Abstract
Objective.
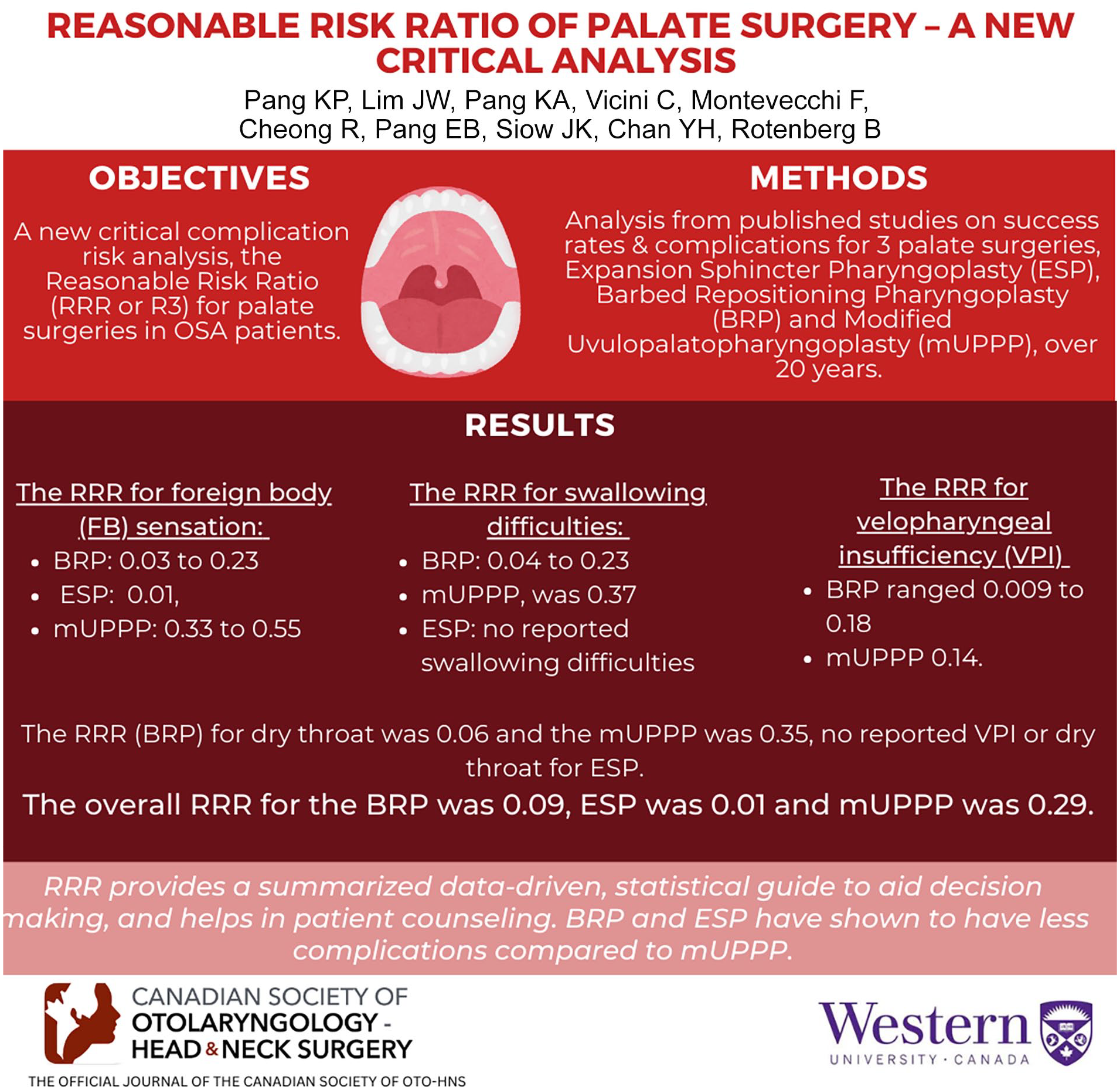
A new critical complication risk analysis, the reasonable risk ratio (RRR or R3) for palate surgeries in obstructive sleep apnea patients.
Methods.
