Abstract
Background:
Little is known about the adoption by athletic administrators (AAs) of exertional heat illness (EHI) policies, and the corresponding facilitators and barriers of such policies within high school athletics. This study describes the adoption of comprehensive EHI policies by high school AAs and explores factors influencing EHI policy adoption.
Hypothesis:
We hypothesized that <50% of AAs would report adoption of an EHI policy, and that the most common facilitator would be access to an athletic trainer (AT), whereas the most common barrier would be financial limitations.
Study Design:
Cross-sectional.
Level of Evidence:
Level 4.
Methods:
A total of 466 AAs (82.4% male; age, 48 ± 9 years) completed a validated online survey to assess EHI prevention and treatment policy adoption (11 components), as well as facilitators and barriers to policy implementation. Access to athletic training services was ascertained by matching the participants’ zip codes with the Athletic Training Locations and Services Project. Policy adoption, facilitators, and barriers data are presented as summary statistics (proportions, interquartile range (IQR)). A Welch t test evaluated the association between access to athletic training services and EHI policy adoption.
Results:
Of the AAs surveyed, 77.9% (n = 363) reported adopting a written EHI policy. The median of EHI policy components adopted was 5 (IQR = 1,7), with only 5.6% (n = 26) of AAs reporting adoption of all policy components. AAs who had access to an AT (P = 0.04) were more likely to adopt a greater number of EHI-related policies, compared with those without access to an AT. An AT employed at the school was the most frequently reported facilitator (36.9%).
Conclusion:
Most AAs reported having written EHI policy components, and access to an AT resulted in a more comprehensive policy.
Clinical Relevance:
Employment of an AT within high school athletics may serve as a vital component in facilitating the adoption of comprehensive EHI policies.
Exertional heat illness (EHI), specifically the emergent medical condition exertional heat stroke (EHS), remains a concern within high school athletics, where the absence of proper management and care can result in catastrophic outcomes.2-4 Evidence shows a significant reduction in the incidence of EHI with the implementation of policies,5,11 such as heat acclimatization and environment-based activity modifications. Policies surrounding the proper recognition (ie, accurate assessment of internal body temperature via rectal thermometry), treatment (ie, whole-body cold-water immersion [CWI]), and care (ie, cool first, transport second) are also supported based on previous literature demonstrating 100% survival when utilized. 6
Previous literature has shown that access to an appropriate healthcare provider within high school athletics serves as a facilitator to promote positive change and increases the likelihood of the development and adoption of comprehensive health and safety policies.10,15,23 Despite the presence of an athletic trainer (AT) being associated with a more comprehensive approach to health and safety within high school athletics, there remains a struggle to adopt EHI-specific health and safety policies. 25 Athletic administrators (AAs) such as athletic directors are a vital component of the sports medicine team and have been regarded as key persons to facilitate positive change for policies related to emergency action plans, lightning, and EHI.9,21,23,25
The AA’s oversight of the athletics program and their placement as a member of the broader sports medicine team allows them to provide valuable input, guidance, and support for the local adoption of health and safety policies. This is particularly true for high schools that do not have access to appropriate healthcare providers. 1 For the latter, the AA may be the sole person within the high school to adopt health and safety policies, which may increase the likelihood of health and safety policies being insufficient in comparison with current best practices.
To date, there has been a paucity in the literature examining the knowledge of AAs on topics related to adoption of health and safety policies and facilitators, and barriers related to adoption. Importantly, a policy adopted by a school may include some but not all the necessary components outlined in best practices. Thus, comprehensive (all components) policy adoption is imperative to improve patient outcomes. Previous research has been focused specifically on the adoption of emergency action plans,9,15,22 thus prompting the need for further inquiry into EHI. The purpose of this study was to describe the adoption of comprehensive EHI policies in place within United States (US) high schools by AAs. As a secondary aim, we sought to investigate the factors, facilitators, and barriers influencing the adoption of EHI health and safety policies in US high school athletic departments.
Methods
Using a cross-sectional design, AAs were surveyed via an online questionnaire (Qualtrics, LLC) on factors associated with EHI policies in their respective high schools. This study was ruled exempt from review by the University of Connecticut Institutional Review Board.
Participants
People classified as AAs for high school athletics programs in the US were invited to participate in this study. AAs’ contact information (email address, n = 6939) were acquired from publicly available websites (ie, state high school athletics associations and public high schools). Participant recruitment occurred during the 2018 to 2019 academic year. Participant responses were included in the final analysis if the following criteria were met: (1) participant identified as an AA, (2) participant was employed at a high school within the US, and (3) >80% of the questions from the survey were answered. Overall, 838 participants responded to the survey, 372 participants were removed from the final analysis for failing to meet the inclusion criteria; 466 participants were included in the data analysis, resulting in an overall response rate of 6.71%.
