Abstract
Background:
Patients with type 2 diabetes (T2D) require continuous management to achieve optimal outcomes. Socioeconomic barriers can impede the delivery of optimal diabetes care. During the COVID-19 pandemic, telemedicine likely reduced common barriers to care compared with in-person visits. This study investigated the impact of telemedicine on no-show rates and diabetes outcomes in publicly insured patients and the potential link to reduced socioeconomic barriers.
Methods:
This retrospective study analyzed the records of 819 patients with T2D at the Yale Medicine Diabetes Center (YMDC). From June 2019 to March 2020, patients had in-person clinic visits, followed by telehealth visits from March to December 2020 due to system-wide COVID-19 isolation mandates. No-show rates, glycemic control metrics, and other biomarkers were compared in the same patients between their in-person and telehealth visit periods.
Results:
Patients utilizing telemedicine averaged no-show rates of 0.34 ± 0.69 compared with 1.19 ± 1.30 (P < .001) for in-person visits. Average hemoglobin A1c (HbA1c) for telemedicine was 7.93 ± 1.95 compared with 7.91 ± 1.90 (P = .65) for in-person visits. Percentages of patients achieving ≥70% glucose time in range (TIR) on an ambulatory glucose profile (AGP) was 43.90% for telehealth and 45.42% (P = .76) for in-person visits.
Conclusion:
Publicly insured patients with T2D showed significantly reduced no-show rates and comparable glycemic control during telemedicine visits compared with in-person visits. Telemedicine visits may be associated with lower no-show rates due to a reduction of socioeconomic barriers. Future studies are warranted to further clarify potential associations of specific socioeconomic barriers to missed visits.
Keywords
Introduction
In 2019, 37.3 million Americans, or 11.3%, of the population were diagnosed with type 2 diabetes (T2D). 1 It is projected that by 2050, the prevalence of diabetes will increase to 25% of the US adult population. 2 In addition, existing estimates indicate that one out of every four dollars in US health care costs is spent on caring for people with diabetes. 3 Alongside the significant rise in the incidence of diabetes, there is an extreme shortage of primary care clinicians in the United States.4,5
Primary care providers face significant challenges due to constantly increasing patient populations and ever-advancing diabetes interventions available. Given these challenges, patients struggle with the management of their T2D and experience worse health outcomes. 6 In addition, patients of low socioeconomic status (SES) and the elderly encounter additional socioeconomic barriers that can prevent the achievement of their health care goals.7-9 Many studies have investigated the drivers of socioeconomic health outcome disparities experienced by patients of low SES.7-9 Affordability of medication, lack of transportation, childcare, inability to take medical leave from work, and food insecurity are some of the major barriers to health care access and positive health outcomes. 8 The elderly population faces many of the same barriers when it comes to the management of chronic diseases, including transportation and financial hardship.10-13
Chronic disease management, like diabetes, requires regular clinical visits, medication access, and treatment plan adjustments. Without transportation, patients experience delays in clinical interventions resulting in negative health outcomes. 14 Patients experiencing income or food insecurities were associated with increased HbA1c levels, increased BMIs, and worsened complications. 15 Approaches to reduce socioeconomic barriers to diabetes care include incorporating accessible technology such as telehealth visits, smartphone applications, and other connected devices. 16 Telehealth visits may reduce transportation-related expenses and other socioeconomic barriers for patients with T2D.
