Abstract
Background
Challenges in accessing comprehensive sexual and reproductive health (SRH) information and care leave many individuals with spina bifida (SB) vulnerable to unmet SRH needs, risking unfulfilling sexual experiences and increasing susceptibility to coercion and abuse. Accurate tools are essential to measure SRH knowledge and self-efficacy in adults with SB.
Objective
This study aimed to evaluate the internal consistency and construct validity of domains of a newly developed survey that assesses SRH knowledge and self-efficacy in partner and provider discussions among adults with SB.
Methods
The SRH survey, recently validated for content, was distributed via REDCap with support from the National Spina Bifida Association (SBA) through social media, including SBA's Facebook, and the Adult Advisory Committee. Responses were de-identified, and each participant received a unique survey ID. Internal consistency of the self-efficacy subscales was assessed using Cronbach's alpha and Kuder-Richardson Formula 20 (KR-20) was used for the knowledge scale. Principal component analysis (PCA) evaluated scale structures. Analyses were conducted using SPSS.
Results
Ninety participants completed the SRH survey. Most respondents were female (75.5%). Participants’ ages ranged from 18 to 77 years (mean = 40.47, SD = 12.897) and 85.6% identified as non-Hispanic White. Both the self-efficacy scale for partner discussions (α = 0.914, five items) and provider communication (α = 0.958, eight items) had excellent internal consistency. PCA supported construct validity, with a single-factor structure explaining 75.3% of variance for partner communication and 78.0% for provider communication, indicating that each set of items measures a cohesive underlying construct of self-efficacy within its respective communication domain. KR-20 indicated low internal consistency for the SRH knowledge scale (KR-20 = 0.426, 11 items), likely due to limited response variability.
Conclusion
The SRH self-efficacy scales for partner and provider communication demonstrated excellent internal consistency (reliability) and construct validity among adults with SB. In contrast, limited variability in knowledge responses suggests that the current knowledge scale may require refinement to better capture differences in SRH knowledge across individuals.
Keywords
Lay summary
Adults with spina bifida often receive little guidance about sexual and reproductive health, which can affect their safety, relationships, and ability to communicate with partners and healthcare providers. This study tested a new survey designed to measure how confident adults with spina bifida feel when discussing sexual and reproductive health, as well as what they know about these topics. Ninety adults completed the survey online. Results showed that the survey reliably measured confidence in talking with both partners and healthcare providers. However, most participants answered the knowledge questions in similar ways, suggesting that the knowledge section of the survey may need improvement to better capture differences in what people know. Overall, this survey shows promise as a tool to support better communication and education around sexual and reproductive health for adults with spina bifida.
Introduction
Individuals with disabilities, including those with spina bifida (SB), often face significant barriers when seeking sexual and reproductive health (SRH) services.1–6 Studies show that healthcare providers, caregivers, and educators frequently hold misconceptions, such as viewing individuals with disabilities as asexual, that further contribute to their lack of access to SRH education and care.5,7,8 As a result, only approximately 5% of adults with SB report ever having discussed their sexual health with a healthcare professional.6,9–11 Studies show that most were unsure if the SRH education they received in school applied to them, as it was typically delivered in a general setting and focused on individuals without disabilities. 8 This lack of access to SRH care and knowledge can lead to negative health outcomes and increased vulnerability to sexual abuse and coercion.5,12,13
Most adults with SB express the desire for sexual intimacy and relationships; however, they report unique challenges related to social isolation, dating, and perceived barriers to sexual intimacy including fear of painful intercourse and bowel and bladder leakage.10,14–16 Despite this, 50% of adults with SB report being sexually active by age 23.9,14,16 Both men and women with SB often have limited knowledge about their reproductive health, sexual function, and how the challenges associated with SB affect their ability to have positive sexual satisfaction and intimacy.14,16–20 In fact, approximately half of adults with SB report dissatisfaction with their sex lives, which impacts overall quality of life (QOL) since QOL is directly affected by sexual satisfaction.14,21 This lack of knowledge and care, in combination with the fact that adults with SB have a strong desire for more information regarding their SRH, increases the importance of finding creative ways to implement sexual health discussions in the clinical setting.9,22
Health care providers, including those in well-established, interdisciplinary SB clinics, report significant challenges and apprehension in discussing SRH with their patients with SB. 22 Although the Spina Bifida Association (SBA) has issued guidelines encouraging patient-centered SRH discussions for individuals with SB, standardized approaches for delivering this education remain limited. 14 Additionally, gaps persist in understanding how individuals with SB prefer to receive SRH information. Psychometrically sound tools are essential to accurately assess SRH knowledge, self-efficacy, and sexual risk profiles. They enable reliable data collection to inform targeted interventions and patient-centered care. Currently, few tools exist to measure SRH constructs specifically for adults with SB. This hinders providers’ ability to address unique SRH needs and evaluate the effectiveness of SRH education in improving outcomes. Developing and validating these tools is critical for advancing SRH education, determining individual SRH needs in the clinic, and enhancing quality of life for adults with SB.
