Abstract
Introduction:
Many modifiable risk factors for chronic diseases are related to dietary patterns and physical activity. This study aims to establish the prevalence of adequate fruit and vegetable intake and physical activity among community-ambulant patients in Singapore.
Methods:
A cross-sectional study was conducted among community-ambulant patients using convenience sampling. Data were collected through a survey questionnaire, covering self-reported level of physical activity and daily fruit and vegetable intake. Demographic information, awareness and adherence to recommendations were summarised using descriptive statistics. To identify factors influencing awareness and behaviour, exploratory logistic regression analyses were performed.
Results:
Three hundred and eighty-five complete responses were analysed. For intake of fruits and vegetables, 29.1% and 21.3% of participants were aware of and adherent to the fruit and vegetable intake recommendation respectively. For physical activity, 21.3% and 26.8% of study participants were aware of and adherent to the recommendation respectively. Only 4.7% and 5.5% of participants were aware of and practising both recommendations respectively. Gender, age, ethnicity and body mass index were found to have significant influence on the awareness of the recommendations. However, there was no significant factor found to be contributing to the adherence to the recommendations.
Conclusion:
Awareness of and adherence to lifestyle recommendations among patients remain low despite ongoing publicity efforts. Many are not fully aware of and adherent to the dietary and physical activity recommendations publicised. Apart from intensifying public outreach on every possible occasion and delivering messages in manners understandable by our older patients, strategies targeting the knowledge–behaviour disconnect among working middle-aged patients also deserve continued attention in the near future.
Introduction
In recent decades, the proportion of deaths associated with non-communicable diseases (NCDs) has been increasing. 1 The rising trend of lifestyle-related diseases presents a major global public health challenge, and is fast becoming a burden on population health, draining resources from healthcare systems worldwide.2–5 Various modifiable risk factors for NCDs have been identified, including hypertension, hypercholesterolaemia, obesity, sedentary lifestyle, tobacco use and inadequate intake of fruit and vegetables. 6 Many of these modifiable risk factors are closely related to dietary patterns and physical activity, and are important in chronic disease prevention. 7
Various national and international guidelines have recommended at least 150 min of moderate-intensity aerobic physical activity per week, or 75 min of vigorous-intensity aerobic activity, or equivalent alternatives, for healthy adults.8–11 In addition, as fruits and vegetables are naturally low in energy content while rich in dietary fibre, vitamins and minerals, at least two servings of fruits and two servings of vegetables are recommended daily. Meeting these recommendations has been shown to reduce the risk of cardiovascular diseases, type-2 diabetes, cancers and premature mortality.12,13
Despite well-known benefits of an active lifestyle, and adequate fruit and vegetable intake, health authorities globally have been experiencing difficulty in encouraging their respective populations to adopt the recommendations. In a study conducted by the United States Centre for Disease Control and Prevention, less than 20% of men and 15% of women engaged in these two lifestyle strategies. 14 In Brazil, more than half of the adult population was found to be overweight, and failed to practise any kind of physical activity during leisure time, or consume fruits and vegetables regularly.15,16 Similarly in Singapore, the 2010 National Health Survey revealed that only one in five adults engaged in regular exercise during their leisure time. Even with inclusion of physical activity at work, and walking or cycling while travelling to and from places in addition to leisure-time physical activity, only six in 10 adults had sufficient total physical activity.17,18
In an effort to improve adherence to recommendations and combat chronic diseases, a wide range of research and interventions have been trialled, with limited success.19–21 In Singapore, for instance, the Ministry of Health has recently declared war on diabetes and rolled out a series of long term campaigns, such as the ‘Eat, Drink, Shop Healthy’ Challenge and National Steps Challenge, to encourage active lifestyle and healthy eating habits, including adequate fruit and vegetable intake.22,23 While such publicity strategies through mass education campaigns, news coverage and advertisements have also been implemented in various settings, it is not known how much impact these efforts have on actual behavioural changes, especially among patients with existing medical conditions and chronic diseases.24–26 As such, our cross-sectional study aims to establish current prevalence of adequate fruit and vegetable intake and physical activity among community-ambulant patients in Singapore. A secondary exploratory objective is to investigate the associations with socio-demographic and contribution of different factors towards awareness of and adherence to recommendations for physical activity and intake of fruits and vegetables. This will help to guide the future development of health promotion strategies that aim to reduce the burden of obesity and chronic diseases.
