Abstract
Background:
Few studies have been conducted to investigate the socioeconomic profiles of patients with ankylosing spondylitis (AS) and their associations with disease severity and disability.
Objectives:
The objectives of this study were to identify clusters of patients with AS according to their socioeconomic characteristics and to evaluate the associations between these clusters and the severity of the disease and permanent disability.
Design:
This was a cross-sectional and multicentre study.
Methods:
Patients with AS from the REGISPONSER study were included in this analysis. A cluster analysis was conducted using information on sociodemographic (age, sex, race, marital status, education) and socioeconomic (employment, profession, housing conditions and social level) characteristics. Disease burden and permanent disability were compared between the different clusters using logistic regression adjusted for disease duration and disease activity.
Results:
A total of 866 patients with AS were included. Two clusters were identified according to socioeconomic characteristics: Cluster 1 (n = 476), with a predominantly low socioeconomic profile, and Cluster 2 (n = 390), with a predominantly high socioeconomic profile. After adjusting for disease duration, patients in Cluster 1 had a longer diagnosis delay, greater body mass index and greater structural damage than those in Cluster 2. Access to biologic disease-modifying anti-rheumatic drugs (bDMARDs) was similar for both groups. However, patients in Cluster 1 had a greater prevalence of permanent disability than those in Cluster 2 after adjusting for disease duration and disease activity (30.8% vs 13.2%, odds ratio 2.58 (95% confidence interval 1.76–3.83)).
Conclusion:
This study suggests that the socioeconomic status of patients with AS may have implications for disease severity and permanent disability, despite the similar use of bDMARDs.
Background
Axial spondyloarthritis (axSpA) is a chronic rheumatic disease that mainly affects the axial skeleton and sacroiliac joints, although other peripheral manifestations, such as arthritis, enthesitis and dactylitis, may occur. According to the Assessment of Spondyloarthritis International Society (ASAS) classification criteria, 1 patient with axSpA can be classified as having radiographic axSpA (r-axSpA or ankylosing spondylitis (AS)) or nonradiographic axSpA (nr-axSpA) depending on the presence of sacroiliitis on a pelvic X-ray.
The hallmark symptom of patients with axSpA is inflammatory back pain, which can lead to structural damage and, consequently, a deterioration in mobility, 2 quality of life, psychological status and work productivity.3,4 Both clinical and socioeconomic factors have shown to be independently associated with sick leave; specifically, university education and male sex have been independently associated with a lower risk of sick leave, while older age and greater disease activity were found to be independently associated with a greater risk of sick leave. 5 In addition, work disability has been demonstrated to be associated with high disease activity and functional impairment, confirming the role of clinical factors in sick leave.
Many studies have focused on factors associated with work disability and work participation, taking into account not only individual-level socioeconomic factors but also country-level factors. 6 A recent study from the ‘Dévenir des Spondyloarthrites Indifferenciées Récentes (DESIR)’ cohort demonstrated that work disability was mainly explained by disease activity and function rather than socioeconomic factors in patients with recent axSpA. 7 Similarly, a Spanish study showed that permanent disability was strongly associated with functional and structural damage, although socioeconomic factors were poorly evaluated. 8 These studies have focused mainly on identifying factors associated with disability, but no studies have been conducted to examine the socioeconomic profile of patients with a greater probability of permanent disability. Total permanent disability is a condition in which an individual is no longer able to work due to injuries, while partial permanent disability refers to a situation in which the worker’s normal performance is impaired by 33% or more, but he or she can perform the basic tasks of his or her normal job. Conversely, transitory disability is a situation in which the worker is temporarily unable to work.
In the 1990s and 2000s, partial or total permanent disability was frequently recognized in patients with AS, mainly due to the high prevalence of severe clinical forms of AS and the absence of effective drugs that could control disease activity and ankylosis. In fact, according to the National Institute of Statistics, there has been a reduction in disability prevalence since the generalized use of biological disease-modifying antirheumatic drugs (bDMARDs). 9 For example, from 2008 to 2020, the disability rate of the general Spanish population between 35 and 44 years of age was reduced by 18.5%. Similarly, the disability rate of persons between 45 and 64 years of age was reduced by 5.2%–6.9%. 9 However, we hypothesize that patient socioeconomic status plays a role in disability risk, independent of access to drugs, such as bDMARDs.
