Abstract
Background:
Annual peaks in temperature and humidity exceed manufacturers’ specifications for blood glucose test strip storage in Thailand. Health Promoting Hospitals (HPH) do not always provide the same level of health services that hospitals do since they often only turn on air-conditioning units during working hours.
Methods:
The blood glucose testing performance of 4 glucose meters were investigated for short and long terms stress at 5 simulated conditions. Temperature and relative humidity (RH) at 5 HPHs in different regions of Thailand were monitored for 9 weeks during April to July 2019. The use of air conditioning in storage rooms for storing test strips was surveyed at 131 HPHs using questionnaires.
Results:
Median-paired differences of glucose measurements with stressed test strips in 5 simulated conditions significantly differed (P < 0.05) both in the short term (3 days) and in the long term (30 days) with 4 glucose meters when compared to unstressed test strips. The average temperature of all HPHs exceeded 30°C (86°F). The average RH was 84%. There was only one HPH that occasionally turned on its air conditioners. Most HPHs kept both opened and unopened vials of test strips in rooms without air conditioners. Further, 21.4-32.0% of HPHs kept test strips at room with air conditioners.
Conclusions:
This study provides evidence for poor performance of blood glucose testing by glucose meters that are affected by adverse environmental conditions. The environmental for test strips storage at HPHs should be considered to prevent analytical errors of glucose measurement.
Keywords
Blood glucose (BG) testing by glucose meter is the most common point-of-care testing (POCT) that is defined as diagnostic testing at or near the site of patient care.1,2 Sub-district Health Promoting Hospitals are hospitals that are operated by the Ministry of Public Health and only have primary care capabilities to often serve people within districts. Blood glucose is commonly performed at the point of need at sub-district health promoting hospitals (HPH) in Thailand for rapid screening risk groups for diabetes mellitus (DM) and monitoring glucose levels for glycemic control to prevent complications among DM patients in communities. 3 A survey on the use of glucose meters found that 93% of HPHs performed BG testing with glucose meters in 2015, which later increased to 100% in 2018.4,5
The performance of BG measurement depends on many factors, including temperature, humidity, user expertise and measurement principle, and the manufacturing technology of the glucose meter and test strip. 6 A previous study had represented 41% and 38% of DM patients in hot weather zone of southwestern United States that known about the effect of heat on glucose meters and test strips, respectively. 7
Thailand is located in tropical climate zone and experiences hot weather throughout the year from 28.1°C (82°F) with minimum temperatures of approximately 2.3°C (36°F) in winter (February 2016) and a maximum temperature of approximately 44.6°C (112°F) in summer (April 2016). Relative humidity (RH) ranges between 72-74% throughout the year and decreases to 62-69% in the summer. Southern Thailand has the highest humidity with average RH ranges of 79-80%.8,9 Previous studied found high temperature and high RH at hospital practices in a tropical clinical setting of Thailand decreased glucose concentrations obtained from a glucose meter with a glucose oxidase-based system. 10 Glucose test strips of 5 test systems were kept at −5°C or at 50°C within 30 minutes had little effect on the glucose measurements when compared to those kept at room temperature. 11 Therefore, the performance of BG testing by glucose meter should be investigated under stressed environmental conditions to prevent potential adverse effects influencing clinical decisions making.
This study investigated the performance of BG testing by glucose meter when test strips were stressed at inappropriate temperatures and humidity in 5 stressed conditions, monitored temperature and relative humidity at actual sites for test strip storage at 5 HPHs in Thailand, and surveyed the test strip storage locations at sub-district HPHs.
Methods
Characterization of Glucose Meters and Test Strips
This study was conducted with 4 glucose meters. Details of enzyme, coenzyme coated on test strips, measurement principles, temperature for storage test strips recommended by the manufacturer, and the operating temperature and relative humidity are shown in Table 1.
Characterization of Glucose Meters and Test Strips and Temperature and Relative Humidity Profile for Stressed Conditions.
