Abstract
Dysphagia is a symptom of various underlying medical conditions. It can be attributed to age related changes, neurological, cognitive, respiratory and gastrointestinal diseases. These conditions may cause functional and anatomical changes along the swallowing tract. Impaired swallowing function and oromotor insufficiencies may result in inadvertent aspiration of fluids and/or particles during dental procedures. This article attempts to highlight the importance of identifying patients with dysphagia and discusses ways to reduce life threatening conditions that may arise during dental procedures.
Introduction
Dysphagia, or swallowing difficulty, occurs as a symptom of underlying medical conditions such as Parkinson’s disease, stroke, myasthenia gravis, deconditioning, muscular sclerosis, chronic obstructive pulmonary disease and achalasia. The prevalence of dysphagia is one in 25 adults in the United States 1 and 8–33.7% amongst community dwelling elderly2–4 in the UK, Korea and Japan. In the acute hospital setting in Singapore General Hospital we receive an average of 563 dysphagia related referrals per month in the inpatient setting, and an average overall attendance rate of 1237 per month, over the age of 65 years, in both inpatient and outpatient settings.
A breakdown in either neurological, cognitive, muscular, respiratory or gastrointestinal systems can result in physical or neurological impairments affecting the oral, pharyngeal or oesophageal swallowing mechanism, and/or the coordination of the entire swallowing process.
Anatomical changes to the tongue, oral cavity and swallowing tract following surgery, chemotherapy or radiation therapy to treat head and neck cancer can cause dysphagia. Long term side effects from radiation therapy result in fibrosis of the soft tissue and muscles in the irradiated zone, xerostomia and trismus, which will contribute to difficulty in swallowing. Critical care management, such as intubation or tracheostomy, can result in anatomical changes in the airway and pharyngeal tract. Deconditioning, following acute medical events, affects pharyngeal muscle strength, overall alertness, and tolerance. Swallowing difficulties resulting from cognitive issues may stem from varying alertness levels, reduced awareness of food or fluid in the oral cavity, decreased sensory processing and the lack of cognitive ability to respond, volitionally or reflexively. Muscle atrophy and deterioration of oral structures also occur with ageing. A list of some causes of dysphagia is shown in Table 1.
Causes of dysphagia.
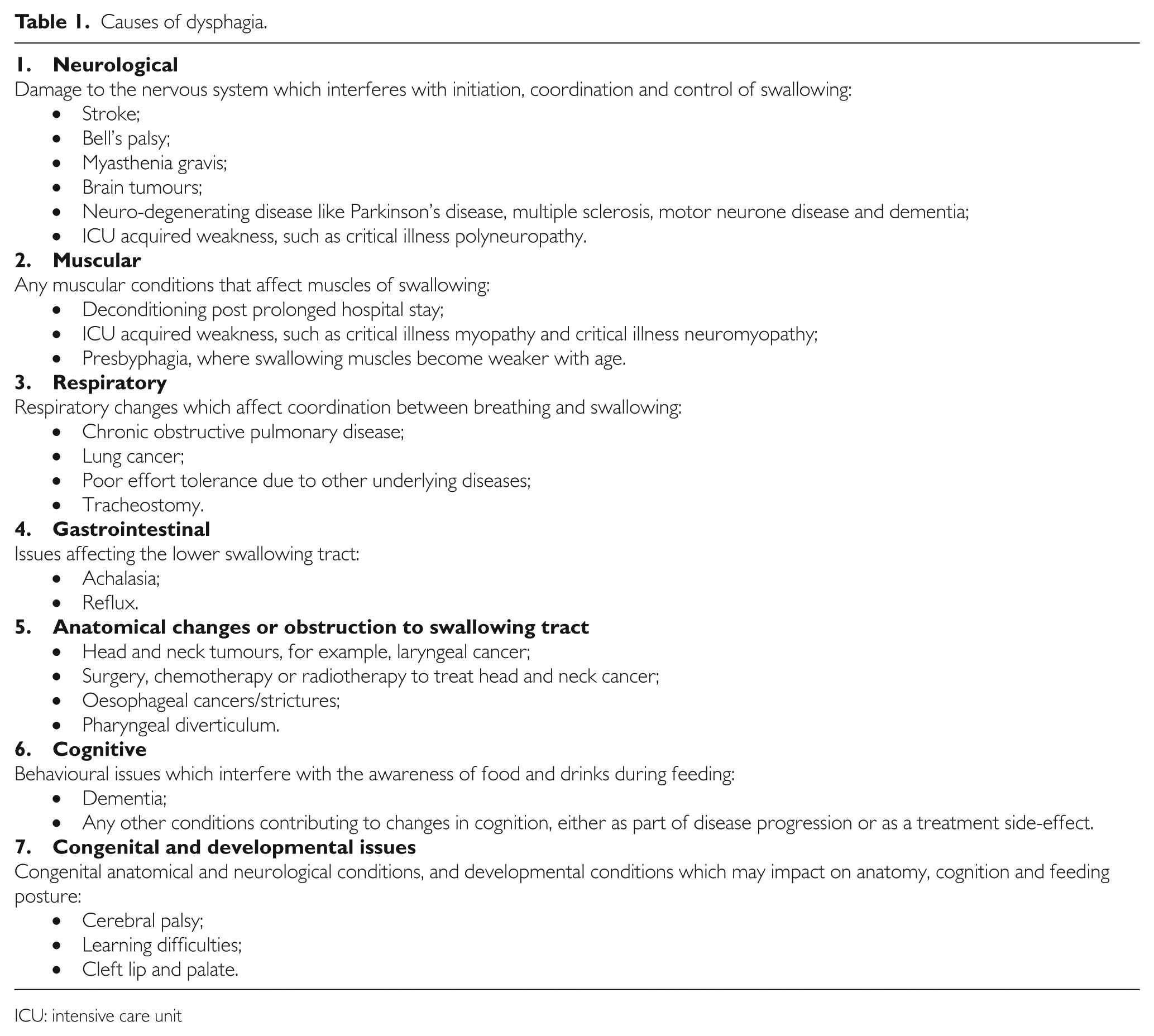
ICU: intensive care unit
Dysphagia may lead to aspiration. An impaired balance between body defence mechanisms (cough and mucociliary action, lymphatic clearance and cellular immune defences) and aspiration of food and secretions can develop into pulmonary complications 5 such as aspiration pneumonia, which is potentially life-threatening. This increases caregiver burden and requires lifestyle alterations for patients and their families.
