Abstract
We present a case report of a 66-year-old female who underwent salvage arthrodesis after a failed Scandinavian Total Ankle Replacement secondary to aseptic loosening and talar subsidence. Secondary to the loss of talar integrity the decision was made to proceed with revisional ankle arthrodesis. To maintain limb length the primary surgeon (EH) elected to use a custom cage implant in combination with an intramedullary nail construct in a single stage approach. The custom cage was augmented with autograft & allograft cancellous bone in addition to allograft recombinant human bone morphogenic protein, and allograft adult mesenchymal stem cells. The incision sites healed post-operatively without incident and at post-op week 16 the patient progressed to full unrestricted weight bearing in normal shoe wear with a gauntlet ankle brace. Although an isolated report, this case shows promise for further development of the technique. We believe this revisional arthrodesis technique warrants further research and consideration as a potential addition to the failed total ankle arthroplasty treatment algorithm.
Introduction
The Scandinavian Total Ankle Replacement (STAR) is an uncemented, three-component, mobile-bearing design with titanium plasma-sprayed ingrowth surfaces on the tibial and talar components, and a meniscal-type polyethylene liner. Investigational use of the STAR implant in the US began in 1998, while approval for clinical use didn’t come until 2009. Due to the delay of clinical use, North American studies reporting outcomes of the design are lacking compared to European counterparts. Although tibiotalar arthrodesis has historically been the gold standard for ankle arthritis, recent advances in total ankle replacement (TAR) design and expanding indications have led to an increased number of TARs performed. Despite improved survivorship and increased reliability of overall clinical outcomes, the increasing popularity of TARs has led to increased incidences of implant failure and subsequent need for revision.
Although results have improved over time, survival rates of TARs still lag behind those of total hip and total knee arthroplasties. Causative factors for TAR failure have been described as technical error including poor sizing and malposition, medial and lateral gutter impingement, aseptic loosening, infection, wound dehiscence, displacement or breakdown of polyethylene spacer, and persistent pain.1–7 Presently available literature presents a wide range of TAR survival rates. Brunner et al. reported a STAR survival rate of 45.6% in 77 ankles at 14 years. 8 Daniels et al. reported a STAR survival rate of 66% in 111 ankles at a mean follow-up of 9 years. 9 Mann et al. reported a STAR survival rate of 90% in 84 ankles at mean follow-up of 10 years. 10 Nunley et al. reported a STAR survival rate of 93.9% in 82 ankles at a mean follow-up of 61 months and a survival rate of 88.5% at 107 months. 11 Wood et al. reported STAR survival rate of 80% at mean follow-up of 9 years. 12
Multiple factors need to be considered for successful management of a failed TAR, including loss of bone stock, malalignment, fractures or erosions of malleoli, condition of soft tissues, degree of degeneration of adjacent joints, and the presence of infection. Goals of treatment for failed TAR must be aimed towards restoration of limb length, alignment, stability, and function of the limb. Potential treatment options include revision TAR, ankle arthrodesis, or amputation. The choice of revision procedure largely depends on the amount and quality of bone stock, as well surgeon experience.1,5,7 Revision TAR may not be feasible in cases of large bone deficits, active infection, or poor vascular supply. A revision TAR may be desirable due to the advantage of preservation of ankle range of motion, but it also carries with it increased risks of complications and early failure in comparison to primary TAR. Kotnis et al. reported persistent pain in 40% of patients undergoing revision TAR following STAR failure compared to persistent pain in 20% of patients undergoing salvage arthrodesis. 5 In addition, reluctance from the FDA for approval of long-stemmed prostheses has considerably narrowed surgical options in cases of talar collapse. 13
Although ankle arthrodesis is a more reliable means of treatment for failed TAR and provides more predictable outcomes in comparison to revision arthroplasty, successful salvage arthrodesis is more difficult to achieve than primary arthrodesis due to shortening of limb and difficulties with fusion due to variable vascular status of talus and/or presence of talar collapse.1,5,7,14 Two important issues affecting the decision-making for surgery of failed TARs are the extent of large bony void and determination of the best method of fixating the fusion. 2 Methods for salvage arthrodesis include intramedullary nailing with or without femoral head allograft, anterior plating, compressive screws, or used of an intramedullary nail through a trabecular metal implant. Excessive bone loss usually will necessitate a tibiotalocalcaneal (TTC) arthrodesis. Berkowitz et al. recommended salvage arthrodesis for failed TARs with talar bone defect less than 2 cm. 15 For bone defects greater than 2 cm, tricortical allograft or autograft, femoral head allograft, or distal tibia allograft are recommended in order to restore limb length and maintain a biomechanical advantage of muscles and tendons crossing the ankle joint. In cases of collapse from talar avascular necrosis or with painful subtalar joint arthritis, a TTC arthrodesis is indicated. 15