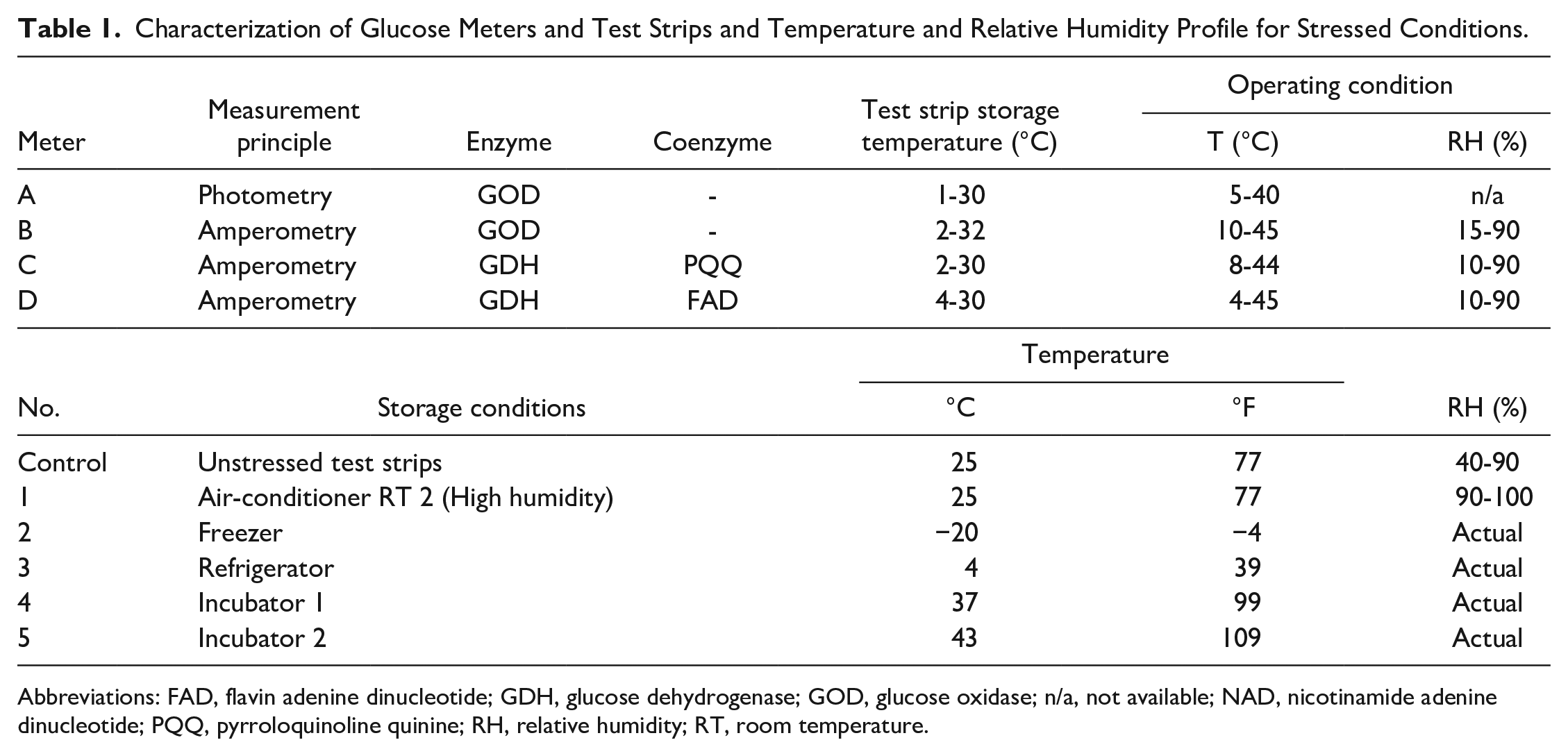
Abbreviations: FAD, flavin adenine dinucleotide; GDH, glucose dehydrogenase; GOD, glucose oxidase; n/a, not available; NAD, nicotinamide adenine dinucleotide; PQQ, pyrroloquinoline quinine; RH, relative humidity; RT, room temperature.
Simulated Conditions for Test Strip Storing
Six conditions were simulated, including air-conditioned RT (unstressed), air-conditioned RT (40-90% RH), airconditioned RT with high RH (>90%), frozen (−20°C), refrigerated (4°C), incubated (35-39°C) and incubated (40-45°C). The temperature and humidity profiles of the unstressed (control) test strips and 5 stressed conditions for test strip storage are presented in Table 1.
Glucose test strips were divided into 3 groups: group 1-short term (3 days with a single use); group 2-long term (30 days after opening the test strip vial 3 times per day, with each vial opening at least 10 minutes after the previous opening); and group 3 – unstressed (control) test strips stored at room temperature (RT).
Test strip groups 1 and 2 were stressed in 5 simulated conditions in parallel with unstressed test strips group 3 as the control group. After being stressed, all 3 test strip groups were used for measurement of BG by 4 glucose meters using blood quality control (QC) materials.
Performance Investigation of BG Testing by Glucose Meters
Two blood QC materials were used for the precision evaluations, Lot no. BG62-001; glucose 110-153 mg/dl and Lot no. BG62-002; glucose 83-115 mg/dl. Precision was performed by measurements of BG testing by glucose meters which was repeated 5 times for each level of blood QC material. Blood glucose data was calculated for median and 95% CI. The median-paired differences of BG testing by glucose meters between stressed and unstressed test strips (the control). Wilcoxon signed rank test was used to compare the differences in medians. P-value at <.05 was statistically significant.
