Abstract
The axillary arch is a rudimentary part of the latissimus dorsi. Generally it has a single insertion either into tendon of the pectoralis major, coracobrachialis or fascia over the biceps. Clinically, this anomalous muscular slip is known to cause neurovascular compression of nearby structures. The present case reports an unusual bifurcated fibrous insertion of an axillary arch with Y-shaped limbs. The stem of this muscle was a fleshy belly measuring 7.8 cm. The upper limb of this muscle, measuring 5.6 cm, was attached to the fascia covering the short head of biceps brachii and the coracoid process while its lower limb, measuring 5.1 cm, ended by merging with the brachial fascia over the biceps brachii below the deltoid muscle. The persistence of such a Y-shaped anomalous axillary arch might restrict the hyperabduction of the arm and compress the neurovascular structures passing below it.
Introduction
The axillary arch muscle is also known as Langer’s muscle, m. achselbogen or pectorodorsalis. This muscle is a small and thin variant muscle that originates from the anterior border of the latissimus dorsi, passes through the axilla and is inserted into the pectoralis major. It may insert on the pectoralis minor, fascia covering the biceps brachii, coracobrachialis or coracoid process of the scapula. 1 Rizk and Harbaugh reported the prevalence of the axillary arch in 8.6% of the cadavers they examined. 2
The axillary arch muscle develops embryologically from the pectoral muscle mass. It is hence generally innervated by the medial pectoral nerves. 3 However, because of its close relationship with the latissimus dorsi, it may receive nerve supply from the thoracodorsal nerve. 4
The axillary arch muscle is known to cause neurovascular compression of the arm as it crosses it. However, previous reports also highlighted the clinical complications that were manifested by the presence of an axillary arch such as thrombosis of upper limb, lymphodermia, shoulder instability and thoracic outlet syndromes. 5 Therefore, the presence of an axillary arch muscle is not only an interesting anatomical variation, but is also of clinical significance.
Case report
During routine dissection, we came across an axillary arch muscle in the region of the left axilla in a male cadaver aged about 46 years. This variant muscle originated from the anterior border of the latissimus dorsi, passed through the floor of and continued deep into the anterior wall of the axilla. While it crossed the coracobrachialis superficially, it became aponeurotic and near the medial border of the biceps brachii it divided into upper and lower fibrous bands, appearing Y-shaped. The upper band passed upwards and was attached to the fascia, covering the short head of the biceps brachii and the coracoid process of the scapula; the lower band passed downwards, attaching to the brachial fascia just below the level of insertion of the deltoid muscle (Figure 1). All neurovascular structures, such as axillary vessels and the nerves of the brachial plexuses, passed beneath this variant structure (Figure 2). The stem of the Y-shaped muscle was 7.8 cm in length. The upper band measured 5.6 cm and the lower band 5.1 cm in length. The muscle belly in the stem of the Y-shaped muscle was supplied by the nerve twigs from the medial pectoral nerve.
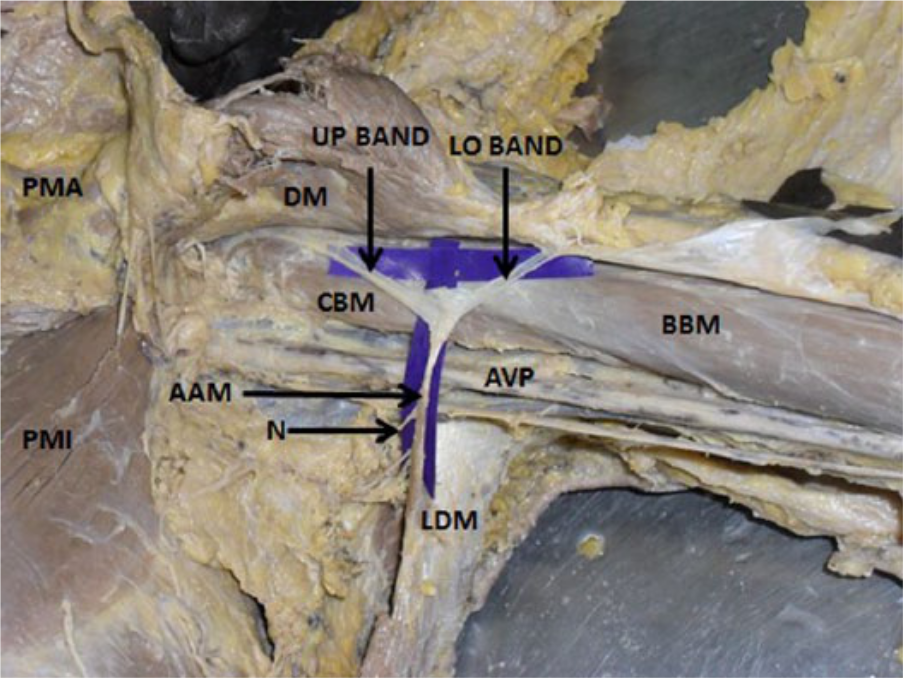
Dissection of axilla and upper arm of left side showing axillary arch muscle (AAM) originating from latissimus dorsi muscle (LDM) along with the two limbs; upper (UP) and lower (LO) bands. Branches of medial pectoral nerve (N) are seen supplying the axillary arch muscle.

Schematic diagram to show the pattern of Y-shaped axillary arch originating from the latissimus dorsi muscle and dividing into upper and lower bands. The neurovascular bundle of the axillary and brachial region being crossed superficially by the stem of the arch can also be seen.
Discussion
The presence of the axillary arch is known to cause syndromes involving neighboring structures such as median nerve entrapment and axillary vein entrapment as well as costoclavicular compression syndrome.6,7 Previous studies have mentioned the number of axillary arch muscles, but few have examined their atypical shape and attachment. Lama et al. reported an axillary arch muscle coexisting with the chondrohumeralis. 8 A case of a completely fleshy axillary arch inserting into the coracobrachialis has been reported by Mujahid Khan et al., 5 but none of these studies mentioned the fibrous bifurcation at its insertion as reported here. Loukas et al. reported multiple insertions of the axillary arch muscle into the pectoralis major, pectoralis minor and coracoid process, 9 but there was no insertion on the brachial fascia. In the present case, the upper and lower attachments were widely separate from each other and on different structures and areas.
The axillary arch muscle slips are not only potential sources of various compression syndromes, but also can complicate the procedures in the case of staging lymph nodes and axillary surgery. 10 It may also affect the lymphadenectomy of the axilla 11 and cause shoulder instability, leading to hyperabduction syndrome. 12 The presence of the axillary arch can also mislead diagnostic interpretation as it may appear as ovoid density and be confused as a mass within the axilla in a mammogram. 13 This anomalous muscle slip is believed to be predisposing to a local recurrence of malignant conditions such as melanoma and carcinoma of the breast. 14
Conclusion
The peculiar appearance of the axillary arch, with its bifurcated fibrous insertion into two distant sites on the arm, is a unique variation, giving rise to the possible danger of restricted hyperabduction at the shoulder joint. It can also compress the neurovascular structures passing below, leading to neurovascular compression syndrome and making this case noteworthy.
Footnotes
Acknowledgements
We acknowledge Mr Ganesh N Prasad, Artist, Department of Pathology, Kasturba Medical College, Manipal for the schematic diagram.
Conflict of interest
The authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