Analysis from published meta-analyses, systematic reviews on success rates, and complications encountered for 3 palate surgeries, expansion sphincter pharyngoplasty (ESP), barbed repositioning pharyngoplasty (BRP) and modified uvulopalatopharyngoplasty (mUPPP), over 20 years. The RRR is derived from a ratio of the percentage of each respective complication over the success rate of that particular surgical procedure. The benchmark RRR of tonsillectomy is set at 0.035 to 0.078. An RRR below this benchmark value is more favorable as tonsillectomy is a widely accepted ENT procedure with risks to benefit well accepted.
Results.
The RRR for foreign body (FB) sensation (BRP) ranged from 0.03 to 0.23 (mean RRR of 0.14), FB sensation (ESP) 0.01, FB sensation (mUPPP) ranged from 0.33 to 0.55 (mean RRR of 0.44). The RRR for swallowing difficulties (BRP) ranged from 0.04 to 0.23 (mean RRR of 0.11), mUPPP, was 0.37; no reported swallowing difficulties with the ESP. The RRR for velopharyngeal insufficiency (VPI) (BRP) ranged from 0.009 to 0.18 (mean RRR of 0.07), and RRR VPI (mUPPP) was 0.14. The RRR (BRP) for dry throat was 0.06 and the mUPPP was 0.35, with no reported VPI or dry throat for ESP. The overall RRR for the BRP was 0.09, ESP was 0.01 and mUPPP was 0.29.
Conclusion.
RRR provides a summarized data-driven, statistical guide to aid decision-making, and helps in patient counseling. BRP and ESP have been shown to have less complications compared to mUPPP.
Introduction
Obstructive sleep apnea (OSA) is a sleep disorder that results in upper airway collapsing during sleep. As the muscles of the upper airway are all relaxed and paralyzed (especially during dream sleep), any form of negative pressure in the upper airway would cause the airway to collapse and close; this results in stoppages in breathing, hypoxemia, sympathetic activation, tachycardia, and hypertension. Anatomically speaking, airway patency is a balance between the container (the craniofacial skeleton) and the contents (the soft tissues, like the tonsils, tongue, palate, lateral walls, sinus turbinates, nasal septum, and adenoids). It would be simplistic to assume that surgical removal of crowded soft tissue content (like the tonsils, palate, and tongue base), would achieve a high level of post-surgical success. Physiological processes are also in play. Eckert described the complex balance of critical Pressure, Arousal threshold, Loop gain, and Muscle responsiveness (PALM scale) which generates the condition of OSA. 1
There is a delicate balance between the anatomical basis of OSA and the above physiological factors (PALM scale) which determine whether a patient would suffer a prolonged apneic episode or cross the arousal threshold into lighter sleep (frontal cortical arousal) aided by increased muscle responsiveness. For the anatomical component, reducing the soft tissue content in the upper airway and thus reducing intra-luminal critical pressure has been shown to benefit the OSA patient. The upper airway collapse in OSA is often multilevel noted at the velopharynx, the base of tongue, and/or the lateral pharyngeal walls. Palatal collapse is the commonest site of obstruction/collapse, the traditional palatal surgery techniques for OSA (namely the traditional uvulopalatopharyngoplasty or their modified versions) have been known to have a higher incidence of postoperative morbidities. The older palatal techniques tend to be more ablative removing a significant amount of the palatal arches, the uvula, and the tonsil pillars as well. The consequent thick fibrotic palatal scar has been known to be associated with dry throat sensation, and velopharyngeal incompetence. Palatal surgery techniques based on more reconstructive principles, address the lateral pharyngeal walls and preserve some or part of the uvula appear to result in less long-term postoperative morbidity.
We sought to investigate the ratio between the mean complication rate (of each respective complication) over the mean success rate of the respective surgical procedure. This reasonable risk ratio (RRR) would aid the surgeon to make an informed decision on the choice of palatal surgical procedure [expansion sphincter pharyngoplasty (ESP), barbed repositioning pharyngoplasty (BRP), and modified uvulopalatopharyngoplasty (mUPPP)] and to provide better preoperative counseling of the respective success rate and complication/s to the patient. A high RRR (high complication or low success rate) would be less favorable.
For ease of reference and simplicity, the authors suggest referring to the reasonable risk ratio as the “R-cube or R 3 ” of a procedure.
Materials and Methods
Search Strategy
We performed a systematic literature search using Medline, Google Scholar, Cochrane Library and Evidence-Based Reviews (from January 2000 to December 2022) databases for keywords of, and procedures that included the expansion pharyngoplasty, ESP, functional expansion pharyngoplasty, barbed pharyngoplasty, BRP, barbed suspension pharyngoplasty, uvulopalatopharyngoplasty, mUPPP, complications, morbidity, success rates and/or results, and in their different combinations and permutations.