Medical advancements have significantly improved life expectancy for individuals with SB, which makes the need for access to SRH care, education, and screenings even more critical.23,24 In a prior study by this institution, content validation was established for a SRH survey using a modified Delphi method. 25 The Sexual Practice, Abuse, Risk, Knowledge, and Self-Efficacy (SPARKS) Survey was developed to address critical gaps in understanding SRH among adults with SB. The SPARKS Survey assesses five domains: sexual knowledge, current sexual practices, risky behaviors, experiences of abuse, and self-efficacy in sexual health. This study focuses on the psychometric evaluation of the sexual knowledge and self-efficacy sections, specifically assessing internal consistency, reliability and construct validity in this population.
Methods
Preliminary survey development
Institutional Review Board approval was obtained from The University of Alabama at Birmingham (UAB) (IRB-161021001) for the development and evaluation of a de-identified sexual health survey assessing intimacy, sexual and reproductive knowledge, and sexual abuse individuals with in SB. The survey was initially vetted locally in the UAB adult SB clinic. 25 Following preliminary data and a targeted literature review, the survey was revised, and a modified Delphi method was used to establish content validity. 26
Survey instrument
The survey consisted of six parts. Based on their answers to specific parts, branch logic was used to guide additional follow up questions. For example, participants were routed to sex-specific questions based on sex assigned at birth. The first part was concerned with demographic variables which included, sex, sexual orientation, race, ethnicity, age, education status, who resides in their home, and various diagnosis specific questions (type of SB, functional level of lesion, ambulation status, presence of hydrocephalus, and bladder management). The second part measured their baseline sexual health knowledge with 11 true/false questions and one multiple choice question. This section also included general questions about where they received education on SRH. The third part of the survey included questions on their current and past sexual practices including dating history and sexual experiences. The fourth part was concerned with their sexual safety and risk profile. This section included both sexual and general risky behavior. The fifth part included questions on historical and current sexual, emotional, and physical abuse. The final section was related to self-efficacy to discuss SRH with their partner(s) and/or their medical team. These questions were designed in a 5-point Likert format, from “strongly disagree” to “strongly agree.” Particular attention was given to provide respondents the option to select “prefer not to say.” In this study, internal consistency and construct validity was determined only for the true/false questions in the knowledge/education domain and the full self-efficacy domain. For clarity, item-level results are referred to by their assigned codes (e.g., SK_1, SE_3) throughout the manuscript. Full item descriptions are included in Tables 1, 2 and 3.
Item-Total: Self-Efficacy with Partner.

*The “Corrected Item-Total Correlation” measures how well each item correlates with the overall scale score, excluding the item itself. This statistic is used to determine how well an item fits within the rest of the scale. Higher values indicate that the item is consistent with the other items in the scale.
