Abstract
Compliance with medical interventions is crucial for the effectiveness of treatment strategies in public health. Approaches to encourage compliance with health interventions vary in both form and methodology. During ordinary times, public health campaigns mainly rely on educational efforts or incentives while in more severe circumstances, governments might take enforcement measures and even penalties for noncompliance. When interventions pose potential risks to personal interests (e.g., health risks of side effects; social risks of exclusion), individuals find it challenging to comply with such medical measures, resulting in negative consequences for both personal healthcare and public welfare. In this paper, we introduce an effective way to promote compliance with such interventions in the area of public health: enhancing sense of control. We explore three specific compliance behaviors: disclosure of personal information, vaccination, and acceptance of water resource reallocation. These behaviors, while beneficial to public health, pose personal risks like privacy breaches and health-related side effects. Through four studies, we demonstrate that the positive effect of sense of control on compliance behaviors with public health interventions is mediated by reducing perceived personal risk of the intervention. Individuals with a higher sense of control perceive lower personal risk of the medical interventions, leading to increased compliance. Additionally, our research identifies a boundary condition that if the interventions pose no harm to personal interests, the effect of sense of control will be attenuated. By concentrating on interventions that could potentially harm personal interests, our study provides deeper insights into the circumstances and reasons behind individuals’ reluctance to comply with public health interventions. The current research sheds light on the psychological processes driving compliance decisions and offers valuable strategies for health professionals and governments to enhance medical adherence.
Keywords
Introduction
Compliance with medical measures, often referred to as ‘compliance’ or ‘adherence’ in medical literature, is a critical determinant of health outcomes. The term ‘comply’ suggests acting in accordance with a wish or command (Oxford Languages, 2023). In the area of public health, this could range from simple routine behaviors such as handwashing to prevent the spread of infectious diseases (Luby et al., 2005) to more complex and long-term commitments such as adhering to medication regimens for chronic conditions (DiMatteo, 2004). Failure to comply with prescribed medical regimens can compromise treatment effectiveness and lead to disease progression or even death. World Health Organization (2003) revealed that approximately 50% of patients do not take their medications as prescribed, especially for chronic illnesses. In developed nations, such noncompliance has been identified as one of the primary reasons for hospital admissions among the elderly (World Health Organization, 2003). The financial implications of noncompliance behavior are staggering, with associated medical costs estimated at around $100 billion annually (Sokol et al., 2005). Therefore, it is a vital issue of promoting compliance behavior in public health, for both personal healthcare and public welfare.
Practices to foster compliance behavior in public health are diverse and flexible. During ordinary times, public health campaigns might rely on educational efforts, nudging strategies, or incentives, such as discounted gym memberships to encourage physical activities (Bethancourt et al., 2014) or taxation measures on unhealthy products (Wright et al., 2017). However, in more pressing circumstances, such as the COVID-19 pandemic, governments might take enforcement measures, including self-surveillance, compulsory lockdowns, obligatory mask mandates in public places, and even penalties for noncompliance. Such measures may raise individuals’ concerns about their personal interests, leading to perceived risks of the interventions and resistance to compliance. The current research focuses on compliance behaviors at the risk of affecting personal interests, and demonstrates the effect of sense of control in reducing perceived risk of interventions and promoting compliance behaviors.
Our research makes three significant contributions to the literature. First, it presents enhancing sense of control as an effective approach to foster compliance across various health interventions and diseases. Second, our study shifts the focus from promoting positive outcomes to reducing perception of negative consequences, offering a new perspective on compliance. Lastly, we highlight the importance of classifying health interventions based on potential personal risks, enhancing understanding of why individuals might be reluctant to comply. This insight is particularly valuable for medical professionals, suggesting that strategies should be tailored to different types of interventions, considering their risk levels, and aiming to improve patients’ sense of control.
Literature and hypotheses
Compliance behavior in public health
“Compliance behavior” refers to individuals’ adherence to rules, guidelines, or standards (Bobek et al., 2013; Cialdini & Goldstein, 2004; Cialdini & Trost, 1998). Compliance is a response to a request asking for a specific action (Cialdini & Goldstein, 2004), which means individuals have the option to refuse but choose to change their behavior to comply (Bobek et al., 2013). In the area of public health, compliance behavior plays a vital role as it directly correlates with the effectiveness of health interventions and outcomes for entire populations.
