Abstract
Purpose
Most children hospitalized with traumatic brain injury (TBI) acquire new impairments that impact function and health-related quality of life. However, there is a lack of standardized, multidisciplinary, longitudinal rehabilitative services for children with TBI.
Methods
This single center, retrospective study evaluated rehabilitative services during acute hospitalization and identified the frequency of unmet needs, defined as new or untreated impairments at the first acquired brain injury (ABI) clinic visit.
Results
Analysis was conducted for 148 children hospitalized for TBI (mild/complicated mild [51%], moderate [14%], or severe [35%]) and evaluated at ABI clinic (median of 63 [43–122] days post-hospitalization). Eighty-two (55%) patients had at least one unmet need at initial clinic assessment. Executive function impairments were found in children with mild/complicated mild TBI (32%), despite only 5% of them receiving speech therapy (ST) prior to the clinic. Only 13% of children with severe TBI received outpatient ST at first clinic visit despite 26% and 20% identified as having executive function and communication impairments. Earlier consultation of physical therapy, occupational therapy, ST, and physiatry was associated with discharge home versus inpatient rehabilitation, all
Conclusion
This study demonstrates the importance of timely inpatient acute hospital rehabilitative care coordinated with longitudinal, multidisciplinary follow-up for children after TBI.
Introduction
Traumatic brain injury (TBI) is a leading cause of death and disability in children in the United States (U.S.) and is a critical global problem.1–5 Of the 475,000 children who sustain a TBI annually in the U.S., 50,000–60,000 are hospitalized.6–8 Although most children survive TBI, a majority of those hospitalized acquire new, short- or long-term functional impairments in at least one domain (e.g., cognitive, emotional, physical) that may impact health-related quality of life, activities of daily living, and school outcomes.1,2,9–11
Inpatient and outpatient rehabilitation services are vital in improving a child's functional outcomes after TBI.1,9,12 However, a multicenter randomized controlled study of children hospitalized with severe TBI (Glasgow Coma Scale [GCS] score < 9) showed that only 40% received inpatient physical therapy (PT) or occupational therapy (OT) and only 26% received speech therapy (ST). 13 Similarly, many children have new unmet and changing rehabilitation needs post-hospitalization. 9 Evidence-based guidelines exist for the treatment of mild (presenting GCS 13–15) and severe (presenting GCS <9) pediatric TBI, but each lacks guidance on inpatient and outpatient rehabilitation and longitudinal follow-up.14,15 In response to this critical need, some pediatric centers have initiated longitudinal outpatient programs and inpatient rehabilitation guidelines for comprehensive care of children with TBI..9,16–19 At this institution, the Division of Physical Medicine and Rehabilitation (PM&R) initiated a monthly multidisciplinary acquired brain injury (ABI) clinic in 2013; the Division of Pediatric Critical Care Medicine partnered with PM&R to develop and implement PT and OT guidelines in 2018. 20
The first objective of this study was to analyze the frequency of unmet needs identified in children seen in ABI clinic, after TBI hospitalization. An unmet need was defined as either a previously diagnosed or new functional impairment identified as necessitating new referral for treatment upon clinic visit. The second, more exploratory, objective was to examine the impact of early acute hospital rehabilitation intervention on hospital disposition post-TBI.
Methods
This was a retrospective, single center study performed at a 315-bed tertiary care and Level I trauma center with an average of 334 pediatric TBI admissions per year (83% mild [GCS 13–15], 7% moderate [GCS 9–12], and 10% severe [GCS < 9]) based on query of the data submitted to the National Trauma Databank (NTDB). 21 The NTDB is the data repository maintained by the American College of Surgeons (ACS). All Level 1, 2, and 3 trauma centers verified by the ACS are included. It is the largest source of data regarding injured patients and their hospital-level care.
Ethical considerations
This retrospective chart review study was approved as exempt by the Institutional Review Board (IRB STUDY20050220).
Patient population
An electronic chart review was performed of all patients ages one month to 18 years who were hospitalized with any severity of TBI between February 2013 and November 2018 and evaluated in ABI clinic post-hospital discharge. Children were excluded if their ABI was atraumatic or if they were hospitalized elsewhere prior to referral to ABI clinic due to lack of access to hospital records. According to data submitted to the NTDB, fewer than 10% of pediatric patients with TBI hospitalized at this center during the study period were evaluated in ABI clinic. See Supplement for details on hospital care for pediatric patients with TBI and the multidisciplinary services offered at ABI clinic.
In this study, the cohort was divided into children with either severe (GCS < 9), moderate (GCS 9–12), mild (GCS 13–15), or complicated mild TBI (defined as GCS 13–15 with traumatic intracranial abnormality visible on neuroimaging) with prolonged symptoms. 22 ABI clinic typically focused on those with complicated mild, moderate, or severe TBI rather than children with mild TBI. However, this retrospective analysis did reveal 10 children seen in clinic with mild TBI and normal neuroimaging, in addition to the 66 with complicated mild TBI, and these two designations were combined for purposes of analysis. All services participating in ABI clinic (PT, OT, ST, behavioral health, neuropsychology, PM&R) evaluated patients in person while social workers were available as needed via pager to attend to specific needs during the approximately two-hour visit. Supplemental Table S1 outlines the various tools and evaluations used to identify reported impairments by various clinicians, which were not protocolized but rather personalized dependent upon the patient's condition. The ABI nurse coordinator produced comprehensive recommendations and a written summary that included findings, recommendations, referrals, and educational materials for the family that was also documented in the medical record.
Outcomes
The primary outcome was the frequency of unmet needs at first ABI clinic visit. As mentioned previously, an unmet need was defined as either a previously diagnosed or new functional impairment identified as necessitating new referral for treatment upon clinic visit. ‘Unmet needs’ did not necessarily mean the provider failed to provide needed services at a previous point in time, such as at acute hospital discharge, but that the need was newly identified. The secondary outcome was the association between time to acute hospital-based rehabilitation therapy referral (days to receipt of PT, OT, ST, and PM&R consultation) and discharge disposition to home or inpatient rehabilitation. Of note, this data was collected from a time prior to the implementation of mobility guidelines at this institution, which mandate acute hospital rehabilitative therapy consultations for pediatric intensive care unit (PICU) admissions greater than 72 h. 20
Data collection
Data collected included patient demographics, injury characteristics including TBI severity, timing and type of acute hospital rehabilitative therapies (PT, OT, ST, PM&R), and hospital discharge disposition. Other descriptive variables that were collected included severity of illness scores, intracranial monitoring use, and details of the ABI clinic evaluations. For the purposes of acute hospital discharge disposition, a single patient who was discharged to a long-term care facility was excluded from analysis. TBI severity was classified using the first recorded GCS score in the absence of neuromuscular blockade. Pediatric Logistic Organ Dysfunction (PELOD-2) scores 23 were calculated for patients admitted to the PICU based on the worst score for each organ system throughout the entire admission to adjust for severity of illness.