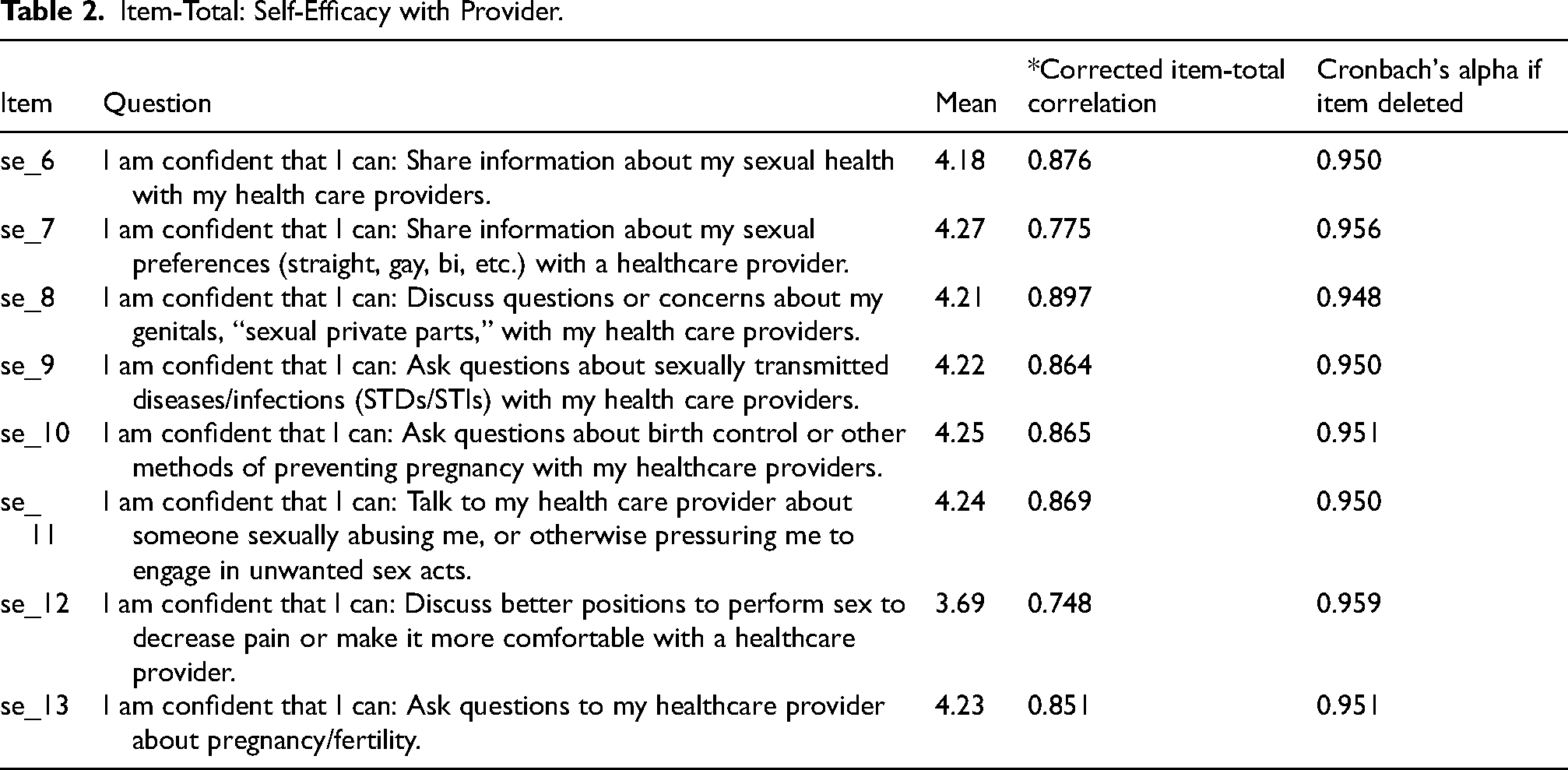
Item-Total: Self-Efficacy with Provider.
Item Analysis of Sexual Health Knowledge Items.

*SK12 and SK13 were scored as correct only if participants selected the single correct option and no incorrect options.