For instance, adherence to recommended vaccination schedules ensures the prevention of diseases and the achievement of herd immunity (Jung & Albarracín, 2021; Omer et al., 2009; Tanimoto, 2021). Similarly, guidelines on handwashing, mask-wearing, and social distancing are crucial for managing and mitigating the spread of diseases like the flu or COVID-19 (Khan et al. 2022; Tori & Tanimoto, 2022). In chronic diseases such as tuberculosis or HIV, following prescribed treatment protocols is critical to manage the condition and prevent transmission (Munro et al., 2007). Additionally, periodontal therapy requires the patients’ long-term compliance to a periodontal maintenance program in dental prophylaxis (Umaki et al., 2012).
Given the crucial role of compliance behavior in health interventions, plenty research has examined the factors that influence compliance behaviors (Block & Keller, 1995; Champion & Menon, 1997; Janz & Becker, 1984). The Health Belief Model (HBM) suggests six factors that influence individuals’ decisions to comply with health recommendations, including perceived susceptibility (likelihood of getting a disease), perceived severity (seriousness of contracting an illness and possible consequences), perceived benefits (belief in efficacy of the advised action), perceived barriers (potential negative aspects of health interventions), cues to action (strategies to activate compliance), and self-efficacy (Becker, 1974; Hochbaum, 1958; Rosenstock, 1960, 1974). The model has been proved effective in many health interventions such as adherence to screening mammography recommendations (Champion & Menon, 1997), AIDS-protective guidelines (Janz & Becker, 1984), and acceptance of dengue vaccines (Kabir et al., 2021). Apart from HBM, Feng et al. (2023) demonstrated that cultural antecedents and social norms also shaped individuals’ compliance behavior that people in more individualistic areas were more reluctant to comply with lockdown orders during the pandemic. Individuals’ knowledge (Adler & Newman, 2002), accessibility of healthcare services (Mechanic & Meyer, 2000), political beliefs (Painter & Qiu, 2020), and trust in government (Shanka & Menebo, 2022) are also proven to positively influence compliance behaviors.
Although compliance often benefits the public, it may pose risks to personal interests. For instance, newly introduced vaccines might have side effects, potentially harming health. Similarly, preventive measures requiring the report of personal information to control the spread of a pandemic might threaten individual privacy. When people perceive that compliance behavior may pose risks to their personal interests or cause harm, they tend to resist compliance. For example, teenagers referred to concerns about social image and not fitting in with friends when they talked about the barriers of quitting smoking (Amos et al., 2006). People reported higher vaccine hesitancy due to concerns about vaccine side effects, though this hesitancy decreased as vaccine uptake became more prevalent (Lu, 2023). To mitigate the trade-off between public welfare and personal interests, existing research has explored ways to encourage compliance by highlighting public benefits. For example, eliciting prosocial concerns (i.e., priming non-vaccinated participants to think about how much they would worry about infecting others) has been found to increase the vaccination intent in densely populated areas in the US (Jung & Albarracín, 2021). Researchers have also developed epidemic models aimed at predicting individuals’ decision-making on this trade-off, integrating both individual-based risk assessment and society-based risk assessment strategies (Kabir et al., 2023; Khan & Tanimoto, 2023, 2024). However, little research has focused on reducing individuals’ concerns about personal interests, even though addressing these concerns can also serve as an effective intervention by reducing the perceived risk of negative outcomes (Weinstein, 1993). In this research, we highlight an important factor – sense of control – as an effective way to promote compliance behavior by alleviating perceived risk associated with health interventions, as will be elaborated in the next section.
Sense of control and compliance behavior
Sense of control, as a psychological concept, refers to an individual's perception of having control over their actions and consequently, the events in the external world (Moore, 2016). As an agent exerts effort to obtain the desired outcome (Shultz et al., 1986), the contingency between one's behavior and the outcome generates the feeling of control (Moore et al. 2009). Sense of control can be independent of actual control, and thus is subjective and can be influenced by situational factors such as an incidental choice that is irrelevant to the focal task, familiarity of the stimulus, or active involvement (Langer, 1975). Interestingly, research has shown that sense of control can be more powerful in predicting subsequent behaviors compared to actual control and can even be dissociated from it (Averill, 1973; Burger, 1989). For example, Brandimarte et al. (2013) demonstrated that increasing perceived control over information release and access reduced privacy concerns, even when actual control over the information remained constant.
