Abstract
Chronic disease burden is expected to increase in Singapore as the population ages. Medication therapy is a common and cost-effective modality to manage the top three chronic diseases, i.e. hypertension, hyperlipidaemia and diabetes locally. However, about one-third of patients stop taking their newly prescribed medications within 10 days. This nonadherence problem is associated with poor clinical outcomes and substantial financial loss. This study aimed to determine patients’ drug information needs and concerns, and the potential nonadherence rate in patients with unaddressed concerns. This prospective cross-sectional study was conducted in four polyclinics over a period of six months. A total of 127 participants who met the inclusion criteria were consecutively sampled when they were filling prescriptions at the polyclinic pharmacies. Each recruited participant was administered a structured questionnaire face to face by the trained investigators in a standardised manner. The majority of the participants (95.2%) felt that information regarding the new chronic medication, especially the medications’ indications, side effects and dose, should always be given at the point of collection. Delivery of information through verbal advice and written information were most preferred. Top concerns with medications were side effects, long-term safety and drug interactions. Almost one-half of the participants (42.5%) would not take the new medications if they had unaddressed concerns about their medications. The findings from this study provide us with a better understanding of patients’ drug information needs and concerns, and the potential prevalence of nonadherence amongst primary care patients with unaddressed concerns.
Introduction
Between 2004 and 2010, the total disease burden in Singapore increased by 15%. 1 Hyperlipidaemia, hypertensive disease and diabetes mellitus accounted for 38.4% of the total attendance (5.264 million) in all public primary healthcare centres, i.e. polyclinics. 2 Together, these top three medical conditions contributed to 52% of the disease burden amongst Singapore residents. 3 With an ageing population, the chronic disease burden that Singapore will be facing over the coming years will increase astronomically if no effective intervention is implemented to contain them.
Medications provide one of the most common and cost-effective treatment modality for these top three local chronic conditions. However, one-third of patients stop taking their new chronic medications within 10 days of being prescribed. 4
Nonadherence to medications, especially newly prescribed ones, is one of the commonly reported causes of discontinuation of pharmacotherapeutic treatments. This nonadherence is associated with poor clinical outcomes such as suboptimal haemoglobin A1C, which may then lead to poorer quality of life, higher hospitalisation and morbidity rates. This can also result in substantial financial burden due to poorly controlled diseases.5,6
The cause of nonadherence can be intentional and nonintentional. Fear of side effects associated with the medication, ignorance of the importance of taking them, and poor knowledge of their medications are some of the common reasons that contribute to the nonadherence problem. 7 Educating patients about their medications is an effective intervention to address this nonadherence issue. A patient starting a new medication is unfamiliar with it and may have more medication-related concerns. Additional drug information support for these patients may thus be required to address their concerns so that medication adherence is not affected.8–10
Hence, this study aimed to determine the drug information needs and concerns of local patients, as well as the potential nonadherence rate in these patients with unaddressed concerns. The knowledge gleaned from this study can empower healthcare professionals to tailor interventions that better meet the drug information needs and concerns of our local heterogeneous patient population. Equipped with a better knowledge of their medications, this may in turn improve patients’ adherence to new chronic medications and subsequent clinical outcomes.
Methods
This prospective cross-sectional study was conducted in four polyclinics located in the Eastern region cluster of Singapore from June to November 2013. This study was approved by the SingHealth Centralised Institutional Review Board (CIRB no: SHP2013/395/D).
The recruited participants were at least 21 years old and were prescribed at least one new chronic medication. Participants who could not understand or converse in English, Mandarin, Chinese dialects or Malay, as well as those who utilised specialised pharmacy-related services such as a medication review service, were excluded.
Using an assumed effect size of 50%, it was estimated that 120 participants were required to examine the relationship between the preferred modes of drug information delivery for newly prescribed chronic medication and each sociodemographic factor with 80% statistical power at 5% significance level.
Categorical variables were compared using chi-square or Fisher exact tests. All analyses were performed using IBM SPSS Statistics for Windows, Version 21.0. Armonk, NY: IBM Corp, at the 5% significance level.
