Abstract
Objectives
Children scheduled for surgery and anesthesia often experience fear and anxiety before the procedure, as well as pain afterward. While medical treatments are essential for managing these challenges, design strategies that positively influence environmental and psychological factors can significantly improve children's experiences and their overall subjective well-being. This narrative literature review examines “design for well-being” strategies that support the subjective well-being of children undergoing surgical procedures.
Background
According to the World Health Organization, health is defined not merely as the absence of disease but as a state of complete physical and mental well-being. Achieving such well-being requires not only medical care but also the optimization of environmental and psychological conditions that impact emotional states. Today, evidence-based, multidisciplinary approaches are recommended to promote well-being. In health-related design, one focus is on improving the quality of medical care, while another addresses non-medical factors that influence subjective well-being.
Methods
This research employs a non-systematic literature review methodology, utilizing existing literature and evidence-based approaches to synthesize relevant strategies.
Results
Enhancing subjective well-being—through evidence-based design strategies such as age-appropriate environmental modifications, sensory-friendly elements, and interactive distraction tools—alongside optimized medical practices in pediatric surgeries contributes to improved clinical outcomes and reduced perioperative stress. The review highlights “design for well-being” strategies, which effectively support the subjective well-being of children undergoing surgical procedures.
Conclusions
Emphasizing “design for well-being” strategies is crucial for enhancing the overall experiences and well-being of children undergoing surgery. Future research should focus on the implementation and long-term impact of these design interventions to further validate their effectiveness and scalability.
Introduction
The World Health Organization (WHO) defines health not merely as the absence of disease or infirmity, but as a state of complete physical, mental, and social well-being. From this perspective, complete well-being is achieved when an individual's emotional and cognitive needs are fully met—when they “feel good and function well” (World Health Organization, 2024). In the field of positive psychology, this concept is referred to as “subjective well-being,” and it has been identified as a key goal in addressing the emotional challenges associated with hospital processes, particularly for pediatric patients who often experience distress (Ravens-Sieberer et al., 2014). Children often undergo painful procedures during their time in the hospital (Friedrichsdorf & Goubert, 2019; Salmela et al., 2011; Stevens et al., 2011; Vejzovic et al., 2020). Preoperative evaluations, such as blood drawing, physical examinations, and imaging procedures, are common interventions that can trigger fear, anxiety, or discomfort in children. Some of these procedures, such as blood draws or intravenous access, can even cause pain. Additionally, the administration of sedative premedication—whether intramuscularly or intravenously—to alleviate pre-surgery anxiety, as well as the induction of anesthesia via a mask, is often distressing for pediatric patients. After surgery, the pain associated with recovery from anesthesia further contributes to the overall traumatic experience (Chow et al., 2020; Friedrichsdorf & Goubert, 2019; Kain et al., 2006; Kar et al., 2015; Kennedy et al., 2008; Salmela et al., 2011; Stevens et al., 2011; Vejzovic et al., 2020). Fear, anxiety, and pain are mental states that vary among individuals and significantly influence how the body responds to medical interventions (Chow et al., 2020; Kain et al., 2006; Kar et al., 2015; Kennedy et al., 2008; Salmela et al., 2011). In children, inadequate management of pain following surgical procedures can lead to heightened fear and anxiety in response to future medical treatments, causing long-term stress about potential procedures. Moreover, poorly managed pain during early childhood not only exacerbates emotional distress but also has negative implications for brain development, potentially affecting children and adolescents throughout their lives (Chow et al., 2020; Escalona-Espinosa et al., 2023; Kain et al., 2006; Kar et al., 2015; Kennedy et al., 2008; Young, 2005). Healthcare professionals employ various methods, including pharmacological interventions, behavioral guidance techniques, and parental support, to alleviate the pain, fear, and anxiety experienced by children undergoing surgical procedures (Di Sarno et al., 2023; Friedrichsdorf & Goubert, 2019; Gai et al., 2020; Menés Fernández et al., 2023; Pancekauskaitė & Jankauskaitė, 2018; Peters, 2015). Pharmacological approaches are commonly used due to their ease of application and high effectiveness, often requiring minimal cooperation from the patient. However, while effective, these approaches are not without potential side effects and may not always be sufficient on their own. Younger children, in particular, may resist taking medication (Di Sarno et al., 2023; Gai et al., 2020; Pancekauskaitė & Jankauskaitė, 2018). In addition to pharmacological methods, non-invasive education and practice tools based on physical sensations offer safe alternatives for managing both pain and anxiety. Cognitive behavioral therapy and behavior management techniques—such as coping skills and distraction methods—are also widely used, although these approaches typically require more time to implement effectively (Gai et al., 2020; Liossi & Franck, 2008; Pancekauskaitė & Jankauskaitė, 2018; Peters, 2015). In addition to the medications and techniques used by healthcare professionals to manage pain and anxiety, both internal and external factors play a significant role in fostering positive emotions in children (Goubert & Friedrichsdorf, 2019; Menés Fernández et al., 2023; Peters, 2015). Therefore, optimizing these factors alongside medical interventions is crucial for reducing fear and anxiety and enhancing subjective well-being in children scheduled for surgery. All potential influences on the emotional state of pediatric patients, including environmental, psychological, and social factors, should be carefully considered to create a holistic approach to their care (Liossi & Franck, 2008; Pancekauskaitė & Jankauskaitė, 2018). Pain, anxiety, and fear can be effectively managed through a multidisciplinary approach. However, many evidence-based interventions, tools, and methods designed to reduce procedural pain and fear remain underutilized in pediatric care (Di Sarno et al., 2023; Escalona-Espinosa et al., 2023; Liossi & Franck, 2008; Rusy & Weisman, 2000; Stevens et al., 2011; Vejzovic et al., 2020).