Questionnaire
With the guidance of current position and consensus statements, the questionnaire was developed by a content area expert, policy evaluation experts, and a clinical AT (30 years of high school clinical experience).3,4 After the development of the questionnaire, 4 high school AAs pilot tested the survey and provided feedback in areas of clarity, relevance, and importance. The final version of the questionnaire included the following sections: (1) demographics, (2) adoption of written EHI-related policies, (3) oversight and modification of written policies, and (4) facilitators and barriers to policy development. The precaution adoption process model (PAPM) was used to assess the AAs’ “readiness to act” for questions related to policy adoption. 28 The PAPM is used to predict behavior based on 8 stages ranging from the person being unaware there is an issue or a policy is needed to maintenance (ie, a school has a policy and is maintaining the policy; Table 1). 28 These questions allowed for AAs to select their current adoption (eg, (1) do you have a policy and (2) what are your thoughts related to having these policies) of a written policy at their school using Likert responses. For example, a participant may not be considering having this written policy or they may have had it for >6 months (see Table 1 for PAPM stage operational definitions). Participants were asked to report what had facilitated or were barriers to adopting (1) a comprehensive EHI prevention policy, (2) a policy for the use of rectal thermometry in the diagnosis of EHS, and (3) a policy for having a CWI tub setup.
Operational definitions of PAPM stages

PAPM, precaution adoption process model.
Access to Athletic Training Services
To ascertain an AA’s access to athletic training services, we utilized data from the Athletic Training Locations and Services (ATLAS) Project. 1 AAs provided the zip code of their high school, which was then matched with the data from the ATLAS Project to determine whether an AT was employed at the respective school during the data collection timeframe. Data were coded as athletic training services available, athletic training services not available, or unknown. Data were coded as unknown if the zip code had several high schools with varying access to athletic training services as it was uncertain which high school the AA’s response was specifically from.
Data Analysis
Both policy adoption and corresponding facilitators and barriers data (eg, dichotomized adoption, PAPM stages, components adopted) are summarized and presented as summary statistics (ie, proportions, mean, median, interquartile range (IQR) 25%-75%). A Welch t test was used to determine whether there were differences in adoption (yes/no) of an EHI prevention and treatment policy with participant age and number of students enrolled in the school, with the mean difference (MD) and 95% CI reported. The assumption of homogeneity of variances was violated, as assessed by Levene’s test for equality of variances (age, P = 0.02; students, P < 0.001) resulting in the use of the Welch t test rather than an independent-sample t test. Differences in the Welch t test results were presented as MD and 95% CI. A chi-square test for association (χ2) was conducted between adopting an EHI prevention and treatment policy and access to athletic training services, years in role (ie, AA) at the school, and whether the AA ever treated an EHI (yes/no) or an EHS (yes/no). A Mann-Whitney U test was used to determine whether there were differences in the number of components adopted between access to athletic training services, and whether the AA ever treated an EHI or an EHS. Statistical results were considered significant at P < 0.05 and analyses were performed in SPSS (Version 27, IBM Corp).
Results
A majority of the respondents to this survey were from Ohio (n = 63, 13.5%), California (n = 60, 12.9%), or New York (n = 51, 10.9%). Participants were on average 48 ± 9 years old with 1014 ± 870 students enrolled in the school. A majority (n = 383, 82.4%) of the AAs were male and had worked in the profession for >15 years (n = 358, 76.8%).
Adoption
The aggregate data showed 77.9% (n = 363) of AAs reported adopting a written policy for EHI prevention and treatment. The policy component with the highest adoption was “my school has written policies and procedures on modification of protective equipment” (80.2%, n = 243), whereas the component with the lowest adoption was “my school has written policies and procedures for use of a rectal temperature for diagnosis and evaluation of EHI” (Table 2; 14.6%, n = 108). The median number of components adopted overall was 5 (IQR = 1,7), with only 5.6% (n = 26) of AAs reporting adoption of all 11 components (Figure 1). The largest distribution across PAPM stages was in the adoption of a written policy for rectal temperature for the diagnosis and evaluation of EHI (Table 3; Unaware needed = 36.9%, Unaware if have = 11.0%, Decided not to act = 7.3%, Not considering = 24.3%, Considering = 5.3%, Decided to act = 0.7%, Acting = 2.0%, Maintaining = 12.6%).