Although previous research has documented that individuals with a lower sense of control exhibited heightened compliance behavior due to increased reliance on expertise (Aaronson et al., 1988) or a tendency to avoid taking responsibility (Botti et al., 2009), these compliance behaviors typically serve personal interests rather than potentially causing harm. For example, Aaronson et al. (1988) found that pregnant women with low sense of control attached more importance on the information from their healthcare provider and books rather than from the media and friends. However, the link between sense of control and compliance behaviors at the risk of personal interests is still under question. In the current research, we argue that when compliance to health interventions may potentially cause harm to personal interests, sense of control would conversely have positive effects on compliance behaviors as reasoned below.
Firstly, sense of control motivates individuals to take into action (Bandura, 2000). Individuals with a higher sense of control believe that they can achieve better outcomes than others, leading them to respond more actively to health interventions (Harris, 1996; Zhang et al., 2021), while those with low control are significantly associated with less self-initiated preventive care (Seeman & Seeman, 1983). Umaki et al. (2012) investigated the relationship between personality traits and patient compliance. They demonstrated that sense of control can regulate the patients’ emotions and was positively associated with problem-focused coping, leading to more compliance to long-term periodontal maintenance.
Secondly, sense of control proves to be highly correlated with risk perception (Horswill & McKenna, 1999; Martinez et al., 2011; Nordgren et al., 2007). Individuals with a higher sense of control believe that they can obtain superior outcomes than others (Harris, 1996), leading to reduced risk perception and an increase in risk-taking behaviors. For instance, Martinez et al. (2011) found that an increased sense of control encouraged risk-seeking behavior in gambling. Similarly, Horswill and McKenna (1999) manipulated participants’ sense of control in a video simulation by assigning them roles either as a driver (high control) or a passenger (low control). They found that those acting as drivers engaged in more risk-taking behaviors such as over-speeding, close-following, and overtaking. Therefore, we propose that, for the public health interventions that may potentially harm personal interests, individuals with a higher sense of control perceived lower risk of the interventions, leading to higher compliance with these interventions. To put it formally:
As previously proposed, a heightened sense of control could diminish an individual's perceived risk associated with health interventions, thereby enhancing compliance behaviors. Consider interventions that are inherently harmless to personal interests, such as handwashing and maintaining a healthy diet, which present no significant risk. Accordingly, we suggest a boundary effect: if the health interventions pose no threat to an individual's personal interests, the influence of sense of control on compliance behavior is likely to be diminished (see conceptual framework in Figure 1).
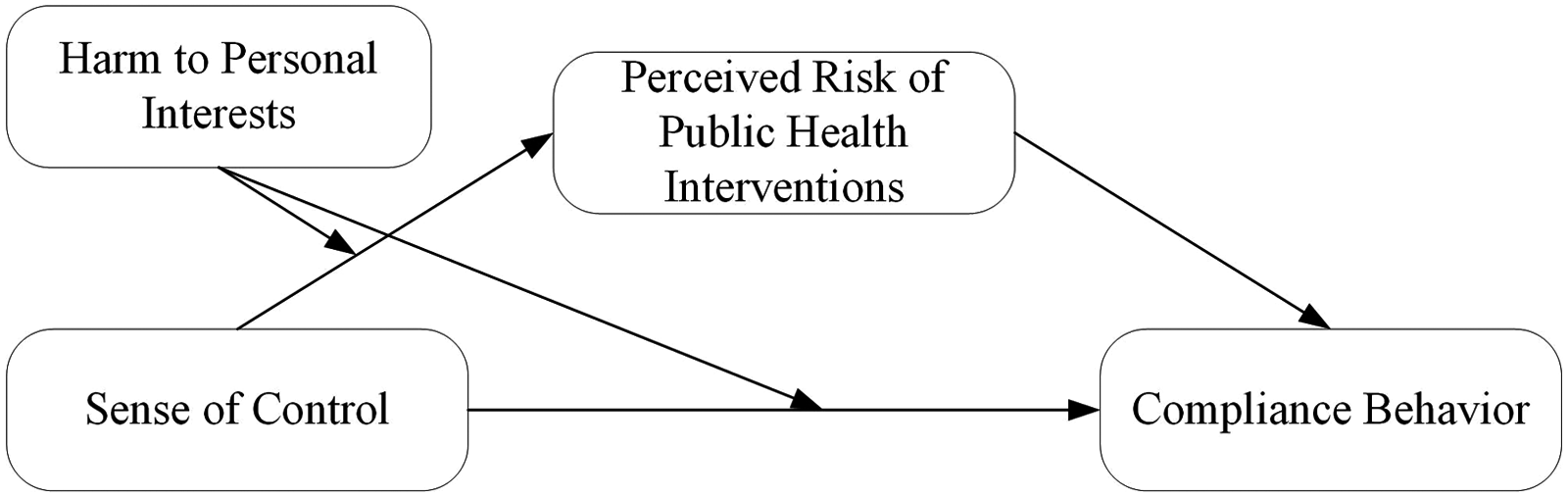
Conceptual framework.
