Abstract
Introduction
Fibromyalgia is a specific rheumatic disease belonging to the functional somatic syndrome group. It is characterized by chronic pain of unknown origin and generalized stiffness in many body part. 1 Multimodal therapy includes gabapentin, antidepressants, psychiatric/psychological therapy, and physical therapy. However, effective and complete therapy has yet to be established.
Aromatherapy has been used for relaxation in some medical institutions and can help patients improve their quality of life (QOL) by relieving symptoms in various situations. Lavender (Lavandula officinalis) relieves insomnia, ylang-ylang (Cananga odorata) regulates heart palpitations and blood pressure, and neroli (Citrus aurantium) helps with insomnia and depression. 2 These oils commonly contain linalyl acetate, terpinene-4-ol, benzyl acetate, and limonene. While there are reports of the use of these essential oils and others for pain and stress relief,3,4 few have evaluated geranium (Pelargonium graveolens Fam. Geraniaceae) essential oil (EOPG), which is expected to have a relaxing effect. Animal research using mice to see the impact of EOPG demonstrated a significant reduction of blood pressure and heart rate following EOPG inhalation. 5 Clinical study on aromatherapy for fibromyalgia has investigated the effects of lavender essential oil on pain and sleep, but no study evaluated the effects of aromatherapy with geranium essential oil on mental stress and anxiety symptom. 6 Currently, a definitive overall mechanism underlying aromatherapy has yet to be established. However, several mechanisms of action have been reported, including neurologically mediated pathways associated with olfactory stimulation by inhalation of essential oil or pharmacological pathways that regulate either peripheral or centrally mediated.7–11 In the neurological pathway, neurotransmission to the brain is thought to occur following olfactory stimulation by the odorant. Pharmacological delivery pathways include absorbing oil components from the olfactory mucosa or lungs and transferring them to the brain through circulation. The EOPG used in this study contains lipid-soluble low-molecular-weight compounds that can pass the blood-brain barrier. In our previous mouse experiment, we found that linalool, citronellol, and geraniol, components of EOPG, were detected in the brain when EOPG was administered via inhalation. 5 In addition to these transmitters, psychological effects may involve applying essential oils, especially in humans. Therefore, we hypothesized that the impact of essential oil inhalation is not only due to psychological effects via olfactory stimulation but also achieved by pharmacological delivery pathways.
Objective assessment of stress uses measurements of hormones in both blood and saliva. These measurements are known to correlate with physiological responses to mental stress and are used to objectively assess stress.
Collecting saliva samples is less stressful than collecting blood or urine samples and is widely used in studies of mental stress assessment. In this study, we measured cortisol and chromogranin A (CgA) concentrations in saliva. Cortisol levels are known to increase in response to stress from high levels of tension or anxiety but not from cognitive or other simple tasks. 12 CgA is a stress marker and has been reported to show transient increases in response to mental stress and workload. 13 Therefore, measuring these mediators is feasible to evaluate stress responses from a different perspective.
Our research group aimed to apply aromatherapy clinically to treat refractory disease. In the treatment of mental stress and anxiety symptoms of fibromyalgia, drug therapy is complex and carries the risk of side effects. Complementary medicine has been introduced for treatment, 1 and we investigated aromatherapy with EOPG, which is expected to have a relaxing effect, as an intervention method. In this study, we used EOPG aromatherapy for fibromyalgia patients, who tend to show lower QOL because of chronic pain, emotional instability, and sleep disturbances. We hypothesized that aromatherapy with EOPG would decrease blood pressure and heart rate via the autonomic nervous system in fibromyalgia patients. We also expected that State-Trait Anxiety Inventory (STAI) scores, a measure of anxiety and stress, and salivary CgA and cortisol concentrations would decrease with aromatherapy treatment. A randomized crossover study was to investigate the effects of aromatherapy on autonomic modulation such as blood pressure and heart rate changes and the alleviation of anxiety and stress.