Methods
Study design and data collection
A cross-sectional survey was conducted in a 330-bed acute care hospital in Singapore, from September 2016 to December 2016. Participants were selected by convenience sampling among patients filling prescriptions at the outpatient pharmacy. Inclusion criteria for participant selection were: (1) community-ambulant adult patients between the age of 21 and 80 years who are not confined to bed or institutionalised as a result of disease or surgery; (2) without prescribed restriction of diet and exercise; (3) able to communicate in English or Mandarin. Participants were excluded if they withdrew their participation at any point of the data collection or were unable or unwilling to give verbal consent for participation. The study protocol was vetted by Singhealth Centralised Institutional Review Board (ref.: 2016/2837).
The three-page survey questionnaire was administered by a single study investigator, who would clarify queries and reinforce definitions to the respondents during data collection. The questionnaire (Appendix 1) was divided into three section: demographic information, dietary habits and exercise regime. Both open-ended and closed-ended questions were used to elicit information from the participants. Separate illustrative charts for exercise types and portion sizes for food (Appendix 2) were also used during data collection to help participants estimate their level of physical activity and daily fruit and vegetable intake. While there may be varying interpretations and aspects of ‘adequacy’ in fruit and vegetable intake and physical activity in different countries or healthcare settings, we define the standards for the purpose of this study as adherence to Singapore’s Health Promotion Board (HPB) recommendations: (1) two servings of fruits and two servings of vegetables daily, and (2) at least 150 min of moderate-intensity aerobic physical activity per week, or 75 min of vigorous-intensity aerobic activity, or equivalent alternatives. These recommendations have been consistently conveyed over the years while other guidelines such as the food pyramid and macro-nutrient consumptions have undergone considerable revisions.
Sample size calculation and statistical analyses
Based on an infinite population, with 5% margin of error and 95% confidence level, 385 survey responses were needed.27,28 Demographic information, awareness and adherence to lifestyle recommendations were summarised using descriptive statistics. Predictive ability of awareness towards actual adherence to recommendations was determined using one-way analysis of variance. To identify factors influencing awareness and behaviour, logistic regression analyses were performed with the following patient demographics: gender, age, ethnicity, education level, body mass index (BMI), history of long term medication use, tobacco use and alcohol consumption. All the analyses were performed using IBM SPSS Version 17.0 (Chicago: SPSS Inc.).
Outcome measures
The primary outcome measure of this study was the prevalence of adequate fruit and vegetable intake and adequate physical activity among community-ambulant patients in Singapore. The secondary exploratory outcome measure was significance of selected demographic factors affecting awareness and adherence to at least one of the dietary and lifestyle recommendations of interest.
Results
In total, 389 patients were approached at the hospital’s outpatient pharmacy for survey participation while they were waiting for their prescriptions to be filled. Three hundred and eighty-five patients completed the survey questionnaire. Figure 1 details the participant enrolment process for the study.
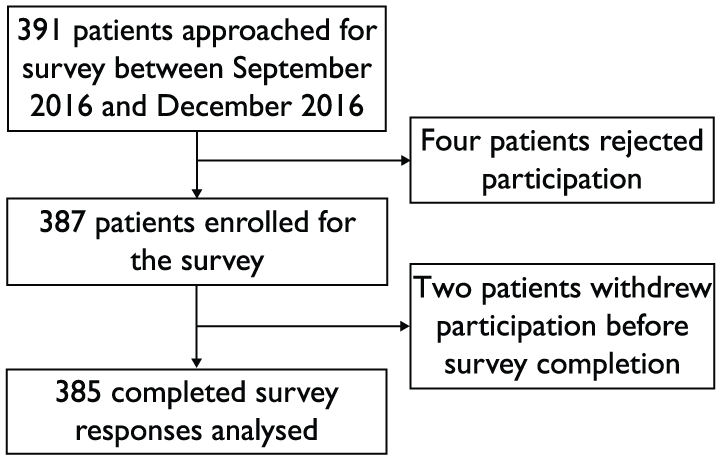
Participant enrolment flowchart.
Characteristics of the participants
Of the 385 patients who completed the survey, 197 (51.2 %) were male, with most of them above 40 years of age (68.3%) and of Chinese ethnicity (54.0%). The majority of the participants had at least secondary education (76.9%). The mean BMI of the participants was 22.81 kg/m2. Other demographic characteristics of the study participants are summarised in Table 1.
Baseline characteristics of study participants (n = 385).

BMI: body mass index.
Awareness of and adherence to recommendations
For intake of fruits and vegetables, 29.1% of participants were aware of the recommendation on daily intake of two servings of fruits and two servings of vegetables. However, they consumed only 1.04 servings of fruits and 1.78 servings of vegetables daily on average, with 78.7% of participants failing to consume the recommended two servings of fruits and two servings of vegetables on any typical day. Common reasons given for non-adherence were personal dislike of fruits (49.6%) and vegetables (49.2%) and lack of time to prepare or purchase (42.3%).
