Abstract
Background:
Seven landmark randomised controlled trials, with some that began as early as the 1990s, observed the prediabetic state, namely, impaired glucose tolerance and impaired fasting glucose conditions, against the impact of lifestyle interventions such as physical activity, to prevent or delay the onset of type 2 diabetes mellitus. In addition to the landmark trials, this systematic review examines 14 studies that retained a focus on prediabetic individuals and measured the efficacy of physical activity on improving glucose tolerance.
Results:
Type, duration and intensity of structured physical activity can have unique benefits to prediabetic individuals. It is posited that diabetes prevention programmes must target prediabetic individuals as belonging to a high-risk group, separate and distinct from those identified with overall risk factors. While the transition from prediabetes to type 2 diabetes mellitus is not completely deterministic, the conversion rate is phenomenally higher among those with impaired glucose tolerance than those with normal glucose levels.
Conclusion:
Tenets of health behaviour models do support inferences that prediabetic individuals are potentially more inclined to weighing the risks and benefits of progressive illnesses and would therefore be more receptive to active participation in interventions. More research is required to develop evidence-based diabetes prevention programmes linked to structured physical activity intervention.
Introduction
During the past few decades, there has been a growing concern with the incidence and prevalence of diabetes. This is because diabetes-related comorbidities, complications and the overall quality of life years lost are major concerns for healthcare systems worldwide.1,2 The global prevalence of diabetes among adults aged 20 to 79 is 8.8% and is estimated to rise to 10.4% by 2040, with one in two adults remaining undiagnosed. 3 The economic impact of diabetes is staggering at US $1.7 trillion, with low- and middle-income countries accounting for US $800 million of this total amount 2 and about 12% of global health expenditure spent on diabetes. Type 2 diabetes (T2DM) is the most prevalent form and in high-income countries, accounts for up to 91% of diabetes. 3 According to a report collated in 2012, T2DM is among the top 10 leading causes of death for those over 60-years old and also for years of life lost due to disability. 4 In Singapore, about 11.3% of the people suffer from diabetes 5 and a projection using the Markov model 6 projects that the prevalence of prediabetes and diabetes will rise steadily from 15.5 % to 24.9 % and from 13.3 % to 22.7 %, respectively, from 2010 to 2035. 7
Suffice to say, the process of urbanisation, ageing trends and demographic shifts in incidence and prevalence of T2DM are red flags signalling the need for a pre-emptive strike in managing T2DM, that is, potentially prevent its onset. To this end, the intermediate condition of T2DM; prediabetes is worth noting. The condition with higher-than-normal blood glucose but below the criterion for T2DM is considered as prediabetes. Clinically, there are two conditions: (a) impaired glucose tolerance (IGT) is a fasting blood glucose level of 6.1–7.0 mmol/l and 2-hour plasma glucose of greater or equal to 7.8 and less than 11.1mmol/l and (b) impaired fasting glucose (IFG) is measured as fasting plasma glucose between 6.1 and 7.0 mmol/l and 2-hour plasma glucose as less than 7.8 mmol/l. Aside from these conditions, the World Health Organisation (WHO) defines prediabetes as intermediate hyperglycaemia. 8 IGT is more common than IFG and its global prevalence was estimated to be 6.7% in 2015 and is projected to be 7.8% by 2040. 3
The T2DM epidemic is an outcome of genetic and epigenetic predispositions fusing with modifiable behavioural and environmental risk factors. 9 As such, population-based intervention, physical environments tailored for physical activity, policies that penalise purchase of foods rich in fat and sugar are various forms of settings-based interventions; are often deployed to manage or prevent diabetes. However, most studies show that intensive interventions involving diet, increased physical activity and loss of weight are more effective,1,2 also known as lifestyle modifications. Historically, both pharmacological intervention with metformin and intensive lifestyle changes have been utilised in diabetes prevention programmes. 10 The cost effectiveness of these intervention treatments has been explored in diabetes prevention programmes in Australia, France, Germany, Switzerland and United Kingdom using the Markov Model 6 which simulates long-term progression of many progressive diseases including T2DM. Here, both metformin and intensive lifestyle changes increased life expectancy among those with T2DM and cost savings for the latter were higher in most countries. 11 A cost-effective simulation of the US Diabetes Prevention Programme showed that the cost per quality-adjusted life year (QALY) for the lifestyle intervention was superior to pharmacological intervention (metformin) at US$8,000 and US$29,000 per QALY, respectively. 12
Aside from non-modifiable factors such as genetic, sex, age, family history of diabetes; excess body weight, poor nutrition and physical inactivity are the key risk factors[3]. Conventionally, the guidelines for lifestyle modifications on physical activity, dietary change and weight loss for T2DM are also extended to those with IGT and IFG. 13 It may be an erroneous assumption that the lifestyle modification regime prescribed for T2DM is equally suitable for those with prediabetes, as is the underplaying of physical activity in the intervention equation. Therefore, it is worth exploring the efficacy of structured physical activity (SPA) among prediabetics.