Results and Discussion
Participants
Ten patients were enrolled in this study; five were assigned to the CI group and five to the IC group (Table 1). Five were excluded from the analysis because they discontinued regular visits before the completion of the study.
Subject Characteristics.

Values are mean ± SD, percentages.
Normality
We performed the Shapiro-Wilk test to see the distribution of data. All numerical data followed a normal distribution except some had fewer values due to the missing dataset.
Measurements of Blood Pressure and Heart Rate
Blood pressure and heart rate were measured before and after aromatherapy to evaluate the autonomic regulatory effects of aromatherapy.
Comparison of Blood Pressure and Heart Rate Before and After Aromatherapy
To assess the immediate effect of aromatherapy, we compared blood pressure and heart rate measurements before and after the aromatherapy procedure at each patient's return visit (Table 2). Blood pressure measured before and after the procedure in the EOPG treatment showed no significant difference for systolic or diastolic blood pressure. Meanwhile, there was a significant increase in diastolic blood pressure in the control treatment (P = .02). A substantial decrease in heart rate after aromatherapy compared to the pretreatment value was observed in both treatments (P < .001).
Changes in Blood Pressure and Heart Rate Before and After Aromatherapy.

Comparison of Blood Pressure and Heart Rate at the Beginning and the End of the Study
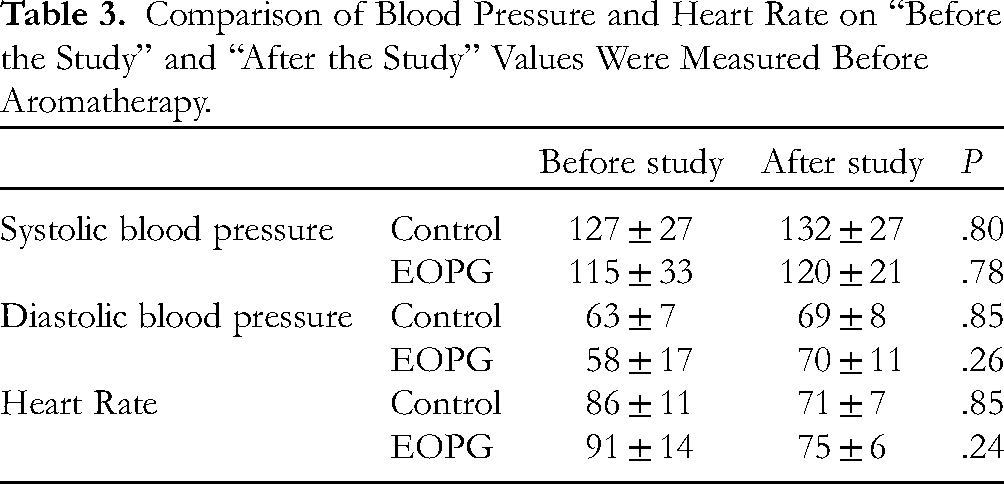
As shown in Table 3, we compared blood pressure and heart rate measurements at the beginning and the end of the study for each patient, with “Before the study” as the study start date and “After the study” as the study end date. There were no significant changes in any of the parameters.
Comparison of Blood Pressure and Heart Rate on “Before the Study” and “After the Study” Values Were Measured Before Aromatherapy.