For physical activity, 21.3% of study participants were aware of the recommendations by HPB. The mean time spent on moderate-intensity physical activity was 90 min per week and 73.2% of participants reported that they did not engage in at least 150 min of moderate-intensity physical activity on any typical week. Common reasons given for physical inactivity were perceived poor health (40.4%) and laziness or tiredness (38.3%).
Out of the 385 participants surveyed, only 18 (4.7%) participants were aware of both recommendations and 21 (5.5%) patients reported to have met both recommendations. About one in four participants were aware of and were able to meet either recommendation respectively. One hundred and fifty-four (40.0%) participants were reportedly unable to meet the recommendations as they were not aware of them in the first place. On the other hand, 73 (19.0%) participants failed to meet the recommendations despite being aware of them. Surprisingly, there were 97 (25.2%) participants who met the recommendations despite not being aware of them. That was reportedly due to their general awareness of health benefits for dietary fibre intake and exercise while not knowing the specific recommended amounts. These findings are tabulated in Table 2.
Awareness and adherence of study participants (n = 385).

Awareness in dietary recommendation was not predictive of adherence (
Factors affecting awareness and adherence
Two logistic regression analyses were performed to assess the influence of pre-defined demographic factors that may be associated with levels of awareness and adherence to at least one of the dietary and lifestyle recommendations of interest. Gender, age group, ethnicity and BMI were found to have significant influence on the awareness of the recommendations. Collectively, these four factors alone explained 20.2% of the variation.
On the other hand, there was no significant factor found to be contributing to the adherence to the recommendations. These findings are summarised in Tables 3 and 4 respectively.
Factors affecting awareness of at least one of the dietary and lifestyle recommendations of interest.

BMI: body mass index; CI: confidence interval.
Factors affecting adherence to at least one of the dietary and lifestyle recommendations of interest.

BMI: body mass index; CI: confidence interval.
Discussion
Considerable evidence has accumulated in recent decades regarding the importance of adequate physical activity and intake of fruits and vegetables in the management of chronic diseases.29–31 A review of literature revealed that exercise confers significant therapeutic benefits in metabolic syndrome-related disorders, heart and pulmonary diseases, musculoskeletal diseases, a number of cancers and mental illnesses. 32 Guidelines and public health strategies have also accorded increasing attention to these non-pharmacologic interventions to chronic disease prevention and management.22–26
In our study, however, significant proportions of patient participants were found to be unaware of and not adhering to the specified dietary and lifestyle recommendations of interest despite intensive publicity by the health authorities over the years.33–36 Also, being aware of the recommendations did not translate into corresponding adherence to them, presenting a potential knowledge–behaviour disconnect. Although similar findings have been reported and reasons were explored in similar studies from other countries, the observation from our study may be further explained by several additional reasons befitting the cultural context in Singapore.14–16
First, 49.6% and 49.2% of our study participants reportedly ‘disliked fruits’ and ‘disliked vegetables’ respectively. These personal preferences and perceptions could be a result of lifestyle habits adopted since their youth due to potential economic reasons or low recognition of the associated health benefits by the parents then. 37 At the national level, there may be a need to study and review the state of nutrition education and awareness, identify gaps and determine whether ongoing nutrition messages are indeed achieving their intended objectives among the average Singaporeans.
Second, 42.3% of our study participants claimed that they did not have time to prepare healthier food at home. Hectic work commitment and related stress may be contributors to this phenomenon. 38 It was also noted that as the proportion of dual-income families increases due to rising costs of living, the practice of eating out has become increasingly common in Singapore.39,40 However, food items sold in most eateries in Singapore are not usually served with fruits, these having to be purchased separately. In addition, the vegetable component in local food choices is also often small in portion size. Collectively, these may help to explain the external factors surrounding the lack of fruit and vegetable intake among our participants.
Third, there seemed to be considerable inertia among our patients with self-reported ‘poor health’ to get physically active. Among 188 (48.8%) patients who provided reasons for their physical inactivity 76 (40.4%) cited poor health. Nonetheless, it was unclear whether those who cited poor health as the reason were indeed unsuitable for the recommended level of physical activity or actually facing difficulty of concurrently managing their chronic diseases alongside competing commitments. Similar to our Taiwanese counterparts, middle-aged Singapore residents exercise least regularly.18,41 Health promotion strategies targeting middle-aged patients who continue to work may warrant more attention in the future.
