Abstract
Some patients with severe dysphagia need to undergo percutaneous endoscopic gastrostomy (gastrostomy feeding), which improves nutrition but leads them to feel they are not living like human beings. The KT (Kuchi-kara Taberu, or ingesting orally in Japanese) index was developed in order to comprehensively assess and intervene in problems with eating and swallowing. We present three cases where the KT index improved quality of life after gastrostomy feeding. Through continued nursing care using the KT index, the patient in Case 1 was able to eat orally again; the patient in Case 2 could eat a piece of jelly and communicate a little; and the patient in Case 3 was able to ingest a small amount of food orally, with support from her husband. Thus, the feeding support provided by the KT index radar chart improves quality of life, even after the implementation of gastrostomy feeding. Further studies are needed to investigate how the KT index best helps elderly patients with severe dysphagia live like human beings while taking into account the perspectives of patients and their family members.
Introduction
Elderly patients admitted to acute hospitals often have eating and swallowing problems, which happens at Ward E3 (mixed specialties) of the Matsumoto Medical Center. Oropharyngeal dysphagia increases with age and can have devastating health implications, such as malnutrition and aspiration pneumonia. Age-related dysphagia, potentially resulting in ethical and moral issues, is the result of the naturally diminished function of senescent swallowing, and the comorbidity of many age-related diseases and their treatments.1,2
Some patients with severe dysphagia need to undergo percutaneous endoscopic gastrostomy (PEG), also known as gastrostomy feeding. These patients’ nutrition can be improved by gastrostomy feeding, but they feel they are not living like human beings. Eating and drinking should be related to enjoyment, communication, and fulfillment until the end of life. Recently, the KT (Kuchi-kara Taberu, or ingesting orally in Japanese) index was developed by Koyama and others in order to comprehensively assess and intervene in problems with eating and swallowing.3,4 In this report, we present three patients who were able to improve their quality of life even after undergoing gastrostomy feeding, through the use of KT index radar charts and its ensuing nursing care, in cooperation with other clinical and allied health staff. The usefulness of the KT index radar chart will also be discussed.
The KT index (English version)
As described by Maeda et al., 4 the KT index consists of 13 items relating to physical, nutritional, and medical conditions. These 13 items are “willingness to eat,” “overall condition,” “respiratory condition,” “oral condition,” “cognitive function while eating,” “oral preparatory and propulsive phase,” “severity of pharyngeal dysphagia,” “position and endurance while eating,” “eating behavior,” “daily living activities,” “food intake level,” “food modification,” and “nutrition.” The patients are examined through noninvasive tests and daily conditions and changes are assessed. Each item on the KT index is rated 1 (worst) to 5 (best) points. The KT index, drawn in a radar chart, provides visual information and helps caregivers recognize weak items they should focus on. It also shows the effects of intervention through the comparison of before-and-after charts, as suggested by the developers. 3
Case reports
Case 1
An 81-year-old man with ischemic heart disease and Alzheimer’s disease was transferred to our hospital due to pseudomembranous enterocolitis. On admission, he was 168 cm in height and 50 kg in weight. The levels of serum albumin, sodium, urea nitrogen, creatinine, and C-reactive protein were 2.0 g/dL, 140 mEq/L, 21 mg/dL, 0.98 mg/dL, and 9.83 mg/dL, respectively. His HbA1c level was 5.2%. He needed total assistance for the activities of daily life. After prolonged abstinence from food due to aspiration pneumonia and repeated pseudomembranous enterocolitis, PEG was implemented. As shown in Figure 1, his initial and second assessments of the KT index radar chart before the implementation of PEG indicated the worsening of “willingness to eat” and “severity of pharyngeal dysphagia.” By implementing oral care, with oral cavity cleaning and modified thermal stimulation using an ice-cold cotton swab five times a day, he was able to eat orally again. The third assessment of his radar chart four weeks after PEG (52 days after the initial assessment) showed improvement of several items regarding eating and swallowing—“oral condition” and “oral preparatory and propulsive phase.”

The KT index radar chart in Case 1. The KT index was assessed on the 77th hospital day when a speech-language therapist intervened, on the 91st hospital day when percutaneous endoscopic gastrostomy was implemented, and on the 129th hospital day.
Case 2
An 80-year-old woman with type 2 diabetes, and dementia with Lewy bodies, was referred and admitted to our hospital due to aspiration pneumonia. On admission, she was 151 cm in height and 38 kg in weight. The levels of serum albumin, glucose, sodium, urea nitrogen, creatinine, and C-reactive protein were 2.5 g/dL, 144 mg/dL, 131 mEq/L, 15 mg/dL, 0.28 mg/dL, and 4.96 mg/dL, respectively. Her HbA1c level was 5.6%. She needed total assistance for the activities of daily life. Video endoscopic examination showed erroneous swallowing of saliva; PEG was hence implemented. Along with continuing nursing care, her radar chart (Figure 2) indicated that “severity of pharyngeal dysphagia” was not apparently improved despite her consistent “willingness to eat.” In addition to oral care with oral cavity cleaning and modified thermal stimulation, sensory stimulation to improve her low arousal made it possible for her to eat a piece of jelly and communicate a little with her family members. The third assessment of the KT index performed 111 days after the first one showed the improvement of “overall condition.”