Selection Criteria
All relevant studies (adult studies only) published between January 2000 to December 2022 were included. All included studies had to be published in English and those that documented the respective procedure with that respective procedure outcomes, success rate with or without documented complication rates, and/or morbidity rates. We preferred longer post-procedure follow-up duration; we included meta-analysis and systemic review data.
Data Extraction
For studies that met the inclusion criteria, data was extracted into a standardized worksheet. Extracted data included the name of the first author, year of publication, study design, number of study subjects in each treatment group, the description of the surgical procedure, preoperative and postoperative apnea hypopnea index (AHI), their success rates, follow-up duration, and their respective complication rates.
Reasonable Risk Ratio
The primary ratio (known as the RRR) to be derived would be the ratio between that particular complication rate (in percentage) over the success rate of that particular surgical procedure (in percentage). For every procedure, there might be a few known complication/s associated with it, hence, each procedure would have a specifically different ratio of a certain complication over that procedure’s known success rate. For example, for postoperative foreign body (FB) sensation for ESP, the published complication rate might be 1.2%, over (divided by) the published ESP success rate of 80%; hence, the RRR would be 1.2/80 = 0.015. The arbitrarily deemed “reasonable” and/or acceptable rate of a complication would be referenced from the most common ear, nose, and throat procedure performed internationally, which would be the tonsillectomy procedure; hence, the complication associated with this commonest procedure would be the secondary hemorrhage. In general, the secondary hemorrhage rate for tonsillectomy surgery would range from 3.5% to 7.8%. 2 Liu et al reported in these 1438 post-tonsillectomy patients, the serious secondary bleeding that required surgical intervention was 3.5% while the overall admission rate was 7.8%. 2 Based upon the presumption of 100% success rate of the tonsillectomy procedure (tonsillitis does not recur after surgery), the RRR of tonsillectomy ranges from 3.5/100 to 7.8/100 yielding ratios of 0.035 to 0.078. This RRR benchmarks the already widely acceptable complications to success ratio in the common procedure of tonsillectomy.
The RRR is an entity that takes into account the success rate of that particular surgical procedure (as the denominator), hence, if the success rate is higher (more favorable), with the numerator as the complication rate, this would render the RRR more “acceptable” and more “reasonable” as a procedure to be offered to and to be performed for that particular patient. The RRR would provide the surgeon with a good reference and guide in the decision-making process with the overall complication rates and success rates incorporated into 1 ratio. The objective is not to simplify the procedure selection process, but to further filter and streamline the process of informed decision-making, considering the expected/possible complications that might arise based on the likely success rate.
Surgery Techniques
Surgeries were based on previously described palatal surgery techniques. The ESP as described by Pang and Woodson, 3 the functional expansion pharyngoplasty as described by Sorrenti and Piccin, 4 the barbed reposition pharyngoplasty (BRP) introduced by Vicini et al, 5 the mUPPP (uvular preservation or recreation surgically) as described by Li et al. 6
Statistical Method
Meta-analysis was conducted using the Cochrane Review Manager (version 5.3, The Nordic Cochrane Centre; The Cochrane Collaboration, London, England). Random effect models are used to generate pooled estimates for the overall success rates.
The study protocol and methodology were reviewed and approved by the respective hospital Ethics Committee/Institutional Review Board.
Results
In order to obtain the RRR, the higher powered and higher statistically significant studies were utilized, and the pooled average success rate and complication rate of the respective procedures (BRP, ESP, mUPPP) were calculated.
