Abstract
Patients with advanced stage or recurrent cervical cancer represent a population with limited chemotherapeutic options. More specifically, patients with recurrent disease have a poor salvage rate, with a 5-year survival rate of less than 10%. This year, the first prospective phase III clinical trial exploring the anti-angiogenic agent, bevacizumab, was published, meeting its primary endpoint, with a significant improvement in overall survival. As such, a review of anti-angiogenic therapy in the treatment of this disease is warranted.
Introduction
In 2011 an estimated 529,800 cases of cervical cancer were diagnosed worldwide, with 275,100 deaths [Jemal et al. 2011]. Regionally, in the United States, an estimated 12,360 cases will be diagnosed in 2014, with 4020 deaths [Siegel et al. 2014]. In the European Union, the crude incidence of cervical cancer is 13.2/100,000, and the crude mortality is 5.9/100,000 women/year [Lynge et al. 2009]. This discrepancy between global and regional disease burden is attributable to the disproportionately high burden of cervical cancer in developing, resource-poor countries lacking adequate healthcare infrastructure and screening programs. Nonetheless, despite advances in screening, vaccination and treatment of early stage disease, a proportion of patients will be diagnosed with advanced stage (stage IVB), recurrent or persistent cervical cancer.
Chemotherapeutic options for patients with advanced stage or recurrent disease have been explored and are based on phase II and III clinical trials completed under the auspices of cooperative groups, most notably the Gynecologic Oncology Group (GOG). In this setting, goals of care are centered on disease control and palliation of symptoms, as cure is exceedingly rare [Greer et al. 2010]. Since Dr Thigpen’s initial paper in 1981, a number of chemotherapeutic agents, both single drug and combination regimens, have been studied in the treatment of advanced and metastatic cervical cancer with limited gains in overall survival (OS) [Thigpen et al. 1981, 1995; McGuire et al. 1989, 1996; Sutton et al. 1989; Look et al. 1998; Bookman et al. 2000; Schilder et al. 2000; Curtin et al. 2001; Fracasso et al. 2003; Muggia et al. 2005; Garcia et al. 2007; Omura et al. 1997; Bloss et al. 2002; Moore et al. 2004; Long et al. 2005; Monk et al. 2009b]. Importantly, cisplatin + paclitaxel has been established as the backbone for future trials, although OS approaches only 13 months in highly selected populations [Thigpen et al. 1981].
The poor oncologic outcome in this patient population represents and unmet clinical need, and catalyzed the exploration of novel treatment paradigms. In an era of molecular medicine, the development of biologic therapies, to be used solely or in conjunction with cytotoxic chemotherapy, is implicit. Following publication of the results of GOG 240, a renewed interest in utilization of anti-angiogenic therapies for the treatment of cervical cancer has emerged. This review article discusses the concept of angiogenesis within the tumor microenvironment, describes the biologic rational of anti-angiogenic therapy in cervical cancer and subsequently details clinical trials investigating various anti-angiogenic agents in the treatment of this disease.
Angiogenesis
Targeting the cancer microenvironment, specifically neovascularization, via vascular endothelial growth factor (VEGF) pathway inhibition, evolved as our understanding of tumor biology was refined over the past three decades. Following several, novel, in vitro and in vivo studies, it became evident that angiogenesis was essential for tumor invasion and metastasis, and was required for tumor growth beyond 1–2 mm3 [Folkman, 1971; Eskander et al. 2011]. This process requires the recruitment of vasculature, circulating endothelial cells and pro-angiogenic mediators (Yancopoulos et al. 2000).
All members of the VEGF family of ligands stimulate cellular responses by binding to tyrosine kinase receptors on the cell surface causing dimerization and activation through trans-phosphorylation. The three main subtypes of the VEGF receptors (VEGFRs) are numbered VEGFR-1, VEGFR-2 and VEGFR-3. Typically membrane-bound, the VEGFRs have an extracellular portion consisting of seven immunoglobulin-like domains, a single transmembrane spanning region and an intracellular portion containing the split tyrosine kinase domain. Through alternative splicing, cytoplasmic VEGFRs can also exist.