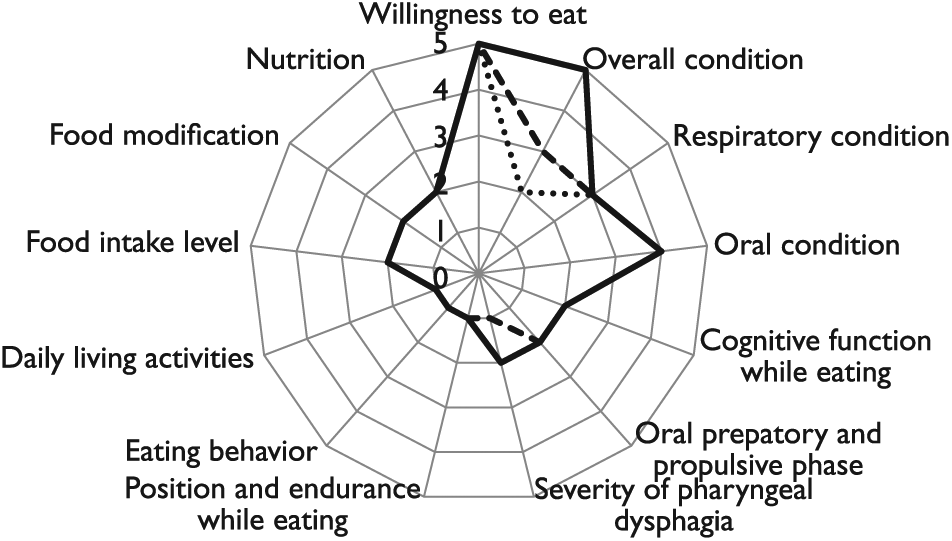
The KT index radar chart in Case 2. The KT index was assessed on the first hospital day when a speech-language therapist intervened, on the 10th hospital day when video-endoscopic examination of swallowing was conducted, and on the 112nd hospital day (at hospital discharge). At the initial assessment, the rate of “severity of pharyngeal dysphagia” was two (overlaid). Percutaneous endoscopic gastrostomy was implemented on the 23rd hospital day.
Case 3
An 86-year-old woman with type 2 diabetes and hypertension (cessation of treatment) was admitted to our hospital due to dehydration, renal failure, and decubitus ulcer on her hip and back. On admission, she was 157 cm in height and 45 kg in weight. The levels of serum albumin, glucose, sodium, urea nitrogen, creatinine, and C-reactive protein were 2.5 g/dL, 306 mg/dL, 148 mEq/L, 76 mg/dL, 2.28 mg/dL, and 23.37 mg/dL, respectively. Her HbA1c level was 6.7 %. She needed total assistance for activities of daily life. While her nutrition gradually improved after central venous nutrition, she became less willing to eat. Video endoscopic examination showed premature spillage of food into the pharynx, and impaired cough reflex, after which PEG was implemented. Through continued nursing care with the KT index radar chart, she was able to continue to ingest a small amount of food orally with the support of her husband. Her “willingness to eat” also improved (Figure 3). The rate of “willingness to eat” decreased 36 days after the initial assessment, but increased 98 days after that. The KT index item “oral preparatory and propulsive phase” could not be ascertained from the video endoscopic examination; this assessment could not be carried out without invasive tests.

The KT index radar chart in Case 3. The KT index was assessed on the 22nd hospital day two weeks before central venous nutrition was started, on the 58th hospital day when video-endoscopic examination of swallowing was conducted, and on the 120th hospital day four weeks after percutaneous endoscopic gastrostomy was implemented.
Discussion
We present three patients, who were able to feel like human beings, even after initiating gastrostomy feeding, due to use of the KT index chart for feeding support. Their vital signs improved; and their family members became happier. This in turn evoked similar feelings in the medical staff. The oral intake of food, even to a miniscule degree as in Case 2, seemed to improve quality of life, and the KT index radar chart was useful in this respect. The KT index was developed to comprehensively assess the eating-related conditions of elderly people. Koyama describes, in the preface of a textbook, how we can respect human dignity by supporting the maintenance of oral intake in an aged society. 3 Her words were consistent with a newly-set goal in the Ward E3 of our hospital for patients with severe dysphagia, which is to be able to live like a human being even after gastronomy feeding is initiated. Before then we had feared causing aspiration, and were less active in championing feeding support; and withheld food or fluid after the implementation of PEG.
In this study, a trained nurse of the Ward E3 assessed the KT index simply, and without invasive tests, after which she plotted a KT index radar chart for the three patients presented. The KT index radar chart was referred to for nursing interventions in individual patients who had problems with eating and swallowing; this was carried out in cooperation with other clinical and allied health staff, especially speech-language therapists whose therapy in oropharyngeal dysphagia is well appreciated. 5 The effect of nursing intervention, including feeding support and oral care, can be visually recognized by comparing radar charts of the KT index and assessed repeatedly during the clinical course. As with the results of their KT index radar charts, we realized there was insufficient feeding support for the KT index items of “position and endurance while eating” and “eating behavior.” In addition, their radar charts indicated that cooperation with multidisciplinary clinical and allied health staff would lead to comprehensive care for the patients. A limitation of this study was the sample size of only three cases. Applying the use of the KT index to a larger population would indicate the type of patients that would respond well to its use, as well as its effects on those who had initiated gastrostomy feeding.
Conclusions
We show that feeding support is suitable for individual patients by using the KT index radar chart. Using the chart improves quality of life, even after gastrostomy feeding is initiated. Further studies are needed to refine the use of the index in helping elderly patients with severe dysphagia live like human beings.
Footnotes
Acknowledgements
The authors are grateful to the other members of Nutrition Support Team of National Hospital Organization Matsumoto Hospital for their collaborations.
Declaration of Conflicting Interest
The authors declare that there are no conflicts of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
