Abstract
Introduction
Residency training is often carried out in busy clinics and a framework for teacher–resident conversation is essential for clinical teaching considering the time constraints. Clinical teachers can be viewed as professional role models who translate theory into practice and a partner in practice who includes residents in the treatment decision-making process. 1 A clinical teacher’s or preceptor’s role is one that requires multiple skill-sets. The clinical teacher bridges the essentials of education and clinical practice to facilitate the resident’s (learner–practitioner’s) learning. Preceptorship lies in the domain between teaching (relaying knowledge in a group or individual setting) and mentoring (providing individual support that goes beyond technical knowledge). It is often far easier for the clinical teacher to fall back on instruction rather than allowing the resident some freedom to practice. Thus, it is a challenge to strike the right balance that creates a positive and rich environment where experiential learning with feedback can occur in clinical practice. Additional challenges that the clinical teacher may face include meeting the needs and expectations of residents with varied learning skills and preferences.
Clinical teachers thus assume simultaneous and multiple roles during clinical teaching; they diagnose and manage both patients and learners simultaneously. They are problem-solvers of patients’ conditions and learners’ needs, communicators, preceptors and professional role models. 2
The model of the one-minute preceptor (OMP) in microskills was first proposed by Neher et al. in 1992. 3 It was designed for clinical teaching in busy practices and comprises a sequence of microskills that facilitates one-on-one teaching in clinical preceptorships. The traditional model of teaching by instruction or apprenticeship transfers technical content and questions factual recall. The OMP model involves the learner in the interpretation and application of data.
The clinical teacher can use the OMP process to entrust the ownership of the patient with a clinical problem to the resident utilising the five microskills: (1) Getting a commitment; (2) Probing for evidence; (3) Teaching general rules; (4) Reinforcing what is right; and (5) Correcting mistakes. 3 Each microskill can be used on its own or in any sequence to cater to different learning situations. 4 The first two microskills are useful for the diagnosis and determination of the resident’s knowledge base and reasoning in patient assessment, and to realise the teaching value of the case for the resident. The next three microskills focus on precepting by generalising key points for the residents in clinical diagnoses or standardised approaches in solving a category of clinical conditions. Resident competencies are achieved through the constant reinforcement and recognition of what is done right. They are informed of the effectiveness and impact of their work done correctly. When residents make mistakes, the provision of feedback on errors, omissions or misunderstandings in a non-threatening manner at appropriate times and settings help to create awareness of undesirable outcomes and consequences. This will aid residents to avoid making future mistakes. 5
Since the early 1990s, the National Dental Centre Singapore (NDCS) has collaborated with the National University of Singapore’s Division of Graduate Dental Studies to provide supervised clinical training in the five dental specialties for residents. Faculty in the three-year Residency Training Programmes (RTP) are clinical teachers of associate consultant level grade and above; that is, clinicians on the Ministry of Health Dental Specialist Register.
NDCS RTP faculty face a similar dilemma as faculty in internal medicine ambulatory clinics of having to teach and maximise teachable moments with residents in very busy outpatient clinics.6,7 In medicine, the OMP approach is a useful communication framework that helps the learner acquire problem-solving skills while presenting cases to the faculty.8–11 In dentistry, the OMP model has been adapted for use in an undergraduate dental school teaching clinic in the United States to enhance faculty–learner interaction, promote critical thinking in learners and encourage learners to use scientific evidence in formulating and supporting patient care decisions in the clinic. 12 The use of OMP in clinical teaching has been shown to be easy to learn and effective in helping preceptors improve their teaching.13,14 With the establishment of the SingHealth Duke-NUS Oral Health Academic Clinical Programme (ORH ACP) in 2014, faculty development workshops in the OMP microskills were conducted for NDCS RTP faculty.
Prior to 2014, no formal faculty development programmes were held and no feedback was sought from residents on their perceptions of the clinical teaching they had received in NDCS. The aim of this study was, thus, to assess if the OMP faculty workshops had an effect on residents’ perceptions of clinical teaching in NDCS. Clinical teaching in NDCS was simply defined for this study as the performance of teaching activities related to the OMP microskills. We hypothesised that residents would perceive the quantity and quality of clinical teaching and, in particular, the use of the OMP microskills more favourably one month after the faculty had attended the OMP workshop.