Sample
The sample consisted of 90 adults with SB recruited through the national SBA to increase the likelihood of a representative sample from this population. Eligibility criteria included individuals aged 18 years or older, diagnosed with SB, and able to complete an online survey written in English.
Exploratory factor analyses (EFAs) using principal component analysis (PCA) as the extraction method were conducted on two self-efficacy subscales. The partner communication subscale included five items, yielding a participant-to-item ratio of 18:1. The provider communication subscale included eight items resulting in ratio of 11.25:1. This sample size was considered sufficient for factor analysis based on established guidelines for participant-to-item ratios. 27 Accordingly, the sample size was deemed sufficient to support robust factor analysis for both subscales.
Data collection
Data were collected through an online survey hosted on REDCap, a secure, web-based platform. The survey link was distributed via the SBA Facebook page and through collaborations with the SBA Adult Advisory Committee, which helped promote the survey to additional adult SB groups. To encourage participation, the survey was also shared within social media communities associated with SB. To protect confidentiality, each participant was assigned a unique, de-identified survey ID.
Data analysis
Demographic characteristics of the sample were described using frequencies. Internal consistency was assessed using Cronbach's alpha for the partner communication self-efficacy subscale (five items) and the provider communication self-efficacy subscale (eight items). The Kuder-Richardson Formula 20 (KR-20) was used for the sexual health knowledge scale, which consisted of true/false (binary) items. Assumptions for the use of Cronbach's alpha were evaluated by examining item-level skewness and kurtosis. The partner and provider self-efficacy subscales were analyzed independently due to their clinical distinction. Individuals may feel confident discussing SRH with a partner but not with a healthcare provider (or vice versa), representing conceptually distinct domains of communication self-efficacy. These analyses were conducted separately to evaluate the internal consistency reliability of each domain. To assess the convergent relationship between the two subscales, a Pearson correlation coefficient was calculated between their total scores.
Corrected item-total correlations were also calculated for each item within the partner and provider self-efficacy subscales to assess item performance. These correlations reflect the extent to which each item aligns with the overall construct by correlating with the total score of the remaining items. Items with low correlations were flagged for review; however, all items in both subscales demonstrated strong contributions to their respective scales. 27
EFA was used to examine the underlying structure of the self-efficacy items, following established best practice guidelines for factor analysis reporting. 28 Separate EFAs were conducted to evaluate the construct validity of the self-efficacy items for communication with a partner and communication with a healthcare provider. Prior to each analysis, assumptions for factorability were assessed using the Kaiser-Meyer-Olkin (KMO) measure of sampling adequacy and Bartlett's test of sphericity. PCA was chosen as the extraction method as an appropriate data reduction technique for initial scale validation. Factors were retained based on eigenvalues greater than 1.0, and the percentage of variance explained was used to evaluate model strength. Item loadings ≥ 0.40 were considered acceptable indicators of the underlying construct. Due to low internal consistency and binary response format, EFA was not conducted on the sexual knowledge items, limiting further psychometric analysis for that domain.
All analyses were conducted using SPSS, version 29.0.2.0, to confirm the reliability and construct validity of the knowledge and self-efficacy domains.