Design researchers aiming to enhance patient well-being define subjective well-being not by the absence of negative emotions, but by the predominance of positive ones (Diener et al., 1999). Designing healthcare environments—such as the physical setting, social connections, and external surroundings—based on principles of well-being involves promoting healthy behaviors, fostering participation, and developing sustainable methods for complete well-being and happiness. This process requires critical thinking and innovation in design. Design thinking is widely acknowledged as an effective method for solving problems by understanding human needs and responding with innovative solutions. Among the various areas of interest for design researchers, pediatric care has emerged as a focus (Cartland et al., 2018; Diener et al., 1999; Gaminiesfahani et al., 2020; Marques da Rosa et al., 2022; Peng et al., 2022; Trottier et al., 2019).
Method
We used a narrative review approach, which is a form of evidence-based synthesis that aims to bring together findings from various studies for reinterpretation or to reveal potential connections (Greenhalgh et al., 2018; Thorne, 2018). This method is particularly suitable for exploring complex, interdisciplinary fields such as health and design, as it allows for contextual analysis and thematic integration across different types of evidence.
Our research question was: “Are there any design strategies that have a positive effect on the subjective well-being of children undergoing operations under general anesthesia, beyond medical applications?”
To address this question, we conducted a three-step literature search using Google Scholar (English-language publications only): We first explored factors that negatively affect the well-being of children scheduled for surgery. Next, we reviewed design literature that discusses the relationship between design and well-being for children. Finally, we identified design-related interventions reported to support subjective well-being and aimed to generate forward-looking suggestions based on this synthesis.
Studies were included if they contained at least two of the following keywords (or their synonyms): pediatric anesthesia/anesthesia and anxiety, design for well-being/well-being, design for subjective well-being/well-being, positive design or design interventions. Although articles were not selected strictly by publication year or keyword match, the focus was on ensuring that each included study provided evidence-based insights pertinent to the topic, pediatric anesthesia and subjective well-being. We excluded studies focusing on adults, healthy children, and case reports.
