Abstract
There is currently little data regarding the ideal management for a patient who has undergone recent percutaneous coronary intervention (PCI) and subsequently develops dengue fever. Patients with recent PCI are at high risk of stent thrombosis with cessation of dual anti-platelet therapy. On the other hand, patients with dengue viral infection are at high risk of bleeding. Managing patients with recent PCI and dengue involves the delicate balancing of the risk of thrombosis and bleeding. Careful consideration of the timing of coronary intervention and the severity of the dengue infection is required. We describe the management of the anti-thrombotic therapy in three different patients with dengue infection and recent PCI and discuss our approach to managing such patients.
Introduction
Coronary artery disease is prevalent within South-east Asia, and there has been an increasing number of percutaneous coronary intervention (PCI) procedures performed with concomitant anti-thrombotic use.1,2 At the same time, in these countries, the prevalence of dengue infection is high due to the endemic nature of the disease.3-5
Patients undergoing PCI require a period of dual anti-platelet therapy (DAPT) post-procedure, depending on the stent used as well as the clinical scenario. Omission of anti-platelet agents is associated with potentially fatal stent thrombosis. The patient with dengue infection will typically have a drop in platelet count at the diathesis phase at day 3 to 5 of fever. The risk of bleeding is the highest toward the end of febrile period and during the first 2 days after resolution of fever. When managing a patient with a recent PCI who concomitantly develops dengue infection, the physician will have to consider both the risks of bleeding from dengue 6 as well as the risk of thrombosis from cessation of anti-platelet therapy. 7 In this paper we describe three such cases and discuss a possible algorithm for anti-thrombotic management during acute dengue infections.
Case series
Case 1
A 63-year-old male patient was admitted with chills and myalgia. He had a high-grade fever for 4 days. On admission he was febrile but hemodynamically stable. Laboratory analysis on admission showed hemoglobin 14.9 g/dl, hematocrit 39%, platelet count 75,000/mcL, and positive dengue antigen. He was diagnosed with dengue. Two months prior to the admission he developed stable angina and underwent elective cardiac catheterization, which revealed triple vessel coronary disease. Over two staged procedures (the last occurring 1 week prior to the current admission), a total of four drug-eluting stents (DES) and one bare-metal stent (BMS) were implanted in all three of his coronary arteries. He routinely consumed aspirin 100 mg once daily (OD) and clopidogrel 75 mg OD.
On the second day of hospitalization the patient’s platelet count went down to 46,000/mcL without any sign of active bleeding. Aspirin and clopidogrel were halted. The platelet count rose to 55,000/mcL on the third day, and on the fourth day increased to 97,000/mcL. Clopidogrel 75 mg OD was started on fourth day, and aspirin 100 mg OD was started on fifth day. On follow-up 6 days after discharge, the patient was in good condition without any signs of bleeding (see Figure 1).
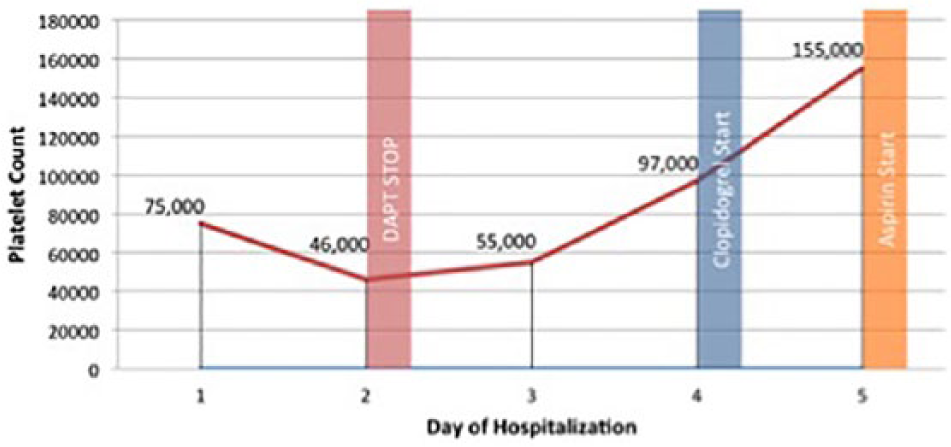
Platelet changes and anti-platelet management in Case 1
Case 2
A 77-year-old male patient was admitted for lethargy and fever for 3 days. On admission he was febrile but hemodynamically stable. His initial hematocrit was 40% and platelet count was 91,000/mcL. He was suspected to have dengue infection, which was subsequently confirmed by a positive dengue antigen.
Seven months previous, he underwent percutaneous coronary intervention with one DES to the right posterior descending artery and right posterior lateral artery, respectively. He was planned for 1 year of DAPT with aspirin and clopidogrel. Four years prior, he also had DES implantation at the bifurcation of his LAD/D1 for angina.