Results
Participants
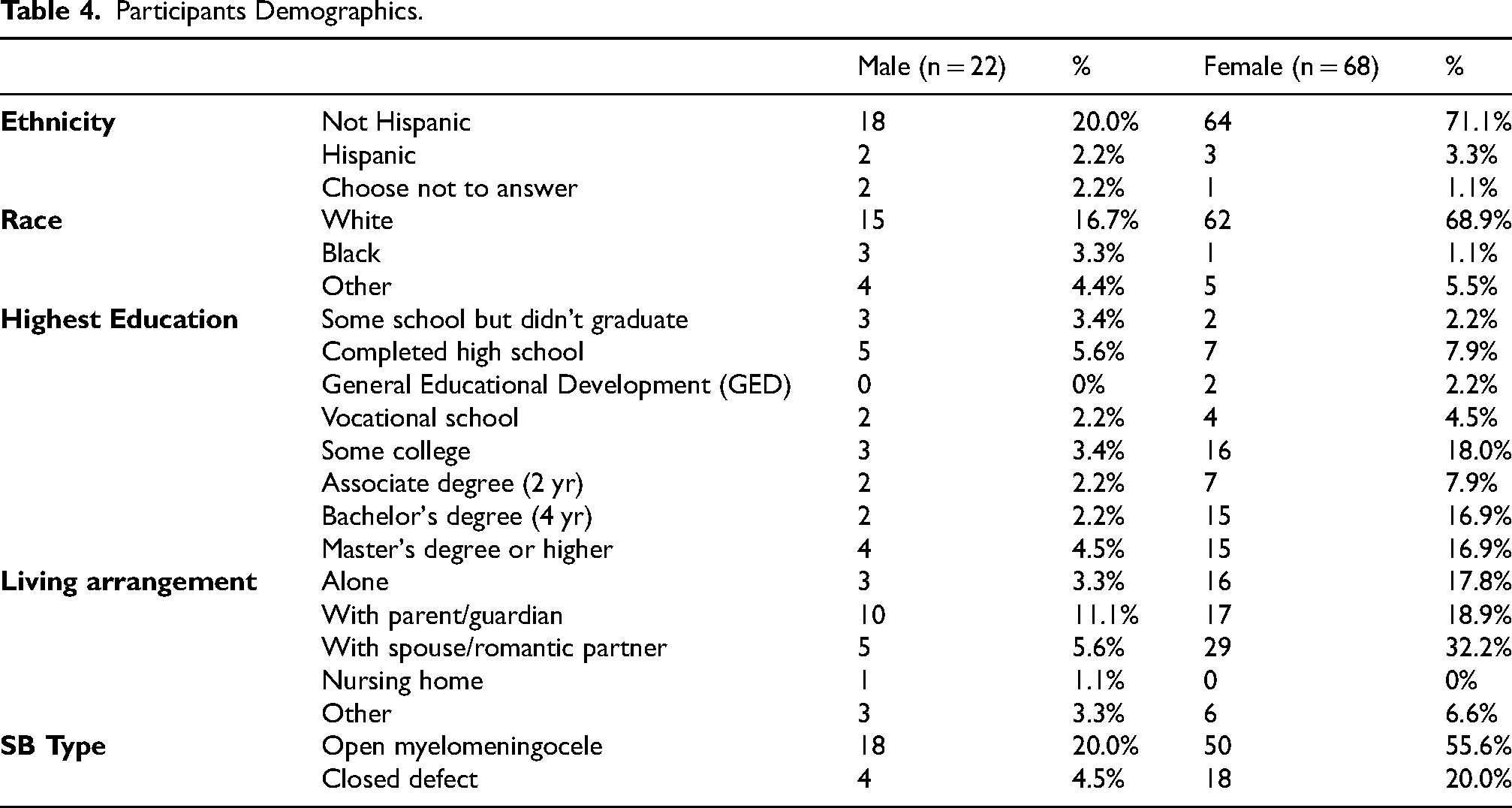
As seen in Table 4, the survey was completed by 90 adults with SB. Most participants (97.5%) filled out the survey alone but two indicated that they filled it out with a family member. In this sample, most respondents (68) indicated that they were born female (74.7%) with males representing 24.2%. Most respondents identified themselves as non-Hispanic (90.1%), White (84.6%), and heterosexual (72.2%). Regarding education, the most common categories were some college and a master's degree (each 20.9%), followed by a bachelor's degree (18.7%), high school diploma or General Educational Development (GED) only (15.4%), an associate degree (9.9%), vocational school (6.6%), and not completed school (5.5%). Living arrangements varied, with 37.4% living with a spouse or romantic partner, 29.7% living with a parent or guardian, and 20.2% living alone. Most participants had open myelomeningocele (74.7%), with 25.3% having a closed defect.
Participants Demographics.