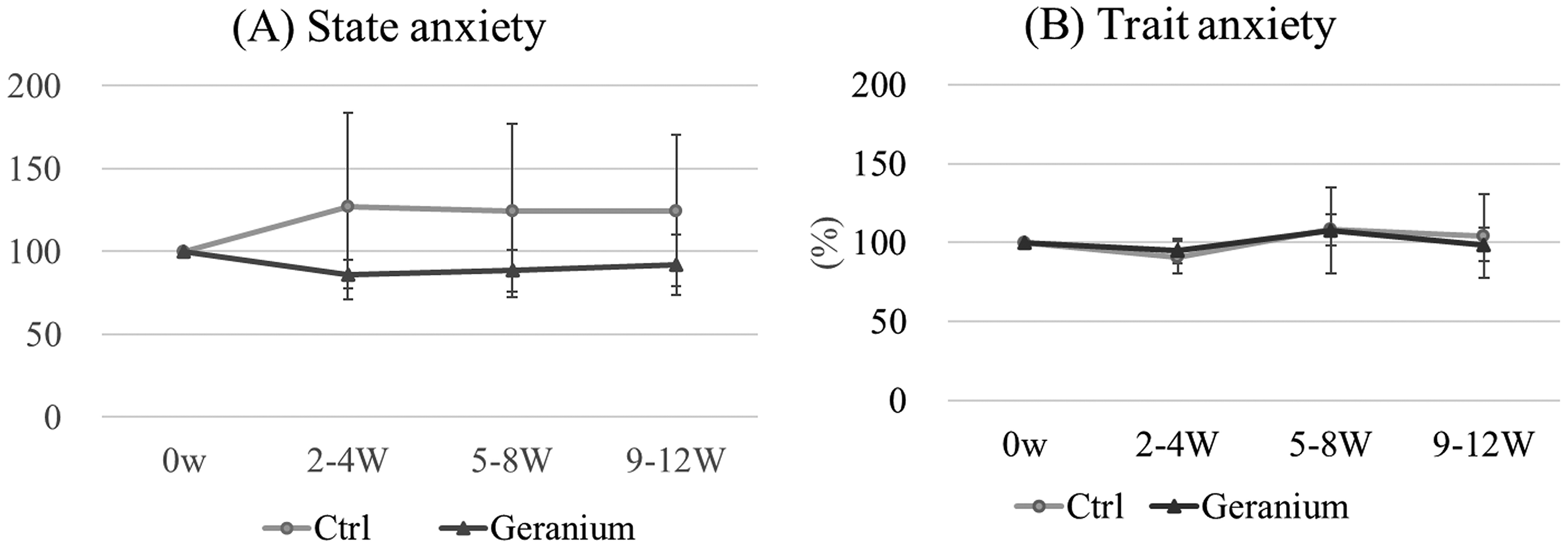
Comparison of STAI scores (state anxiety and trait anxiety) at the beginning and end of the study STAI scores (state and trait anxiety) were compared “Before study” and “After study.” Figure 1A shows state anxiety. State anxiety scores (mean ± standard deviation, P-value) were not significantly different in either the control group (51.0 ± 12.2 vs 49.2 ± 11.1, P = .83) or the EOPG group (55.8 ± 16.0 vs 54.0 ± 10.8, P = .86).

Comparison of STAI scores “before the study” and “after the study,” (A) state anxiety and (B) trait anxiety.
Figure 1B shows trait anxiety. Similarly, there was no significant difference between “Before study” and “After study” in both the control group (53.2 ± 10.4 vs 55.8 ± 17.4, P = .80) and the EOPG group (58.0 ± 16.4 vs 60.0 ± 10.0, P = .84).
The box shows the median, 25th, and 75th percentiles, and the whisker plot shows the upper and lower extremes.
Comparison of STAI Scores (State and Trait Anxiety) at Each Visit for Each Treatment
In Figure 2A, the state anxiety scores indicate a slight trend towards a decrease with the EOPG treatment, although there was no significant difference between treatments (P = .09). Figure 2B demonstrates the Trait anxiety scores, which also did not show a significant difference between treatments (P = .63).
Changes in STAI state and trait anxiety scores at each visit, (A) state anxiety and (B) trait anxiety.
STAI scores were expressed as a percentage change from the initial measurement before treatment. All STAI scores were determined before aromatherapy implementation at each visit. Mean ± SD, n = 5, repeated measures ANOVA.