During the COVID-19 pandemic, telemedicine became a mainstream model of care to prevent the spread of SARS-COV-2. 17 Telemedicine includes a combination of both video and phone visits where patients can meet with their health care providers remotely. 18 These visits include annual visits, follow-up appointments, sick visits, laboratory result discussions, or medication changes. Telemedicine allows patients to access medical care from their location of convenience, without having to manage transportation, medical leave from work, childcare, or other undue financial costs. 18 The use of virtual care delivery models has been shown to provide flexibility to clinicians and to increase access to care in rural areas. 19 Several studies have suggested that telehealth models for diabetes care would also be cost-effective for patients. 18 While other pre-pandemic studies conducted show the effectiveness of telemedicine in managing T2D and lowering HbA1c, they lack a sufficient sample size to achieve validity. 18 ,20-22
The COVID-19 pandemic created an opportunity to analyze the effectiveness of telemedicine in managing T2D using a large sample size. Furthermore, there have been limited studies on the effectiveness of telemedicine in achieving positive health outcomes for T2D patients most marginalized by traditional models of health care, including patients of low SES and the elderly population. 23 For this reason, we conducted a retrospective cohort study to analyze the impact of telemedicine in the management of publicly insured patients with T2D served by the Yale Medicine Diabetes Center. The study aimed to evaluate the impact of telemedicine visits during the COVID-19 pandemic on patient no-show rates, HbA1c, ambulatory glucose profiles, and lipid profiles compared with the same metrics during in-person visits prior to the COVID-19 pandemic.
Methods
Setting and Study Population
Patient records were obtained from the YMDC, the joint clinical practice of the Yale School of Medicine and Yale New Haven Health. The study subjects were patients with type 2 diabetes who received care exclusively from endocrinologists or diabetes specialists at the YMDC. Patients included in this retrospective study had a confirmed diagnosis of type 2 diabetes for at least one year before 2019, had at least one HbA1c measurement available for both study periods, and were prescribed either oral medications or insulin or both for glycemic management. The final inclusion criteria included all patients who were publicly insured through either Connecticut (CT) Medicaid or Medicare. 