Spain is a European country with a public national health system in which conventional synthetic (cs-) and b-DMARDs are free of charge regardless of patient income or employment. For this reason, the Spanish Registry of Spondyloarthritis (REGISPONSER) is an excellent registry for evaluating different socioeconomic profiles of patients with AS and their associations with disease severity and permanent disability.
Based on the above, the study aimed to conduct an unsupervised analysis to identify profile clusters of patients with AS according to their socioeconomic characteristics and to evaluate whether these clusters are associated with disease severity and permanent disability.
Methods
Design and population
REGISPONSER is an observational, cross-sectional and multicentre study that includes patients who meet the European Spondyloarthropathy Study Group (ESSG) criteria for SpA. 10
Twenty-one participating hospitals included patients between March 2004 and March 2007 according to the following criteria: (a) fulfilled the ESSG classification criteria for SpA, (b) had blood tests available within 15 days of the inclusion visit and a complete radiographic study within the previous year and (c) agreed to complete all self-administered questionnaires. The registry has previously been widely described. 11
The investigator identified the diagnosis that best fit the clinical profile of the patient, including AS (AS according to the modified New York criteria 12 ), psoriatic arthritis, inflammatory bowel disease-SpA, juvenile SpA, reactive arthritis or undifferentiated SpA. For this ancillary analysis, only patients with a diagnosis of AS were considered.
Data collection
A specific case report form was used to collect clinical data during a single face-to-face meeting with each patient. Information concerning clinical events that occurred before the study visit was retrospectively collected by asking patients or checking their medical records.
The variables evaluated in this study were divided into six groups:
- Sociodemographic data: age, sex, race (white, black, Latin or other), marital status (single, married, divorced or widowed), education (university, bachelor, secondary, elementary or illiterate), body mass index and smoking history.
- Socioeconomic data: employment (employed, unemployed, housekeeper, student or retired), profession (university (employment that requires university studies), technician, employee, skilled worker or nonskilled worker), housing conditions (luxury, optimal, good, deficient or inadequate) and social level according to the Graffar scale (upper, upper-middle, middle, lower-middle or underclass). 13
- Clinical characteristics: age at diagnosis, disease duration, diagnosis delay, family history of SpA, axial pain, buttock pain, synovitis ever, heel enthesitis ever, dactylitis ever, inflammatory bowel disease ever, psoriasis ever, acute anterior uveitis ever, HLAB27 status and urethritis, cervicitis or diarrhoea 1 month before arthritis.
- Burden of the disease: Disease activity was evaluated using the C-reactive protein (CRP) levels (mg/L), the Bath Ankylosing Spondylitis Disease Activity Index (BASDAI), 14 the patient’s global visual analogue scale 15 and the Ankylosing Spondylitis Disease Activity Score (ASDAS). 16 Function was evaluated using the Bath Ankylosing Spondylitis Functional Index (BASFI) 17 and structural damage was evaluated using the Bath Ankylosing Spondylitis Radiology Index (BASRI) for the spine and total axial skeleton (which includes the spine and sacroiliac joints). 18 The Mental Health Survey (MSF12) and the Physical Health Survey (FSF12) of the SF12 questionnaire were completed by the participants. 19
- Treatment: previous and current treatments were collected, such as nonsteroidal anti-inflammatory drugs (NSAIDs), csDMARDs (sulfasalazine, methotrexate or leflunomide) and bDMARDs (tumour necrosis factor (TNF) blockers).
- Disability: On the case report form (CRF), patients were asked about disability at the time of the study visit. According to Spanish social security, two groups of disabilities exist: transitory disability (in which the worker is temporarily unable to work) and permanent disability. Permanent disability can be classified into the following subgroups: (a) partial permanent disability (disability that causes a 33% or greater loss of normal performance, but does not prevent the individual from performing fundamental job tasks); (b) total permanent disability (disability that disqualifies a worker from performing all or the fundamental tasks of their profession, but still allows the individual to perform fundamental tasks associated with another profession); (c) absolute disability (disability that completely disqualifies a worker from any profession or trade) and (d) severe disability (disability that requires the individual to seek the assistance of another person for most essential life tasks). 20 In this study, we focused on permanent disability irrespective of the specific subgroup.
