Abstract
Objectives:
This systematic literature review synthesizes and assesses empirical research concerning the use of the built environment as a therapeutic intervention in adult mental health inpatient facilities. The review explores the impact of facility design on patient outcomes.
Background:
There is a growing recognition that the built environment in mental health facilities must strike a balance between ensuring safety and providing a therapeutic atmosphere. A review addressing how facility design contributes to this therapeutic environment is warranted.
Methods:
Database searches were conducted in CINAHL, Embase, PsychInfo, PubMed, and Web of Science from inception up to March 10, 2022. The Scottish Intercollegiate Guidelines Network (SIGN50) critical appraisal checklists were used to assess the quality of included studies.
Results:
Of the 44 peer-reviewed studies identified from nine countries, several factors emerged as vital for the therapeutic environment in mental health inpatient facilities. These included personal spaces prioritizing privacy and control of the environment, daylight-optimized spaces, versatile communal areas promoting activities and interaction, designated areas for visits and spiritual/contemplative reflection, homelike environments, the inclusion of artwork in units, open nursing stations, and dedicated female-only areas. Yet, there is a need for research yielding stronger evidence-based designs harmonizing with therapeutic needs.
Conclusion:
This review offers initial guidance on designing mental health facilities that foster a therapeutic environment, while highlighting that the influence of facility design on mental health inpatients is considerably under-researched.
Keywords
Introduction
The significance of the physical environment in healthcare settings cannot be overstated. Over the years, its role in enhancing the quality of healthcare delivery has been researched and is now better understood. Several literature reviews have shown that well-designed physical healthcare environments can positively impact patient health, well-being, and safety (Dijkstra et al., 2006; Huisman et al., 2012; Jamshidi et al., 2020; Ulrich et al., 2008). Among such contributions, Ulrich et al. (2008) identified several design factors that play a pivotal role in enhancing patient outcomes, including single-bedded rooms, access to daylight, ergonomic designs, and appropriate acoustic environment and ventilation systems.
However, when considering specialized areas like mental health settings, the design conversation takes on different dimensions. Historically, the design of these facilities has been primarily safety-oriented, leading to the practice of “safe wards”—a combination of physical structures and operational protocols intended to minimize the risk of self-harm and suicide. However, tThere is a growing recognition that the design of mental health facilities should balance safety features with therapeutic environments to promote well-being and recovery (Chrysikou, 2019; Lundin, 2021; Oostermeijer et al., 2021; Ulrich et al., 2018).
To contribute to this evolving discourse, this systematic literature review aimed to identify and synthesize empirical research on the use of the built environment as a therapeutic intervention in mental health inpatient facilities. Thus, the question guiding this review was as follows: What design factors of adult mental health inpatient facilities influence patient outcomes and satisfaction? This review covered a wide range of patient outcomes, such as individual experiences (e.g., emotional states, feelings of safety, and overall well-being), behavioral responses (e.g., social interaction), and direct clinical interventions (e.g., medication intake and length of stay). Additionally, the review considered safety outcomes that can indirectly be influenced by the therapeutic environment, including aggression, seclusion, self-harm, and suicide. Outcomes directly related to the physical safety of patients (i.e., falls, infections) were excluded.
Several literature reviews have made notable contributions on exploring the impact of mental health inpatient facilities on social interaction (Jovanović et al., 2020) and on seclusion and restraint (Oostermeijer et al., 2021). A literature review by Weber et al. (2022) synthesized research on relationships between physical and socio-physical environmental characteristics of inpatient mental health facilities and their effect on patient mental health, well-being, and recovery outcomes. Our review aimed to expand on this knowledge by adopting a different perspective. Unlike Weber et al. (2022), who concentrated primarily on outcomes, our review synthesized evidence based on design factors. Additionally, we included forensic facilities and Intensive Psychiatric Care Units (IPCU) within our scope. In doing so, we aimed to encompass a broader range of design influences, deepening our understanding of their effects on patient outcomes. Another distinguishing aspect of our review laid in its approach to recognizing the complex nature of research that examines the impacts of facility renovation and relocation. In such scenarios, patients experience multiple design changes, making it challenging to associate specific design interventions to specific patient outcomes due to the number of alterations introduced. This approach diverges from Weber’s methodology, which established connections between outcomes and specific design factors that were part of a multifactorial intervention involving multiple design changes. Our review took a novel approach by dedicating a section to examining these scenarios, rather than isolating specific design factors of a multifactorial intervention and associating them to specific outcomes. In the discussion and implications for practice, we identified the discernible trends and shared elements across these multifactorial interventional studies. This approach aligns with the methodology employed by Dijkstra et al. (2006) in their earlier review and highlights the continuity in research direction.
Through our review, we aimed to enhance the discourse on the role of design in mental health inpatient facilities, offering the evidence base to inform future design practices. Furthermore, this review will support the development of a quality assessment tool being produced by the Scottish Government and NHSScotland Assure, aimed at assessing the safety and therapeutic quality of mental health estates.
Method
This review was commissioned by the Scottish Government and NHSScotland Assure, who provided the research team with the review question and inclusion criteria. The review was conducted by a multidisciplinary team of two healthcare scientists, a research manager, and an architect, all with a background in the healthcare-built environment and research.
Search Strategy
Searches were conducted in five electronic databases, including CINAHL (Ebsco), Embase (Ovid), PsycINFO (Ovid), PubMed, and Web of Science from their inception up to March 10, 2022. The reference lists of all included studies were hand searched for potentially relevant articles. In addition, extensive handpicking was informed by the reference lists from studies that were identified but did not meet the inclusion criteria (e.g., systematic literature reviews and critical reviews). Search strategies were developed by the lead author (L.R.L.) and adapted to each database using a comprehensive list of search terms related to the setting, population, and intervention or phenomenon of interest. The search strategy was guided by the principal architect (S.G.) and reviewed by a librarian for accuracy (Supplementary File 1).
