Abstract
The aim of the present study was to characterize the chemical composition and to evaluate the anti-inflammatory and anti-nociceptive properties of the essential oil from the leaves of Phyllanthus muellerianus (Kuntze) Exell. The essential oil was hydrodistilled and characterized by gas chromatography-flame ionization detection and gas chromatography coupled with mass spectrometry analyses. The anti-inflammatory activity was evaluated on carrageenan-induced rat paw edema while the anti-nociceptive test was based on hot plate analysis. The hydrodistillation afforded 0.09% (dry weight basis) of pale yellow oil. Thirty-eight compounds representing 94.8% were identified in the oil. The major components of the oil were hexahydrofarnesyl acetone (11.6%), isocaryophyllene (9.8%), and limonene (9.4%). The oils of P. muellerianus displayed anti-nociceptive effect at a rate independent of reaction time and dose (P < 0.001). The rate of inhibition increased exponentially as the dose increases with optimum activity at 400 mg/kg. The carrageenan-induced edema model revealed the suppression of inflammatory mediators at a very high significant value (P < 0.001) for all doses, showing activity comparable to a standard drug at 4 hours after carrageenan injection. Collectively, the essential oils depressed the nociceptors and most likely acted as centrally mediated opioid analgesics while the anti-inflammatory mechanisms of the oil might be related to the decrease in the level of iNOS, and cyclo-oxygenase-2 in the edema paw via the suppression of pro-inflammatory cytokines (TNF-α, IL1-β), NO, and PGE2 production. This study confirms the analgesics and inflammatory activities of P. muellerianus.
Phyllanthus muellerianus (O. Ktze) Exell (family Euphorbiaceae) is a deciduous or evergreen shrub with numerous, more or less straggling stems from the base and sometimes with a climbing habit; it also sometimes becomes more tree-like in habit. It can grow up to 12 m tall and is used ethnomedically to treat inflammatory disorders. 1 The roasted powdered twigs are eaten with plant ash to treat dysmenorrhea. The fruits are edible and slightly acidic. 1 Extracts from various parts of P. muellerianus were shown to possess antibacterial, 2,3 anti-diarrheal, 4 anti-Leishmania, 5,6 phytotoxicity, 6 and cytotoxicity 6 activities. Geraniin a major compound of P. muellerianus displayed potent anti-inflammatory, 7 anti-infective, 8 and wound healing properties. 9 Nitidine, an alkaloid, was responsible for the antibacterial action of P. muellerianus against Clostridium sporogenes and Streptococcus pyogenes. 10 The phytochemical investigation on P. muellerianus led to the identification of bis(2-ethyloctyl)phthalate, bis(2-ethylicosyl)phthalate, 3-friedelanone, β-sitosterol and methyl gallate, 11 geraniin, corilagin, furosin, quercetin-3-O-β-d-glucoside (isoquercitrin), kaempferol-3-O-β-d-glucoside (astragalin), quercetin-3-O-d-rutinoside (rutin), gallic acid, methyl gallate, caffeic acid, chlorogenic acid, 3,5-dicaffeoylquinic acid, and caffeoylmalic acid. 10 The main compounds of the stem bark essential oil of P. muellerianus were (E)-isoelemicin (36.40%), (E)-caryophyllene oxide (22.54%), and α-cadinol (11.23%). The oil showed good antibacterial activity against C. sporogenes, S. mutans, and S. pyogenes, 12 Klebsiella granulomatis, 13 P. aeruginosa, S. aureus, and Bacillus subtilis. 14
Pain in humans is defined as “an unpleasant sensory and emotional experience associated with actual or potential tissue damage, or described in terms of such damage”; it activates nociceptors in the body tissues that convey signals to the central nervous system, where they are processed and generate multiple responses, including injury and inflammation. 15 Thus, the word “Nociception” denotes the peripheral and central nervous system processing of information about the internal or external environment as generated by nociceptor activation. Inflammation process is the basis of many physiological and pathological diseases such as atherosclerosis, allergy, rheumatoid arthritis, diabetes, neurodegeneration, and cancer. 16 There are several mediators involved in inflammation. Histamine, serotonin, bradykinin, and prostaglandins (PGs) are involved in the increased vascular permeability.
