Abstract
Underserved population, specifically immigrants with limited English proficiency (LEP), often do not receive equitable, high-quality healthcare. There is a lack of understanding regarding physicians’ perspectives on treating this population. This study describes the perspectives of primary care providers (PCPs) in the United States (US) on the challenges of treating LEP patients and identifies ways to improve the healthcare system to better meet the needs of this population. We conducted semi-structured interviews with 20 PCPs across the US and analyzed the data using grounded theory methodology. Three main themes emerged from the data: (1) challenges faced by healthcare providers in treating LEP patients, (2) strategies adopted by physicians over years of practice, and (3) practical recommendations for improving the current healthcare system to better serve LEP patients and deliver higher-quality care. Implementing patient–provider language-matching systems could significantly improve the care experience for LEP patients.
Quality of care is a multifaceted concept that encompasses the effectiveness, safety, and patient-centeredness of health services (Campbell, Roland, and Buetow 2000). Despite progress in increasing access to healthcare, quality remains a significant challenge in the United States (US) (Hanefeld, Powell-Jackson, and Balabanova 2017). Addressing quality issues requires a comprehensive approach that considers the complex interplay of factors influencing healthcare delivery (Hanefeld et al. 2017).
Underserved populations generally receive lower quality care, defined here in line with the Centers for Medicare & Medicaid Services (CMS) as “the degree to which health services for individuals and populations increase the likelihood of desired health outcomes and are consistent with current professional knowledge” (CMS 2024). In this context, quality encompasses both clinical effectiveness (e.g., accurate diagnosis, adherence to evidence-based guidelines) and interpersonal processes (e.g., culturally and linguistically appropriate communication, respect for patient preferences). For example, Elk et al. (2018) conducted a systematic literature review on palliative care for cancer patients and found that underserved and minority patients receive a lower quality of palliative care (Elk et al. 2018). Similarly, Fernandez and Becker (2017) found that underserved women experience healthcare disparities and lower quality of care in the US for services related to cervical or breast cancer (Fernandez and Becker 2017).
The underserved population includes immigrant populations and people with limited English proficiency (LEP). Currently, more than 22 million individuals with LEP reside in the US (Ramirez et al. 2023), a figure that fluctuates with shifts in immigration trends and policy changes under different administrations. LEP individuals will likely encounter the healthcare system—particularly through primary care physicians (PCPs)—at some point while living in the US (Buckman et al. 2020). These policy shifts, combined with existing health system barriers, underscore the need for culturally and linguistically appropriate care to reduce disparities.
Primary care serves as the initial point of contact for most patients, providing evaluation, assessment, and ongoing care across age groups and a wide spectrum of medical issues (Kroenke 2004). PCPs, including family doctors, pediatricians, and internal medicine specialists, play a pivotal role in delivering continuous, coordinated care that builds long-term relationships with patients (Detz, López, and Sarkar 2013). This continuity fosters trust, supports chronic disease management, and improves health outcomes through personalized care plans (Detz et al. 2013). However, with the growing number of LEP patients, communication barriers in primary care settings have become a significant challenge, affecting the quality of care and the doctor-patient relationship (Ramirez et al. 2023).
While federal law, including the civil rights provisions of the Affordable Care Act and Title VI, mandates that healthcare providers receiving federal funding ensure equal access for LEP patients (Chen, Youdelman, and Brooks 2007), many LEP patients remain dissatisfied with interpreter services, citing poor communication and lower quality of care (Flores 2005). Additionally, physicians often rely on ad hoc translators, such as family members or staff, to save time, further complicating the communication process (Paradise et al. 2019).
Michalec et al. (2015) conducted a qualitative study involving five focus group sessions with both medical interpreters and healthcare providers to examine the challenges faced by patients with LEP within obstetrical and neonatal services. Their findings highlighted that healthcare providers recognized the value of professional medical interpreters in facilitating communication and improving the quality of care (Michalec et al. 2015). However, the study also identified institutional- and individual-level barriers to the consistent use of qualified interpreters, whether in-person or via telephonic services. While this study sheds light on broader systemic challenges, its limitations include a narrow focus on obstetrical and neonatal services, excluding providers from other specialties and diverse healthcare settings.
Similarly, Gadon, Balch, and Jacobs (2007) conducted a focus group study within a small private practice, including PCPs, specialists, and practice managers. They found that physicians often relied on family members and friends as interpreters rather than professional services (Gadon, Balch, and Jacobs 2007). However, this study was limited by its small sample size and its focus on a single private practice in the US, reducing the generalizability of its findings. Additionally, the study did not account for the availability of existing language translation services within the practice, which could have influenced physicians’ reliance on ad-hoc interpreters.