A structured questionnaire, developed by the investigators, was administered face to face by trained investigators in a standardised manner. The questionnaire solicited information on demographics, education level and literacy as well as participants’ responses on the drug information preference, mode of delivery and their concerns.
Should information of the new medication always be given at the point of collection?
What are the four pieces of information you need about the new medication? Which one is most important to you?
(Note: Based on reasonable assumption by the research team, the current time window for dispensing allows for approximately four pieces of information to be communicated.)
How would you prefer to receive the information on the new medication?
Do you have any concerns with taking or using the new medication? If yes, what are they?
If necessary, how would you obtain more information about the new medication after leaving the clinic? Why do you choose to obtain the required information via this mode?
Will you take your new medication if you have some unresolved concerns about the new medication? Why?
Results
A total of 127 participants, with a median age of 59 ± 10.1 years, completed the survey. There were 46.5% and 53.5% of female and male participants, respectively. The ethnicities of the participants were representative of Singapore’s ethnic composition: Chinese (78.7%), Malays (15.0%) and Indians (6.3%). The majority of the participants (94.5%) had at least primary education, and 70.1% were literate in English.
Drug information needs
Most participants (95.2%) felt that information on the new chronic medications should always be given at the point of collection. ‘Indication’, ‘side effects’, ‘how to take the medication’ and ‘long-term safety’ were the four most commonly reported drug information that participants perceived they need when they collect their newly prescribed chronic medications (Figure 1).
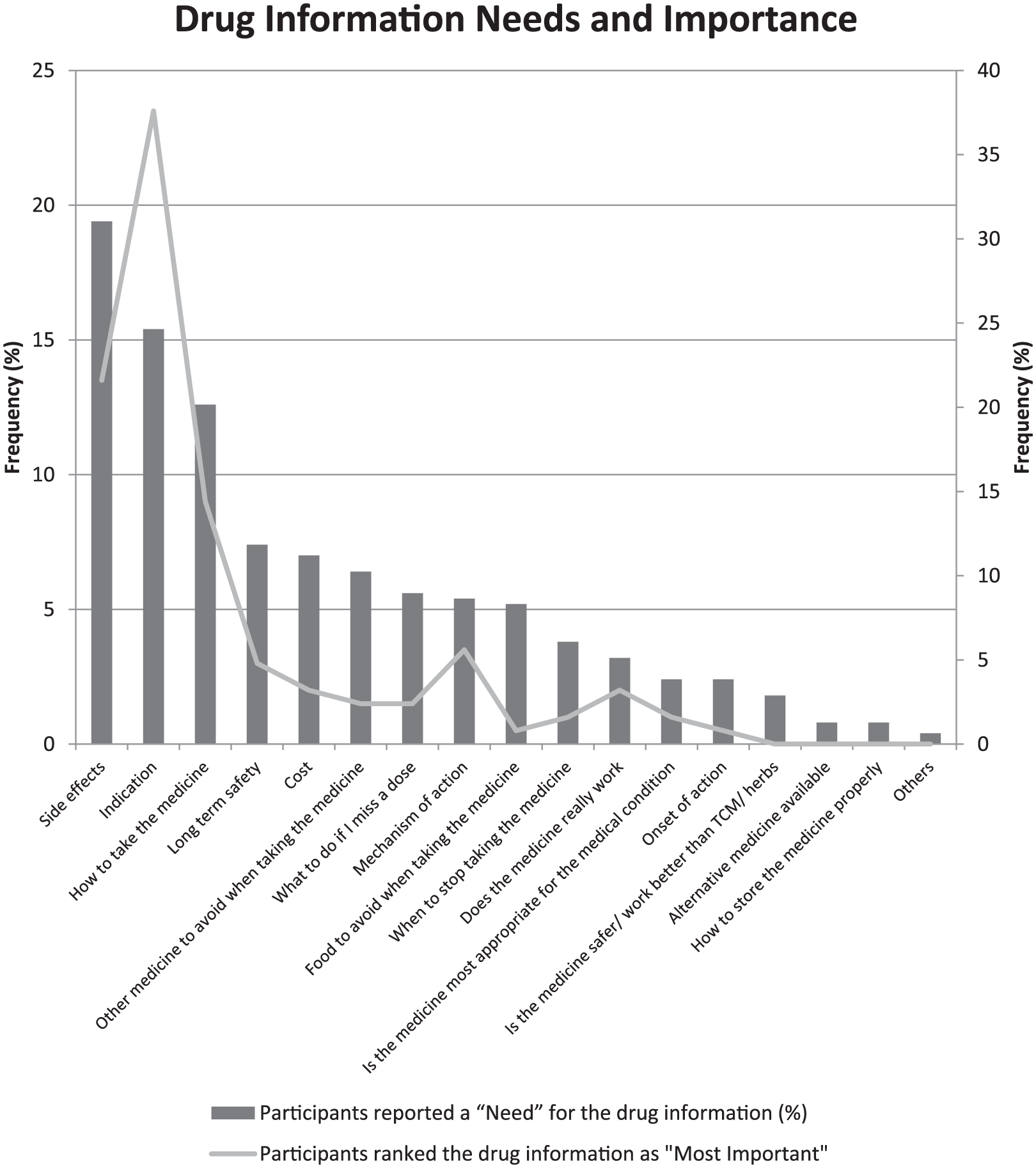
Distribution of drug information needs and importance.