Role of speech and language therapists and dentists
Diagnosis and management of dysphagia
The diagnosis and management of oral and pharyngeal dysphagia involves a multidisciplinary approach, often including professionals such as doctors of various specialties (e.g. neurologists, otorhinolaryngologists, gastroenterologists, head and neck surgeons, radiation oncologists), dentists, dietitians, nurses and Speech and Language Therapists (SLTs). SLTs are heavily involved in assessing and managing dysphagia. As part of clinical assessment by the SLT, medical information, oro-motor abilities and swallow function are evaluated. Objective swallow assessments such as Videofluoroscopic Study of Swallowing and Fibreoptic Endoscopic Evaluation of Swallowing can be used to visualize anatomy and swallowing function in real time.
Broad intervention techniques include restoration of normal swallow function via rehabilitative exercises and compensatory modifications to diet consistency and patient behaviour. Rehabilitative exercises work on strengthening the muscles involved in swallowing. Compensatory techniques offer a quick solution to prevent aspiration during feeding, such as modifying food and fluids texture, feeding mode, feeding posture or performing various manoeuvres such as chin tuck or head tilt.
Apart from macroaspiration of food and fluids, ongoing microaspiration of saliva secretions along with oral bacteria can occur. Large bacterial load in the mouth from poor oral hygiene can be aspirated into the airway.6,7 Maintaining optimal oral health significantly reduces the risk of aspiration pneumonia in the dysphagic individual.8,9
Caregiver training in providing oral hygiene
Dentists and SLTs should educate dysphagic patients and their caregivers on the importance of good oral hygiene in preventing aspiration pneumonia. SLTs can also screen for basic oral health issues during dysphagia assessments 10 and inform patients and their attending dentists. Caregivers and patients should be actively engaged in providing regular oral hygiene as oral bacteria accumulate daily. Good oral hygiene techniques using soft toothbrushes, interdental brushes and dental floss are recommended.
Bed-bound dysphagic patients should be seated in an upright position or placed side-lying during oral hygiene procedures to allow oral fluids and debris to flow out anteriorly or laterally. The use of fluoride toothpaste, preferably non-foaming, is recommended. As these patients may have poor control of water in the oral cavity, the amount of water used for rinsing must be reduced. Teeth and dentures should be cleaned after meals to remove food residue accumulation. Caregivers may use a wet gauze to remove food residue lodged in the buccal vestibules of the mouth for those who are unable to rinse effectively after eating. The use of chlorhexidine 0.12–0.2% mouthwash helps in the reduction of the bacterial load in the mouth. Cleaning of the dorsum of the tongue with soft cloth, soft toothbrush or tongue blade decreases bacteria on the tongue.