Hospital Routines for Pediatric Patients Scheduled for Surgery
The analysis of the selected literature revealed several hospital routines. These routines were examined in order to identify specific distress points that could affect children's subjective well-being in the hospital setting. Enhancing the subjective well-being of pediatric patients scheduled for surgery requires careful observation and identification of “
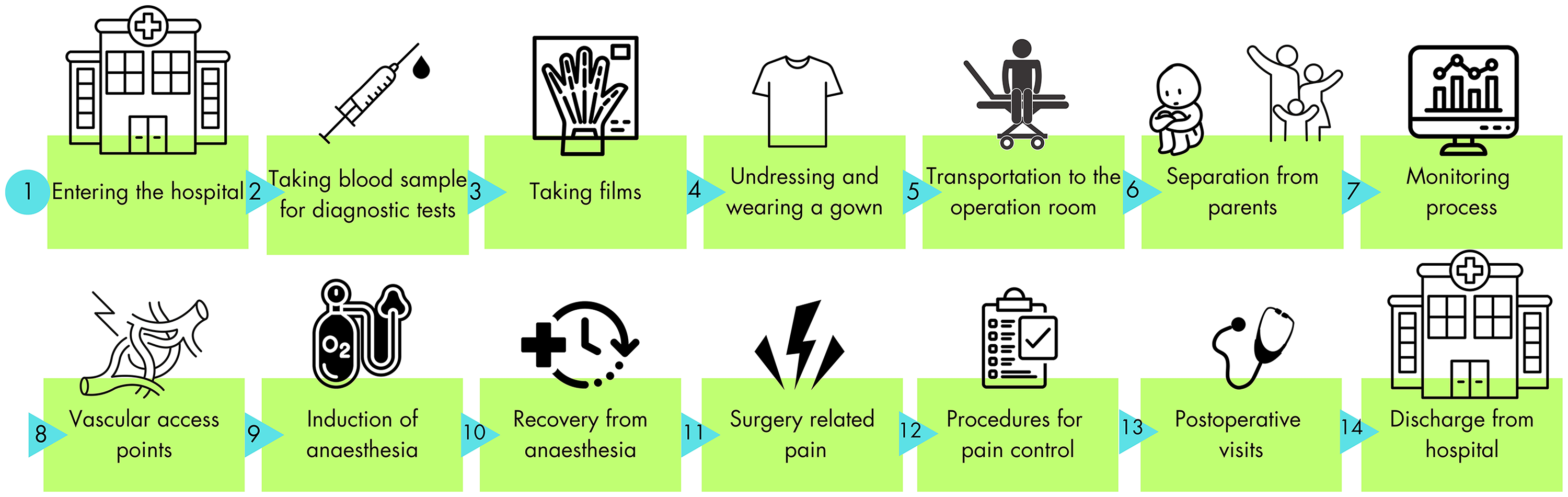
Hospital routines for pediatric patients scheduled for surgery.
Children, Surgery, and Social Environmental Factors Affecting Subjective Well-Being in Surgery Patients
When planning studies on subjective well-being in pediatric patients scheduled for surgery, it is essential to consider both the characteristics of the children and the medical procedures involved (Diener et al., 2018; Fontoura et al., 2023; Kerimaa et al., 2024; Simonetti et al., 2022). Factors such as mental and motor development, temperament, and the severity of fear and anxiety play a significant role in influencing a child's personal subjective well-being (Aykut & Isik, 2018; Isik et al., 2010). Additionally, procedural characteristics—whether the surgery is minor or major, the length of hospital stay, postoperative treatment plans (e.g., the use of epidural catheters, postoperative pain levels, the need for repeated interventions, and prolonged hospital stays)—can all affect a child's emotional state. Similarly, the type of anesthesia, the intensity of pain experienced, and the methods and medications used for pain control are critical factors that influence a child's emotional well-being (Kain et al., 2006; Young, 2005). The presence of a supportive, compassionate, and protective family or social environment further contributes positively to the child's emotional state (Espinel et al., 2014) (Figure 2).