Monitoring of Temperature and Relative Humidity at Sub-District Health Promoting Hospitals (HPHs)
Temperature and relative humidity at actual sites for test strip storage at 5 HPHs were measured and recorded every hour for 9 weeks by calibrated automatic data loggers with acceptable maximum permissible errors (MPE). The 5 HPHs were in Phitsanulok, Kamphaeng Phet, Chiang Rai, Sakon Nakhon, and Songkhla provinces. The locations of the 5 HPHs are shown in Figure 1. Temperature and relative humidity data were monitored during April to July 2019. Means of temperature and RH among HPHs were compared by ANOVA; Tamhane statistic. P-value at <0.05 was statistically significant.
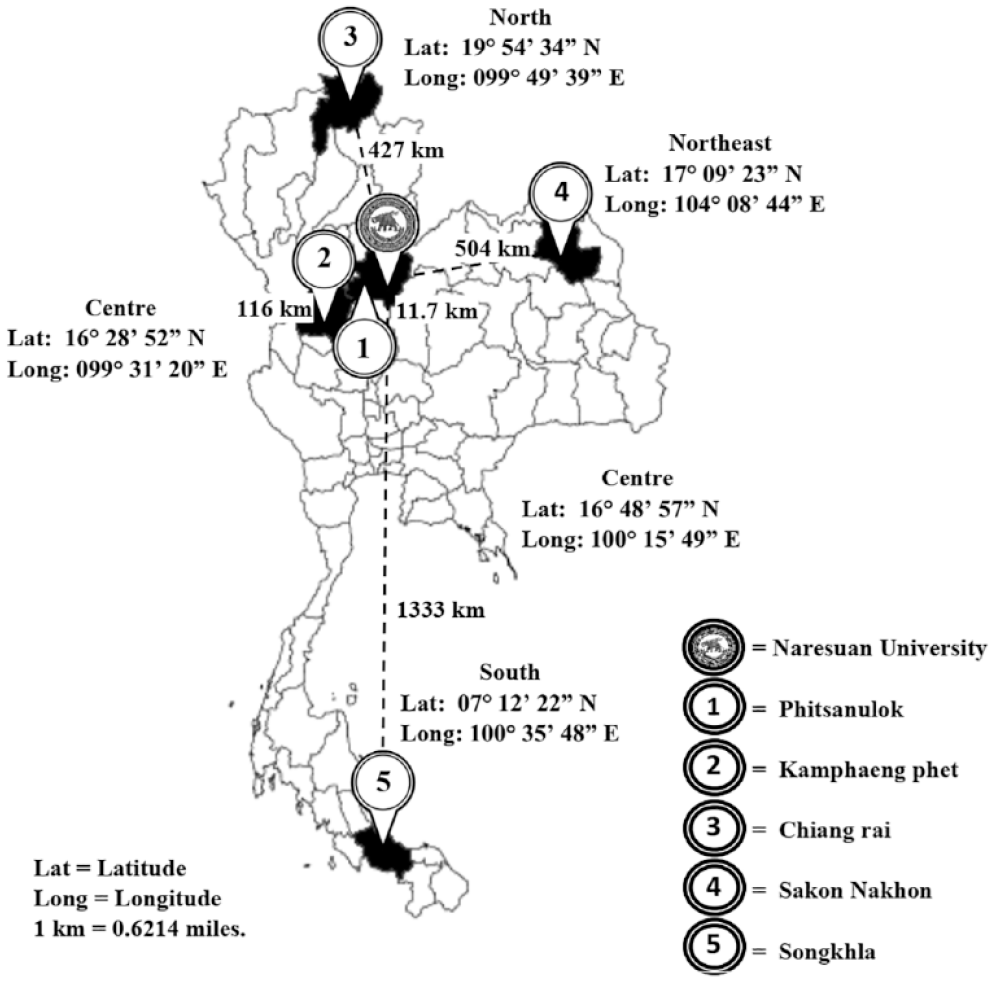
Locations of each provincial HPH in each Thai region in this research to study temperature and relative humidity data which was recorded every hour for 60 days from April to July 2019.
Surveying the Test Strip Storage Locations at Sub-District Health Promoting Hospitals (HPHs)
A questionnaire was distributed among HPH staff related to how they store blood glucose test strips. One hundred and thirty-one HPHs responded to the questionnaire. Descriptive statistics were used for data analysis.