On the fourth day of hospitalization, his platelet count dropped to 43,000/mcL. There were no signs of active bleeding. Aspirin and clopidogrel were stopped. His platelet counts reached a nadir of 19,000/mcL on the seventh day. The platelet count rose to 55,000/mcL on the ninth day, on which he was loaded with aspirin 300 mg and clopidogrel 300mg followed by a regular dosing. On outpatient follow-up on day 12, the patient’s platelets had recovered to 161,000/mcL and he was stable.
Case 3
A 55-year-old male patient was admitted with fever, rigors and muscle aches for 3 days. On admission he was febrile, hemodynamically stable, with spontaneous bruising noted on his arms. Laboratory analysis showed hemoglobin 15.4 g/dl, platelet count 83,000/mcL, white blood cell count 5,900/mcL, and positive dengue IgM antibody. He was diagnosed with dengue with warning signs. He was previously diagnosed with unstable angina 2 months prior to this admission, underwent cardiac catheterization and was found to have one-vessel coronary disease. At that time he was implanted two DES in ostial to proximal LAD. He routinely consumed aspirin 100 mg OD and clopidogrel 75 mg OD.
Aspirin and clopidogrel was immediately stopped after the patient was diagnosed with dengue with warning signs. Further hydration was given with Hartman’s and normal saline. On the next day his platelet count was dropped to a minimum of 38,000/mcL, and he developed even more ecchymosis on his forearms. His platelet was gradually increasing and on day 5 of hospitalization the platelet count was 127,000/mcL. Aspirin 100 mg OD and clopidogrel 75mg were restarted on this day (see Figure 2).

Platelet changes and anti-platelet management in case 3.
Discussion
We describe the management of the anti-thrombotic therapy in different scenarios of concomitant dengue and recent PCI. There is currently little evidence regarding the ideal management for the patient who has recent PCI and develop dengue fever. Patients with recent PCI are at high risk of stent thrombosis without DAPT.8,9 On the other hand, patients with dengue viral infection are at high risk of bleeding.10-12 Pesaro et al. published several recommendations on the topic but these were based primarily on expert opinion. 7 In summary, Pesaro’s recommendations were as follows: (a) stop all anti-platlets in dengue hemorrhagic fever, (b) continue both anti-platelets in patients with less severe dengue and high risk of thrombosis unless platelet <50,000/mc, and (c) hold at least one anti-platelet if dengue and low thrombotic risk. 7 Managing patients with recent PCI and dengue involves the delicate balancing of the risk of thrombosis and bleeding. Their management should consider the timing of coronary intervention and the severity of the dengue infection.13,14
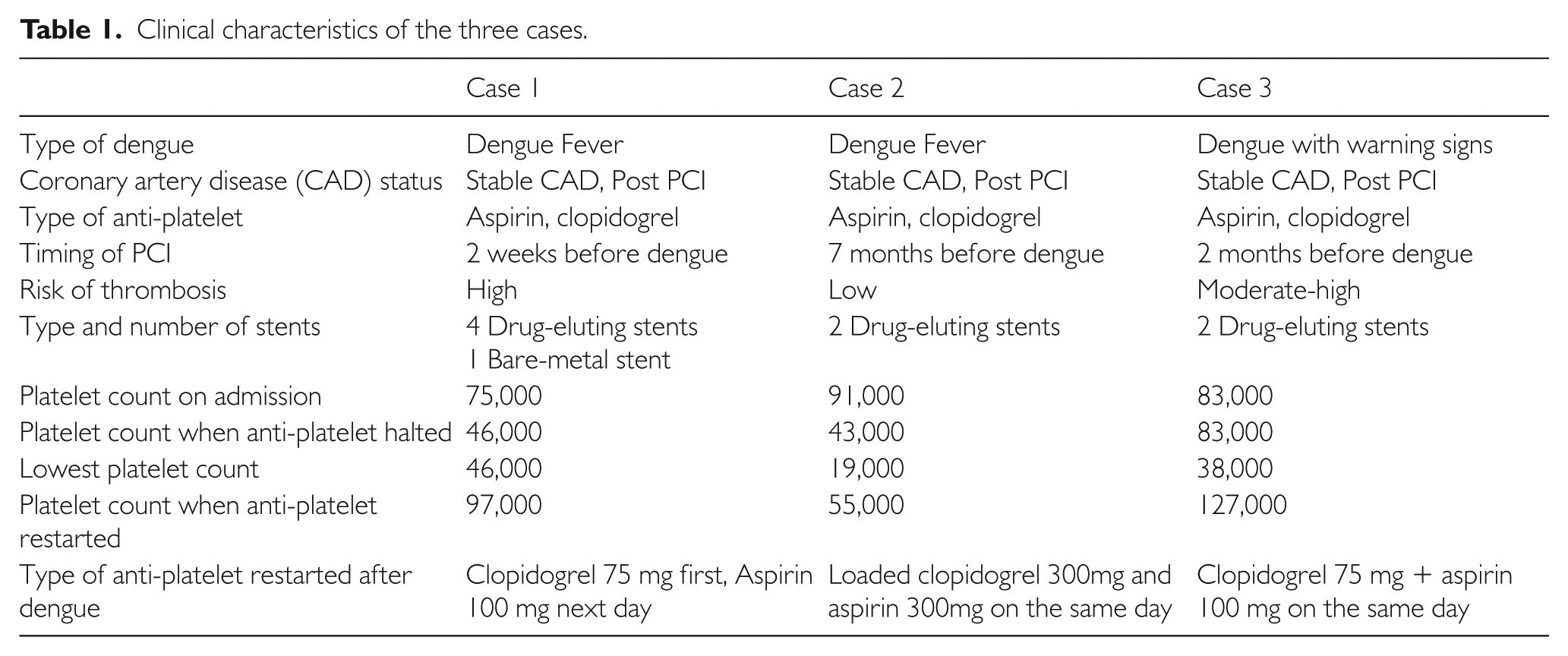
Table 1 summarizes the clinical characteristics of the three cases. The three cases describe different situations of post-PCI patients who develop dengue fever. Timing of coronary intervention and the number of coronary stents implanted make a difference in thrombotic risk stratification. Current guidelines recommend stable PCI patients to take DAPT for at least 6 months after DES implantation; this reduces the risk of adverse events from 3.6% to 0.5%.7,15 The risk of thrombosis is highest in the initial phase after stent implantation, and interruption of anti-platelet therapy during this time puts a patient at high risk of stent thrombosis (even temporary discontinuation within this time period might be associated with higher thrombosis rate). Coronary intervention with multiple stents also increases the risk of stent thrombosis.
Clinical characteristics of the three cases.