Type and frequency of functional impairments identified during acute hospitalization and at the first clinic visit were recorded. These new impairments were extracted from notes in the patients’ charts, at both the acute hospitalization period and first clinic visit. In the hospital, impairments were diagnosed by consulting clinicians; however, not all rehabilitation professionals may have been consulted. No routine, validated measures were used to assess inpatient or outpatient function or determine the need for new referral; rather, clinical judgement determined the need for new referral. In the clinic, new impairments were defined as those not previously identified during either acute hospitalization or inpatient rehabilitation. Screening for these impairments was standardized by having the same physical, occupational, and speech therapists perform indicated standardized testing (Table S1). Baseline (pre-TBI), acute hospital discharge, and initial ABI clinic neurological status was assigned by study personnel via the Pediatric Cerebral Performance Category (PCPC) scale, which measures neurologic impairments ranging from 1 (age appropriate) to 6 (brain death) using information from the electronic medical record.24,25 Authors performing chart review were trained by senior faculty in the use of PCPC scores, which were generated based on data from the retrospective chart review for research purposes. Evaluations specific to PT, OT, and ST clinical practice (Table S1) were used to determine reported impairments, which were then identified on chart review.
Data analysis
Descriptive statistics were reported using median and interquartile range (IQR) for continuous data, and frequencies for categorical data were used to describe sample characteristics. Wilcoxon rank sum and Fisher exact tests were used to evaluate associations of covariates with primary and secondary outcome variables.
Multivariable logistic regressions were performed to explore the relationship between days to each acute hospital rehabilitative service consultation (PT, OT, ST, PM&R) to hospital disposition, adjusted for initial motor GCS scores as a marker for severity of illness. This marker was chosen because it was the most reliably assessed part of the patient's GCS score for all inpatients. Logistic regressions were performed for each service separately due to a potential for collinearity and because not all children in the cohort received all services. An additional analysis of PICU TBI patients was performed using electronic PELOD-2 scores
23
to adjust for severity of illness. Analysis was conducted on the type and frequency of impairments identified at the first ABI clinic visit and the type and frequency of new referrals recommended at ABI clinic. Missing data was not imputed.
Results
Patient and injury characteristics and hospital care
Analysis was performed for 148 children (median [IQR] age of eight [2–13] years and 68% male) who were hospitalized for TBI and evaluated at ABI clinic at least once (Table 1). The most common TBI mechanism was motor vehicle accident (n = 67, 45%) followed by abusive head trauma (n = 24, 16%). Seventy-six (51%) children had mild TBI, 20 (14%) had moderate TBI, and 52 (35%) had severe TBI.
Patient demographics and injury characteristics.
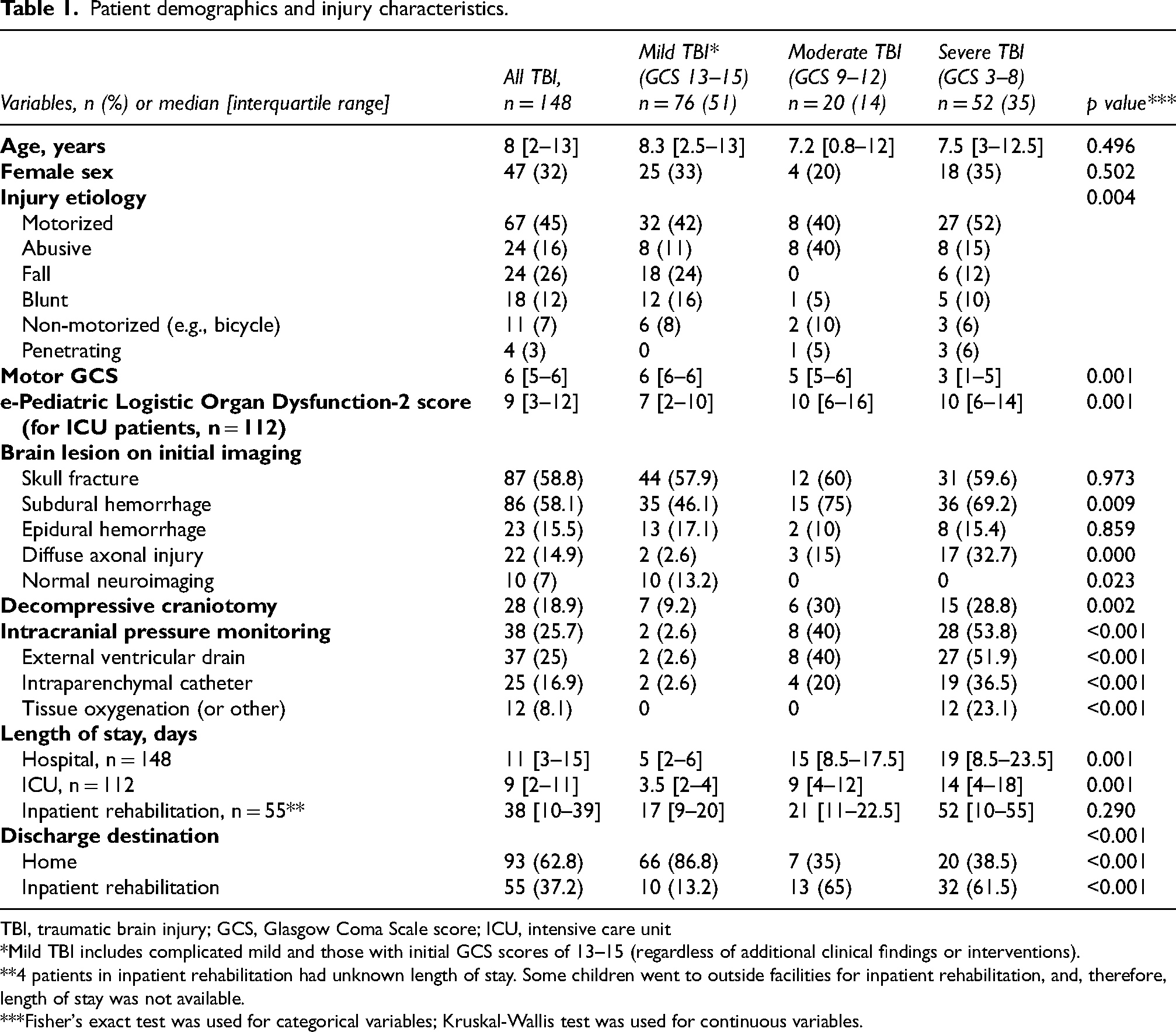
TBI, traumatic brain injury; GCS, Glasgow Coma Scale score; ICU, intensive care unit
*Mild TBI includes complicated mild and those with initial GCS scores of 13–15 (regardless of additional clinical findings or interventions).
