Abstract
Background:
The National Dental Centre Singapore (NDCS) has been educating learners since the late 1980s. However, in this time, no formal feedback about these educational activities has been garnered from education stakeholders (comprising learners and faculty). Furthermore, no formal faculty development efforts to improve the educational activities have been done.
Purpose:
The aim of the study was to collect data from learners about the NDCS’s educational activities and the faculty’s attitude towards teaching.
Methods:
A survey was administered to 239 education stakeholders from May to July 2015. The survey on learners focused on learners’ perceptions on the importance and frequency of the One-Minute Preceptor (OMP) five-step microskills model of clinical teaching, and the quality and quantity of teaching overall. For faculty, the survey focused on their attitudes around teaching.
Results:
A total of 92 responses were received from learners. Learners perceived the OMP elements to be important (mean Likert scores ranged from 4.13–4.44 out of 5). However, they reported infrequent use of this teaching model by the faculty (range 3.06–3.50 out of 5). While learners reported quality and content of teaching to be adequate, they felt the number of clinical hours for teaching could be increased. The faculty reported positive attitudes towards teaching.
Conclusion:
This study provided educators with valuable feedback on the NDCS’s educational activities, identifying strengths and weaknesses of the programmes that they can work towards improving.
Introduction
The oral health care team in the National Dental Centre Singapore (NDCS) comprises various healthcare professionals including clinicians, oral health therapists, dental surgery assistants, dental assistants, dental technicians, radiographers, radiographic assistants, dental technicians, assistant dental technicians and staff nurses/ nurse managers/ enrolled nurses.
The NDCS has been involved in various areas of education of the oral health care team since the late 1980s to the early 1990s, when it was the Government Dental Clinic. Over the years, the NDCS has provided structured education programmes in collaboration with several education institutions for the oral healthcare community. Namely, these are:
The National University of Singapore-Master of Dental Surgery Residency Training Programme (NUS-MDS RTP). The residency training programme offers training in various dental specialties leading to Master of Dental Surgery
The Institute of Technical Education’s (ITE) Nitec in Dental Assisting programme (Nitec DA) for Dental Surgery Assistants, leading to the Certificate in Dental Assisting
The ITE Nitec in Dental Technology programme for dental technicians, leading to the Certificate in Dental Technology (Nitec DT)
The dental hygiene practical module for oral health therapists in Nanyang Polytechnic’s Diploma in Dental Hygiene and Therapy (DHT) course
The NDCS also organises professional development programmes such as the General Dentistry Lecture Series, Journal Clubs, Continuing Professional Education (CPE) talks, an Annual Scientific Meeting (ASM), and in-house training programmes for dental assistants. Practising dental professionals in NDCS’s oral health care team would have participated in one of the four structured education programmes mentioned above, or participated in one of NDCS’s professional development programmes, or both.
Teaching in the dental specialties primarily involves clinical work in an outpatient setting. Teaching methods employed often follow the traditional model of on-the-job interaction and apprenticeship. The primary goal of teaching clinics is to provide efficient, appropriate and quality patient care and clinical service. Residents are often seen as extra pairs of hands providing assistance in clearing patient caseloads during clinics. Any teaching that happens is usually carried out as and when the opportunity arises when patients are attended to. Faculty in the NUS-MDS RTP are of associate consultant level and higher. These are clinicians on the Ministry of Health (MOH) Dental Specialist Register. They will have had at least 2–3 years of specialist working experience following completion of a 3-year postgraduate residency programme recognised by the Dental Specialist Accreditation Board.
Teaching of dental surgery assistants (Nitec DA) involves both didactic instruction and practical chair-side assistance sessions in the clinic. Teaching of the dental technicians (Nitec DT) involves both didactics and practical sessions in the dental laboratory for clinical cases. Faculty for both auxiliary programmes above include clinicians of various grades: Dental Officers (DO), Registrars (R), Senior Registrars (SR), Associate Consultants (AC), Consultants (C) and Senior Consultants (SC). Dental auxiliaries in the faculty include Dental Surgery Assistants (DSA), Senior Dental Surgery Assistants (SDSA), Clinic Coordinators (CC), Senior Dental Technicians (SDT) and Principal Dental Technicians (PDT).