Eligibility Criteria
For studies to be included in the review, they had to meet the following criteria: Investigate the effect of the facility design (architecture, interior design, and ambient features) on patient outcomes. This may include clinical, behavioral, emotional/well-being, or safety outcomes that can indirectly be influenced by the therapeutic environment. Studies that report on patient experiences or perceptions of the facility design, or staff insights on the impact of the design on patient outcomes. The study is conducted in adult mental health inpatient facilities including acute and long-stay services, psychiatric intensive care units, and forensic units. The study consists of empirical research that has been peer-reviewed and is written in English.
No restriction was placed on the type of study design and country. Studies were excluded if they focused on child, adolescent, geriatric, or emergency departments or were conducted exclusively with populations diagnosed with organic mental illnesses. This is because the balance of benefits, constraints, and challenges associated with these populations might differ from the target population of this review. However, if these populations and settings were part of a more extensive sample that met our inclusion criteria, they were considered for inclusion. Studies that exclusively focused on the design of smoking areas, sensory rooms, or general inpatient settings were also excluded. Moreover, studies were ruled out if they were based on expert opinion, literature reviews, commentaries, audits, and dissertations or if they were presented as posters or abstracts at conferences.
Study Selection
A first screening (reading the title and abstract) of all the studies and a second screening (assessing the full text of eligible studies) was conducted independently by two reviewers (L.R.L. and J.K.) based on the inclusion and exclusion criteria. Disagreement between the reviewers occurred 0.05% in the first screening (n = 32 studies) and 29.09% in the second screening (n = 15 studies). A consensus meeting between reviewers resolved disagreements. A third reviewer (G.O.) made the final decision when a consensus could not be reached. For this literature review, we used the Scottish Intercollegiate Guidelines Network’s SIGN50 checklists to assess the methodological quality of the studies and adopted their evidence grading system (SIGN, 2019). However, in applying this methodology, we noticed its lack of specific criteria for qualitative and controlled pre- and post- intervention studies. Recognizing the indispensable value of these study designs in our context, we adapted the SIGN50 hierarchy to integrate qualitative research as Level 3 evidence and controlled pre- and post-intervention studies as Level 2 evidence. Adjustments to the evidence hierarchy are detailed in Supplementary File 2.
Data Extraction, Synthesis, and Integration
Data from the included studies were extracted by the lead author and included, where available, the authors, year, country, study design, sample population, number and characteristics of participants, type and characteristics of the inpatient facility, phenomenon of interest or intervention, data collection method(s), outcome measures, results, limitations identified by the authors, sources of funding, and design factor investigated or reported in the study.
