Abstract
Background:
Studies evaluating nursing educational initiatives in rapid tranquillisation procedures are lacking.
Objective:
This pilot study in a public hospital in Singapore evaluated the effect of an educational training intervention on knowledge and confidence of nurses using rapid tranquillisation in two medical wards.
Method:
The study design was a pilot pre- and post-test single-group design on a voluntary sample of 75 nurses. The educational training intervention comprised of a 60 min interactive presentation followed by a small-group-based case discussion conducted by an advanced nurse practitioner. Knowledge was measured using a ‘test the knowledge’ questionnaire; a Likert scale measured perceived level of confidence.
Results:
The knowledge score (overall score = 11) was significantly improved from pre-training (average score: 5.1 (standard deviation, 1.3)) to post-training (average score: 8.1 (standard deviation, 1.8)), t = −12.61, p < 0.001. The participants were more confident after training (p < 0.001).
Conclusion:
This study has shown that a classroom training intervention of nurses in rapid tranquillisation procedures improved knowledge and confidence in dealing with patient violence in hospitals and added to the safe practice of rapid tranquillisation. Further studies evaluating the long-term and clinical impact of training with more rigorous study designs are needed to replicate these promising findings.
Introduction
Violent behaviour towards health care workers is an emergency situation that calls for prompt management, with emergency department and psychiatric wards being the most violent hospital environments.1–4 Medical and surgical wards are other settings in which these behaviours are commonly encountered, and nurses are the professional group at highest risk. 5 A study in Singapore revealed that in excess of 70% of healthcare workers from public hospitals reported experience of aggression or violence from patients and their families. 6 Violent behaviours commonly occur in patients with physical illnesses, delirium, dementia, learning disability, antisocial or borderline antisocial personality disorder, psychosis and other psychiatric illnesses or substance use disorders.7–9 Moreover, organisational procedures and difficult interactions between professionals, patients and patient visitors can increase the likelihood of patient and visitor violence.5, 10
Violent patients may be subject to rapid tranquillisation, which is defined by the National Institute for Health and Care Excellence (NICE) guidelines as, ‘Use of medication by the parenteral route (usually intramuscular or, exceptionally, intravenous) if oral medication is not possible or appropriate and urgent sedation with medication is needed’ and should only be considered once de-escalation and other strategies have failed and there is potential for harm to the patient or others if no action is taken. 11 Benzodiazepines and antipsychotics, which are commonly used in this procedure, carry serious drug-related adverse effects, including severe respiratory depression, extrapyramidal side-effects and cardiac arrest.8, 12–16 Therefore, monitoring of patients after rapid tranquillisation is pertinent for early detection of adverse effects.
All too often, rapid tranquillisation may be administered by staff with little or no awareness of serious drug-related risks or monitoring requirements. Verbal de-escalation techniques may negate the use of psychotropic medications but this seldom occurs if nursing staff are not empowered through training. Therefore, the challenge in management of violent behaviours may be compounded by poor staff training and inadequate understanding of the various conditions and factors that play an interactional role in the genesis of violence and medication-related risks. Arguably, patient safety is paramount in rapid tranquillisation, which is a high-risk intervention often used with physical restraint.17, 18
In 2017, Changi General Hospital’s policy on rapid tranquillisation was updated to include additional safeguards for patient safety. These included cardiac monitoring when using antipsychotics, enhanced care after rapid tranquillisation, nursing monitoring of clinical parameters and maximum daily dosing for adults and older adults. A review of the literature on rapid tranquillisation training and practice was undertaken to facilitate policy updates and revisions. The need for specific training in rapid tranquillisation was exemplified by an Irish study 19 of a mental health nursing practice, in which 53% of nurses questioned reported that they had received no formal training in rapid tranquillisation. Studies evaluating the effects of nursing training in rapid tranquillisation are lacking, to the best of our knowledge, and the current study was designed to evaluate the effects of an educational initiative on knowledge and confidence of nurses in the usage of rapid tranquillisation procedures. Two international experts with previously published research on rapid tranquillisation were approached by the first author in January 2017, to assist with the current study on nursing training.
This pilot study among nurses aimed to evaluate the effect of educational training intervention on knowledge and confidence of nurses using rapid tranquillisation to manage violence in patients in two acute medical wards. We hypothesised that participants would have improved knowledge and confidence in the management of violence using rapid tranquillisation after attending the educational training intervention. The usefulness of the training was also evaluated.
Methods
The study design was a pilot pre- and post-test single-group design on a voluntary sample of nurses in two participating medical wards. These wards were identified because the likelihood of violence was high.
All nursing staff working in the two participating medical wards in various nursing categories were eligible to attend the training session. No exclusion criteria were applied.