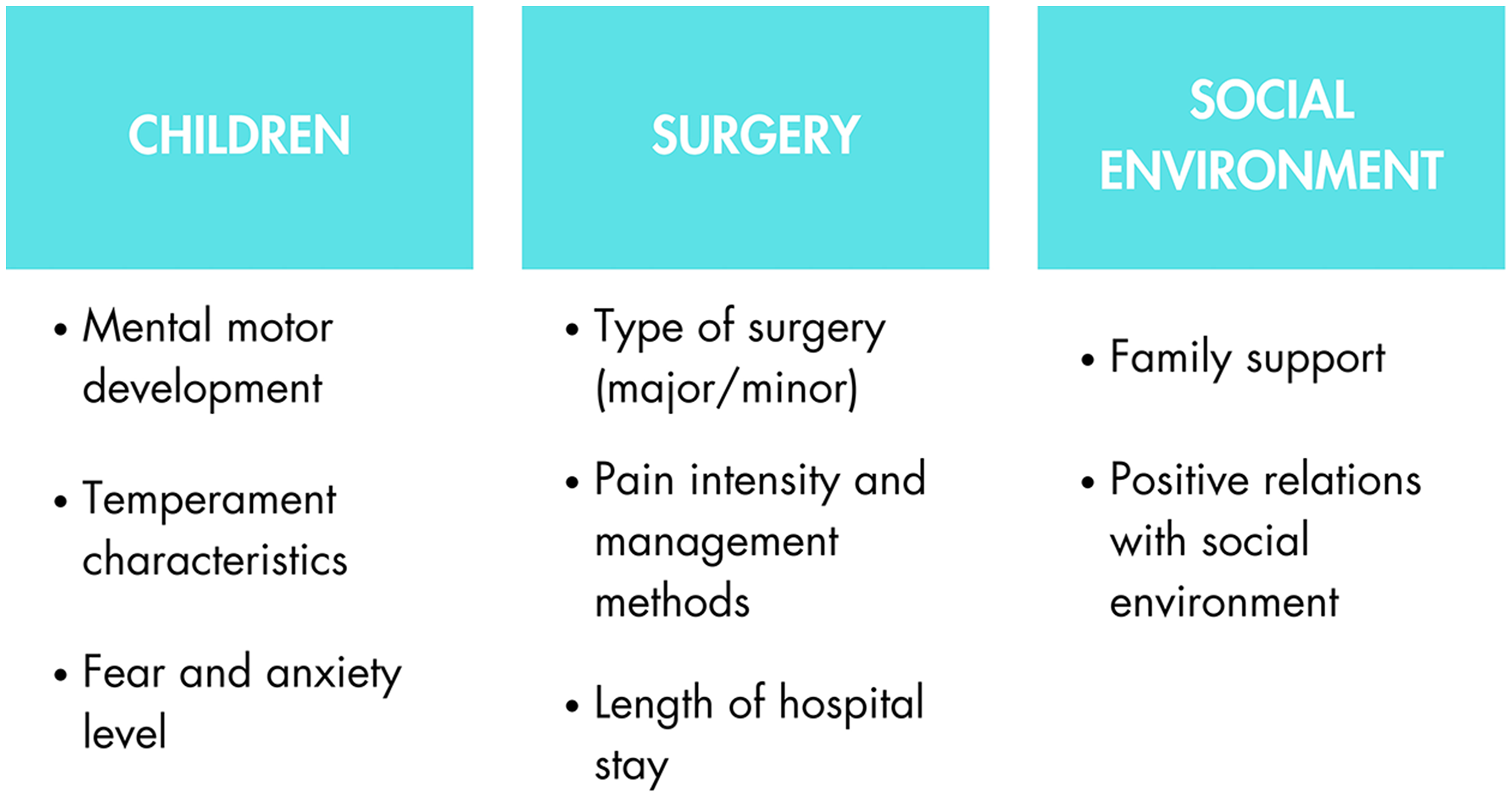
Children, surgery, social environment-related factors affecting subjective well-being of the pediatric patients scheduled for surgery.
Team Members Providing Healthcare Services to Children Scheduled for Surgery
Another important factor in research on subjective well-being in pediatric patients is identifying the healthcare team responsible for their care (Peng et al., 2022). In the hospital setting, pediatric surgeons, nurses, anesthesiologists, psychologists, nutritionists, transport staff, cleaning personnel, and office workers are all directly or indirectly involved in providing health services to children undergoing surgery. This team consists of multiple stakeholders, including healthcare professionals and support staff, whose coordinated and goal-oriented collaboration plays a crucial role in positively influencing children's health and subjective well-being (Frush & Krug, 2014; Javaid et al., 2024; Peng et al., 2022).
Designs to Improve Subjective Well-Being in Hospital Routines for Pediatric Surgery Patients
In addition to the methods used by healthcare professionals to positively impact children's overall health, numerous design approaches can be developed by design researchers (Boon, Baha et al., 2020; Boon, Rozendaal et al., 2016; Diener, 1984, 2001; Eid & Diener, 2004; Fredrickson, 2001; Frush & Krug, 2014; Lyubomirsky, 2007; Lyubomirsky et al., 2005; Peng et al., 2022) (Table 1).
Approaches for Improving Subjective Well-Being in Hospital Routines for Children Scheduled for Surgery.

