Abstract
Objective
Autophagy was reported to be essential for maintaining chondrocyte function, and reduced autophagy leads to osteoarthritis (OA). Previous studies showed involvement of heat shock stress in the control of autophagy in cells. This study sought to investigate the effect of hyperthermia on the expression of autophagy-related proteins in articular cartilage and the progression of naturally occurring OA in Hartley guinea pigs.
Design
Radiofrequency pulses of 13.56 MHz were applied to the animals’ knees for 20 minutes to induce hyperthermia. The knee joints were resected at 8 hours, 24 hours, 72 hours, 7 days, and 6 months after hyperthermia. Serial sections of knees were examined for histopathological changes. The expression levels of Unc-51-like kinase 1 (ULK1) and Beclin1 were analyzed by immunohistochemistry.
Results
Analysis of the distribution of positive cells showed that, in cases of moderate OA, ULK1 and Beclin1 expression levels were significantly decreased in the superficial zone (SZ) and middle zone (MZ) (P < 0.01) compared with normal cartilage. Seven days after exposure to radiofrequency waves, expression levels of ULK1 and Beclin1 were augmented in the SZ in animals with mild OA. The severity of cartilage degradation was significantly reduced (P < 0.01) in the radiofrequency-treated knees versus the untreated knees.
Conclusions
This study showed that heat stimulation enhanced autophagy in healthy knee chondrocytes and chondrocytes in knees with mild OA. The study also showed that long-term periodic application of hyperthermia suppresses aging-related progression of OA. The activation of autophagy by radiofrequency hyperthermia may be an effective therapeutic approach for osteoarthritis.
Introduction
Knee osteoarthritis (OA) is a joint disease that is most frequently encountered in clinical practice, and the pathogenesis involves various factors such as mechanics, genetics, and aging. Because the disease originates in articular cartilage, it is important to maintain the health of articular cartilage at the cellular level to prevent and treat OA, specifically, maintaining the health of chondrocytes that are responsible for metabolism.
Recent studies revealed that autophagy, the basic homeostatic mechanism in eukaryotes, 1 plays an extremely important role in cellular apoptosis and that autophagic malfunction results in cell death. 2 Autophagy is induced by stress such as reactive oxygen species and nutrient starvation and it then degrades degenerated proteins and cellular organelles to generate components or energy essential for the survival of the cells. Compared with proteosomal degradation, which is specific to proteins, lysosomal degradation is complicated and handles various substances as substrate. The mechanism underlying the transportation of substrates to the lysosome is called autophagy. 3 Because of its association with aging, autophagy can be a target of preventive or treatment drugs for diseases that develop or progress with aging. 4 In a study using humans and other animals with OA, a functional decline in autophagy was observed in the superficial layer of the articular cartilage, 5 and a study is currently underway to develop a preventive drug for OA that activates autophagy in articular cartilage. 6
In animals, heat stimulation of articular cartilage suppressed the progression of OA, 7 presumably because heat stimulation upregulates the production of heat shock proteins (HSPs), a group of proteins that protect cells from environmental stress. HSP70, which is induced in a large quantity and represents HSP, has been shown to inhibit the apoptosis of chondrocytes. 8 At the same time, an increasing number of studies have reported the involvement of heat shock stress in the control of autophagy in different cells. Heat exposure triggered autophagy in a human hepatoma cell line, 9 rat cardiomyocytes, human alveolar basal epithelial cells, 10 a mouse spermatocyte cell line, 11 and human cervical cancer cells. 12 These findings suggest that heat shock stress induces HSP in articular cartilage and suppresses the progression of OA through the activation of autophagy. In this study, we therefore investigated the effect of hyperthermia on the expression of autophagy in articular cartilage and the progression of OA in Hartley guinea pigs with naturally occurring OA.
Methods
This study was conducted according to protocols approved by the local Animal Care Ethics Committee at Nippon Medical School, Tokyo, Japan.
Animals
Three-month-old female Hartley guinea pigs, the spontaneous aging-related OA model, were purchased from Sankyo Labo Service Co. (Tokyo, Japan). Animals were housed in cages, maintained in a room under controlled conditions at 24°C with 12-hour lighting, and given free access to food and water. Following hyperthermia or without treatment, animals at ages 5, 9, and 18 months were euthanized with intraperitoneal injections of a lethal dose of sodium pentobarbital (Somnopentyl; Kyoritsu Seiyaku, Tokyo, Japan) ( Fig. 1 ).