The reporting of this study conforms to the Strengthening the Reporting of Observational Studies in Epidemiology statement. 21
Statistical analysis
Only patients with a diagnosis of AS and complete data for socioeconomic variables were included. A cluster analysis (unsupervised statistical learning methods) was conducted to discover hidden patterns of socioeconomic profiles in these patients with AS. Cluster analysis was conducted using the following variables: age, sex, race, marital status, education, employment, profession, housing conditions and social level according to the Graffar scale.
Clustering was conducted using an iterative partitioning k-means method. The optimal number of clusters was estimated using the ‘NbClust’ package, which provides 30 indices and proposes the best clustering scheme based on all combinations of the number of clusters, distance measures and clustering methods. 22 NbClust provides the number of clusters proposed by all the indices and proposes the best number of clusters according to the majority rule.
After clustering patients, the sociodemographic and socioeconomic variables were compared across the clusters to evaluate whether these groups represented different profiles of patients. Then, the clinical characteristics were compared across clusters using univariate logistic regression. Since the clinical characteristics (such as peripheral and extramusculoskeletal manifestations) can appear over time and depend on the disease duration and diagnosis delay, the univariate analyses were adjusted for these two variables. Similarly, the disease burden and permanent disability were compared across the socioeconomic clusters using univariate logistic regression adjusted for disease duration, diagnosis delay and disease activity (i.e. ASDAS-CRP) since these factors have been described to be associated with both socioeconomic status and disability.
The data were processed and analysed using RStudio v.1.0.143. All comparisons were bilateral, and a p value <0.05 was considered significant.
Ethical considerations
This study was approved by the Ethics Committee (‘Ethics and Health Research Committee’) of the Reina Sofia University Hospital of Córdoba (Spain) on 21 April 2006, with the code ‘REGISPONSER-FASE II’, and all the participants signed an informed consent form to participate in the REGISPONSER registry.
Results
A total of 866 patients who were diagnosed with AS by a rheumatologist and who had complete socioeconomic data were included in this analysis. The description of the included population is depicted in Table 1.
Description of the population included in the analysis.

AAU, acute anterior uveitis; ASDAS-CRP, Ankylosing Spondylitis Disease Activity Score; BASDAI, Bath Ankylosing Spondylitis Disease Activity Index; BASFI, Bath Ankylosing Spondylitis Functional Index; BASRI, Bath Ankylosing Spondylitis Radiology Index; bDMARDs, biological disease-modifying antirheumatic drugs; BMI, body mass index; global VAS, patient’s global visual analogue scale; CRP, C-reactive protein; csDMARDs, conventional synthetic disease-modifying antirheumatic drugs (sulfasalazine, methotrexate or leflunomide); IBD, inflammatory bowel disease; MASES, Maastricht Ankylosing Spondylitis Enthesitis Score; NSAIDs, non-steroidal anti-inflammatory drugs; NSJ, number of swollen joints; SD, standard deviation.
Cluster analysis using sociodemographic and socioeconomic variables
The best clustering scheme yielded by the NbClust function was three clusters followed by two clusters as the second option. However, the scheme of three clusters led to only eight patients in one of the groups; thus, a two-cluster scheme was employed for further analysis.
Overall, Cluster 1 (n = 476, 55.0%) showed a low socioeconomic profile compared to Cluster 2. Patients in Cluster 1 were predominantly married (81.5% vs 71.0%, p < 0.001), with secondary/elementary studies or illiterates (95.6% vs 26.9%, p < 0.001), were unemployed or housekeepers (48.9% vs 32.6%, p < 0.001), had a high frequency of being skilled or nonskilled workers (99.6% vs 51%, p < 0.001), lived in good, deficient or inadequate housing conditions (72.1% vs 34.1%, p < 0.001) and were lower-middle or underclass social levels (8.4% vs 0.5%, p < 0.001) compared to Cluster 2 (Table 2). Conversely, patients in Cluster 2 (n = 390, 45.0%) showed a high socioeconomic profile, being patients predominantly unmarried (either single, divorced or widowed), had a university or bachelor level of education, were employed or retired, worked in university or technician professions, lived in luxury or optimal conditions and were upper, upper-middle or middle social levels.
Comparison of the sociodemographic and socioeconomic characteristics between the two clusters.