Internal consistency
To evaluate the assumptions required for internal consistency analysis using Cronbach's alpha, skewness and kurtosis were examined for each self-efficacy item. Skewness values ranged from −1.92 to −0.71 and kurtosis values ranged from −0.38 to 3.92, indicating acceptable levels of normality for Likert-scale data. These results support the appropriateness of using Cronbach's alpha for assessing internal consistency in the self-efficacy scales.
The partner communication self-efficacy subscale demonstrated excellent internal consistency, with a Cronbach's alpha of 0.914 across five items (Table 5). Corrected item-total correlations ranged from 0.669 to 0.850 (Table 1). The highest correlation was observed for confidence in refusing unwanted sexual activity (SE_3, 0.850), while the lowest was for sharing medical information with a partner (SE_1, 0.669). Deletion of any item did not improve the scale's reliability, with alpha values remaining high (0.879 to 0.921) if an item was deleted.
Internal Consistency.

The provider communication self-efficacy subscale also demonstrated excellent internal consistency, with a Cronbach's alpha of 0.958 across eight items (Table 5). As shown in Table 2, corrected item-total correlations ranged from 0.748 to 0.897. The highest correlation was observed for confidence discussing genitals/ “sexual private parts” with a provider (SE_8, 0.897), while the lowest was for sharing information about sexual orientation (SE_12, 0.748). Cronbach's alpha remained above 0.94 with any single item removed, indicating that all items contributed meaningfully to the scale.
While the two subscales were analyzed separately, the combined 13-item self-efficacy scale also demonstrated strong internal consistency (Cronbach's alpha = 0.965), further supporting the strength of the full self-efficacy domain (Table 5). A Pearson correlation was conducted to assess the relationship between the partner and provider self-efficacy subscales. Results indicated a strong, statistically significant positive correlation (r = 0.852, p < 0.001). This suggested that individuals who reported greater self-efficacy in communicating with a partner also tended to report higher self-efficacy when communicating with healthcare providers.
In contrast, the sexual health knowledge scale, consisting of 11 true/false (binary) items, demonstrated low internal consistency, with a KR-20 of 0.426 (Table 5). As shown in Table 3, most items were answered correctly by more than 90% of participants, with five items (SK_1, SK_4, SK_5, SK_10, and SK_11) exhibiting near-ceiling effects (≥ 99% correct). Item-level variance ranged from 0.000 to 0.074, further supporting restricted variability. Due to the binary nature of the items, limited item variance, and violation of assumptions required for principal component analysis (e.g., continuous and normally distributed data), PCA was not conducted on this domain. These psychometric limitations reduce the scale's ability to detect differences in sexual health knowledge and preclude its inclusion in further factor analysis.
EFA
For the self-efficacy partner communication scale (five items), the KMO was 0.854, and Bartlett's test of sphericity was significant (χ2(10) = 316.692, p < 0.001), indicating factorability of the data. One factor emerged with an eigenvalue of 3.77, explaining 75.3% of the total variance. Factor loadings ranged from 0.774 (SE_1) to 0.912 (SE_3), and communalities ranged from 0.599 to 0.832 (Table 6).
Principal Component Analysis for Self-Efficacy: Partner Communication Subscale.

Extraction method: principal component analysis. One factor extracted. Kaiser-Meyer-Olkin (KMO) = 0.854; Bartlett's test χ2(10) = 316.692, p < 0.001. Eigenvalue = 3.77; variance explained = 75.3%.
For the self-efficacy provider communication scale (eight items), the KMO was 0.858 and Bartlett's test was also significant (χ2(28) = 820.339, p < 0.001). A single factor was extracted with an eigenvalue of 6.240, accounting for 78.0% of the variance. Factor loadings ranged from 0.799 (SE_12) to 0.925 (SE_8), and communalities ranged from 0.638 to 0.855 (Table 7). These results support the unidimensional structure of both subscales and suggest that each domain captures a distinct yet cohesive aspect of SRH communication self-efficacy.
Principal Component Analysis for Self-Efficacy: Provider Communication Subscale.