Design for Subjective Well-Being
Many design methods are employed to enhance the subjective well-being of patients. Subjective well-being is a broad, multifaceted concept that encompasses the cognitive and emotional perceptions, experiences, reflections, and evaluations that individuals attribute to their lives. The cognitive component represents global and domain-specific life satisfaction, while the emotional component includes both positive and negative effects. Lyubomirsky (2007) defined subjective well-being as “the experience of joy, contentment, or positive well-being, combined with a sense that one's life is good, meaningful, and worthwhile.” Similarly, Eid and Diener (2004) described subjective well-being as “references to one's multi-dimensional evaluation of their lives, including cognitive judgments of life satisfaction as well as affective evaluations of moods and emotions.” In simpler terms, Diener et al. (1999) defined high subjective well-being as the predominance of positive emotions, rather than the mere absence of negative emotions. Despite varying expressions, most definitions agree that subjective well-being comprises both emotional and cognitive components. Positive affect encourages individuals to actively engage with their goals and surroundings, supporting them in pursuing new objectives (Lyubomirsky et al., 2005). Research has consistently shown that happier individuals are more motivated to pursue goals and embrace new challenges (Fredrickson, 2001; Lyubomirsky et al., 2005). Desmet and Pohlmeyer (2013) build on this understanding in their concept of positive design, which emphasizes the role of design in eliciting positive emotions by supporting individuals’ pursuit of personally meaningful goals. These goals can include tasks such as following steps to maintain health or embracing challenges like undergoing surgery to improve health. From this perspective, integrating emotionally supportive elements into hospital routines can enhance subjective well-being and reduce stress. This insight is particularly relevant in pediatric healthcare settings, where children scheduled for surgery often face heightened anxiety and emotional vulnerability. In such contexts, design can play a key role in creating environments that foster calmness, security, and positive engagement. Thus, drawing on theories of positive design presents a valuable opportunity for improving children's well-being during preoperative care. By applying these design principles, we may support not only emotional resilience but also better clinical outcomes (Boon, Baha et al., 2020; Boon, Rozendaal et al., 2016; Toledo-Delgado et al., 2013; Tonetto, da Rosa et al., 2021; Tonetto, Pereira et al., 2020). At this stage, one of the key areas of focus for design researchers in promoting well-being is developing research that enhances health and well-being in hospital settings. While objective (external) well-being is considered crucial in the healthcare field, Groeneveld et al. (2018) highlight that designers and design researchers often face challenges in this area. There is a growing need for new strategies that contribute to both the medical goals and subjective well-being of patients and healthcare providers. Positive affect has been linked to reductions in morbidity, pain, and other disease symptoms (Howell et al., 2007; Lyubomirsky et al., 2005, Pressman & Cohen, 2005). Designers have made significant contributions to improving the subjective well-being of pediatric patients in hospital settings. In these efforts, design for subjective well-being addresses not only objective aspects of well-being, such as nutrition and the physical structure of healthcare facilities but also subjective elements, including the child's self-assessment, the illness, the hospital environment, and the quality of health services (Boon et al., 2020; Richey & Klein, 2014; Toledo-Delgado et al., 2013).
Designers should observe medical processes and collaborate with a team to develop appropriate methods. The effectiveness of these interventions should be assessed using reliable and valid evaluation techniques in studies aimed at improving the subjective well-being of pediatric patients scheduled for surgery (Figures 3 and 4).