Case report
The patient is a 66-year-old female with past medical history significant for hypertension, hyperlipidemia, obstructive sleep apnea, anxiety, asthma, and morbid obesity who is 2 years status-post 3 piece mobile bearing TAR surgery to her right ankle with tendoachilles lengthening. Her initial procedure was performed to address severe post-traumatic arthritis to her right ankle after suffering an ankle fracture years prior. Two months after her initial TAR, the patient fell at home fracturing her medial malleolus. She underwent open reduction internal fixation (ORIF) of this fracture with the primary author without complication. At the time of the medial malleolar ORIF the TAR was appreciated to be in correct alignment without migration from the original implanted position.
The patient resolved the medial malleolar fracture without issue however with progression to full weight bearing she developed pain to both her ankle and subtalar joints. Serial computed tomography (CT) imaging was obtained showing severe progressive cystic changes to the subtalar joint, cystic changes surrounding the tibial total ankle component, posterior displacement of the talar total ankle component, 15 degrees varus angulation at the level of the ankle joint, and hypertrophic bone growth to the anterior and posterior ankle joint margins (Figure 1). The patient failed exhaustive conservative treatment including physical therapy, bracing, and corticosteroid injection therapy. After 19 months without resolution of symptoms, and being unable to return to pre-operative levels of daily activity, the patient elected to pursue conversion to TTC arthrodesis. With conversion of her TAR to a TTC arthrodesis it was expected that we would need to span the osseous deficit which would remain with removal of her implant. Without a supportive graft she would have a significant loss in limb length to the affected side. As it would result in too much donor site morbidity to obtain a tri-cortical bone autograft sizable enough to span the deficit, the decision was made to use a combination of autograft cancellous bone, allograft demineralized cortical bone with adult mesenchymal stem cells, and allograft recombinant human bone morphogenic protein (rHBMP) with a custom cage truss implant to allow for maintenance of limb length with osteoinductive and osteoconductive potential. This construct was intended to provide structural support and prevent migration of the bone graft.
Pre-op CT imaging.
For the purpose of custom implant design, a pre-operative CT scan was obtained and measurements were collected for the fabrication of a custom cage truss implant (4Web Medical, Frisco, TX, USA) created specifically for the patient with a central opening to allow for the passage of a TTC intramedullary (IM) rod. The design and fabrication process included participation in a meeting with the designing engineers to discuss the patient condition and surgical plan. Using three-dimensional (3D) software reconstructions of the patient’s anatomy acquired from the CT scan, the bone resections were planned and the engineers then designed a custom titanium truss implant to occupy the anticipated deficit after removal of the total ankle construct. Following surgeon design approval, the patient specific device was 3D printed.
Once the custom cage implant had been fabricated we preceeded with our surgical plan. Attention was initially directed medially and the internal fixation from previous medial malleolar ORIF was removed in total without incident. Attention was then redirected to the anterior ankle joint. The anterior incisional approach was carried out using a linear incision centered on the tibialis anterior tendon. The branches of the superficial peroneal nerve and anterior arteriovenous structures were preserved and the extensor retinaculum was incised at the lateral border of the tibialis anterior tendon. The ankle joint capsule, significantly hypertrophied from previous intervention, was incised and the three-component total ankle implant was readily accessible. The poly component was explanted and noted to have significant wearing predominantly on the medial aspect consistent with the patient’s varus deformity. The hypertrophic bone growth to the anterior ankle was resected and the tibial total ankle component was removed revealing significant cystic changes consistent with pre-operative imaging. The talar total ankle component was then leveraged free from the residual body of the talus again uncovering cystic changes consistent with pre-operative imaging. The hypertrophic bone growth to the posterior ankle joint was then resected to create an even plane for the purpose of our cage implant. Through a separate incision the subtalar joint was prepared for arthrodesis with removal of residual cartilage from the arthritic joint and autograft cancellous bone was then harvested from the body of the ipsilateral calcaneus.
