Abstract
Low dopamine levels may cause depressive symptoms. Dopamine is also involved in sexual behavior. Rotigotine is a nonergolinic dopamine agonist. Fluoxetine, an antidepressant that acts as a selective serotonin (5-HT) reuptake inhibitor, may cause moderate or severe sexual dysfunction. This study aims to investigate the effects of rotigotine-loaded microspheres (RoMS) and rotigotine on fluoxetine-induced impairment of sexual function and their efficacy in depression-model rats. Rats with depressive-like behavior, induced by bilateral olfactory bulbectomy, were treated intragastrically with fluoxetine and co-administered RoMS or rotigotine subcutaneously. Then, copulatory behavior and open field tests were conducted. Serum luteinizing hormone and testosterone levels were assayed with enzyme-linked immunosorbent assay kits. The concentrations of 5-HT, dopamine, and norepinephrine were measured in the raphe nucleus and amygdala. The results showed that sexual function was decreased in olfactory bulbectomy rats and significantly deteriorated by fluoxetine. Co-administration of RoMS partly reversed the fluoxetine-induced impairment of sexual function, but rotigotine administration did not produce any improvement. Hyperactivity in olfactory bulbectomy rats was significantly attenuated by fluoxetine but was not influenced by co-administration of RoMS. Compared with the fluoxetine group, RoMS increased the testosterone, luteinizing hormone, dopamine, and norepinephrine levels. These findings indicated that RoMS improved the fluoxetine-induced impairment of sexual function and did not affect its antidepressant efficacy in depressive rats, which provides a potential treatment for patients with depression that can reduce the possibility of sexual dysfunction. Additionally, co-administration of fluoxetine with RoMS may be beneficial for Parkinson's disease patients with depression.
Keywords
Introduction
Depression is the most common psychiatric disorder and a major cause of disability worldwide. Depression is related to an increase in vulnerability to cardiovascular disease, stroke, diabetes, and cancer. Additionally, it is associated with a significant reduction in lifespan because of suicide (Beurel et al., 2020). Major depression is the leading cause of disability worldwide and affects an estimated 350 million individuals globally. In addition to mood symptoms, individuals with major depression experience impairments of occupational, physical, and social functioning (Bijlsma et al., 2014).
A challenge of depression management is the inconvenient effects of antidepressants. Sexual dysfunction is a common cause of antidepressant discontinuation (Rothschild, 2000) and may occur at the seventh day after initiation of antidepressant treatment. Furthermore, side effects of antidepressants decrease patient compliance. Less than 30% of patients with depression adhere to the prescribed drug therapy because of an adverse sexual event. Fluoxetine is a selective serotonin reuptake inhibitor that is widely used to ameliorate depressive symptoms. Sexual dysfunction associated with fluoxetine treatment continues to be a major compliance issue for antidepressant therapies. The reported incidence of fluoxetine-induced sexual dysfunction is approximately 30–60% (Sukoff Rizzo et al., 2008). Fluoxetine resulted in a marked reduction in the number of non-contact penile erections in sexually experienced male rats (Sukoff Rizzo et al., 2008) and produced inhibitory effects on male rat copulation, particularly on ejaculation. Fluoxetine has also been reported to disrupt paced mating behavior in sexually experienced female rats.
Bupropion, a dopamine and norepinephrine reuptake inhibitor, is indicated for treatment of depression. Bupropion has no negative impact on sexual function, and it even improves sexual function for those with sexual impairments (Pereira et al., 2014). Activation of the dopaminergic nervous system may be a strategy to exert antidepressant effects without sexual dysfunction, which will improve both tolerability and compliance in the management of depression (Bijlsma et al., 2014). The involvement of dopamine in depression is thought to be dependent upon motivation and reward (Just, 2015). Homovanillic acid is a metabolite of dopamine and is decreased in the cerebrospinal fluid in patients with depression (Cerebrospinal fluid monoamine metabolite concentrations in depressive disorder: A meta-analysis of historic evidence. Ogawa S, Tsuchimine S, Kunugi H. J Psychiatr Res. 2018 Oct;105:137–146. doi: 10.1016/j.jpsychires.2018.08.028.). Additionally, hypofunction of the mesolimbic dopaminergic system is considered to be related to the etiology of depression. Dopamine also plays a major role in sexual behavior. Dopamine in the brain is involved in triggering the erectile response and mediating the anticipatory phase of sexual behavior (Giuliano & Allard, 2001). Clinical and pre-clinical evidence has shown that deficits in dopaminergic transmission and stimulation may be associated with anhedonia (Breuer et al., 2008).
Rotigotine is a nonergolinic agonist of dopamine D3/D2/D1 receptors used to treat Parkinson's disease (PD) (Tian et al., 2013). It is a lipid-soluble agonist with a molecular weight of 315 Da. The rotigotine concentration peaks at 2 h after intramuscular injection and decreases rapidly after 2 h, and rotigotine is completely eliminated at 20 h after a single administration (Lv et al., 2019). Rotigotine-loaded microspheres (RoMS), developed by Shandong Luye Pharmaceutical Co., Ltd. (Yantai, China), were prepared with poly(lactide-co-glycolide) as a drug carrier. RoMS provide continuous delivery of rotigotine with a relative steady drug concentration in the plasma and brain after intramuscular injection in rats. The plasma level of rotigotine peaked on day 4 after a single intramuscular injection of RoMS, and rotigotine was still detected in the circulation on day 14 after RoMS treatment. RoMS exerted consecutive efficacy in PD rats for 14 days and produced synergistic antinociception with acetaminophen or celecoxib (Wang et al., 2016). A Phase III clinical trial of RoMS in China and a clinical study of RoMS in the USA were conducted on PD patients. Depression is a common and disabling psychiatric condition in PD. A previous study showed that up to 50% of PD patients experience depression in the course of their illness (Weintraub, 2020). It is still not clear whether rotigotine can alleviate the impact of antidepressant treatment on sexual function in patients with depression. The present study aims to investigate the effects of the dopamine receptor agonist rotigotine, especially in RoMS, which can continuously release rotigotine for more than 14 days, on fluoxetine-induced impairment of sexual function in sexually experienced male rats and the efficacy of fluoxetine in a rat model of depression induced by bilateral olfactory bulbectomy.
Materials and Methods
Animals
Female and male Sprague–Dawley rats (IMSR Cat# TAC:icr, RRID:IMSR_TAC:icr) weighing 200 to 250 g were obtained from Jinan Pengyue Company, China. Animals were housed and maintained on a 12-h light/dark cycle at a controlled temperature (23–25°C) and humidity (43%–47%) with unlimited access to food and water. The animals were acclimatized in the laboratory for 1 week. Female and male animals were in different cages in the experimental room, with two rats per cage. The experimental protocol was approved by the Ethics Committee of Yantai University. All experiments were performed in accordance with the National Institutes of Health Guide for the Care and Use of Laboratory Animals (NIH Publications No. 8023, revised 1978).
