Abstract
School communities are not immune to the alarming increase in opioid-related deaths occurring in the United States during the past decade. The purpose of this article is to share how a middle school in New York State, beginning in the late fall of 2022, successfully implemented a program to reduce the likelihood of opioid overdose deaths in their building through expansion of the accessibility of and education and training in use of naloxone, an opioid antagonist. The program is applicable for all K-12 campuses and follows the Model of Greater Awareness, Improved Training, and Increased Availability of and Accessibility to Intervention Devices, based on the steps successfully used for out-of-hospital cardiac arrest emergencies. Because opioid addiction does not discriminate, it is confidently projected that these targeted actions will proactively and positively reduce the likelihood of opioid overdose deaths in our school setting, including for students, faculty, staff, administrators, and visitors, when and should they occur.
Automated external defibrillators (AEDs) are ubiquitous in many of our communities, including public and private settings. There are likely few individuals unfamiliar with the device’s signage featuring prominent AED letters and a red heart and lightning bolt image (Figure 1) indicating the location of this life-saving emergency equipment and its rectangular storage cabinet (Figure 2). According to the National Heart, Lung, and Blood Institute (2023), out-of-hospital cardiac arrests (OHCAs) account for about 350,000 deaths each year in the United States. The current survival rate for OHCA is about 10%, double the percentage from the year 2000 (Brooks et al., 2022). Important contributors to this improvement in survival rate include
improved CPR education with expanded training offerings and
an increase in the availability of and access to AEDs (Brooks et al., 2022).

Common Signage Used in the Pierre Van Cortlandt Middle School Indicating an AED’s Location

A Common Automated External Defibrillators (AED) Storage Cabinet in the Pierre Van Cortlandt Middle School
Background Information
A current and significant cause of unintentional deaths in the United States is opioid-related drug overdoses (see Figure 3; National Institute on Drug Abuse, 2023). However, unlike OHCAs, Figure 3 shows that opioid overdose deaths continue to rise year-to-year, with the rate having an inflection point to a steeper, positive slope around 2013–2014. According to the National Institute on Drug Abuse (2023), in 2021, over 106,500 deaths were associated with illicit or prescription drugs. Of these deaths, greater than 80,000 (75%) deaths were related to opioids. In particular, Friedman et al. (2022) report an exponential rise in adolescent overdose deaths since 2019, and these deaths are largely associated with opioid-type compounds. Due simply to the sheer number of lives lost each year, it is likely that many individuals across the United States know directly or indirectly (e.g., only by a few degrees of separation) someone that has experienced a loss associated with an opioid overdose.
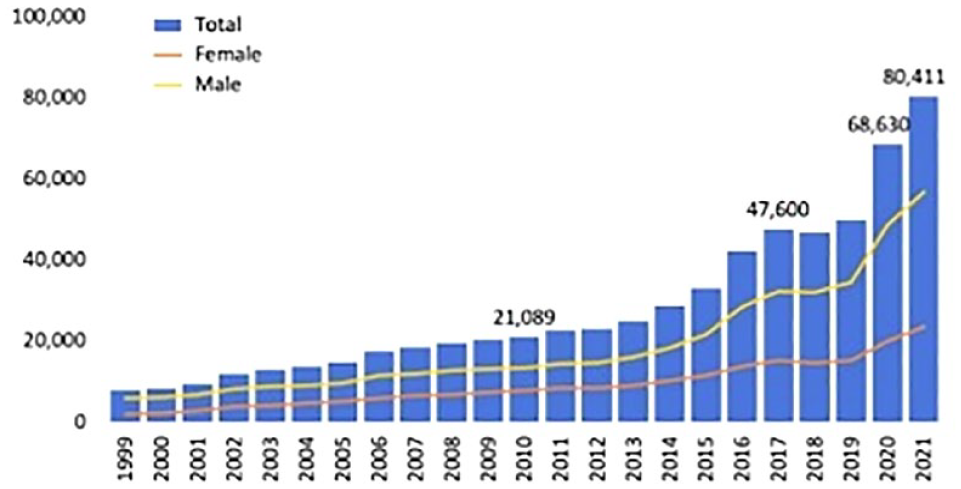
National Overdose Deaths Involving Any Opioid
Similar to the reasons resulting in improved OHCA outcomes (increased awareness; education and training leading to higher quality CPR delivery; and enhanced access to and use of AEDs), comparable tools exist to address opioid overdoses. These tools include greater awareness, education, and training about and improved availability, accessibility, and the use of the opioid antagonist naloxone—tools, the authors collectively call the Model of Greater Awareness, Improved Training, and Increased Availability of and Accessibility to Intervention Devices. Although an action plan for increasing awareness of education regarding opioid overdose treatment was available (Readiness and Emergency Management for Schools, n.d.), a key enabling and differentiating element of our school’s model is the inclusion of naloxone, with its recent availability as an over-the-counter (OTC) medication in a non-prescription form known as NARCAN®. More specifically, the U.S. Food and Drug Administration (FDA, 2023) approved NARCAN® 4-mg nasal spray for OTC use on March 29, 2023. With the OTC, non-prescription form of naloxone now available, the opioid antagonist has increased accessibility and, thus, can be more widely dispersed and strategically located. It is posited that this improved awareness, education, training, availability, and accessibility will result in quicker delivery and use of naloxone during emergencies, thereby improving opioid overdose outcomes.