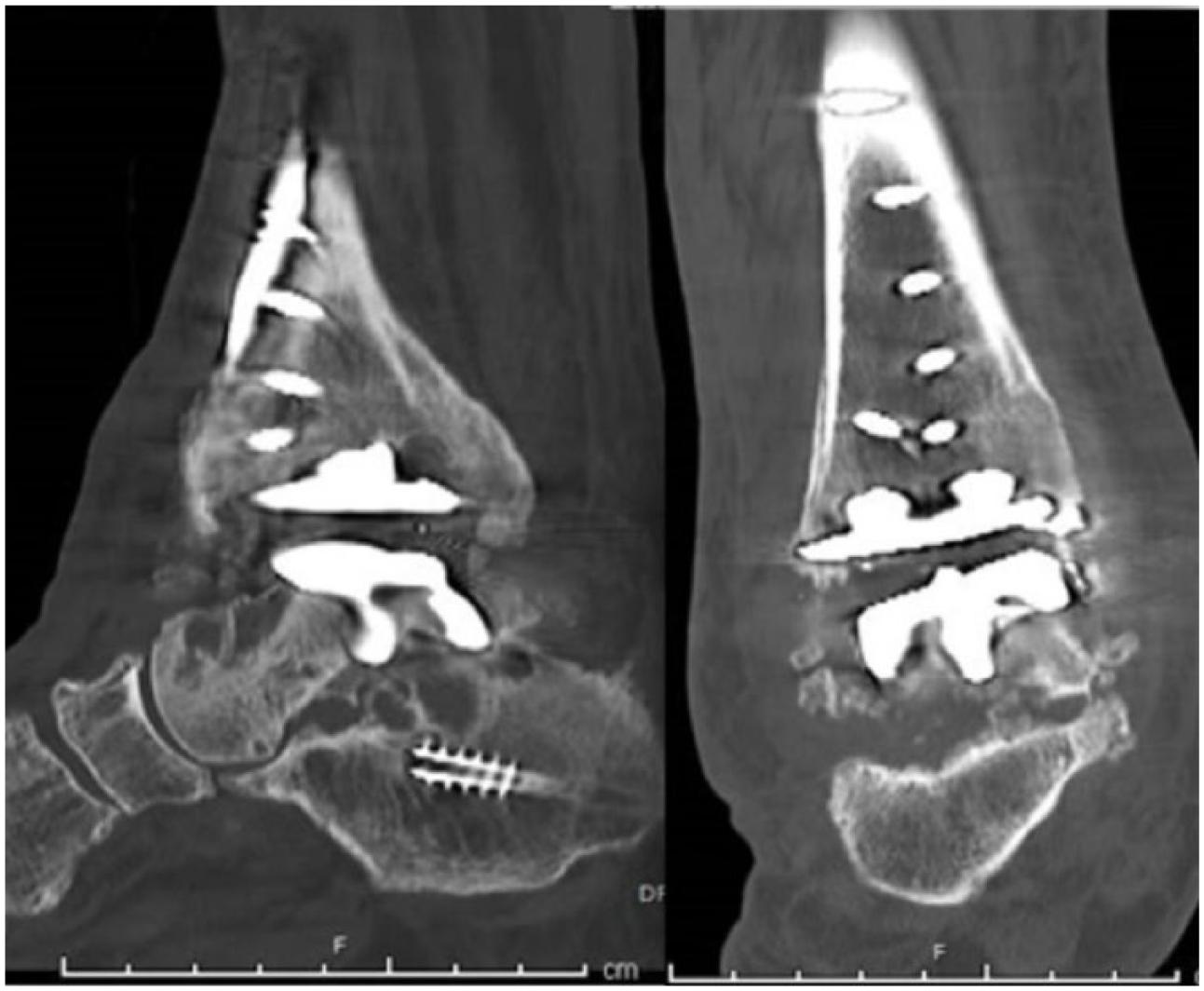
The custom cage implant was then temporarily placed into the ankle arthrodesis site for evaluation on intra-operative fluoroscopy. The position of the arthrodesis was at 10-degree external rotation of the foot with slight posterior displacement of the residual talus and without any flexion or frontal plane rotation. The custom implant was removed and packed with autograft cancellous bone in addition to allograft rHBMP with bovine collagen, and allograft demineralized cortical bone with adult mesenchymal stem cells. The implant with graft was again inserted into the fusion site and temporarily fixated in place with the guide wire for our IM rod through the central opening in our implant in a retrograde fashion. The distal tibia was reamed and a size 10 150mm IM rod was advanced across our subtalar and ankle joints spanning the custom implant. This was then securely fixated in static fashion with compression across our implant using a total of seven 5.0 screws. The incision was then closed in anatomic layers and a posterior splint with sugar tong was applied (Figure 2).