Parsons et al. (2014) conducted a qualitative study based on interviews with 22 physicians practicing in a large, inner-city teaching hospital in Toronto, Canada. Their findings indicated that physicians navigating language discordance made decisions to either “get by” or “get help” based on factors such as time constraints, patient acuity, and ease of access to translation services. These decisions often created ethical dilemmas related to ideal practice, responsibility, and informed consent (Parsons et al. 2014). While this study provided valuable insight into physicians’ perspectives on treating LEP patients, it was limited to a single-site study with participants from only two medical specialties. Furthermore, data collection occurred in 2009, making some of its findings potentially less relevant today due to technological advancements and the increased availability of third-party translation services.
A recent study by Quigley et al. (2025) examined provider perspectives on delivering in-person care to Spanish-preferring patients. They found that both language-concordant providers and those using interpreters preferred direct communication in the same language as the patient. Providers employed varying communication strategies and reported needing more time to care for Spanish-preferring patients for different reasons (Quigley et al. 2025). However, this study only considered Spanish-speaking patients, limiting its applicability to LEP populations speaking other languages.
Folsom et al. (2025) conducted a national survey through the Society of Gynecologic Oncology database between November and December 2023, finding that providers reported increased stress and a lack of time when caring for LEP patients. A notable portion of respondents (39 percent) were fluent in languages other than English, which could have skewed results if those languages were prevalent among their patient population. Additionally, most respondents worked in urban academic centers, meaning the findings primarily reflect higher-resource institutions. The survey also covered only a few major topics related to LEP patient care, limiting the depth of insight into provider challenges (Folsom et al. 2025).
These studies collectively highlight the persistent challenges physicians face in treating LEP patients, including reliance on ad-hoc interpreters, barriers to professional interpreter use, and ethical dilemmas in communication. However, their limitations—such as narrow specialty focus, single-site studies, small sample sizes, and limited generalizability—underscore the need for further research.
To the best of our knowledge, there are not enough studies exploring and describing the challenges faced by PCPs and the strategies they use when encountering patients with LEP. Therefore, this study aims to address this gap by examining the experiences of PCPs in treating LEP patients. Specifically, we seek to explore the following research questions: (1) How do PCPs describe the challenges they encounter when providing care to LEP patients? (2) What strategies do PCPs employ to overcome language and cultural barriers in delivering care? (3) What recommendations do PCPs propose to improve healthcare systems in order to enhance care for LEP patients? Insights gained from this research will shed light on the barriers PCPs face in providing care for LEP patients and inform policy development to improve the quality of care in healthcare settings.
Methods
To understand the perspectives of PCPs on treating patients with LEP, we conducted a qualitative study using grounded theory methodology involving PCPs from various states across the US. This approach enables us to understand the meanings that social actors assign to their lived experiences (Lincoln and Guba 1985). Moreover, it allows researchers to “move beyond preconceived notions of what phenomena mean in a particular setting” (Bartunek and Seo 2002).
Participants
We employed a purposeful sampling approach (Patton 1990) and applied the following criteria: (1) being a PCP and (2) working within public or private practices in the US. Purposeful sampling was selected for this study to ensure the inclusion of physicians with direct experience providing care to patients with LEP, as they could offer rich, relevant insights aligned with our research objectives. While theoretical sampling is traditionally employed in grounded theory to guide data collection based on emerging concepts, our study context required identifying participants in advance to capture a broad range of perspectives across specialties, settings, and levels of experience. This approach allowed us to gather diverse, information-rich cases at the outset, which were then analyzed using grounded theory principles, including constant comparison, to refine and integrate categories as the analysis progressed. The participants were screened for inclusion criteria before scheduling their interview time. Participants were exposed to the study flyer before attending the interview sessions. They were aware that the first author is a researcher, and the second author is a physician.
Data Collection
Upon receiving ethics approval, we began recruiting participants through our personal and professional networks. We also asked each participant if they would be willing to distribute our recruitment flyers within their own professional networks. The semi-structured interviews, each lasting 60 to 90 minutes, were conducted with participants via a secure online video-conferencing application. All interviews were recorded with the participants’ permission. During the interviews, we asked participants to describe their lived experiences, routines, challenges, and strategies relevant to treating LEP patients. At the end of each interview, we asked each participant to describe their experience of treating LEP patients in one sentence (Table 1). As data collection and preliminary analysis progressed, certain interview questions were refined or expanded to explore emerging concepts and clarify developing categories, in keeping with grounded theory’s iterative approach. The first author conducted the interviews.
Direct Quotes from Some of the Participants.

Data collection took place between June 2024 and September 2024. Throughout the process, the lead author reviewed the recordings immediately after each interview to monitor consistency across the data. New data were compared with previously collected data to identify emerging insights. After interviewing the 18th physician, we observed that no new codes were emerging from the data. To confirm data saturation, we conducted and analyzed interviews with two additional physicians, resulting in a total of 20 participants. Two participants could not make it to the scheduled interviews due to schedule conflicts and other personal commitments.