Prediabetes is a prolonged condition where the transitioning phase to T2DM cannot be clearly determined. There is even contention that the cut-off point and diagnosis at lower levels 14 may incapacitate the healthcare system from providing necessary care and attention. What is certain is that many can remain undetected, with those even under 45 at risk. It has been said, ‘Physical activity, while not a drug, can behave like one.’ 15 A 12-year cohort study done in the UK showed that physical activity reduced the risk of T2DM independent of body weight change. 16 The variant forms of physical activity 17 need to be defined (aerobic, leisure, moderate, vigorous, resistance and interval) with measurement mechanisms that can be similarly applied across all studies. This systematic review will focus on SPA embedded within diabetes prevention trials and programmes to enhance the understanding of the direct role of SPA in preventing or delaying the onset of T2DM among prediabetics.
Methods
Search methodology
The initial stage of the study search was intentionally broad to ensure prediabetes as a subject matter was not subsumed by T2DM. Figure 1 presents a search flowchart conducted from August to September 2016, where two sets of data range were used. Landmark diabetes prevention trials (LDPTs) are the cornerstones of diabetes prevention efforts and the search mode ensured retrieving original and follow-up articles with data range set from January 1997 to September 2016. Three iconic trials: the US Diabetes Prevention Programme (DPP), the Finland Diabetes Prevention Study (DPS) and the China Da Qing Study (DQS) were all published by 2002. The diabetes prevention translation trials (DPTTs) followed their footsteps with some modifications. Logically, DPTTs were more likely to be researched and published thereafter and data range was modified to August 2002 to September 2016 for this next batch of search. The search for other independent diabetes prevention trials (IDPTs) was also set at this data range. Search was restricted to English language and human subjects with no geographical restrictions.
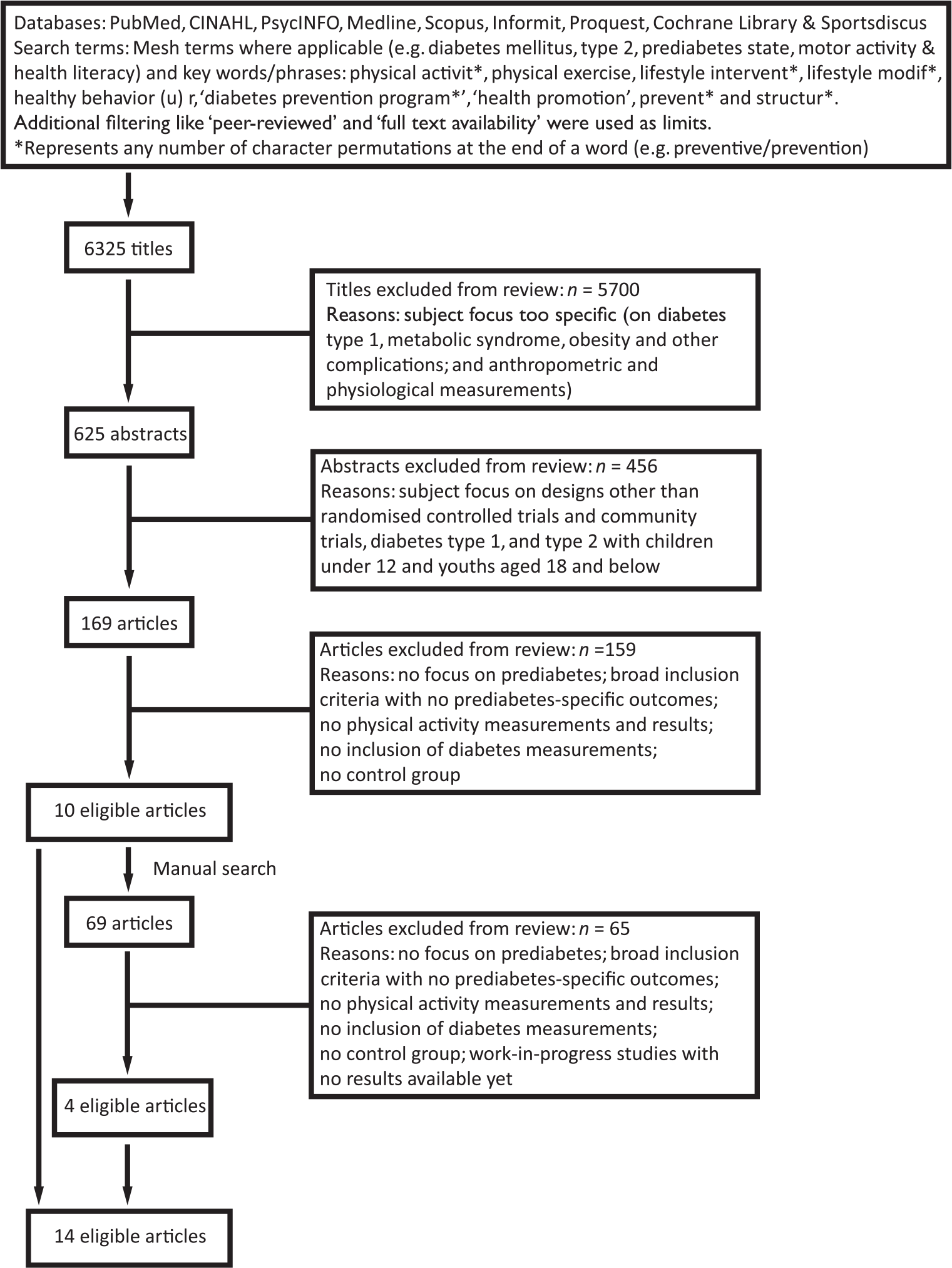
Flowchart for electronic and manual searches of studies from January 1997–September 2016 (landmark diabetes prevention trials) and August 2002–September 2016 (diabetes prevention translation trials and independent diabetes prevention trials).