Following the Joanna Briggs Institute methodology for mixed-methods review, the extracted quantitative data were transformed into qualitized data to facilitate integration with data extracted from qualitative studies (Lizarondo et al., 2020). Data were categorized based on design factors, followed by similarities in the outcomes, to produce a set of integrated findings. The criteria for incorporating findings into the synthesis included either the presence of multiple studies or a single in-depth study that offered comprehensive data. The confidence in the body of evidence that formed each finding was assessed based on the quantity of the studies, the SIGN50 level of evidence assigned to each study, the study limitations, the consistency across the studies, and the generalization of the finding. The certainty in the body of evidence for each finding was graded as either very low, low, moderate, or high.
Results
The final selection consists of 44 studies (see Figure 1), which include 19 quasi-experimental studies—of which only five involved a control group—, two randomized control trials, three retrospective cohort studies, three cross-sectional studies, two post-evaluations, and 15 qualitative studies. An overview of the characteristics of the included studies can be found in Table 1. An expanded version of the study characteristics can be found in Supplementary File 3.
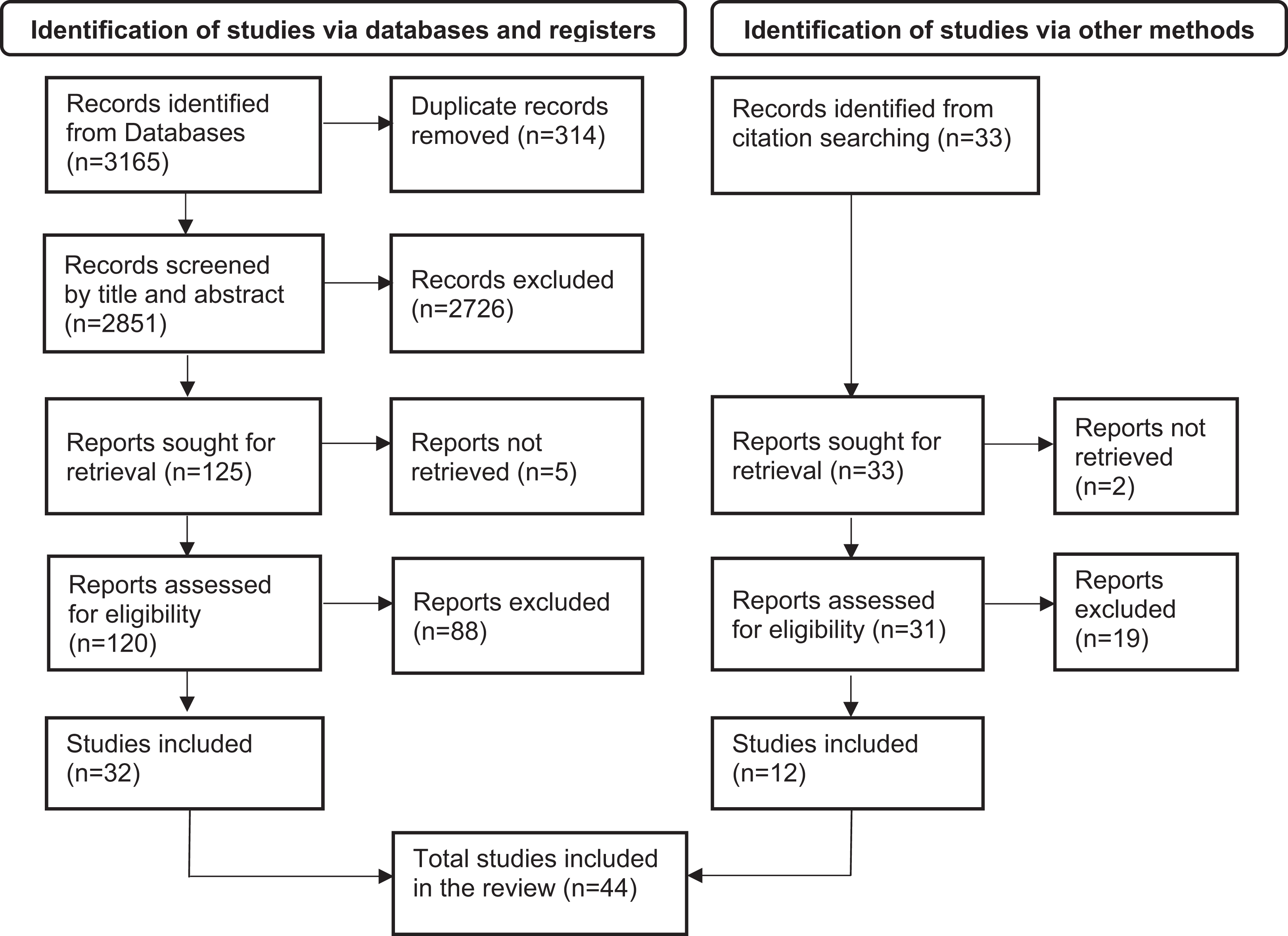
The Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) flowchart for selection process of studies in the systematic review.
Characteristics of the Included Studies.
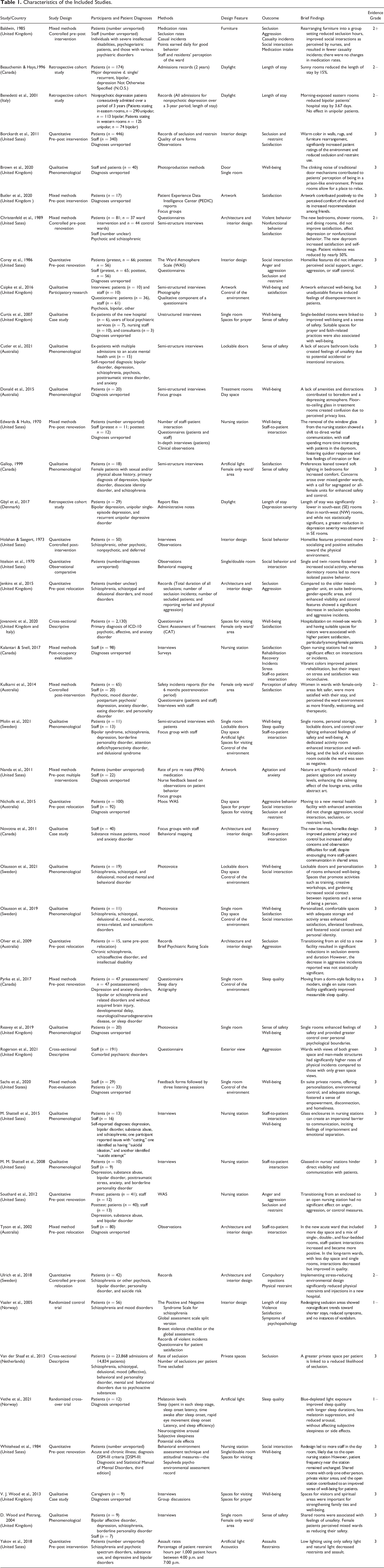
The selected studies were published between 1968 and March 2022, deriving from nine countries, including the United States (n = 13), United Kingdom (n = 10), Canada (n = 5), Australia (n = 6), Sweden (n = 4), Norway (n = 2), Netherlands (n = 1), Denmark (n = 1), Italy (n = 1), and one study conducted jointly in Italy and England (n = 1). The largest study included 14,834 participants (cross-sectional study), and the smallest study included nine participants. Of the ward-level studies, the largest study included 199 wards, and the smallest included one. Studies were conducted at acute mental health inpatient facilities (n = 13); IPCUs (n = 2); forensic inpatient settings, including high, medium, and low security (n = 8); and multiple studies involved more than one type of mental health inpatient setting (n = 4). In 21 studies, the type of adult mental health inpatient setting was unspecified. Participant diagnoses were not disclosed in 16 studies and data sample sizes were unspecified in six studies. Several studies also included data from geriatric (Baldwin, 1985; Borckardt et al., 2011), organic mental illness (Baldwin, 1985), and child and adolescent services (Borckardt et al., 2011). In one mixed-methods study, only the qualitative study was relevant for this literature review (Csipke, 2016).
Patient outcomes identified included medication intake, length of stay, quality of sleep, seclusion and restraint (physical and pharmaceutical restraint), aggression (verbal and physical aggression), violence and vandalism, social interaction and activity (staff–patient, patient–patient, and patient–visitor interaction), satisfaction with the environment, stress, agitation and anxiety, sense of safety, and well-being (e.g., feelings of being bothersome and threatening to the staff, hope, power and control, sense of integrity and self-respect, negative self-image, and prison-like and homeliness feeling).