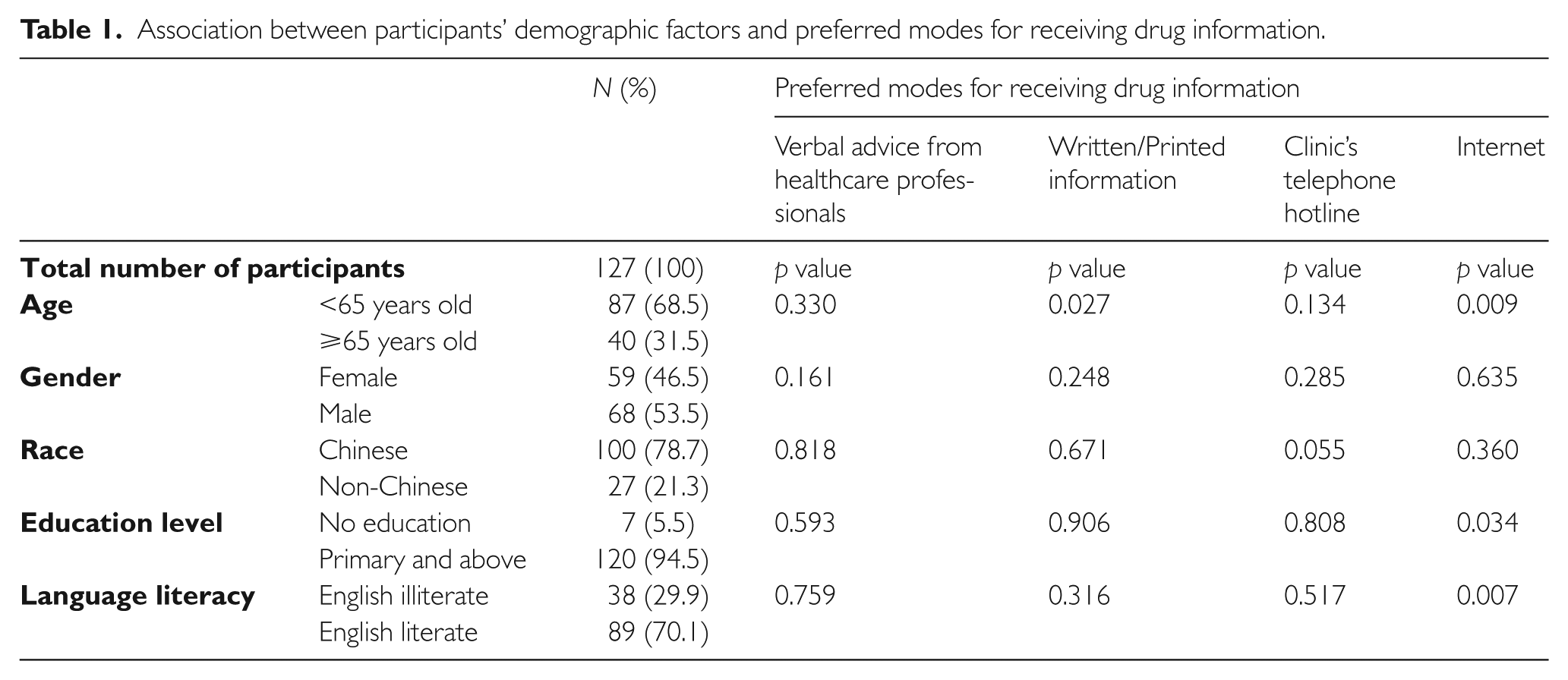
The most preferred mode for receiving drug information on their new chronic medications was verbal advice from healthcare professionals (Figure 2). Elderly participants above 65 years old (p = 0.009), and participants with no proper education (p = 0.034) preferred drug information to be available on the internet. Participants’ English literacy was identified as a factor affecting their preference to use the internet as a source of drug information (p = 0.007). Participants who were less than 65 years old had greater preference for written/printed information for their newly prescribed chronic medications than those who were older (Table 1).