Methods
Study design
This is a one-group pretest–posttest design, 15 and the study was approved by the SingHealth Centralized Institutional Review Board (Ref: 2014/2200).
Subjects
Residents who were in the first or second year of specialty residency programmes (endodontics, oral and maxillofacial surgery, orthodontics, periodontics and prosthodontics) were included in this study. Third-year residents were excluded as they were unable to participate in the post-workshop survey since they had left the dental residency programmes.
OMP workshops
The OMP workshops were customised and taught in-house, with input from the Academic Medical Education Institute (AM.EI) faculty. Three separate workshops were conducted for clinical faculty, distinguished by specialty disciplines from May to August 2014: (1) Oral and Maxillofacial Surgery; (2) Orthodontics; and (3) Grouped faculty from Endodontics, Periodontics and Prosthodontics. Overall, 90.2% (37/41) of NDCS clinical faculty participated in the OMP workshops. Reading material on the OMP was emailed to all participants one month prior to the workshop. The workshops were interactive and comprised lectures, videos and role play. The role plays were specific to the different specialties and there were reflection and group discussions on the application of OMP in the current clinical teaching context. At the end of the workshops, laminated cards summarising the skill sets of the OMP and literature for further reading were given to all workshop participants.
Pre- and post-workshop surveys
The pre- and post-workshop resident surveys were designed in consultation with AM.EI faculty. The surveys were administered by an executive in the ORH ACP office. All first- and second-year residents from the specialty residency programmes were given the same questionnaire before and one month after the workshops for clinical faculty were held (see Appendix 1). They were asked to rate the overall quantity of clinical teaching (1–3, 3 = Excellent), the five elements of OMP on how adequately they were performed in the learning environment (1–5, 5 = Extremely), their perceptions of the most important of the five microskills and the overall quality of clinical teaching (1–4, 4 = Excellent).
Analysis
Descriptive statistics, such as percent, means and standard deviations, were generated for participant demographic characteristics as well as for the summary responses to the survey items. To determine the impact of the OMP workshop on clinical teaching by the NDCS faculty, we compared residents’ perceptions of clinical teaching and the five microskills, as obtained from pre-workshop and one-month post-workshop surveys. Given that the ratings were obtained on a Likert scale, we used non-parametric statistical tests (Wilcoxon signed-ranks tests) to identify the change in residents’ perceptions, and displayed the results of those tests visually by graphing the percentages of respondents whose views on teaching became more negative, did not change or became more positive.
Results
A total of 34 residents participated in the pre- and post-workshop surveys. Of these, 16 were first-year residents and 18 were second-year residents. The demographics of the 34 residents are shown in Table 1.
Demographic data.

Residents’ perceptions on the quantity of clinical teaching did not differ (p = 0.480) between pre- and post-workshop assessments (Figure 1).