Teaching of the dental hygiene module in Nanyang Polytechnic’s Diploma in Dental Hygiene and Therapy programme (NYP DHT) for oral health therapists primarily involves clinical supervision of patients treated at the dental hygiene clinics at the Health Promotion Board. The faculty includes clinicians of various grades (R, SR, AC, C, SC) as well as oral health therapists. In the past decade, no formal session has been conducted to solicit feedback from NDCS stakeholders on the quality/standard of educational activities conducted by the NDCS. Furthermore, little has been done by way of formal faculty development to enhance the faculty’s teaching skills.
In 2012, Duke-National University of Singapore Medical School (Duke-NUS) launched the Academic Medicine Education Institute (AM.EI), which aims to support scholarship and educational development of SingHealth’s Academic Medicine faculty. The NDCS asked AM.EI to implement a faculty development workshop for their faculty. Following a review of the teaching environment, NDCS staff and AM.EI faculty decided that a workshop focused on the One-Minute Preceptor (OMP) model of teaching would be the most relevant for dental healthcare education.
The OMP model was developed in 1992 by two faculty members from the University of Washington School of Medicine. The model was designed to enable effective and efficient teaching of family practice residents, while addressing patients’ needs in a clinical setting. 1 The OMP model has been used in many clinical settings to create an active and engaging learning environment.
For instance, in medicine, the OMP approach is a useful communication framework that helps the learner acquire problem-solving skills while presenting cases to the faculty.2–5 The framework consists of five sequential teaching behaviours (also called microskills): getting a commitment, probing for supporting evidence, teaching general rules, reinforcing what was done right and correcting mistakes.
The OMP model was adapted for use at a teaching clinic in an undergraduate dental school in the United States (the School of Dentistry at Oregon Health & Science University) to fulfil several teaching/learning objectives. These included enhancing faculty–learner interaction, promoting critical thinking in learners, and encouraging learners to use scientific evidence in formulating and supporting patient care decisions in the clinic. 6
Applying these microskills would aid NDCS faculty in maximising teachable moments in busy outpatient clinic settings, where learners and faculty are pressured to be as efficient as they are thorough in the treatment of each patient. These characteristics of how teaching is conducted in our dental outpatient clinic setting are similar to those reported in internal medicine ambulatory care clinics.7,8
On 26 August 2014, the SingHealth Duke-NUS Oral Health Academic Clinical Programme (ORH ACP) was established. In view of this, it was timely and fitting to conduct a general survey of stakeholders (learners and faculty) in the NDCS regarding their perception of educational activities carried out by the NDCS. The administrators wanted to identify the NDCS’s strengths and weaknesses as an education provider, as well as to gain a better understanding of the educational landscape for the planning of future development programmes in education.
The literature reviewed for the study comprised types of evaluations used to assess dental programmes. However, most of the evaluations were of overseas programmes9–11 and dental schools, 12 and the survey questionnaires did not reflect our stakeholders’ interests or their experiences. The purpose of this study was to obtain a baseline understanding of the learner’s perspective of the teaching conducted by the NDCS, as well as the faculty’s perspective of the educational environment at the NDCS.
As the OMP model is one of the major faculty development efforts, the study sought to ascertain the level of importance learners placed on the faculty’s practice of OMP microskills in clinical teaching. It also hoped to find out the learners’ perception of how frequently they thought OMP microskills were practised by NDCS faculty in the NUS-MDS RTP, and the NYP DHT programme.
We categorised respondents into three groups. The respondents in Group 1 comprised learners in the NUS-MDS RTP and those in the NYP DHT programme. Group 2 respondents comprised learners in the Nitec DA or Nitec DT programme. An additional group (Group 3) consisted of respondents who had attended professional development programmes run by the NDCS but had not been enrolled in any of the four structured education programmes. Group 3 respondents were not considered in this study.
The hypothesis put forth was that there would be no difference between Group 1 and Group 2 learners in their perception of quality of teaching, quality of NDCS teachers and quantity of teaching.