Barbed Repositioning Pharyngoplasty
There were 2 higher powered meta-analyses published on the success rates and complications of the BRP. Neruntarat et al 7 documented an 84.96% success rate of the BRP in 104 OSA patients and a 79.9% success rate in the ESP in 104 OSA patients (Table 1). Saenwandee et al 8 analyzed 20 articles with a total of 762 OSA patients who had the BRP performed, the authors reported an impressive 85.2% success rate, however, the authors also documented a suture extrusion (FB, sensation) rate of 18%, dysphagia (20%), velopharyngeal insufficiency (VPI)/nasal regurgitation (15%), and dysgeusia (3%); the mean follow-up range was 1 to 26 months (average 6 months post-surgery). Iannella et al 9 had 140 OSA patients who underwent the BRP, they assessed their patients post-operatively with the Palate Postoperative Problem Score, at a mean follow-up of 26 months. The authors described a 20% postoperative FB sensation rate, a 9% swallowing difficulty rate, 8% rhinolalia, and 2% nasal regurgitation. Moffa et al 10 performed a systemic review of the complications and side effects of BRP and documented in 14 studies with 769 OSA patients (age range 23-81 years old), with an average of 16 months follow-up, that the long-term complication rates were FB sensation (7.8%), sticky mucus in the throat (5.9%), dysphagia (3.6%), rhinolalia (3.1%), throat phlegm (1.1%), nose regurgitation (0.8%), dry throat (0.6%), and throat lump (0.3%). A study with a longer follow-up time, at 41 months (40 OSA patients), by Pang et al, 11 showed that the complication rate of the BRP lower with, FB sensation (2.5%), swallowing difficulties (5%), sticky mucus/post-nasal drip (10%) and dry throat (5%) (Table 1).
Showing the Respective Success Rates and Complication Rates of the Respective Procedures.

n = number of patients included. References are in superscript.
Abbreviations: BRP, barbed reposition pharyngoplasty; ESP, expansion sphincter pharyngoplasty; mUPPP, modified uvulopalatopharyngoplasty; VPI, velopharyngeal insufficiency.
Reasonable Risk Ratio (BRP)
Utilizing the Saenwandee et al 8 success rate of 85.2%, and the Iannella et al 9 FB sensation rate of 20%, the RRR (BRP) for FB sensation would be 20/85.2 = 0.23. With the Moffa et al 10 FB sensation rate at 7.8%, the RRR (BRP) for FB sensation would be 7.8/85.2 = 0.09 (Table 2). Similarly, with the other studies, an average RRR (BRP) for FB sensation would be 0.14. The average results are as follows (Table 2):
RRR (BRP) FB sensation—0.14
RRR (BRP) swallowing difficulties—0.11
RRR (BRP) voice change—0.07
RRR (BRP) VPI/nasal regurgitation—0.07
RRR (BRP) post-nasal drip—0.09
RRR (BRP) dry throat—0.06
Overall RRR (BRP) (Table 3)—0.09
Showing the Respective Reasonable Risk Ratio of the Respective Procedures.

References are in superscript.
Abbreviations: BRP, barbed reposition pharyngoplasty; ESP, expansion sphincter pharyngoplasty; mUPPP, modified uvulopalatopharyngoplasty; VPI, velopharyngeal insufficiency.
Showing the Respective Reasonable Risk Ratio Rates and Their Overall Average of the Respective Procedures.

References are in superscript.
Abbreviations: BRP, barbed reposition pharyngoplasty; ESP, expansion sphincter pharyngoplasty; FB, foreign body; mUPPP, modified uvulopalatopharyngoplasty; VPI, velopharyngeal insufficiency.
Expansion Sphincter Pharyngoplasty
The most recent and largest meta-analysis performed on the ESP was published in 2023 by Pang et al. 12 Pang et al 12 included 16 studies with 747 OSA patients who had the ESP performed, with a mean follow-up time of 9.5 months (follow-up range 3-36 months). Their mean age was 41.3 years old, mean body mass index was 28.2; their mean pre-op AHI was 32.3, and post-op AHI was 10.0 (P < .05), the mean pre-op ESS 11.4, reduced to post-op 5.3 (P < .05), the mean pre-op snore visual analogue scale (VAS) decreased from 8.7 to 2.9 (P < .05). The overall pooled success rate for all 747 patients was 80.0%. Based on the Pang et al 11 long-term complications of ESP (mean 41 months follow-up, with 84 OSA patients who had the ESP performed) (Table 1), the FB sensation rate was 1.2%, and the post-nasal drip rate was 2.4%.