11 Insurance status was used as a proxy to select patients of low SES, covered by Medicaid, and the elderly population, covered by Medicare. There were no exclusion criteria for baseline glycemic control as measured by HbA1c or AGP data sets from continuous glucose monitors (CGM). Patients were transitioned to telehealth visits via system-wide communications that provided step-by-step instructions. CGM data was uploaded into the Electronic Medical Record (EMR) prior to patient visits by use of existing clinic support resources. The exclusion criteria included: patients with type 1 diabetes, under the age of 21, private insurance status, and deceased at the start of data collection. Eligibility criteria is summarized in Figure 1. All patient data were obtained between June 2019 and December 2020 via the EMR. This study had no follow-up period.
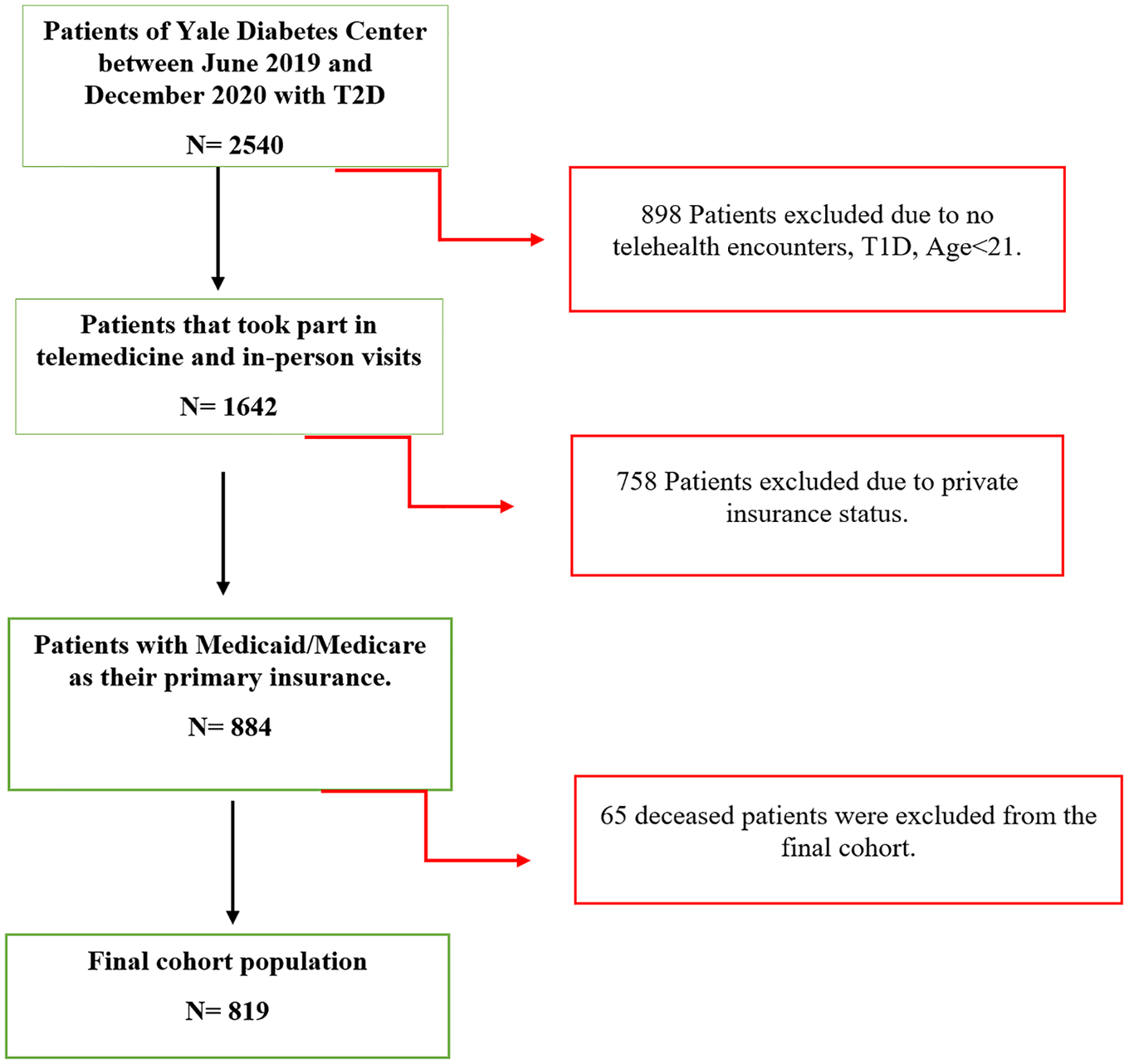
Inclusion and exclusion criteria. Patients excluded from the study are highlighted in red.
Study Design
This research study was conducted as a retrospective cohort study of 819 patients at the YMDC using EMR data from June 2019 to December 2020. All 819 patients attended at least one in-person visit at the YMDC from June 2019 to March 2020. The same patients then attended at least one telehealth visit at the YMDC from March 2020 to December 2020 during a system-wide transition to telehealth imposed during the COVID-19 pandemic. Among this cohort, biomarker data was compared between in-person and telehealth visits. Electronic medical records were used to obtain the following data: HbA1c, glucose time in range (TIR), and lipid profiles. Average percent glucose TIR was obtained through analysis of AGP data sets from CGM devices, as available, for both in-person and telehealth visits.
The intervention consisted of one or more telemedicine visits with the patient’s diabetologist, including physician associates (PA), nurse practitioners (NP), or physicians (MD). All patients offered a telehealth visit were also provided remote support by clinic staff to facilitate CGM data upload. The telemedicine visits occurred every three months on average, or a frequency decided by the provider based on the patient’s needs. The study was carried out under IRB protocol #2000033766 and JDAT ID #2381293.
Outcomes
The primary outcome measures were the percent changes in HbA1c and percent changes in patients achieving a goal percent glucose TIR of ≥ 70% during the telehealth visit phase compared with the in-person visit phase. The percent glucose TIR is a metric for patients who wear a CGM device. Glucose TIR is defined as the percentage of time a patient’s glucose level falls within the range of 70-180 mg/dL. In addition, patient no-show rates were compared between telehealth and in-person visit phases. A no-show was recorded if the patient did not appear for their visit without rescheduling or canceling at any time during the nine months for each visit arm of the study. Other outcome measures including LDL, HDL, total cholesterol, and triglycerides were also collected. These data points were obtained by electronic medical record extraction or manual chart review via Joint Data Analyst Team (JDAT) at Yale University. All data was stored on a secured Yale Box drive.