Data Analysis
We transcribed all interviews, yielding 660 pages of text. During a reflective group discussion, the authors agreed that a prominent pattern regarding the management of strategies had emerged collectively during data collection. An excel file was used to analyze the data. Consequently, we decided to focus on “treating LEP patients” as the overarching lens for our analysis, while remaining open to new observations from the data. Data collection and analysis were conducted concurrently, following the grounded theory approach described by Strauss and Corbin (1990). We employed the constant comparison method to analyze interviews as they were collected, comparing new data with existing codes and categories to refine, merge, or expand them as appropriate. Insights from ongoing analysis informed the focus of subsequent interviews, enabling a deeper exploration of emerging categories and their interrelationships (Strauss and Corbin 1990).
Using grounded theory methodology, our data analysis unfolded in three stages. We employed the constant comparison method to compare newly emerging categories with those identified earlier, refining and integrating them as the analysis progressed (Strauss and Corbin 1990). During the first stage (open coding), each of the authors open-coded the data from interviews with 20 physicians practicing in internal, pediatric, and family medicine; this involved reading the transcriptions and assigning labels to specific units of text to capture their meaning (Charmaz 2014). For example, if a physician stated, “It’s that they don’t have time,” we coded this as “lack of time.” Similarly, for the quote as “Sometimes these patients don’t want to trust us and think we are outsiders,” we assigned the open code of “lack of trust.”
During axial coding, we compiled the initial codes that pertained to treating patients with LEP. We then segregated codes relating to the same content into categories, while constantly comparing them with each other (Lincoln and Guba 1985). This process led to 712 codes and 12 categories. Constructing categories is a highly inductive process (Merriam and Tisdell 2015); therefore, our research team discussed the categories and their meanings many times, and sometimes re-labeled or merged them. For example, labels such as “lack of time,” “schedule conflict,” “booked up,” and “full schedule” were categorized under the broader theme of “lack of adequate time in scheduling.” We ensured saturation of our categories when no new properties of the category emerged during data analysis (Charmaz 2014). The following steps were adopted from Beigi et al. (2024) and were used to calculate the data saturation ratio:
Step 1: Find the number of unique categories for the set.
We reviewed the last three interviews and summed the number of unique categories identified. This total (3) was used as the denominator to calculate the saturation ratio
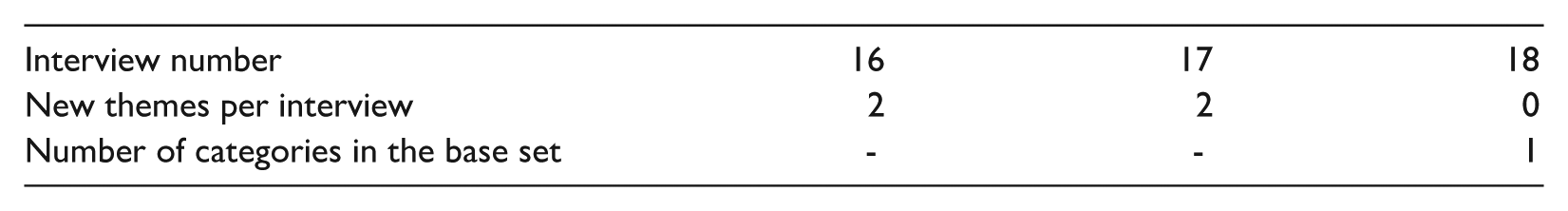
Step 2: Find the number of unique categories in the run.
We utilized a set of two and analyzed data from two more interviews. Upon reviewing these additional interviews, we found no new categories in this set.
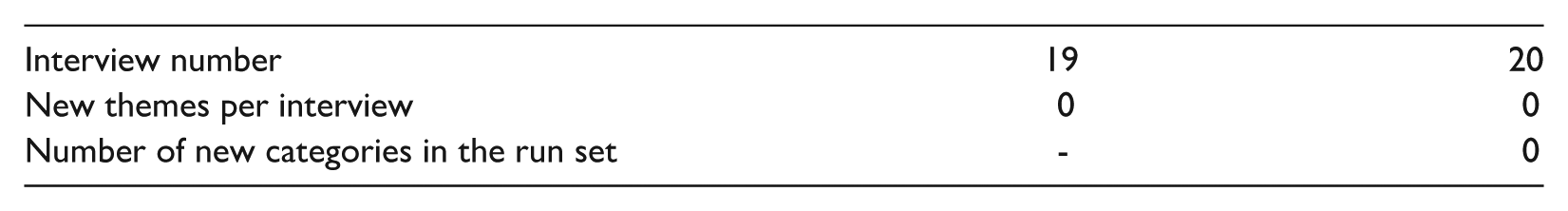
Step 3: Calculate the saturation ratio.