Study 1
Study 1 aimed to provide initial evidence of the positive association between sense of control and compliance behaviors when the latter potentially posed risks on personal information privacy. To achieve this, we collected data in the context of COVID-19 in China when self-surveillance was implemented to control the spread of the pandemic. Given that self-surveillance required the complete disclosure of personal health condition, places they visited, and individuals they interacted with on a daily basis, it raised individuals’ concerns about privacy which might hinder their intent to comply. In such a context, we conducted a survey immediately after the peak of COVID-19 in China, on March 15, 2020. We collected data on sense of control and willingness to disclose personal information for self-surveillance purposes across China. Our data spanned 29 different provinces and municipalities. Moreover, because our data covered multiple provinces and areas in China, with varying severities of COVID-19, we were able to take advantage of the natural variation in disease severity and further test the robustness of our hypotheses across different levels of severity.
Method
Two hundred ninety-nine respondents from Credamo (a Chinese crowdsourcing data-collection platform similar to Amazon Mechanical Turk; 51.5% female,
We obtained the number of accumulated confirmed cases of 29 different provinces and municipalities from January 19, 2020 to the date of our data collection (i.e., March 15, 2020). The data was collected and displayed on DX Doctor COVID-19 Global Pandemic Real-Time Report (http://ncov.dxy.cn/ncovh5/view/en_pneumonia; retrieved March 16, 2020), a website authorized by the Chinese government which aggregated COVID-19 confirmed cases globally and updated each day. We matched the accumulated confirmed cases of each province with our survey data as the measurement of severity of COVID-19.
Results
Consistent with our hypothesis, a regression analysis showed that participants with a higher sense of control were more willing to disclose health-related personal information for self-surveillance purposes (
We removed three respondents whose locations could not be identified, leaving 296 respondents from 29 different provinces and municipalities. We used the number of accumulated confirmed cases by province to represent the severity of COVID-19. After controlling severity of COVID-19, results of regression analysis still revealed a significant positive effect of sense of control on compliance with disclosing personal information (
Discussion
Study 1 provided preliminary evidence that individuals’ sense of control was positively associated with compliance behavior with public health interventions when there was a potential harm to personal interests (H1). We conducted the investigation in the context of COVID-19 and selected the typical medical intervention – disclosing personal information for self-surveillance – as the corresponding compliance behavior, as it threatened personal privacy. Participants with a higher sense of control reported higher willingness to disclose their personal information. This result remained consistent after accounting for variations in the severity of COVID-19, thereby demonstrating the robustness of the effect.
Study 2
Study 2 aimed to find longitudinal evidence that participants’ compliance tendency varied as their sense of control changed over time. We examined the same compliance behavior as in Study 1 (disclosure of personal information) and assessed individuals’ willingness to comply at two distinct stages of the pandemic respectively. We collected data on April 14, 2020 (time 1) immediately after the peak of COVID-19 in China and tracked the same participants till August 28, 2020 (time 2) when the lockdown had been released in most areas in China.
Method
Nine hundred eighteen participants (46.7% female,
At time 2 when the lockdowns had been released in most areas in China, we sent our survey to the same 918 respondents and got 736 completed questionnaires back (48.9% female,
Results
Sense of control and self-disclosure
We ran regressions at time 1 and time 2, separately. Results revealed that participants with a higher sense of control were more willing to disclose their personal information at both time 1 (
Longitudinal evidence
A one-way repeated measures ANOVA was conducted to compare sense of control and self-disclosure at the two time points (time 1 and time 2). Results showed that participants’ sense of control at time 2 was significantly higher (
Discussion
Study 2 replicated the findings in Study 1 and provided longitudinal evidence that participants’ willingness to comply with health interventions increased due to the rise in their sense of control, offering initial causal evidence that the increase of sense of control can improve willingness to comply with health interventions. Building on this, Study 3 expands Study 2 in several important ways. First, in Study 3, we established a causal relationship by directly manipulating sense of control. Second, we also measured perceived risk of health interventions, and tested perceived risk as the downstream of sense of control. Third, to broaden the applicability of our findings, in Study 3, we tested compliance behavior in a European context, specifically in the UK, where the primary preventive measure during the pandemic has been vaccination. Accordingly, we measured vaccination intention as another indicator of compliance behavior.