Statistical Analyses
All demographic data are expressed as numbers and percentages (Table 1). All continuous data are expressed as mean (M) ± standard deviation (SD), including the primary and secondary outcomes of the study. The primary outcome, change in HbA1c, was used to determine the power of the study, with an expected difference in two populations to be 1.0 with a standard deviation of 0.5. Based on a paired t-test model, a sample size of 819 patients revealed the power of the study at 100%. 24 Statistical analyses consisted of paired t-tests, for all primary and secondary outcomes (Tables 2-3). This method of analysis incorporates paired cohorts across all continuous variables. A P-value of <.05 was considered statistically significant. All data were analyzed using SAS v9.4. The study did not analyze subgroup interactions. Since this was a paired cohort study, regression analysis was not conducted for confounding factors.
Sample Characteristics of 819 (N) Patients a .

Continuous data reported as mean with standard deviation (M±SD).
Diabetes Outcomes Across In-Person and Telemedicine Visit Durations.
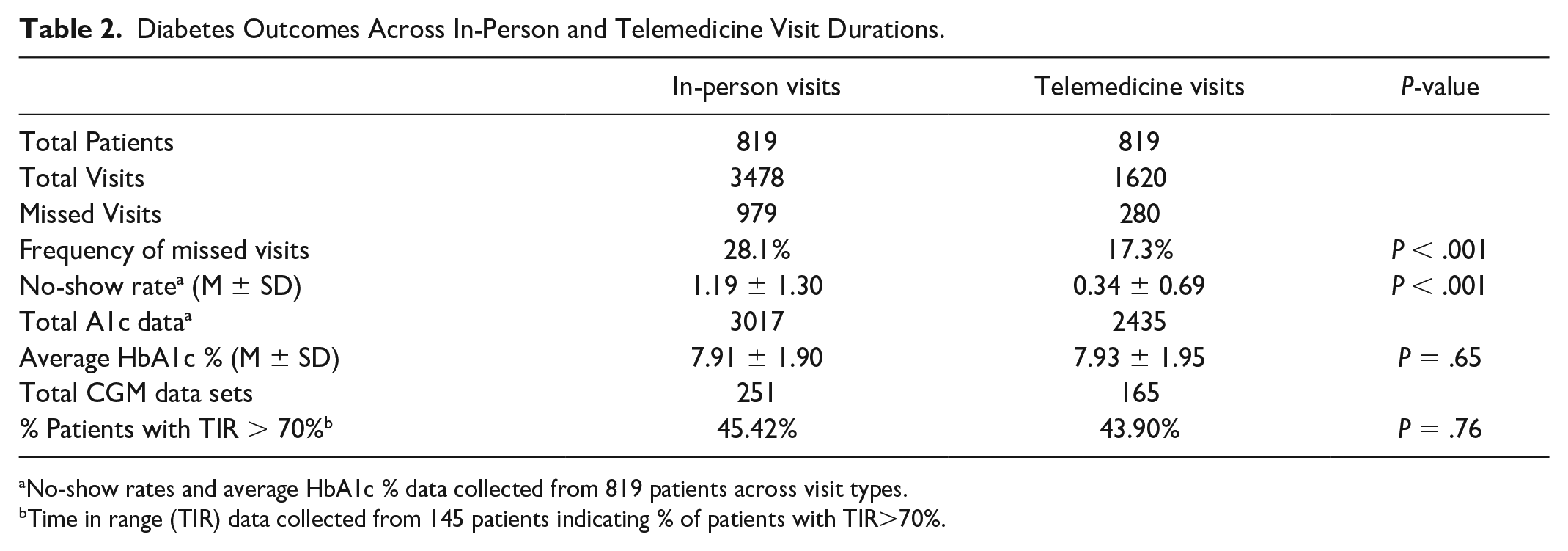
No-show rates and average HbA1c % data collected from 819 patients across visit types.
Time in range (TIR) data collected from 145 patients indicating % of patients with TIR>70%.
Lipid Profile Analysis in T2D Care for In-Person and Telemedicine Visits.