**4 patients in inpatient rehabilitation had unknown length of stay. Some children went to outside facilities for inpatient rehabilitation, and, therefore, length of stay was not available.
***Fisher's exact test was used for categorical variables; Kruskal-Wallis test was used for continuous variables.
Neuroimaging was performed on all 148 children in the cohort. The most common imaging findings were subdural hemorrhages (58%) and skull fractures (59%) (Table 1); 10 children who followed-up in clinic classified as mild TBI and had normal neuroimaging, including MRI of the brain. Of 112 (76%) children initially admitted to the PICU, 34% underwent invasive intracranial pressure (ICP) monitoring during hospitalization, including two children initially classified as mild TBI.
A total of 93 (63%) children were discharged home and 55 (37%) were admitted to inpatient rehabilitation. Median hospital length of stay was 11 (3–15) days and inpatient rehabilitation length of stay was 38 (10–39) days. Children who were discharged to rehabilitation had a longer hospital length of stay than those discharged to home (20 [12–23] vs. 6 [3–7] days respectively,
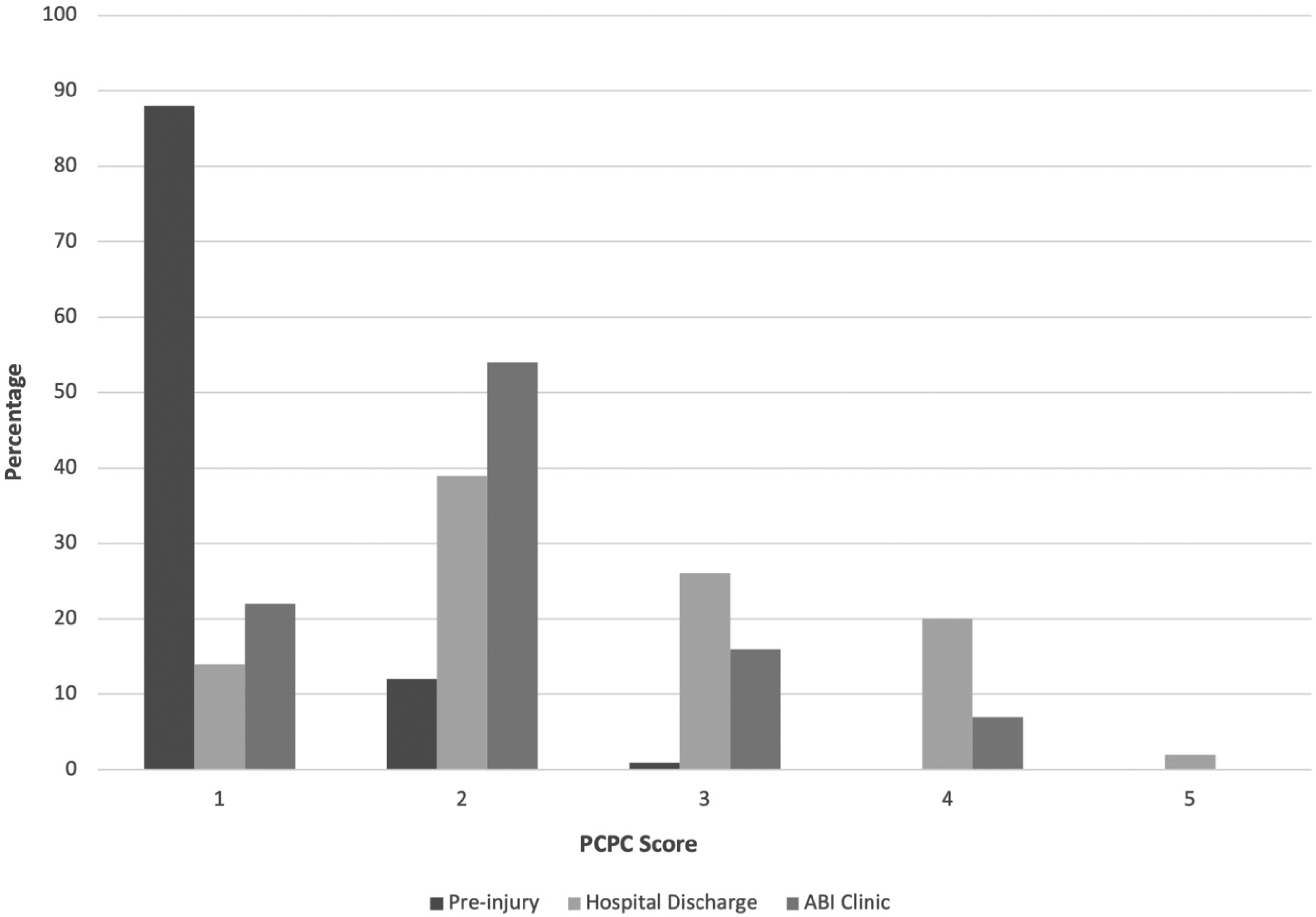
PCPC scores assessed pre-injury, at hospital discharge, and at initial ABI clinic visit in the overall study cohort. PCPC scores range from 1 to 6: 1 = no disability, 2 = mild disability, 3 = moderate disability, 4 = severe disability, 5 = coma, and 6 = brain death. PCPC, Pediatric Cerebral Performance Category; ABI, acquired brain injury.
Rehabilitation services that evaluated patients in the acute hospital and at the initial ABI clinic visit are shown in Table 2. During hospitalization, 74% of patients received PT, 67% OT, 78% ST, and 59% PM&R consultation, with days to consultation from hospital admission being three days for PT,2–6 four days for OT,2–7 three days for ST,2–8 and four days for PM&R2–9 (Table 2). The most common functional impairments at acute hospital discharge were in executive function (77%), mobility (64%), fine motor (54%), and communication (54%).