Drugs
RoMS were provided by Luye Pharmaceutical Co., Ltd. (Batch number: 20170222). Fluoxetine (RRID:SCR_000037) and rotigotine were purchased from Sigma Aldrich (St. Louis, MO, USA).
Olfactory Bulbectomy
Olfactory bulbectomy was performed to prepare the animal model of depression (Riad et al., 2017). Male rats were intraperitoneally (i.p.) injected with sodium pentobarbital at a dose of 50 mg/kg. A midline incision was made in the brain. Bilateral burr holes were drilled at 2 mm lateral from the midline and 8 mm anterior from bregma. The main olfactory bulb and the accessory olfactory bulb were aspirated with a hypodermic needle. Then, the rats were allowed to recover for 14 days before further experimental procedures were conducted.
Ovariectomy Surgery
Ovariectomy surgery was carried out by a ventral abdominal incision performed under anesthesia induced by sodium pentobarbital (50 mg/kg, i.p.). The ovaries and oviducts were ligated (1 cm from the ovary) and then removed. The skin and muscle were separately sutured. To avoid postsurgical infection, penicillin (8,000 U/dose) was administered (i.p.) for 3 consecutive days.
Experimental Design
The animals were divided into six groups (n = 8 in each group), including a control group, an olfactory bulbectomy group, a fluoxetine group (10 mg/kg), a fluoxetine plus RoMS group, and a fluoxetine plus rotigotine group. The olfactory bulbectomized animals were treated intramuscularly with a single dose of rotigotine (20 mg/kg) or RoMS (20 mg/kg). Two hours later, they were treated intragastrically with fluoxetine at a dose of 10 mg/kg, once a day for 14 days. The animals in the control and olfactory bulbectomy groups received an equal volume of vehicle. The copulatory behavior and open field tests were performed on the 14th day. Then, serum luteinizing hormone and testosterone levels were assayed with enzyme-linked immunosorbent assay kits. Serotonin (5-HT), dopamine, and norepinephrine levels in the raphe nucleus and amygdala were also measured by ultra-high performance liquid chromatography tandem mass spectrometry (UHPLC-MS/MS) (RRID:SCR_017805) (Fig. 1).
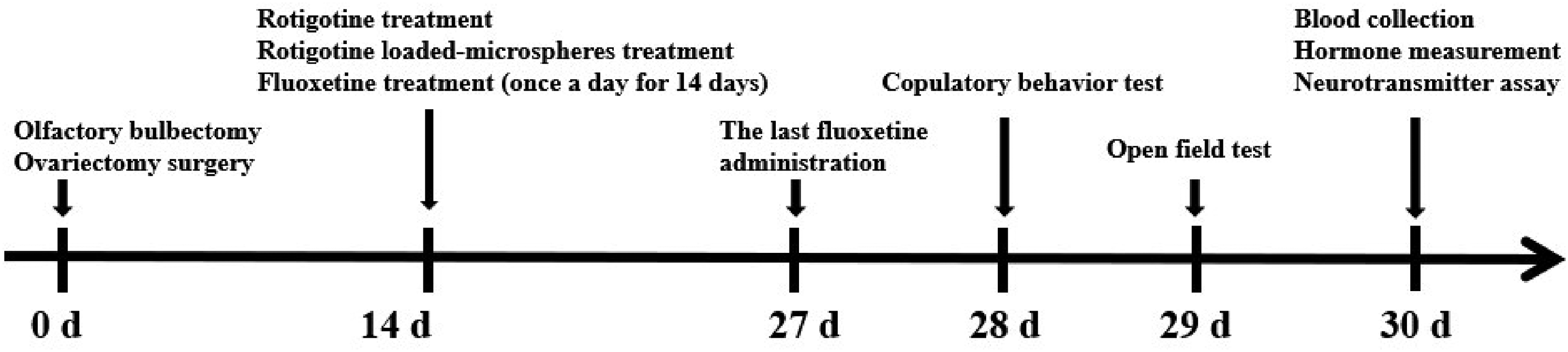
Experimental design and timeline.
Copulatory Behavior Test
At 24 h after the last fluoxetine administration, copulatory behavior was assessed from 7:30 to 10:30 pm (dark phase). One male rat was placed in a cage (52 cm × 32 cm × 19 cm) that was illuminated by a red light. After a 10-min adaptation, the copulatory behavior test was conducted by the introduction of a sexually receptive ovariectomized female rat. At 48 and 6 h prior to the behavioral test, the ovariectomized animals were induced into estrus by subcutaneous injection of estradiol benzoate (20 mg/rat) and progesterone (0.5 mg/rat). The precoital and coital behaviors were recorded with a camera (Logitech, C930E, Shenzhen, China) for 30 min. The behavior categories were scored by an experimenter who was blinded to the treatment. The percentages of male rats in each group showing intromissions and ejaculating were also determined.
Open Field Test
At 24 h after copulatory behavior test, an open rectangular plastic box (75 cm × 75 cm × 40 cm) was used to conduct the open field test. After a 1-h acclimation period, in which the animals acclimated to the test room while in their home cage, each rat was placed in the center of the open field and allowed to explore for 10 min. Then, the animal was allowed to explore the surrounding area for 5 min. The total distance and mean speed of rats were recorded with a camera (Logitech, C930E, Shenzhen, China) and then were analyzed with SMART3.0 software (Panlab Harvard Apparatus, Massachusetts, USA). The olfactory bulbectomy-induced depressive animals showed hyperactivity in the open field. Antidepressant treatment reduced the total distance and the mean speed.
Measurement of Serum Luteinizing Hormone and Testosterone Levels
At 24 h after open field test, the rats were anesthetized with isoflurane, and then blood was obtained from the abdominal aorta with a tube. After centrifugation at 3,500g for 10 min, the serum was collected. The serum luteinizing hormone and testosterone levels were measured with enzyme-linked immunosorbent assay kits specific for testosterone (Reacts with Mouse and Rat; Sensitivity: 0.07 ng/ml; Abcam, Cambridge, Britain) and luteinizing hormone (Reacts with Mouse and Rat; Sensitivity: 0.01 ng/ml; R&D Systems, Minnesota, USA) according to the manufacturer's instructions.