Of the 44 studies identified, 34 directly explored the influence of design factors on patient outcomes, reported on patients’ experiences or presented staff and carers perspectives on how such design factors impact patients. The synthesis of these studies is presented first and systematically organized by design factors—ranging from patient bedrooms and communal areas to clinical spaces, interior design interventions, and ambient factors. This is followed by the findings from the remaining ten studies that focus on the processes of either transitioning patients to a new facility or refurbished one.
Patient Bedroom
When considering patient bedrooms, privacy stood out as a recurrent theme in many studies, highlighting its role in providing patients with a sense of autonomy and control over their surroundings. One particular study by Van der Schaaf et al. (2013) found that when patients have more private space, they are less likely to be secluded.
Single rooms
Looking into the specifics of bedroom configurations, a total of ten studies reported the positive impact of having single or twin rooms on patient outcomes. Ittelson et al. (1970) found increased social activity in patients staying in single and twin rooms, while dormitory rooms were characterized by more isolated passive behavior (e.g., lying on a bed from two thirds to three fourths of the time spent in their rooms). In the study by Whitehead et al. (1984), patients described that sharing a room with only one other person made them feel better compared to dormitory style. Pyrke et al. (2017) identified an improvement in sleep quality after the renovation of a facility that transitioned from dormitory-style rooms to single rooms. This renovation also incorporated a climate control system (ventilation, lights, and acoustics) as well as soundproofed walls and doors. Similarly, qualitative data indicated that single rooms contributed positively to patient well-being (Brown et al., 2020; Curtis et al., 2007; Molin et al., 2021; Olausson et al., 2019; Reavey et al., 2019; Sachs et al., 2020) and feelings of safety (Curtis et al., 2007; Molin et al., 2021; Reavey et al., 2019; D. Wood and Pistrang, 2004). In these studies, participants perceived single rooms as places for quietness and safety where they could withdraw from staff, other patients, and the overall soundscape environment.
Lockable doors
In one study, staff highlighted the importance of lockable doors in patient rooms for enhancing patients’ sense of safety (Molin et al., 2021). Similarly, patients emphasized that these doors imparted feelings of comfort and normality (Olausson et al., 2021). In addition, ex-patients in the Cutler et al. (2021) study expressed concerns about feeling unsafe in bathrooms without locks or those that could be easily opened from the outside, citing potential inadvertent or deliberate intrusions by other patients.
Control of the environment
Several studies emphasized the importance for patients to have control of the environment in their rooms. Having personally controllable room appliances and fixtures, such as windows, showers, heating, light and acoustics, was associated with a sense of empowerment (Csipke et al., 2016), well-being (Molin et al., 2021; Sachs et al., 2020), and improved sleep quality (Pyrke et al., 2017). In addition, a sense of homeliness was associated with patients having personalization over rooms (e.g., photographs, artwork, and gifts) (Olausson et al., 2019, 2021; Sachs et al., 2020), comfortable beds, and the use of personal bedding (Olausson et al., 2019, 2021). Having storage space in patient rooms was also evidenced in two studies as contributing positively to patient satisfaction (Molin et al., 2021; Sachs et al., 2020). Furthermore, lockable cabinets and private wardrobes for personal belongings were highlighted as important for patients’ perceptions of safety and control (Molin et al., 2021).
Communal Spaces
Spaces for activities, visitors, and spiritual/contemplative reflection
Several studies reported that, based on patients experiences of the physical environment, day spaces designed to promote activities increased their interaction with staff (Olausson et al., 2021; Molin et al., 2021) and reduced feelings of boredom (Donald et al., 2015; Olausson et al., 2019). Further outlining the importance of specific spaces, several studies highlighted the value of designated areas, both communal and private, for visitor meetings. These areas were associated with strengthening family ties and enhancing well-being (Jovanović et al., 2020; Molin et al., 2021; Wood et al., 2013), as well as lifting patient spirits (Whitehead et al., 1984). The provision of spiritual or contemplative areas also resonated positively with patient well-being in two studies (Curtis et al., 2007; V. J. Wood et al., 2013). By contrast, Nicholls et al. (2015) identified, based on patients’ and staff perceptions of the new “atmosphere,” no change in levels of aggression, social interaction, seclusion, and restraint after moving to a new facility that included space for prayer/reflection, recreational courtyards, multiple therapeutic spaces, and family-friendly space. However, the authors acknowledged that the results could have been influenced by the nature of the atmosphere which involves more than just the building or environment; it also requires social occupation and interactions.
Female only ward/areas
Several studies found an association between female-only areas and an enhanced sense of safety. First, a study comparing a mixed-sex ward to a similar ward comprising a female-only area identified that the latter had fewer incidents and female patients had a better experience of care, sense of safety, and satisfaction with the environment (Kulkarni et al., 2014). Similarly, in two qualitative studies, female patients perceived mixed-sex wards as reducing their safety and control (Gallop et al., 1999; D. Wood & Pistrang, 2004). They were concerned about male patients and wished for an all-female unit or a unit with segregated communal areas (Gallop et al., 1999). In addition, female patients from mixed-sex wards reported feeling vulnerable when sexually harassed or intimidated by male patients (D. Wood & Pistrang, 2004). However, due to the previous experiences of sexual and physical abuse, and/or safety trauma of the studies population sample, the generalization of these results should be treated with caution. In contrast, a recent cross-sectional study involving 2,130 patients from 18 acute mental health hospitals with mixed-sex and single-sex wards found that hospitalization in a mixed-sex ward was associated with higher patient treatment satisfaction. Interestingly, compared to male patients, for whom the effect of the type of wards was marginal, females reported higher satisfaction with mixed-sex wards (Jovanović et al., 2020).