Proportion of AAs reporting adoption of each of the written policy components
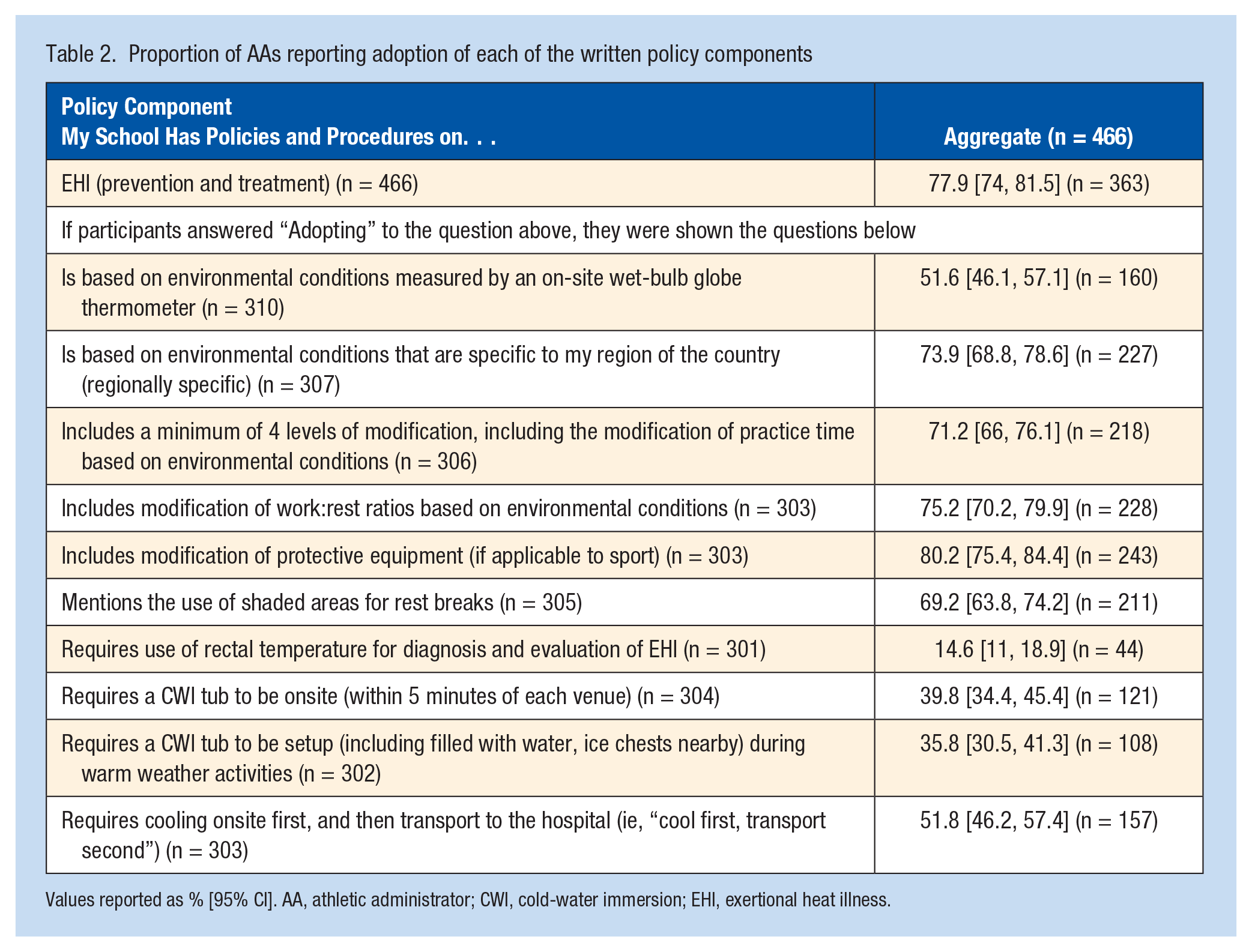
Values reported as % [95% CI]. AA, athletic administrator; CWI, cold-water immersion; EHI, exertional heat illness.
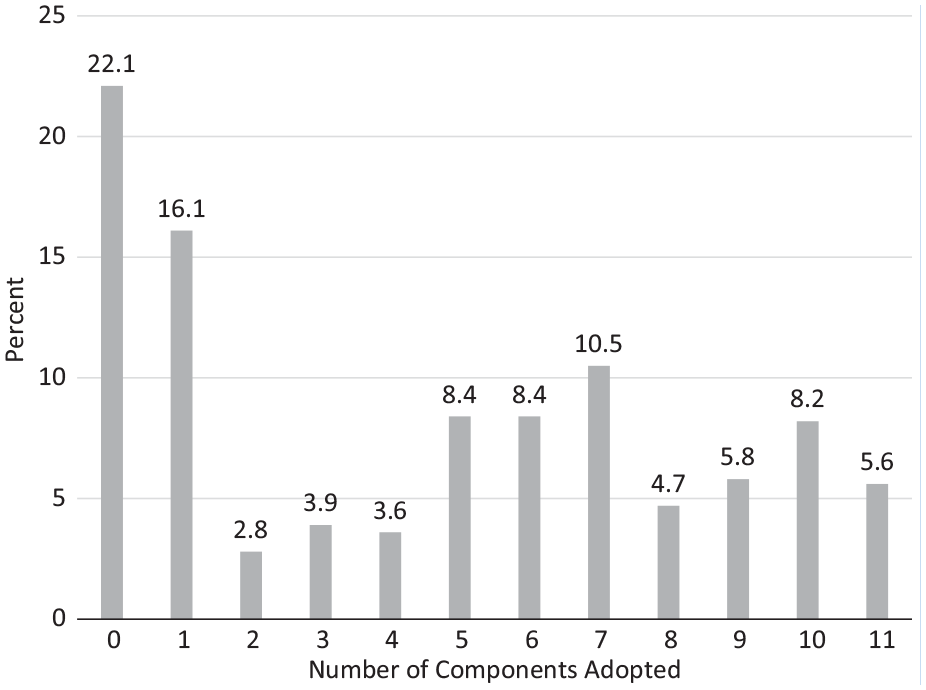
Number of components of an EHI policy adopted (0-11 components, median = 5; IQR = 1,7). EHI, exertional heat illness; IQR, interquartile range.