Methods
Study design
This is a descriptive post-programme evaluation. The protocol was sent to SingHealth CIRB (Ref: 2015/2219) and it was deemed exempt from review because it is a programme evaluation.
Subjects
For this study, 239 full-time NDCS staff and MOH Holdings dental officers posted to the NDCS for a 6-month rotation were invited to participate in the survey. Table 1 shows the distribution of the survey and the response rate from various categories of staff in the oral health care team. Some of these faculty respondents also possessed the viewpoint of learner, having undergone training at the NDCS before. This explains why some respondents could answer questions in all three survey sections.
Distribution of the survey and the return response rate across staff categories in the oral healthcare team.

Survey
The three survey sections are: (A) Survey for Learners; (B) Survey for Faculty; and (C) Other Comments (to be completed by both learner/faculty respondents). Both sections (A) and (B) are branched surveys (see Figure 1 for the branching and Appendix for the survey).
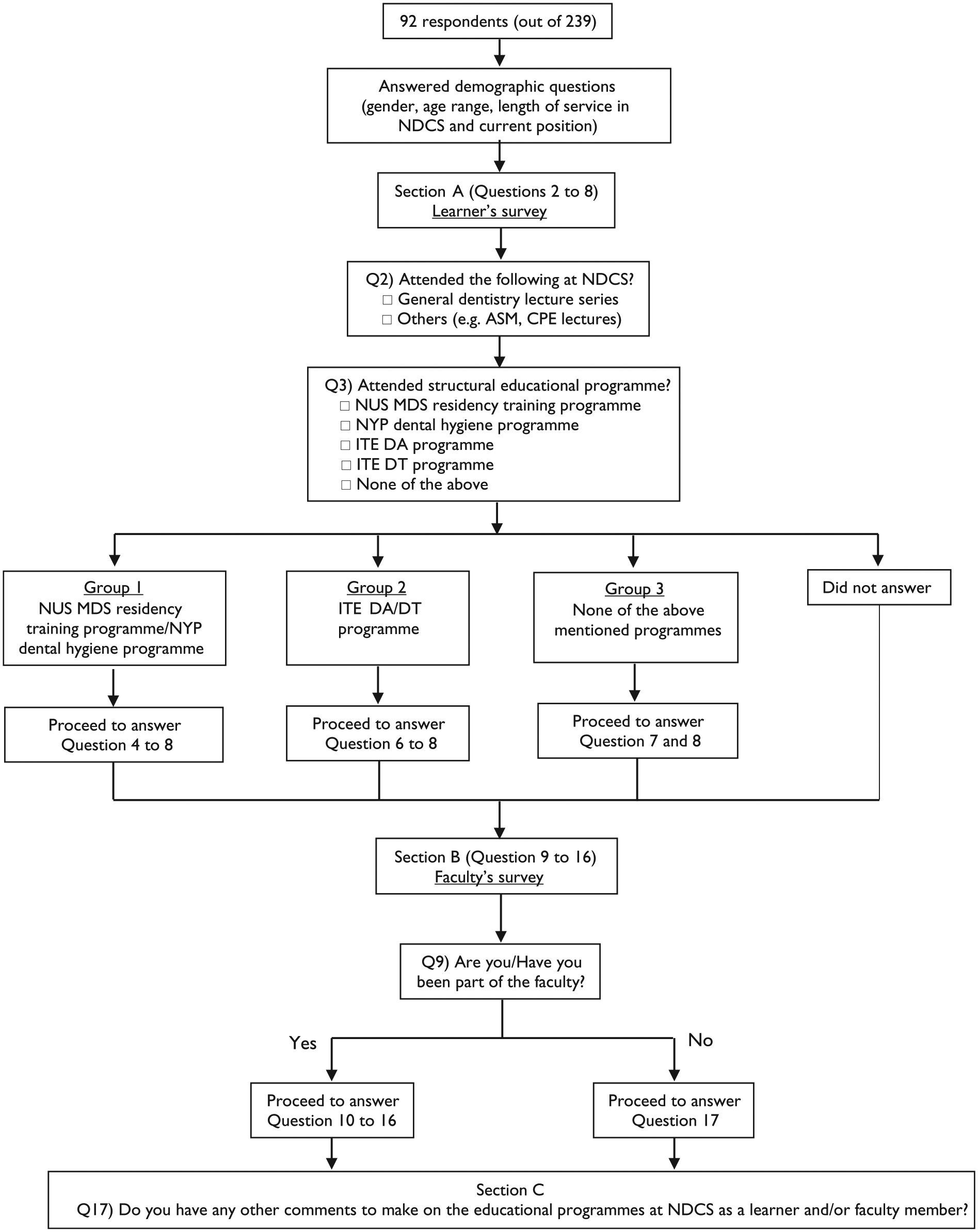
Overview of the branched survey.