Study selection criteria
Trials with pre-test/post-test design were included if the primary or secondary outcome was the incidence of T2DM and prediabetes had been identified according to standard screening guidelines. 8 SPA had to be part of the trials understood as ‘planned, structured, repetitive and purposeful’ 18 exercise delivered through advice, supervision or training and only studies with control groups were included. An alternative intervention was also considered as a control mechanism.
Broad inclusion criteria of high-risk individuals for trials with no specific assessment of prediabetics with IGT or IFG were excluded, as were studies of T2DM with no inclusion of prediabetes. Special-interest studies on gestational diabetes, metabolic syndrome or those dealing with pregnant women, children or adolescents were excluded. Where the efficacy of study had no basis for comparison with a control group, it was considered irrelevant. When it was difficult to establish subject matter through abstracts, the articles were retrieved and reviewed to ascertain relevancy.
Classifying intervention and outcome
Given the paucity of studies on SPA, independent of other interventions, articles researched included diet and pharmacological interventions. Only the efficacy of SPA is reviewed in this paper. Outcomes focused on the incidence of diabetes, glycaemic control and changes in physical activity behaviour. Given the heterogeneity of studies, no meta-analysis was conducted.
Study selection review
The selection of study was based on a dual review process (Joseph Edwards and Hassan Hossainzadeh). Database search was initiated by both reviewers based on the same search terms. The shortlisted abstracts were co-reviewed and exclusion criteria resulted in 169 articles. Thereafter, concurrence from both reviewers on critical inclusion criteria like the presence of physical activity and diabetes measurements, generated 14 eligible articles for systematic review.
Results
There was no consistency in measurements used for insulin resistance and physical activity and they varied from study to study. LDPT, DPTT and IDPT participants had a body mass index (BMI) range greater than 21.5 kg/m2 and less than 40.3kg/m2 and were all 30-years old and above. Among studies selected, only the LDPT group of studies had a representative spread of trials conducted in Europe, US and Asia.
Landmark diabetes prevention trials
The DQS, 19 DPS 20 and DPP 10 studies were pioneering efforts. The DPP is well renowned owing to its large sample size (n = 3234) and its appeal as an anchor reference for community programme initiatives. These three epidemiological milestones are also complemented by four other trials: the Japan Diabetes Prevention Programme (JDPP), 21 Indian Diabetes Prevention Programme (IDPP), 22 Vasterbotten Intervention Programme (VIP) 23 and Study on Lifestyle Intervention – SLIM (Maastricht). 24 Numerous articles have been published in relation to these studies and only the original articles and follow-up results (where available) of these studies have been assessed here. While physical activity measurement is a key consideration for review, the JDPP is an exception without one. Nonetheless, it has been included, given its standing as a landmark trial. These studies set the tone for contextualising the genesis and evolution of prediabetes research. The LDPT studies covered various levels of exercise, from the basic criterion of structured exercise (SE) to including supervised exercise (SUE), aerobic exercise (AE), resistance exercise (RE) or occupational exercise (OE). The type of exercises linked with respective studies is indicated in Table 2.
The 7, 13 and 20-year follow ups on the US DPP, 10 Finnish DPS 25 and China DQS 26 showed 49%, 32% and 43% lower incidence of diabetes in the intervention group than the control group, respectively. In all these studies, the incidence of diabetes was the primary outcome. In sum, all participants in these seven trials were either overweight or obese (BMI > 30 kg/m2). The age range across all seven studies was between 35 and 72.
‘Light, moderate, strenuous and very strenuous’ terminologies were used to describe exercise intensity but definitions varied. For example, DQS equated different forms of exercise ranging from 5, 10, 20 and 30 minutes as one unit of exercise and defined levels of intensity based on this unit of measurement. Maastricht considered the non-compulsory resistance training provided as strenuous while VIP had an intensive 1-month full stay intervention with aerobic and resistance training sessions. 24 In all of these studies, sedentary lifestyle at baseline was not a prerequisite and some participants in the JDPP 21 and IDPP 22 were already meeting physical activity goals before the trials commenced and were merely encouraged to maintain the same level of activity.