Clinical characteristics and burden of disease between clusters
Clinical characteristics were compared between the two clusters to evaluate the factors associated with each socioeconomic profile (Table 3). According to univariate analysis, patients in Cluster 1 (the group with a lower socioeconomic status) were significantly older (51.6 (12.1) vs 44.5 (12.2) years, p < 0.001), had an older age at diagnosis (37.0 (12.5) vs 32.7 (10.3) years, p < 0.001), had a longer disease duration (14.6 (11.2) vs 11.6 (9.9) years, p < 0.001) and had a greater body mass index (27.6 (4.6) vs 25.9 (25.9) kg/m2, p < 0.001). These differences remained significant after adjusting for confounders. Interestingly, a greater diagnosis delay (odds ratio (OR) 1.02 (1.00–1.04)) and a greater prevalence of smoking (OR 1.59 (1.01–2.50)) were found in the low socioeconomic profile (Cluster 1) than in the high socioeconomic profile (Cluster 2) in the adjusted analysis.
Comparison of the clinical characteristics between the two clusters.
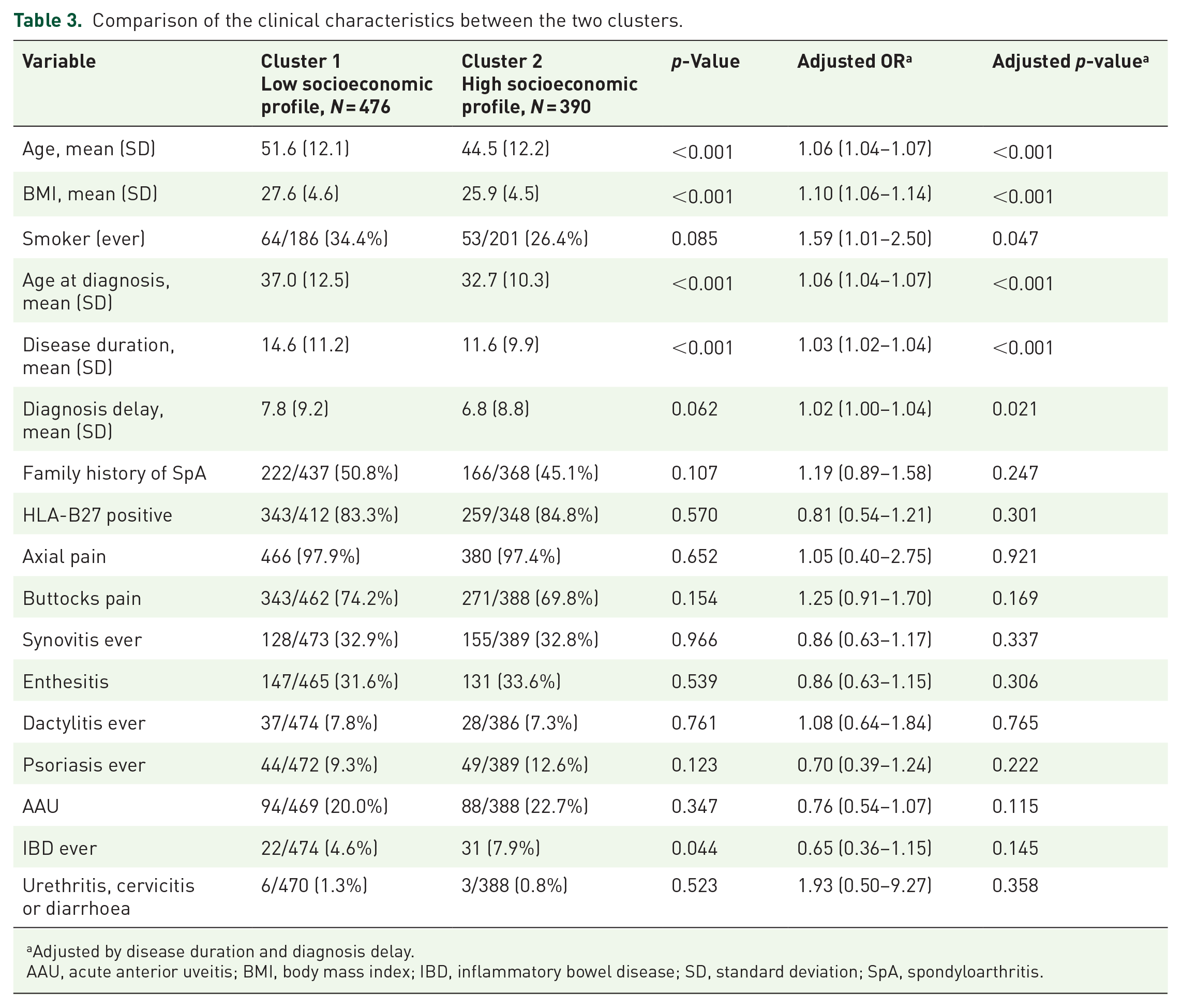
Adjusted by disease duration and diagnosis delay.