All respondents were asked for basic demographic information including gender, age range, length of service in the NDCS and current position. Respondents were classified into three groups based on the programme they underwent as learners.
Group 1 comprised learners who had undergone the NUS-MDS RTP or the NYP DHT programme. Group 2 comprised those who had enrolled in the Nitec DA or Nitec DT programmes. Group 3 comprised self-identified learners who had attended professional development courses, but had not been enrolled in any of the NDCS structured educational programmes (see Figure 1).
Learners from Group 1 were asked to rate the five elements of the OMP model on how important (1–5, 5=Extremely important) they were in the learning environment and how frequently (1–5, 5=Extremely Frequent) they were demonstrated by faculty.
Learners from Group 1 and 2 were asked to rate the quality of teaching, quality of NDCS teachers (1–5, 5=Excellent) and quantity of teaching (1–3, 3=More than sufficient) in general.
All respondents (Groups 1, 2 and 3) were asked two open-ended questions about what worked and what did not in the programmes they had attended. Those who answered “yes” to being former or current faculty in the Section B (Faculty Survey) were directed to a set of questions regarding their teaching.
There were 13 Likert scale questions (1–5; 1=Disagree, 5=Strongly Agree) on the respondents’ perception of the quality of teaching and the teaching environment at NDCS. In addition, in two open-ended questions, respondents were asked about what they felt was working, and what was not, in the programmes they were teaching.
Eventually, all respondents were branched to an open-ended question in Section C where all participants could add other comments they had as a learner and/or faculty. The survey was reviewed by eight sample stakeholders for relevance, ease of use, language and clarity of questions (1 DO, 5 DSAs, 1 R and 1 C).
Administration of survey
The NDCS Director of Education met with the clinical staff in three departments (Restorative Dentistry, Orthodontics, and Oral & Maxillofacial Surgery), in addition to the dental auxiliary staff (DSAs, SDSAs, Dental Assistants DAs), Senior Dental Assistants (SDAs) and DTs, radiographers/ radiographic assistants) to give an overview of ORH ACP-Education and the purpose of the general survey. A list of NDCS stakeholders in education (learners and faculty members) was then identified (N=239).
At the end of April 2015, the NDCS Director of Education sent an email with a Google survey link to 161 staff (120 clinicians, oral health therapists, staff nurses/ nurse managers/ enrolled nurses, and 41 auxiliaries). Paper copies of the survey were sent through the ACP office to 78 staff members who did not own email accounts (26 DT and 52 SDSA, DSA, SDA and DA). All identified NDCS stakeholders were thus sent an invitation to participate in the general survey anonymously.
The survey was administered between 1 May and 31 July 2015. During this period, three email reminders were sent by the ACP office. Collation of survey data was done by an executive in the ACP office. De-identified data was sent to Duke-NUS Medical Education, Research and Evaluation Department (MERE) staff to provide basic descriptive and inferential statistics.
Analysis
Descriptive statistics were used to report on the collated data. Wilcoxon Signed Rank Tests were used to assess trends using the neutral rating of ‘3’ as the median on all items except for quantity of teaching where the median was set at ‘2’.
To test for statistical significance (p<0.05, 95% confidence intervals), the Mann–Whitney U test was performed. This allowed the researchers to compare the mean values of Group 1 against Group 2 in the three domains: quality of teaching, quality of NDCS teachers and quantity of teaching.