Results
Performance of BG Testing by Glucose Meters When Test Strips Were Stressed in Simulated Conditions
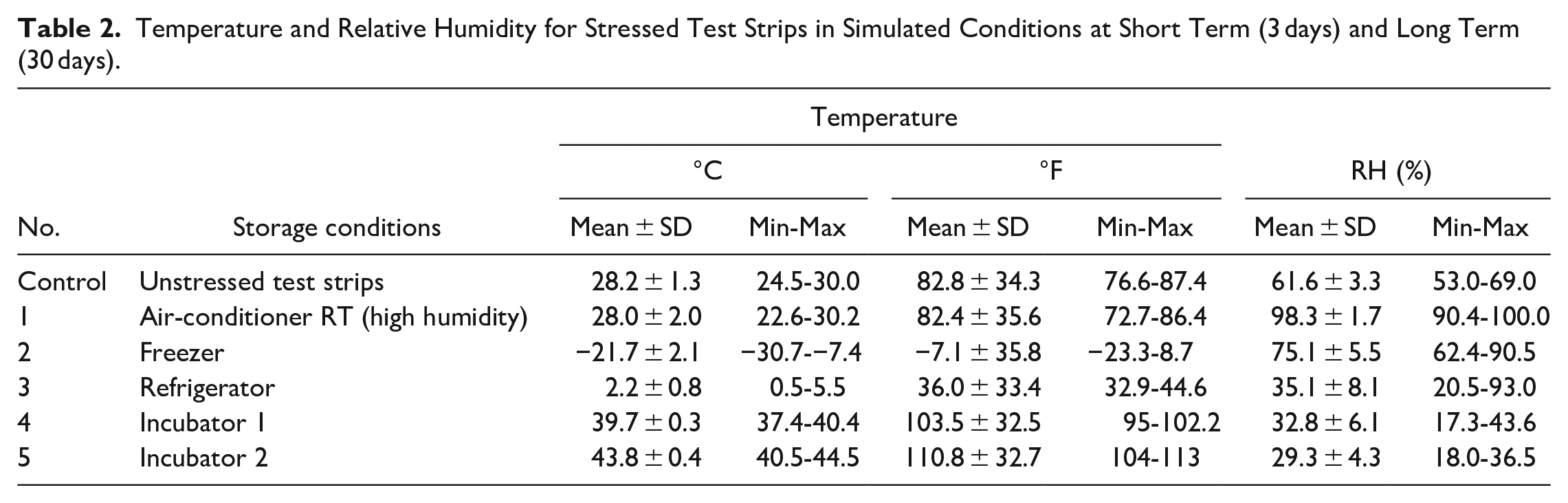
The temperature and relative humidity of the unstressed (control) conditions and 5 stressed conditions are presented in Table 2. The absolute median-paired differences of glucose measurements are shown in Figure 2. Median-paired of glucose measurements with stressed test strips in 5 simulated conditions significantly differed (P < .05) both in the short term (3 days) and long term (30 days) of the 4 glucose meters when compared to unstressed test strips.
Temperature and Relative Humidity for Stressed Test Strips in Simulated Conditions at Short Term (3 days) and Long Term (30 days).
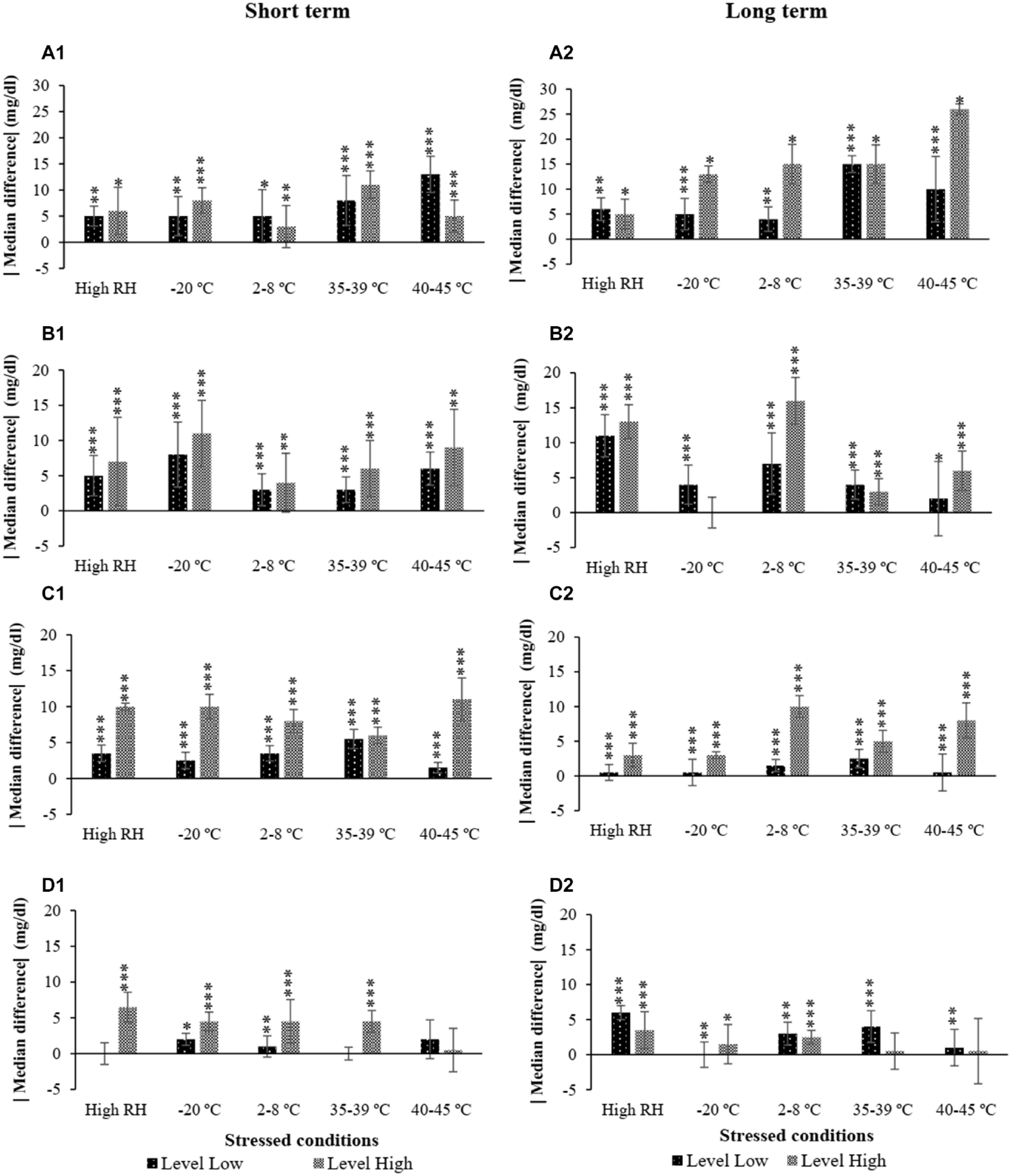
Shows the glucose absolute median-paired differences between stressed and unstressed strips of the 4 principles of glucose meter and test strips. Glucose levels were measured with 2 levels of quality control (QC) materials: low and high. Two storage sets at different