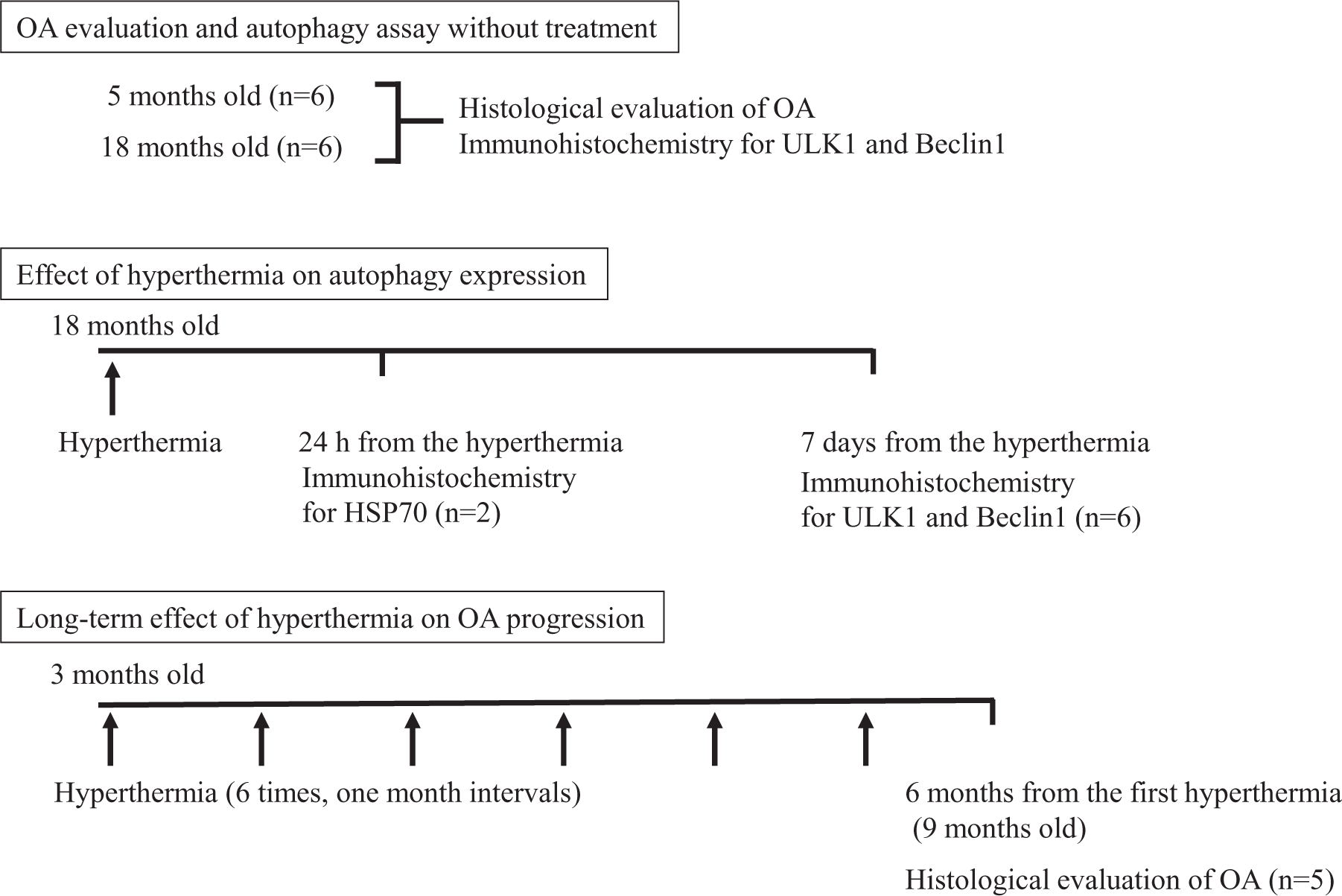
Schema of the experiment. The number and age of animals used in each experiment are shown.
Hyperthermia Using Radiofrequency Waves
A Thermotron-RF-300 (Yamamoto Vinita, Co. Ltd, Osaka, Japan), which can generate a 13.56-MHz radiofrequency pulse to heat the animals’ knees, was used to induce hyperthermia. The knee was tightly sandwiched by skin-contact bipolar applicators at the center of the internal and external condyle of the femurs. Hyperthermia of the right knees was induced using a radiofrequency wave of 10 W for 20 minutes under anesthesia with intraperitoneal injections of sodium pentobarbital (30 mg/kg body weight). A sterilized thermocouple was inserted from the lateral side between the patella and femur to measure the temperature changes inside the knee joint caused by diathermy. The left knees were used as controls.
Tissue Preparation
The bilateral knee joints were resected at 24 hours, at 7 days, and at 6 months after hyperthermia, (1 month after the last induction of hyperthermia), fixed in 4% paraformaldehyde for 1 day, decalcified in ethylenediamine tetraacetic acid (pH 7.0) for 3 days, then embedded in paraffin. Serial sagittal sections (4 μm thick) were cut, stained with safranin O–fast green and examined for histopathological changes. Immunohistochemical staining was also performed.
Immunohistochemistry
The expression levels of Unc-51-like kinase 1 (ULK1), an inducer of autophagy; Beclin1, a regulator of autophagy; and HSP70 were analyzed by immunohistochemistry. Paraffin-embedded samples were first deparaffinized in xylene and rehydrated in graded ethanol and water. For antigen unmasking, sections in 10 mM sodium citrate buffer (pH 6.0) were heated in a microwave oven and kept at 80°C to 85°C for 10 minutes. Slides were cooled for 20 minutes at room temperature after antigen unmasking. After washing with Tris-buffered saline (TBS), sections were treated with 3% H2O2/TBS, and blocked with 10% rabbit serum for 20 minutes at room temperature. The following steps were performed. Antibodies to ULK1 (1:100 dilution), Beclin1 (1:200 dilution), and HSP70 (1:500 dilution) (Santa Cruz Biotechnology) as well as negative control IgG (1 µg/mL) were applied and sections were incubated overnight at 4°C. After washing with TBS, sections were treated with 3% H2O2 for 10 minutes, washed with TBS, incubated with biotinylated goat anti-rabbit secondary antibody (Millipore) for 30 minutes at room temperature, and then incubated for 30 minutes using the Liquid DAB + Substrate Chromogen System (Dako, Hamburg, Germany). Slides were washed, and sections were incubated with 3,3′-diaminobenzidine (DAB) substrate for 3 to 10 minutes.