Clinical Spaces
Nursing station
Changes in the configuration of nursing stations, transitioning from traditionally glass-enclosed nursing stations to more open designs, have been associated with improved patient–staff interactions and communication (Edwards & Hults, 1970; M. Shattell et al., 2015; M. M. Shattell et al., 2008), as well as well-being (Whitehead et al., 1984). Two studies observed that staff spent more time in the dayroom when the nursing station glass was removed (Edwards & Hults, 1970; Whitehead et al., 1984). Additionally, patients reported feeling less bothersome and threatening to the staff. They also expressed a greater sense of power and control in their interactions with nursing station staff, coupled with feelings of freedom as opposed to sensations of imprisonment and confinement (Edwards & Hults, 1970; M. Shattell et al., 2015).
In contrast, a post-occupancy evaluation by Kalantari and Snell (2017) that included only staff, found that open nursing stations did not enhance patient satisfaction, rehabilitation, or staff–patient interactions without compromising safety or reducing the number of incidents between patients. However, the results from this study should be interpreted with caution due to potential staff bias in their perception of the safety offered. Southard et al. (2012) found no statistically significant difference in patient therapeutic milieu when comparing the nursing station before and after removing the glass enclosure. They also recorded no perceived increase in patient anger or aggression toward staff.
Treatment rooms
As well as privacy in bedrooms and bathrooms, ensuring privacy in treatment rooms was identified as contributing positively to patient well-being. In the study by Donald et al. (2015), treatment rooms with floor-to-ceiling glass, observable from the rest of the unit, were perceived by patients as confusing. Essentially, a space they considered to be “private” became visible to others.
Interior Design Interventions
Furniture/seating arrangements
Only one study purposely investigated the effects of changes in furniture and seating arrangements as a single intervention. Baldwin (1985) found that rearranging ward furniture from non-social patterns into group seating arrangements in the dayroom—three or more chairs facing within three feet radius of the table—contributed to reducing the number of hours of seclusion and the number of casualty incidents. However, no changes in medication rate were observed.
Artwork and color
This review included three studies that identified the positive effect of artwork on patients. Nanda et al. (2011) found that the presence of realistic nature, abstract-representational, and abstract art led to a reduction in the average daily medication required, compared to days without it. Notably, this effect was more pronounced for realistic nature art than for abstract-representational or abstract art. Nurses also expressed that nature art had a calming effect on patients compared to the abstract art, which was described as irritating, or even headache-inducing. In Butler et al. (2020), participants reported increased satisfaction with the physical environment when nature and abstract-related wall paintings—created by professional artists with input from patients—were displayed in the IPCU. Csipke et al. (2016) reported that patients described the artwork as “brightening up” the ward and enhancing their sense of well-being.
Regarding color, an interventional study by Kalantari and Snell (2017) used different color tones across the unit—vibrant and saturated in treatment areas and warmer and more soothing colors in communal areas and bedrooms. While no association was found between the color and patient satisfaction or stress—as perceived by staff—the study concluded that the color scheme improved patient recovery and rehabilitation.
Ambient Features
Acoustic environment
Two studies reported the effects of various acoustic environmental features on patient outcomes. Brown et al. (2020) found that certain door design features, such as the use of traditional mechanical cylinders—evident from the clinking of keys carried by staff—were perceived by patients as evoking feelings of being in prison. These feelings were further exacerbated by the spatial layout, characterized by high ceilings and large open spaces. On the other hand, Yakov et al. (2018) assessed the impact of minimizing noise from staff and patients, combined with soft music in lieu of television, and introducing live therapeutic music on rates of assaults and restraint. Although there was a reduction in those outcomes, the study could not conclusively attribute these results to the noise reduction interventions as they were implemented concurrently with a low-lighting intervention. Nonetheless, when considering both interventions together, the study observed a significant 72% reduction in assaults and restrains 11 months post-implementation.
Artificial light
A longitudinal, pre- and post-intervention study found that low lighting, using only safety and natural lighting in the day room, was positively associated with a reduction in assault and restraint rates during the evening hours compared to the baseline period (Yakov et al., 2018). Similarly, Gallop et al. (1999) found that patients favored soft lights in their bedrooms for increased comfort, compared to the staff’s standard use of flashlights for routine checks and nighttime visibility. In another study, the lighting—termed “healing lights”—in bedrooms of a new facility were perceived by nurses to enhance patient sleep quality and relaxation (Molin et al., 2021).
Lastly, a randomized crossover trial involving 12 patients showed that a blue-depleted light environment, applied in the evening from 06:30 pm to 06:50 am in bedrooms, bathrooms, hallways, and common areas, improved sleep quality— the total sleep time was 8.1 minutes longer compared to the control. However, the sample might not resemble all patients as some left the ward from 08:00 to 05:00 pm and could have been exposed to higher lights levels during the day (Vethe et al., 2021).