Given the subject matter being reviewed, measurement standards used for physical activity and glycaemic control are critical markers for appraisal, and DPP, VIP and Maastricht are worth noting as meeting expectations. See Table 1 and Table 2 for measurement details and overview of LDPT respectively.
Landmark diabetes prevention trials – glucose/insulin resistance and physical activity measurements.

Time units of 5, 10, 20 and 30 minutes of physical activity of different levels of intensity equated to one unit.
Rate or ratio of energy expended.
Device that measures the body’s response to activity by sensing heart rate.
Measure of maximum volume of oxygen in millilitres per kg of body weight.
Maximal test as above, conducted on a bicycle ergometer.
Note: JDPP – lifestyle intervention was tailored to each subject’s preference and physical activity recommendations were instructive. While JDPP falls short of the physical activity measurement as an inclusion criterion, it is an exception here, owing to its standing as a landmark trial.
HOMA-IR: Homeostatic Model Assessment of Insulin Resistance; HbA1c: glycated haemoglobin.
Landmark diabetes prevention trials: an overview.
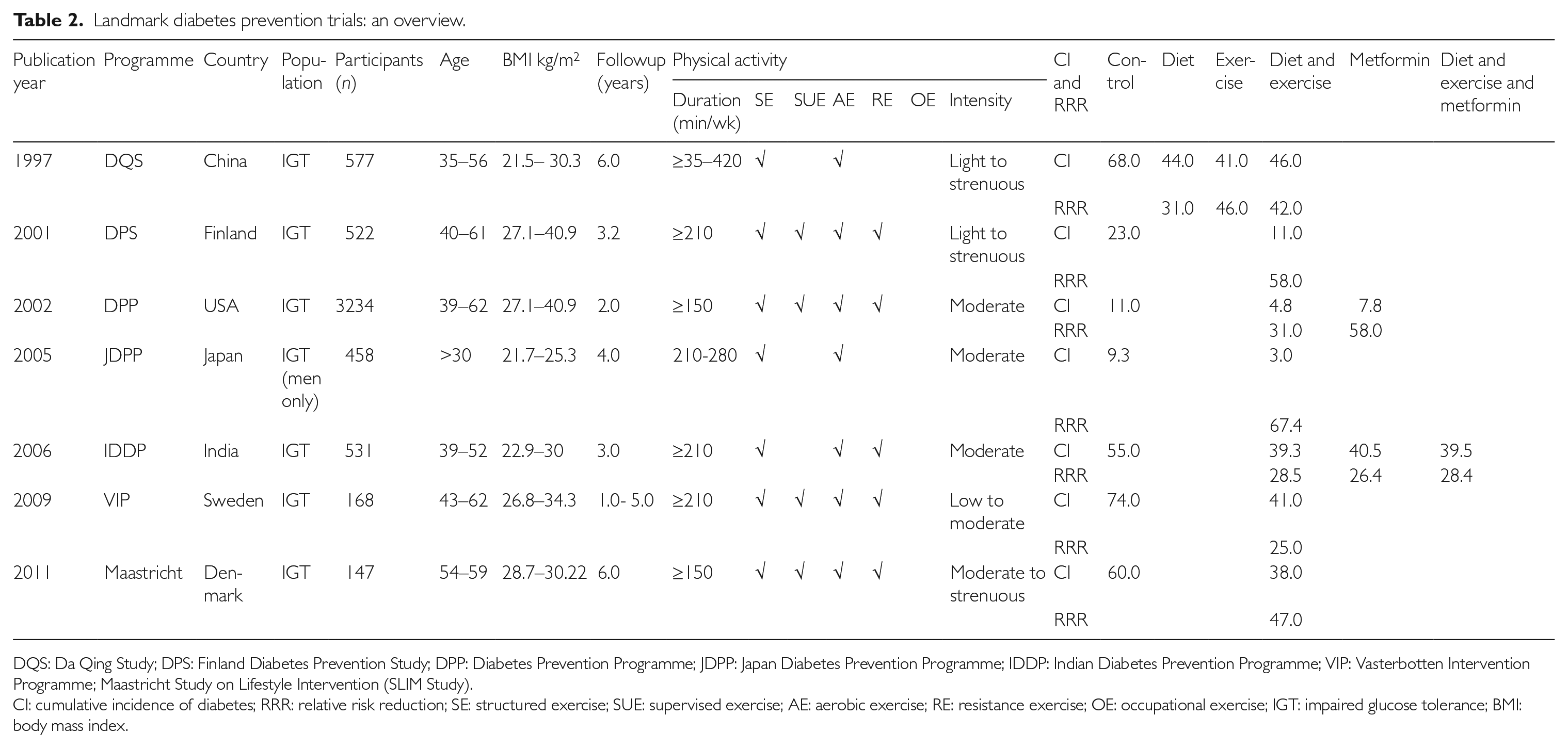
DQS: Da Qing Study; DPS: Finland Diabetes Prevention Study; DPP: Diabetes Prevention Programme; JDPP: Japan Diabetes Prevention Programme; IDDP: Indian Diabetes Prevention Programme; VIP: Vasterbotten Intervention Programme; Maastricht Study on Lifestyle Intervention (SLIM Study).
