient or to public health and need to be assessed. As our patient did not present with a rash upon admission and only upon the eighth day of illness, and was clinically improving upon rash onset, there was no indication for further assessment.
Differential diagnosis of rashes involving the soles and the palms.

Potentially life-threatening conditions or conditions of public-health significance.
Conclusions
In summary, we report a novel addition to the cutaneous manifestations of dengue. Second, dengue has joined the list of differential diagnoses in a patient with a rash over the soles of the feet.
Footnotes
Acknowledgements
None.
Authors’ contributions
T.B.H. reviewed the literature, conceived the case report, obtained written consent and drafted the manuscript. S.S. reviewed, edited and approved the final version of the manuscript.
Availability of data and materials
Data sharing is not applicable to this article, as no data sets were generated or analysed during the current study.
Conflict of interest
The authors declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Informed consent
Written patient informed consent was obtained from the patient.
Ethical approval
The institution does not require ethical approval for cases reports involving fewer than three people.
Funding
The authors received no financial support for the research, authorship and/or publication of this article.