Changes in Salivary Stress Markers
We measured CgA and cortisol as stress markers in saliva samples to provide a more objective assessment of the impact of aromatherapy on stress (Figure 3). One patient was unable to have saliva samples collected due to an underlying medical condition; therefore, saliva samples from that patient were not analyzed. There were no significant differences in CgA between the two treatments (P = .97). Cortisol increased transiently in the control group 2 to 4 weeks after treatment initiation; no trend of increase was observed in the EOPG group, but cortisol did not differ between treatments (P = .08).

Changes in concentrations of salivary stress markers, (A) CgA and (B) cortisol.
Stress markers, CgA and cortisol, were expressed as percentage changes from the concentrations before treatment. Saliva samples were collected before the aromatherapy. Mean ± SD, n = 4, repeated measures ANOVA.
Concomitant Medications
In this study, 3 of 5 patients took medications that could affect cardiac function, blood pressure, or both. Cardiovascular drugs may affect autonomic responses. Two patients were prescribed analgesic drugs. These drugs may impact the results to some extent; however, we did not exclude those patients from the study because it would cause a further reduction in the number of patients in each group. We confirmed that those patients didn’t change their medication throughout the experimental periods. In addition, no patient was prescribed female contraceptives or other hormonal drugs.
This study measured blood pressure and heart rate as a simple method to evaluate aromatherapy's relaxing effect, ie, the autonomic nerve regulation effect. The measurements in this study showed a significant increase in diastolic blood pressure before and after the aromatherapy procedure in the control group, while aromatherapy with EOPG did not cause an increase in diastolic blood pressure. Essential plant oils such as EOPG comprise multiple compounds, ie, linalool, citronellol, and geraniol. Linalool has been reported to affect the cardiovascular system by decreasing sensitivity to sympathomimetic agonists, thereby increasing vasodilatory responsiveness.14,15 Diastolic blood pressure is known to be more variable in value than systolic blood pressure, depending on the stiffness and distensibility of the blood vessels. 16 Based on the findings of the aforementioned research, it is hypothesized that the constituents of EOPG may exert a vasodilatory effect, thereby preventing the elevation in diastolic blood pressure subsequent to aromatherapy. Salivary stress markers, CgA and cortisol concentrations, fluctuate in saliva in response to autonomic nerve stimulation and are considered indicators of a subject's mental stress response.12,13 CgA generally shows a transient increase in response to workload,12,13 while cortisol reflects stress caused by tension and anxiety and is not increased by simple task. Since fibromyalgia is a disorder characterized by chronic pain and stress in daily life, we repeatedly assessed the concentration of CgA and cortisol levels in saliva during the aromatherapy process. The EOPG tended to suppress the elevation of cortisol at a specific time; however, the trend did not reach statistical significance.
The present study has some limitations. First, the study has a small number of patients, and the beta error is possible due to a lack of power in the statistical process. Initially, ten patients were required for each treatment with a power of 0.8, but only five patients could obtain data during the study period. Due to the small sample size, the present study should be considered a pilot study, and further studies with a larger size are necessary. Second, due to the nature of the crossover study, there is a question of whether the washout period was enough to eliminate the effect of the first treatment. In addition, because some patients dropped out after completing the first treatment, the benefit from the crossover study regarding having the same patient in both treatments is diminished. Furthermore, hormones and mood can fluctuate during each day, which can affect the results of the measurements. In this study, outpatients were admitted only during the limited time period of 1 to 4
Conclusions
In this clinical study, the use of EOPG in fibromyalgia patients did not change heart rate, but aromatherapy with EOPG was suggested to reduce the increase in diastolic blood pressure in fibromyalgia patients. Although there were no significant differences in the effects on heart rate and anxiety symptoms, the possibility of beta error due to the small number of cases to evaluate the effects of aromatherapy with EOPG is noted as a future issue. This study is a step toward building evidence for the introduction of aromatherapy into clinical practice, as it is the first to evaluate the effects of aromatherapy with EOPG on hemodynamics, anxiety scores, and stress markers for fibromyalgia patients. Although the results were not conclusive, there is a potential impact of incorporating the therapy into clinical practice with some additional larger studies.