Daylight
Three retrospective cohort studies showed the positive effect of bright and sunny rooms on the length of stay of patients experiencing a depressive phase of bipolar disorder. However, this impact was unclear for unipolar depressive patients. Beauchemin and Hays (1996) identified that patients with depression who stayed in brighter, sunnier rooms (reaching up to 50,000 lux on a bright day) had a 2.6 day shorter length of stay than those in dull rooms (with a maximum of 3,000 lux). More recently, Gbyl et al. (2017) identified that patients with a depressive phase, either as part of a unipolar or bipolar disorder, had a shorter average length of stay of 29.6 days when accommodated in rooms receiving more direct natural light (facing southeast with up to 60,000 lux) compared to a control group in rooms facing northwest (maximum of 3,000 lux). Similarly, the study by Benedetti et al. (2001) involving 602 unipolar and bipolar patients reported a 3.67-day shorter length of stay for depressed patients with bipolar affective disorder staying in eastern rooms (receiving direct sunlight in the morning) compared with those in western rooms (direct sunlight in the evening). This study, however, did not note a sunlight effect on the length of stay for unipolar depression, a finding that contrasts with Gbyl et al. (2017). Given their design, these studies have limitations that might imply a lack of causality for the observed difference in the length of stay. For instance, factors such as the time patients spent in their rooms, how often curtains were opened or closed, variations in pharmacological regimes, or illness severity, were not reported in any of these studies.
Outside view
This review included only one study examining the impact of the content of the view from the room window on patients. Rogerson et al. (2021) conducted a cross-sectional study across 101 wards and identified higher aggressive behavior in wards that offered a view of both nature and man-made structures compared to a view exclusively of nature. Nonetheless, the findings of this study should be treated with caution, given that survey responses were unevenly distributed across all wards. Additionally, the study did not account for certain variables that might influence aggression, such as the addition of extra staff to facilitate observations.
Multifactorial Interventions
Interior design
In four studies, modifications to the interior design that provide a more home-like environment, such as warm wall colors, a wall and door painted with bright solid colors, placement of decorative throw rugs, plants, and modern furniture, and seating arrangements for small group interactions, were found to have an impact on patient outcomes. For example, Borckardt et al. (2011) found, when compared to the previous facility design, a reduction in the use of seclusion and restraint along with an increase in patients’ satisfaction with the new physical environment. Similarly, Holahan and Saegert (1973) identified enhanced social interaction, patient satisfaction, and less isolated passive behavior in a renovated ward compared to a nonrenovated one. Vaaler et al. (2005), when comparing a traditional design seclusion area with another that was identically structured but redecorated to mimic a home-like environment, identified that the latter reduced vandalism and increased patient satisfaction, especially in women. There was no substantial effect on symptoms of psychopathology or length of stay. In contrast, Corey et al. (1986), using the Ward Atmosphere Scale (WAS) to assess how staff and patients perceived the inclusion of home-like features before and after the redesign of a mental health facility, did not find an impact on perceived social support (functional measure of social interaction), anger and aggressive behavior, or staff control (functional measure of seclusion and restraint).
Interior design and architectural features
This review included six studies that explored the impact of the renovation of an existing facility or the relocation to a new purpose-built unit or hospital involving simultaneous alterations in both the design and architecture. In the study by Jenkins et al. (2015), the relocation to a new IPCU that included en-suite bedrooms, gender-specific areas, a layout that enabled higher visibility, control of the environment, spaces for activities, and lockable toilets, led to decreased aggressive incidents and the number and total duration of seclusion episodes, compared to the old ward. Similarly, in a study by Ulrich et al. (2008), a comparison between the old and control facility and a new facility incorporating enhanced stress-reducing environmental features (e.g. privacy, control, visibility, natural light, art and communal areas) revealed a decrease of 6.8% in patients receiving injections (pharmaceutical restraints) after the transition. However, there were no differences for patients who required physical restraints. Although, the number of physical restraints for patients who received at least one type of restraint decreased by 50%.
Christenfeld et al. (1989), involving pre- and post-assessments of four control and two experimental wards, found that extensive design changes in the day room, and the transition to an open nursing station, led to a 50% reduction in violent episodes. The study did not find a difference in nonfunctional behavior between renovated and control wards. In addition, patients reported greatest satisfaction and an improvement in self-image with the renovated dayroom. Similarly, the findings from Tyson et al. (2002) implied that increased day space enhanced staff-patient interaction, yet due to other changes accompanying the relocation, these results should be interpreted with caution. Olver et al. (2009) reported that the relocation to a new purpose-built secure unit that included more indoor and outdoor recreational areas, single rooms and access to more daylight, led to a reduction in the number of seclusion events and seclusion episodes exceeding 4 hr. However, the study did not find a reduction of aggressive incidents as perceived by staff. Novotná et al. (2011) identified that the new low-rise, homelike design not only improved privacy and control for the patients, but also increased safety concerns and observation difficulties for staff. In addition, behavior mapping activities on the units revealed increased staff–patient communication, occurring primarily in the patients lounges, adjacent kitchens, and lobby areas.
Discussion
This review included 44 studies where the impact of different factors of the facility design on patient outcomes were investigated or reported based on patient, staff, or carer experiences of the physical environment. This number differs from a similar literature review conducted by Weber et al. (2022), which included 26 studies. The difference in the quantity of included studies could be attributed to our broader inclusion criteria. For example, unlike Weber’s literature review, we included research from forensic units and studies using the WAS. We also included five studies—excluding those from forensic settings—published between the end date of Weber’s search (September 2020) and ours (March 2022). In contrast, our review excluded studies focusing solely on organizational factors like open/locked wards. Although they play a significant role in mental health inpatient settings, we chose not to include these in the review based on our consideration that they are more related to organizational procedures than to the physical design itself, and hence would require a separate comprehensive literature review. Despite the larger quantity of studies included, our review echoes Weber’s in acknowledging the difficulties and complexities of conducting research in these environments.