CI: cumulative incidence of diabetes; RRR: relative risk reduction; SE: structured exercise; SUE: supervised exercise; AE: aerobic exercise; RE: resistance exercise; OE: occupational exercise; IGT: impaired glucose tolerance; BMI: body mass index.
Diabetes prevention translation trials
Very few (three) DPTTs met the inclusion criteria. Most DPTTs tend to recruit participants based on overall risk factors where anthropometric measures such as BMI and waist–hip ratio (WHR) are used to verify weight loss as a primary outcome with physical activity assessment relegated to secondary status or no consideration at all. Similarly, glucose tolerance is often not measured. The studies selected for DPTT varied in terms of prescribed duration and intensity of physical activity but met the basic guidelines provided by the WHO of at least 150 minutes of moderate-intensity aerobic physical activity throughout the week or its equivalent of strenuous aerobic physical activity. WHO’s recommendation includes even leisure time, occupational and planned physical activities. 19
The search outcome for DPTTs is indicative of the sparsity of research materials available – associating prediabetes with physical activity. Studies adopting overall risk factors as inclusion criteria, with no monitoring and assessment of prediabetes, and deliberately focusing only on obesity were excluded. Though the inclusion of overweight individuals was acceptable for this review, on analysis, the sample populations in all DPTTs were obese individuals, though this may have been undeliberate. Comparatively, LDPT had overweight and obese individuals.
The Worksite Diabetes Prevention Programme (WDPP) 27 only used fasting glucose as a measurable outcome, which does not fall under the guidelines for identifying prediabetes. 8 Again, there was no unified standard of measurement for physical activity across all studies. The physical activity measurement tool in the 3-year follow up Finland study was found to be unreliable for the elderly.28,29 Substantive reduction in fasting glucose and HOMA-IR (Homeostatic Model Assessment of Insulin Resistance) clinical measures were stated but no incidence of T2DM or risk reduction rate were computed in the Healthy-Living Partnership to Prevent Diabetes (HELP-PD) study.30,31 Two of these studies had a sample size of less than 80 (WDPP and HELP-PD). The Finland study was a pilot project where the sample size of 45 was allocated as 12 for ‘care as usual’, 18 for ‘basic care intervention’ and 15 for ‘intensive intervention’ and presumably affects the level of confidence for comparison purposes, given the small sample size. Statistical shortfall aside, in the 3-year follow up of the Finland study, the incidence of diabetes was 33.3% in the ‘care as usual’ group compared with 23% in the combined intervention groups (one intervention with prescribed physical activity and another with an intensive physical activity programme) with relative risk reduction for the intervention group at 32% for those with IGT. 29 Table 3 provides a summary of details.
