Abstract
Transient Perivascular Inflammation of Carotid artery syndrome (TIPIC syndrome) is a non-specific inflammatory thickening of the carotid artery. The exact etiology of this syndrome is poorly understood. We will describe the radiological findings of a rare case of TIPIC syndrome in a patient with myelodysplastic syndrome and discuss the potential pathophysiological mechanisms.
Keywords
Introduction
Transient Perivascular Inflammation of Carotid artery syndrome (TIPIC syndrome) is characterized by perivascular non-specific inflammatory thickening of the carotid artery, clinically presenting as ipsilateral neck pain, triggered by neck movement. It is also known as “carotidynia” or “Fay syndrome” described as pain in the region of carotid bifurcation. 1 Referred pain in the periauricular and periorbital region may also be seen due to stimulation of the sympathetic plexus around the carotid artery.2,3 Lecler et al. 4 have reported an incidence of 2.8% in patients presenting with acute neck pain. International Classification of Headache Disorders (ICHD-2) removed carotidynia from a distinct clinical entity in 2004 and it is now considered a manifestation of various diseases. 5 We, hereby, describe TIPIC syndrome in a case of myelodysplastic syndrome. To the best of our knowledge, the TIPIC syndrome has never been reported in a patient with myelodysplasia.
Case report
A male patient in his seventies presented with complaints of progressively increasing left-sided neck pain, tenderness, fever, difficulty in swallowing, and progressive weakness for 3 months. Ultrasonography (USG) examination of the neck revealed circumferential soft tissue thickening around the left common carotid artery, extending till bifurcation (Figure 1(a)). CT angiography confirmed the findings of USG (Figure 1(b)–(d)). No evidence of dissection or luminal stenosis was seen. The contralateral carotid artery was normal. Imaging findings and clinical history were suggestive of Transient Perivascular Inflammation of Carotid artery syndrome (TIPIC syndrome) and treatment with anti-inflammatory drugs was started. The patient was also on antitubercular drugs for tubercular spondylodiscitis at D9–D10 level which was diagnosed 4 months back. He also had left pleural effusion. Laboratory investigations of present admission showed deteriorating blood counts with anemia and thrombocytopenia. Peripheral smear showed 10% blast cells with left shift. Bone marrow examination showed hypercellular marrow with dyspoiesis. Chromosomal analysis was done which showed 7q deletion. A diagnosis of myelodysplastic syndrome with excess blasts was made. However, despite treatment, the patient developed sepsis and succumbed after 2 weeks. (a) USG image shows circumferential hypoechoic thickening of left common carotid artery (arrows). Axial (b,c) and oblique sagittal (d) CT angiography images show circumferential perivascular soft tissue thickening around the left common carotid artery extending distal to bifurcation (arrows in d). Note compression of adjacent left IVJ in c.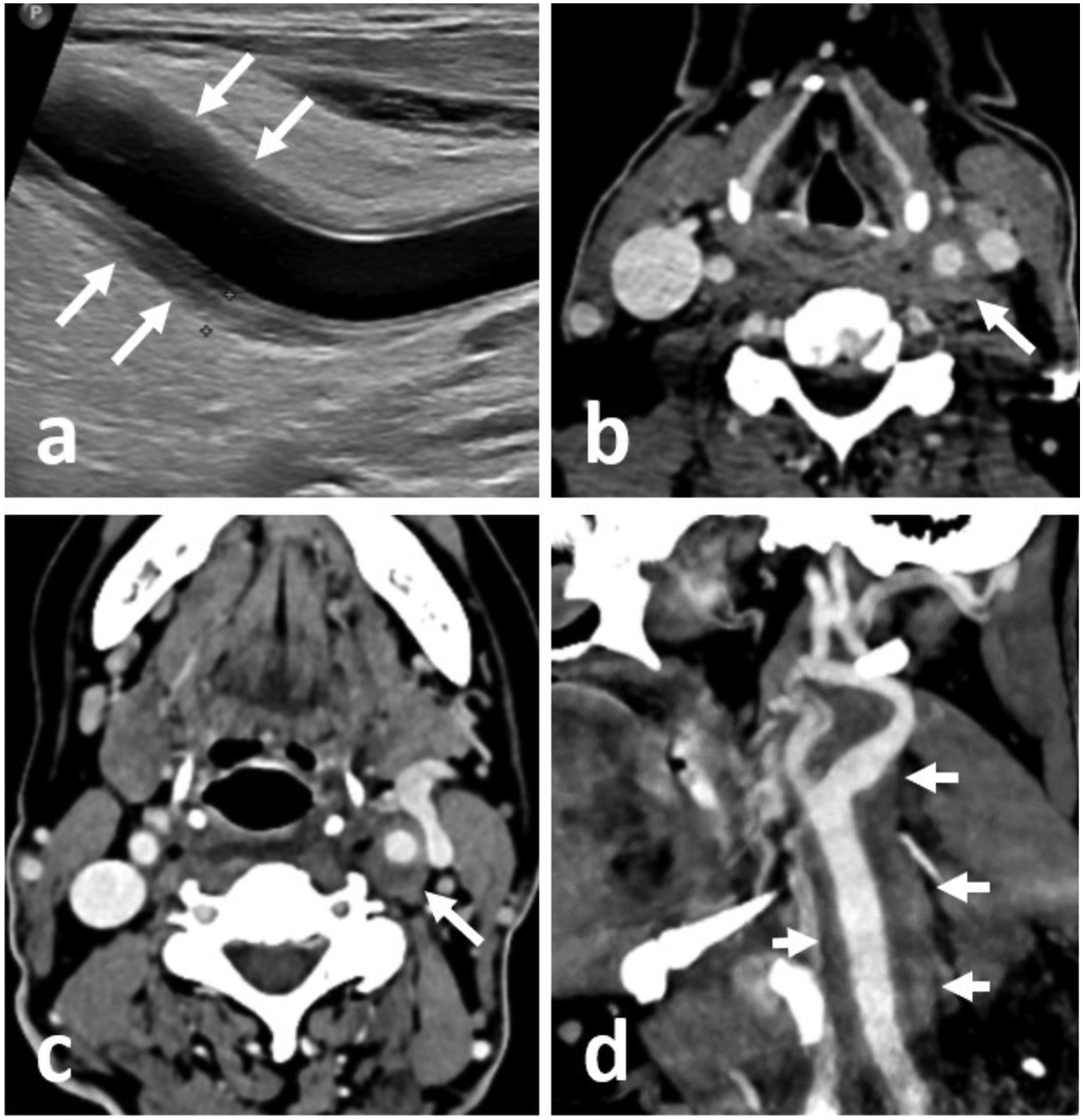