We calculated the ratio of new categories in the run set to the unique categories in the base set. The result was 0 percent, which is below the threshold of 5 percent, indicating that saturation had been adequately achieved.
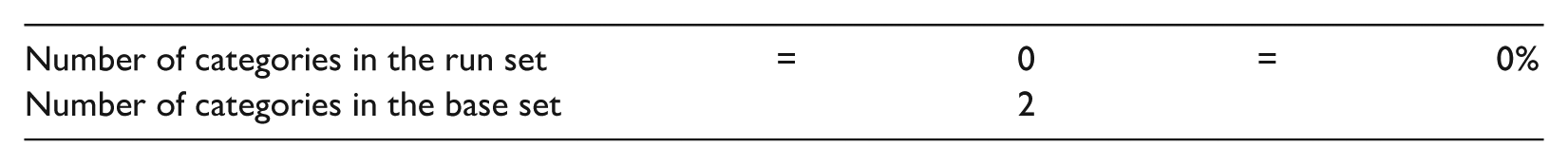
In the final stage (selective coding), the first author coded all the transcripts while keeping in mind the categories and codes generated in previous stages. The second author then reviewed all the codes. In cases of disagreement, the two authors discussed the codes until they reached a final decision. To perform an inter-rater reliability test, a qualitative colleague was invited to code 70 quotations from interview transcripts separately, and the data reached 90-percent agreement. Throughout the analysis process, the authors kept a shared journal in which they iteratively and collaboratively explored the relationships between the emergent categories and organized the findings into a model (Figure 1). Although the analytic process was guided by grounded theory methodology, the aim of this study was not to construct a formal, generalizable theory. Instead, our analysis generated a substantive, context-specific framework grounded in the data. Using constant comparison and iterative refinement, we integrated the emergent categories into a conceptual figure that visually depicts the relationships among them and situates the findings within the context of physicians’ perspectives on caring for patients with LEP. Figure 1 serves as an integrative representation of our results, providing a visual synthesis that links the study’s categories and highlights their interconnectedness in practice.
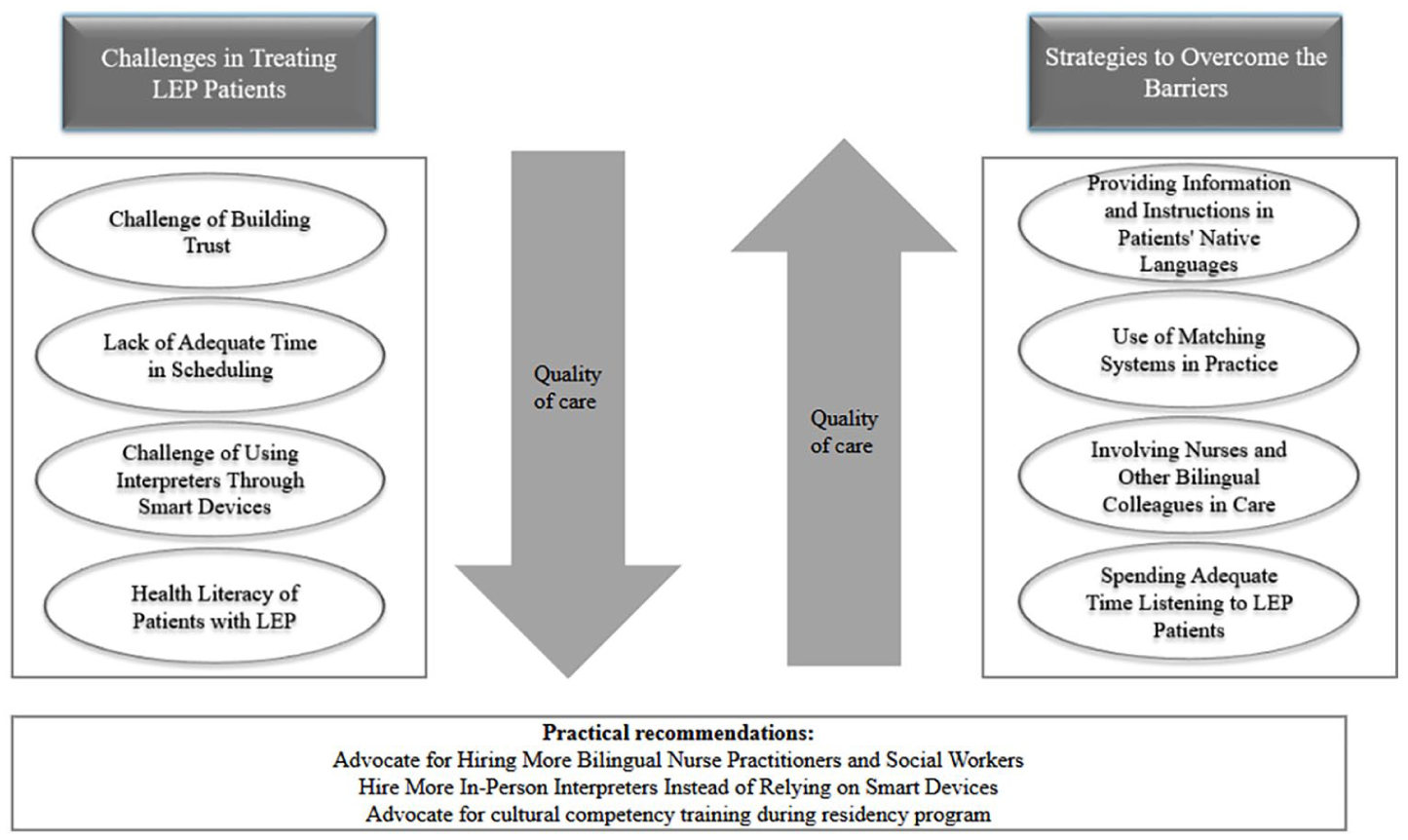
Summary of findings.