The aim of the present study was to report the volatile compositions, anti-inflammatory and anti-nociceptive activities of essential oils from the leaves of P. muellerianus grown in Nigeria.
A pale yellow oil was obtained in a yield of 0.90% (v/w), calculated on a dry weight basis. The volatile compounds are displayed in Table 1, along with their percentages and retention indices calculated on a HP-5 column. Thirty-five compounds amounting to 94.8% of the volatile contents were identified in the leaf oil of P. muellerianus. Monoterpene hydrocarbons (10.7%), oxygenated monoterpenes (15.1%), sesquiterpene hydrocarbons (16.9%), and oxygenated sesquiterpenes (32.3%) were the main classes of compounds present in the oil. Fatty acids are also identified in considerable amounts (14.6%). The major constituents of the oil were hexahydrofarnesyl acetone (11.6%), isocaryophyllene (9.8%), and limonene (9.4%). Other significant compounds of the oil were caryophyllene oxide (5.9%), pentadecanal (5.5%), phenylethyl alcohol (3.8%), (E)-β-ionone (3.4%), and β-caryophyllene (3.3%). This is the first report on the essential oil constituents of the leaf of P. muellerianus. The chemical compositions of the studied leaf oil were found to differ from the data obtained from the stem bark oil. 12 (E)-Isoelemicin and α-cadinol, the main compounds of the stem bark oil, were not found in the studied leaf oil while the content of caryophyillene derivatives in the leaf oil were much lower than the stem oil.
Chemical Constituents of Essential Oil of P. muellerianus.

aElution order on HP-5MS column.
bRetention indices on HP-5 column.
cLiterature retention indices.
dComparison with authentic compounds.
The chemical compositions of the leaf oil of Nigerian grown P. muellerianus were also found to differ considerably from our previous findings on the compositions of essential oils from the leaves of Nigerian grown P. amarus, dominated by linalool (36.4%) and phytol (13.0%) 17 ; and P. reticulatus consisting mainly of β-pinene (18.1%) and β-caryophyllene (11.9%). 18
The essential oils in test doses of 500, 1000, 1500, and 2000 mg/kg body weight showed no contrary effects on the behavioral responses in the tested rats following 14 days observation. No mortality or weight change was observed. Therefore, a highest dose of 400 mg/kg given to rats in this study was considered to be safe.
The results of the anti-nociceptive effect of P. muellerianus oil (PMEO) using the hot plate method are presented in Figure 1, while Figure 2 shows the maximum percentage analgesia of the oil samples in relation to dose and time. The analysis was conducted based on dose dependent of 100, 200, and 400 mg/kg of rat body weight. Statistical significance of P < 0.05 was used to test the level of confidence of the values. As shown in Figure 1, all test doses increased analgesia and pain resistant of the Wistar rats. Compared to the lower dose (100 mg/kg), the 200 and 400 mg/kg dose of PMEO showed analgesic effect against the hot plate response in rats (P < 0.001). Aspirin (100 mg/kg) also showed a potent analgesic effect as expected. In the study, the activities of the 200 and 400 mg/kg oil were comparable and even exceeded the analgesic effect of aspirin at the 30th to the 90th minute. The activity of the 100 mg/kg oil increased steadily within the 60th to the 120th minute (P < 0.01).

Effect of the PMEO leaves on hot plate anti-nociceptive: control, standard, and PMEO, represent 1 mL saline solution, 100 mg/kg of aspirin, and 1 mL of 100, 200, and 400 mg/kg of oil, respectively. *P < 0.05, **P < 0.01, and ***P < 0.001 statistically compared to the control.
Percentage inhibition of PMEO on hot plate model in Wistar rats. Saline solution (1 mL/kg); ASA, aspirin (100 mg/kg); PMEO; 100 mg/kg, 200 mg/kg, and 400 mg/kg.