Diabetes prevention translation trials – an overview.
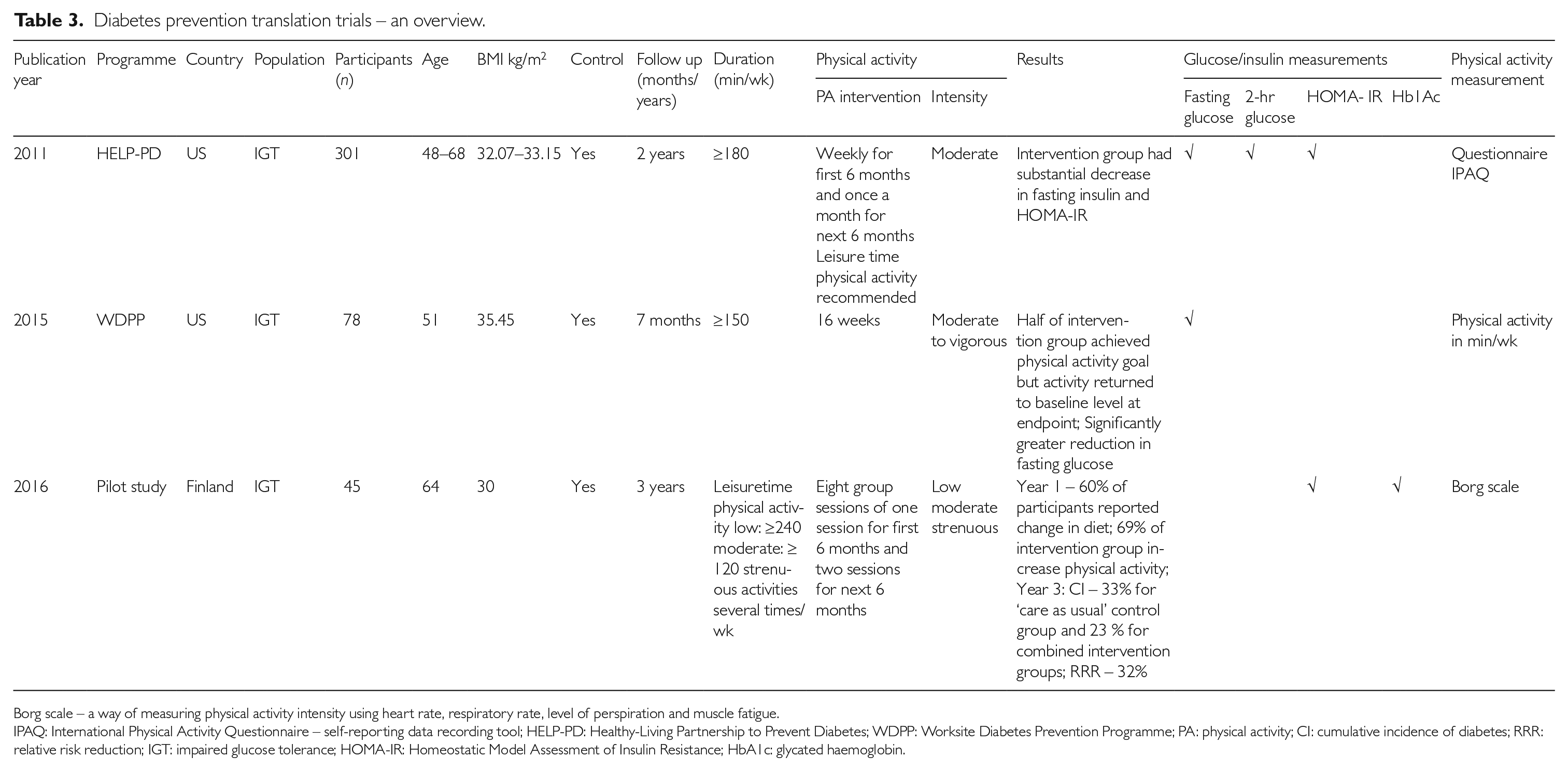
Borg scale – a way of measuring physical activity intensity using heart rate, respiratory rate, level of perspiration and muscle fatigue.
IPAQ: International Physical Activity Questionnaire – self-reporting data recording tool; HELP-PD: Healthy-Living Partnership to Prevent Diabetes; WDPP: Worksite Diabetes Prevention Programme; PA: physical activity; CI: cumulative incidence of diabetes; RRR: relative risk reduction; IGT: impaired glucose tolerance; HOMA-IR: Homeostatic Model Assessment of Insulin Resistance; HbA1c: glycated haemoglobin.
Independent diabetes prevention trials
Only four studies met the selection criteria out of 75 articles reviewed. Each IDPT was markedly different in intervention. The goal of one study was to examine how physical activity affects glycaemic control independent of diet composition and diet-induced weight loss. To achieve this, qualified individuals were sent for a 6-week diet programme and had to stabilise weight for 3 weeks before being considered for trial participation – that is, achieve dietary stabilisation. This study also ensured that participants were physically inactive, as only subjects with sedentary occupation and lifestyle – (less than twice per week of aerobic exercise that was less than 20 minutes per session) were selected. Those with IFG or IGT were also considered and 17 of the 47 prediabetics achieved normal glucose level after training. 32
Another study explored how physical activity and metformin influence glucose tolerance, including placebo effects overlaid on different intervention groups and concluded that metformin did not underscore the effects of physical activity on glucose tolerance among prediabetics. The study does concede that it did not consider isolating effects of physical activity on IFG and IGT participants respectively. 33 The Japanese study only changed the frequency of diet and physical activity intervention in both groups to assess how it affects those with IFG, a diabetic condition less common. A 3-year follow up witnessed a cumulative incidence of diabetes of 12.2% in the frequent intervention group and 16.6% in the less frequent one. 34 Lastly, home-based physical activity counselling (PAC) was explored with education and tele-counselling 35 among US war veterans and yielded no difference among ‘usual care’ and PAC groups in glycaemic control. Among the four, the most significant results came from the study with the dietary-stabilisation component, where 36% of prediabetics reverted to normalised glucose levels at the 24-week endpoint. A summary of clinical markers observed and an overview are provided in Tables 4 and 5, respectively.
Independent diabetes prevention trials: glucose/insulin resistance and physical activity measurements.
