Abstract
Little is known about the new Diagnostic and statistical manual of mental disorders, fifth edition, diagnosis of Avoidant–Restrictive Food Intake Disorder (ARFID). Without sufficient knowledge about the disorder, its detection and treatment are hampered. This study highlights eight cases diagnosed with ARFID between 2013 and June 2016 who presented to our treatment facility, the only specialized Eating Disorders program in Singapore. Informed consent was obtained from the patients and their parents, and their case notes retrieved and reviewed. There were five males and three females, with ages ranging from 15 to 39 years, a mean age of 20 years and body mass index of 16.1 kg/m2 at time of diagnosis. The presentation of cases was heterogeneous, including selective eating behaviors, very restricted food choices, anxiety towards specific foods and with comorbid mood symptoms. A majority of the cases displayed ARFID symptoms early in childhood, suggesting the need to inform parents, educators and healthcare professionals. The study also found a high treatment default rate amongst the patients, warranting further investigation. Due to the heterogenous presentation of ARFID, the authors appeal for further exploration to be carried out and more to be done to increase the awareness of this condition in both the medical profession and general population.
Introduction
Avoidant–Restrictive Food Intake Disorder (ARFID) is a new diagnostic category in the Diagnostic and statistical manual of mental disorders, fifth edition (DSM-5). Prior to the introduction of DSM-5, patients who failed to meet sufficient nutritional or energy needs because they ate only certain food types or avoided certain foods due to color, texture, smell or consistency, or due to abdominal pain or fear of vomiting were often put under the DSM-5 diagnosis of Feeding Disorder of Infancy or Early Childhood. The issue was that this diagnosis was not well-known amongst doctors and was rarely used. Furthermore, the diagnostic criteria required patients to have an age of onset lower than six years or to suffer from weight loss, further excluding some of the aforementioned patients. 1 At other times, they were put into the very general and diverse group of Eating Disorder-Not Otherwise Specified, which is often also utilized for patients who cannot meet the full criteria for Anorexia Nervosa and Bulimia Nervosa, even though this group of patients did not display typical features of either.
With the introduction of DSM-5 in 2013, ARFID is now used for this group of patients. This new category side-steps the challenges previously faced and enables this condition to be better studied. It is described in DSM-5 as an eating or feeding disturbance (e.g. apparent lack of interest in eating or food; avoidance based on the sensory characteristics of food; concern about aversive consequences of eating) as manifested by persistent failure to meet appropriate nutritional and/or energy needs associated with one (or more) of the following:
Significant weight loss (or failure to achieve expected weight gain or faltering growth in children);
Significant nutritional deficiency;
Dependence on enteral feeding or oral nutritional supplements;
Marked interference with psychosocial functioning. 2
Our study aims to provide a descriptive report on the clinical profile of patients diagnosed with ARFID in Singapore between 2013 and 2016, since the first publication of DSM-5 in 2013. We will describe the clinical characteristics, including dietary history, risk factors, co-morbidities, physical findings and investigations to understand ARFID better. It will also add depth and breadth to the existing ARFID literature, especially for Asia, where there is none, to our knowledge.
Case report
Patients presenting to Singapore General Hospital (SGH), a tertiary hospital in Singapore with the largest eating disorder treatment program, were recruited for this study. Patients who received inpatient or outpatient assessment and treatment by a consultant psychiatrist in SGH, and who had been diagnosed with ARFID between 2013 and June 2016 were identified through the SGH Department of Psychiatry Eating Disorders patient database. The patients were contacted over the phone regarding participation in the study. Ethical approval was obtained from SingHealth Centralized Institutional Review Board and informed consent was obtained from all eight patients involved in this study. If the patient was below the age of 21 years, consent was obtained from their parents as well. The researchers retrieved and reviewed the patients’ medical records, obtaining qualitative clinical characteristics relevant to the study.
There were five males and three females, with ages ranging from 15 to 39 years and a mean age of 20 years at time of diagnosis. The patients had a mean body mass index (BMI) of 16.1 kg/m2 at time of presentation.
Presentation of symptoms
The majority (seven) of the patients began displaying symptoms of ARFID in early childhood and adolescent years, and one patient (P6) in adulthood.
The patients who displayed symptoms during childhood reported selective eating behaviors, with very restricted food choices (Table 1). They also reported anxiety with certain foods, in which exposure to these foods will contribute to the experience of nausea, and at times even fear of vomiting.
Clinical Characteristics of the Patients.