Rehabilitation service consultation and sequelae identified at a) acute
Table 2a. Rehabilitation service consultation and sequelae - identified during acute
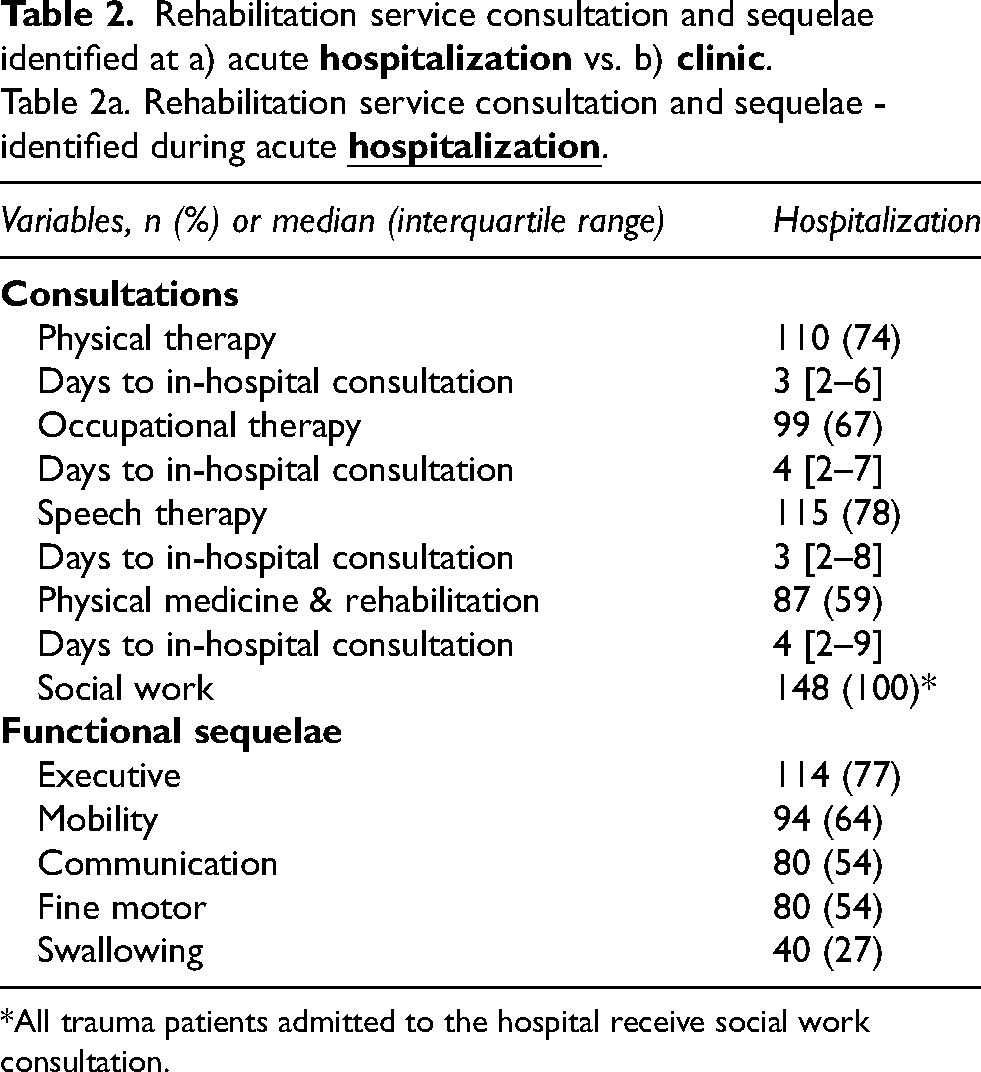
*All trauma patients admitted to the hospital receive social work consultation.
Rehabilitation service consultation and sequelae - identified at
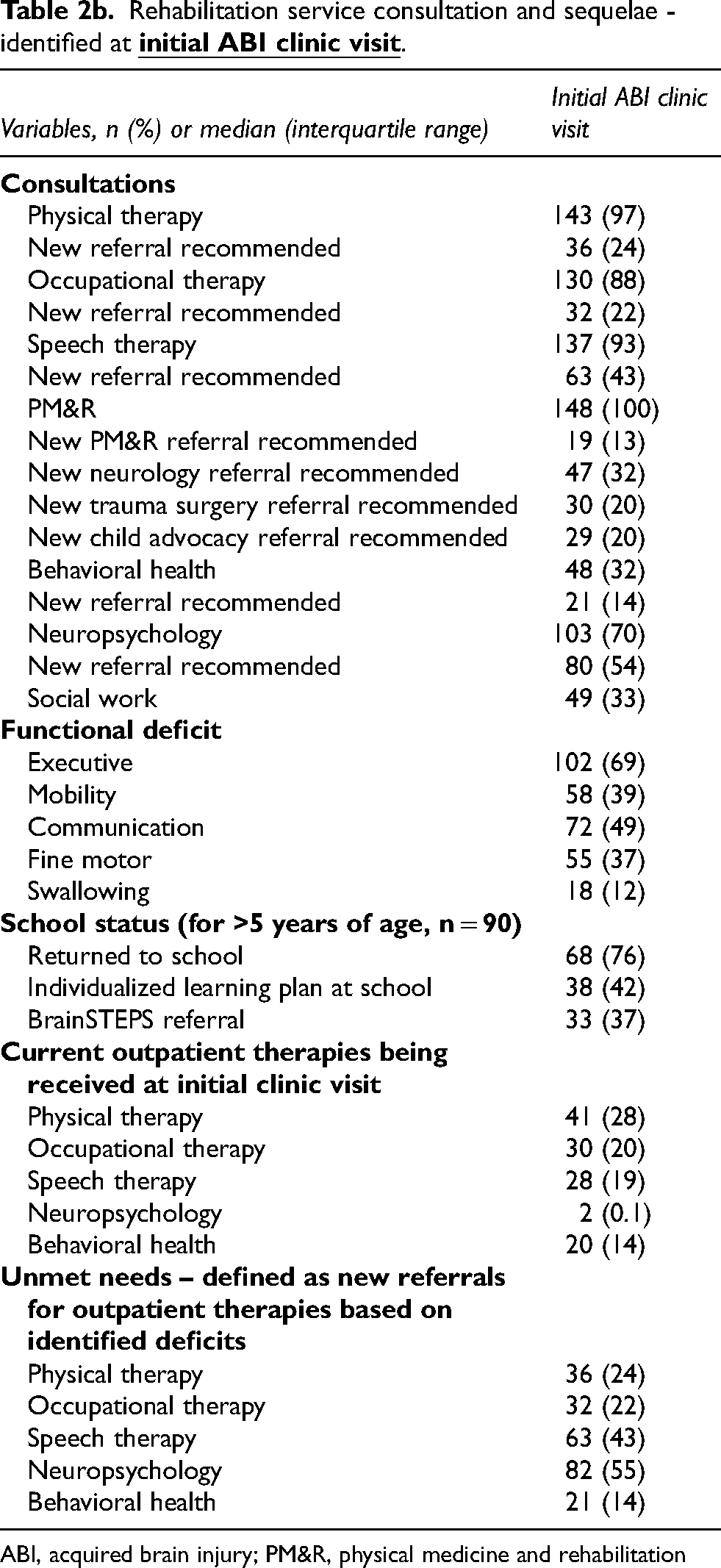
ABI, acquired brain injury; PM&R, physical medicine and rehabilitation
Primary outcome: ABI clinic consultation, impairments, and unmet needs
The first multidisciplinary ABI clinic visit occurred at a median 63 (IQR 43–122) days after acute hospitalization and 42 (27–68) days from inpatient rehabilitation discharge. It is acknowledged that this method of calculating time to clinic visit from acute hospital discharge may be extended for children who went to inpatient rehabilitation after acute hospitalization. However, the time from acute hospitalization period to first clinic visit is a consistent and accurate measure for the entire cohort. PT, OT, ST, and PM&R evaluated 97%, 88%, 93%, and 100% of patients during the clinic visit, respectively. Neuropsychology and behavioral health specialists evaluated 70% and 32% of patients at clinic visits (Table 2). Fifty-eight (39%) children who visited the ABI clinic returned for a subsequent ABI clinic visit. See supplemental material regarding when new referrals were made to PM&R clinic from ABI clinic, and the Clinical Care Standards at this institution.