Quantification and Localization of Positive Cells in Cartilage
ULK1 and Beclin1 localization in each cartilage zone was assessed systematically by counting positive cells in the superficial zone (SZ) and middle zone (MZ). Three pictures were taken under 40× magnification, showing the weightbearing area of the medial tibial plateau. Then, the number of ULK1- and Beclin1-positive cells was counted in each section and expressed as the percentage relative to the total number of cells counted in each zone. This was repeated a minimum of 3 times for each section. The identification of each zone was based on cell shape, morphology, orientation, and pericellular matrix deposition. The depth of each zone was recorded for each section for comparative analysis of the frequency of positive cells in each zone.
Histological Severity of Osteoarthritis
In the central medial tibial plateau stained with safranin O–fast green, areas showing maximal pathology were examined. Semiquantitative histopathological grading was performed based on a modified Mankin scale 13 as follows: 0, normal cartilage; 1-5, mild OA cartilage; >6, OA cartilage.
Statistical Analysis
Statistically significant differences between the 2 groups were determined with t-tests. P values <.05 were considered significant. All statistical analyses were performed using StatMate V (ATMS Co. Ltd, Tokyo, Japan).
Results
Spontaneous Osteoarthritis
Because the progression of OA is influenced by the rearing environment, we used a semiquantitative histochemical-histologic scoring system to evaluate the aging-related severity of knee OA in untreated guinea pigs. 13 In 5-month-old guinea pigs (n = 6; body weight, 580-625 g), histological severity was 1.17 ± 0.75, and the cartilage surface was smooth and was stained well with safranin O. On the other hand, 18-month-old guinea pigs (n = 6; body weight, 1050-1255 g) had a histologic severity score of 7.12 ± 1.72, and fibrillation was observed on the cartilage surface. In addition, safranin O staining was decreased in the middle layer. These findings indicate a significant correlation between aging and the progression of disease severity (P < 0.001) ( Fig. 2A ). However, even among the 18-month-old animals, most of the articular cartilage structure was maintained, with no lesions involving fissures reaching the deep layer of the cartilage ( Fig. 2B ).
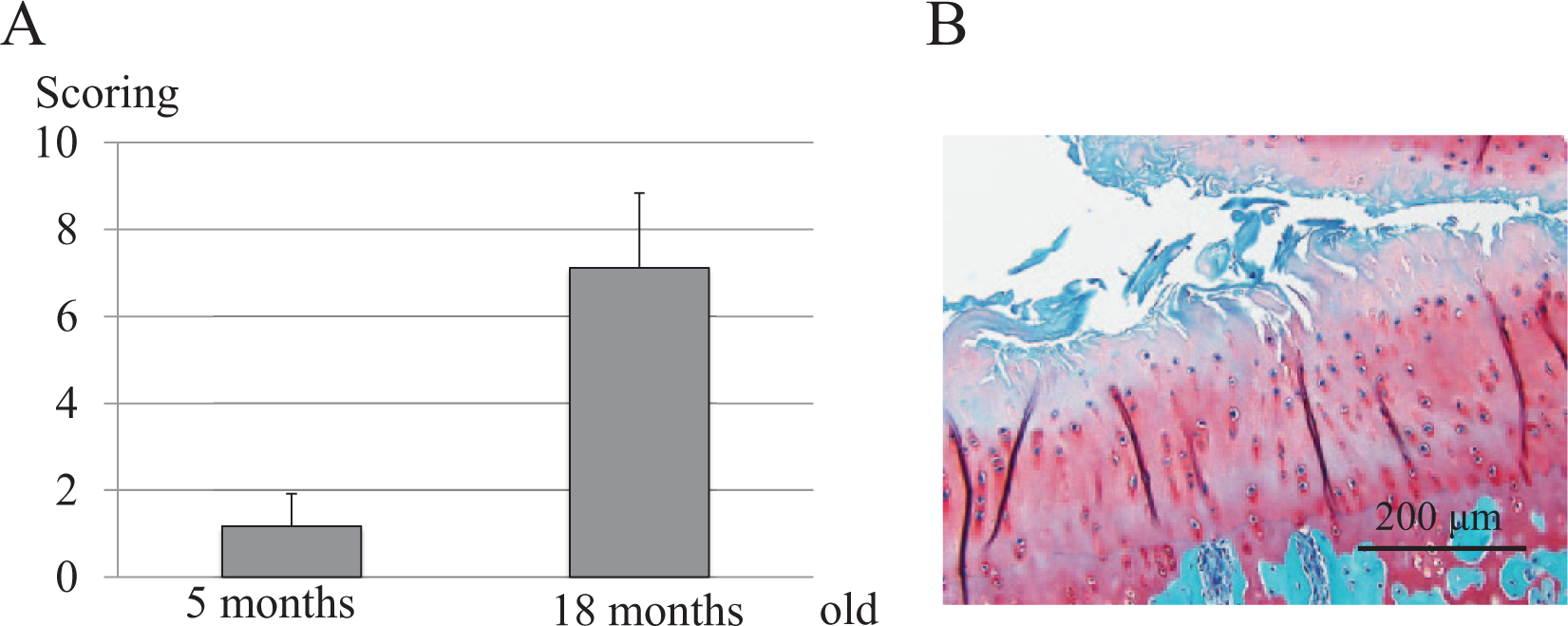
Development of spontaneous histological osteoarthritis (OA) in Hartley guinea pigs. (
Aging- and Osteoarthritis-Related Suppression of Autophagy
To reveal how aging and OA changes the expression of autophagy-related proteins in chondrocytes, the expression of ULK1, an inducer of autophagy, and Beclin1, a regulator of autophagy, was immunohistologically investigated. In healthy 5-month-old animals, cells positive for ULK1 and Beclin1 were abundant in the superficial and middle layers of the cartilage ( Fig. 3 ). Quantitative analysis of the distribution of positive cells revealed that the percentage of ULK1- and Beclin1-positive cells in healthy cartilage of 5-month-old animals (modified Mankin scale, 0) was approximately 70%, with more positive cells in the superficial zone than in the middle zone. Compared with these healthy cartilages, the percentage of cells positive for ULK1 and Beclin1 in the superficial and middle zones was significantly lower in cartilages with mild OA (modified Mankin scale, 1-5). In healthy cartilages in 18-month-old animals, ≤20% of the superficial zone cells were positive for the proteins, and the number of cells in both zones was significantly lower compared with cartilages of 5-month-old animals. Furthermore, almost no positive cells were observed in cartilages with mild OA and OA (modified Mankin scale, ≥6) ( Fig. 4 ). These findings show that the number of cells expressing autophagy-related proteins in chondrocytes decreases because of aging or OA regardless of aging.