While analyses were conducted using non-parametric tests, the results showed little substantive difference compared with those garnered via parametric tests. Therefore, the means of all ratings were reported to aid in interpretation. All statistical analyses were performed using SPSS Version 23.
Results
There was an overall response rate of 38.5%, with completed surveys returned by 92 staff. The response rates from various categories of staff in the oral health care team are indicated in Table 1. The demographics of the 92 respondents are shown in Table 2.
Demographics of the 92 respondents who completed the survey.

Learners
Of the 92 respondents, 81.5% (75/92) had attended an educational programme in NDCS. Of these 75 identified learners, 21.3% (16/75) were from Group 1. Fourteen had attended the NUS-MDS RTP, while two had attended the NYP DHT programme. This 21.3% answered all questions related to the five microskills. Group 1 represents 41% (16/39) of the pre-identified past learners from the NUS-MDS residency training programme or the NYP DHT programme, and to whom the survey was sent.
Figures 2 and 3 show how the learners rate the importance of the five microskills, and their perception of demonstration frequency in their clinical learning environment. The importance rating of each microskill was significantly higher than the neutral rating of ‘3’ (p<0.05).

Overall mean ratings on the Importance of the 5 Microskills.

Overall mean ratings on the Frequency of the 5 Microskills performed by Faculty.
As for frequency of the five microskills performed by faculty, only “obtaining a commitment” and “teaching general rules” showed significantly higher ratings than the neutral rating of ‘3’ (p<0.05). The importance rating of the five microskills have higher overall mean ratings (4.13–4.44) than the frequency rating of the microskills demonstrated by faculty, as perceived by learners (3.06–3.50).
Group 2 comprised 22.7% (17/75) of the self-identified learners. Thirteen had attended the Nitec DA programme, while four had attended the Nitec DT programme. Group 2 represents 19.1% (17/89) of the original population of learners targeted for this group in the survey.
Group 1 and 2 respondents account for 44% (33/75) of all self-identified learners who had attended a structured programme by the NDCS (NUS-MDS RTP, Nitec DA, Nitec DT and NYP DHT). Both groups were asked to rate the quality of teaching in general, the quality of NDCS teachers specifically, and the quantity of teaching provided during their NDCS programme.
The overall mean ratings for quality of teaching, quality of NDCS teachers and quantity of teaching are illustrated in Figure 4 and 5, respectively. The value of the rating Group 1 respondents gave for the quality of NDCS teachers was significantly higher than the median rating. The quantity of teaching, meanwhile, had a significantly lower rating than the median (p<0.05). Among Group 2 respondents, only the rating of the quality of NDCS teachers was significantly higher than the median rating (p<0.05). Comparatively, Group 2 gave higher ratings than Group 1 in all three categories. Only quantity of teaching was rated significantly higher for Group 2 over Group 1 (2.12 vs. 1.75, p=0.034).
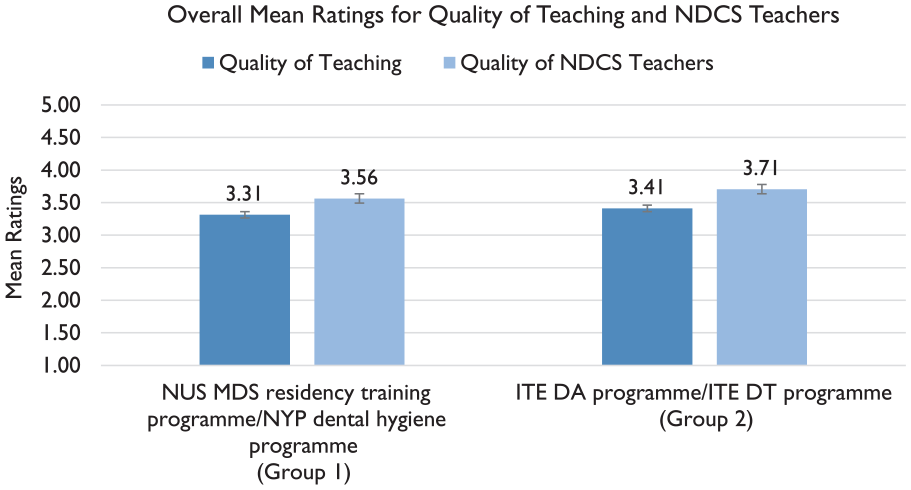
Overall mean ratings for Quality of Teaching and NDCS Teachers.