Study 3
In Study 3, we examined another form of compliance behavior, getting vaccinated. This behavior carries potential health risks and leads to vaccine hesitancy, particularly when the vaccine has not been widely tested (Lu, 2023). During the pandemic, COVID-19 vaccines were rapidly developed and introduced to the public shortly after the outbreak commenced. Concerns about potential side effects of COVID-19 vaccines decreased the acceptance of these vaccines (Dror et al., 2020). Therefore, this study measured consumers’ willingness to comply with the government's requirement for vaccination. To establish the causality between sense of control and compliance behavior, we directly manipulated sense of control, employing a single factor (high vs. low sense of control) between-subjects design. We expected that a higher sense of control would increase vaccination intent by reducing perceived health risks associated with the side effects of COVID-19 vaccines. Thus, we also tested perceived health risks of the vaccines as a mediator.
Another factor that might influences vaccination is self-efficacy: people might think their compliance with health interventions is not effective in preventing the pandemic from spreading and thus are unwilling to get vaccinated (Limbu et al., 2022). We therefore also measured self-efficacy to rule out this alternative explanation.
Method
One hundred eighty-eight UK residences who
Given that having a choice can be an effective way of increasing perceived control (Averill, 1973), we manipulated sense of control by varying across conditions whether participants were given a choice of different COVID-19 vaccines. Specifically, all participants first read a paragraph introducing COVID-19 vaccines. Next, participants in the high-control condition were told that there were three vaccines available, developed by different companies (i.e., Pfizer-BioNTech, Moderna, and Johnson & Johnson), and were asked to choose one if they decided to get vaccinated. Those in the low-control condition were told that only one vaccine (Johnson & Johnson) was now available so it was the only option if they decided to get vaccinated. As a manipulation check of sense of control, participants indicated how much they agreed with the statements “I can control my life” and “My life is in my control” (1 =
Participants then answered questions about willingness to get vaccinated (“how hesitant are you to get vaccinated,” “to what extent are you willing to get vaccinated,” with the first question reverse coded; 1 =
Results
Manipulation check
A one-way ANOVA verified the manipulation of sense of control. Participants in the high-control condition perceived higher sense of control (
Willingness to get vaccinated
A one-way ANOVA on willingness to get vaccinated revealed a significant main effect of sense of control (
Perceived health risks of the vaccine
A similar one-way ANOVA was conducted on perceived health risks of the vaccine. Results showed that participants in the high-control condition perceived significantly lower risk of having side effects (
Mediation analysis
Mediation analysis (PROCESS Model 4 with 5,000 bootstrapping samples; Hayes, 2017) showed that perceived risk mediated the effect of sense of control on willingness to get vaccinated (indirect effect:
Self-efficacy
A one-way ANOVA was also conducted on self-efficacy and the results was marginal significant. Participants in the high-control condition reported higher self-efficacy (
Discussion
Study 3 further demonstrated the positive effect of enhancing sense of control on participants’ compliance behavior regarding vaccination by directly manipulating sense of control. Compared to participants in the low sense of control condition, those in the high sense of control condition perceived a lower risk of having side effects from the vaccines, resulting in significantly higher intentions to get vaccinated. Overall, results of Study 3 reaffirmed the positive effect of sense of control on people's compliance behaviors by reducing perceived risk of health interventions (H1).
Study 4
In previous three studies, we demonstrated that individuals with a higher sense of control were more willing to comply with preventive interventions in public health, including disclosing personal information and getting vaccinated. The positive effect of sense of control on compliance behavior was mediated by the perceived risk of preventive interventions, meaning that high sense of control reduced individuals’ perceived risk of the interventions, thus promoting compliance behavior. In Study 4, we aimed to examine a boundary effect that if the health interventions have no harm to individuals’ personal interests, the effect of sense of control on compliance behavior will be attenuated (H2). We created a fictional waterborne virus called “Eosyn” and manipulated the risk of preventive health interventions. Study 4 was preregistered at https://aspredicted.org/6GW_G5M.