The severity of dengue infection also impacts management. The patient in case 3 was diagnosed with dengue with warning signs, and all anti-platelet therapy was halted shortly after the diagnosis was made in view of the high bleeding risk. In cases 1 and 2, bleeding manifestations were not observed and the anti-platelet regime was halted once the platelet count fell below the cut-offs discussed below.
Recommendations
We propose an algorithm to guide post-PCI patients with dengue infection (Table 2). Risk stratification by thrombotic and bleeding risks should be performed. The high thrombotic risk category includes, among others, patients with recently implanted DES ⩽3months or BMS/angioplasty ⩽1 month, complex interventions (e.g. left main or bifurcation stenting) and use of multiple stents (especially if small stents and/or long stents). The low thrombotic risk category includes, among others, patients with implanted DES >3 months or BMS/angioplasty >1 month. These criteria are not exhaustive and are based on expert opinion; this should be determined by the clinician on a case-by-case basis. All patients with clinically significant bleeding should have their anti-platelet therapy stopped, especially if the platelet count is <100,000/mcL. For those without any bleeding tendencies and high thrombotic risk, we propose a cutoff of <50,000/mcL, similar to Pesaro et al., who recommended a cutoff of 50,000/mcL based primarily on expert opinion. 7 For those with low thrombotic risk, a higher cutoff of 70,000/mcL may be considered as it may be difficult to predict the nadir of the drop in platelet levels in the initial stages. Another possible option available to the clinician is the sequential cessation of anti-platelet therapy (i.e. cessation of one anti-platelet first). There is evidence available for a shorter duration of DAPT (at least 1 month) for certain DES (e.g. the polymer-free and carrier-free drug-coated BioFreedom); in such special situations, the earlier cessation of DAPT may be considered on a case-by-case basis.
Recommended antiplatelet management in post-PCI patient with dengue infection.

Option of stopping one anti-platelet first may also be considered.
In case 1, DAPT was restarted sequentially without loading, while in case 2, both anti-platelets were loaded concurrently. In case 3, both anti-platelets were restarted concurrently but not loaded. This reflects the varying practices among clinicians in an area without much prior evidence. In general, we recommend that in the high thrombotic risk category, DAPT should be loaded once safe and if there are no contraindications; in the low risk group, loading is less of a necessity.
These recommendations are a collation of our local clinical experience and further research would be needed to validate this workflow. The balance between the risk of stent thrombosis and bleeding is a fine balance that the clinician has to manage, and these risks should always be communicated clearly to the patient.
Limitations
The limitations of our study include the small number of cases. Our findings may not be generalizable to other populations and will need to be further validated. Nonetheless, these findings provide reasonable clinical recommendations for the clinician to consider when faced with such a difficult scenario.
Conclusions
In conclusion, we describe the management of the anti-thrombotic therapy in three different patients with dengue infection and recent PCI and discuss our approach to managing such patients.
Footnotes
Author contributions
All authors contributed to the design of the study and writing of the manuscript.
Availability of data
Data sharing is not applicable to this article as no datasets were generated or analyzed during the current study.
Declaration of Conflicting Interest
The authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Ethical approval
Not applicable for case series.
Informed Consent
Written informed consent was obtained from the patients for their anonymized information to be published in this article.