PAPM responses from AAs aggregated (n = 466) within each policy component
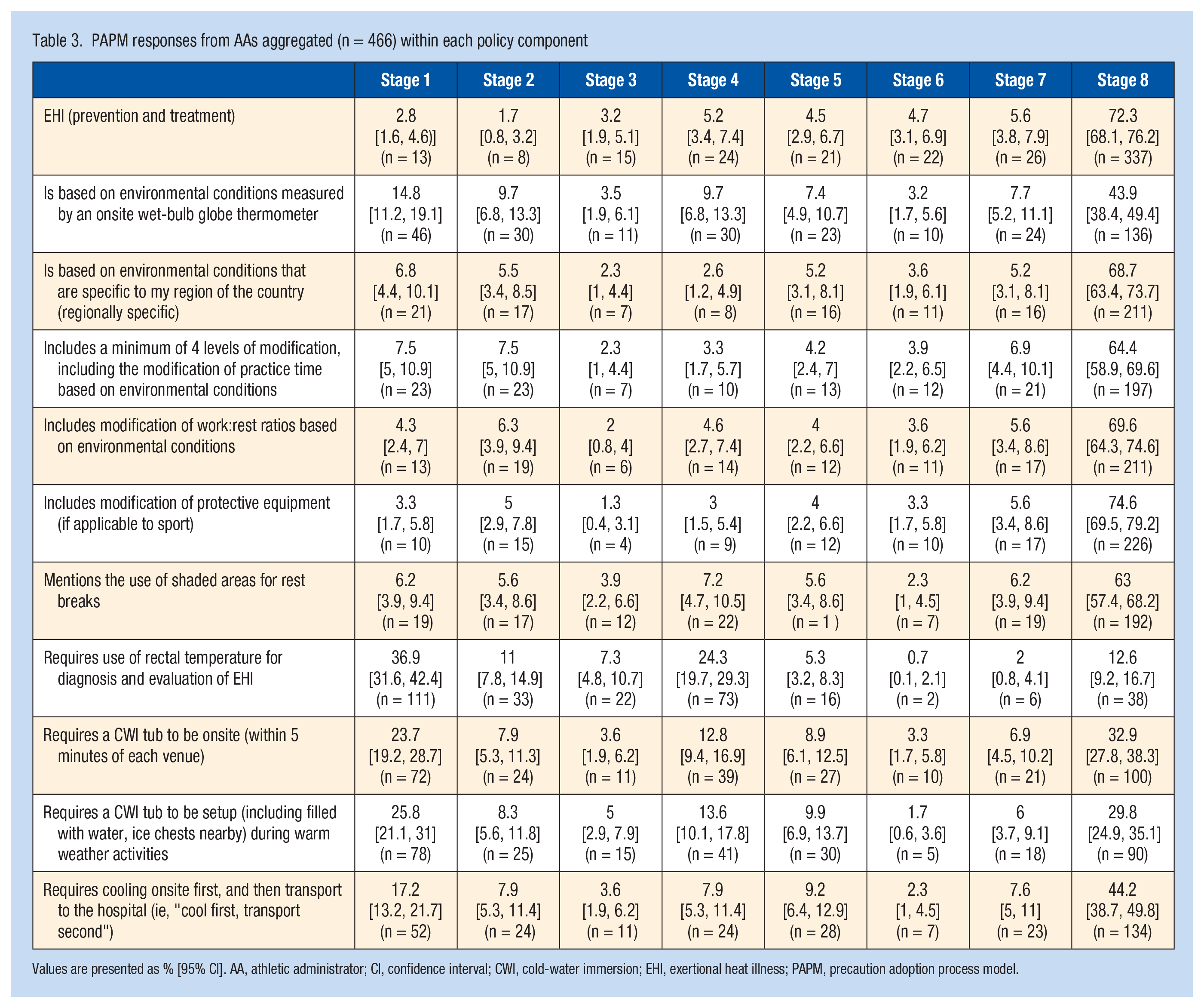
Values are presented as % [95% CI]. AA, athletic administrator; CI, confidence interval; CWI, cold-water immersion; EHI, exertional heat illness; PAPM, precaution adoption process model.