Reasonable Risk Ratio (ESP)
Utilizing the Pang et al 12 success rate of 80.0%, and the Pang et al 11 FB sensation rate of 1.2%, the RRR (ESP) for FB sensation would be 1.2/80.0 = 0.01. Similarly, with the post-nasal drip rate of 2.4% and a success rate of 80.0%, the RRR (ESP) post-nasal drip would be 2.4/80.0 = 0.02 (Table 2). The average results would be as follows (Table 2):
RRR (ESP) FB sensation—0.01
RRR (ESP) post-nasal drip—0.02
Overall RRR (ESP) (Table 3)—0.015
Modified Uvulopalatopharyngoplasty
He et al 13 in 2019, documented in their meta-analysis, 435 OSA patients (from 11 studies) who had the mUPPP performed, an overall success rate of 55.9% at an average of 23 months follow-up. Tang et al 14 performed a meta-analysis of published data over 40 years, and included 24 studies with 2189 OSA patients, with a mean follow-up of over 12 months (range of 1 month to 20 years). The complications documented included VPI (24 studies, n = 191), difficulty swallowing (7 studies, n = 83), taste disturbances (4 studies, n = 10), voice changes (7 studies, n = 46), FB (9 studies, n = 427), and dry pharynx (7 studies, n = 150). When the authors pooled the 24 studies together, VPI was the least common sequelae reported in 8.1% of the cases. FB sensation was the most commonly reported sequelae at 31.2%, with difficulty swallowing (17.7%), dry pharynx (23.4%), voice changes (9.5%), and taste disturbances (8.2%) being the most to least likely (Table 1). Pang et al 11 had similar postoperative FB sensation rate of 18.7%, post-nasal drip (15.6%), and dry throat (15.6%).
Reasonable Risk Ratio (mUPPP)
Utilizing the He et al 13 success rate of 55.9%, and the Tang et al 9 FB sensation rate of 31.2%, the RRR (mUPPP) for FB sensation would be 31.2/55.9 = 0.55. With the Pang et al 11 FB sensation rate at 18.7%, the RRR (mUPPP) for FB sensation would be 18.7/55.9 = 0.33 (Table 2). Hence, the average RRR (mUPPP) for FB sensation would be 0.44. The average results are as follows (Table 2):
RRR (mUPPP) FB sensation—0.44
RRR (mUPPP) swallowing difficulties—0.37
RRR (mUPPP) voice change—0.17
RRR (mUPPP) VPI/nasal regurgitation—0.14
RRR (mUPPP) post-nasal drip—0.28
RRR (mUPPP) dry throat—0.35
Overall RRR (mUPPP) (Table 3)—0.29
Discussion
The older traditional modified UPPP (mUPPP) technique had its focus on ablating and removing redundant soft palatal tissue, compared to newer palatal surgical techniques that aim to reconstruct and alter the direction of the vector forces within the oro-pharyngeal area during sleep. Due to this old ablative philosophy, complications like velopharyngeal incompetence, constant lump in throat sensation, FB sensation, persistent phlegm in throat, difficulty swallowing, dry throat sensation, and voice change were more common previously. There could be different reasons for this postoperative lump in throat sensation from the mUPPP, some believe that it is related to the thick scar or white band of scar tissue that forms on the edge of the palate, that touches the base of tongue region, while others postulate that the absence of the uvula, might accentuate the phlegm from the nasal cavity dripping posteriorly, like a post-nasal drip. With the introduction of the barbed sutures, the self-locking, and knotless sutures, some patients complain that they can feel the protruding sutures (if not placed correctly and deep enough) like a FB sensation in their throat. Moreover, with the thread placed in the soft palate region, extrusion is always a known potential complication.
Considering the commonest ear, nose, and throat surgery performed (the tonsillectomy procedure), the average secondary hemorrhage rate would range from 3.5% (0.035) to 7.8% (0.078) (2); using this as a benchmark, it would not be unreasonable to accept a comparable rate of complication risk at 0.035 to 0.078 for palatal surgeries for OSA. However, considering that palatal surgeries are more complicated, intricate, and complex (with more possible complications compared to the tonsillectomy procedure), it might be prudent to also include the overall success rate of each individual palatal procedure. Hence, the introduction of the RRR.
Another crucial element of a postoperative complication, should not only be confined to the incidence of the complication but the severity and importance of the complication (some might refer to this as “harm”). A persistent dry throat and/or a FB sensation can be extremely debilitating. Persistent velopharyngeal insufficiency would also be a terrible morbidity to have.