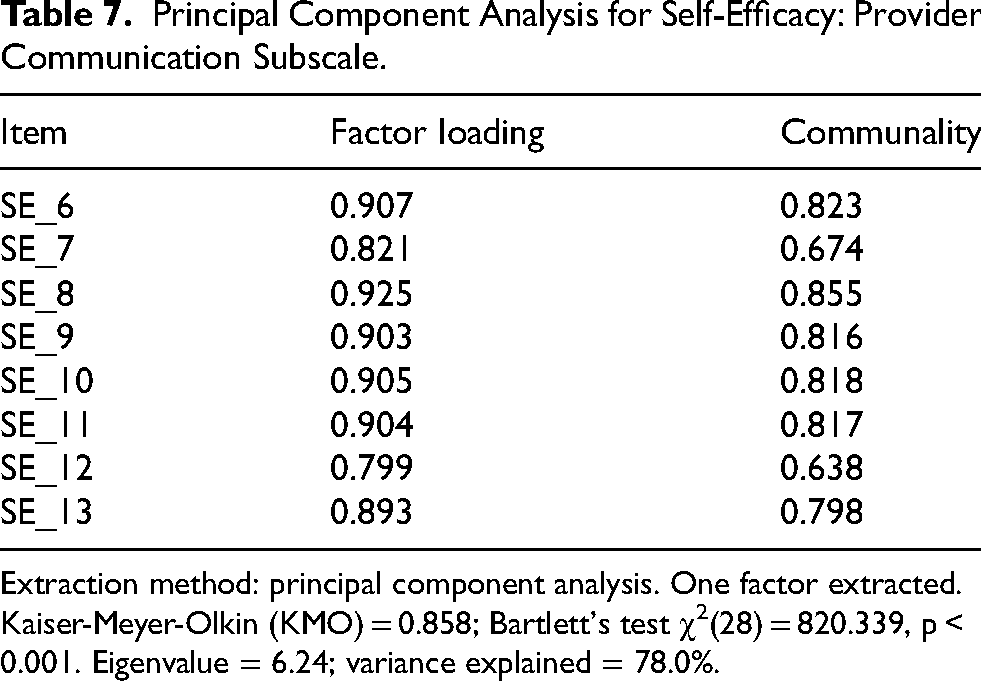

Extraction method: principal component analysis. One factor extracted. Kaiser-Meyer-Olkin (KMO) = 0.858; Bartlett's test χ2(28) = 820.339, p < 0.001. Eigenvalue = 6.24; variance explained = 78.0%.
Discussion
Self-efficacy plays a crucial role in influencing learning and behavior, particularly in health-related contexts. It affects how well a message is heard, understood, and trusted, and how effectively new knowledge is translated into practice. Grounded in social cognitive theory developed by Bandura, self-efficacy has been shown to be a strong predictor of behavior change, including in populations with physical disabilities. 29 Measuring SRH knowledge and self-efficacy with this survey can provide insight into how these domains influence SRH behavior, particularly in areas such as risky sexual behavior, partner communication, and abuse screening. The survey's focus on self-efficacy provides a mechanism to explore how SRH literacy, access to information, and confidence in seeking SRH care from providers relate to SRH outcomes in adults with SB. Given the predictive power of self-efficacy in behavior change, this survey holds potential for guiding effective, theory-driven SRH interventions. 30
Consistent with this theoretical framework, this study demonstrated that the self-efficacy scale to communicate SRH with a partner and the self-efficacy scale to communicate SRH with health professionals in adults with SB exhibit high internal consistency and strong construct validity. While the two subscales were highly correlated (r = 0.852), they were retained as distinct domains due to their clinical relevance. This relationship supports both the internal coherence of the construct and its convergent validity. The combined 13-item scale also demonstrated excellent internal consistency (Cronbach's α = 0.965), but EFA supported a two-factor solution, with items loading most strongly onto their intended subscale. Communicating about SRH with a partner versus a healthcare provider involves different social dynamics, goals, and comfort levels, differences consistently emphasized by both stakeholders and clinical experts during survey development. Although the high alpha values (Cronbach's α > 0.90) could suggest potential item redundancy, expert review affirmed that each item captured a clinically meaningful aspect of SRH communication, and no items were removed. These findings support the psychometric strength and clinical utility of the survey as a tool for assessing SRH-related self-efficacy in adults with SB.