Comparisons
AAs who were older (49 ± 9 years) had a statistically greater likelihood of having a written policy for EHI prevention and treatment than AAs who were younger (Table 4; 46 ± 11; t141 = -2.68, P = 0.008, MD, -3.11 [-5.41, -0.82]). Chi-square tests of association found a statistically significant association between the adoption of a written EHI prevention and treatment policy with the treatment of an EHI previously (P = 0.05). In addition, AAs who reported treating an EHI previously reported adopting more components (median = 6, IQR = 2,6) than those who had not treated an EHI (median = 5, IQR = 0,5; P = 0.01). Further, Mann-Whitney U tests found AAs who had access to an AT reported more components of an EHI policy (median = 5, IQR = 1, 5) than those without access to an AT (median = 3.5, IQR = 0,3.5; P = 0.04). There were no differences between years in role at the school as an AA (P = 0.61) and treating an EHS previously (P = 0.83) with the number of components adopted.
Descriptive data of characteristics (eg, demographic information of participant and social determinants) compared with prevalence of adopting an EHI prevention and management policy
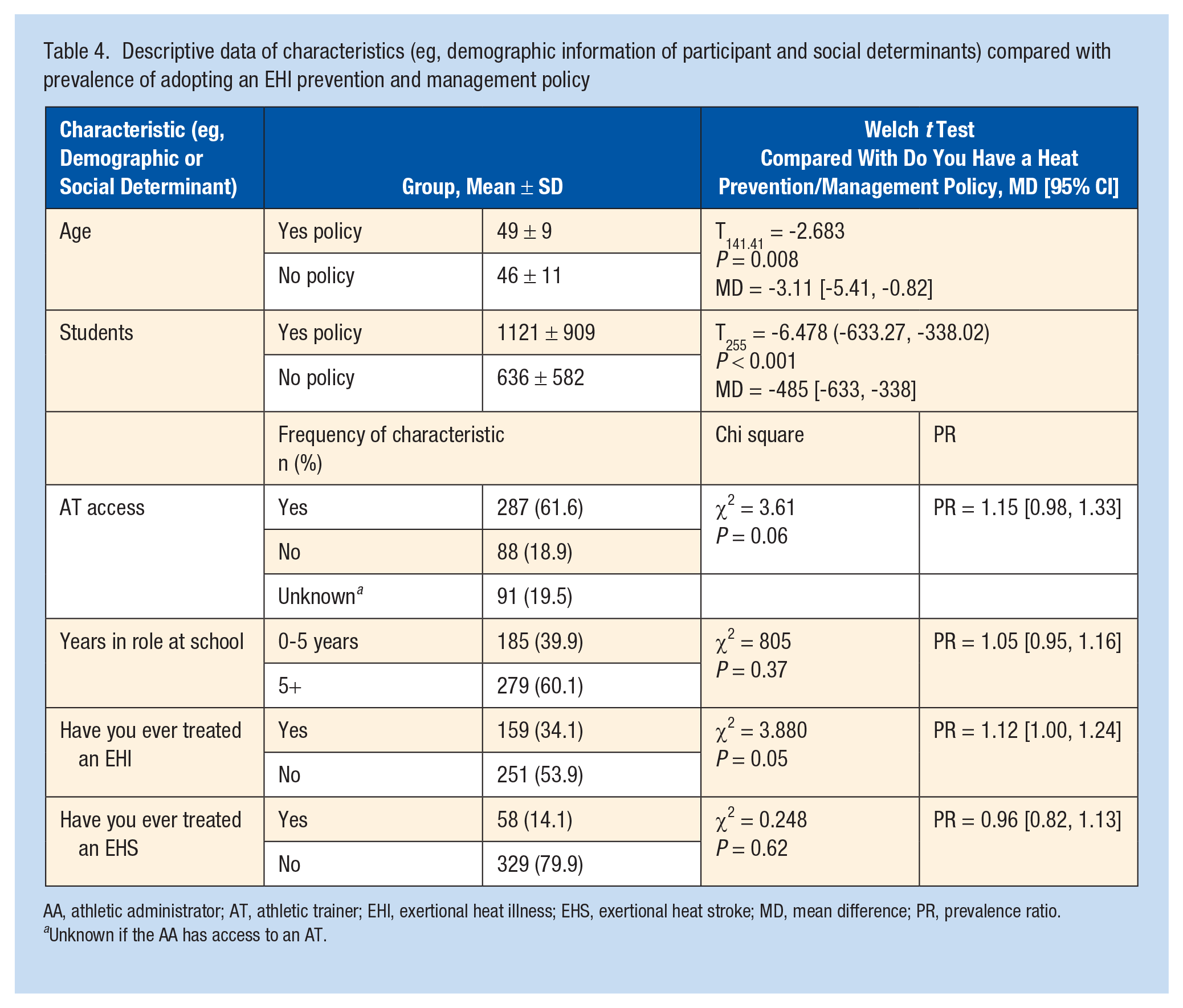
AA, athletic administrator; AT, athletic trainer; EHI, exertional heat illness; EHS, exertional heat stroke; MD, mean difference; PR, prevalence ratio.
Unknown if the AA has access to an AT.