Delving into our results, several findings emerged from the literature review that can guide future design efforts to contribute to the therapeutic environment and inform best practice. To provide a concise overview, we compiled a summary table to outline the findings, along with their confidence levels and recommendations for practice (see Table 2). First, our review found evidence suggesting that incorporating a more home-like environment into mental health wards could minimize the institutional feel and enhance comfort and satisfaction. Specific changes might include incorporating plants, selecting comforting colors for walls, or modern furniture that make the space feel more like a home than a clinical setting. The provision of private spaces, specifically single-bedded rooms, and enabling control of the environment, such as ventilation, lighting, acoustics, and personalization of rooms, emerged as other crucial design factors. They were found to enhance feelings of safety, well-being, and sleep quality, pointing to designs that focus on patient privacy and environmental control. Such insights align with Paopulas et al. (2014), whose review synthesis identified the provision of home-like designs and private spaces to be associated with decreased vandalism and violence, and increased social interaction.
Confidence Level and Recommendations for Practice
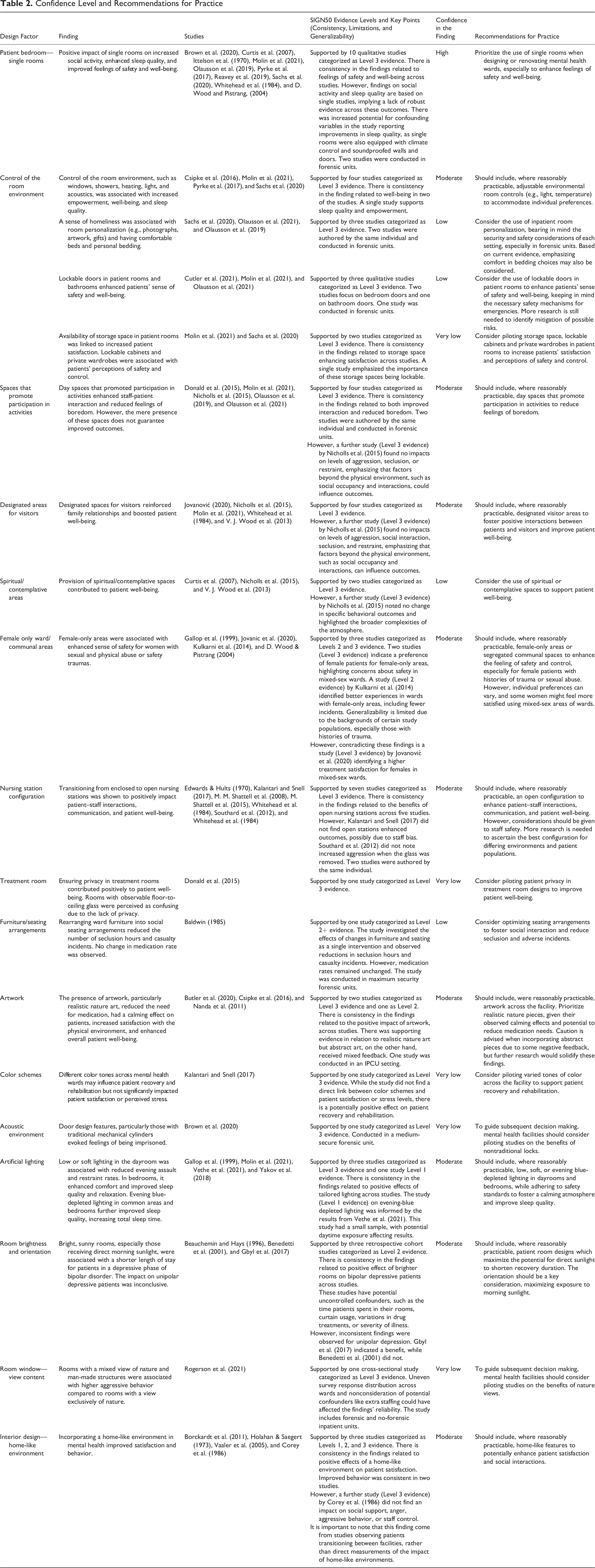
Communal spaces designed to promote interaction and activity was also a common theme, emphasizing their role in reducing feelings of isolation and boredom, and contributing to improved overall well-being. Additionally, the need for dedicated family visitation areas and spaces for spiritual/contemplative practices came to the fore, associated with improved well-being, indicating the importance of incorporating these spaces into facility designs. The provision of spaces for females, especially those who have experienced past trauma, was deemed valuable, suggesting a need for gender-focused areas or wards to enhance their feeling of safety and well-being. Our findings revealed a preference among patients for open nursing stations, as they tend to foster improved staff–patient interactions and better communication, leading to a more collaborative care atmosphere. However, while open configurations have their merits, staff safety and specific environmental factors must be taken into account. More research is essential to determine the best nursing station configuration, considering varying environments and patient populations.
Daylight emerged as a pivotal design consideration, particularly for patients during depressive episodes of bipolar disorder. Room designs that maximize daylight intake was found to positively influence their recovery. Lastly, the integration of artwork, especially those depicting nature, emerged as a positive design strategy throughout our review. Such aesthetic integrations were correlated with reduced stress levels and heightened patient satisfaction. However, it is worth noting the nuances in selecting artwork, in particular, abstract artwork. This was found by Salonen et al. (2013) to have potential negative implications for patients in general healthcare facilities. In line with these insights, our recommendations urge practitioners to exercise caution when opting for abstract art pieces. Yet, it is essential to acknowledge that further research is required to provide a more definitive stance on this observation.