AAU, acute anterior uveitis; BMI, body mass index; IBD, inflammatory bowel disease; SD, standard deviation; SpA, spondyloarthritis.
There were no significant differences between clusters found for other clinical characteristics except for a lower prevalence of inflammatory bowel disease history (4.6% vs 7.9%, p = 0.044) in Cluster 1 than in Cluster 2. However, this difference disappeared after adjusting for confounders.
Regarding the burden of the disease (Table 4), patients from the low socioeconomic group had significantly higher mean CRP levels (9.3 (14.0) vs 7.4 (10.2) mg/L, p = 0.023), greater mean ASDAS-CRP (2.8 (1.1.) vs 2.5 (1.1), p < 0.001), higher BASDAI (4.4 (2.3) vs 3.9 (2.4), p = 0.001) and BASFI scores (4.3 (2.6) vs 3.6 (2.7), p < 0.001), poorer mental component scores (48.2 (12.8) vs 45.6 (15.4), p = 0.006) and physical component scores (34.0 (10.6) vs 34.5 (13.1), p = 0.006) on the SF12 questionnaire, and higher BASRI total (7.8 (3.9) vs 6.3 (3.8), p < 0.001) and cervical scores (6.9 (3.2) vs 5.7 (3.2), p < 0.001) compared to patients from the high socioeconomic group. Interestingly, only the SF12 mental component, BASRI total and BASRI cervical scores remained significant after adjusting for disease duration, diagnosis delay and disease activity, suggesting that patient socioeconomic status is independently associated with poorer mental health and greater structural damage.
Comparison of the treatment and burden of the disease between the two clusters.

Adjusted by disease duration, diagnosis delay and ASDAS-CRP.
ASDAS-CRP, Ankylosing Spondylitis Disease Activity Score; BASDAI, Bath Ankylosing Spondylitis Disease Activity Index; BASFI, Bath Ankylosing Spondylitis Functional Index; BASRI, Bath Ankylosing Spondylitis Radiology Index; bDMARDs, biological disease-modifying antirheumatic drugs; CRP, C-reactive protein; csDMARDs, conventional synthetic disease-modifying antirheumatic drugs (sulfasalazine, methotrexate or leflunomide); global VAS, patient’s global visual analogue scale; MASES, Maastricht Ankylosing Spondylitis Enthesitis Score; NSAIDs, non-steroidal anti-inflammatory drugs; NSJ, number of swollen joints; SD, standard deviation.
Treatment use between clusters
Previous and current drug use was compared between clusters to evaluate whether socioeconomic status was associated with access to treatment. As expected, the use of NSAIDs (both ever and currently) was similar between the groups. In addition, the rates of having ever used bDMARDs (30.6% and 27.5% for Clusters 1 and 2, respectively) and the rates of currently using bDMARDs at the time of the study visit (20.3% and 19.9%, for Clusters 1 and 2, respectively) were similar across groups, suggesting similar access to these treatments. However, greater current use of csDMARDs was found in Cluster 1 (i.e. the low socioeconomic profile) than in Cluster 2 (i.e. the high socioeconomic profile) (19.7% vs 27.1%, p = 0.011, respectively), although this difference disappeared after adjusting for confounders.
Permanent disability between clusters
Finally, we compared the permanent disability between clusters (Figure 1). The prevalence of permanent disability in the low socioeconomic profile was greater than in the high socioeconomic profile (30.8% vs 13.2%, p < 0.001), while the prevalence of transitory disability was low in both groups. Interestingly, after adjusting for disease duration, diagnosis delay and disease activity, logistic regression showed an OR of 2.44 (95% CI 1.63–3.71) for permanent disability in the low- versus high socioeconomic profile, confirming the greater likelihood of this permanent disability in patients with a lower socioeconomic status (Table 4).

Prevalence of permanent and transitory disability between clusters.