Beginning in 2014, when naloxone was a prescription medication, the New York State Education Department (NYSED), Student Support Services, provided a guidance memo to school nurses regarding its use. The memo stated that “neither New York State Public Health Law §3309 nor the nurse’s scope of professional practice allow a school nurse or a licensed practical nurse under the direction of an RN, who has not been issued a patient-specific order by a physician, to administer an opioid antagonist” (NYSED, 2014, para. 3). The memo went on to say that a school nurse in possession of an opioid antagonist and already trained in its use may administer the medication in a life-and-death emergency to a student with a known or suspected overdose. School nurses were also advised to discuss this with their school’s administration.
More recently, in 2019, the New York State Department of Health (NYSDOH) et al. updated a guidance document in response to the FDA approval of intranasal spray delivery system of NARCAN® and to align with state-level approved training for non-medical school staff. The background information in this guidance explains that New York state law and the implementing regulations allow trained individuals to administer naloxone in an emergency to persons suspected of having an opioid overdose. It went on to explain that schools participating in this program may permit volunteer employees to be trained, as well as maintaining an adequate supply of opioid on site. Three options were outlined for schools implementing the program:
School/school district registers with the NYSDOH to operate an opioid overdose prevention program, as required by the school medical director.
School/school district allows school nurses to execute non-patient-specific orders and protocols for administering the opioid-related overdose treatment to students and staff in school.
The school/school district staff received training as a participant in a NYSDOH registered opioid overdose prevention program that is operated by another organization (2019).
In all three of these options, the guidelines specified that a valid non-patient-specific order and protocol issued by a licensed physician or advanced registered nurse practitioner was required for registered nurses (e.g., the school nurse) to administer naloxone. The guidelines speak to required and available training, along with which programs qualified for access to free supply of naloxone. Prior to implementation of the new opioid overdose model presented in this article, our school fell under the first program mentioned, with naloxone being stored in the school’s health office and the only employee trained in its use being the school nurse. At this time, we are not aware of any new specific state-level guidance and directions in response to the FDA announcement of OTC availability of naloxone.
This article’s thesis is grounded in the FDA’s March 29, 2023, ruling that increases the access and availability of naloxone by changing it from prescription to OTC and thereby reducing ambiguity and complexity of laws and regulations. However, we recognize that naloxone is still a drug, albeit now an OTC drug. Thus, through careful and diligent thought and with the support of our district’s medical director, we have developed a strategy to more widely distribute naloxone in our school (beyond the nurse’s office), by placing the opioid antagonist in secured, alarmed cabinets. By placing naloxone in secured, alarmed cabinets, not only did the opioid antagonist’s accessibility and availability improve but the likelihood of someone, for example, a student, gaining free access to is addressed and reduced.