In 1993, following several years of collaborative laboratory efforts between the University of California San Francisco and Genentech, Dr Ferrara’s laboratory reported that anti-VEGF monoclonal antibodies exerted a potent inhibitory effect on the growth of three tumor cell lines injected subcutaneously into nude mice[Kim et al. 1993]. Interestingly, the antibody had no effects on the cell lines in vitro. Several parallel studies confirmed in vivo growth inhibition, which correlated with decrease tumor microvessel density and inhibition of tumor angiogenesis[Kim et al. 1993; Warren et al. 1995; Borgstrom et al. 1996, 1998, 1999]. Ultimately, bevacizumab, a humanized monoclonal antibody directed against VEGF, was synthesized and used in early proof of concept studies. Bevacizumab neutralizes VEGF-A and blocks its signal transduction through both VEGFR-1 and VEGFR-2, as demonstrated by the inhibition of VEGF-induced cell proliferation, survival, permeability, nitric oxide production, migration and tissue factor production.
The first phase I clinical trial assessing the safety, pharmacokinetics and tolerability of bevacizumab was conducted in 1997 [Margolin et al. 2001]. In the United States, bevacizumab gained Food and Drug Administration (FDA) approval in February 2004, following a randomized double-blind phase III clinical trial assessing the impact of addition of bevacizumab to irinotecan, 5-fluorouracil and leucovorin (IFL) in the upfront treatment of patients with unresectable metastatic colorectal cancer (OS survival advantage) [Hurwitz et al. 2004]. Additional phase III trials were conducted in metastatic nonsmall cell lung cancer (OS advantage) [Sandler et al. 2006], metastatic breast cancer (mBC) [Miller et al. 2007], renal cell carcinoma (progression-free survival advantage), and recurrent glioblastoma multiforme (progression-free survival advantage), all of which met their primary endpoints, thus supporting FDA approval of bevacizumab for these indications [Escudier et al. 2007]. Importantly, in November 2011, FDA commissioner Margaret Hamburg revoked accelerated approval of bevacizumab in HER2-negative mBC, given lack of an OS advantage and a lack of improvement in quality of life.
Angiogenesis and cervical cancer: the biologic rationale
The limited success achieved with traditional cytotoxic chemotherapy in patients with recurrent and metastatic cervical cancer is multifactorial. Patients with cervical cancer represent a unique population, as radiation and chemotherapy exposure for primary therapy are hypothesized to alter the disease biology. Upfront chemosensitizing radiation therapy may select for radio-resistant and/or chemotherapy-resistant cell populations, particularly if there is crossover with respect to mechanisms of drug resistance. Additionally, these patients commonly suffer from obstructive uropathy and acute kidney injury, limiting clearance of cytotoxic compounds from the systemic circulation. Lastly, cancer foci recurring in the previously irradiated field may have compromised blood supply and relative hypoxia, limiting delivery of cytotoxic drugs. These unique characteristics may explain the limited response to retreatment with traditional chemotherapy and highlight the importance of studying novel biologic strategies.
Biologically, tumor neovascularization imparts an aggressive course in cervical cancer, where aberrant and abnormal vascularity identified on colposcopic examination may indicate invasive disease. Mechanistically, this is explained by the effects of E6/E7 on downstream angiogenic pathways. Upregulation of the E6 oncoprotein is hypothesized to directly stimulate VEGF production [Lopez-Ocejo et al. 2000; Toussaint-Smith et al. 2004]. In elegant transgenic mice experiments, Coussens and colleagues were able to reproduce progressive invasive squamous cell carcinoma of the epidermis with HPV 16, E6 and E7 oncogene expression [Coussens et al. 1996]. Additionally, angiogenic proliferation along the basement membrane of premalignant cervical lesions, infected with high risk human papilloma virus (HPV) subtypes, was demonstrated in archival tissue specimens, further validating activation of the angiogenic switch as mediated by HPV infection [Smith-Mccune and Weidner, 1994]. Ultimately, E6 mediated degradation of p53 and E7 inactivation of pRb result in increased VEGF and hypoxia inducible factor 1α (HIF1α), promoting angiogenesis and tumor growth (Figure 1).