Method
Four hundred respondents were recruited from Prolific (a crowdsourcing data-collection platform) for a small monetary payment. Each participant received £0.40. We randomly assigned participants to one of four conditions in a 2 (sense of control: high vs. low) * 2 (risk of intervention: high vs. low) between-subjects design. We manipulated sense of control through a writing task (Cutright, 2012). In the low control condition, participants recalled a threatening experience in which they were not in control of the outcome. We asked them to write the details about (1) the threat /uncertainty in the experience, (2) what they had done but failed to gain control, and (3) what aspects of that experience eventually got out of control. In the high sense of control condition, participants recalled a threatening experience in which they were in control of the outcome. We asked them to write the details about (1) the threat /uncertainty in the experience, (2) what they had done to successfully gain control, and (3) what aspects of that experience eventually got in control. As a manipulation check, participants indicated how much they agreed with “I can control my whole life” and “My life isn’t under my control” (the second question reverse-coded; 1 =
Participants then read a fictional article about the outbreak of the Eosyn virus. We described Eosyn as a virus that spreads through dirty water and seafood and can cause dangerous dehydration and failure of organs. In the high-risk condition, participants learned that the government planned to introduce a potent antibiotic named “Antivirax” into the city's water supply. While effective against Eosyn, Antivirax has been linked to
Results
Manipulation check
Results of a two-way ANOVA revealed a successful manipulation of sense of control and perceived risk of preventive health interventions. Participants reported significantly higher sense of control (
Willingness to compliance
A two-way ANOVA was conducted on willingness to comply with sense of control and perceived risk of the interventions as independent variables. Results revealed a significant main effect of sense of control (
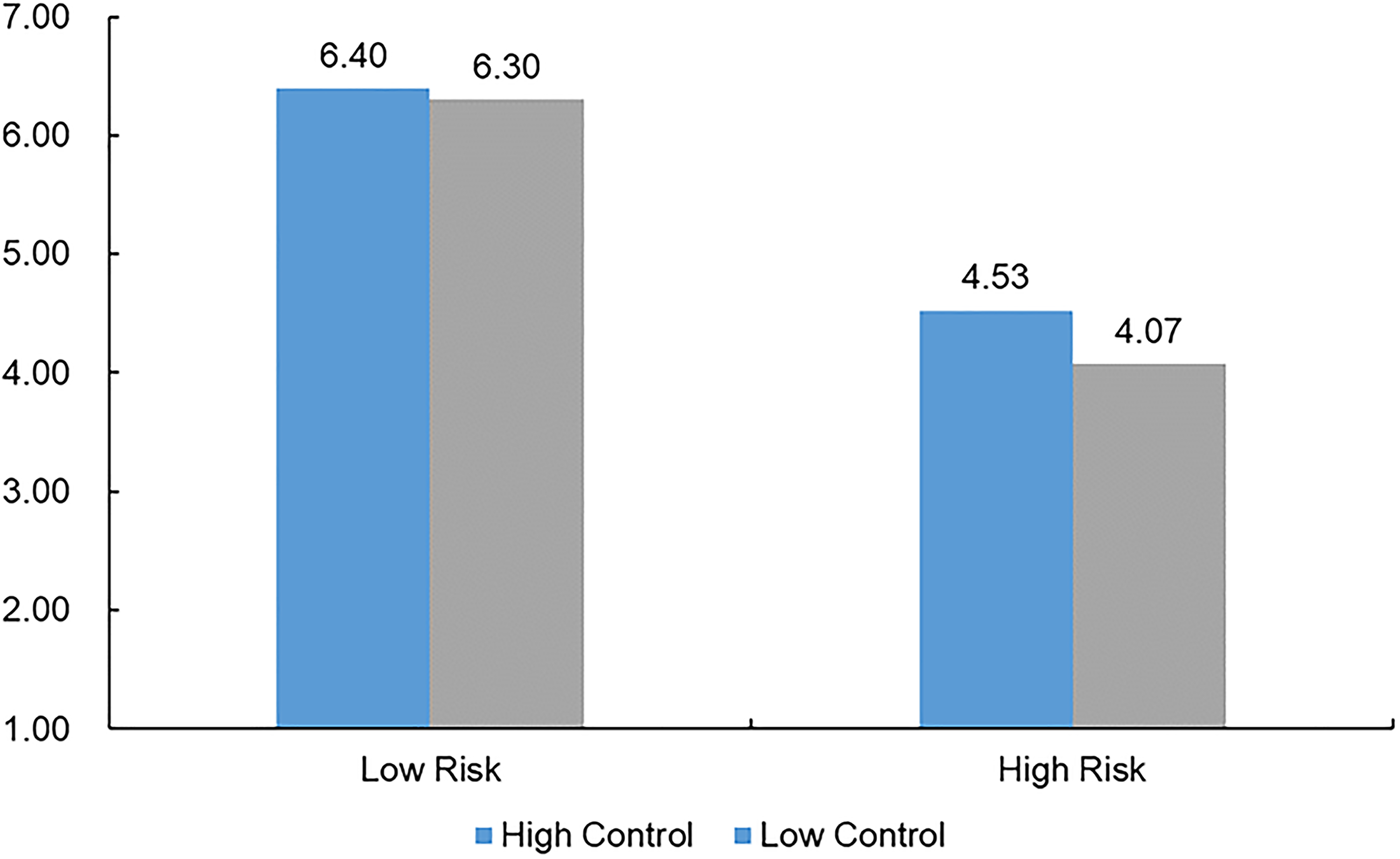
Study 4: Willingness to comply as a function of sense of control and perceived risk of the interventions.