In 104 OSA patients, Neruntarat et al 7 documented an 84.96% success rate of the BRP, while Saenwandee et al 8 reported an impressive 85.2% success rate in their meta-analysis of 762 OSA patients with the BRP done. We utilized the meta-analysis with the larger 762-patient cohort. However, Saenwandee et al 8 also reported a FB sensation rate of 18% (at 6 months follow-up), Iannella et al 9 documented a 20% FB sensation rate at 26 months follow-up, while Moffa et al 10 reported a lower rate of 7.8% (16 months follow-up). Swallowing difficulties after the BRP range from 3.6% 10 to 20% 8 (Table 1). In terms of the patient cohort size, Moffa et al 10 who documented complications at 16 months, had the largest meta-analysis with 769 OSA patients. Utilizing these data, the overall average RRR (BRP) was 0.09.
There are fewer published complications associated with the ESP procedure. Based on the largest meta-analysis of 747 patients who had the ESP done, the pooled success rate was 80.0%. 12 From the author’s review of the 16 articles in 15 years, 12 the main long-term complications were of FB sensation (1.2%) and post-nasal drip (2.4%). 11 Therefore, the overall average RRR (ESP) was 0.015.
Tang et al 14 documented in 2189 OSA patients who had the mUPPP performed, with over a year follow-up duration, comparatively higher complication rates, 31.5% FB sensation rate, 17.7% swallowing difficulties, 8.1% VPI and 23.4% postoperative persistent dry throat. With He et al 13 meta-analysis of 435 OSA patients who had the mUPPP done, the success rate was 55.9% (23 months follow-up). Hence, the overall RRR (mUPPP) was 0.29.
Overall, it can be deduced that the newer reconstructive palatal surgery techniques (like the BRP and ESP) have much less short and long-term complications/side effects, compared to the older palatal ablative techniques (like the mUPPP) that resect the uvula and soft palatal edges resulting in a thick scar and/or hard band of fibrosed tissue. We noted that the reviewed articles did not indicate their respective hemorrhage rates or infection rates post-operatively.
We acknowledge and recognize some shortcomings of this paper:
(a) Some of the articles have patient sample sizes that are relatively small, moreover, some of the individual procedure numbers are even smaller.
(b) As with most multi-center surgical studies and meta-analyses, the individual surgeon performing the procedure may have a slightly different technique and this may contribute to and affect the percentage of the respective success rates and complication rates.
(c) With different multiple article analyses and multiple procedures analyzed, there will inevitably be different sample sizes for each of the respective procedures, ESP, BRP, and mUPPP.
(d) We had to arbitrarily select the “newer” palatal surgery techniques based on the fact that most reconstructive palatal techniques and lateral pharyngeal wall techniques were mostly the ESP and BRP, and those procedures with relatively larger meta-analyses that have been published.
(e) Unfortunately, with the utilization of different articles for different procedures, the follow-up durations of each procedure is also different.
(f) As this study is the first to describe and introduce the concept of the RRR in palate surgery, more investigative work needs to be performed to validate this new RRR of palate surgery.
(g) The RRR is not meant to imply nor suggest that ESP is a better procedure, the selection criteria before any surgery, should be based on robust diagnostic criteria (like clinical examination, polysomnogram [PSG] and drug induced sleep endoscopy [DISE]). The RRR is actually to aid surgeons decide for themselves if the clinical exam and/or DISE suggests doing a particular surgical procedure, then the surgeon has a better idea of what sort of complications to expect postoperative and its incidence over the likelihood of its success rate. The RRR is NOT a preoperative selection criterion in itself.
Conclusion
With the introduction of newer reconstructive palatal surgery techniques, the incidence of complications and side effects of the respective procedures are much reduced compared to the older palate surgery techniques. However, because their success rates are also different, sleep specialists need to be cognizant of the various success rates and complications rates combined; therefore, we introduce this new RRR that better aids the surgeon make an informed decision on which procedure to perform in and to allow better preoperative counseling of the respective success rate and complication/s to the patient.
Footnotes
Acknowledgements
None.
Author Contributions
All the authors have contributed substantially to the research, writing and production of this article.
Availability of Data and Materials
All data and materials are available for analysis upon requests; all data are obtained from meta-analysis of the referenced stated publications as stated and indicated.
Consent for Publication
All the above authors consent and agree to the publication. There are no patient personal data involved in this meta-analysis.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethics Approval and Consent to Participate
The study has been approved by the ethics committee and the Institute Research Board. As this is a meta-analysis, there are no primary first-hand direct human subjects involved in this meta-analysis.