Biologic rational of anti-angiogenic therapy in the treatment of cervical cancer.
Clinical evidence that angiogenesis plays an important role in locally advanced cervical cancer has accumulated over the past decade. Specifically, overexpression of VEGF has been associated with adverse oncologic outcomes in numerous solid tumors, including cervical cancer [Kudelka et al. 1997, 1998; Cooper et al. 1998; Ferrara et al. 2004; Ferrara, 2005; Ferrara and Kerbel, 2005]. In an early study, Cooper and colleagues assessed tumor angiogenesis in 111 archived tumor specimens by measuring intratumor microvessel density (IMD) [Cooper et al. 1998]. High IMD was associated with a poor prognosis and remained a significant prognostic factor within a Cox multivariate analysis. More recently, intratumoral VEGF was shown to be upregulated in cervical cancer specimens relative to control cervical tissues, with higher VEGF levels being associated with advanced stage, increase risk of nodal metastasis, and worse progression-free survival (PFS) and OS [Guidi et al. 1995; Cheng et al. 2000; Loncaster et al. 2000; Lee et al. 2005]. Additionally, cluster of differentiation 31 (CD31) expression, found on endothelial cell surfaces, and used as an immunohistochemical marker of angiogenesis, has been shown to be significantly associated with tumor size and the presence of lymph vascular space involvement in patients with clinical stage 1B squamous cell cervical cancer [Silva-Filho et al. 2006]. In a post-trial ad hoc analysis of GOG protocol 109, a total of 173 tumor tissue specimens were assessed for expression of markers of tumor angiogenesis including VEGF, thrombospondin-1 (TSP-1, anti-angiogenesis factor), CD31 and CD105 (tumor-specific endothelial marker) [Randall et al. 2009]. After adjusting for prognostic clinical covariates, high CD31 microvessel density was an independent prognostic factor for PFS [hazard ratio (HR) = 0.36; 95% confidence interval (CI): 0.17–0.75; p = 0.006) and OS (HR = 0.36; 95% CI: 0.17–0.79; p = 0.010).
To date, several parallel strategies targeting angiogenesis have been explored, with VEGF dependent and non-VEGF dependent downstream targets (Monk et al. 2013).
Bevacizumab and cervical cancer
Anti-angiogenic therapy in cervical cancer has shown promising results compared with historical cohorts. In the first case series describing the use of bevacizumab in patients with recurrent cervical cancer, despite heavy pretreatment (the patients had a median of 3 prior regimens), there was a 67% overall response rate [Wright et al. 2006]. Treatment was well tolerated, with only one grade 4 adverse event (AE) noted (table 1).
Bevacizumab studies in cervical cancer.

AEs = adverse events; DFS = disease-free survival; GI = gastrointestinal; GOG = Gynecologic Oncology Group; HTN = hypertension; n = number of subjects; NR = not reported; OS = overall survival; PFS = progression-free survival; PS = performance status; Q = every; RR = response rate; SAE, serious adverse effect.
These preliminary results catalyzed the synthesis and opening of GOG protocol 227C, a phase II trial designed to evaluate the efficacy and tolerability of bevacizumab in the treatment of recurrent cervical cancer [Monk et al. 2009a] (Table 1). Amongst the 46 eligible and evaluable patients, 38 (82.6%) received prior pelvic radiation as well as either one (n = 34; 74%) or two (n = 12; 26%) cytotoxic regimens for recurrent disease. A total of 11 patients (23.9%; 2-sided 90% CI: 14–37%) survived progression free for at least 6 months, and five patients (10.9%; 2-sided 90% CI, 4–22%) had partial responses, with a median response duration of 6.2 months (range: 2.83–8.28 months). The median PFS and OS were 3.40 months (95% CI: 2.53–4.53 months) and 7.29 months (95% CI, 6.11–10.41 months), respectively. These results compared favorably with historical phase II GOG trials in this setting [Tewari and Monk, 2005].