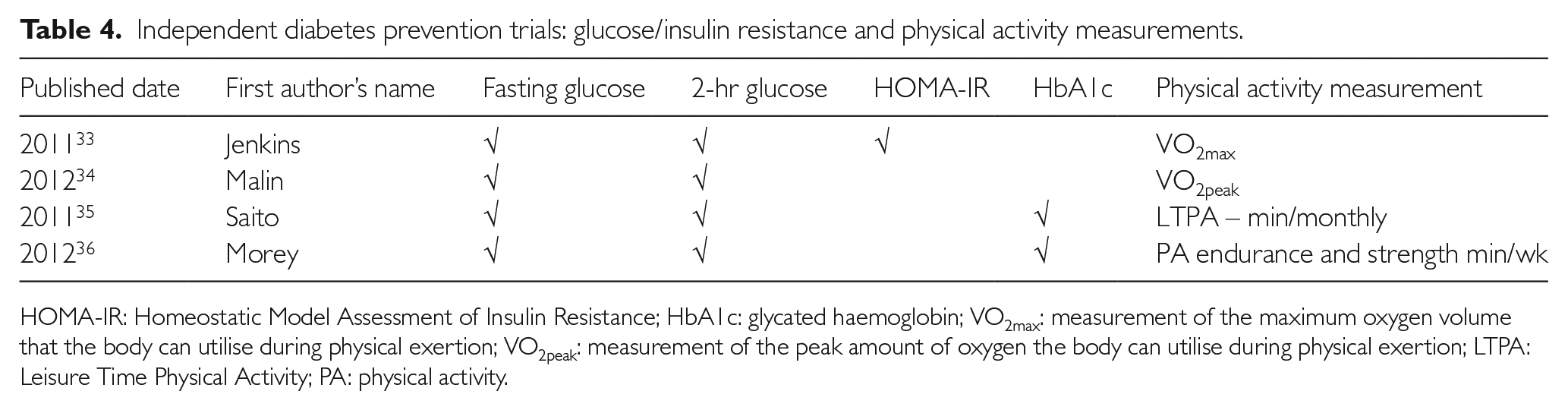
HOMA-IR: Homeostatic Model Assessment of Insulin Resistance; HbA1c: glycated haemoglobin; VO2max: measurement of the maximum oxygen volume that the body can utilise during physical exertion; VO2peak: measurement of the peak amount of oxygen the body can utilise during physical exertion; LTPA: Leisure Time Physical Activity; PA: physical activity.
Independent diabetes prevention trials: an overview.

BMI: body mass index; PA: physical activity; PAC: physical activity counselling; VO2peak: measurement of the peak oxygen volume the body can utilise during physical exertion; CI: cumulative incidence of diabetes; PA: physical activity; RCT: randomised controlled trial; IFG: impaired fasting glucose; IGT: impaired glucose tolerance; LTPA: Leisure Time Physical Activity.
Discussion
The missing link
The saliency of SPA in embattling prediabetes to avert T2DM is understated and under-explored. Physical activity traverses the morphological and physiological aspects of the human body and has the ability to impact the body at a metabolic level – stimulating changes that either delay the onset of T2DM or reset the body to normal glucose control, as in Jenkins’ IDPT. 32
In the IDPT studies reviewed, it became evident that the type of physical activity examined was also critical; from leisurely activity to even differentiating between aerobic and resistance training. The intensity, duration and frequency of muscular contractions contribute to caloric energy expenditure in physical activity. 36 Resistance training among the elderly yields favourable results of fasting glucose and glycated haemoglobin (HbA1c) for those with prediabetes and a normal glucose level compared with those already suffering from T2DM. 37 In addition, administering regular exercise training results has a sustaining effect.38-41 Cohort studies for men 42 and women 43 have also substantiated the benefits of resistance training for both sexes with aerobic exercise compounding a greater benefit. Similar benefits of improving glycaemic control through resistance training among those with IGT have been documented by other authors. 44 Besides resistance training, interval training that was not explored in this systematic review is also gaining new grounds. Interval training involving repetition of high exercise intensity with longer or similar periods of recovery, while aerobic in nature, also engages the anaerobic mode, a combination that propels mitochondrial functions to excel and supports the hypothesis that metabolic pathways are enhanced to improve glucose tolerance. 45
This paper posits that the prediabetic condition is a high-risk phase that warrants special attention. In aetiology, 46 where the agents of exposure cannot be singled out to a causal condition among individuals, the alternative is to focus on the determining agents of the incidence rate. In policies toward disease prevention, the tendency is to focus on high-risk individuals and whole population which inadvertently blindsides attention away from the uniqueness of the role of SPA among prediabetics – the missing link in current diabetes prevention programmes.
Tunnel vision
Risk-pooling individuals in prevention strategies may appear more effective from methodology and cost perspectives. While some of the landmark trials had group sessions, the intervention was primarily at an individual level for all of them. The translation trials thereafter, adopted the more cost-efficient group interventions. There is no single determinant for transition to T2DM and the escalation potential of prediabetes to T2DM is probably underrated. According to some estimates, the annual conversion rates of prediabetes to diabetes is between 5–10% with a similar percentage reverting to normal glucose level and it is argued that diabetes risk for those with prediabetes is no different from those with a combination of other risk factors. 47 However, annual conversion rates can be misleading, as progression happens over time. In the Hoorn Study in Denmark, given 6.5 years of follow up, the risk of conversion to diabetes was 10 times more likely among those with IGT or IFG than in people with a normal glucose level. 48 LDPTs have shown benefits of intervention only for those with prediabetes.10,19,20 Every individual diagnosed with T2DM would have also undergone the prediabetic state, though the length of this period varies. 49
Aside from epidemiological and pathophysiological considerations, the patterns of human behaviour would also suggest that prediabetic individuals would be more willing to weigh the risks and benefits and participate more actively in intervention programmes. Therefore, the prediabetic state is a fertile ground for health theories to thrive in their applications. The Theory of Planned Behaviour fuses intentions with behaviour in action. 50 The Trans-theoretical Model considers behavioural continuity as presumptuous and beckons stages of intervention. 51 The Social Ecological Model highlights the interplay between society and the eco-system. 52 Last but not least, the Social Cognitive Theory draws from these theories acknowledging environment, behavioural capabilities, expectations, self-efficacy, reciprocity and even emotional coping responses, 53 and was utilised in the HELP-PD study. 30 These theories would have greater translation value among those (prediabetics) who feel more predisposed to acquiring T2DM over time.