Materials and Method
Participants
We enrolled patients who visited the outpatient pain clinic at the International University of Health and Welfare Shioya Hospital between June 1, 2019, and June 1, 2020. The patients have been under outpatient care since October 2018 and met the fibromyalgia diagnostic criteria published by the American College of Rheumatology in 2016. The criteria for the diagnosis of fibromyalgia were a score on the widespread pain index (WPI) of ≥7 and symptom severity (symptom severity (SS), which includes fatigue, sleep, cognitive function, and general symptoms) scale score of ≥5 or WPI 3-6 and SS scale score ≥9. The state of the condition meeting or exceeding these criteria must have been present for three months or longer. Furthermore, the patient's condition must have persisted for at least one year. A power analysis revealed that 10 experimental and 10 control subjects were required to obtain 80% power at the 5% significance level. The exclusion criteria were patients with allergies to EOPG and macadamia nut oil.
Essential Oil
EOPG (Green Flask, Tokyo, Japan) extracted by steam distillation from the leaves of P. graveolens was used as the essential oil for aromatherapy, and macadamia oil (Kaneda Shoji Co., Ltd, Tokyo, Japan) was used as the carrier oil. The essential oil used in this study was the same as that used in a previous study on animals. This essential oil was analyzed by GC-MS and found to contain 21.9% citronellol, 13.3% geraniol, and 6.3% linalool as its main components. 5 We prescribed either 1% EOPG in macadamia oil or macadamia oil only, depending on the assignment of the study group. At the time of the initial treatment, we provided a training course so the patients could perform aromatherapy independently. They were asked to perform aromatherapy once or twice daily at home, alone or with a family member. The in-hospital aromatherapy lasted about 15 min and covered the area from the elbow to the fingertips of one arm. We provided bottles that held 60 mL of oil and guided the patients to use 60 mL in one week of self-therapy.