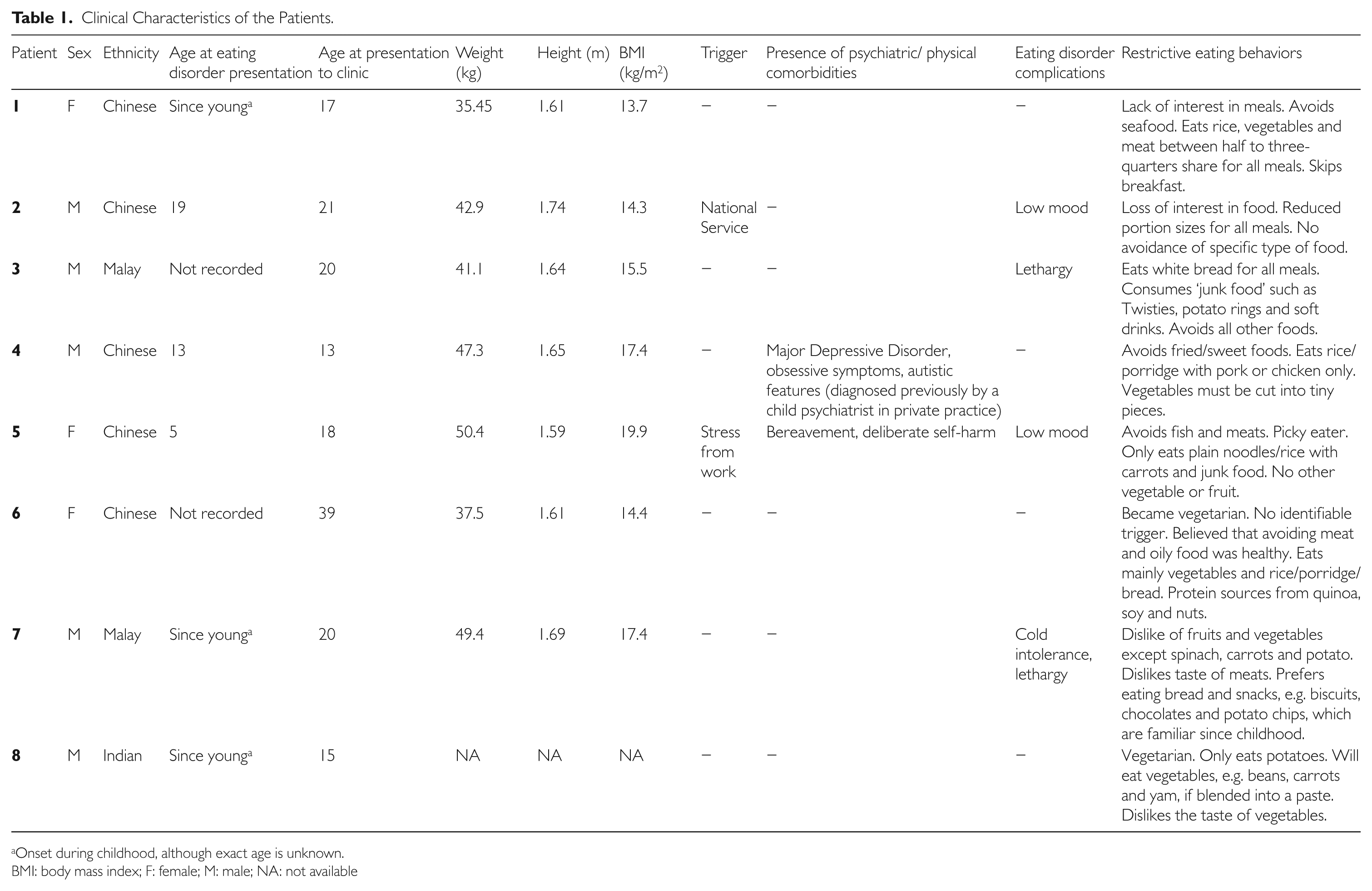
Onset during childhood, although exact age is unknown.
BMI: body mass index; F: female; M: male; NA: not available
The disturbance in these patients’ eating would continue throughout primary and secondary school, and for two of them (P3 and P7), into adulthood. Four patients (P1, P4, P5 and P8) sought treatment in their adolescent years, three patients (P2, P3 and P7) in early adulthood and one patient (P6) in her 30s. Two patients (P3 and P7) were diagnosed prior to enlistment for National Service, a compulsory two-year military service for males in Singapore. These two male patients were identified during the pre-enlistment medical screening and were referred to SGH for assessment of an eating disorder. One of the patients (P3) had a disturbance in eating, with a dietary intake restricted to white bread alone, while the other (P7) disliked fruits, vegetables and meats and restricted himself to bread, packaged snack food and other processed food.