Measurement of 5-HT, Dopamine, and Norepinephrine Concentrations
The rats were decapitated, and the brains were quickly removed. The raphe nucleus and the amygdala were dissected according to their precise location described in a brain atlas (Charles Watson, George Paxinos. The rat brain in stereotaxic coordinates. 5th Edition). The concentrations of 5-HT, noradrenaline, and dopamine were measured using UHPLC-MS/MS (Agilent, California, USA). The UHPLC system consisted of a SIL-30ACMP autosampler, an Applied Biosystems Sciex 4500 system triple quadrupole mass spectrometer (AB Sciex, Foster City, CA, USA), two LC-30AD pumps, and a CTO-30A column oven (Shimadzu Corporation, Kyoto, Japan). Samples were separated on a column (2.1 mm × 100 mm, 1.8 µm, Waters, Milford, MA, USA) at 40°C. The mobile phase consisted of solvent A and solvent B. Solvent A consisted of 0.1% formic acid in water, and solvent B consisted of 0.1% formic acid in acetonitrile. Gradient elution was conducted according to the following conditions: 1.0–3.0 min, gradient to 20% B; 3.0–4.0 min, gradient to 50% B; 4.0–4.5 min, held at 50% B; 4.5–4.6 min, gradient to 2% B; 4.6–5.0 min, held at 2% B. The sample (2 µL) was injected with an autosampler. Mass spectrometry was carried out according to the following ionization parameters: ion spray voltage 5,500 V, ion source gas 1 55 psi, curtain gas 12 psi, ion source gas 2 55 psi, entrance potential 10 V, source temperature 570°C, dwell time of each MRM transition 40 ms. Quantification was performed using Analyst Instrument Control and Data Processing software version 1.6.2 (AB Sciex) (Liu et al., 2018; Sha et al., 2017).
Statistical Analysis
The percentage data of copulatory behavior test were analyzed with Kruskal-Wallis one-way ANOVA analysis followed by Fisher exact test. The data of intromission latency and ejaculation latency were analyzed with Kruskal-Wallis one-way ANOVA followed by Dunnett's test. The other data were expressed as means ± SD and were analyzed with one-way ANOVA followed by Tukey's post-hoc test. A value of p < 0.05 was considered statistically significant.
Results
Effect of RoMS on the Proportion of Animals Showing Intromissions and Ejaculation and on the Intromission Latency and Ejaculation Latency