Facilitators and Barriers
Having a medical professional present at the school was the most reported facilitator for adopting both a written policy for EHI prevention (n = 172, 36.9%) and the use of a rectal thermometer as a component within the policy (n = 138, 29.6%). The presence of a medical professional and having a model policy (ie, seeing someone else’s or using a template to fill in) were the most reported facilitators for setting up a CWI tub during warm weather events (n = 175, 37.6%). The most common barrier for a comprehensive EHI prevention policy (n = 51, 10.9%) was the school’s AT not being full time, and financial limitations for CWI tub setup (n = 103, 23%); the most common barrier for use of a rectal thermometer for the diagnosis of EHS was “I am not comfortable using a rectal thermometer” (Table 5; n = 149, 32.0%).
Facilitators and barriers reported by AAs
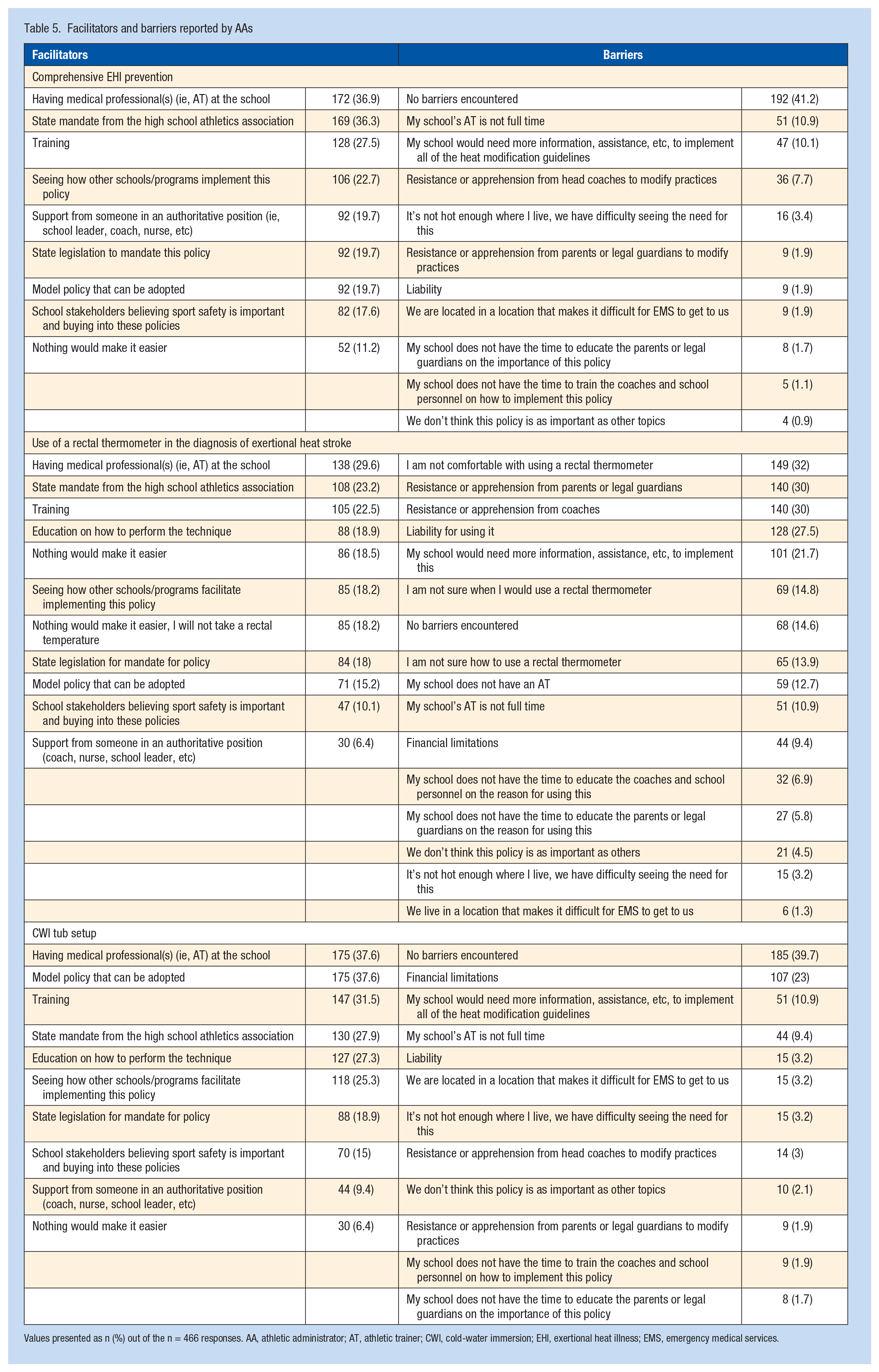
Values presented as n (%) out of the n = 466 responses. AA, athletic administrator; AT, athletic trainer; CWI, cold-water immersion; EHI, exertional heat illness; EMS, emergency medical services.