Precautions for dental procedures in patients with dysphagia
Regular dental visits are important to maintain oral health. However, dental procedures can pose an aspiration risk if dentists are unaware about the patient’s dysphagia. Treatment positions, such as lying patients supine, and the use of fluids during dental procedures may contribute to aspiration. Dysphagic patients may be unable to control and manage oral fluids safely due to reduced buccal, lingual and palatal muscle tone and strength. This may cause spillage of fluids into the pharynx. Patients also may have reduced pharyngeal strength and poor airway protection. They could inadvertently ingest and aspirate on fluids, debris and bacteria during dental procedures (Figure 1). In addition, some dysphagic patients may silently aspirate due to poor sensory feedback. This means they may not report difficulties or show overt symptoms such as coughing, choking, gagging or gurgling.
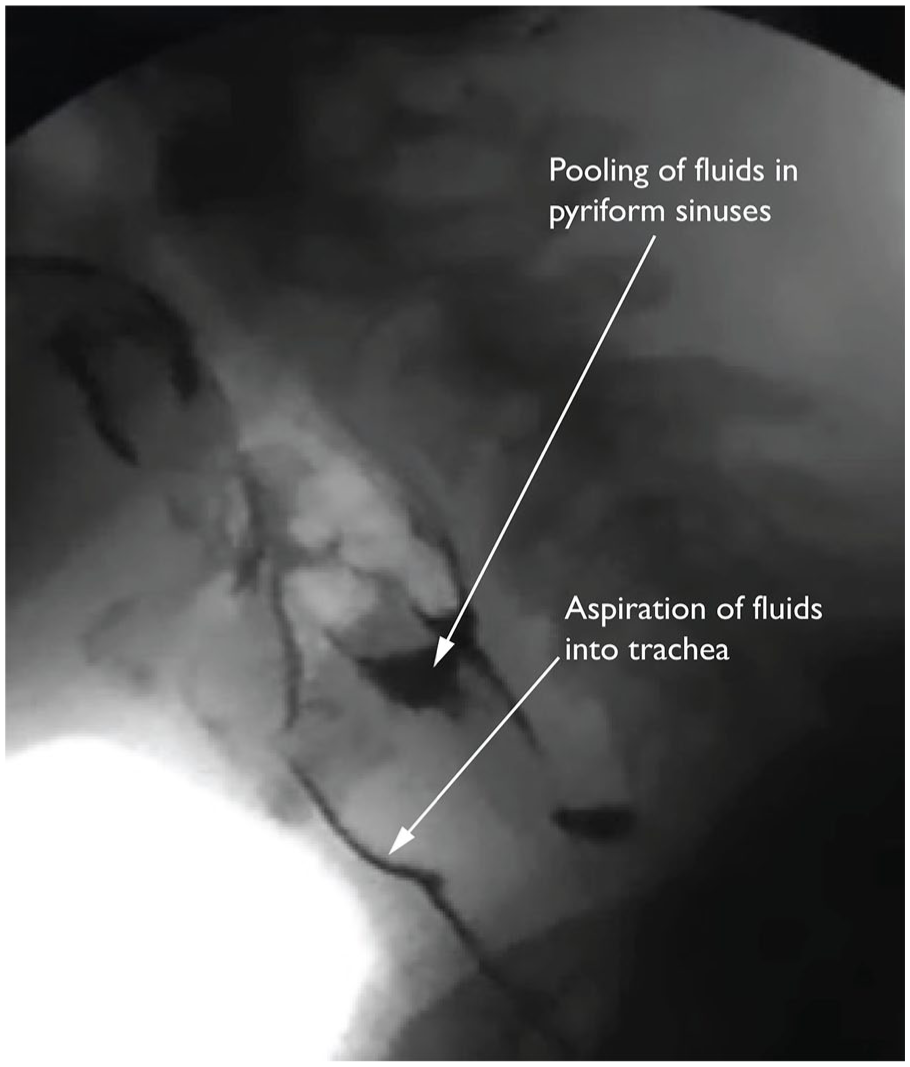
Aspiration of fluids into the airway, and pooling of fluids in the pyriform sinuses, which presents a potential aspiration risk (lateral view of head and neck region on videofluoroscopy).
SLTs can alert dentists to the severity of the patient’s dysphagia by issuing information cards (Figure 2) or memos. Also, SLTs can recommend appropriate compensatory strategies and special precautions to prevent aspiration during the oral care regime. 10 The prognosis of the patient’s dysphagia is helpful for dentists to make clinical decisions around the importance and urgency in carrying out dental procedures. Dentists may withhold certain procedures if the patient’s dysphagia is likely to resolve over six months. Preventive measures should commence early if the dysphagia is likely to deteriorate over time.