The proportion of animals in the fluoxetine group showing intromissions (0/8 = 0.0%) was lower than those of the olfactory bulbectomy group (8/8 = 100.0%). However, RoMS administration attenuated the fluoxetine-induced decrease in these proportion (8/8 = 100.0% versus 0/8 = 0.0%). The percentage of males showing intromissions in the fluoxetine plus rotigotine group is 2/8 = 25%, (Figs. 2A and 3A). The proportion of animals ejaculating in the fluoxetine group (0/8 = 0.0%) was lower than those of the olfactory bulbectomy group (7/8 = 87.5%). The proportion of animals ejaculating in the fluoxetine plus RoMS group (7/8 = 87.5%) was increased when compared with that of the fluoxetine group (0/8 = 0.0%), (Figs. 2C and 3C). The intromission latency and the ejaculation latency in the fluoxetine group were higher than those of the olfactory bulbectomy group (p < 0.01). However, the intromission latency and the ejaculation latency in the fluoxetine plus RoMS group were significantly decreased (p < 0.05). Rotigotine treatment did not reverse the fluoxetine-induced prolongation of the intromission latency and the ejaculation latency, (Figs. 2B, 2D, 3B and 3D).
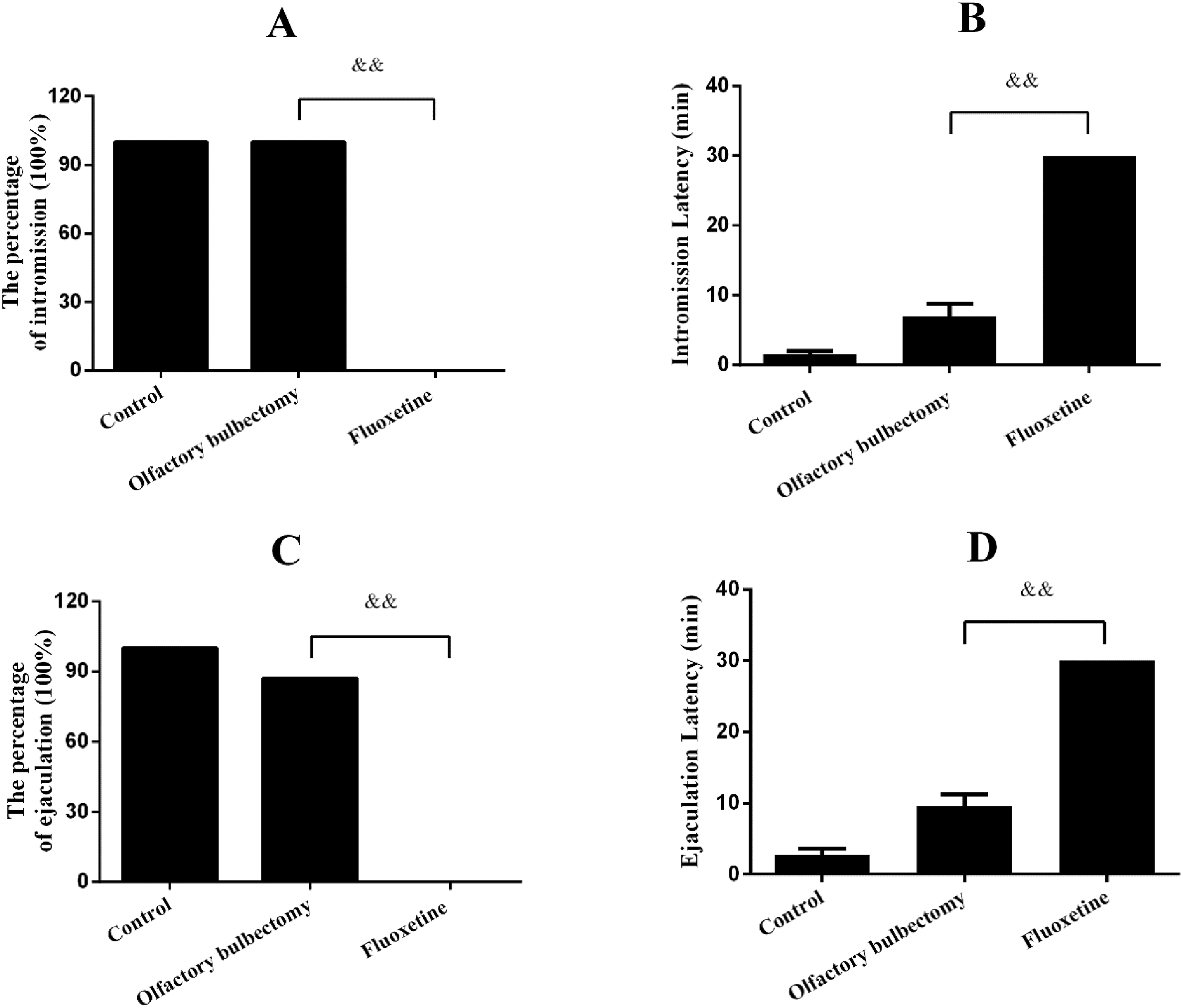
Effects of fluoxetine on
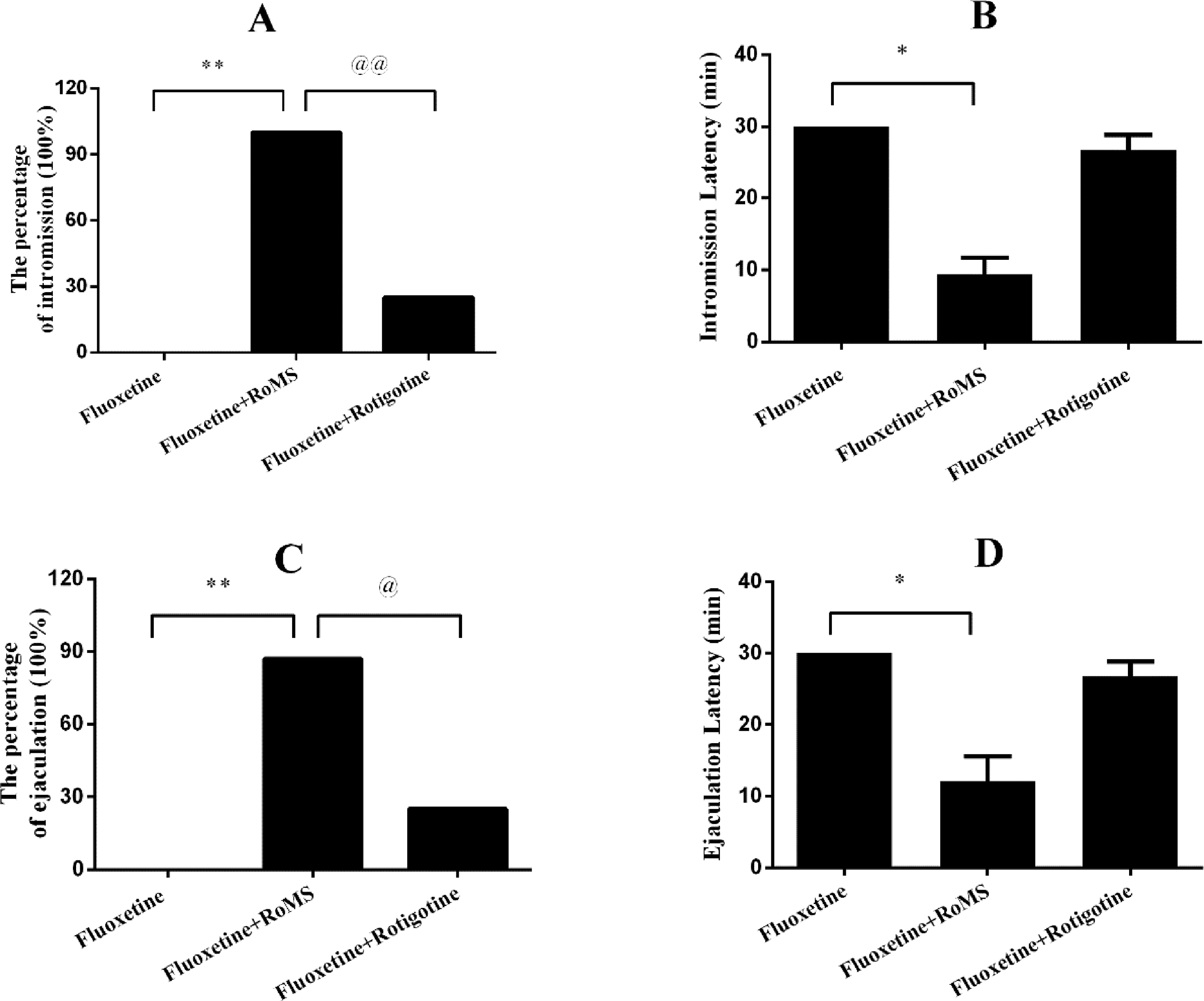
Effects of RoMS on
Effect of RoMS on the Mean Speed and Total Distance
The mean speed and total distance in the open field test are shown in Fig. 4. The mean speed and total distance in the olfactory bulbectomy group were significantly increased compared with those of the control group (p < 0.05, Figs. 4A and 4C). Fluoxetine administration significantly reduced the mean speed and total distance (p < 0.01, Figs. 4A and 4C). Compared with the fluoxetine group, the mean speed and total distance in the fluoxetine plus RoMS and fluoxetine plus rotigotine groups were not significantly different (Figs. 4B and 4D).
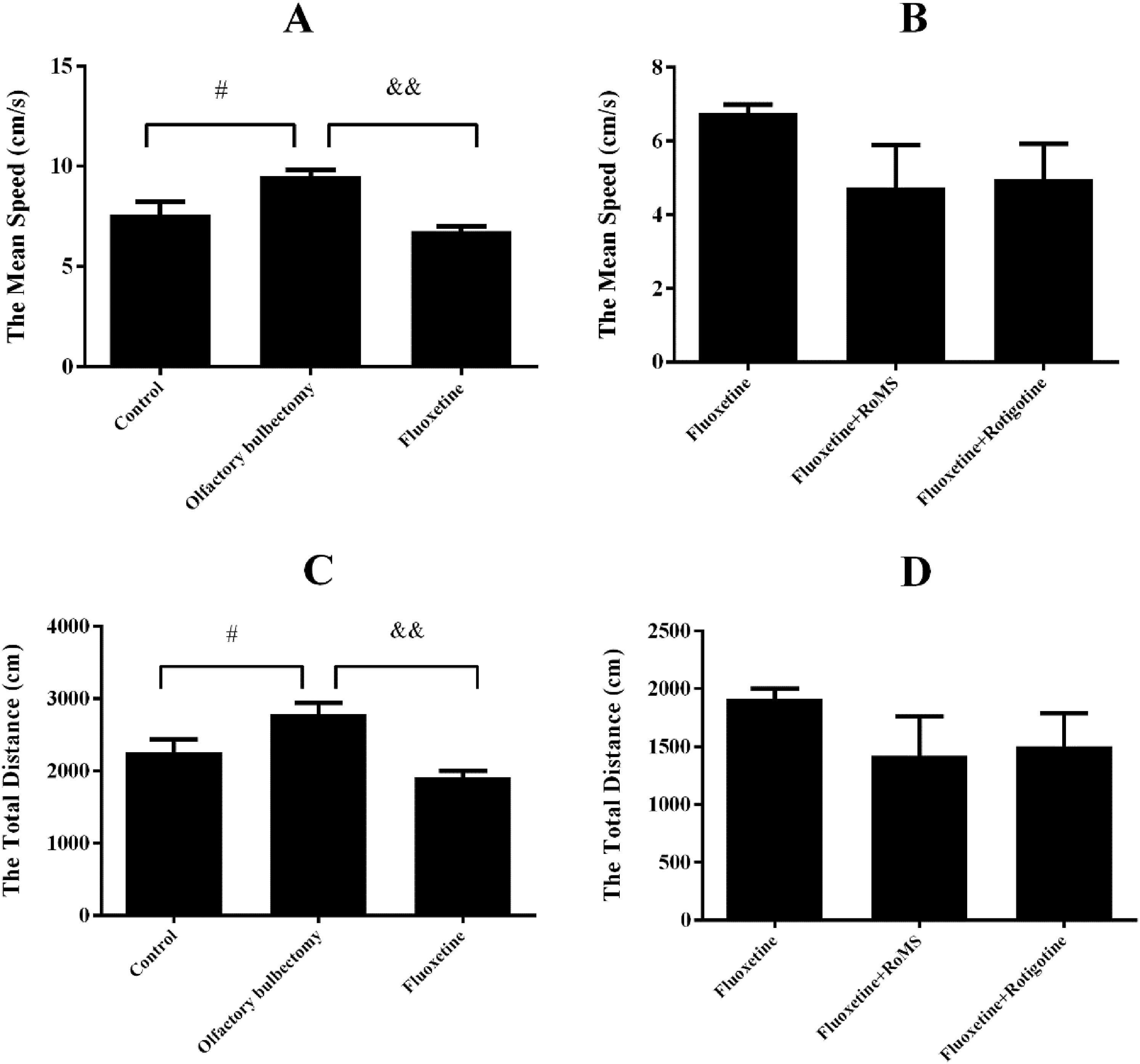
Effects of fluoxetine on
Effect of RoMS on Serum Luteinizing Hormone and Testosterone Levels