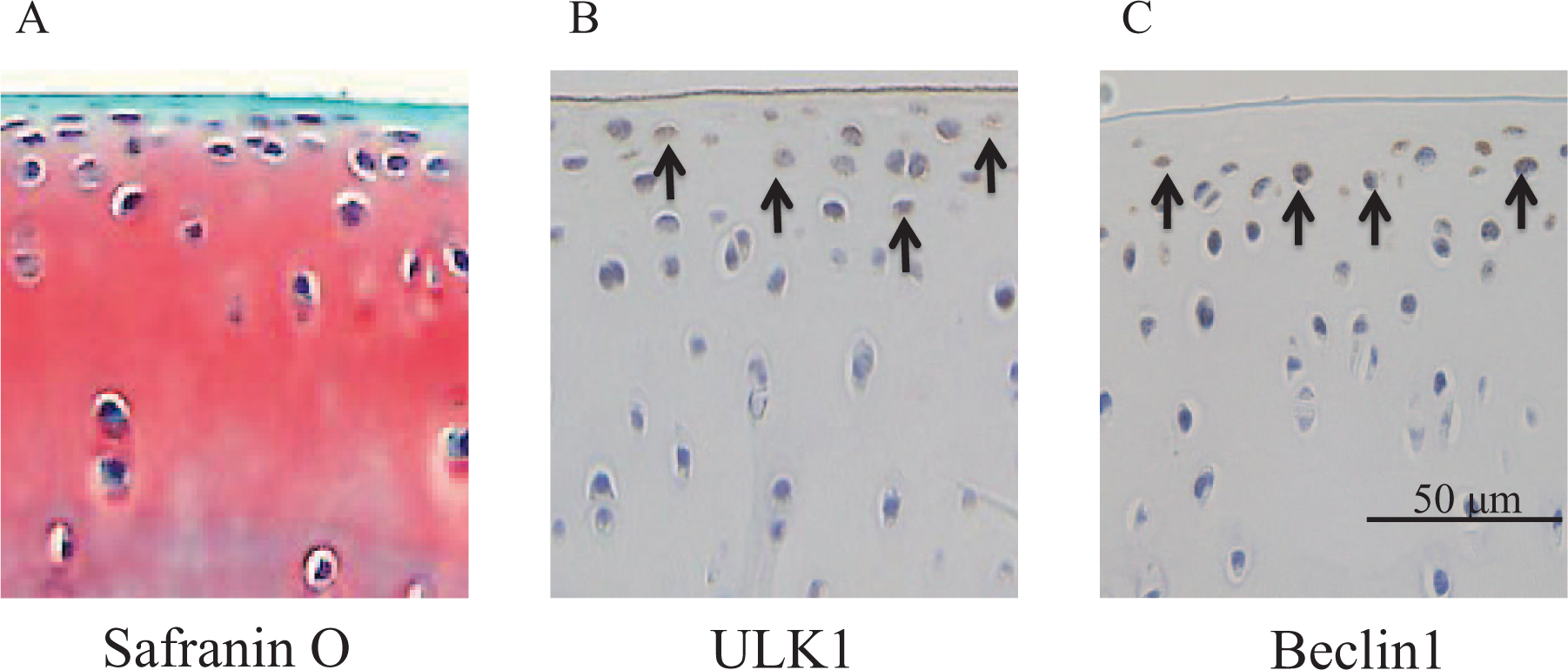
Unc-51-like kinase 1 (ULK1), and Beclin1 expression in normal cartilage. (
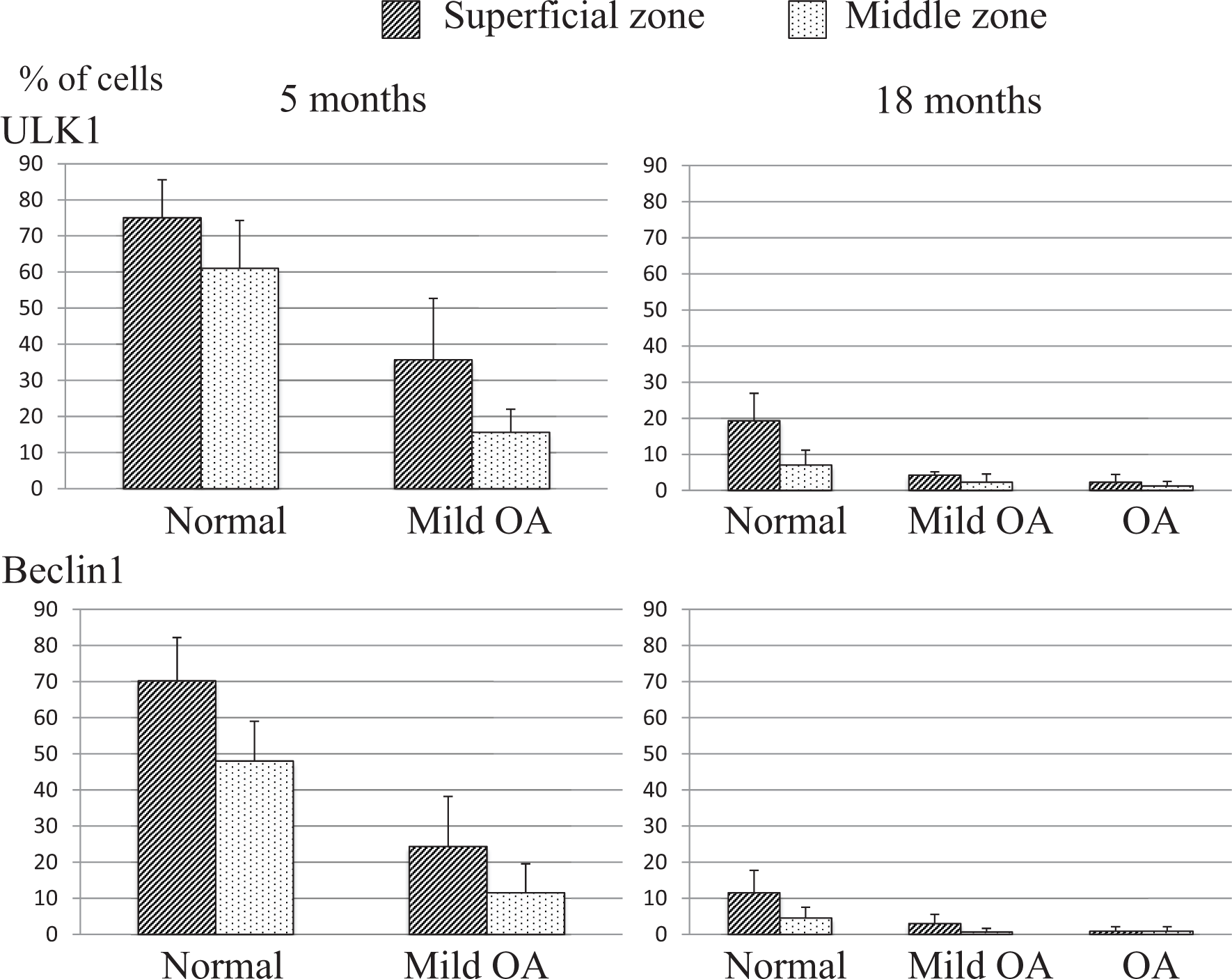
Aging-related decrease of autophagy. Quantification of ULK1- and Beclin1-positive cells in normal and mild osteoarthritis (OA) cartilage in 5-month-old animals, and in normal, mild OA, and OA cartilage in 18-month-old animals was performed. In mild OA of 5-month-old animals, the percentage of ULK1- and Beclin1-positive cells was significantly reduced in the superficial zone (SZ) and middle zone (MZ) compared with those in normal cartilage. In cartilage of 18-month-old animals, ULK1 and Beclin1 expression was significantly reduced in the superficial zone and middle zone compared with those in cartilage of 5-month-old animals.
Changes in Intra-articular Temperature and Expression of HSP70 after Radiofrequency Ablation
Hyperthermia-related change in intraarticular temperature measured using a thermocouple revealed that the temperature increased from 32.5°C to 40°C in about 6 minutes, was maintained at 40°C for 14 minutes, and then returned to the original temperature in about 3 minutes after the termination of radiofrequency ablation ( Fig. 5A ). In the present hyperthermia model, it was possible to maintain the intraarticular temperature at around 40°C for more than 10 minutes. The tissue was collected 24 hours after the induction of hyperthermia for the immunohistological study of HSP70. The results showed that HSP70-positive cells were significantly increased in all the layers of the articular cartilage ( Fig. 5B ).