Study Design
The study used a crossover design. Patients were randomly assigned to the CI group (Control→Intervention) and the IC group (Intervention→Control). Groups were assigned using the envelope method. The study period was a total of 6 months. In the CI group, patients were prescribed macadamia nut oil in the first three months of aromatherapy and 1% EOPG in the second 3 months. In the IC group, patients were prescribed 1% EOPG in the first half and macadamia nut oil in the second half. At the crossover point, the oil type was changed at the next return visit (2 weeks later) as a washout period (Figure 4).
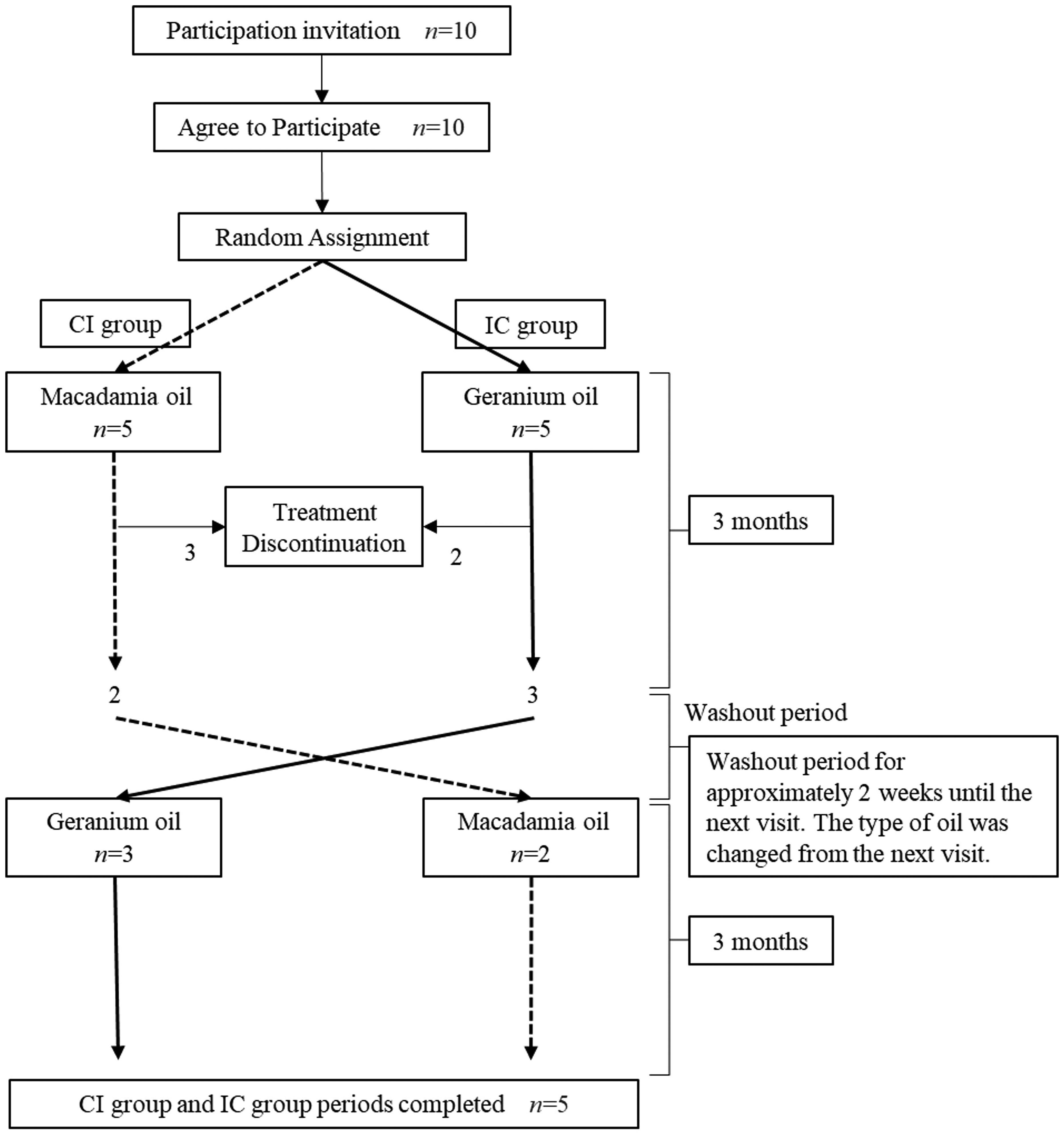
Experimental schedule.
Measurements and Data Analysis
Aromatherapy was administered along with regular medical care to consent for research participation. A trained pharmacist dispensed the aromatherapy oil at each patient visit. Before using the oil, all patients underwent a patch test to check for allergic reactions to EOPG. 17 1% EOPG containing macadamia nut oil was applied to the forearm from the elbow to the fingertips. We monitored allergic reactions such as erythema for 30 min after application. On the second visit, we interviewed the patient to rule out delayed allergic reactions, which would have prevented us from using the oil in the future.
The outpatient nurses handled the consultation and measured blood pressure and heart rate as in a regular medical examination. Furthermore, the STAI and measurement of stress markers in saliva were conducted at each outpatient visit during the intervention period to assess stress and anxiety associated with chronic pain. The required items were measured, and the specimens were collected according to the procedure in Figure 5. We prescribed treatment oil at each patient's return visit (2-4 weeks).