Trustworthiness
The first author is a qualitative researcher specializing in the healthcare experiences of individuals with LEP. As a first-generation immigrant, she brings both scholarly expertise and lived experience to this study. The second author, an international graduate and physician with training in qualitative research analysis, is bilingual and has firsthand knowledge of the challenges LEP individuals encounter in navigating an English-dominant healthcare system. Both authors have personally witnessed the struggles of their loved ones in accessing and understanding healthcare services due to language barriers. These perspectives enrich the study’s analysis, and readers are encouraged to consider them in interpreting the findings.
Results
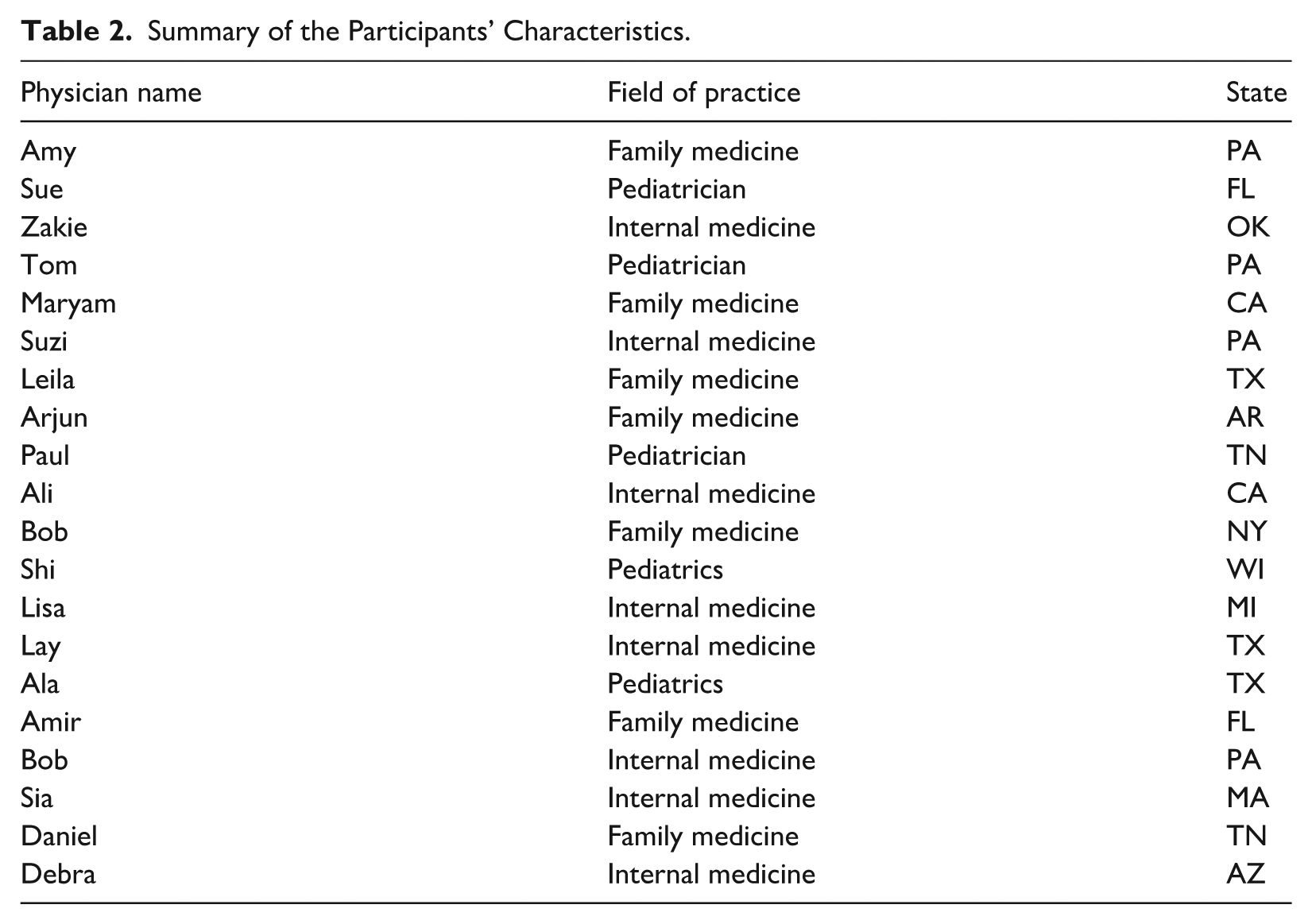
Thirty-five percent of our participants practiced family medicine, 25 percent were pediatricians, and 40 percent were internal medicine physicians. Seventy-five percent of participants could speak fluently in at least one language other than English. Additionally, 45 percent of participants were female. The majority of participants were practicing in Pennsylvania, Florida, or California at the time of the interviews (Table 2). Below, we discuss the categories that emerged from the data, supported by direct quotations.
Summary of the Participants’ Characteristics.
Challenges of Treating Patients with LEP
Lack of adequate time in scheduling
All participants, without exception, identified the lack of adequate time for treating patients with LEP as a significant barrier to providing quality care. Their busy schedules left them with insufficient time to spend with LEP patients and fully address their concerns. Su, a pediatrician in private practice in Florida, explained, “For physicians, it’s not that they don’t want to listen; it’s that they don’t have the time.” Similarly, Zakie, an internal medicine doctor practicing in teaching hospitals in Oklahoma, shared, “I always ask them to teach me back through the interpreter, so I can ensure they understand my recommendations and can follow them on their own. This takes time, and it’s a challenge in itself.”
Challenge of building trust
The majority of participants described difficulties in building trust with patients who have LEP, regardless of whether in-person or device interpreters were used. They emphasized that trust between the doctor and patient is essential to the care process, yet it is often undermined when the cultural aspects of communication are not considered by the interpreters. For example, Suzi, an internal medicine doctor, explained, “It’s not just about language; it’s about emotion too. I think if there’s no emotion in communication, then the patient can’t trust the provider. Trust and connection are important for establishing positive care.” Similarly, Maryam, a family medicine practitioner in California, stated, “It’s tough when some parts of communication are lost in translation . . . They [LEP patients] don’t believe us.”