Given the clinical activity noted in the pretreated population, Radiation Therapy Oncology Group (RTOG) protocol 0417 was developed, exploring the safety and efficacy of the addition of bevacizumab to standard chemoradiation (CRT) [Schefter et al. 2012] (Table 1). Between 2006 and 2009 a total of 60 patients were enrolled. The median follow up was 12.4 months (range: 4.6–31.4 months). Most patients had (International Federation of Gynecology and Obstetrics (FIGO) stage 2B (63%) disease and with a Zubrod performance status (PS) of 0 (67%). A total of 80% of cases were squamous. There were no treatment-related serious AEs. More recently, oncologic outcomes were published, with 81% 3-year OS and a 23% locoregional failure rate [Schefter et al. 2014].
Another phase II clinical trial exploring the combination of cisplatin 50 mg/m2 day 1 + topotecan 0.75 mg/m2 days 1, 2, 3 + bevacizumab 15 mg/kg day 1 on a 21 day cycle was recently published [Zighelboim et al. 2013]. A total of 27 patients with persistent or recurrent cervical cancer, with no prior chemotherapy for recurrence, were enrolled. The 6-month PFS was 59% (80% CI: 46–70%), with median PFS and OS of 7.1 months and 13.2 months respectively. Unfortunately, grade 3–4 hematologic toxicity was common (thrombocytopenia 82%, leukopenia 74%, anemia 63%, neutropenia 56%) on this treatment regimen. The majority of patients (78%) required unanticipated hospital admissions for supportive care and/or management of toxicities.
Prospective phase III clinical trial incorporating bevacizumab in the treatment of cervical cancer: GOG 240
Following the results of GOG 227C (described earlier), advancement of bevacizumab into the phase III arena was deemed a scientific priority. Ultimately, GOG 240, a four-arm prospective randomized trial exploring platinum and nonplatinum doublets with and without the anti-angiogenic agent bevacizumab was designed, meeting its accrual goal in less than 3 years (Figure 2) [Tewari et al. 2014].

Gynecologic Oncology Group protocol 240 schema.
From April 2009 to January 2012, the trial accrued 452 patients. Over 220 patients were treated with each of the chemotherapy backbones and patients were well matched for histology (p = 0.308), ethnicity (p = 0.800), as well as disease status: recurrent versus persistent versus advanced (p = 0.298). Notably, the majority of patients on each chemotherapy backbone had a GOG PS of 0 (PS 0–1 required for enrollment). As anticipated, 75% of the entire study group had previously received platinum and this was evenly distributed between the 2 backbones (p = 0.666). The topotecan + paclitaxel arm was shown to not be superior or inferior to the cisplatin + paclitaxel arm (HR 1.20; 95% CI: 0.82–1.76). Median OS in the topotecan containing doublet was 12.5 months versus 15 months in the cisplatin + paclitaxel arm. These results were interpreted as indicating that the nonplatinum chemotherapy doublet was not superior to cisplatin-paclitaxel for efficacy.
Importantly, the investigators showed a significant improvement in OS in the bevacizumab containing arms relative to nonbevacizumab controls (17 months versus 13.3 months respectively; HR = 0.71; 95% CI: 0.54–0.95; p = 0.0035) (Figure 3). Analogous improvements in PFS were identified (8.2 months bevacizumab containing arm and 5.9 months in control arm) (HR = 0.67; 95% CI: 0.54–0.82; p = 0.0002). Exploratory sub-analysis further indicated the beneficial effects of bevacizumab in patients with prior platinum exposure, recurrent or persistent disease and squamous histology. Importantly, the benefits of bevacizumab persisted in patients with recurrent disease in a previously irradiated field, which was hypothesized to be relatively hypoxic. These findings represent the first time a targeted anti-angiogenic agent has shown an improvement in OS in patients with gynecologic cancer.