Design for subjective well-being template in hospital routines.
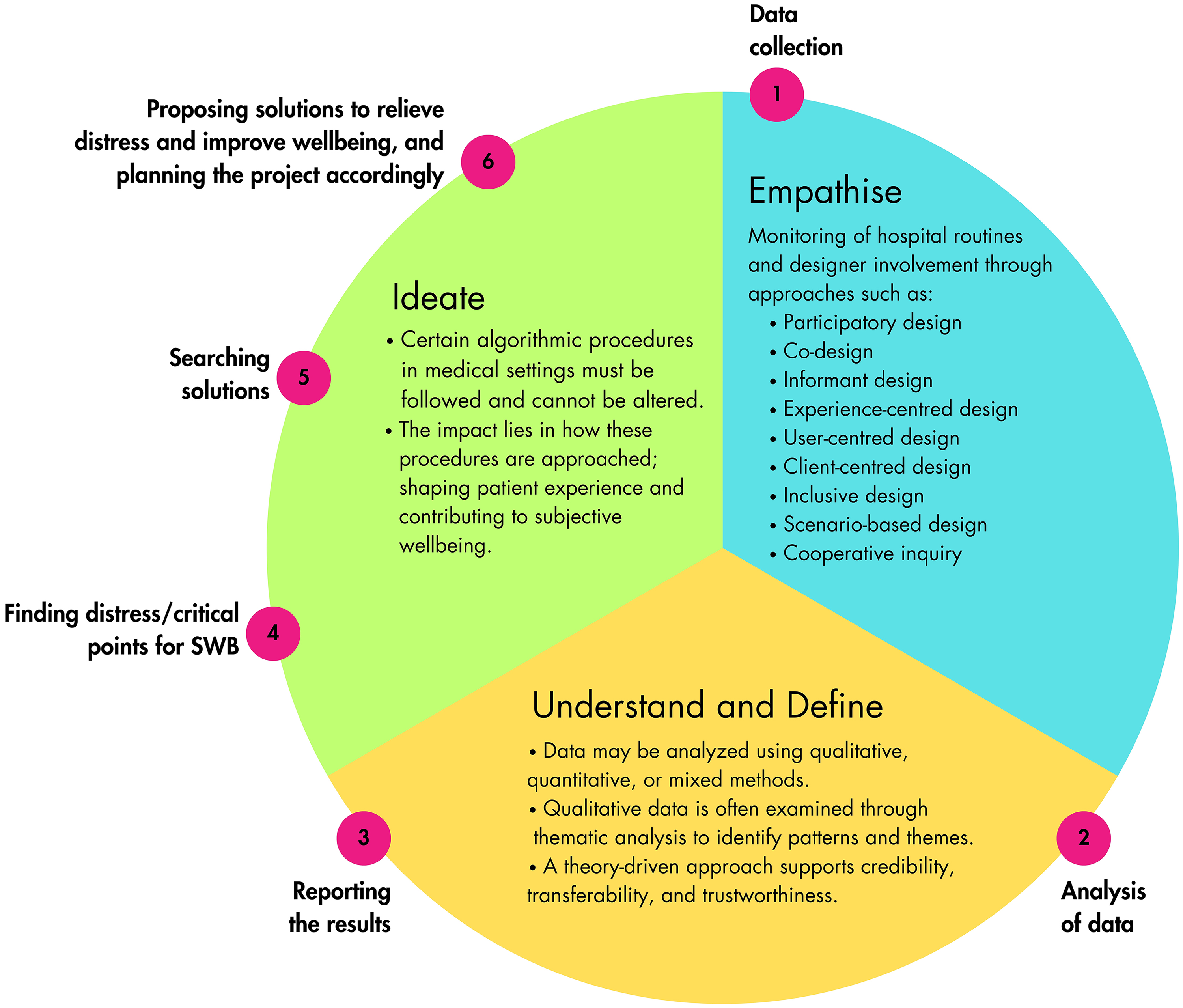
Design framework targeting subjective well-being in surgery planned pediatric cases.
Overview of Design Research on Subjective Well-Being in Hospital Routines
Children's experiences during hospitalization may impact their subjective well-being (Diener et al., 1999; Ryan & Deci, 2001). Studies have shown that hospital routines often have a negative effect on children's well-being, leading to feelings of fear, anxiety, and sadness (Wakefield et al., 2010). Even the act of coming to the hospital, an unfamiliar environment for most children, can be a major source of stress. Creating a sense of familiarity with the hospital experience has been shown to be an effective method for alleviating this stress. Giraldi and colleagues (2019) found that wayfinding systems and communication design products can significantly improve pediatric patient experiences, not only by helping children navigate unfamiliar hospital spaces, but also by making these environments feel more familiar. In this context, familiarity refers to the use of child-friendly visual cues such as recognizable symbols (e.g., animals, shapes), bright and engaging colors, simple and intuitive signage, and playful illustrations. These elements help transform the hospital from a stressful, unknown environment into a space that feels safer and more emotionally accessible to children. An early study of Gershon et al. (2004) assesses the feasibility and effectiveness of virtual reality (VR) as a distraction for children undergoing venous port insertion. The study found that VR not only helped reduce self-reported anxiety but also decreased physiological stress indicators such as heart rate and blood pressure during the procedure. By immersing children in engaging virtual environments, the VR experience provided a form of distraction, promoting emotional security and enhancing subjective well-being in an otherwise stressful medical context. Similarly, incorporating fun elements such as interactive virtual games and gamification strategies during hospitalization has been shown to significantly improve the emotional and psychological well-being of children undergoing cancer infusion treatments (Boon et al., 2020; Toledo-Delgado et al., 2013; Tonetto et al., 2020). These playful and engaging activities provide children with a sense of agency and distraction from the stressful hospital environment, helping to reduce anxiety, boost mood, and enhance overall emotional resilience during treatment. Gamification can also encourage adolescents to engage in inpatient and develop a better understanding of their illness (Cook et al., 2010, Gershon et al., 2004; Giraldi et al., 2019; Li et al., 2011; Lindsay et al., 2019; Wilson & McDonagh, 2014). Play therapy is another valuable intervention in pediatric healthcare settings, enhancing the emotional, cognitive, and social well-being of children (Bratton et al., 2005; Godino-Iáñez et al., 2020). Studies have shown that playing games during hospitalizations significantly improves subjective well-being in children receiving cancer treatment, including those undergoing infusion therapy. One such study by Fontoura et al. (2023) focused on the emotions of hospitalized children and proposed a design intervention aimed at improving their subjective well-being during their hospital stay. Using a qualitative approach—including observations, semi-structured interviews, and participatory mapping with children, caregivers, and healthcare professionals—the study highlights how design interventions can enhance children's emotional well-being during hospital routines by fostering participation and emotional engagement. Additionally, interactive toy robots that engage with pediatric patients to reduce pain, stress, and anxiety have been successful in this regard (Jeong et al., 2015). A notable example in healthcare is the use of audiovisual resources—such as a closed-circuit TV system that allowed children to see their carer(s), watch a DVD movie, or listen to their carer(s) via a microphone—to reduce the need for anesthesia during radiotherapy treatment and to prepare children and their families before the procedure (Engvall et al., 2018; Willis & Barry, 2010).