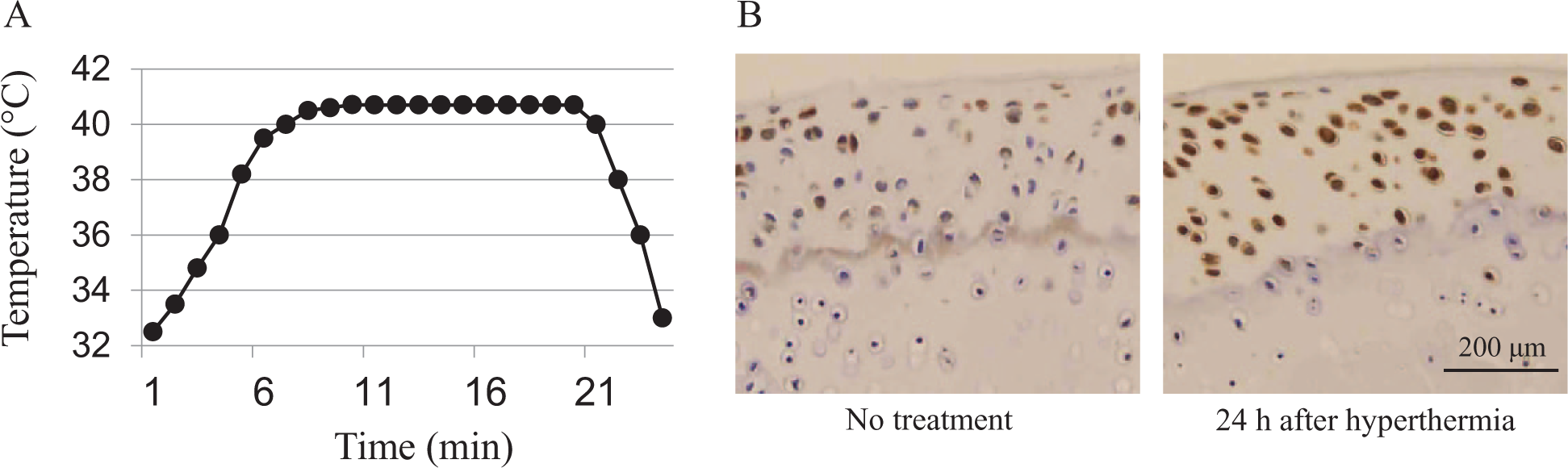
Change of temperature inside the joint and enhancement of HSP70 expression. (
Effect of Radiofrequency Ablation on Autophagy
Figure 6 shows the immunohistological findings of autophagy-positive cells at 7 days after heat stimulation of the knee in 18-month-old guinea pigs. Compared with the age-matched unstimulated controls, a significant increase in the expression of ULK1 and Beclin1 was observed in chondrocytes in the superficial and middle zones in healthy animals and animals with mild OA. In healthy cartilage, the prevalence of ULK1-positive cells in the superficial and middle zone was increased 2.5- and 6-fold, and that of Beclin1-positive cells was increased 5- and 6-fold, respectively. Although not as large as in healthy cartilage, the fractions of ULK1- and Beclin1-positive cells were also increased in mild OA cartilage. Autophagy-positive cells were seldom detected in OA cartilage even after the induction of hyperthermia.
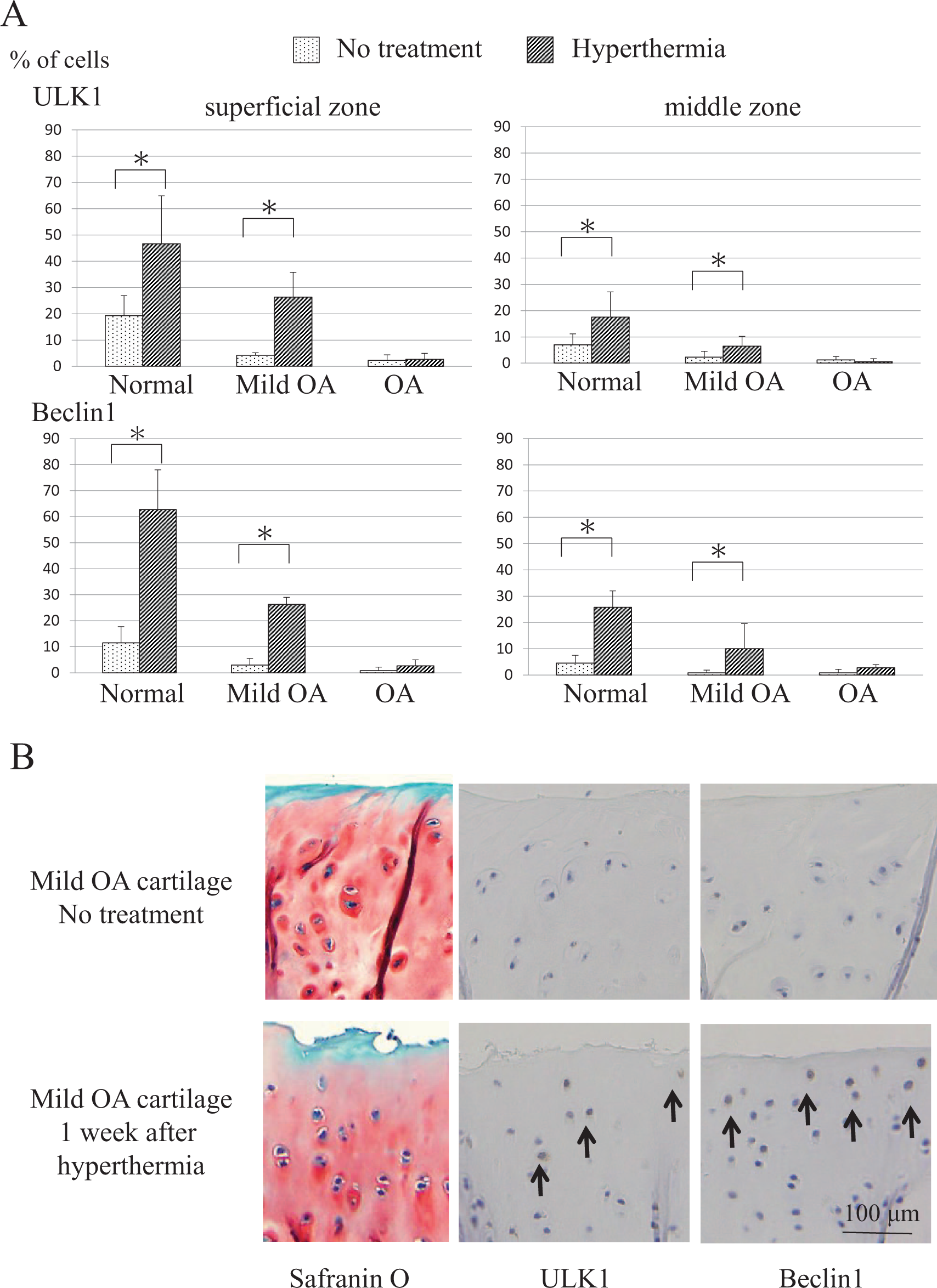