Discussion
The main purpose of this study was to investigate the adoption of comprehensive EHI policies as reported by US high school AAs, as well as to determine potential facilitators and barriers to adopting these policies. Our main findings were (1) a majority of AAs reported having an EHI policy, (2) very few AAs reported having a written policy for the diagnosis (eg, rectal temperature) and management of EHI, and (3) AAs with access to an AT had more components in their written EHI policies than those without an AT. The most frequently reported facilitator for having a written EHI policy was having a medical professional (such as an AT) present at the school. However, the most common responses for barriers included not having a full-time AT for having a comprehensive EHI policy, comfort level with using a rectal temperature for diagnosis, and financial limitations for having a CWI tub setup.
Our study finds 77.9% of AAs had an EHI policy. This finding is higher than previous research by McLeod and Cardenas, 15 who found 44.7% of AAs working in Arizona high schools had heat-related policies. A potential explanation for this difference may be that our study specifically asked about recognition and management policies, whereas McLeod and Cardenas 15 inquired about “additional heat-illness policies” in general. Further, our study was a national representation, whereas McLeod and Cardenas 15 focused on a single state (Arizona). By using the PAPM as a “readiness to act” model, we were able to identify AAs who displayed different health behaviors for each of the components of an EHI policy. For example, 36.9% of AAs reported they were unaware they should have a policy for the use of rectal temperature to diagnose EHI. In addition, 4.8% reported they decided not to have this policy. These findings are extremely interesting given 28% of ATs have decided not to act on this policy, and ATs have stated in previous literature that support from an authoritative position would facilitate their implementation of this policy. 25 Knowledge of the PAPM suggests that those who fall in the stages other than the “decided not to act” stage, may be more impressionable to implement a new behavior (or policy in this case).28,29 Given that AAs appear to be, at minimum, willing to learn what rectal temperature is, may indicate their support to identify strategies to implement this best practice.
Sport safety policy research with AAs as participants has found those earlier in their in professional role, larger school enrollment, and in suburban schools as having more comprehensive emergency action plans. These findings are somewhat mirrored in our study as those working in larger schools were more likely to have an EHI policy. However, this study found older AAs were more likely to have a policy than younger AAs. This may suggest sport safety best practice and corresponding policy educational initiatives may be facilitating improved knowledge on these topics, resulting in policy change. As with many other topics, previous experience typically facilitates behavior change,28,29 which appears to be supported by our findings as well. Although more AAs reported not being involved with the care of patients with EHI, those who had been involved with the care of EHI patients reported a higher number of components, compared with those who had not been involved in the care of an EHI patient. These findings indicate the need for further research into the influence of an integrated transdisciplinary and interdisciplinary approach on patient outcomes.
Access to Athletic Training Services
Our study supports that access to athletic training services is associated with having EHI policies. ATs are essential healthcare professionals with training to develop and implement EHI policies. Further, ATs have been identified as the primary persons responsible for the development and implementation of life-saving policies.17,20 Access to athletic training services not only facilitates the development of healthcare policies9,10,22,23 but also improves patient outcomes.12,19,26,27 Our results indicate that having access to an AT served as the most reported facilitator for adoption of a comprehensive EHI prevention policy (36.9% of AAs reporting), the use of a rectal thermometer for the diagnosis of EHS (29.6% of AAs reporting), and the setup of a CWI tub for EHS treatment (37.6% of AAs reporting). This finding is similar to previous work by several other researchers, including McLeod and Cardenas.10,15,22 While access to an AT was not significantly associated with the adoption of an EHI policy (prevalence ratio [PR] = 1.15 [0.98-1.33]; P = 0.06) within our data, the prevalence of responses by AAs focused on medical professional access highlights their understanding of the role, training, and expertise of an AT in the realm of EHI management. These findings further support the need to increase the number of secondary schools with access to athletic training services and written EHI policies.
Facilitators
While access to an AT served as the highest (%) facilitator of EHI-related policy adoption, a mandate from the state’s high school athletics/activities association served as the second highest facilitator noted by AAs for comprehensive EHI prevention policies (36.3%), use of a rectal thermometer for EHI diagnosis (23.2%), and CWI tub setup (27.9%). Furthermore, schools with more students enrolled were more likely to have an EHI policy compared with schools with fewer students (Table 4).
Despite the aforementioned notion that access to an AT serves as the highest facilitator for EHI-related policies, it must be noted that adoption of best practices for the recognition and treatment of EHS is abysmal among ATs. Previous literature shows that 16.9% to 33.3% of ATs reported adopting policy components for the recognition (ie, assessment of rectal temperature) and treatment (ie, CWI) of EHS patients.14,25 Further, in the assessment of ATs who reported treating a patient suspected cases of EHS, only 3.2% and 51.6% assessed rectal temperature and immersed the patient in ice water, respectively. 18 Despite the low adoption of EHS best practices among ATs, state-level mandates have been proposed as facilitators for adoption of both EHS-related and emergency action plan policies; the latter is supported by a greater number of emergency action plan policies in states with requirements than without. 24 These facilitators highlighted in this study (ie, presence of an AT and state-level mandates for EHS policies and EAPs) should be used as a guide to how secondary school AAs can enhance heat safety at their schools.