Contrary to our initial expectations, the available body of evidence did not offer an exhaustive exploration of the topic. For certain design factors, we identified only one single study highlighting its importance. While this does not undermine the potential significance of these elements, it does prevent us in forming robust, evidence-based recommendations. Yet, these factors have been recommended in evidence synthesis for general facilities. For instance, Ulrich et al. (2008) presented compelling evidence that views of nature can alleviate patient pain and stress, and that access to daylight and proper lighting can mitigate depression. Furthermore, while certain factors have not been studied or reported for mental health facilities, there is growing evidence from general healthcare facilities. For example, evidence synthesis has shown the positive effect of an appropriate thermal environment and exposure to natural elements on well-being (Iyendo et al., 2016; Salonen et al., 2013). While we have provided preliminary insights and recommendations based on the current literature, it is evident that more research is essential to fully comprehend and underscore all design factors that can contribute to the therapeutic environment of mental health facilities. Furthermore, it is vital to note that the recommendations provided should be adapted to the specific constraints and requirements of individual settings and patient populations for the most effective implementation.
Limitations and Future Research
We acknowledge that the review findings are rooted in studies that presented some methodological limitations. For example, most of the pre- and post-intervention studies lacked control groups or did not match the intervention wards, neither did they included controls for possible confounding factors such as changes in organizational procedures, management protocols, treatment methods, or changes in the staff's mood level. Furthermore, several studies used small convenience samples that limited the generalization of findings, and often participants were different pre- and post-intervention. However, we recognize that the transient nature of these populations means that it is almost inevitable that participants will change over time. Other limitations are related to the methodological quality of qualitative studies such as lack of triangulation and reflexibility. Additionally, the quality of the responses in some studies could have been influenced by factors such as the passage of time, the benefit of hindsight, or possibly by several social and cultural factors. Future research should address these limitations.
Moreover, the limitations extend to the methods of our review. We solely focused on empirical, peer-reviewed studies in English, thus excluding valuable insights from gray literature and non-English research. Additionally, we noticed that some studies used a general label, “adult inpatient psychiatric settings,” which might include other types of settings not specifically part of our research criteria. However, we believe that the information we obtained from these studies is significant and contributed positively to the review. For the future, we encourage researchers to specify the type of mental health setting they are studying. This extra detail will greatly help future reviews to categorize and understand the research more effectively.
During our review, we encountered difficulties in the effective application of the SIGN50 methodology (SIGN50, 2019). This primarily arose because the study designs frequently observed in this specific research domain, such as controlled pre- and post- intervention studies or qualitative studies, are not fully addressed by SIGN50. This highlights the need for alternative methodologies better tailor to assess the methodological quality inherent to the typical study designs in this area.
While our systematic review aimed to highlight the impact of individual design factors on patient outcomes, it is crucial to recognize an inherent limitation in isolating these factors in interventional studies that involved multiple design changes. Future research might consider conducting controlled studies that manipulate one design feature at a time to provide a clearer understanding of their individual impacts.
Conclusions
This systematic literature review examined the existing body of published literature on the topic and shed light on the gaps in knowledge. Although the studies included in this review have limitations, initial findings suggest various design factors that should be considered when designing or renovating a facility to enhance its contribution to the therapeutic environment. These encompass (1) patients’ personal space designed to emphasize privacy and control of the environment; (2) spaces designed to optimize daylight exposure; (3) flexible communal areas promoting activities, socialization, and designated areas for visits and spiritual reflection; (4) environments that evoke a home-like feeling, minimizing the institutional aura; (5) the inclusion of artwork across the unit; (6) open designs for nursing stations; and (7) dedicated female-only areas or wards. Future research is still needed to provide more robust evidence-based designs that align with the therapeutic and clinical environment.
Implications for Practice
The current body of literature provides an indication of how the built environment of mental health inpatient settings can be used as a therapeutic intervention for patients.
Based on research conducted in inpatient mental health settings, practitioners can identify and implement design factors that contribute positively to patient outcomes to produce evidence-based designs, tools, guidance, and policies.
Several gaps in the evidence and limitations are identified, providing avenues for further investigation in this area.
Supplemental Material
Supplemental Material, sj-pdf-1-her-10.1177_19375867231219031 - The Role of the Built Environment as a Therapeutic Intervention in Mental Health Facilities: A Systematic Literature Review
Supplemental Material, sj-pdf-1-her-10.1177_19375867231219031 for The Role of the Built Environment as a Therapeutic Intervention in Mental Health Facilities: A Systematic Literature Review by Laura Rodríguez-Labajos, Joanne Kinloch, Susan Grant and Geraldine O’Brien in HERD: Health Environments Research & Design Journal
Supplemental Material
Supplemental Material, sj-pdf-2-her-10.1177_19375867231219031 - The Role of the Built Environment as a Therapeutic Intervention in Mental Health Facilities: A Systematic Literature Review
Supplemental Material, sj-pdf-2-her-10.1177_19375867231219031 for The Role of the Built Environment as a Therapeutic Intervention in Mental Health Facilities: A Systematic Literature Review by Laura Rodríguez-Labajos, Joanne Kinloch, Susan Grant and Geraldine O’Brien in HERD: Health Environments Research & Design Journal
Supplemental Material
Supplemental Material, sj-pdf-3-her-10.1177_19375867231219031 - The Role of the Built Environment as a Therapeutic Intervention in Mental Health Facilities: A Systematic Literature Review
Supplemental Material, sj-pdf-3-her-10.1177_19375867231219031 for The Role of the Built Environment as a Therapeutic Intervention in Mental Health Facilities: A Systematic Literature Review by Laura Rodríguez-Labajos, Joanne Kinloch, Susan Grant and Geraldine O’Brien in HERD: Health Environments Research & Design Journal
Footnotes
Acknowledgments
The authors would like to thank the librarians at Public Health Scotland and the Scottish Government and NHSScotland Mental Health Built Environment Short Life Working Group for their support with the study.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Supplemental Material
The supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