Effect of hyperthermia on autophagy. (
Effect of Radiofrequency Ablation on the Progression of Osteoarthritis
Hyperthermia was induced once a month up to 6 times in the knee of 5-month-old guinea pigs (n = 5), and the knee articular cartilage was collected 1 month after the last heat stimulation (6 months after the first induction of hyperthermia) for comparison with untreated controls (n = 5). Semiquantitative histopathological grading showed that while the histologic score was 4.83 ± 0.79 in control knees, the score was 3.17 ± 0.30 in the heat-stimulated knees, with a significant reduction in the severity of OA in the latter (P < 0.05) ( Fig. 7 ). No adverse events due to hyperthermia were observed.
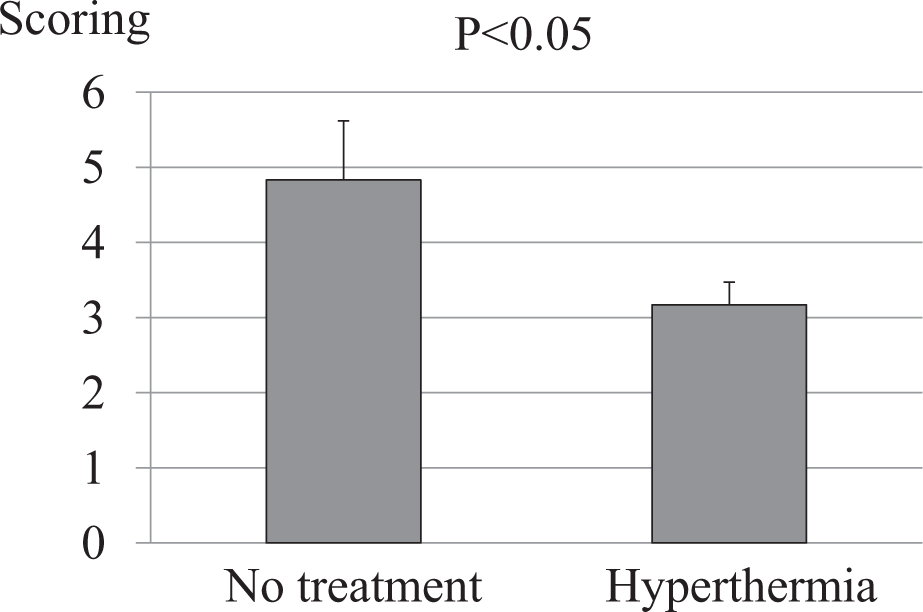
Effect of hyperthermia on osteoarthritis (OA) development in guinea pigs. Semiquantitative histopathological grading (modified Mankin scale) for untreated control knees (no treatment) (n = 5) and knees treated with hyperthermia 6 times in 6 months (n = 5) are shown. P < 0.05, control versus hyperthermia.