Challenge of using interpreters through smart devices
Seventy-five percent of participants believed that the primary challenge in treating patients with LEP stems from using smart devices, such as iPads, to connect with third-party contractors for interpretation services. Using a device instead of a person creates anxiety and discomfort, especially for older patients. Additionally, they felt that many interpreters lack proper medical training and cultural competencies, which impacts the quality of communication. For instance, Zakie, an internal medicine doctor, asserted
The help that you can get from an in-person translator is then what you do through the iPad as well . . . I think in person is the best. And there is the effect of culture and body language that is missing in using iPad interpreters.
Similarly, Leila, a family doctor practicing in Texas, shared, “I caught one word that was wrongly translated by her [the interpreter]. I assume it happens more often than the one time I caught the mistake .. . . I am not sure, but I don’t think they [interpreters] get enough training.”
Health literacy of patients with LEP
Some participants in this study observed that the challenges in treating LEP patients often stem from their level of health literacy. Participants noted that if LEP patients are literate and educated in their own language, it becomes easier for providers to connect with them and explain the next steps in their care. However, when patients lack health literacy, using interpreters or ad hoc translators further complicates the process of educating the patients on medication use, referrals, or the reasons for follow-up visits. For example, Zakie, who has been practicing internal medicine for over 20 years, explained:
But as long as the medical literacy part is there—they know, for example, about diabetes, hypertension, usual stuff, or their own care, whatever chronic conditions they have like heart disease—it works for us. As long as they are educated on that end, it makes it easier.
Strategies Used by PCP to Overcome Barriers
Involving nurses and other bilingual colleagues in care
A few participants (5 out of 20) believed that seeking help from bilingual nurses or physician colleagues was very beneficial when treating patients with LEP. For example, Zakie, who previously worked in a state with a high number of immigrants from Nepal, often asked his Nepali-speaking colleagues to join him in the patient room. This practice ensured that interpreters did not miss key information and helped create a more comfortable environment for patients. Zakie explained, “Yes, always. I used to go find that nurse to just come in for a second, and then the patient would feel more comfortable talking to me.”