Discussion
Study 4 first provided a boundary condition for the positive effect of sense of control on compliance behavior. Our data indicated that the effect of sense of control on compliance behavior was more evident when the preventive measures in public health had potential risk to personal interests. In contrast, when the preventive measures were introduced without risks, the effect of sense of control on compliance behavior was diminished. Secondly, Study 4 manipulated sense of control by a recall and writing task, proving that willingness to comply with preventive interventions in public health was influenced by a general sense of control over life or other events, not the controllability of the virus itself. It clarified that a high sense of control on previous experience could spill over to the context of public health and promote compliance behavior. Lastly, we made up a fictional “Eosyn” virus and preventive measures about water source reallocation, completely unrelated to COVID-19 pandemic. This demonstrated that our findings had broad applicability in public health research, extending well beyond the specific context of the COVID-19 pandemic.
General discussion
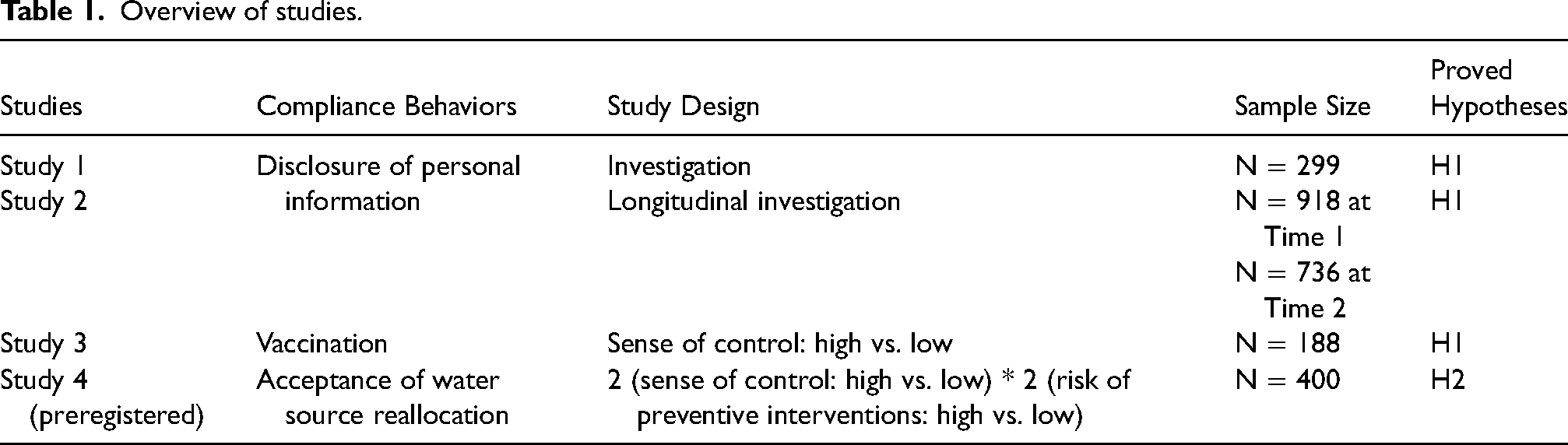
Compliance with public health interventions is crucial for both individual health and public welfare. In recent years, the importance of understanding and enhancing individual compliance with medical interventions has gained widespread recognition, especially after COVID-19 pandemic (Bargain & Aminjonov, 2020; Peitz et al., 2021; Swami & Barron, 2021). This research aimed to explore sense of control as an effective way to motivate compliance with public health interventions, particularly focusing on the interventions which may cause potential risks to individual's personal interests. A series of studies (overview in Table 1) supported our hypotheses that a heightened sense of control positively influenced compliance behaviors by reducing the perceived risk associated with the interventions. Furthermore, we identified a boundary condition: when interventions do not present personal risks, the beneficial effect of sense of control on compliance would be mitigated.