temperature and humidity conditions have been tested with short term (A1, B1, C1 and D1) and long term (A2, B2, C2 and D2). (A) Photometry-GOD, (B) Amperometry-GOD, (C) Amperometry-GDH-PQQ, (D) Amperometry-GDH-FAD. Significantly different of median-paired differences by Wilcoxon signed rank test at *P < 0.05, **P < 0.01, ***P < 0.001.
Temperature and Relative Humidity at 5 Sub-District Health Promoting Hospitals (HPHs)
The temperature and relative humidity at test strip storage sites at 5 HPHs are shown in Table 3 and Figure 3. The average temperature of the 3 HPHs exceeded 30°C (86°F) and temperatures exceeded 35°C on some days. The average RH was around 84%. Only one HPH occasionally turned on the air conditioner in the storage room.
Temperature and Relative Humidity Data (n = 1440) From Five Sub-District Health Promoting Hospitals (HPHs) in Thailand Recorded for 8 weeks Period From April to July.
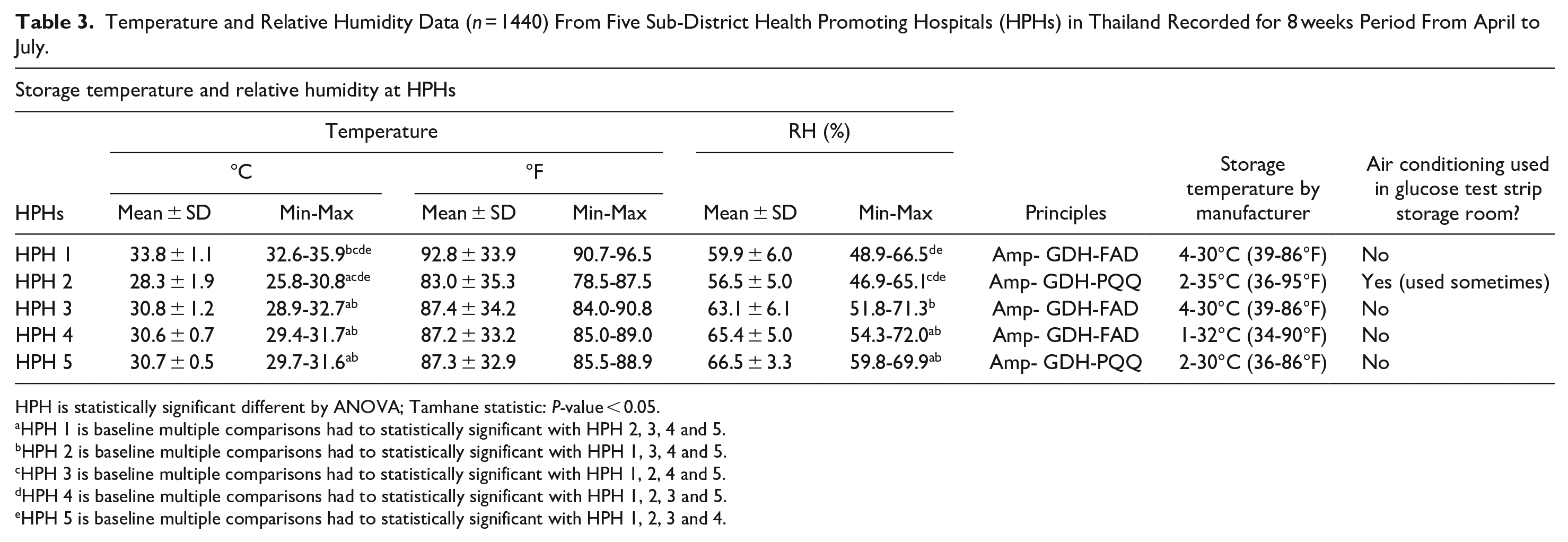
HPH is statistically significant different by ANOVA; Tamhane statistic: P-value < 0.05.