The SingHealth Centralised Institutional Review Board, Singapore, was contacted by the first author and exemption from a formal application for ethical approval was confirmed, as this study was an educational improvement initiative.
Our educational package comprised a training intervention session conducted by an advanced nurse practitioner, who has expertise in conducting nursing training in rapid tranquillisation. Eleven such sessions were conducted during the 2 month study period to ensure maximum participation by nurses working in the identified wards. Electronic invitations were circulated to the nursing managers, along with a timetable for the training sessions; participants were scheduled to attend one of 11 sessions. Participants received written information of the study and verbal consent to training and participation was obtained at the start of the training intervention to facilitate voluntary participation.
In early May 2017, we conducted a pre-pilot test run of the educational package, with administration of pre- and post-training questionnaires to 11 nurses from the two medical wards.
The nursing training consisted of a 60 min interactive presentation and a small-group case-based discussion. The interactive presentation was combined with case examples to reinforce learning and facilitate critical thinking. At the end of the presentation, participants were engaged in two case-based scenarios as a targeted small-group activity to facilitate integration of knowledge and application to clinical practice.
Pre- and post-training questionnaires were administered at the start and end of training. An outline of the training content is listed in Table 1.
Content of training course.

Emphasis was placed during training intervention on nursing monitoring of patients after rapid tranquillisation.
The pre- and post-study data were collected at the start and end of the training sessions. A survey in a paper questionnaire with components on demographic data and perceived level of confidence in managing violent patients using a Likert scale of one (not at all confident) to five (very confident) was used. A higher confidence score indicates greater knowledge of rapid tranquillisation procedures. Knowledge was tested using ‘test the knowledge’ questionnaire in a predominantly true-or-false question format. A final section on evaluation of the usefulness of the training was also included. All data were anonymised.
Improvement between pre- and post-test knowledge scores was tested using McNemar’s test. Overall knowledge score was calculated by summing the number of questions (Q1, Q2.1, Q2.2, Q3.1, Q3.2, Q3.3, Q4a.4A, Q4a.4B, Q4b.4A, Q4b.4B and Q4c) answered correctly, with a maximum overall knowledge score of 11. The pre- and post-test knowledge scores were then compared using the paired t test, and the mean (standard deviation (SD)) score was presented. Subgroup analysis of registered nurses and other nursing staff on pre- and post-test knowledge scores was also conducted. An internal consistency measure of the questionnaire was undertaken using Cronbach’s alpha. Confidence of participants before and after training was compared using the Wilcoxon signed rank test. Median and interquantile range scores of confidence were also presented. Statistical significance was considered for a two-tailed p < 0.05. Statistical analysis was performed with SPSS statistical software, version 19.0 (IBM Corp., Armonk, NY, USA).