The Speech Therapy Department in Singapore General Hospital, in collaboration with National Dental Centre Singapore, developed a card for individuals with dysphagia to alert their dental professionals about their dysphagia prior to any procedures being carried out.
During registration, dentists usually obtain patients’ medical histories and medication usage via the use of self-reported questionnaires. These questionnaires should also include the presence and severity of dysphagia. Dentists should also confirm with patients on the presence of dysphagia prior to each session, as dysphagia severity could change with time. Dentists should be able to recognize general symptoms of dysphagia (Table 2) 11 together with potential signs of difficulty managing fluids during dental procedures. The severity of dysphagia must be considered when formulating dental treatment plans. Dentists should understand the patient’s need for fluid modifications, such as limiting the bolus size or changing the thickness of their beverages. This helps dentists gauge the risk of using fluids during procedures; for example, a patient who can manage only teaspoon amounts may not tolerate the use of water spray. Manual dental caries removal and scaling of teeth with hand instruments is encouraged. Patients who are unable to drink safely via continuous drinking will suggest their inability to control the continuous flow of fluids in larger amounts. Those who require thicker fluid consistencies for drinking are at higher risk of aspiration. Some dysphagic patients also have decreased neurosensory perception which impedes the protective coughing reflex. Adequate suction and saliva evacuation with help from dental surgery assistants prevent fluid accumulation during treatment. The dental team must keep their focus during procedures to reduce aspiration risk and not rush through treatment.
Symptoms of dysphagia. 11

Potential symptoms due to difficulty managing fluids during dental procedures.
A supine position during dental treatment should be avoided as it results in fluids flowing towards the oropharynx and increases aspiration risk. The treatment chair should not tilt more than 45 degrees (Figure 3). If aspiration risks are not managed, the patient can aspirate during treatment and may develop life-threatening severe aspiration pneumonia. After dental procedures, patients should be advised to monitor for signs of aspiration pneumonia, such as shortness of breath, cough or fever, and to seek immediate medical attention if unwell.

Tilt dental chair no more than 45 degrees for the dysphagic patient.
Protection of the airway during dental procedures is important when treating dysphagic patients. The use of a gauze trap or rubber dam prevents filling residues and small dental objects like crowns or implant screws from dropping into the oropharynx. Small dental tools such as implant screwdrivers can be secured with dental floss attached out of the mouth for easy and immediate retrieval if there is a loss of grip. Foreign body ingestion or aspiration could occur if a dislodged object is not retrieved before it passes the oropharynx. It can be fatal if the foreign body enters the airway and results in laryngeal spasm or airway obstruction.
When using impression materials, dentists should select the right sized impression tray for dental arch impression. Impression material of optimum viscosity should be used. The use of runny impression mix or excessive amounts of impression should be avoided as it can result in choking and aspiration. The patient should sit upright for the procedure. The use of high vacuum suction will aid in the removal of impression residue.
Dental prostheses to aid oral phase dysphagia
Specialized dental prostheses such as a palatal lift appliance can be fabricated to assist in swallowing for patients who experience oral dysphagia. It acts as a positioning device to assist the closure of the velopharyngeal port due to soft palate insufficiency by displacing the weakened soft palate to the normal palate position during swallow. 12 If tongue to palate contact is weak, a palatal augmentation prosthesis which artificially lowers the palatal vault enables the residual tongue volume or activity to contact the palate, 13 resulting in an improvement in bolus transportation and a decrease in the amount of oral and pharyngeal residues. 14 This reduces the aspiration risk after meals. A speech bulb prosthesis can be made to obturate palatal defect due to cancer resection to reduce nasal regurgitation. These prosthetic interventions help these dysphagic patients in swallowing and improve their quality of life.
Conclusion
The recognition of dysphagia in patients by dentists is of paramount importance. Detailed medical history taking and written memorandums or cards from SLTs can inform dentists of the patient’s dysphagic condition prior to dental treatment. This will enable the dentist to take necessary precautions to prevent aspiration during dental treatment. In addition, specialized dental prosthesis can be fabricated for suitable dysphagic individuals to assist in swallowing when eating.
Footnotes
Author contribution
Both authors researched literature and conceived the review. Both authors wrote, reviewed and edited the manuscript and approved the final version of the manuscript.
Availability of data and materials
Data sharing is not applicable to this article as no datasets were generated or analysed.
Declaration of conflicting interests
The authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