Discussion
Autophagy plays an important role in the homeostatic maintenance of healthy knee chondrocytes, and therefore, autophagy-related proteins such as Beclin-1 are expressed at high levels in the superficial chondrocytes. 14 In early OA, Beclin-1 mRNA was upregulated in the cartilage because catabolic stress enhances autophagy. 15 However, in another study, autophagy was reduced in the cartilage that underwent aging-related degeneration. 16 Also in the present study, an aging-related reduction in proteins involved in autophagy was observed in the knee cartilage of guinea pigs with naturally occurring OA, which is histologically similar to humans. Furthermore, the downregulation of autophagy was observed in the cartilage of same-age animals due to the progression of OA.
Because the augmentation of autophagy appears to benefit the treatment of OA or prevent disease progression, research is currently underway to suppress mTOR, the negative regulator of autophagy. 17 Autophagy can be activated by administering drugs or by changing the cellular environment. 18 In our study, we focused on the effect of hyperthermia, a treatment modality for OA in daily clinical practice, on the expression of autophagy-related proteins, revealing that heat stimulation enhanced autophagy in healthy knee chondrocytes and those in knees with mild OA. When stimulated by heat, cells induce a group of HSPs that protect cells from environmental stress. HSP70, which is expressed in the largest amount among known HSPs and are a family of HSP, was shown to suppress apoptosis in chondrocytes. 8 A previous study has shown that the pre-treatment of mesenchymal stem cells with heat stress suppressed apoptosis induced by oxidation stress through the activation of autophagy by suppressing mTOR. 19 Therefore, the cytoprotective actions of heat may be applied to treat degenerative diseases or prevent their progression.
This study also showed that the long-term periodic application of hyperthermia suppresses the aging-related progression of OA. We are interested in basic research findings on the response of articular cartilage in knee OA to long-term heat stimulus without mechanical stress. Hojo et al. 20 reported that in cultured cells, proteoglycan metabolism in chondrocytes increased when heated to 39°C or 41°C, but decreased at 43°C. Also in humans, heat stimulation at 40°C upregulated the expression of proteoglycans in the cartilage through the mechanism involving the accumulation of HSP70 in chondrocytes. In a study using rabbits, the use of 2.45-GHz microwave irradiation, which is used commonly in clinical practice, to increase the intraarticular temperature in the knee to around 40°C strongly enhanced the expression of proteoglycan and type II collagen in the articular cartilage. 21 Similarly, a significant increase in proteoglycan expression was observed in rat knees when the intraarticular temperature was increased to 40°C by microwave irradiation. Furthermore, the intra-articular administration of glutamine, which enhances the expression of HSP70, upregulated the expression of HSP70 and proteoglycan. 22 However, the expression of proteoglycan was not enhanced when the expression of HSP70 was suppressed by the inhibitors, showing that in small animals, heat stimulation of the knee joint at 40°C activates the metabolism of matrix proteins in the cartilage partly through the upregulation of HSP70. In addition, the progression of OA was suppressed after the heat stimulation of the knee in the rat model of OA involving anterior cruciate ligament transection. 7 HSP and autophagy protect cells cooperatively through crosstalk at both ends of homeostasis, that is, anabolism and catabolism, respectively. A report of the involvement of the HSP transcription factor HSF in the suppression of autophagy 23 suggests that chronological changes in the activation of autophagy by heat stimulation are complicated.
In this study, heat stimulation was performed at 13.56-MHz radiofrequency by placing the bipolar applicator on the medial and lateral sides of the knee. Noncontact-type monopolar applicators may be effective in the microwave diathermy of small animals, but in humans, the heat can travel only a few centimeters deep in the superficial layer, not through the entire articular cartilage. In contrast, bipolar radiofrequency applicators can heat deep inside the articular cartilage. 24 In addition, thermotherapy with radiofrequency hyperthermia improves clinical symptoms more than microwave diathermy. 25 The Hartley guinea pig spontaneously develops OA similar to that of human OA in the knee joint; thus, it is used as an aging-related OA model. Although small animals were used in this study, we plan to use the same radiofrequency hyperthermia technique to treat OA in future clinical studies.
There are several limitations in this study. First, no preliminary study was performed to elucidate the optimum frequency and duration of thermotherapy. To reveal the effect of long-term thermotherapy on the progression of OA, we performed hyperthermia in guinea pigs under general anesthesia once a month to minimize the invasiveness. Therefore, we plan to investigate whether the progression of OA is affected by the frequency of hyperthermia in the future. Second, this study did not elucidate the effective duration of thermotherapy. We evaluated the effect of hyperthermia histopathologically 1 month after the last session of hyperthermia. As in the first limitation, it is unclear how long the hyperthermia-induced activation of autophagy and suppression of OA progression last after the termination of final heat stimulation.
Footnotes
Authors’ Note
This study was conducted at Nippon Medical School, Tokyo, Japan.
Acknowledgments and Funding
The authors thank Mr. Tsuneo Takasugi (Yamamoto Vinita, Co. Ltd, Osaka, Japan) for his kind advice on the use of the Thermotron-RF-300. This research was supported by a Grant-in-Aid for Scientific Research from the Ministry of Education, Culture, Sports, Science and Technology, Japan (23590723).
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Approval
Ethical approval for this study was obtained from Nippon Medical School Animal Care Committee (ref,No.23-160, 24-121, 25-080).
Animal Welfare
The present study followed international, national, and/or institutional guidelines for humane animal treatment and complied with relevant legislation.