Barriers
It is imperative that we examine the perceived barriers to policy implementation to ensure athletic departments have an appropriate policy in place for the prevention, recognition and care of EHI. Interestingly, a majority of AAs reported “no barriers encountered” to implementing an EHI policy and a CWI policy. Yet, these policies did not have high compliance. AAs that did report barriers to the use of rectal thermometry included their discomfort with using it (32%), resistance from parents (30%), resistance from coaches (30%), and fear of liability. AAs participating in our study reported that their lack of comfort surrounding the use of a rectal thermometer was the highest barrier as it relates to the diagnostic tool to assess internal body temperature and determine EHS. While the AA should not be the person to assess a suspected EHS patient’s rectal temperature, their lack of comfort could potentially serve as a barrier for an AT. Only credentialed healthcare providers, such as ATs, should be assessing rectal temperature. AAs in a supervisory role are more likely to be a barrier to an AT performing rectal thermometry compared with resistance ATs or administrators may encounter from others (eg, parents/legal guardians, coaches, etc). 25 Often, this resistance arises due to the lack of education and common misconceptions on the use of a rectal thermometer to assess internal body temperature in exercising persons. 16 Perhaps the underreporting of successful management of EHS at the secondary school level has contributed to this perceived barrier that ATs will be held liable if they obtain a rectal temperature, despite the unlikely nature of this given an ATs scope of practice. Providing AAs with education on the methods and techniques used to assess rectal temperature as well as case studies where EHS has been managed properly may increase their comfort level with this diagnostic technique, thus potentiating the support, and use, of this technique among ATs in the high-school setting. 7 This support from the AAs can potentially have a positive effect on other stakeholders to ensure the AT is supported in the use of rectal thermometry and improve heat safety.
Financial limitations were identified as the largest barrier to having a CWI tub setup during warm weather events (39.7%). While financial limitations can, and often do, regulate what items can be purchased for an athletics department, AAs must reframe their priorities to include life-saving equipment such as a CWI tub. A CWI tub can come in many different forms. It may be a 100-gallon tub that is developed primarily as a horse trough, which costs approximately $100 (via Ace Hardware February 2022). Other methods for CWI may include use of a bathtub, garbage can, kiddie pool, or other type of basin that holds water and in which most persons could be fully immersed. Alternatively, approaches such as the utilization of the TACo method may serve as both an affordable and effective method of cooling 8 ; however, it must be emphasized that CWI using a tub where the patient can be fully immersed yields the greatest cooling rates. 13 Other options to offset the costs associated with acquiring these life-saving tools are to solicit support from various funding sources (eg, grant programs, corporate/individual donations, team booster clubs, etc). Recently, the National Federation of High School Associations awarded $1.5 million in grant funding to supply wet bulb globe thermometers to high schools to provide the means to monitor onsite environmental conditions and implement appropriate EHI prevention modification strategies. In addition, among other organizations/foundations, the Zach Martin Foundation donates cold tubs to high schools. Although the present study found barriers regarding the use of rectal thermometry and financial impacts to CWI, we have provided solutions that may assist AAs and ATs with ensuring heat safety for secondary school athletes.
Limitations and Future Research
This study has significant limitations. We assessed only high school AAs; without receiving input from other stakeholders within each respective high school (eg, AT, principal, nurse, superintendent, coach, etc), we are unable to gain an understanding of the factors associated with policy adoption at the school level (ie, the interplay between all athletics program stakeholders). Unfortunately, AAs have a historically poor response rate for research surveys. While our response rate is similar to that of other studies,22,23 the low number of respondents limits the generalizability of our findings.
Conclusion
AAs are uniquely positioned to influence the health and safety for all high school athletes. The development of EHI policies allows for proactive planning to prevent or properly respond to a heat-related event. This study shows that although most AAs report adopting an EHI policy, the policy is often incomplete, leaving gaps in their high school’s emergency preparedness. This study suggests having an AT, having state mandates for emergency action plans and EHI policies, and schools with more students were all facilitators for EHI policy adoption. Barriers for EHI policy adoption consisted of lack of comfort or fear of liability regarding rectal thermometry as well as a financial barrier regarding CWI. Efforts to improve policy adoption are necessary and may include increasing access to athletic training services and improving knowledge initiatives to better inform AAs and other stakeholders on these policies.
Footnotes
The following authors declared potential conflicts of interest: S.E.S-M. received a grant from the Eastern Athletic Trainers’ Association, gave expert testimonies in legal cases pertaining to sport-related death, has grants pending with the NIH relating to work, and was a guest speaker at state and national meetings. W.M.A. received royalties from Springer Nature for an edited textbook.
This study was fully funded by a research grant from the Eastern Athletic Trainers’ Association, Inc. This work is the author’s own and not that of the United States Olympic & Paralympic Committee, or any of its members or affiliates.