Discussion
Various initiatives have been implemented to support the holistic health of children undergoing surgery. These range from environmental design interventions, such as hospital architecture and the arrangement of physical conditions including temperature, noise levels, color schemes, and spatial layout, to behavioral design strategies that influence how children experience and interact with the healthcare setting (Cartland et al., 2018; da Rosa et al., 2021; Gaminiesfahani et al., 2020). Numerous well-established environmental design interventions—such as anesthetic induction rooms, incorporation of natural daylight within operating theaters, nature-inspired murals, and curated music selections—are routinely employed in advanced pediatric surgical settings in developed countries. These strategies have demonstrated substantial efficacy in mitigating perioperative anxiety and promoting the subjective well-being of pediatric patients. For instance, anesthetic induction rooms often feature abundant natural light alongside nature-themed murals to cultivate a serene and calming environment (Cartland et al., 2018; Ulrich et al., 2008). Interventions can range from low-cost behavioral strategies to more resource-intensive architectural changes. While behavioral interventions rely on the consistent efforts of practitioners and can be implemented more flexibly, architectural design typically involves significant financial investment, planning, and institutional support. These changes are often beyond the control of individual practitioners. However, when thoughtfully implemented, architectural interventions can offer long-term benefits, creating environments that consistently support subjective well-being, without requiring ongoing individual effort (Figure 5).
Categorization based on their difficulty of implementing.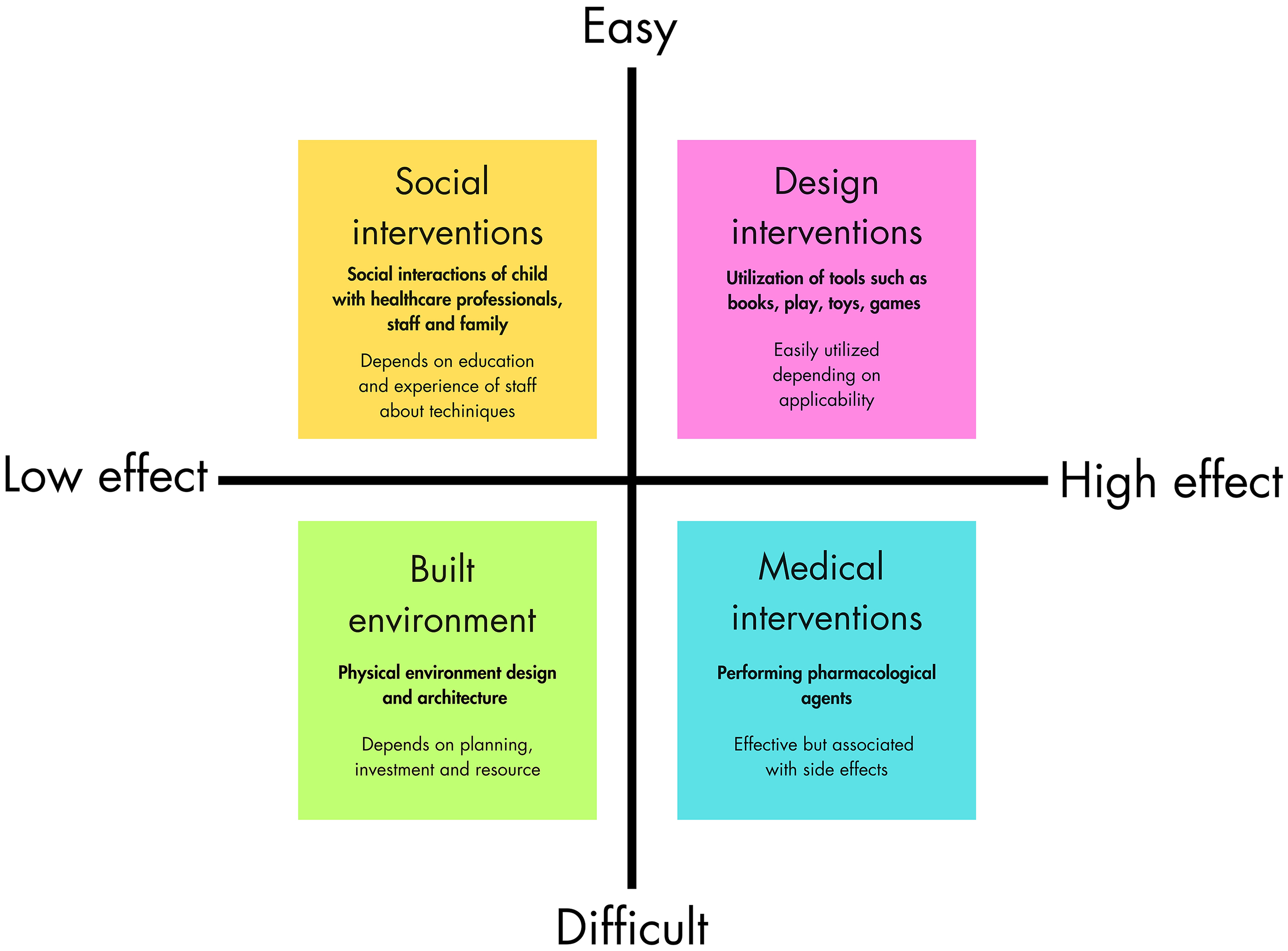
Optimizing the physical environment, for example, through lighting, noise control, and color choices, can effectively enhance comfort and reduce anxiety in pediatric patients. However, such interventions often require significant investment of time and resources upfront. In contrast, behavioral strategies have been more commonly adopted over time by experienced healthcare professionals. For instance, physicians have employed techniques to improve children's acceptance of medication (Isik et al., 2008; Kar et al., 2015; Kerimaa et al., 2024; Trottier et al., 2019). Pharmacological interventions to manage preoperative anxiety are also available, though they may present drawbacks due to potential side effects. Therefore, the balance between feasibility and effectiveness across these different approaches must be carefully considered when designing pediatric healthcare experiences.