The most common functional impairments at the first ABI clinic visit overall were executive function (69%) and communication (49%). Children with severe TBI had the highest frequency of mobility impairments (52%), whereas those with moderate TBI had the highest frequency of communication (60%), swallowing (30%), and executive function (80%) impairments. Figure 2 displays the frequency of new impairment compared to baseline at first clinic visit by TBI severity.
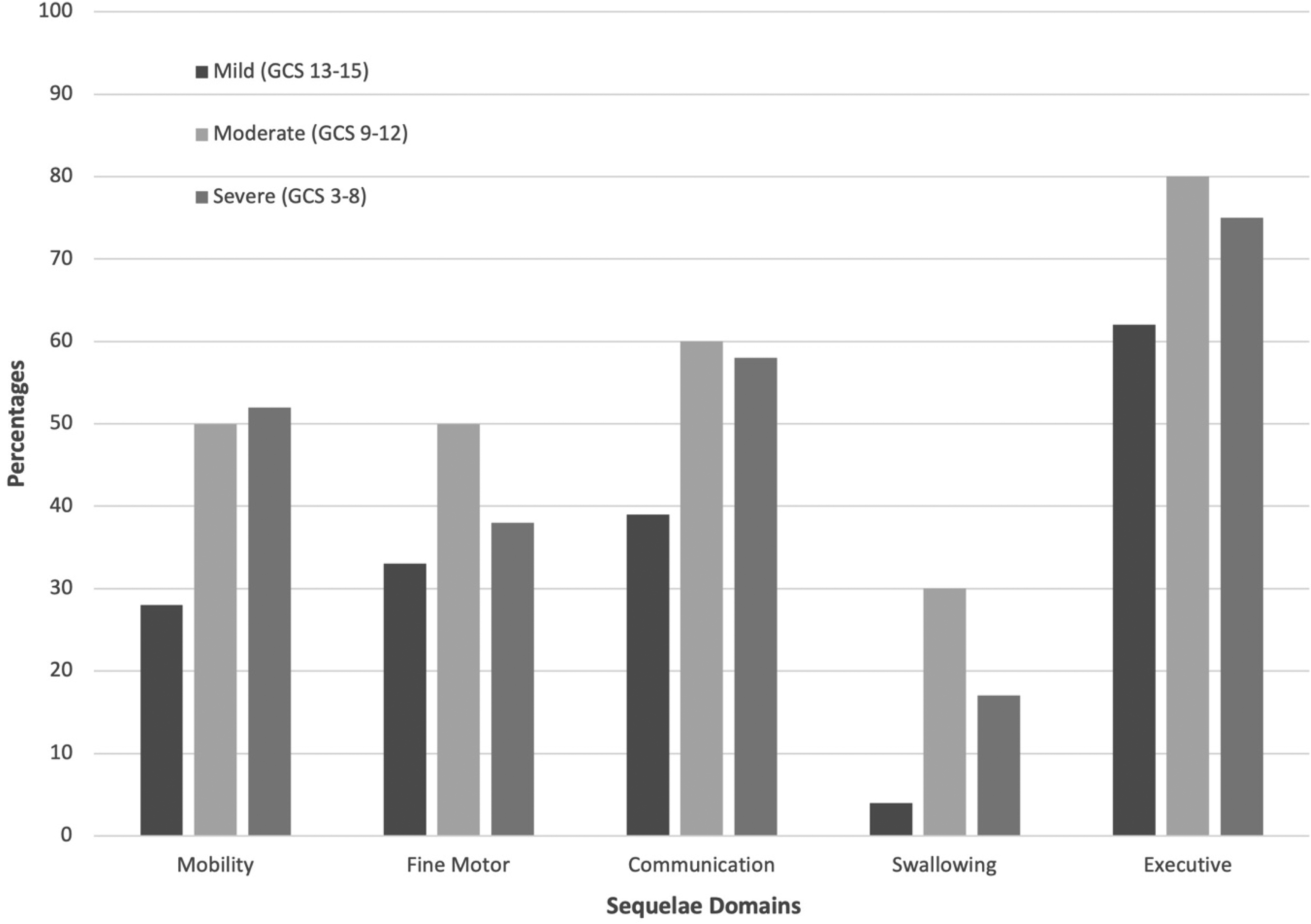
Frequency of functional sequelae by domain as identified at initial acquired brain injury clinic visit and reported by mild, moderate, and severe traumatic brain injury groups. GCS, Glasgow Coma Scale.
Unmet needs were identified in 82 patients (55%). The most common referrals were ST (43%) and neuropsychology (54%), paralleling the most common impairments (Table 2, Figure 3). Overall, sixty-eight (76% of school-age children) had returned to school by the first ABI clinic visit, 38 of whom had an individualized learning plan. Thirty-three (37% of school-age children) were referred to BrainSTEPS, a non-profit state program whose mission is to facilitate return to school participation for children with newly acquired brain injury.