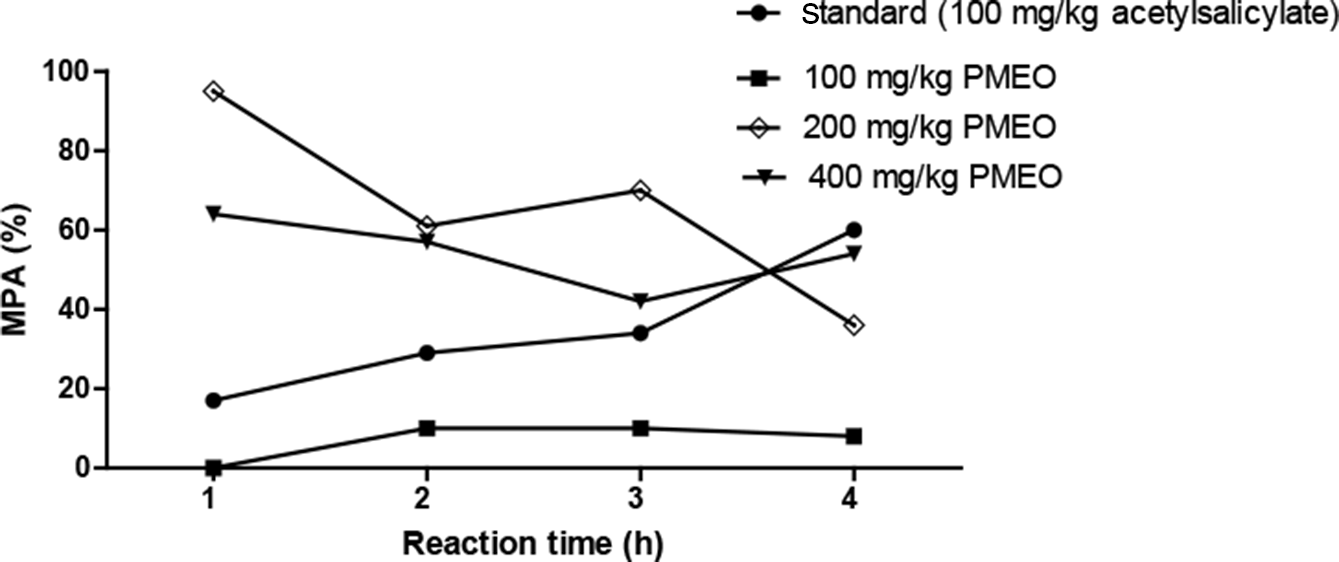
Percentage analgesia as shown in Figure 2 showed a steady increase in the activity of the standard drug (aspirin) which increased relative to reaction time (17-60%). The 200 and 400 mg/kg PMEO exhibited very high activity at the first and second hour within the range of 57% to 95%. However, the activity reduced at the third and fourth hour.
In the carrageenan-induced acute inflammation (Figure 3), PMEO-treated groups significantly reduced the mean maximal swelling attained at 1 to 4 hours (P < 0.001) for all the doses. As expected, the reference drug, diclofenac (100 mg/kg), caused a significant inhibition of post carrageenan edema.

Effect of the PMEO leaves on carrageenan-induced inflammation: control, standard, and PMEO represent 1 mL saline solution, 100 mg/kg of diclofenac, and 1 mL of 100, 200 and 400 mg/kg of PMEO respectively. P < 0.05, P < 0.01, and ***P < 0.001 statistically compared to the control.
We have evaluated the analgesic and anti-inflammatory activities of PMEO to clarify the pain- and inflammation-relieving effects. The hot plate test was carried out to ascertain either the peripheral or the central acting effect with response of cerebral cortex or spinal cord integration of the essential oils. 15 The test is widely used to clarify the analgesic and most especially the effect of opioid drugs on the spinal cord. In our study, we found that the oil (100, 200, and 400 mg/kg) exhibited anti-nociceptive effect in hot plate-induced pain. In addition to the activity, the effect was prolonged showing a high rate of absorption and inhibition of the pain receptors. These observed effects could be due to the inhibition of nociceptors. Phyllanthus species has been shown to be an excellent candidate for analgesic remediation. Hydroxyl alcoholic extracts of P. amarus, P. fraternus, P. stipulates and P. orbiculatus caused anti-nociceptive of about 2 to 6-fold more active than aspirin when administered orally, 19 while the high anti-nociceptive activity of P. corcovadensis was alluded to the inhibition of the synthesis of cyclo-oxygenase products derived from arachidonic acid and by independent of activation of opioid receptors. 20
Analgesic activities of essential oils have been widely reported; they easily penetrate the blood-brain barrier and act in the central nervous system thereby behaving as a psychoactive drug. The high structural diversity of the essential oil constituents increases their synergistic effects. Major constituents of PMEO had previously been reported for high activity. A study observed that the daily oral administration of (R)-(+)-limonene for 15 days, inhibited the spared nerve injury (SNI)-induced mechanical hyperalgesia by 63%. 20 Therefore, the relative activities observed in the PMEO can be attributed most likely to the inhibition of opioid receptors.