Overall survival (3A) and progression-free survival (3B) in chemotherapy alone versus chemotherapy + bevacizumab arms on Gynecologic Oncology Group 240 [reproduced with permission from Tewari et al. 2014].
As with all novel agents, therapeutic benefits must be weighed against potential toxicity and impact on quality of life. Within the bevacizumab-containing arms, there was an increase in grade ≥3 GI and genito-urinary (GU )fistula (n = 5), as well as grade ≥2 hypertension, grade ≥4 neutropenia and grade ≥3 thrombocytopenia. This did not translate into a significant deterioration in health-related quality of life (QoL). The full QOL data have yet to be published and the effects of bevacizumab on symptom palliation are yet to be determined. Additionally, the impact of bevacizumab on GI and GU fistula formation is being investigated in an ancillary data study in an effort to identify cervical cancer patients at risk for this life altering complication.
The significant improvement in OS identified in GOG protocol 240 is linked to the limited postprogression survival in this patient population due to lack of effective salvage strategies. As explained by Broglio and colleagues, a significant PFS advantage (HR = 0.73, p = 0.03) translates into a significant OS advantage (HR = 0.61, p = 0.008) when median survival postprogression on study is estimated to be 6 months [Broglio and Berry, 2009]. Conversely, in the setting where alternate treatment options exist, the postprogression survival is extended and the survival advantage is diluted. With an analogous calculated PFS, in a simulated study, the HR for OS would rise to 1.29 (p = 0.262) if postprogression survival was estimated to be 18 months.
As detailed above, the burden of cervical cancer is greatest in impoverished, resource-poor countries lacking effective screening modalities. The cost implications and feasibility of incorporating anti-angiogenic agents into the treatment algorithm of advanced cervical cancer on a global level are understood. Traditionally, cost-effectiveness studies for novel agents do not perform in favor of the drug primarily due to drug costs and expenditures associated with marketing, which partially offset the extensive costs encountered during the drug development and clinical trial phases. Unless the agent can effectively reduce treatment-related toxicities and prolong survival at a reasonable cost, the new drug will likely be cost-ineffective. However, with time the costs of new therapies are expected to decrease, resulting in improvement in the cost-effectiveness ratio. During the early days of highly active antiretroviral therapy for acquired immunodeficiency syndrome (AIDS), drug costs appeared prohibitive, but currently protease inhibitors and zidovudine (AZT) are widely distributed in resource poor, impoverished countries in Africa [Montaner et al. 2006].
Multitargeted VEGFR tyrosine kinase inhibitors (TKIs)
Based on the promising results identified with use of bevacizumab, exploration of alternate, novel anti-angiogenic agents, targeting parallel pathways commenced. Preclinical models illustrated that HPV-associated cervical cancer-derived cell lines co-expressed the receptor tyrosine kinase (RTK) cKit, implicating cKit in cervical carcinogenesis [Caceres-Cortes et al. 2001].
Additionally, fibroblast growth factor (FGF) and platelet-derived growth factor (PDGF) have been identified as targets in the angiogenic cascade. PDGF binding to the PDGF receptor β (PDGFR-β) is essential for pericyte recruitment and blood vessel maturation[Jain and Booth, 2003]. The FGF family of ligands activates angiogenesis via interaction with FGF receptors 1 and 2 [Rusnati and Presta, 2007]. Interestingly, it is thought that signaling via these alternate pathways (PDGF, FGF) may mediate resistance to VEGF inhibition, supporting a multi-targeted approach[Benjamin et al. 1998, Erber et al. 2004, Casanovas et al. 2005, Batchelor et al. 2007, Lu et al. 2008]. In response to receptor-ligand binding, downstream signaling pathways, PI3K-Akt-mTOR and Ras-MEK-Erk are activated and have been identified as potential targets for drug development [Ferrara et al. 2003; Ferrara and Kerbel, 2005].