This is where design interventions become especially valuable—offering creative, cost-effective, and human-centered solutions that extend beyond medical treatment to support children's emotional well-being (Payam et al., 2023; Peng et al., 2022; Pressman & Cohen, 2005). These interventions focus on the experiential dimensions of the perioperative process. Designers have increasingly made meaningful contributions by creating playful, engaging, and child-centered solutions within healthcare environments. Their efforts aim to emotionally prepare children for surgery, using tools such as therapeutic toys and interactive games (Bratton et al., 2005; Cook et al., 2010; Giraldi et al., 2019; Godino-Iáñez et al., 2020). Designers can contribute across a broad spectrum, from creating supportive, engaging environments to developing toys and activities that promote emotional comfort and engagement.
Limitations
Narrative reviews are sometimes considered less standardized than systematic reviews due to the absence of predefined protocols, but they offer important advantages, especially for exploring complex, multidisciplinary topics where evidence is diverse and emerging. In this article, the narrative review method enabled a broad and interpretive synthesis of findings from both healthcare and design disciplines. It was particularly useful in identifying research directions and generating new perspectives on how design can contribute to pediatric well-being in surgical contexts. We followed best practices for narrative reviews by clearly defining our research question, conducting a structured literature search, and referencing evidence-based sources.
While this approach provided valuable insights, we acknowledge the inherent challenges of embracing topic due to its complex and multi-dimensional nature. Intervention studies often differ in methodology, settings, and outcome measures, making direct comparisons difficult. Many reviews highlight high heterogeneity and moderate-quality evidence in this field.
Conclusion
In conclusion, this narrative review aims to emphasize the role that design researchers can play in supporting the holistic health and subjective well-being of children scheduled for surgery. The goal of designs intended to improve the subjective well-being of pediatric patients is not to completely eliminate the negative experiences associated with surgery and anesthesia, but to mitigate them while enhancing positive experiences. By increasing subjective well-being alongside optimizing medical practices during surgical interventions, an inherently traumatic process for this vulnerable patient group, there can be not only medical improvements but also social and economic benefits. Further research on “design for well-being” by design researchers, in collaboration with healthcare professionals who often focus on objective well-being, will contribute significantly to improving patient health with minimal harm.
Footnotes
Authors Contributions
The main idea and literature review of this review article, along with the preparation and writing stages, were carried out by Dr. Hande Işık Tosun. Prof. Dr. Berrin Işık structured and reviewed the article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