Carrageenan is widely used to induce paw edema in rodents to validate anti-inflammatory effect of drugs or herbs. This model is considered to be a biphasic model. The early stage (1-2 hours) contributes to the release of histamine, bradykinin, and serotonin which facilitate the increased synthesis of PGs from surrounding tissues of the injured site. The late phase (3-4 hours) is characterized by the increased level of PG mediated by the elevated modulation of leukotrienes and bradykinin. During this phase the cyclo-oxygenase-2 (COX-2) converts arachidonic acid into PG which is a key factor of inflammation regulation. In this experiment, carrageenan-induced edema in the hind paw of rats was inhibited by all the extract doses. Phyllanthusmuellerianus oil significantly inhibited the edema formation; 1, 2, 3, and 4 hours after the injection of carrageenan in the hind paw of rats. These results indicated that the phytoconstituents present in PMEO most likely inhibited the inflammatory mediators of the initial as well as late phase of inflammation induced with carrageenan.
Terpenoids are established anti-inflammatory agents which inhibit the production of NOS-2 and COX-2 proteins, and NOS-2, COX-2, TNF-α mRNAs, and NF-κB. 21 Many essential oils effectively inhibit pro-inflammatory cytokine production. α-Humulene from C. verbenacea prevented neutrophil migration and TNF-α production 22 ; 1,8-cineole inhibited TNF-α and IL-1β in human lymphocytes. 23 Terpinen4-ol suppressed the production of TNF-α, IL-1β, IL-8, IL-10, and PGE2 by lipopolysaccharide (LPS)-activated monocytes. 24 In the present investigation, PMEO revealed the presence of hexahydrofarnesyl acetone and limonene. Limonene, a monoterpenoid possesses strong anti-inflammatory and analgesic properties by preventing the production of NO, PGE2, IL-1β, IL-6, and TNF-α, as well as the expression of iNOS and COX-2 proteins in LPS-treated RAW 264.7 cells, suggesting that it down-regulated pro-inflammatory mediators and cytokines. 25 The relative anti-inflammatory observed in PMEO could be attributed to the inhibition of the pro-inflammatory mediators in a synergistic effect of all the constituents present in the essential oils. The methanolic extract of P. acidus at a dose of 500 mg/kg showed higher activity than the ethyl acetate and petroleum ether extracts and inhibition was attributed to the mediating of the release of phospholipase A2 that stimulates the inflammatory mediator release. 26 Similar activities was observed in the methanolic extracts of P. reticulatans, 27 while the lignin content of P. amarus successively inhibited the bradykinins, platelet activating factor, and endothelin-1(ET-1). 16
In conclusion, the present study demonstrates the potent in vivo anti-inflammatory and anti-nociceptive activities of PMEO in a hot plate model and carrageenan-induced-edema. The results indicate that PMEO acts by inhibiting nociceptors in a centrally analgesia mechanism which is a relative of the opioid anti-nociceptors. Furthermore, assessment of anti-inflammatory activity shows a very high activity which is independent of dose or time of exposure. The study shows inhibition of pro-inflammatory mediators at both stages of carrageenan-induced inflammation which is attributed to the inhibition of NO, PGE2, IL-1β, IL-6, and TNF-α, as well as the expression of iNOS and COX-2 proteins in LPS-treated RAW 264.7 cells and other pro-inflammatory mediators. The activities could be attributed to the constituents of the essential oils acting in synergy. This study validates the ethno-botanical use of the plant among locals as a pain mediator.