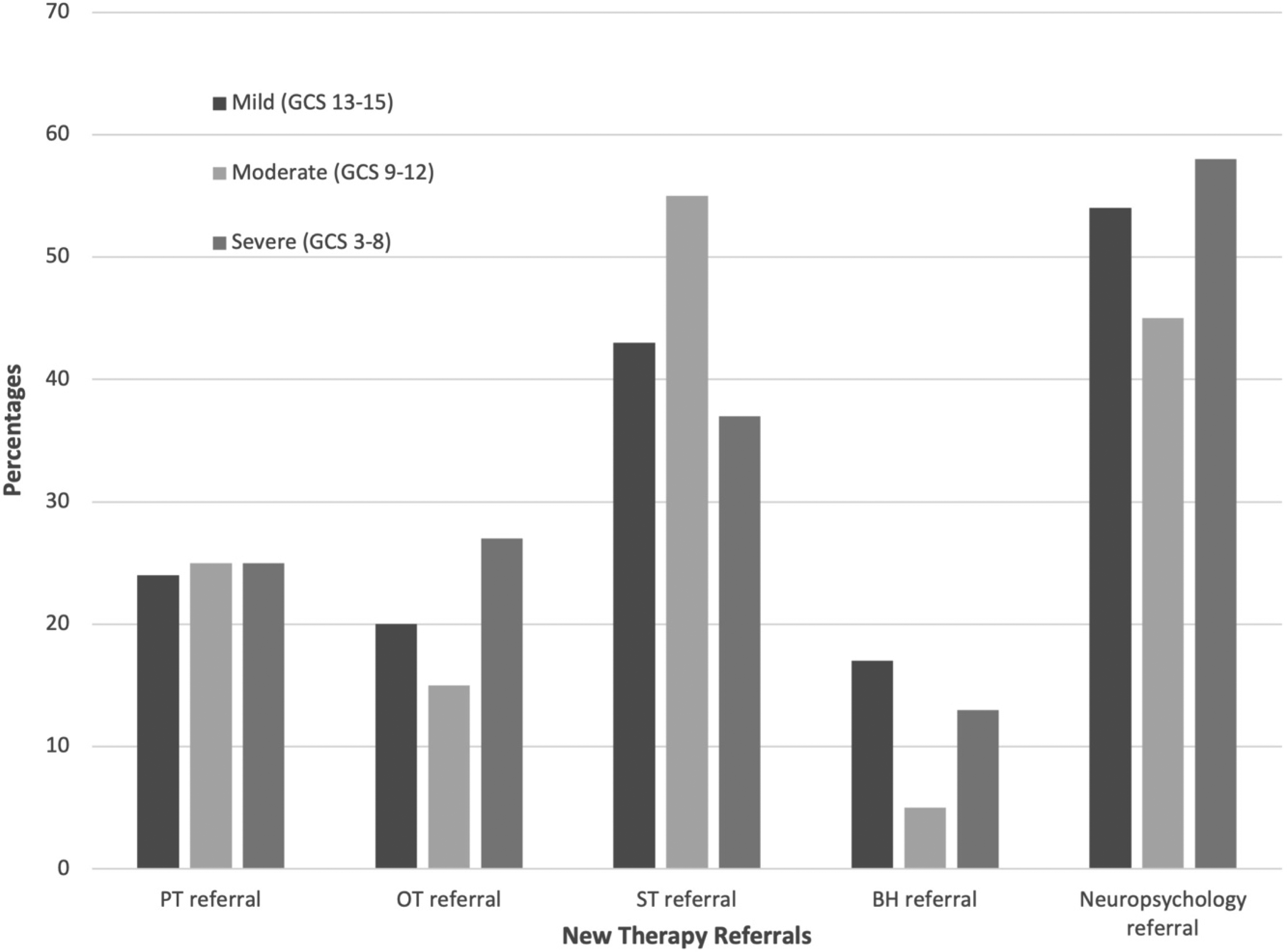
Unmet needs, defined as new referrals for functional sequelae identified at initial ABI clinic visit, by mild, moderate, and severe TBI groups. ABI, acquired brain injury; TBI, traumatic brain injury; GCS, Glasgow Coma Scale; PT, physical therapy; OT, occupational therapy; ST, speech therapy, BH, behavioral health.
Altogether, social work and behavioral health specialists identified many unmet psychosocial needs at the initial ABI clinic visit (Table 2). Social work professionals were paged for consultation in 33% of patient visits, and 32% of the patients saw behavioral health providers at their first clinic, with 21 (14%) new referrals made to behavioral health outpatient services. School issues, grief, mood and post-traumatic stress, sleep, and family issues were prominent concerns. In response, referrals were made for cognitive behavioral therapy, outpatient psychotherapy, visual assessments, early intervention, and confirmation of medical decision makers, along with documentation to communicate needs to the child's school or primary care provider.
Secondary outcome: days to rehabilitation consultations and discharge disposition
Fewer days to acute hospital consultation of PT (odds ratio [95% confidence interval], 0.68 [0.58–0.83],
Multivariable logistic regression for the association of days to each of four types of rehabilitation service consultations and hospital disposition to home. The entire cohort model was adjusted using initial motor GCS; the PICU only model was adjusted using PELOD-2 score and ICP monitoring status.