Discussion
Maggialetti et al. 2 proposed four diagnostic criteria of TIPIC syndrome: acute ipsilateral radiating or non-radiating neck pain, perivascular soft tissue infiltration, exclusion of other causes of neck pain, and improvement within 2 weeks with or without anti-inflammatory drugs. Additionally, a minor criterion of intimal soft plaque was also proposed which may be formed secondary to the healing of the inflammation. 4 There may be involvement of common carotid artery, internal carotid artery, or both.2,4,6 Unilateral involvement is more common than bilateral. Eccentric involvement at carotid bifurcation is a common pattern.2,4 Restriction on diffusion-weighted imaging and enhancement on post-contrast imaging are also commonly seen.2,7 Mild luminal stenosis may be seen in a few cases. Histopathologically, Upton et al. confirmed non-specific inflammation in the involved vessel wall. 8 Erythrocyte sedimentation rate, C- reactive proteins, Serum Amyloid A protein, and D-dimer may be raised. Resolution with anti-inflammatory treatment (Non-steroidal anti-inflammatory drugs or steroids) is seen within a median period of 13 days.
Various etiological factors and diseases have been found to be associated with TIPIC syndrome. Inflammation of the laryngopharynx, cervical lymphadenopathy, high altitude exposure, malignancies, autoimmune diseases like Systemic lupus erythematosus, Rheumatoid arthritis, Sjogren’s syndrome, and Graves disease are known to be associated. 4 Sena et al. 6 reported perivascular thickening around common carotid artery in a case of polycythemia vera who subsequently developed leukemia, postulating this entity as paraneoplastic arteritis.
Myelodysplastic syndrome is a clonal stem cell disorder, commonly seen in the older population which causes dysplastic hematopoiesis leading to cytopenia. Cases with chromosome 7 abnormalities have a poor prognosis. 9 Potential pathophysiological mechanisms of the development of TIPIC syndrome in myelodysplastic syndrome can be autoimmune paraneoplastic arteritis or immunosuppression.4,10 Immunosuppression may be a contributory factor for the development of perivascular inflammation. Our case suggests that the patients with TIPIC syndrome may undergo further evaluation to rule out malignancy or immunosuppression to reach the possible underlying diagnosis which can play a greater role in timely management. Further large-scale studies as well as histopathological studies are warranted in this regard.
Footnotes
Contribution of authors
NC: Concept and design, patient management, manuscript preparation, data collection, literature review. VG: Patient management, data collection, literature review, manuscript preparation, manuscript review, supervision. PM: Patient management, manuscript review. MB: Manuscript review, supervision.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