Taking Action
The school nurse is commonly the only health care professional in the school setting. As identified in National Association of School Nurses (NASN, 2021) Framework for 21st Century School Nursing Practice™, health care leadership is a key principle of the professional school nurse’s role and responsibility. With a realization that opioid addiction and overdosing does not discriminate, the Pierre Van Cortlandt Middle School’s (PVC; Croton-on-Hudson, NY) Health Office professional nurse took a leadership position and created an evidence-based, implementable strategy to directly address and provide actions to improve the potential negative outcomes associated with opioid overdosing. This strategy, Figure 4, is grounded in the model we titled Greater Awareness, Improved Training and Increased Availability of and Accessibility to Intervention Devices, and when executed improves not only student safety and wellbeing but that of faculty, administrators, staff, and visitors while on the campus.
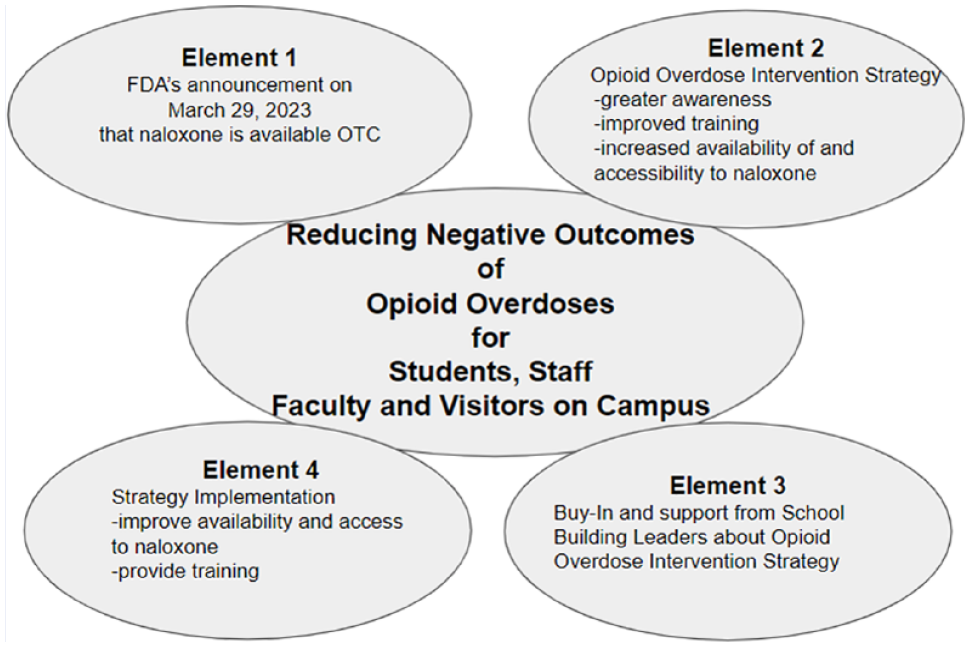
Key Elements of an Opioid Overdose Intervention Strategy
Key elements of the strategy are as follows:
(a) defining secure locations that increase and ensure improved availability of and access to naloxone; (b) offering volunteer training to faculty and staff, for example, through state or local health agencies or the school’s health professional, about opioid overdose events and naloxone delivery; and (c) scheduling future training sessions (e.g., annually).
Opioid antagonist supplies were made available, free of charge to PVC, through state and local governmental agencies, for example, Departments of Health and Boards of Cooperative Educational Services, and the PVC’s Health Office professional nurse provided naloxone-use training at a monthly faculty meeting. As a result of these activities, timelier opioid overdose intervention can occur when and should it happen on campus.