HPH 1 is baseline multiple comparisons had to statistically significant with HPH 2, 3, 4 and 5.
HPH 2 is baseline multiple comparisons had to statistically significant with HPH 1, 3, 4 and 5.
HPH 3 is baseline multiple comparisons had to statistically significant with HPH 1, 2, 4 and 5.
HPH 4 is baseline multiple comparisons had to statistically significant with HPH 1, 2, 3 and 5.
HPH 5 is baseline multiple comparisons had to statistically significant with HPH 1, 2, 3 and 4.
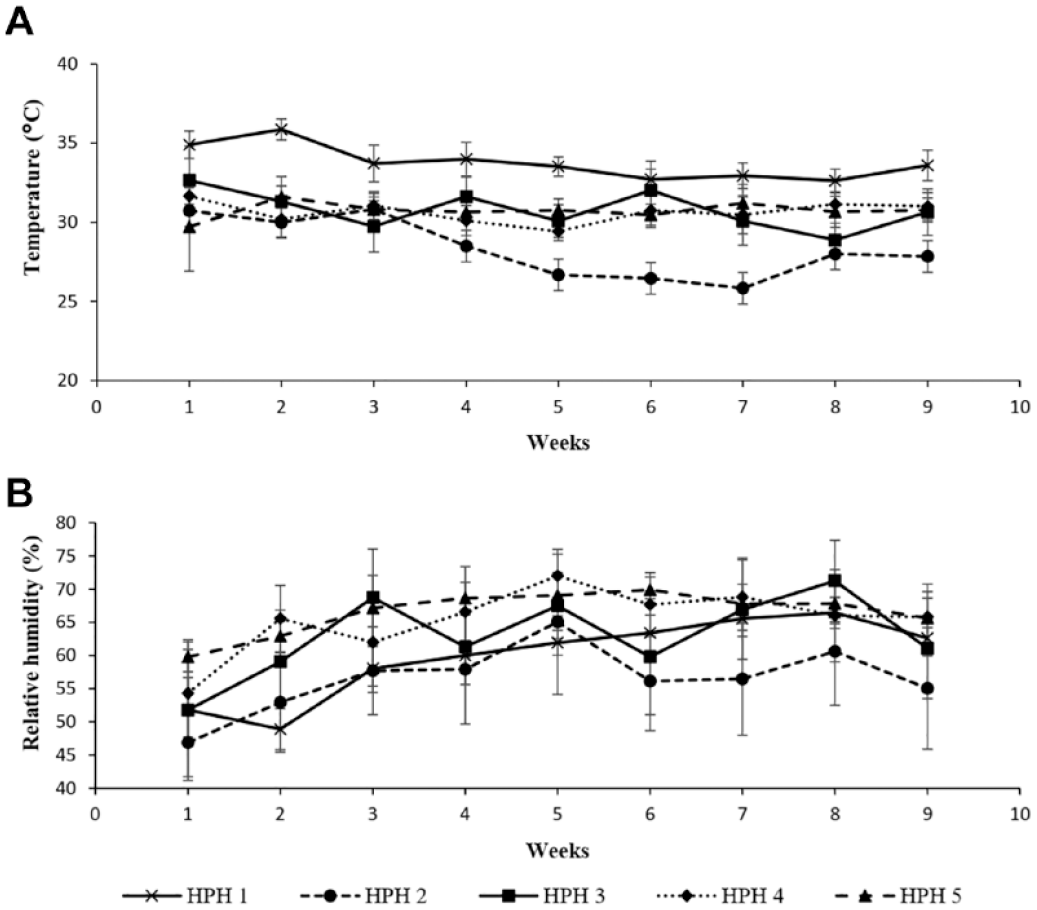
fNine weeks average of temperature and relative humidity recorded every 1 hour (n = 1440) at 5 HPHs in Thailand.