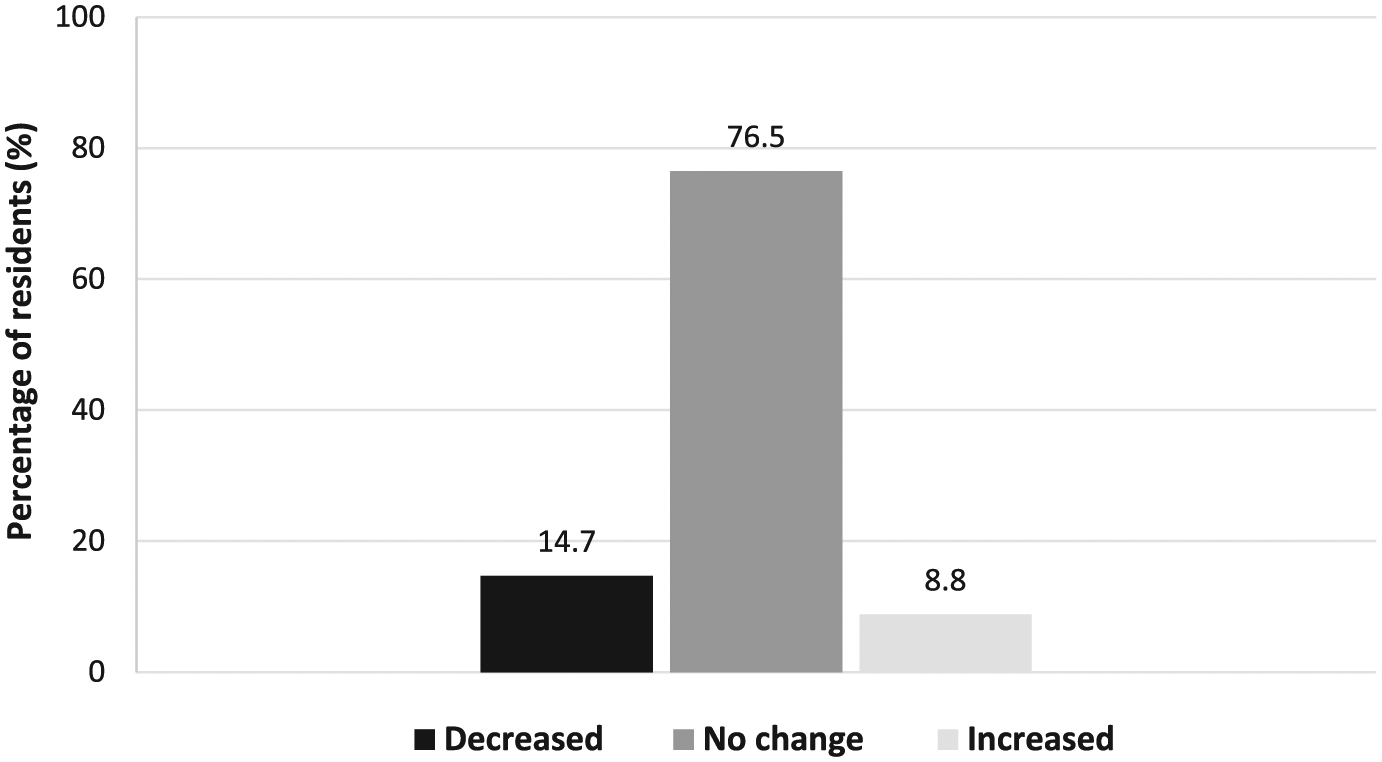
Changes in residents’ perceptions on the quantity of clinical teaching before and after faculty workshops. Residents’ pre- and post-workshop ratings were compared using Wilcoxon signed-rank tests (p = 0.480).
Among the five microskills, there was a significant improvement (p = 0.035) in residents’ ratings on the adequacy of “Teaching general rules”. The ratings on “Reinforcing what is right” also improved quite substantially, but the improvement did not reach statistical significance (p = 0.100). Figure 2 illustrates the changes in residents’ ratings on the five microskills pre- and post-workshop. “Teaching general rules” was chosen by the highest number of residents as the most important microskill both before (35.3%) and after (38.2%) the faculty workshop (Figure 3).

Changes in residents’ perceptions on the adequacy of each microskill. P-values were obtained via comparisons of residents’ pre- and post-workshop ratings using Wilcoxon signed-rank tests.

Changes in residents’ perceptions of the most important microskill before and after faculty workshops.
Residents’ perceptions on the quality of clinical teaching did not differ significantly (p = 0.134) (Figure 4).

Changes in residents’ perceptions on the quality of clinical teaching before and after faculty workshops. Residents’ pre- and post-workshop ratings were compared using Wilcoxon signed-rank tests (p = 0.134).
Discussion
In this study, we sought to determine if residents’ perceptions of clinical teaching improved after clinical teaching faculty attended a one-time OMP workshop. Unfortunately, the results of this study do not suggest that the workshop improved the residents’ perceptions of the quality or quantity of clinical teaching.