Two other patients (P1 and P4) were referred for assessment by their secondary school, who noticed them to be below the healthy weight range for their age group. Three patients (P2, P4 and P8) were referred from other subspecialty physicians who were concerned about their low body weight and disturbance in eating patterns.
For seven out of eight patients, the duration of illness appeared chronic and longstanding, with an average of more than 10 years. The exception was P2, a 20-year-old national serviceman, who developed ARFID while serving his National Service one year prior to seeking treatment. He presented with loss of interest in food and worsening of appetite, precipitated by irregular eating hours and perceived unpalatable food rations provided by his army camp. His disturbance in eating became persistent leading to significant weight loss and necessitated admission to the hospital due to lower limb swelling secondary to hypoalbuminemia secondary to ARFID.
Clinical characteristics
One patient (P4) had been diagnosed previously with Major Depressive Disorder and Autism Spectrum Disorder by a child psychiatrist in private practice. Another patient (P5) had a history of deliberate self-harm during a period of bereavement following the demise of her mother.
Two patients (P2 and P5) presented with low mood at time of assessment and, based on clinical interview and assessment, did not amount to a Depressive Disorder.
Two patients (P3 and P7) experienced physical complications of the illness with lethargy and cold intolerance.
Two patients had identifiable triggers for their eating disorder, one (P2) citing National Service and the other (P5) citing work-related stress.
The criteria specific for ARFID that were commonly present for many of the patients were the apparent lack of interest in eating or food, and often also an avoidance of food that was based on sensory characteristics of food, such as taste.
The mean BMI of 16.1 kg/m2 of the sample population was below the expected healthy weight range. The illness has caused impairment in psychosocial functioning, necessitating hospitalization in one patient (P2), and causing difficulty in engaging during social events such as sporting activities in other patients.
Long-term progress
Of the eight patients who have been assessed and diagnosed with ARFID, all were referred to a dietitian for further assessment and nutritional rehabilitation. Two patients were referred to a psychologist.
Two patients (P2 and P6) managed to reach a BMI within the healthy weight range after returning regularly for treatment and working closely with the multidisciplinary team consisting of a psychiatrist, psychologist and dietitian. The remaining six patients subsequently defaulted follow-up appointments.
Discussion
There are several clinical implications of the findings gathered from our study. To our knowledge, this is the first study to describe a cohort of patients with ARFID in an Asian population. The cases presented highlight the heterogeneous presentation of this condition. Someone who is unfamiliar with this condition may attribute these behaviors to simply ‘picky eating’ as they lack the hallmarks of more established eating disorders such as body image distortion, bingeing and low BMI. This is especially so if the person presents before there are any medical complications. The majority of the patients we presented had their onset of illness in childhood; however, their condition was discovered much later.
For many, their first point of contact may have been their family physician or general pediatrician. As this condition is relatively ‘new’, many doctors may not be aware of it and do not ask questions that would unmask it. This then leads to unpredictable referral and treatment patterns which could ultimately result in a disjointed care plan. 3 In order to overcome this, more should be done to increase the education and awareness of this condition in both the medical profession and the general population. It is also important that parents know the difference between regular picky eating and when it could be ARFID. For those in healthcare, having regular interdisciplinary rounds and hospital talks on ARFID could help raise awareness about this condition. In particular it would be good to target the people most likely to come into contact with such cases such as dietitians, developmental pediatricians, gastroenterologists, psychologists and psychiatrists.
The actual prevalence of this disorder is still not known, in part due to the fact that there has been very little research on rates of eating disorders in very young children. 4 In order to get a better picture of the actual prevalence of this condition we will need well-designed prospective surveillance and population studies.
Some studies have suggested that other disorders, such as anxiety disorder, obsessive–compulsive disorders, attention deficit disorders and autism spectrum disorders may be associated with ARFID. 5 More research is needed to see whether these conditions should be considered risk factors for the development of ARFID. There have also been observations that some patients with an initial diagnosis of ARFID eventually get reclassified as having anorexia nervosa. 6 Future research could help shed light on whether there are predictors that are associated with the development of anorexia nervosa in the course of their illness.
Reasons for the high default rate in our cohort also need to be systematically explored further. It is unclear whether it is contributed by the lack of evidence-based treatment recommendations, or whether patients do not regard their eating pattern as a problem, having presented for treatment many years after onset of the disorder.
Conclusion
With more awareness about the existence of this condition, it is hoped that patients with ARFID will get timely and appropriate care which will lessen the physical and psychological impact that is inevitable if left untreated. More research is needed to assess outcomes and evaluate effectiveness of different interventions.
Footnotes
Declaration of conflicting interests
The authors declare that there is no conflict of interest.
Ethical approval
Ethical approval to report these cases was obtained from SingHealth Centralized Institutional Review Board.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