Evidence-based studies discussed previously validate the premise that prescription and activation of appropriate physical activity benefits prediabetics more than those with T2DM. This is a strong association that has not been capitalised in diabetes prevention programmes. The contention is not with broad inclusion of high-risk individuals in programmes but with the lack of distinction and attention accorded to prediabetes. Neither is there a disagreement that diet and weight loss play a part but that the lower weightage given to prediabetes in risk management and prevention is undermining the potential to target groups more effectively. Cost is equated to efficiency and prediabetes is sacrificed at the altar of health management practice, perpetuating a tunnel vision in health management practice.
All participants in LDPTs and DPTTs were obese. Many trials excluded from this review focused only on weight loss. In such studies, examining and addressing association between SPA and prediabetes was ignored, or reduced to secondary significance. The independent Finland DPT deduced that 60% of participants reported a change in diet and acknowledged the ‘difficulty of separating the effect of physical activity from diet from the effect of change in dietary habits.’ 29 It would seem prudent, or perhaps convenient, to manage diet and physical activity as intertwined entities. However, the IDPTs involving dietary stabilisation 32 demonstrates that effect size of physical activity can indeed be measured independently.
Great leap forward
The IDPTs reviewed are treading in the right direction, though each has its limitations. The Japanese trial 34 allowed the participants in both groups to set their own lifestyle goals. The ‘remote physical activity counselling’ technique was trialled among older adults who were war veterans 35 via tele-counselling. Remote access to lifestyle advice and intervention can be effective among younger adults with the use of digital platforms and devices 54 but inappropriate with other groups, such as older people. The independent trial with physical activity and metformin interventions had too short a time-frame for endpoint assessment to have sustainable validity. 33 The efficacy of aerobic training trial on prediabetics ticked all the right boxes in terms of glycaemic and physical measurements. While acknowledging the lack of employing a control group to compare sedentary lifestyle, the study made a bold conclusion that ‘an IGT-only prediabetic individual is the most responsive to training.’ 33
SPA is a structured format where maintenance and improvement of one or more physical fitness regimes must become a core objective in diabetes prevention. Cardiorespiratory and muscular endurance, muscle strength, body composition and flexibility are health-markers and should be evaluated as outcomes using appropriate measurement tools. 55 Independent trials are making good strides in establishing evidence and the great leap forward would be to translate them into community programmes.
Missing the mark
Assessing and addressing overall risk factors has become the basis of diabetes prevention programmes translated in real-world settings. The 2008 Montana Diabetes Prevention Programme in the US considered one or more risk factors including those directly related to diabetes such as IGT and IFG but also included high blood pressure and other biomarkers of cardiovascular disease as inclusion criteria. 56 The American Association Diabetes Risk Score (ADART) 57 was used in a faith-based intervention among rural African–American church 58 while BMI and family history of diabetes were considered as risk factors for interventions among congregations in rural American churches. 59 Studies in Finland also used a diabetes risk score rather than considering the prediabetic condition as a special interest component of diabetes prevention programmes.60–62 Australia also runs diabetes prevention programmes such as ‘Beat it’ in New South Wales (NSW) and ‘Life’ in Victoria.63,64 These prevention programmes assess overall risk of diabetes using the Australian type 2 diabetes risk assessment tool - AUSDRISK tool 64 and are not designed specifically for prediabetes. Historically, Australia had also embarked on its own diabetes prevention translation trials. The Sydney Diabetes Prevention Programme, NSW65,66 and Victoria’s Greater Green Triangle 67 accommodated broad high-risk inclusion criteria with conditions like obesity and weight loss 63 as the desired outcome. As such, they were categorically removed from this study. Diabetes prevention strategies are missing the mark in both cost and patient-care management.
Designed to move
Given evidence-based facts that support the greater benefits of resistance training for prediabetics; appropriate regimes need to be institutionalised in SPA as part of healthcare management. The efficacy of interval training in delivering benefits needs further exploration and has the potential to be part of the regime that can be included in SPA. Here, there is an opportunity to be ingenious and creative in ‘reshaping’ beneficial exercises into more engaging formats – potentially a ‘designed to move’ (D2M) campaign that puts a positive spin on combatting diabetes and promoting a set of customised regimes within SPA in diabetes prevention programmes.
Footnotes
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Declaration of Conflicting Interest
The authors declare that there is no conflict of interest.