Results
A total of 75 members of nursing staff in various categories attended the course and completed the study pre- and post-test questionnaires. Table 2 shows the results of participants’ demographics.
Demographics of study participants.
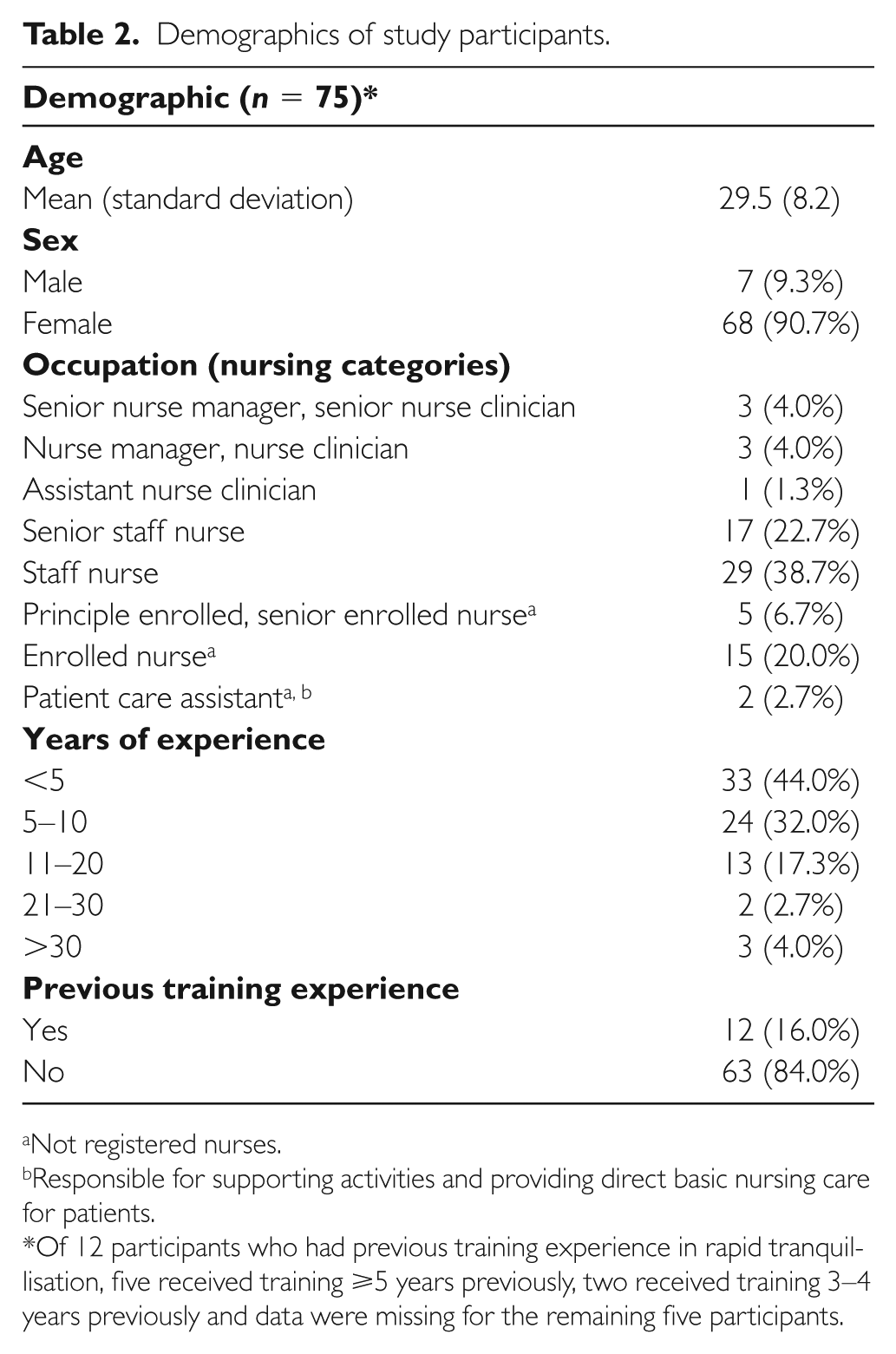
Not registered nurses.
Responsible for supporting activities and providing direct basic nursing care for patients.
Of 12 participants who had previous training experience in rapid tranquillisation, five received training ⩾5 years previously, two received training 3–4 years previously and data were missing for the remaining five participants.
Overall, the response score on knowledge was significantly improved from before training with an average score of 5.1 (SD 1.3) to after training, with an average score of 8.1 (SD 1.8), t = −12.61, p < 0.001. Breaking the questions down, the participants who answered the questions correctly after training showed statistically significant improvement on all questions, p < 0.05, except for question 4b.4B (Table 3).
Test scores before and after training.

Results showed the percentages and frequencies that the participants who ranked the correct order for all the five steps. For each individual step, results showed the percentages and frequencies that the participants correctly ranked the particular step number.
The medical emergency team in Changi General Hospital is a team of clinicians trained in advanced acute care that provide rapid urgent and emergent care to non-intensive care unit patients anywhere in the hospital setting with the intent of preventing hospital complications, especially cardiac arrests.
Test statistic: t value.
The internal consistency measurement of the study questionnaire was undertaken using Cronbach’s alpha; this revealed a score of 0.71.
The training was significant in enhancing the participants’ confidence in managing patients with violent or aggressive behaviour (pre-training, median score 3.0, interquantile range (2.0–4.0) versus post-training 4.0 (4.0–4.0) respectively, z = −7.03, p < 0.001).
Analysis of feedback revealed that 73 out of 75 participants (97.3%) evaluated the training as both valuable and useful.
As the participants were from varying nursing categories, a subgroup analysis of registered nurses and other nursing staff was conducted. Both groups of nurses, separately, showed a statistically significant improvement in the overall response scores. Registered nurses improved from an average pre-test score of 5.2 (SD, 1.2) to a post-test score of 8.2 (SD, 1.6), t = −5.82, p < 0.001. Other nursing staff improved from an average pre-test score of 4.7 (SD, 1.5) to a post-test score of 7.8 (SD, 2.1), t = −3.84, p < 0.001.
Regarding the question 4b.4B, we found that both registered nurses and other nursing staff showed no statistically significant difference from pre-test to post-test. The proportion of other nursing staff who answered this question correctly had increased from 77.3% pre-test to 90.9% post-test (X2 = 0.80, p = 0.371); the proportion of registered nurses who answered this question correctly had increased from 83.0% pre-test to 88.7% post-test (X2 = 0.57, p = 0.450).