Immediate post-op imaging films.
The patient was admitted to observation per PACU protocol. She was discharged to a skilled nursing facility post-op day 2 once pain was controlled on oral analgesics. She remained strictly non-weight bearing to the operative extremity for 12 weeks. Skin staples were removed post-op week 3 and capillary fill time remained immediate to the incision site and distal digits. No signs of clinical infection were appreciated, and the soft tissues healed without incident. She was then transitioned into a short leg cast at post-op week 2. At post-op week 12 she progressed to partial protected weight bearing in a controlled ankle motion boot with physical therapy for gait training. At post-op week 16 the patient was progressed to full unrestricted weight bearing in her normal shoe wear with a gauntlet ankle brace.
The patient followed post-operatively at weeks 1, 2, 4, 6, 8, 12, and 16 with her final post

Weight bearing films 7 months post op.
Discussion
Daniels et al. reported that 7% of 111 patients with STAR prostheses experienced arthroplasty failure with subsequent tibiotalar arthrodesis at mean follow-up of 9 years. 9 Gross et al. reported salvage tibiotalar fusion rates of 93.7% in 111 ankles procedure and salvage TTC fusion rates of 64.7% in 82 ankles at mean follow-up of 34.8 months. Rates of nonunion were significantly higher in patients undergoing TTC arthrodesis vs. tibiotalar arthrodesis. 2 Kamrad et al. reported salvage tibiotalar fusion rates of 90% in 130 ankles and salvage TTC fusion rates of 90% in 58 ankles at minimum follow-up of 12 months; 75% of the failed salvage arthrodesis successfully fused after the 2nd attempt, with 3/188 eventually resulting in amputation. Only 47% of the 188 cases reported satisfaction with salvage arthrodesis. 16 Rahm et al. compared results of primary tibiotalar arthrodesis vs. salvage arthrodesis following failed TAR, with salvage arthrodesis showing significantly worse outcome in reference to pain and function, increased OR time, and increased incidence of revision following arthrodesis with rates of nonunion being similar between both groups. 6
Use of autologous bone in combination with titanium cages has been reported with success in spine surgery. Early attempts at employing the technique in the ankle used a rudimentary mesh titanium cage with morselized femoral head allograft. These cases, however, had disappointing results.17,18
A more recent case report by Hsu and Ellington used a similar custom 3D-printed titanium truss cage with TTC nail and combination of allograft and autograft bone resulted in pain free ambulation with full unrestricted weight bearing at 1 year post-op. 19 The patient was treated for a chronic nonunion of a distal tibial fracture yet the case does show proof of concept.
Although an isolated case report, the case presented here does show promise for further development of the technique. With continued advancement and availability of these custom 3D-printed titanium cage constructs the results seem to be trending toward more positive outcomes. We believe this technique warrants further research and consideration as a potential addition to the failed total ankle arthroplasty revisional arthrodesis treatment algorithm.
Footnotes
Declaration of conflicting interests
The authors declare that there are no conflicts of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