Distribution of the preferred modes of delivery for drug information.
Association between participants’ demographic factors and preferred modes for receiving drug information.
About 65% of the participants would contact a healthcare professional for advice if additional drug information is required after leaving the clinic. Amongst them, 44.6% would return to the clinic soonest possible to speak with a healthcare professional. They would prefer to speak with either a doctor (56.8%), a pharmacist (40.5%) or a nurse (2.7%). About one-third of them (34.9%) would call the clinic hotline while 20.5% would wait till the next clinic visit to clarify with a healthcare professional. Other sources for the required information about their newly prescribed chronic medications included written/ printed information, internet, family and friends.
After leaving the clinic, factors that determined participants’ choice of their preferred modes of drug information were ‘easily accessible’ (37.1%), ‘trustworthy’ (26.1%), ‘informative’ (15.1%) and ‘easy to understand’ (14.7%). Other reasons given included ‘cost effective’, ‘high level of privacy’, ‘do not know how to use the internet’ and ‘difficulty in calling the clinic’s hotline’.
Concerns
More than 70% of the participants had an average of three concerns with their newly prescribed chronic medications. The top three concerns were side effects, interactions with other drugs and long-term safety (Figure 3). This finding resonated with observations reported by other studies.11,12 A delicate balance needs to be maintained by the healthcare professional in keeping the patients well informed about their new drug(s) while not alarming them with all the side effects and discouraging medication adherence.
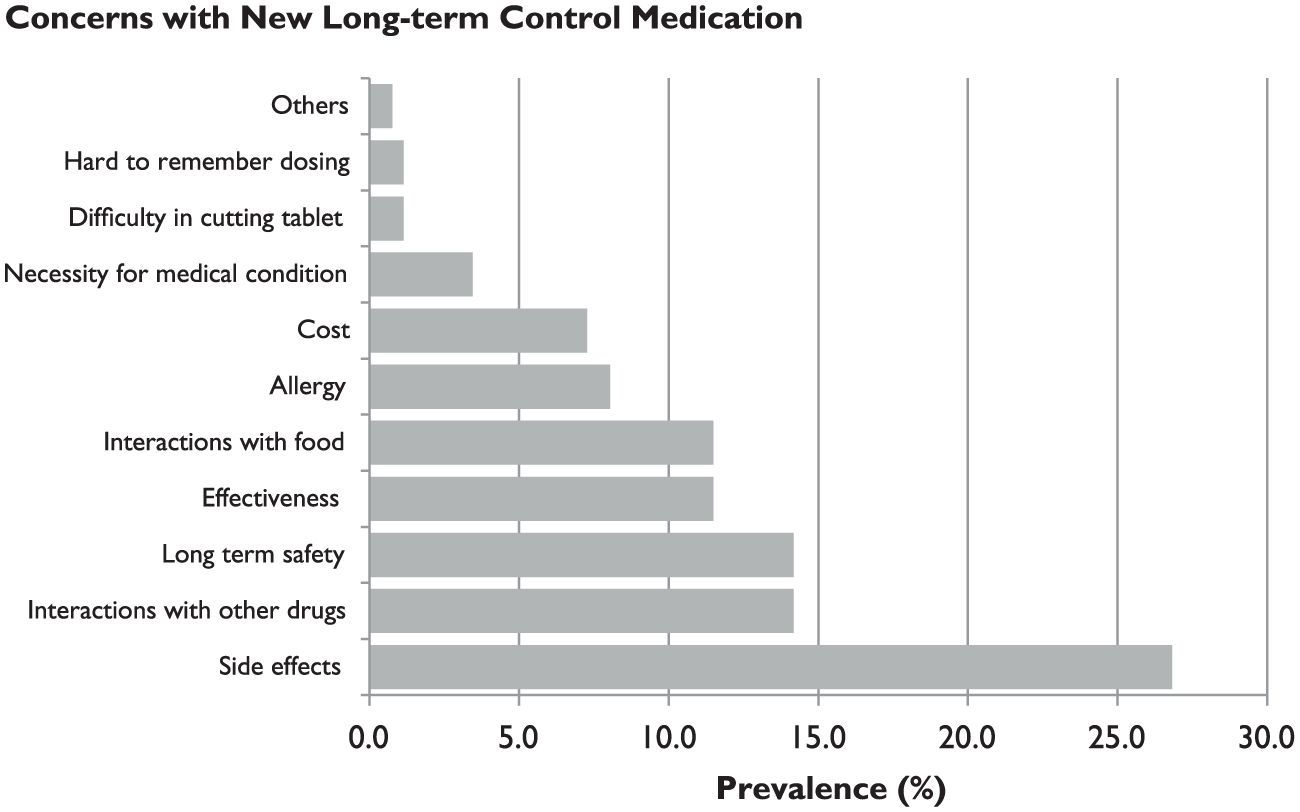
Types of concerns participants have with their new chronic medications.
Potential nonadherence rate in patients with unaddressed concerns
More than one-half of the participants (57.5%) would still take the newly prescribed chronic medication even if they had unresolved concerns about the medication. This was mainly due to the trust in the doctor (44.6%) or pharmacy staff (14.6%), or a belief in the necessity of medication to control their medical condition (27.7%). A belief that they should not miss or delay the taking of the medication, and perception that their concerns were minor, were other reasons cited by the participants.