Overview of studies.
By establishing a causal relationship between sense of control, perceived risk of health interventions, and compliance behavior, our research provides valuable insights into a global concern—enhancing compliance with medical measures. Previous examinations of this issue were largely confined to specific diseases and illnesses (DiMatteo, 2004; Munro et al., 2007; Umaki et al., 2012). Our research, however, covers a wide range of health interventions across different countries and times, looking at various types of interventions, even including imaginary diseases, and our results were consistent across these different scenarios.
In addition, we contribute to the findings on sense of control and its impact on individuals’ decision-making. Sense of control, as a psychological trigger to motivate people to respond actively to solve problems (Harris, 1996), has been proved to be linked to increased risk-taking behaviors (Martinez et al., 2011; Nordgren et al., 2007). Our work extends these findings by showing that a general sense of control over actions or past events can spill over to the issue of health interventions, thus reducing perceived risk of the interventions.
Our research also addresses the mixed findings in previous studies about how sense of control influences compliance behavior (Aaronson et al., 1988; Seeman & Seeman, 1983), where the reasons for these inconsistencies were still unclear. We highlight the importance of differentiating health interventions based on their potential risks to personal interests. For example, interventions like regular handwashing or wearing orthodontic braces mainly require consistent practice (Umaki et al., 2012). However, interventions such as new vaccines with uncertain side effects present potential personal risks. Our study sheds light on these risk-associated interventions and clarifies why people might hesitate to comply with them, especially when personal interests are at stake.
Our findings have several implications for medical professionals and the government to promote compliance behaviors. Recognizing that sense of control can enhance compliance by reducing perceived risks of interventions, medical professionals can tailor their strategies to suit different types of interventions, taking into account their varying levels of risk. For interventions that potentially harm personal interests, enhancing patients’ sense of control is an effective strategy to encourage adherence. This can be achieved by empowering patients with comprehensive information, transparently discussing examination results, and sharing success stories from similar cases. Such approaches can significantly increase patients’ willingness to comply with medical recommendations.
In addition to fostering a sense of control during treatment, our findings indicate that a general sense of control over actions and events can also enhance compliance with health interventions. For instance, governments can implement feedback mechanisms that allow citizens to express their concerns and suggestions about health policies, thereby making them feel more heard and in control. Moreover, during flu seasons or pandemics, proactive measures such as ensuring the availability of food and medicine can help prevent feelings of loss of control among the public.
The limitations of this study highlight potential areas for further exploration. While our research categorizes medical interventions based on their risk levels, focusing on those posing potential personal risks, this doesn’t imply that risk-free interventions are automatically or easily adhered to. In reality, many individuals struggle with maintaining consistent exercise or a healthy diet. Future research can also explore strategies to promote compliance with these seemingly lower-risk interventions, as understanding how to motivate adherence in these areas remains an important challenge.
Supplemental Material
sj-docx-1-pac-10.1177_18344909241260128 - Supplemental material for Motivating compliance behaviors in public health through enhanced sense of control
Supplemental material, sj-docx-1-pac-10.1177_18344909241260128 for Motivating compliance behaviors in public health through enhanced sense of control by Chan Li, Li Jiang, Tingting Wang and Yixia Sun in Journal of Pacific Rim Psychology
Footnotes
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the National Natural Science Foundation of China (grant numbers 72372148).
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