Finally, although it was only 26.8% of the participants whose reported physical activity met the recommendations, a previous study conducted in Singapore established that as much as 73.8% of the population could meet the physical activity guidelines if travel-related activities were included in the computation. 18 This is important for Singapore as the majority of the population travel by foot or public transport owing to low private car ownership. 42 Singapore has also done well in the creation of self-sufficient satellite towns where each housing estate is fully equipped with essential amenities within walking distance, effectively encouraging residents to walk when running errands within their housing estates. However, it is worth noting that travel-related activities may be of lower intensity and it has been suggested that their health effects might be less significant than those of purposeful exercise.43,44 As well, regular exercise may confer additional benefits beyond general health, such as physical fitness, dexterity, strength or even quality of life.43,45–47 The finding that despite engaging in less physical exercise many Singaporeans are still able to achieve relatively high levels of total daily physical activity, if travel-related activities are included, has lessons to be learnt for the selection and implementation of appropriate health promotion strategies at the national level. Studying the patterns of travel-related activity against different socio-demographic characteristics may shed light on unmet needs in supportive infrastructure. Other strategies, such as promoting work–life balance and workplace physical activities, heightening awareness of exercise and recreational facilities and encouraging supportive workplace cultures, may need to be considered.
From the exploratory logistic regression models, it was found that gender, age, ethnicity and BMI were significant factors that may affect the awareness of lifestyle recommendations, but only managed to collectively explain 20.2% of the variation in the rate of awareness. Moreover, none of the factors included in the regression model for adherence behaviour turned out to be significant. It echoed the findings of many previous studies that issues relating to lifestyle and behaviour are often multifaceted, involving the interplay of many known and unknown variables.14–18 As such, it is unlikely that the problems of low awareness of and low adherence to healthy lifestyle practices may be addressed by a few simple or targeted solutions. Nonetheless, the least that healthcare professionals and health campaigners may do is to seize every possible opportunity to remind and motivate patients to take greater initiative in adopting a healthier lifestyle and greater ownership in maintaining their health in the community. This may just help to persuade some patients contemplating it to actually begin their journey of behavioural change. 48
To our knowledge, this is the first local study to evaluate awareness of and adherence to lifestyle recommendations among community-ambulant patients and the results of this study could provide healthcare professionals and government organisations with insights to improve future health promotion initiatives in Singapore. The survey was intentionally designed to be short and simple, covering only pertinent questions to answer our study investigations. This led to an impressive response rate of 99%, thereby reducing the risk of selection bias. Moreover, all the questionnaires were administered by a single investigator with the use of illustrative charts and diagrams. These helped to improve consistency in survey responses and minimise potential information bias during data collection.
There were some limitations in this study. Given that this was a cross-sectional study, it may not be appropriate to extrapolate the findings to other time points. Data collection was done under the assumption that there was minimal reporting bias, and that any ongoing health campaigns, such as the War on Diabetes and National Steps Challenge, had minimal influence on the responses during the recall period.22,23 It was a deliberate decision to include only community ambulant patients in this study because the study team believed that this group of patients has good potential to be engaged and influenced through measures and intervention to encourage adoption of healthier lifestyles. However, the study team was not able to sample patients from the community who have their conditions managed solely by general practitioners. This limits the generalisability of the study findings to other patient groups who may have milder diseases not requiring specialist care. In addition, the definition over what may constitute ‘healthy lifestyle’ is not unified across different countries, cultures and care settings. For this study, we based our awareness of and adherence to ‘healthy lifestyle’ solely on Singapore’s HPB’s recommendations. Therein lies a potential bias as patients who are aware and adherent to recommendations other than HPB’s would be classified as unaware of or non-adherent to our study-specific recommendations. Nonetheless, we settled on HPB’s ongoing recommendations as the team felt that they were probably the most applicable in our local context. As most data were self-reported by the respondents, there could be recall bias. To mitigate this risk, we used illustrative charts to help the respondents during the recall process, and worded the questions neutrally without informing the respondents of what were the actual target recommendations. Finally, we did not attempt to collect personal data that may contain possible confounders, such as personal income data, occupation and exposure to social media, for our logistic regression models. As a result, the possibility of residual confounding from unmeasured demographic factors could not be ruled out and this could have influenced the results.
In conclusion, our study findings suggest that awareness of and adherence to lifestyle recommendations among patients remain low despite years of publicity effort. Many community-ambulant patients in Singapore are not fully aware of and adherent to the dietary and physical activity recommendations that were publicised. Apart from intensifying public outreach at every possible occasion and delivering messages in manners understandable by our older patients, strategies targeting the knowledge–behaviour disconnect among working middle-aged patients who are aware of the recommendations but choose not to act on them also deserve continued attention in the near future.
Footnotes
Appendix 1. Questionnaire on patterns of fruit and vegetable intake and physical activity
Appendix 2. Illustrative charts
Declaration of conflicting interests
The authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