A significant proportion of the participants (42.5%) would not take or use the new medications if they had lingering concerns about the medications. All of them thought it was important to have the concerns addressed first before starting on the new medications.
Hence, it is imperative that healthcare professionals are always accessible to the patients, and are able to provide appropriate drug counselling at every occasion of need.13,14 It would be useful for a contact number or email address to be made available on all medication labels. This will allow the patients who have already left the clinic to reach a healthcare professional for any further clarifications about their new medications should the need arise.
Conclusions
Patients prefer to verbally receive drug information when they collect their newly prescribed chronic medications, especially regarding medication indication, side effects, dose and long-term safety. Side effects, drug interactions and long-term safety of these medications are their top concerns. A significant proportion of patients will not take or use the new medications if they have lingering concerns about their medications.
Footnotes
Acknowledgements
We acknowledge the following pharmacists for their contributions to this study: Sarah Tay Siew Cheng, Huang Yufang and Lee Yu Jie.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Availability of data and materials
Only study team members had access to the data and study materials.
Authors’ contributions
Lawrence Liu Sy Tar: Study idea, study design, data collection, manuscript preparation and manuscript review. Bandy Goh Qiuling: Study design, data analysis, manuscript preparation and manuscript review. Tang Woh Peng: Manuscript preparation and manuscript review. Lo Fei Ling: Manuscript preparation and manuscript review. Rachel Khoo Shu Yuen: Manuscript preparation and manuscript review. Christina Lim: Manuscript preparation and manuscript review. All authors provided final approval for the manuscript.
Conflict of interest
None declared.
Informed consent
Written informed consent was obtained from the patient(s) for their anonymized information to be published in this article.
Ethical approval
This study was approved by the SingHealth Centralised Institutional Review Board (CIRB no: SHP2013/395/D).