Spending adequate time listening to LEP patients
Some participants (21 percent) discussed the importance of spending additional time with LEP patients when it was practical and feasible. They noted that if their schedules allow, they try to extend the visit time to ensure that the patients’ concerns are thoroughly addressed. However, they acknowledged that this is not always possible, as they often run behind schedule.
Sue shared an example of her approach:
So, I have, for example, a child who is now a teenager. She initially had thyroid dysgenesis, a condition of the thyroid gland that resolves, and she stopped taking her medication. The family is from Greece, but they feel like they can share information with me. I take time with the translator to figure out where to go or at least provide reassurance. As a result, I have become their primary care physician for their child. But I know that not everyone is as fortunate as I am. At this point, I still have protected time with my patients, allowing me to afford half an hour for follow-ups and 45 minutes to an hour for new patients. I understand that many pediatricians and other physicians do not have this flexibility.
Similarly, Paul highlighted the trust he has built with LEP families, stating: “I have LEP parents who don’t take their kids to specialists just because they think I listen to them [more than specialists].”
Providing information and instructions in patients’ native languages
The majority of PCPs in this study believed that when patients receive instructions and visit summaries in their native languages, they have a higher likelihood of adhering to their medication regimen and requesting follow-up visits. Sue, a pediatrician practicing in Florida, emphasized this point, stating:
Again, it’s mostly because they [LEP patients] received the information in English, but that’s not their first language. I’ve learned—unfortunately, I think it was about four years into my practice—that Epic, the EHR [electronic health record] system we use, has a feature to provide the medication list and instructions in different languages. That has helped a lot with these patients.
Using matching systems in practice
Three out of 20 participants worked in managed care organizations that utilized a matching system to pair patients with providers fluent in their native languages. This system ensured that patients could communicate effectively with their healthcare providers, fostering trust and improving care outcomes. For example, Maryam, a family doctor, shared her experience: “Now I see more Farsi-speaking patients than any other patients—basically, 90 percent of my patients are Iranian because the schedulers match them with me.”
Practical Recommendations by PCPs to Improve the Quality of Care for LEP Patients
Hire more bilingual nurse practitioners and social workers
Some participants advocated hiring nurses and social workers from diverse ethnic and linguistic backgrounds to facilitate communication with LEP patients. They believed that having bilingual nurse practitioners and social workers would ease follow-up care and streamline referrals for both patients and doctors. For instance, Arjun, a family medicine practitioner at a teaching hospital in Arkansas, remarked, “Well, hiring bilingual doctors is not cost-effective, but hiring social workers and case managers who can speak other languages should be given a priority.”
Hire more in-person interpreters instead of relying on smart devices
Some participants (21 percent) suggested using healthcare resources more effectively by hiring more in-person interpreters—particularly in communities with larger immigrant populations—instead of relying solely on smart devices. Both patients and physicians expressed discomfort with smart devices, highlighting their limitations. For example, Amy, a geriatrician practicing in Pennsylvania, explained:
During residency at my home institute [name removed for privacy], we had in-person interpreters, and it made things so much easier, especially during end-of-life conversations with families from different ethnic groups. But here, where I am currently practicing, we barely have an iPad to connect, and it takes so much time.
Zakie shared a similar experience, noting that while in-person interpreters were available during his residency, they are no longer an option in his current practice: “That [use of in-person interpreters] was so much easier and faster.”
Provide cultural competency training during residency programs
The majority of participants emphasized the necessity of incorporating cultural competency training into residency programs to help residents become familiar with effective ways of treating LEP patients and those from ethnic minority groups. This is particularly important in states where residents will have significant exposure to these populations. For instance, Zackie, an internal medicine doctor, stated, “I hundred percent agree with it; we really need to have training during med school or residency.” Similarly, Sia, an internal medicine doctor practicing in Massachusetts, noted, “The US is a diverse place, and learning about different ethnic cultures and ideas definitely help[s] us as providers to deliver better care.”
Discussion
This study explored PCPs’ perspectives and experiences in treating patients with LEP. The results were categorized into the challenges faced during encounters and visits with LEP patients, strategies adopted over years of practice, and practical recommendations for improving the healthcare system to better address the needs of LEP patients. Based on the findings, PCPs face several challenges when treating patients with LEP, including difficulties in building trust, relying on interpreters through smart devices, and having inadequate time in their daily schedules—all of which impact the quality of care. Despite these obstacles, they identified various tools and strategies to improve care for LEP patients and enhance patient satisfaction. These strategies include involving nurses and other bilingual colleagues in patient care, hiring more bilingual aides or nurses, and incorporating cultural competency training into residency programs. Below, we discuss the theoretical contributions of these findings.