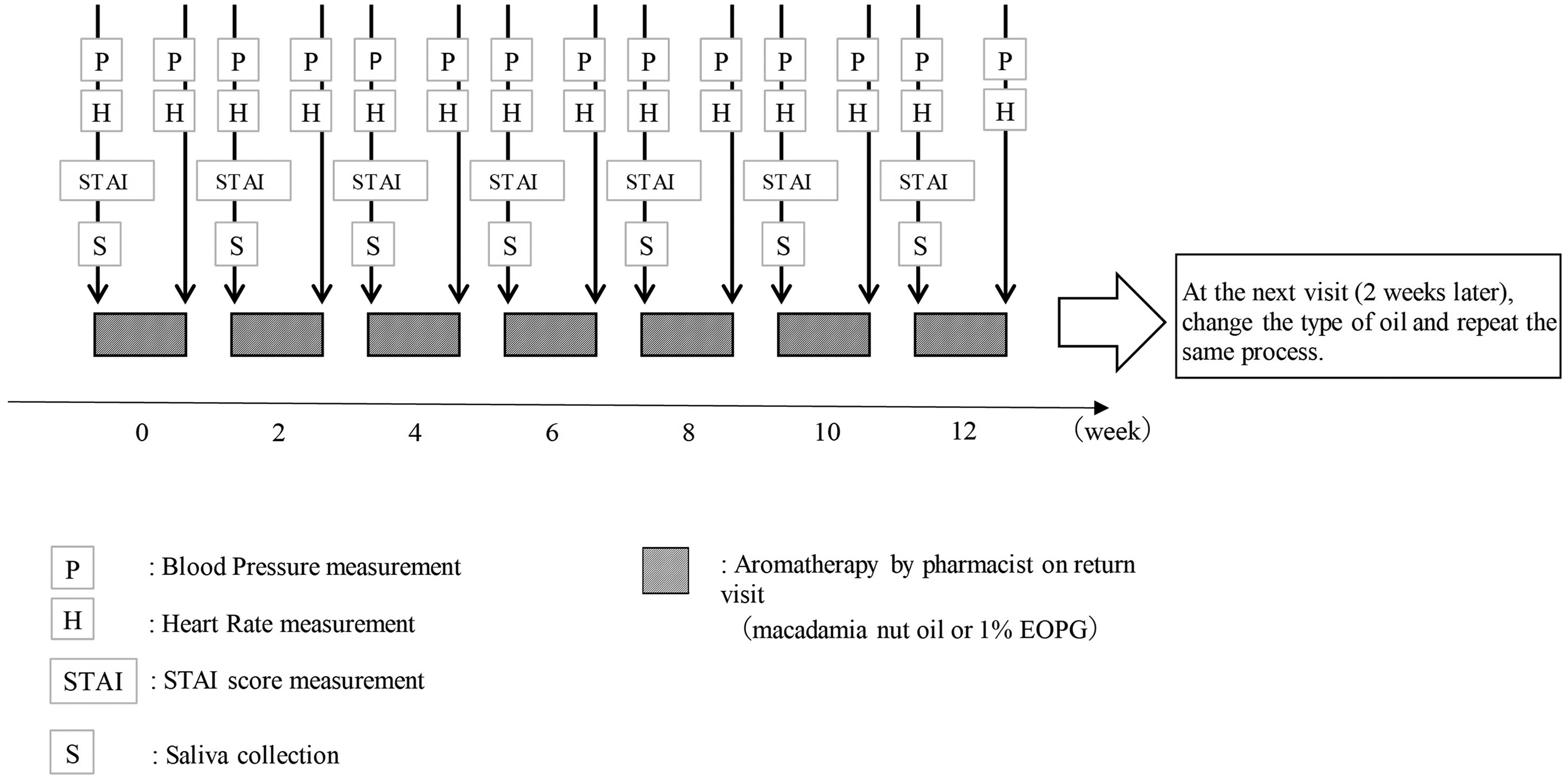
Aromatherapy and sample collection procedures in outpatient consultation.
Heart Rate and Blood Pressure
We took the patients’ heart rates and blood pressure as indexes of autonomic regulatory function. After confirming that the patient was at rest in the outpatient clinic for more than 10 min, those values were measured twice, before and after the aromatherapy, and recorded as “Before aromatherapy” and “After aromatherapy,” respectively, using an electronic blood pressure monitor (ES-H56, Terumo, Tokyo, Japan).