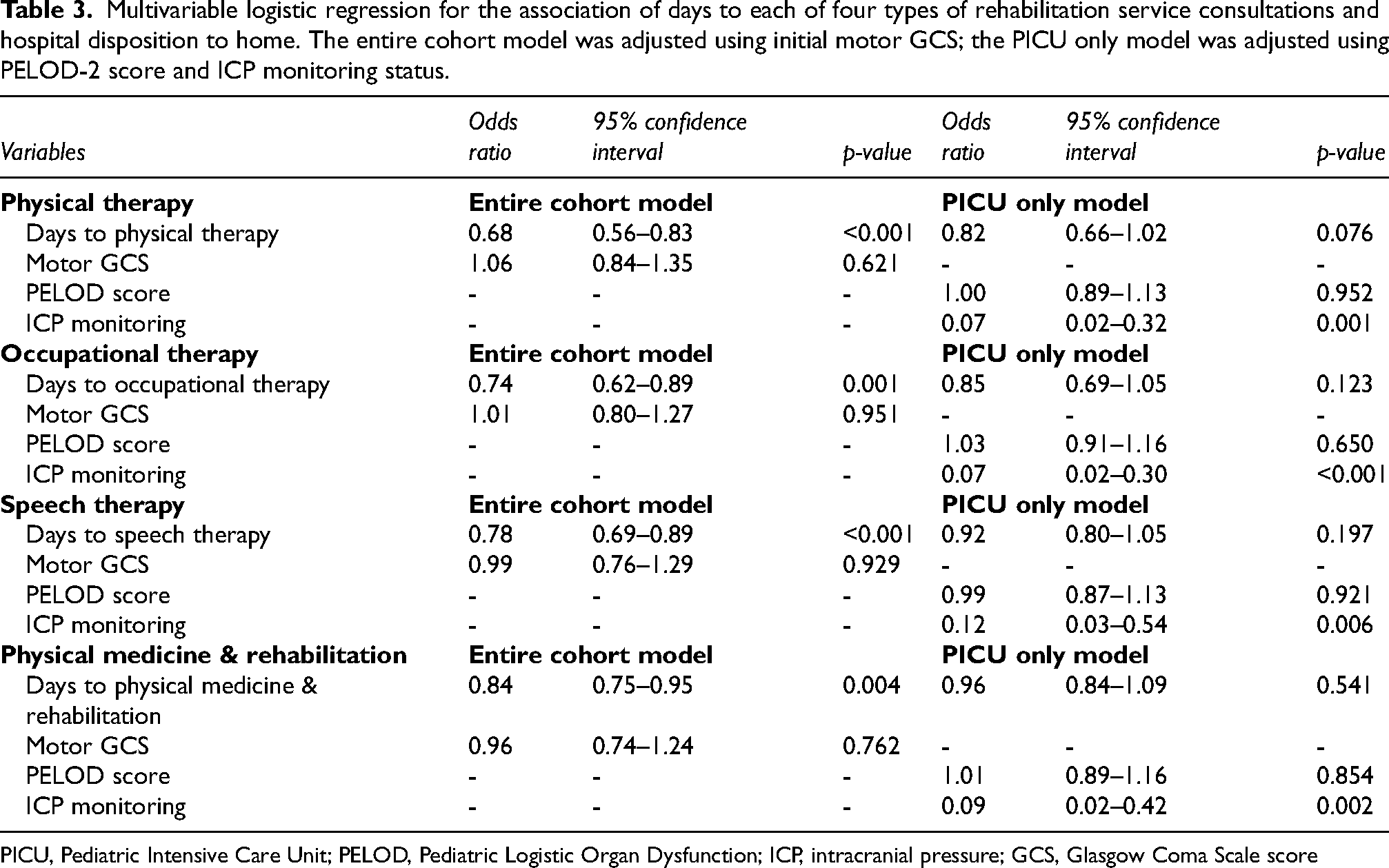
PICU, Pediatric Intensive Care Unit; PELOD, Pediatric Logistic Organ Dysfunction; ICP, intracranial pressure; GCS, Glasgow Coma Scale score
In an exploratory analysis to evaluate the association of time to rehabilitation consultation and disposition of PICU patients, multivariable logistic regressions were performed and adjusted for PELOD-2 scores and ICP monitoring status. In the adjusted models, ICP monitoring status was associated with disposition to inpatient rehabilitation. The odds ratio for ICP monitoring was low and, therefore, negatively associated with home disposition (Table 3). In other words, those with ICP monitors were not associated with home disposition, and instead went to inpatient rehabilitation. Days to consultation of rehabilitation services were not associated with disposition in the PICU only model (Table 3).
Discussion
Children with TBI are at risk for functional impairments that can be recognized in the acute hospitalization period, or they can arise later and subsequently be recognized at clinic follow-up. Early recognition, treatment, and continued follow-up may improve outcomes. In this cohort study of children hospitalized with TBI and evaluated in a post-discharge multidisciplinary clinic, the frequency of new functional sequalae and referrals recommended for unmet needs at follow-up was assessed, as was the association of acute hospital rehabilitation consultations and disposition. The major findings included 1) a majority of children had at least one functional impairment that persisted at acute hospital discharge or was identified at presentation to ABI clinic; 2) over half of children had at least one unmet need for new impairment identified at the first ABI clinic visit requiring new referrals; and 3) a majority of patients received acute hospital-based rehabilitation consultations, with earlier consultation of PT, OT, and ST each associated with discharge to home versus inpatient rehabilitation.
Hospitalized children surviving TBI are at high risk for multi-domain, longitudinal health sequalae after acute hospital discharge, and benefit from coordinated rehabilitative care and follow-up.1,16,26–33 Functional impairments were assessed during acute hospitalization through follow-up at ABI clinic. During the inpatient hospitalization epoch, impairments were highest in executive functioning, followed by mobility, communication, fine motor, and lastly swallowing (77%, 64%, 54%, 54%, and 27%, respectively). The prevalence of these impairments identified in inpatients is comparable to the number of impairments identified in neurocritical care patients in previous studies. 13 Longitudinal studies show that over 80% of children with TBI have significant new impairments at 12 and 24 months in cognitive, physical, and socio-emotional domains. 34
Successful return to the home and school environment post-TBI can be hindered by unmet needs such as executive function impairment and social needs that are undiagnosed or under-treated. Findings from this study show that the most common functional impairments assessed at acute hospital discharge and clinic visit were similar in rank order: executive function, mobility, and communication. Thus, this study highlights the importance of longitudinal outpatient follow-up to identify and treat unmet needs. The most common unmet need/new referral was for neuropsychology (55%), correlating to executive function being the most frequent impairment identified at both acute hospitalization and clinic follow-up. The second most common unmet need/new referral was to ST (43%), which provides care for children with executive processing and communication impairments. The third and fourth most prevalent unmet needs/new referrals were for PT (24%) and OT (22%).
Regarding return to school, it should be noted that BrainSTEPS, the non-profit state program whose mission is to facilitate return to school participation for children with newly acquired brain injury, is only for kindergarten through 12th grade students. Therefore, although earlier referral would be valuable, it is not possible at the ages before kindergarten. As stated previously, 33 children in this study were referred to BrainSTEPS. Due to the nature of how referrals are made wherein anyone can make a referral (including parents), this is likely an underestimation of the number of referrals. Furthermore, the inpatient rehabilitation unit and ABI clinic at this institution are separate entities. During inpatient rehabilitation, a child works with a school teacher who coordinates recommendations from the medical, therapy, behavioral health, and neuropsychology providers with the child's school. It is a team approach for guiding services. The same team approach can be said of school recommendations from ABI clinic, where the child's school needs are addressed over time.