Overall mean ratings for Quantity of Teaching.
Group 3 comprised 56% (42/75) of the self-identified learners who had only attended professional development programmes by the NDCS, but had not attended any of the four structured education programmes.
Non-Learners
Some 18.5% (17/92) of the respondents classified themselves as never having attended any of the education programmes, and were thus branched to Section B (Faculty survey).
Faculty
Of the 92 respondents, 35.9% (33/92) identified themselves as faculty. Fourteen of the 33 had attended structured programmes, and so were required to address Section A of the survey. These 33 respondents represent 60% (33/55) of the original population in this category to whom the survey was sent.
The majority of the faculty respondents (19/33) were involved in one programme. Of the faculty, 36.4% (12/33) were involved in both didactic and clinical teaching. The majority (24/33) had attended a faculty development programme on teaching in the past __ one year, while 90.9% (30/33) indicated an interest to attend one in the future. Figure 6 displays mean ratings of responses to a series of positive and negative statements intended to capture the respondent’s perspective on teaching.

The overall mean ratings for each statement on the Faculty Perspectives on Teaching.
The six negatively framed statements in this section were re-coded during the analysis to indicate a higher score with positive rating. Thus, “I do not enjoy teaching” with a lower initial score would mean they did not agree with this statement – by reversing it, the rating was 4.30; suggesting they do enjoy teaching.
Discussion
The overall mean scores of the perception of actual teaching of the five microskills were lower than the overall mean scores for what learners felt was important in clinical teaching. Learners here refer to respondents who had attended the NUS-MDS RTP and NYP DHT programme. This discrepancy may partly be because OMP workshops had only been recently introduced to faculty, leading to varying degrees of exposure among them.
The frequently demonstrated microskills were “obtaining a commitment” and “teaching general rules”. Prior to the OMP workshops, some faculty members were applying elements of the OMP model either intuitively, or because of other faculty development efforts.
The survey results imply that the OMP approach is simple to learn, yet effective in helping preceptors improve their teaching.13,14 It behoves the department to continue providing relevant programmes that can help the faculty practise these skills. This is vital in view of the importance respondents have shown to place on the demonstration of these skills by faculty.
Overall, respondents who identified as learners perceived the quality of teaching by NDCS teachers to be “good”, and the overall quantity of teaching they were exposed to at NDCS to be “sufficient”. This was also reflected in responses to the open-ended questions: “lecturers are very experienced”, “approachable mentors”, “ample case loads and exposure”, “sufficient clinical cases, variety and complexity for clinical teaching”, and “structured clinical and didactic schedule”.
The difference in the nature and type of work done by Group 1 versus Group 2 respondents in clinics may explain to some extent the perceived difference in quantity of teaching. Group 1 provides treatment to patients under supervision, while Group 2 is primarily involved in assisting clinicians, or providing laboratory support in the clinical setting.
The majority of faculty respondents (72.7%) indicate having attended a faculty development programme (FDP) before. This can be attributed to the systematic implementation of an in-house FDP framework, ongoing since May 2014. The management has been aiming to get all faculty to attain basic knowledge for awareness and appreciation of the first three domains of the Academy of Medical Educators, Professional Standards (2012). 15 These domains are: 1. Designing and planning learning, 2. Teaching and facilitating learning, and 3. Assessment of learning. To date, the OMP (May to August 2014) and Giving Feedback (March–June 2015) in-house workshops conducted in collaboration with AM.EI have been attended by majority of RTP faculty. The DA/DT faculty were introduced to the OMP model via an in-house workshop in August 2015.
As reflected in the comments made in the in the open-ended question section of the survey, the strength of the NDCS’s educational activities lies in the expertise of faculty in the various programmes, as well as its ability to provide learners with a wide variety of clinical cases for teaching.