Discussion
The findings of this study confirms the hypothesis that nurses from the two medical wards in the study were less knowledgeable and less confident about rapid tranquillisation prior to training intervention. After the intervention, there were significant improvements in both knowledge and confidence in managing violence using rapid tranquillisation. In this study, there was a statistically significant improvement in responses to all the questions, with the exception of question 4b.4B., which concerned cardiovascular adverse effect monitoring following administration of haloperidol. The proportion of nurses who answered this question correctly had increased from 81.3% pre-test to 89.3% post-test; however, the result was not statistically significant.
When a subgroup analysis was conducted between registered nurses and other nursing staff, the difference in overall knowledge score pre- and post-test was found to be significant for both registered nurses and other nursing staff, with the exception of question 4b.4B. With regards to this particular question, both registered nurses and other nursing staff had shown an improvement from pre-test to post-test score but this was not statistically significant, suggesting that the difference in nursing categories did not affect the response score to this question.
Notably, 84% of the participants in this study had no prior training in rapid tranquillisation. The paucity of prior training observed in this study is consistent with previous research findings on the management of violent patients.1, 8 In our study, 44% of participants had less than 5 years of work experience. Thus, training and upskilling staff should occur early in their careers 8 and should be an organisational priority. Nurses’ confidence revealed an upward positive shift from three before training to four after training. Although these findings are consistent with earlier studies showing a benefit of educational packages in improving nurses’ knowledge 21 and confidence in dealing with violence,21–23 direct comparability of these studies with ours is limited, owing to different study designs and measurements.
The literature shows that effectiveness of any educational strategy is based on its ability to address the local learning needs; structuring programmes around learning needs is most likely to result in changes in behaviours in the acute setting.24, 25
The learning needs of the nursing staff were discussed by the educational task force with nursing administrators in monthly meetings prior to, during and after training; this was consistent with a more developmental approach to learning.
The high response rate is a strength of this study. The advanced nurse practitioner was involved in conducting all training sessions, thus minimising bias that might have been introduced if there had been multiple trainers with varying styles of delivery of training.
As studies on the effects of nursing training on rapid tranquillisation were lacking, to the best of our knowledge, a ‘test the knowledge’ questionnaire was devised using a best-practice approach. The content of the questionnaire was rooted in the revised policy, which was drawn from best practices through a literature search and published guidelines, thus demonstrating content validity.
A pre-pilot test of the questionnaire on 11 nurses for clarity, readability and sentence structuring, consistent with face validity, was also conducted. The internal consistency of the questionnaire, assessed using Cronbach’s alpha, revealed a score of 0.71, which is regarded as clinically acceptable for a pilot study. However, as this is a novel questionnaire, additional validity and reliability testing is needed.
The following limitations in our study needs acknowledgement. The participants in our study were not randomly selected and there was no control group. The study sample was small and representative of only two acute medical wards. However, as violence is common in medical settings, we contend that our target participant population for educational intervention was appropriate, despite the potential selection bias in the two chosen wards. Additionally, capturing the lasting effects of educational intervention at further time points might have been useful.
Lastly, we concur with the literature that emphasises that systematic, multi-component strategies be employed to manage violent behaviour, with staff training being an integral component of the strategy 26 employed, to enhance knowledge and confidence in managing violent patients. Organisational barriers to managing violence, 26 straddling all levels of hierarchy, needs to be addressed to effect change as part of an overall management strategy.
Future directions and conclusions
To the best of our knowledge, this is the first study in the local setting that evaluates a nursing educational initiative on rapid tranquillisation procedures. This study has shown that a classroom training intervention of nurses in rapid tranquillisation procedures improved knowledge and confidence in dealing with patient violence in hospitals and adds to the safe practice of rapid tranquillisation.
Our initiative on examining nursing training in a pilot sample will be used to shape future training sessions, which will involve blended class room and e-learning approaches.
Future studies with more rigorous designs, such as controlled group, validated instruments and measurement of skill competency are warranted to support the findings of this study. Further research to evaluate the clinical impact of nursing training is needed. This includes evaluating whether educational training of nurses can reduce incidence rates of violence, usage of physical restraints and adverse medication-related outcomes. Larger studies with longer follow-up measurements to evaluate the long-term impact of training are also warranted to replicate our promising findings. We trust that this study will catalyse wider educational research with a focus on patient safety, quality improvement projects and improved patient safety outcomes.
Footnotes
Availability of data and materials
A copy of the study questionnaire can be made available on request.
Conflict of interest
The authors declare that there is no conflict of interest.
Ethical approval
The SingHealth Centralised Institutional Review Board confirmed exemption from a formal application for ethical approval, as this study was an educational improvement initiative.
Funding
This research received no specific grant from any funding agency in the public, commercial or not-for-profit sectors.