Survey of Storage of Test Strips at Sub-District Health Promoting Hospitals (HPHs)
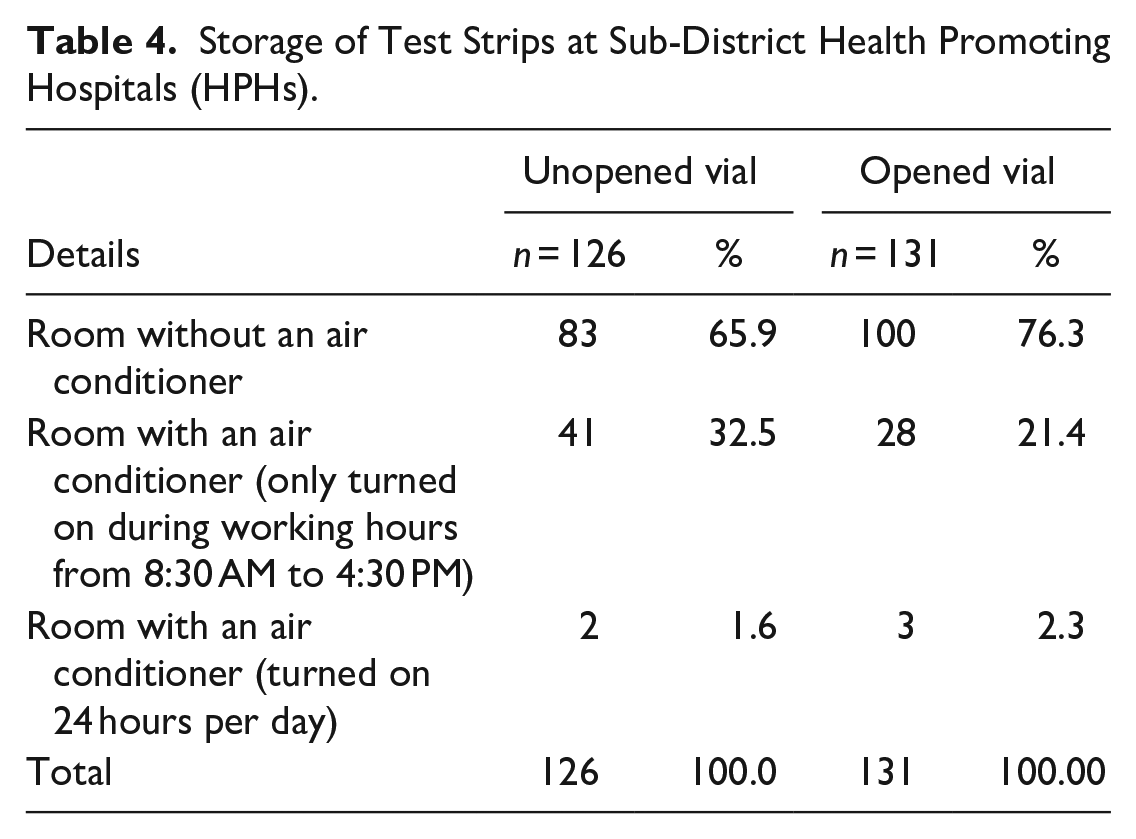
A total of 131 HPHs responded to the questionnaire, with the data presented in Table 4. Most of the HPHs kept both opened and unopened vials of test strips in rooms without air conditioners. Moreover, 21.4-32.0% of HPHs kept test strips at room with air conditioners but the air conditioning units were only turned on during working hours from 8:30 AM to 4:30 PM Monday to Friday. Only 2% of HPHs kept test strips at room with air conditioners turned on for 24 hours per day.
Storage of Test Strips at Sub-District Health Promoting Hospitals (HPHs).
Discussion
Stressed test strips in a short-term was conducted in simulated conditions for 3 days with a single use which is closely related to the actual conditions at diabetes clinics at HPHs and the test strips were used entirely once opened. Most of the 45 HPHs in Phitsanulok, Thailand usually receives test strips from the general provincial network hospitals, which distribute 3 vials on each occasion, with each vial containing fifty strips. 5 The stressed test strips in simulated conditions for 30 days represent long-term storage and daily use of test strips at HPHs. To simulate the routine usage scenarios of blood glucose by glucose meters, test strip vials were opened 3 times per day, with each opening of the test strip at least 10 minutes from the previous opening. Variations in glucose measurements by 4 glucose meters in the long- term condition were greater than the short-term condition.
Five HPHs in Phitsanulok, Kamphaeng Phet, Chiang Rai, Sakon Nakhon, and Songkhla provinces were enrolled in this study, representing HPHs in each region of Thailand. The maximum temperatures in the past 70 years in Phitsanulok, Kamphaeng Phet, Chiang Rai, Sakon Nakhon, and Songkhla Provinces were 42.7°C, 43.6°C, 42°C, 41°C, and 38.6°C, respectively, which typically occurred between March and May. 12 These temperatures exceed manufacture recommendations for storage of test strips. The average annual RH in Thailand did not exceed 72-80% 9 which does manufacture recommendations for operating BG testing by glucose meters. However, some glucose meters in this study had manufacture recommendations to be maintained at RH 10-70%.