The serum luteinizing hormone and testosterone levels in the olfactory bulbectomy group were significantly lower than those of the control group (p < 0.05, Figs. 5A and 5C). Fluoxetine significantly decreased the testosterone levels (p < 0.01, Fig. 5A). RoMS treatment ameliorated the fluoxetine-induced reduction of the serum luteinizing hormone and testosterone levels (p < 0.01, Figs. 5B and 5D). The serum luteinizing hormone and testosterone levels in the fluoxetine plus RoMS group were significantly increased compared with those of the fluoxetine plus rotigotine group (p < 0.05, Figs. 5B and 5D).
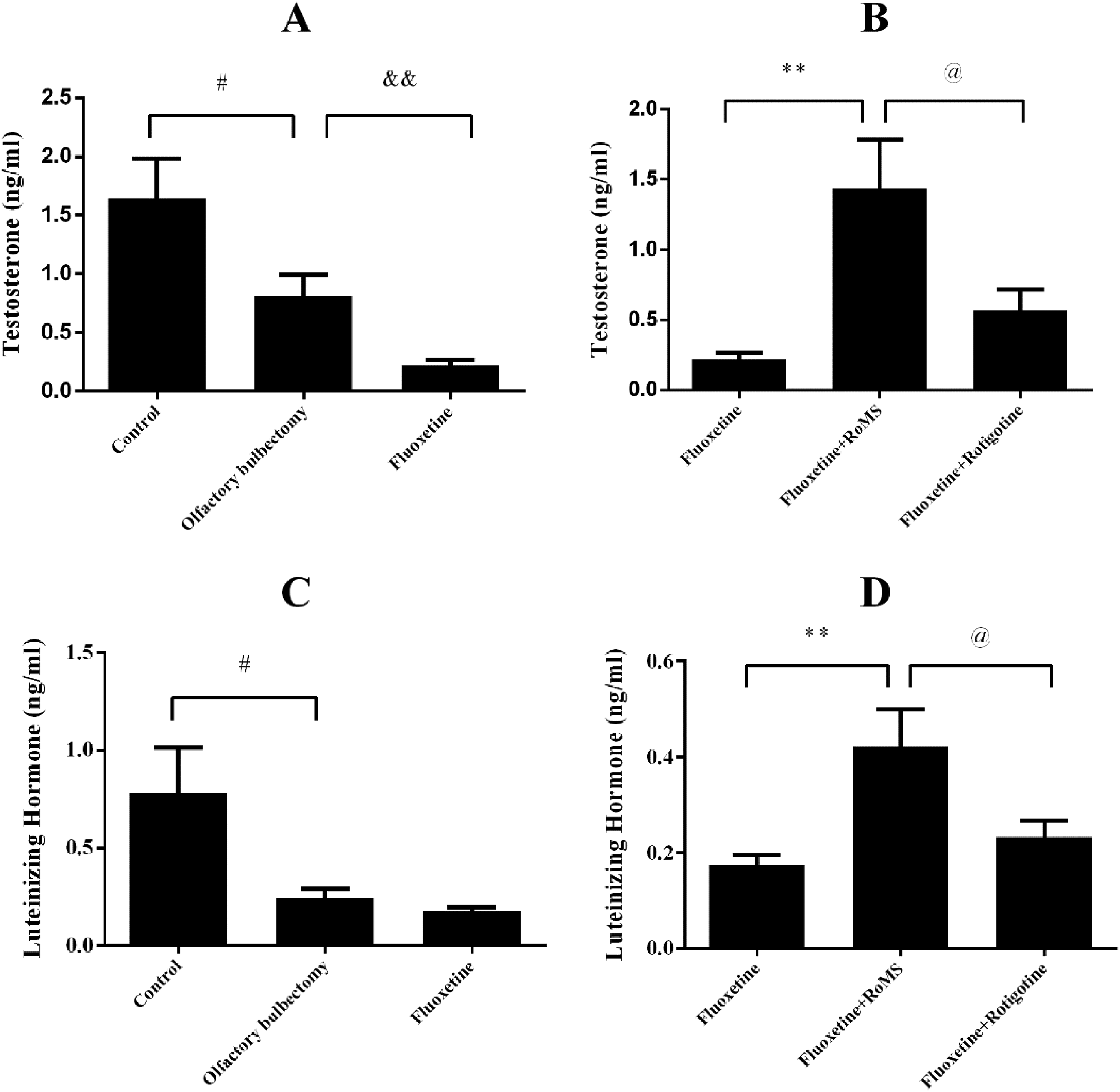
Effects of fluoxetine on
Effect of RoMS on the Dopamine, Norepinephrine, and 5-HT Concentrations in the Amygdala and Raphe Nucleus
The dopamine concentration in the amygdala and raphe nucleus in the olfactory bulbectomy group was significantly decreased compared with that in the control group (p < 0.05 or p < 0.01, Figs. 6A and 6C). The dopamine concentration in the amygdala in the fluoxetine group was lower than that of the olfactory bulbectomy group (p < 0.01, Fig. 6A). Compared with the fluoxetine group, the dopamine concentrations in the amygdala and raphe nucleus in the fluoxetine plus RoMS group were significantly elevated (p < 0.05, Figs. 6B and 6D). Compared with the fluoxetine plus rotigotine group, the dopamine concentration of the raphe nucleus in the fluoxetine plus RoMS group was elevated (p < 0.05, Fig 6D). The norepinephrine concentrations of the amygdala and raphe nucleus in the olfactory bulbectomy group were significantly reduced when compared with the control group (p < 0.05, Figs. 7A and 7C). Fluoxetine administration did not affect the norepinephrine concentration of the amygdala or raphe nucleus in the olfactory bulbectomy rats (Figs. 7A and 7C). Compared with the fluoxetine group, the norepinephrine concentration of the amygdala in the fluoxetine plus RoMS group was elevated (p < 0.05, Fig. 7B). The 5-HT concentrations of the amygdala and raphe nucleus in the olfactory bulbectomy group were significantly decreased when compared with those in the control group (p < 0.05, Fig. 8A). Compared with the olfactory bulbectomy group, the 5-HT concentration of the raphe nucleus in the fluoxetine group was reduced (p < 0.01, Fig. 8C). Compared with the fluoxetine group, neither RoMS nor rotigotine affected the 5-HT concentration of the amygdala or raphe nucleus of fluoxetine-treated rats (Figs. 8B and 8D).