State-Trait Anxiety Inventory (STAI)
The STAI is a self-report inventory that measures the presence and severity of anxiety symptoms and the tendency to become anxious using 40 questions. The STAI consists of two subscales: the State Anxiety Scale and the Trait Anxiety Scale. The State Anxiety Scale measures the intensity of current anxiety, tension, and worry. In contrast, the Trait Anxiety Scale measures the frequency of general feelings such as calmness, confidence, and security. Higher scores indicate more significant anxiety. Different grading criteria are used for men and women to observe status changes. The reduced QOL of fibromyalgia patients may be attributed to pain and mental stress, such as the impact of pain on the activities of daily living (ADL) and anxiety about anticipated pain in everyday life, even in the absence of pain. In this study, we decided to employ the STAI, which is less burdensome for patients, to evaluate the impact of daily aromatherapy on mental stress due to fibromyalgia. We did the STAI score survey before the aromatherapy procedure at each return visit (STAI State and Trait Anxiety Inventory, Japanese version, Sankyobo, Kyoto, Japan).
Salivary Stress Markers
Cortisol and CgA concentrations in saliva were measured to assess stress objectively. Saliva samples were collected before each aromatherapy procedure at each patient visit and stored at −80 °C until analysis. Cortisol and CgA were measured using the electrochemiluminescence immunoassay (ECLIA) and enzyme-linked immunosorbent assay (ELISA), respectively (SRL, Inc., Tokyo, Japan).
Study Outcomes
The primary outcome was changes in blood pressure and heart rate that may be related to autonomic nervous system function. Secondary outcomes are STAI scores and measurements of CgA and cortisol in saliva.
Statistical Analysis
Measurements were checked to see if they followed a normal distribution using the Shapiro-Wilk (S-W) test. We used the Student's t-test to compare one-point data and repeated measures of ANOVA for time course data using the Bell Curve for Excel (Social Survey Research Information Co., Ltd, Tokyo, Japan) when they follow a normal distribution. Values presented were expressed as means (±SD). Statistical significance was set at P < .05. When the p-value was close to 1, it was considered that there was almost no difference. The effect size and power of the model were calculated using the program G*Power 3.1. The significance was set at 5%.
Footnotes
Abbreviations
Acknowledgments
We want to thank Dr Jun Ariyama, Department of Anesthesiology, Tokyo Women's Medical University, Adachi Medical Center, for his cooperation in conducting the study in a clinical setting, Prof. Yasuyuki Momose and Assoc. Prof. Kayoko Maezawa of the Faculty of Pharmaceutical Sciences, International University of Health and Welfare, for their guidance in conducting this study. We thank Dr Yasufumi Suda, Prof. of Orthopedics, Director of Shioya Hospital, International University of Health and Welfare, Ms. Nobuko Sasaki, and Ms. Misaki Akimoto, Pharmacy Department, for their cooperation in conducting the clinical study. We sincerely thank Mr Shinichiro Hayashi of Green Flask Corporation for providing the essential oil for this study. We sincerely thank Mr Shio Murakami of Totolabo Co., Ltd for his careful guidance in implementing aromatherapy.
The Contributions of the Authors
The conceptual framework for this research was designed and developed by Tadaaki Satou and Kiyoyasu Kurahashi. Ryuichiro Masubuchi and Tadaaki Satou performed the data collection and analysis. Ryuichiro Masubuchi and Kiyoyasu Kurahashi were responsible for the composition of the manuscript. All authors have read and agreed to the published version of the manuscript.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Research Ethics
This study was conducted according to the Ethical Guidelines for Medical and Health Research Involving Human Subjects, as approved by the Ethical Review Committee of the International University of Health and Welfare Hospital (Approval No. 13-B-373).
Informed Consent
The participants of this study were informed in writing and orally about the purpose and methods of the study, the fact that participation is voluntary, that there will be no disadvantages due to refusal, and their data are protected. Consent was obtained from each patient beforehand. We obtained written informed consent from each patient before the examination.
Trial Registration
The study protocol was registered with the UMIN Clinical Trials Registry before the study opened (UMIN000043490).