To date, the largest study exploring nonbevacizumab anti-angiogenic agents in the treatment of cervical cancer was reported in August 2010. Monk and colleagues studied pazopanib and lapatinib as single agents and in combination in patients with stage 4B persistent/recurrent cervical carcinoma not amenable to curative therapy and at least one prior regimen in the metastatic setting [Monk et al. 2010] (Table 2). The primary endpoint was PFS, and secondary endpoints were overall OS, response rate (RR) and safety.
Nonbevacizumab anti-angiogenic trials in cervical cancer.
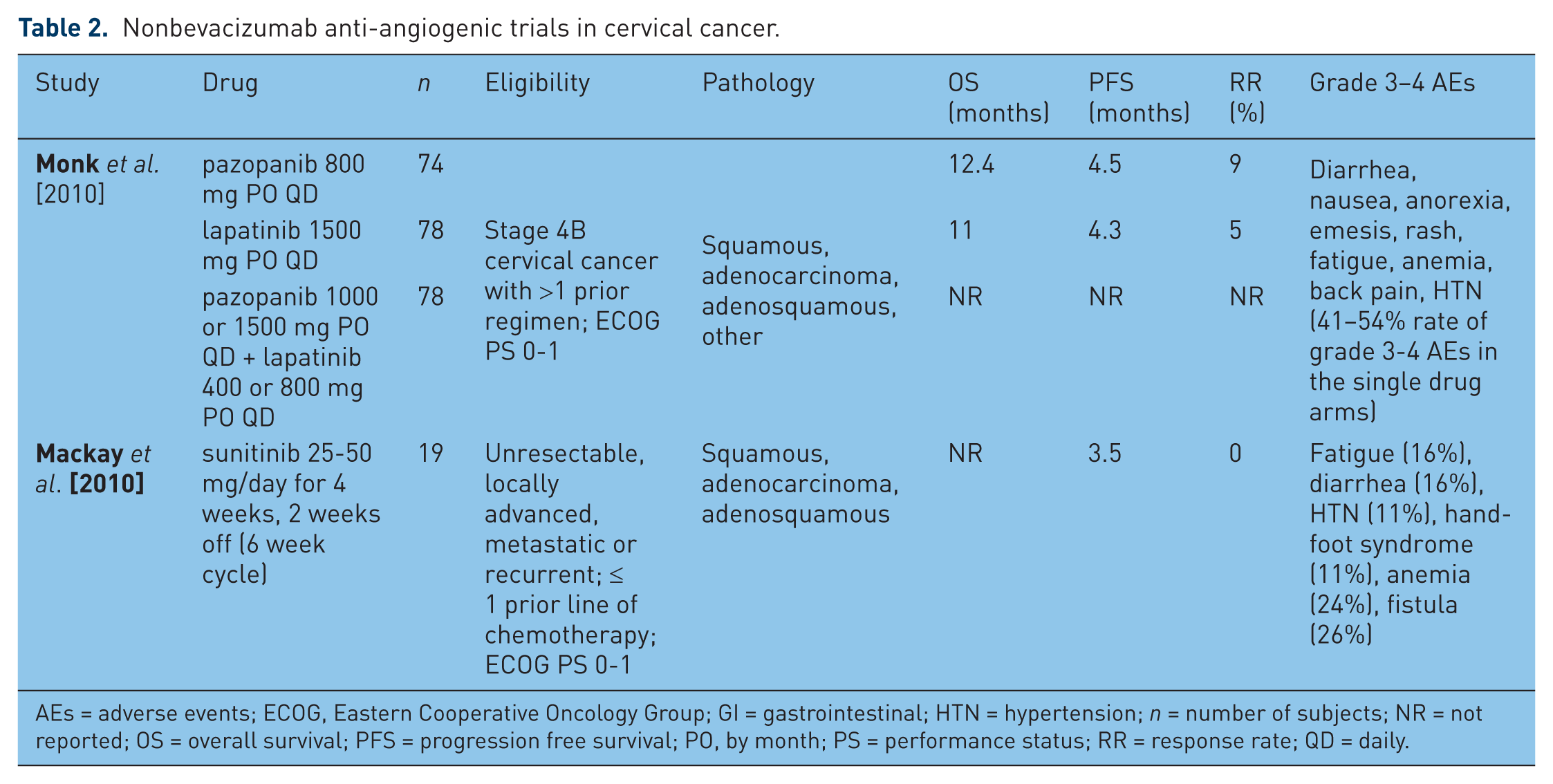
AEs = adverse events; ECOG, Eastern Cooperative Oncology Group; GI = gastrointestinal; HTN = hypertension; n = number of subjects; NR = not reported; OS = overall survival; PFS = progression free survival; PO, by month; PS = performance status; RR = response rate; QD = daily.