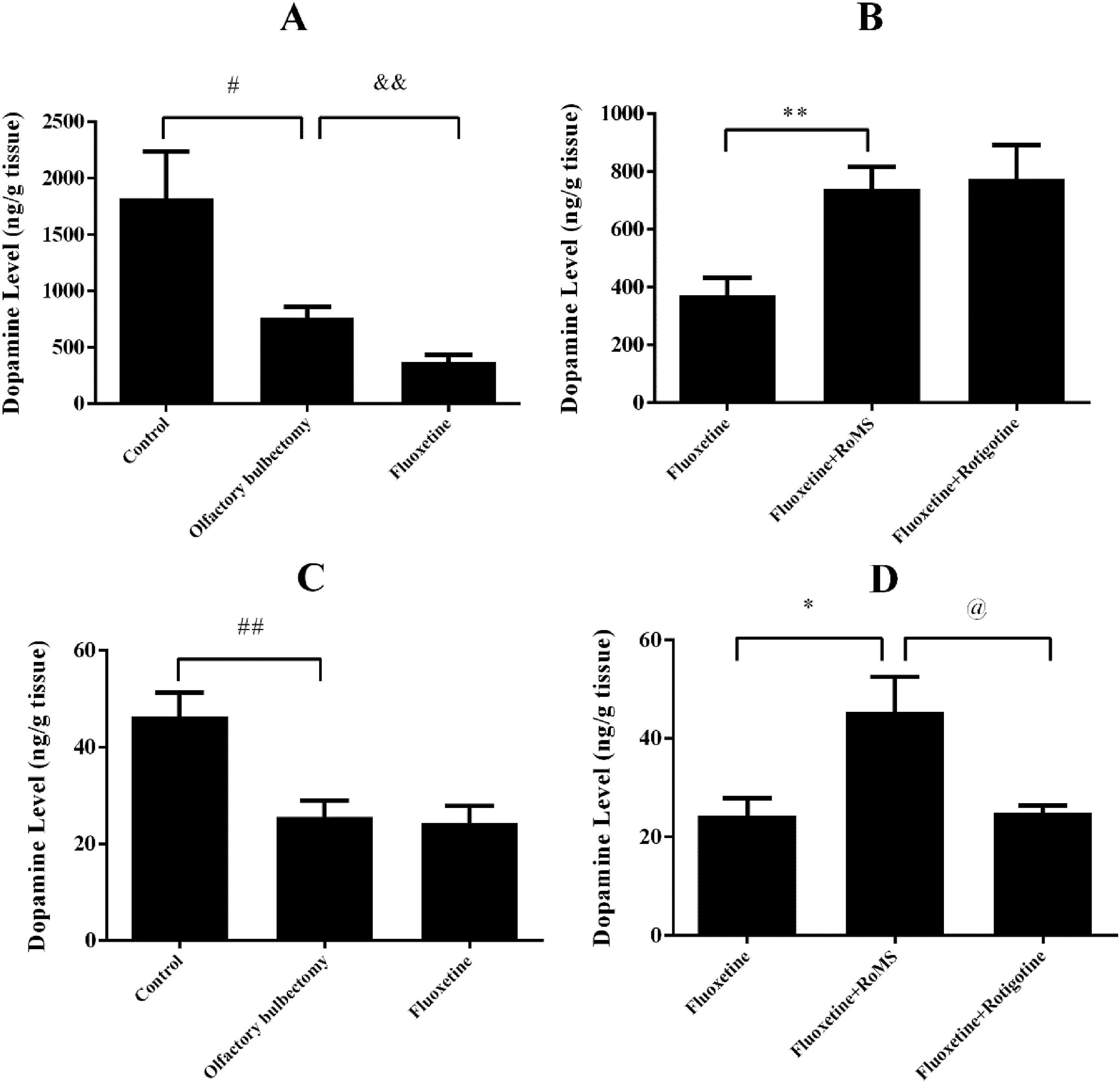
Effects of fluoxetine on
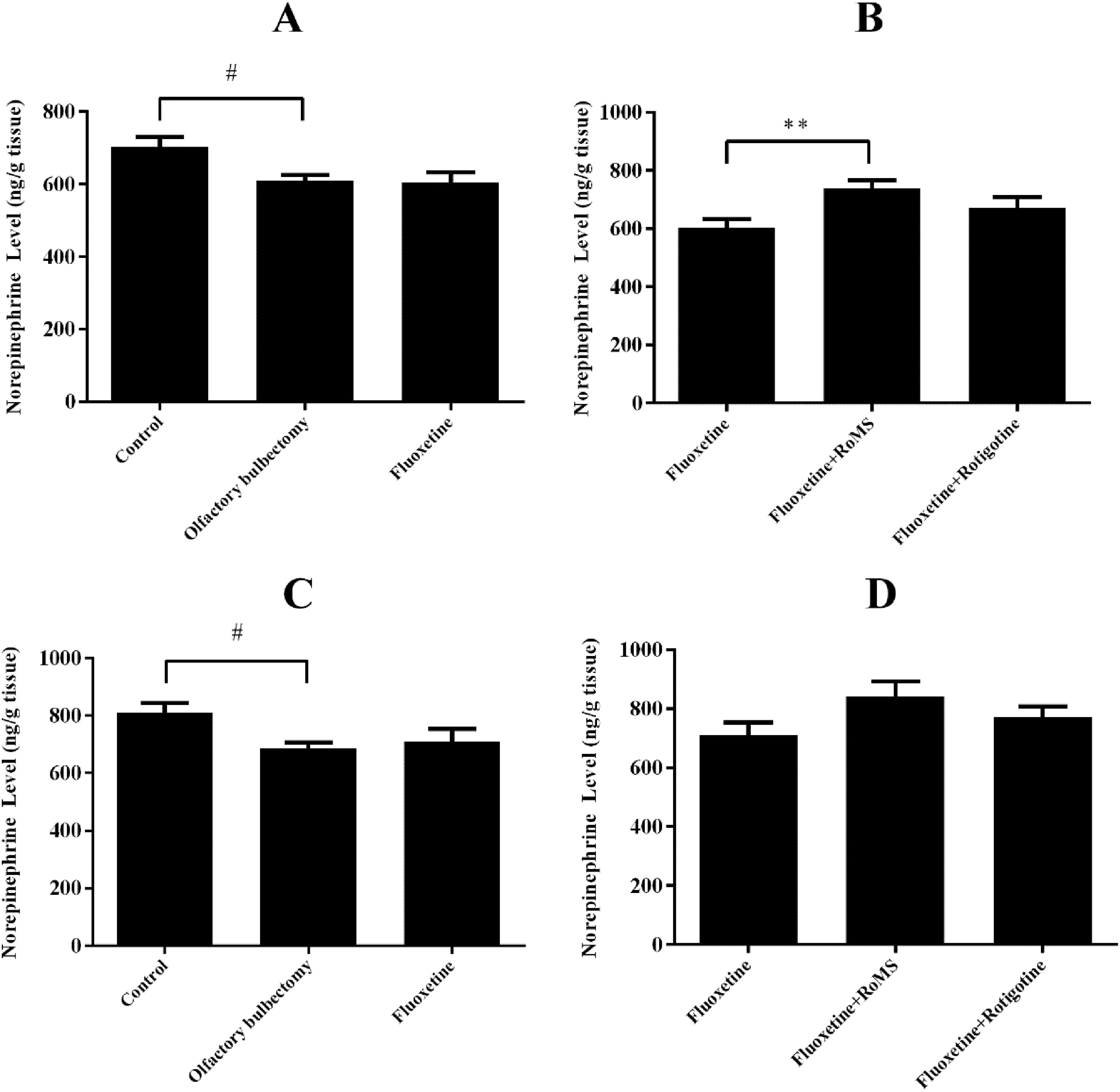
Effects of fluoxetine on
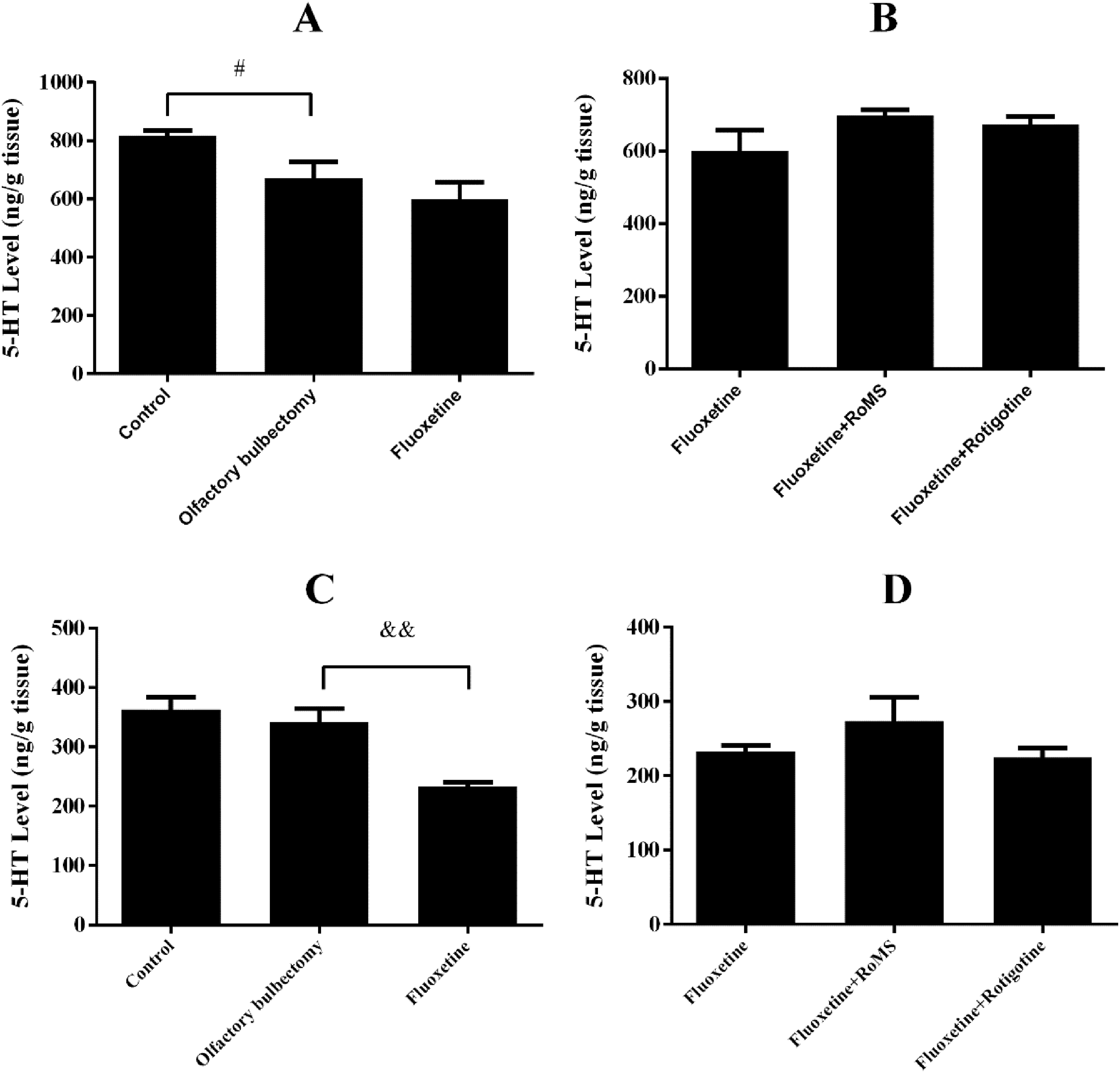
Effects of fluoxetine on
Discussion
Dopamine Agonist Did Not Influence the Antidepressant Effect of Fluoxetine
Bilateral olfactory bulbectomy leads to changes in behavior, neurotransmitter levels, and the endocrine and immune systems. Olfactory bulbectomy-induced symptoms are similar to those of patients with major depression (Oluboka et al., 2018). Olfactory bulbectomy rats show increased exploration in an open field apparatus, which is one of the most widely accepted indices of depressive-like behavior in this model. Hyperactivity in rats is related to the symptoms of depression (Song & Leonard, 2005). The olfactory system is a part of the limbic region, which mediates emotion and behavior. The cortical-hippocampal-amygdala circuit also is affected by olfactory bulbectomy. These neuroanatomical areas are impaired in patients with major depression. Thus, the olfactory bulbectomized animal model is used not only to evaluate antidepressant activity but also to investigate the relationship among systems that are impaired in depression. Numerous studies have demonstrated that chronic antidepressant treatment can reverse most of the behavioral changes observed in the olfactory bulbectomy rat (Külli Jaako-Movits et al., 2006). Fluoxetine is a widely prescribed selective serotonin reuptake inhibitor antidepressant for treatment of patients with depression. The findings of the present study showed that fluoxetine administration reverses the increases in locomotion in olfactory bulbectomy rats, which is consistent with a previous report (Eisenstein et al., 2010; Pilar-Cuellar et al., 2019). In this study, olfactory bulbectomy rats were co-administered fluoxetine and a dopamine receptor agonist. Neither RoMS nor rotigotine altered the effect of fluoxetine on the mean speed and the total distance of mice, indicating that RoMS and rotigotine did not enhance or reduce the antidepressant effect of fluoxetine.