The knowledge scale, by contrast, demonstrated low internal consistency and was therefore excluded from construct validity analyses. The low variability observed in SRH knowledge responses suggests that participants possess a consistently high level of basic SRH knowledge, potentially due to their age at the time of survey, prior education, or healthcare experiences. This uniformity may indicate that the knowledge questions are too basic for this population. Future revisions of the survey could include more nuanced or advanced items to capture a broader range of knowledge. Alternatively, the current knowledge questions could be retained as a preliminary assessment tool, ensuring a foundational understanding while highlighting more complex knowledge gaps. Additionally, establishing that participants possess basic SRH knowledge is valuable for future analyses of other survey domains, such as risky sexual behavior, sexual practices, and experiences of abuse. Confirming that participants have foundational SRH knowledge will strengthen the interpretation of responses in these areas, providing context for understanding behaviors and experiences. Expanding the scope of the knowledge items in future studies could improve the sensitivity of this measure and provide a more comprehensive picture of SRH knowledge in adults with SB.
Previously, content validity was established for this survey, and, to the authors’ knowledge, this is the first survey developed and psychometrically tested to assess SRH in adults with SB. This tool offers a potential resource to help clinicians meet the SBA guidelines for patient-centered SRH discussions. It provides a standardized method for delivering information, determining relevant content, and tailoring communication to individual preferences. Providers have expressed a desire to engage in these discussions but often report a lack of knowledge and training in SRH communication with this population. Since this survey demonstrates content validity and the self-efficacy scales have high internal consistency and construct validity, it could be used to enhance SRH discussions with adults with SB in three key ways: (1) identifying knowledge gaps, (2) evaluating the effectiveness of SRH education interventions, and (3) serving as a clinical tool for providers initiating SRH conversations. Clinicians could use the survey to assess baseline SRH knowledge and practices among adult patients with SB, facilitating more open and informed discussions as well as providing more tailored SRH interventions.
Limitations
This study has several limitations that should be considered when interpreting the findings. First, while the self-efficacy subscales demonstrated high internal consistency and evidence of construct validity, the binary true/false format of the knowledge items limited their psychometric evaluation. Specifically, the knowledge scale did not meet assumptions for factor analysis, and its internal consistency was low, as assessed using the KR-20. As a result, no claims about construct validity can be made for this domain. Additionally, the low variability in responses suggests that the knowledge questions may have been too basic for this sample, potentially limiting the scale's sensitivity in detecting differences in SRH knowledge. This may affect interpretations of how knowledge relates to other domains, such as risky sexual behavior or self-efficacy. Third, although test-retest reliability was initially planned, only eight participants completed the follow-up survey, which was deemed insufficient for meaningful analysis. Therefore, test-retest reliability was not assessed and should be examined in future studies. Finally, the sample may not fully represent all adults with SB, particularly those with lower literacy levels or high caregiver dependence. These individuals may experience challenges in independently completing the survey, potentially limiting the generalizability of these findings.
Conclusion
This study demonstrates that the self-efficacy scales for communicating SRH with partners and health providers for adults with SB had high construct validity and excellent internal consistency, making them valuable tools for assessing SRH knowledge and self-efficacy in this population. The high internal consistency reliability and evidence of construct validity for the self-efficacy scales are particularly significant, as self-efficacy has been shown to be a strong predictor of health behavior. This reinforces the utility of the survey in both research and clinical settings, where it can help identify knowledge gaps, guide SRH interventions, and support patient-centered care. A future study should examine the test-retest reliability of this instrument to increase the utility of this survey in clinical practice and research.
Footnotes
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