Regarding defining the secure location for placement of the naloxone, PVC selected each of its four AED cabinets that are strategically placed throughout the building. Since an opioid overdose is a medical emergency, storing naloxone in AED cabinets was a straightforward decision. This straightforward decision was buttressed by PVC’s AED storage cabinets being electronically monitored by an emergency management service. Thus, during the event of an opioid overdose event and a cabinet is opened to retrieve naloxone, 911 is automatically contacted, and emergency vehicles and responders are immediately dispatched. As part of the action plan, PVC also revised its AED signage to reflect an upgrade to the contents of all four of its emergency response cabinets. Figure 5 shows an example of new, additional signage, identifying the addition of naloxone.

Updated Signage in the Pierre Van Cortlandt Middle School Indicating the AED Cabinet Also Contains Two Doses (4 mg Each) of NARCAN®
Results
As a result of implementing this updated opioid intervention strategy, our school’s AED emergency storage cabinets now include two doses (4 mg each) of naloxone. As stated earlier, these emergency response cabinets are strategically located throughout the school, including the gymnasiums and food-service areas. Figures 6 and 7 show one of PVC’s actual storage cabinets containing an AED and two doses of naloxone, without a pouch and inside a pouch, respectively. As is easily discernable from the figures, adding naloxone to the existing AED storage areas is easily accomplished since the dimensions of a single box that contains two doses of the opioid antagonist is approximately 3.75 inches (height) × 3.00 inches (width) × 2.50 inches (depth; NARCAN® Direct, 2020). Alternatively, naloxone may be provided in a simple blister pack. Each blister pack, containing a single dose of naloxone (4 mg), is about 3.0 inches (height) × 2.5 inches (width) × 0.25 inches (depth; Figure 8).

Emergency Storage Cabinet in the Pierre Van Cortlandt Middle School Containing an Automated External Defibrillators (AED) and Two Individual Doses (4 mg Each) of NARCAN® Illustrating Their Easy Accommodation into the Space

Emergency Storage Cabinet in the Pierre Van Cortlandt Middle School Containing an Automated External Defibrillators (AED) and a Single Pouch With Two Doses (4 mg Each) of NARCAN® Illustrating Its Easy Accommodation in the Allocated Space

Two-Dimensional View, Approximately 2.5 Inches (Width) × 3.0 Inches (Height) of an Individual Dose (4 mg) of NARCAN®
Summary
In summary, using the model of Greater Awareness, Improved Training and Increased Availability of and Accessibility to Intervention Devices, we have increased the education opportunities about and leveraged the improved availability of and increased accessibility to naloxone by strategically placing the opioid antagonist in secured AED cabinets. This strategy proactively and positively reduces the potential for opioid overdose deaths for our students, faculty, administrators, staff, and visitors, when and should they occur. Furthermore, since an opioid overdose is a medical emergency, another advantage of locating naloxone in the AED cabinet is that the latter is electronically monitored by an emergency response team. Thus, upon opening the AED cabinet to gain access to naloxone, 911 is automatically contacted, and emergency vehicles and responders are immediately dispatched. To date, naloxone has yet to be administered to an individual on the PVC campus. Finally, it is anticipated that this project can serve as a model for other K-12 schools to follow.
Footnotes
Acknowledgements
The authors express their appreciation and gratitude to the manuscript’s reviewers and especially to Mrs. Cynthia Galemore, Editor, NASN School Nurse, for her guidance, support, and feedback.
Charles has been a practicing professional school nurse for about 10 years, most recently serving the Pierre Van Cortlandt Middle School since 2022. Charles is also an active FNP. He is the author of numerous health-care-related presentations and publications and a regional board member with NY State’s Nurse Practitioners Association.
Michael is the principal at Pierre Van Cortlandt Middle School in Croton-on-Hudson. Michael’s educational career spans three decades as a teacher and administrator. Michael received NY State’s Outstanding Assistant Principal of the Year Award in 2015. Michael is also an adjunct professor at Pace University’s School of Education.
Nicole is the assistant principal at Pierre Van Cortlandt Middle School in Croton-on-Hudson. Most recently, she was certificated in school management and leadership through Harvard Business School. Nicole’s educational career spaces two-plus decades as a teacher and most recently as an administrator. Nicole is currently the co-facilitator of the Regional Assistant Principal’s Forum.