RoMS Ameliorates Sexual Function Deteriorated by Fluoxetine
Fluoxetine frequently causes sexual dysfunction and can affect all phases of sexual function (arousal, desire, and orgasm) (Jing & Straw-Wilson, 2016). The adverse effects of fluoxetine on sexual function usually persist as long as the medication is taken, and fluoxetine-induced impairment of sexual function cannot be resolved unless fluoxetine is discontinued (Reisman, 2017). Furthermore, recent studies have reported that antidepressant-induced sexual dysfunction can continue after selective serotonin reuptake inhibitor treatment cessation (Bala et al., 2018; Ben-Sheetrit et al., 2015). The side effects of fluoxetine on sexual function are a common cause of non-compliance. Paired mating studies in rats showed that fluoxetine inhibits sexual behavior. The aspects of the sexual response cycle can be disrupted by antidepressant use. Previous studies demonstrated that fluoxetine administration led to marked sexual dysfunction (Sukoff Rizzo et al., 2008). Furthermore, fluoxetine treatment produced a dynamic decline in consummatory and appetitive aspects of sexual behavior in rats (Cantor et al., 1999). The present study showed that fluoxetine not only reduced the intromission frequency and ejaculation frequency but also increased the intromission latency and the ejaculation latency. RoMS improved fluoxetine-induced sexual dysfunction. Therefore, it is reasonable to postulate that the likelihood of sexual dysfunction would be lower in PD patients with depression who were co-administered fluoxetine and RoMS.
RoMS Increased the Levels of Testosterone and Luteinizing Hormone
A previous study reported that fluoxetine administration decreased the luteinizing hormone and testosterone levels in intact rats (Ayala et al., 2018). The present study showed that fluoxetine also diminished luteinizing hormone and testosterone levels in bulbectomized male rats. The sexual function of males is dependent on luteinizing hormone and testosterone levels, and luteinizing hormone is essential for sexual development and reproduction in both men and women. Luteinizing hormone stimulates Leydig cells to secrete testosterone. In a rat model, a decrease in luteinizing hormone led to a reduction in serum testosterone and therefore caused sexual dysfunction (Wang et al., 2016). In male rats, testosterone is thought to have major effects on sexual behavior (Hull & Dominguez, 2007). Testosterone relaxes penile arteries and cavernous smooth muscle. In rats, testosterone increased arterial flow, inhibited venous leakage, and augmented the erectile response after stimulation of the cavernous nerve. The present study showed that the luteinizing hormone and testosterone levels in the fluoxetine plus RoMS group were increased compared with those of the fluoxetine group. Therefore, it seems reasonable to conclude that the elevation in testosterone and luteinizing hormone levels following RoMS administration may be responsible for the observed improvement in fluoxetine-induced impairment of sexual function.
RoMS Regulated the Contents of Neurotransmitters in the Brain
Neurotransmitters in the brain, including 5-HT, norepinephrine, and dopamine, have been proposed to be involved in sexual behavior. Moreover, 5-HT and norepinephrine have been implicated in both the mechanism of action of antidepressants and the pathogenesis of major depression (Ye et al., 2012). The serotonergic system (the amygdala and hippocampus) negatively affects sexual motivation, ejaculation, and orgasm. At the central level, 5-HT plays an inhibitory role in erectile function, lubrication, and sexual interest. Neuroanatomical data have revealed high densities of 5-HT2A/C receptors in areas of the raphe nucleus and amygdala, and 5-HT impairs sexual function by stimulating postsynaptic 5-HT2A and 5-HT2C receptors. Norepinephrine increases arousal by binding to receptors of the central nervous system and inhibits erection by binding with α1 receptors of the peripheral nervous system (Just, 2015). Dopamine is the main neurotransmitter in the central nervous system and facilitates sexual motivation, copulation, and genital reflexes. Dopamine in the hypothalamus also plays a role in erectile function by activating oxytocinergic neurons, followed by activation of neuronal nitric oxide synthase. Furthermore, dopaminergic neurons extend from the caudal hypothalamus, innervating the autonomic and somatic nuclei in the lumbosacral spinal cord. Thus, dopamine can participate in the regulation of both the autonomic and somatic components of penile reflexes. The concentrations of 5-HT, norepinephrine, and dopamine in the amygdala and raphe nucleus were evaluated using the LC-MS/MS technique. The results showed that co-administration of RoMS with fluoxetine increased the concentrations of dopamine and norepinephrine. These findings suggest that increases in norepinephrine and dopamine in the amygdala and raphe nucleus may play at least a partial role in the effects of RoMS on improvement of fluoxetine-induced impairment of sexual function. Compared with RoMS, rotigotine did not ameliorate fluoxetine-induced impairment of sexual function, which may be because of the difference in pharmacokinetics between rotigotine and RoMS. RoMS could release rotigotine for 14 days after a single administration to continuously stimulate dopamine receptors (Lv et al., 2019).
Conclusion
In conclusion, the present data indicate that RoMS improve fluoxetine-induced impairment of sexual function and do not affect the antidepressant efficacy of fluoxetine. The mechanisms may be related to increases in the concentrations of dopamine and norepinephrine in the amygdala and raphe nucleus and the elevated luteinizing hormone and testosterone content in the blood after RoMS administration.
Summary
Fluoxetine deteriorates sexual dysfunction. Rotigotine-loaded microspheres improves fluoxetine-deteriorated sexual function. Rotigotine-loaded microspheres does not affect the antidepressant efficacy of fluoxetine.
Footnotes
Acknowledgment
Author Contributions
Q. W. conducted experiments and performed data analysis. C. Z. performed data analysis and drafted the manuscript. Y. F., S. Y., and Y. Y. conducted a part of experiments. R. L. and L. Z. performed the assay of neurotransmitters. T. W. drafted the manuscript. F. F. participated in research design and revised the manuscript. Q. W. and C. Z. contributed equally to this work.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
This work was supported by the Taishan Scholar Project of Shandong Province. The opinions, results, and conclusions are those of the authors and no endorsement by any institute is intended or should be inferred.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the Taishan Scholar Project of Shandong Province