Experimental
Collection of Plant Sample
The leaves of P. muellerianus were collected from the Onigambari Forest Reserve, Oyo state Nigeria, in November 2017. Botanical identification was accomplished at the Herbarium, Forestry Research Institute of Nigeria (FRIN), Ibadan, Nigeria, where a voucher number, FHI 111386 was deposited.
Hydrodistillation and Analysis of the Essential Oils
Prior to hydrodistillation process the plant samples were air-dried under laboratory shade for 2 weeks (25°C) to reduce the moisture contents. In this process 300 g of air-dried and pulverized leaves of P. muellerianus was used. Hydrodistillation was carried out with a Clevenger-type distillation unit designed according to the specification as described previously. 17,18 The GC and GC-MS analyses as well as the means of identification of the constituents of the essential oils were reported in our earlier publications. 17,18
Study Animals
About 150 to 200 g of Wistar rats of both sexes were accommodated in the Biochemistry Department animal facility of Lagos State University, Ojo-Lagos. The animals were kept in a metal steel cage, where they had unrestricted supply to water and standard pellet food ad libitum. They were acclimatized for 2 weeks before commencement of experiment. Ethical clearance certificate was obtained from the Research Ethical Clearance Committee (RECC) of the University (Approval no: 012/2017/LASU/BCH). The animals were assigned at random to a group of 5 consisting of 6 animals per group: Group 1—Control group (Saline solution); Group 2- Diclofenac treated group 100 mg/kg (standard group); Group 3—100 mg/kg of essential oil; Group 4200 mg/kg of the oil; and Group 5- 400 mg/kg of oil.
Acute Toxicity
The essential oils were tested for acute toxicity study as per standard protocol. 28 Wistar rats were administered 500, 1000, 1500, and 2000 mg/kg of PMEO per oral route. One group received normal saline that served as a negative control. The animals were observed for 12 hours continuously for changes in their behavior. Mortality for the next 14 days was also noted.
Carrageenan-induced Paw Edema in Rats (Anti-inflammatory Test)
Carrageenan-induced rat paw edema was done according to a modification form of an established procedure. 28 Twenty-five Wistar rats (both sexes, 150-200 g each) divided into 6 animals in each groups used for study, induced by subcutaneous injection of a 0.1 mL of 1% freshly prepared carrageenan in saline in the right hind paw of rats and 1 mL of the vehicle were administered for all doses. Paw volume of the injected rats was measured every hour for 4 hours using a plethysmometer (Ugo Basile, Italy).
Hot Plate Test for Anti-nociceptive Study
The experiment was carried out according to the modified method. 29 Thirty mature Wistar rats of both sexes were randomly divided into 5 groups of 6 rats per group. The animals were fasted for 12 hours with provision of clean water ad libitum. Each rat was placed upon the heated metal plate (hot plate) maintained at the temperature of about 50°C to 55°C within the restraining glass cylinder. Group 1 rats received 1 mL/kg of saline solution and served as the control. Group 2 rats received sodium salicylate (100 mg/kg [ASA] [standard control]) and groups 3, 4, and 5 received 100, 200, and 400 mg/kg of PMEO, respectively, per (p.o.). Animal response to the heat varies and such changes includes; kicking of hind foot and jumping about, licking of foot, raising the foot, holding the foot tightly to its body or shaking of the foot. The reaction time was recorded at 30, 60, 90, and 120 minutes after the administration of the treatments. The maximum reaction time was fixed at 30 seconds to prevent any injury to the tissues of the paws. If the reading exceeds 30 seconds, it would be considered as maximum analgesia.
The maximum possible analgesia (MPA) was calculated as follows:
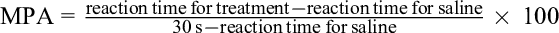
Statistical Analysis
Repeated Measures One way ANOVA Analysis using Dunnett’s multiple comparisons post hoc test was performed using GraphPad Prism (version 7.02), San Diego CA, USA, www.graphPad.com) to compare activity between the control groups and rat treated with the test compounds and values were considered significant at P < 0.05 and above. Results were expressed as mean ± SEM. 28,29
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