In the context of treating patients with LEP, we highlighted the challenges associated with using interpretation services via smart devices. While much of the existing literature emphasizes the benefits of employing formal interpreters(Silva et al. 2016, 2022), there is insufficient evidence addressing the difficulties of using interpreters through smart devices—a cost-saving measure preferred by many healthcare settings. Although formal interpreters offer numerous advantages compared with ad hoc translators (Keller and Carrascoza-Bolanos 2023), many lack cultural competency training and formal education in the medical field. Furthermore, a significant number of LEP patients, particularly those in the later stages of their lives, feel uncomfortable speaking through a device to a third-party during moments of vulnerability. Allocating dedicated interpretation resources to prioritize in-person translators—especially in states with higher populations of LEP patients—can enhance patient satisfaction and provide physicians with greater confidence in delivering quality care.
Our second theoretical contribution pertains to patient–provider matching services. A few managed care plans currently employ patient–provider matching systems during the scheduling process, allowing patients to be paired with providers who speak the same language (Cooper and Powe 2004). According to our participants whose practices have adopted this system, it provides an opportunity to build trust with patients who share the same language while eliminating the need to spend extra time finding interpreters or relying on interpretation services via smart devices (Vergani 2022). Implementing such a system in teaching healthcare settings and regional healthcare facilities can empower physicians to deliver higher-quality care and ensure that patients feel heard and understood.
Additionally, participants in this study highlighted the challenge of managing busy schedules, which often leaves them with inadequate time to spend with LEP patients (Kravitz et al. 2000). Prior research by Ulrich (2022) has shown that dedicating sufficient time to patients not only strengthens the doctor-patient relationship but also improves health outcomes (Ulrich 2022).
As noted by Gadon, Balch, and Jacobs (2007), physicians in private practice would benefit from practical, cost-effective strategies to address language barriers in clinical care (Gadon, Balch, and Jacobs 2007). This observation resonates with our findings, in which participants emphasized the critical need to train future healthcare providers in cultural competency and to equip them with the necessary tools to effectively care for patients with LEP. Such efforts, they noted, would ultimately enhance provider-patient communication and improve health outcomes. Similarly, Michalec et al. (2015) highlighted both institutional and individual-level barriers to the utilization of interpreter services—barriers that were echoed by our participants, who described similar challenges in accessing and using interpretation support (Michalec et al. 2015). Furthermore, Parsons et al. (2014) proposed a “get by” versus “get help” framework to describe decision-making in the context of language discordance (Parsons et al. 2014). This model closely parallels the experiences shared by our participants, who often grappled with ethical and logistical dilemmas when deciding whether to proceed with care despite language barriers or to delay care in hopes of securing interpretation.
In the age of artificial intelligence (AI), where more can be achieved in less time, providing clear instructions and visit summaries for patients with LEP should no longer be a significant challenge (Barwise et al. 2024). Pharmacists, nurses, and other healthcare professionals can leverage various AI tools to deliver more accurate translations of instructions for LEP patients. As the use of AI continues to grow rapidly, the healthcare sector must adapt and incorporate such technologies to improve the quality of care for underserved populations, including those with LEP.
Limitations
The majority of our participants were fluent in at least one language other than English, which may have helped them relate to and understand the struggles of LEP patients. Interestingly, these participants consistently used professional interpreters rather than ad hoc translators. This contrasts with findings from other literature, which indicate that physicians often prefer ad hoc translators because of their cost-effectiveness and convenience for the practice (Gadon, Balch, and Jacobs 2007).
For this study, we focused solely on PCPs, as they serve as the primary point of contact for patients and provide a broad understanding of treating LEP patients. However, we acknowledge that interviewing providers from other specialties might yield different perspectives and strategies for addressing the needs of LEP patients. This study did not explore the intersection of telehealth and treating LEP patients. Further research is needed to investigate physicians’ perspectives and challenges regarding the use of telehealth for treating patients with LEP. This includes examining how telehealth may exacerbate or mitigate existing disparities in access to care for LEP patients, as well as identifying best practices for providing culturally and linguistically competent care via telehealth.
Footnotes
Acknowledgements
We would like to thank the research participants for their generosity in sharing their stories with us.
Ethical Considerations
IRB approval was obtained from the authors’ current institute’s review board.
Consent to Participate
All participants consented to participate in the study. This qualitative work used anonymous data.
Author Contributions
SI did the conceptualization of the idea, data collection, analysis, and write-up.
ON reached out to the participants, helped with data collection, data analysis, and write-up.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Code Availability
Due to the small sample size and the risk of identification, the author cannot share the data and coding.
Data Availability Statement
The author cannot share the data due to the small sample size and the risk of disclosing the identity of the participants.