Lastly, ABI clinic provided an opportunity for behavioral health unmet need assessments and new referrals. Slomine et al. found that multidisciplinary outpatient clinics can provide a central role for routine, longitudinal coordinated assessment and support for recovery. 35 Several centers have discovered profound impairments in sleep disturbance, neuropsychological functioning, and emotional health problems after pediatric neurocritical illness that, if untreated, may impair participation in life functions.36–38 Emotional health impairments are common post-TBI, including post-traumatic stress symptoms or disorder, impaired self-awareness, attention problems, disordered sleep, and psychosocial impairments.39–44 Studies have shown that sleep-wake disturbances are important morbidities after pediatric TBI39,40 and that transitions to school can be difficult, particularly if family issues arise. 45 These concerns all have implications for recovery and may represent modifiable targets for improving outcomes after pediatric TBI. Psychological health interventions after injury should be standardized and customized to address each child's comorbid impairment. Furthermore, social workers are instrumental in assisting families at ABI clinic, including enrolling patients in early intervention, assisting with transportation, providing information about transitioning into adult care, and helping to obtain medical assistance for secondary insurance.
Finally, there is large variability in the provision of rehabilitative services for hospitalized children with TBI. This may be due in part to the paucity of available prospective evidence supporting when and whom to consult, limited hospital resources to support assessment and treatment, and challenges with patient access to services.1,17,46–48 In this study, more than half of the patients admitted with TBI received acute hospital rehabilitative consultations, occurring a median of 3–4 days into hospitalization. These results compare favorably to other studies in that 32% received PT and/or OT consults by day three in a multicenter point prevalence study 49 and a retrospective cohort study from the Pediatric Health Information System database demonstrated 41% received either a PT or OT evaluation and 26% received a ST evaluation. 17 Prior evidence in children with general critical and neurocritical illness found that early rehabilitation was feasible and relatively safe even in the PICU period.13,35,50–53 Randomized trials involving mechanically ventilated adults with primary respiratory failure showed that early PT and OT was associated with shorter return to independent activities of daily living. However, efficacy trials to inform timing and dose of rehabilitation interventions to support evidence-based guidelines for seamless integration of inpatient-outpatient rehabilitation for children with TBI are still vitally needed.2,14
Taken together, these findings strongly suggest the need for collaborative research to inform the development and implementation of evidence-based clinical guidelines. A new standard of care,17,46,54–57 similar to guidelines for neurodevelopmental follow-up of premature neonates and infants with congenital heart disease,58,59 would longitudinally support families of children with TBI. Coordinated, longitudinal multidisciplinary assessments might be offered in person or virtually to improve access to care. These assessments, which have great potential to improve long-term outcomes, may include screening and support for health impairments, post-intensive care/hospital syndrome, and adverse social determinants of health.37,60,61 Further, families in the PICU must be engaged early and equitably. The concept of coordination of personalized care should be embraced, including providing education from the hospital through to primary care, schools, home, and community to better coordinate care that improves long-term outcomes for these children.
Limitations
First, the sample size was limited to patients who attended at least one ABI clinic (less than 10% of pediatric patients hospitalized with TBI during the study period). Approximately 1500 children admitted with TBI at this institution were recorded in the NTDB during the study's time period, most of whom had mild TBI. ABI clinic at this institution is designed to serve children with complicated mild, moderate, and severe TBI. Children with uncomplicated mild TBI (and some with complicated mild TBI) are referred to a separate concussion clinic; their information was not analyzed in this study. Additionally, some families were referred to ABI clinic but did not attend. It can be conjectured that this may be due to geographic limitations (wide catchment area serving four states), lack of insurance coverage, or other socioeconomic limitations; however, this data is unavailable. It is acknowledged that outcomes, variables, and analysis are impacted by the unique features of this study population. Secondly, the relationship of disposition to prompt therapy is potentially confounded by the children's ability to participate in services such as ST. However, other therapies such as PT and OT have many passive interventions included in early mobility that do not require child participation. Third, GCS is a broad assessment of severity. Future studies could use the Acute Injury Score (AIS) for the head based on anatomic findings of neuroimaging for which AIS > 2 is severe. Last, generalizability to other centers may be limited by lack of multidisciplinary rehabilitation follow-up service availability. Despite acknowledging the bias in this group, it is also important to recognize this cohort's great need for rehabilitation.
Conclusions
The major clinical implication of these findings is that children admitted after TBI appear to benefit from longitudinal, coordinated, multidisciplinary follow-up. With ABI clinic, families are assisted in transitioning back to home and school after TBI, including ongoing therapy, behavioral recommendations, durable medical equipment, and school or work accommodations. Prospective studies are needed to assess patients who would benefit the most from such a limited resource and how best to refer inpatients to ABI clinics and ensure access to them.
Supplemental Material
sj-docx-1-prm-10.1177_18758894241312482 - Supplemental material for Multidisciplinary rehabilitation and follow-up for children hospitalized with traumatic brain injury
Supplemental material, sj-docx-1-prm-10.1177_18758894241312482 for Multidisciplinary rehabilitation and follow-up for children hospitalized with traumatic brain injury by Lauren J Alessi, Matthew MacCarthy, Andrew McCormick, Jason Edinger, Amy J Houtrow, Dennis W Simon, Barbara A Gaines, Christopher M Horvat and Ericka L Fink in Journal of Pediatric Rehabilitation Medicine
Footnotes
Acknowledgements
We would like to thank staff in the PICU and Pediatric Rehabilitation Institute at the UPMC Children's Hospital of Pittsburgh, ABI clinic providers, and all patients and their families. We would also like to thank the following people who have been instrumental in data analysis and the development of the clinic: Heather Edwards, MS, CCC-SLP†; Lynn Golightly, MS, CCC-SLP†; Colleen Lyons, MS, CCC-SLP†; Maddie Chrisman, PT, DPT‡; Kimberly Kubistek, OTD, OTR/L§; Jessica Jarvis, PhD, MT-BC#; Katie A. Hayden, MSN, RN#; and Sarah Rubin, MD, MsCL*.
† – UPMC Children's Hospital of Pittsburgh, Department of Speech & Language Pathology, Pittsburgh, PA.
‡ – UPMC Children's Hospital of Pittsburgh, Department of Physical Therapy, Pittsburgh, PA.
§ – UPMC Children's Hospital of Pittsburgh, Department of Occupational Therapy, Pittsburgh, PA.
# – UPMC Children's Hospital of Pittsburgh, Department of Critical Care Medicine, Pittsburgh, PA.
* – Department of Pediatrics, UPMC Children's Hospital of Pittsburgh, Pittsburgh, PA.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by 1K23HD099331-01A1 (CMH), NINDS R01 NS096714 (E.L.F.).
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