A recent general survey that was carried out on educational activities in NDCS revealed that previous learners had considered the use of OMP microskills in clinical teaching important. They valued the use of these skills in clinical teaching but perceived the practice to be infrequent while they were in the dental residency programmes in NDCS. 16 The frequently demonstrated microskills were “obtaining a commitment” and “teaching general rules”. In comparison, for this study, “correcting mistakes” and “teaching general rules” were the most adequately performed activities. The difference may be partly due to current learners in the dental residency programmes wanting to receive feedback on areas for improvement and previous learners who have the benefit of hindsight for reflection, plus the passage of time that may alter their recollection of past residency programme clinical experience.
In this study, current residents tended to view teaching as the most important out of the five teaching activities. This can be partly due to the inherent nature of our local education system and work flow in the NDCS outpatient clinics, where the tendency is for clinical faculty to ensure the patient flow in the residents’ clinics is smooth and that patient treatment provided is efficient and effective, with minimal disruptions. Thus, either the faculty may tend to provide solutions too quickly to the residents, or the residents may want a quick answer to their clinical problem in order to complete the treatment visit and move on to their next patient on the list.
As part of the faculty development framework in the ORH ACP, we encourage all faculty to have basic knowledge and awareness of the first three domains of the Academy of Medical Educators Professional Standards (2014), 17 of which the OMP model is part of the second domain on “Teaching and facilitating learning”. Prior to our in-house OMP workshops, many faculty were applying elements of the OMP model either intuitively or they had attended other AM.EI faculty development programmes.
It is hoped that the OMP model of teaching provides clinical faculty a useful framework to maximise their teachable moments in a busy outpatient clinic setting with residents, in addition to the time spent with them and the patients.
Clinical teaching is central to learning in dentistry and it is important to have skilled, effective clinical teachers.18,19 The assessment of clinical teaching is a subjective process and there is no agreed-upon conceptual definition or reference standard that exists for defining or measuring clinical teaching quality. 20
Limitations
For the survey items in this study, residents’ perceptions on the quality and quantity of clinical teaching were based on their own subjective assessments. Clinical teaching in NDCS was very simply defined in terms of the performance of teaching activities and, in particular, related to the use of OMP microskills. The fundamental premise upon which residents would make their assessment was based on adequacy in the transfer of knowledge and technical content for them to complete a task or procedure, in addition to honing patient-management skills in a good case-mix of cases encountered in the clinics. Developing any objective measures to determine quality and quantity in clinical teaching was beyond the scope of this study.
The majority of faculty involved in clinical teaching with the residents in the five specialty residency programmes in NDCS had attended the OMP workshops (37/41). This study, however, only looked at the residents’ perspectives of the OMP in clinical teaching with regards to their assessment on whether clinical faculty had practiced the OMP more frequently after attending the workshop. It was also only a short-term follow up (one month) and faculty may require more time for actualisation of their learning from the workshop training. Thus, future studies will need to look at clinical faculty’s perspectives of the OMP in clinical teaching, in addition to assessing the long-term effectiveness of faculty teaching through the self-assessment of clinical faculty attending the OMP workshops. 21 Using the triangulation model, peer assessments can also be considered in addition to the resident and self-assessments to provide an overall comprehensive assessment of teaching effectiveness. 22
Conclusion
Our study results revealed a one-time OMP workshop for NDCS faculty did not substantially improve residents’ perceptions of the quality or quantity of clinical teaching. The effort to improve clinical teaching by faculty must be a sustained effort and future studies should investigate the barriers to faculty members’ performance of the OMP microskills. We will also need to get clinical faculty perspectives on the use of the OMP microskills in clinical teaching in the future.
Footnotes
Appendix 1
Acknowledgements
The authors would like to give special thanks to Ms Veronica Lau, Executive, ACP Office Education Unit for the administration and collation of the survey data, to the staff from the AM.EI for their support in the development and implementation of the in-house faculty development workshops and to the staff from the Medical Education Research and Evaluation department for their help in the data analysis.
Declaration of conflicting interests
None declared.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