Discussion
This cross-sectional study provides new evidence of the existence of socioeconomic profiles for patients with AS and confirms their association with disease burden and permanent disability. Despite similar access to bDMARDs between groups, we found that a lower socioeconomic profile was associated with poorer mental health status, greater structural damage and a greater likelihood of permanent disability. In previous studies, the most important factor associated with disability was disease activity, while socioeconomic status was less important.5,7 Interestingly, in this study, we found that socioeconomic status remained a major external factor associated with permanent disability after accounting for disease activity and disease duration, emphasizing the important role of the socioeconomic status in work productivity and loss of employment.
The prevalence of permanent disability in this registry was 23.1%, which was greater than in other cohorts, probably due to the longer disease duration and the longer date of enrolment (2004–2007), when bDMARDs were not widely used. However, despite these two factors, the prevalence of permanent disability was surprisingly high, considering that the mean age of the population was 48.4 years. In the DESIR cohort (which included patients with less than 2 years of disease duration), the described permanent disability rate was 1% at baseline. Conversely, another French study reported a 36% cumulative work withdrawal after 20 years of having the disease, 23 confirming the increasing probability of work disability as the disease progresses.
The unsupervised analysis showed the presence of two profiles of patients according to demographic, social and economic variables: (a) a low socioeconomic status, predominantly patients with secondary or elementary studies, with only 50% employed or retired, skilled and nonskilled professions, with good, deficient or inadequate housing conditions and lower-middle or underclass social levels and (b) a high socioeconomic status, predominantly patients with university or bachelor’s studies, employed or retired, with university or technician professions, living in optimal or luxury conditions and with upper or middle-class social levels.
Interestingly, we found that Cluster 1 (the low-income group) suffered a longer diagnosis delay compared to Cluster 2 (the high-income group). This could be explained by two factors. First, persons with a high socioeconomic status are referred more frequently to practising specialists than persons with a low socioeconomic status, as was demonstrated in a Danish study. 24 Second, education level and income have been demonstrated to be associated with a chronic pain diagnosis rather than SpA. The increased incidence of consultation for chronic pain in persons with low socioeconomic status and manual jobs may influence the physician’s perception and increase the probability of receiving a diagnosis of chronic pain first and causing delay in diagnosing SpA. 25 Additionally, patients who perform manual or physical work often have mechanical or degenerative damage to the spine that coexists with inflammation. This observation implies that mechanical pain can coexist with inflammatory pain, potentially leading to misdiagnosis by a physician.
In addition, Cluster 1 had a greater body mass index than Cluster 2. This finding is in line with an important study conducted in the United Kingdom that demonstrated the association between body mass index and several measures of lower socioeconomic status (such as household income and deprivation), supporting the idea that body mass index plays an important role in determining a person’s socioeconomic status. 26 Interestingly, neither the clinical characteristics nor treatment prescriptions of patients with axSpA differed among the clusters. As mentioned above, the Spanish health system provides csDMARD and bDMARD treatment free of charge, independent of patient income, employment or diagnosis. Thus, similar access to cs- and bDMARDs in this registry was expected. However, despite this similar access to treatment, patients from Cluster 1 showed more severe disease represented by greater structural damage measured by the BASRI, as well as a greater likelihood of permanent disability after adjusting for disease duration and disease activity. This greater disease severity in patients with a lower socioeconomic status may be influenced by different factors. First, a longer diagnosis delay can lead to a delay in the cs- and bDMARD treatment initiation and consequently, poor control of the disease that lasts for years. Second, the higher body mass index in comparison with patients from Cluster 2 has been demonstrated to be associated not only with higher disease activity in axSpA patients 27 but also with a lower rate of success in obtaining a response to anti-TNF drugs.28–30 Third, poorer knowledge of the disease and self-management of biological therapy has been observed in patients with low education levels. For example, in previous studies, patients without a university education had poorer knowledge of the self-management of biological therapy, and unemployed patients were less adherent to treatment.31,32 Fourth, environmental conditions may influence childhood infections and the gut microbiota composition, which could determine the risk of SpA and the early initiation of the disease.33,34 Another possible explanation for the greater structural damage in Cluster 1 could be explained by the greater prevalence of smoking, which has been demonstrated to be directly associated with radiographic progression. 35 Finally, patients with lower income status may have reduced access to supervised rehabilitation and compliance with home-based exercise, 36 which could lead to a greater probability of muscle wasting that reduces their function and physical activity. 37