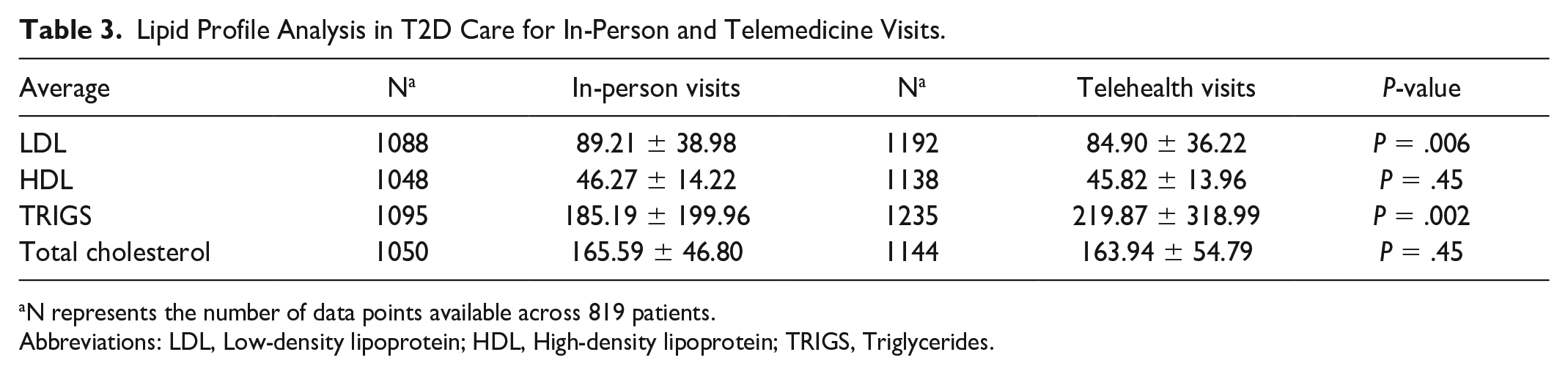
N represents the number of data points available across 819 patients.
Abbreviations: LDL, Low-density lipoprotein; HDL, High-density lipoprotein; TRIGS, Triglycerides.
Results
Table 1 demonstrates the baseline characteristics of 819 patients in the retrospective study. There is no difference between the in-person and telehealth groups as patients are paired to self across time in this study. This cohort represents a diverse population with an average age of 60.41 ± 14.56 years. The study has 56.53% female and 43.41% male with an average duration of diabetes of 7.61 ± 2.83 years. Our study represents the diverse population of New Haven County, with 463 (50.06%) White, 356 (28.32%) African American, and 26 (3.17%) Asian, 10 (1.23%) Native American, and 141 (17.22%) other. Our cohort also includes patients holding public insurance with 52.64% of patients with Medicaid and 44.51% with Medicare.
Table 2 compares diabetes outcomes of the same patients across a nine-month in-person visit period followed by a nine-month telehealth visit period. The average number of in-person visits were 4.24 per patient and the average number of telehealth visits were 1.97 per patient. Based on paired t-test analysis, the in-person duration had a no-show rate of 1.19 ± 1.30 visits compared with a no-show rate of 0.34 ± 0.69 visits during the telehealth duration (P < .001). The no-show rate was recorded as the average number of missed appointments for each patient during the nine-month duration for each visit arm. This represents a 71.4% reduction in the no-show rate during the telehealth duration compared with the in-person duration. (Table 2).
Furthermore, the average percent HbA1c in Table 2 reflects the comprehensive average of all HbA1c data points for the in-person arm compared with all HbA1c data points for the telehealth arm. The average number of HbA1c measurements per patient was 3.68 for the in-person arm and 2.97 for the telehealth arm. The paired t test revealed an average HbA1c of 7.91 ± 1.90 during in-person visits and 7.93 ± 1.95 for telehealth visits (P = .65), demonstrating noninferiority. The study also investigated CGM data to determine the percentage of patients with a TIR of ≥ 70%, defined as glucose levels between 70 and 180 mg/dL for greater than or equal to 70% of a 14-day time period. Guidelines indicate that a TIR ≥ 70% for 14 days correlates to a HbA1c of <7%. 25 The chi-square test showed 45.42% of patients for in-person visits and 43.90% of patients for telehealth visits had a TIR of ≥ 70% with a P-value of .76.