A previous study found poor performance of glucose testing by 4 glucose meters when test strips were stressed at 42°C for 15, 30, 45, and 60 minutes as found in disasters. 13 This study shows the variations of blood glucose after incubating the glucose test strips in 5 simulated conditions according to Thailand’s weather profile, especially high temperature and high RH by using temperature 30°C and RH 70% for unstressed test strips. These conditions are similar to the likely temperatures and RH found at HPHs in Thailand and the manufacturer recommendations for test strip storage. 14
Temperature and RH affects the accuracy of point-of- care glucose measurements in hospital practices in a tropical clinical setting by decreasing the glucose concentrations obtained from glucose oxidase based photometric meters. 9 From previous studies, glucose oxidase starts to lose activity at 37°C and up to 80% of enzymatic activity is lost after 30 minutes of incubation at 60°C. This inactivation of glucose oxidase is irreversible. 15 The midpoint thermal of FAD inactivation and dissociation is 59°C and loss of secondary and tertiary structure is 62°C. The FAD dissociation is responsible for inactivation of GOD. 16
Indoor ambient temperature and relative humidity data from the 5 HPHs in Thailand indicated that only one (HPH2) kept test strips in an air-conditioned room which was sometimes turned on. This lowered the temperature and relative humidity data at HPH2 compared to the other HPHs in this study. The temperature and humidity data indicates that 2 of the 5 HPHs (40%) had actual temperatures and humidity ranges within manufacturer recommendations. However, the average temperature of 3 HPHs were slightly higher than manufacturer recommendations (4-30°C, 39-86°F) for test strip storage.
Most of the 131 HPHs kept both opened and unopened vials of test strips in rooms without air conditioners. Less than 32% of the HPHs kept test strips in rooms with air conditioners, but they were only turned on during working hours from 8:30 AM to 4:30 PM on working days since HPHs in Thailand do not always provide the same level of health services as hospitals. Unopened vials of glucose test strips have an expiration date indicated on the vial label and should be kept by strictly following manufacturer recommendations. Opened test strip vials should be used as soon as possible to avoid false results of glucose even though the manufacturer recommends them to be used within 1 month after opening. Moreover, internal quality control by using glucose control solution from manufacturers is necessary to ensure the quality of the meter and test strip before testing with patient samples.
Storage and operating of BG testing by glucose meter should be at room with temperature and humidity within the range of manufacturer recommendation. If temperature and humidity at HPHs are beyond the range of manufacturer recommendations, HPHs should use air conditioners to maintain the temperature near 25°C and RH to below 70%.
A previous study surveyed 55 meters including meters available in Thailand and found that the manufacturer recommendations for glucose test strips storage at 4-30°C for 45.5% and 2-32°C for 27.3%. 14 Blood glucose testing by glucose meter is useful for public health management of DM in the community.17-19 For success in lifestyle intervention, glucose results obtained from glucose meter and operated at HPHs should be accurate. The storage condition of test strip was an influent factor for the accuracy and precision of blood glucose testing by glucose meter, therefore staff at HPHs must consider inappropriate temperatures and RH for test strip storage. The networking hospitals that supply test strips to HPHs should consider improving the environments at medical storage units for appropriate for test strips storage and management for the distribution of disburse glucose test strip vials to prevent analytical errors of glucose measurement according due to limited air conditioners at HPHs.
Limitations
Thailand has 3 seasons, namely summer, rainy, and winter. This study recorded temperature and RH in April to July during the summer season and the middle of the rainy season in Thailand. The investigation should be divided into 3 periods covering 3 seasons to obtain actual annual temperature and RH data at HPHs.
The stressed conditions in this study were static conditions that differed from dynamic actual weather profiles. Further studies should consider using dynamic conditions similar to actual weather conditions at HPHs for accuracy in parallel with an on-site study with ambient indoor conditions.
Conclusion
Blood glucose measurements using 3 glucose meters with the short-term stressed condition were found to be significantly different compared to unstressed test strips. However, glucose measurements based on amperometry-GOD-FAD meter with short term stressed were not significantly different. Variations in blood glucose measurements by all 4 glucose meters with the short-term conditions and long-term stressed condition were significantly different compared to unstressed strips.
Footnotes
Acknowledgements
The authors would like to thank staff of Health Promoting Hospitals that participated in this study.
Abbreviations
BG, blood glucose; DM, diabetes mellitus; FAD, flavin adenine dinucleotide; GDH, glucose dehydrogenase; GOD, glucose oxidase; HPH, health promoting hospital; HPH, sub-district health promoting hospitals; ISO, International Organization for Standardization; MPE, maximum permissible errors; n/a, not available; NAD, nicotinamide adenine dinucleotide; POCT, point-of-care testing; PQQ, pyrroloquinoline quinone; QC, quality control; RH, relative humidity; RT, room temperature; SD, standard deviation; YSI, Yellow Springs Instruments.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was funded by Thailand Science Research and Innovation (TSRI) /R2563B004.