Patients from Cluster 1 (low socioeconomic status) also showed a greater likelihood of permanent disability than patients from Cluster 2 (high socioeconomic status). We acknowledge that, due to the cross-sectional nature of the study, we cannot establish whether low income is the cause or the consequence of permanent disability. However, considering the greater structural damage, greater prevalence of obesity and greater frequency of ‘blue collar’ jobs in Cluster 1, we can establish the assumption that patients in Cluster 1 are unable to continue their jobs after several years of having the disease. These findings prompted us to consider the health care provided to this patient profile. 38 In addition, preventing and reducing obesity in these patients is important for controlling disease activity, improving treatment efficacy and potentially reducing structural damage. In fact, severe obesity has been described as one factor associated with difficult-to-treat axSpA. 39 Interestingly, treatment with a very low-energy liquid diet can lead to long-term improvements in disease activity after 24 months of follow-up in patients with psoriatic arthritis. 40
This study has several limitations and strengths. One limitation is the cross-sectional nature of the study, which prevents the establishment of a causal relationship between socioeconomic status and permanent disability. However, several associations were demonstrated, which can be confirmed through future prospective studies. Another limitation is that the registry was developed between March 2004 and March 2007, when neither the axial ASAS criteria 1 nor the modified Stoke Ankylosing Spondylitis Spinal Score (mSASSS) index existed. 41 Instead, the ESSG was applied to allow us to include patients within the whole spectrum of the disease and the BASRI was used for the evaluation of structural damage. One strength of this study is the variety of socioeconomic variables collected in the CRF, which allowed us to consider some factors not included in previous studies. For example, the Graffar scale was used to determine the social status and housing conditions of patients. Another strength is the employed methodology (i.e. the clustering analysis), which represents an unsupervised exploratory analytical technique that aims to identify homogeneous groups of cases when the groups are previously unknown. In this sense, this technique may be especially valuable in the identification of clusters based on socioeconomic variables in patients with AS. As a result, we found two profiles of patients with a greater likelihood of permanent disability instead of isolated variables associated with this outcome. Finally, the majority of previous studies have focused on work participation and sick leave, but very few studies have evaluated permanent disability in patients with AS.
Conclusion
In conclusion, the results obtained in this study suggest the existence of two principal socioeconomic profiles in patients with AS: (1) a lower socioeconomic status, which is associated with a longer disease duration, higher body mass index, greater structural damage and a greater likelihood of permanent disability and (2) a higher socioeconomic status, which is associated with a shorter diagnosis delay, better outcomes and a lower risk of permanent disability. In addition, both profiles had similar access to cs- and bDMARDs, suggesting that socioeconomic status may independently influence the severity of the disease and work participation. The evaluation of these socioeconomic variables could help to identify patients at risk of permanent disability and, therefore, contribute to the development and implementation of new care plans that would allow to reduce the incidence of disability in these patients.
Footnotes
Acknowledgements
Authors would like to thank all the investigators from the REGISPONSER study group: P. Zarco-Montejo, Hospital Fundación Alcorcón, Madrid; C. González, Hospital Gregorio Marañón, Madrid; J. Mulero-Mendoza, Hospital Puerta de Hierro, Madrid; J.L. Fernández-Sueiro, Hospital Juan Canalejo, La Coruña; R. Almodóvar, Hospital Fundación Alcorcón, Madrid; J. Gratacós-Masmitjá, Hospital Parc Taulí, Barcelona; X. Juanola-Roura, Hospital Bellvitge, Barcelona; C. Montilla, Hospital Virgen de la Vega, Salamanca; E. Moreno, Hospital San Rafael, Barcelona; A. Juan-Mas, Hospital Fundación Son Llatzer, Mallorca; P. Fernández-Dapica, Hospital 12 de Octubre, Madrid; M.C. Fernández-Espartero, Hospital de Móstoles, Madrid; V. Villaverde, Hospital de Móstoles, Madrid; M.E. Brito-Brito, Hospital Universitario Ramón y Cajal, Madrid; J.C. Torre-Alonso, Hospital Monte Naranco, Oviedo; E. Batlle-Gualda, Hospital General Universitario, Alicante; E. Cuende-Quintana, Hospital Universitario Príncipe de Asturias, Madrid; T. Clavaguera-Poch, Hospital de Palamós, Girona; M. Fernández-Prada, Hospital Universitario de Guadalajara, Guadalajara and E. Judez-Navarro, Hospital Virgen del Perpetuo Socorro, Albacete.