When analyzing lipid profile changes during in-person versus telehealth visits using paired t test analysis, the average LDL during in-person visits was 89.21 ± 38.98 compared with 84.90 ± 36.22 for telehealth visits (P = .006). The average HDL remained unchanged during in-person visits, 46.7 ± 14.22, compared with telehealth visits, 45.82 ± 13.96 (P = .45). Triglycerides were significantly lower during in-person visits, 185.19 ± 199.96, compared with telehealth visits, 219.87 ± 318.99, with a P-value of .002. Total cholesterol remained unchanged from in-person visits, 165.59 ± 46.80, compared with telehealth visits, 163.94 ± 54.79 (P = .45) (Table 3).
Discussion
Our study is among the first to assess the impact of telehealth on diabetes outcomes for patient populations who may encounter socioeconomic obstacles to accessing health care. The study examined records of Medicaid and Medicare patients as a proxy for patients of low SES and elderly patients, respectively. Patients were paired to themselves during in-person and telehealth study periods that were each nine months in duration. The study found a remarkable 71.4% reduction in no-show rates for telehealth visits compared with in-person visits in the same publicly insured patients with T2D. Similarly, various studies evaluating telemedicine across different medical specialties conducted during the pandemic have also found a significant reduction in no-show rates and an improvement in patient satisfaction.26,27 In addition, our study found no significant differences in average HbA1c metrics between patients during in-person and telehealth visit periods. Furthermore, there were no significant differences in the percentages of patients achieving glucose TIR of ≥70%. HbA1c and glucose TIR percentages are well-studied standards in diabetes care to reduce the risks of microvascular complications in patients with T2D. 28
Our study demonstrates a robust improvement in appointment attendance by patients during telehealth visits compared with in-person visits. In addition, telehealth visits were equally effective in achieving optimal diabetes outcomes compared with in-person visits. The reduction of transportation and financial barriers during the telehealth visit period may partially explain the significant improvement in patient visit attendance. These SES barriers have been well established to delay medical care in patients with chronic diseases such as T2D.9,29 Based on the results of this study, telemedicine may be one solution to reduce socioeconomic barriers and improve long-term diabetes outcomes in patients of low SES and the elderly. Reduction in no-show rates overall may lead to better glycemic control, more timely adjustments to medical regimens, and earlier screening for microvascular complications.
Our secondary outcomes included analysis of lipid profiles during the two visit arms of the study. American Diabetes Association (ADA) guidelines recommend an LDL <100 mg/dL, HDL > 50 mg/dL, TRIGS < 150 mg/dL, and total cholesterol < 200 mg/dL to reduce cardiovascular complications in patients with diabetes. 30 Even though the average LDL was below 100 mg/dL for both visit arms as recommended by ADA guidelines, our study results showed a more statistically significant reduction in LDL during telehealth visits compared with in-person visits. On the other hand, triglyceride levels in both visit arms were found to be above the ADA recommended 150 mg/dL, with higher triglyceride levels noted in the telehealth period. These mixed findings may be due to lower quality diets and decreased exercise during the COVID-19 pandemic quarantine restrictions. The HDL and total cholesterol levels showed no significant change between the in-person and telehealth periods. Overall, the lipid panel indices revealed mixed results between the in-person and telehealth visit periods.
This study showed a clear association between telehealth visits and a reduction in no-show rates for patients of low SES status and the elderly population. During the COVID-19 pandemic, multiple similar studies have compared the effect of telemedicine in patients with T2D and have shown either comparable or mixed results.31-33 One systematic review by Wafa and colleagues reported improvements or no change in metabolic markers for T2D such as HbA1c, BMI, and cholesterol. 32 Whereas Russo et al 31 noted a decrease in patient quality of care scores with telemedicine along with a decrease in health screenings associated with T2D when compared with face-to-face visits.
Previous study results and our subsequent findings together suggest the need for an optimized hybrid model, consisting of both in-person and telehealth visits, for patients with diabetes facing socioeconomic barriers to improve chances of realizing their health care goals. Additional studies are warranted to confirm similar reductions in no-show rates with other telehealth models, in the current postpandemic setting where most patients are not isolated in their homes. More specifically, research is warranted to establish a clear association between specific socioeconomic barriers and telemedicine. In the future, telemedicine could become an even more valuable tool for providing more equitable health care for all patient populations.