Weaknesses include insufficient interaction time with the learners in the clinics. Often, faculty are caught between teaching their students while meeting the demands of treating patients in a busy outpatient setting. Moreover, there are challenges faced by faculty with regard to knowing how to deal and engage with a many different types of learners, especially in some of the dental auxiliary programmes. This is reflected in the comments in the open-ended question section: “clinical hours need to be increased to ensure we have more clinical exposure”, “lack of time to think through cases due to tight schedule”, “it can be quite challenging to teach student trainees of diverse age-group and different learning styles” and “sometimes need more time with the resident”. Some of these comments are similar to reported programme strengths and student concerns in overseas dental schools. 12
Limitations
A complex branching questionnaire survey was used in this study to assess a broad, diverse educational landscape with a large sample population. The disadvantage of such a survey is the poor response rate and the inherent limitation of only self-assessed and self-reported needs being provided by responders who volunteered for the survey. 16 The identified stakeholders in education at the NDCS made up the intended sample size. We were hoping for at least a 50% response rate to the survey. The overall response rate of 38.5%, although low, has provided the Centre with a baseline understanding of how learners and faculty view the NDCS’s educational activities. Since the survey results are only from one institution, it precludes the extrapolation of the results to a larger survey group / a wider population in the medical community.
The nil-return status from the seven staff in the category labelled “Senior staff nurse/Senior Nurse Manager/ Senior Enrolled nurse/ Nurse Manager” is attributable to an omission of job category in the demographics info section. It was presumed the respondent would indicate their present position in the “Clinic Coordinator/ Assistant Clinic Coordinator” category. Being medically trained, few of the NDCS’s professional development programmes would have been applicable to, or of interest to them.
The low response rate (<40%) of staff in the category Dental Officers, Radiographer/ Radiographic Assistant, SDA/DA and DT may be attributed to the following factors:
MOH Holdings Dental Officers are subject to two 6-month rotations at the different polyclinics and SingHealth institutions every January and June. When this survey was conducted, it coincided with the rotation season in June.
The professional development programmes conducted by the NDCS likely did not cater to the needs of staff who fell in the categories of Radiographer/ Radiographic Assistant, Senior Dental Assistant/ Dental Assistant and Dental Technician.
Seventeen surveys were returned with the Learner Survey section left blank/incomplete, which could have affected the accuracy of the results. These surveys were returned by respondents who held auxiliary positions such as DSA, DA and DT. It is possible they had left the section blank because they had not attended any professional development programmes, as none that the NDCS organised catered to dental auxiliaries.
For length of service in the NDCS, there was an overlap between the 0–1 and 1–5 years ranges, so respondents who were in service for 1 year may have selected either option in the survey.
The main achievement of this survey was obtaining the view of learners who have undergone one of the four structured education programmes run by the NDCS. To build on these findings, future studies should obtain the perspective of current learners, measure the outcome of the OMP faculty development workshop, and assess the effectiveness and improvement of faculty teaching through self-assessment and by learners. 17
Conclusion
Our survey results revealed several key findings:
Learners consider the use of OMP microskills in clinical teaching important
While learners value the use of OMP microskills in clinical teaching, they perceived the practice to be infrequent while they were enrolled in one of the structured NDCS education programmes
There is room for improvement in terms of the quality of teaching, quality of teachers and the quantity of teaching provided in the structured programmes
Faculty reported interest in attending at least one faculty development programme on teaching in future
Faculty reported positive attitudes towards teaching
We will explore ways to address the identified weaknesses and continue to build on the current strengths of the various programmes. More detailed assessments from both learners and faculty in the four structured education programmes will be considered in future studies in relation to the practice of OMP microskills in clinical teaching.
Footnotes
Appendix
Acknowledgements
The authors give special thanks to Ms Syarafina Halim, Executive, ACP Office Education Unit for the administration and collation of the survey data, and to staff from AM.EI for their support in the development and implementation of the in-house faculty development workshops and the staff from the Medical Education Research and Evaluation (MERE) department for the help in designing the survey and the analysis.
Declaration of conflicting interests
None declared.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