Strengths and Limitations
An important strength of this project is the adequately powered, large, diverse, sample size of 819 patients compared before and during the COVID-19 pandemic with in-person and telemedicine visit methods. Many previous studies have been conducted showing the benefits of telemedicine but with smaller cohort sizes. 20 The COVID-19 pandemic caused a surge in the use of telemedicine, allowing for a large sample size for our retrospective analysis. Another strength is that our study population matched the demographics of the New Haven population at large in terms of race, sex, and disease comorbidities, as well as insurance status for potentially broader generalizability. 34 Furthermore, our study specifically looked at populations most hindered by socioeconomic barriers, people of low SES, and the elderly.
The main limitation of this study is that telehealth visits occurred during the height of the COVID-19 pandemic. The nine-month telehealth visit period occurred during the lock-down period when no in-person clinic visits were conducted. The pandemic resulted in social isolation, declines in healthy dietary habits, and an increase in stress for the patient population. These are potentially confounding factors which could have minimized the effects of telemedicine on T2D outcomes, especially HbA1c and TIR glucose control metrics. Further studies are warranted to gain a better understanding of the impacts of telemedicine in combination with in-person visits in the postpandemic era. Furthermore, specific income and poverty rates were unavailable given the nature of the health system EMR. Insurance status—Medicaid and Medicare—were used as a proxy for low SES for our study population. A direct association cannot be established between telehealth and specific socioeconomic barriers. However, this study does reveal that comparable diabetes outcomes were achieved between in-person and telehealth time periods among patients facing several socioeconomic barriers suggesting telemedicine visits as noninferior to in-person visits for maintaining glycemic control.
Finally, the digital gap and access to technology are established barriers with patients of low SES and elderly patients with diabetes. It is noteworthy that among the 2540 patients at the Yale Diabetes Center, 898 patients were excluded due to nonparticipation in telehealth visits (Figure 1). In addition, the number of telehealth visits conducted were 1620 in total compared with 3478 total in-person visits. The reduction in total telehealth visits during this nine-month period could be attributed to several challenges faced by patients including technological barriers, structural difficulties in transitioning to telehealth, and other obstacles related to COVID-19 pandemic restrictions, all of which contribute as confounding factors.
Continuous glucose monitor data access and availability continues to be a challenge for providers and their patients during both in-person and telemedicine visits as noted by smaller samples compared with HbA1c data in Table 2. As the COVID-19 pandemic posed data availability challenges across all metrics including CGM data collection, further studies are warranted to reveal more specific causal relationships toward the goal of proposing solutions to resolve these technological challenges.35,36
Conclusion
Our retrospective cohort study of 819 publicly insured patients with T2D reveals that telemedicine significantly reduces no-show rates while achieving comparable glycemic control when compared with in-person visits. Analysis of lipid profile indices reveals a reduction in LDL but an increase in triglycerides during the telemedicine period. Telemedicine visits for patients with diabetes may be one solution to reduce socioeconomic barriers, improve visit attendance rates, and improve long-term T2D management outcomes in patients from low-income populations and elderly patients. Future studies are warranted to develop the most optimized and balanced model of telehealth and in-person services for diabetes management in the postpandemic era.
Footnotes
Acknowledgements
Yale Joint Analytics Team (JDAT), Dr Anderew Arakaki, and Dr Rosana Gonzalez-Colaso.
Abbreviations
ADA, American diabetes association; AGP, ambulatory glucose profile; CGM, continuous glucose monitor; EMR, electronic medical record; HbA1c, hemoglobin A1c; JDAT, joint data analyst team; MRN, medical record number; SES, low socioeconomic status; T2D, type 2 diabetes; TIR, time in range; YMDC, Yale Medicine Diabetes Center.
Declaration of Conflicting Interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: JW, MA, PA-C, is an affiliated medical provider at Yale Medicine Diabetes Center.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