Use of this combination regimen was based on preliminary data suggesting at least additive effects with combination of pazopanib and lapatinib in the treatment of solid cancers [Reardon et al. 2013]. Pazopanib is a potent, selective, oral multi targeted RTK inhibitor that targets VEGFR, PDGF receptor (PDGFR) and c-Kit [Monk et al. 2010]. Prior studies confirmed its tolerability in the treatment of solid malignancies, and it is currently FDA approved for use in metastatic soft tissue sarcomas and metastatic renal cell carcinoma [Sloan and Scheinfeld, 2008, Hurwitz et al. 2009]. Conversely, lapatinib is an oral, small-molecule, dual TKI of epidermal growth factor receptor (EGFR) and Her2/neu and is approved by the FDA and the European Medicines Agency (EMA) for use in combination with capecitabine for the treatment of patients with Her2/neu-overexpressing mBC who have received prior therapy including an anthracycline, a taxane, and trastuzumab [Ryan et al. 2008].
Of 230 patients enrolled, 152 were randomly assigned to the monotherapy arms: pazopanib (n = 74) or lapatinib (n = 78). Importantly, the futility boundary was crossed at the planned interim analysis for combination therapy compared with lapatinib therapy and the combination arm was terminated. Most patients (62%) had recurrent cancer. Patients were randomly assigned to pazopanib daily, lapatinib daily, or lapatinib plus pazopanib combination therapy until progression or withdrawal because of AEs. Pazopanib improved PFS (HR = 0.66; 90% CI: 0.48–0.91; p = 0.013) and OS (HR = 0.67; 90% CI: 0.46–0.99; p = 0.045). Median OS was 50.7 weeks and 39.1 weeks, and RRs were 9% and 5% for pazopanib and lapatinib, respectively. The only grade 3 AE >10% was diarrhea (11% pazopanib and 13% lapatinib). Grade 4 AEs were 9% (lapatinib) and 12% (pazopanib). The results of this phase II study confirmed the activity of anti-angiogenic agents in advanced and recurrent cervical cancer, and demonstrated the benefit of pazopanib based on the prolonged PFS and favorable toxicity profile.
Sunitinib, an analogous, oral multi-TKI, exerts its anti-angiogenic effects via inhibition of VEGFR-1, -2 and -3, PDGF α and β, and related RTKs [Chow and Eckhardt, 2007]. Currently, sunitinib is FDA approved for use in patients with metastatic renal cell carcinoma and gastrointestinal stromal tumors. Given the central role RTKs play in tumor cell proliferation and angiogenesis, a phase II clinical trial was developed investigating the efficacy and safety of sunitinib in patients with unresectable, locally advanced or metastatic cervical carcinoma [Mackay et al. 2010] (Table 2). A total of 19 subjects were enrolled on this multicenter phase II study. Unfortunately, there were no documented objective responses on therapy, but morbidity was significant (fistula rate of 26%). Median time to progression was reported as 3.5 months. Given lack of signal, it was determined that sunitinib has insufficient activity as a single agent in cervical cancer to warrant further investigation.
Anti-vascular strategies in the treatment of cervical cancer
Interest into the study of vascular disrupting agents (VDAs) emerged in an effort to circumvent acquired resistance to traditional anti-angiogenic therapies. VDAs result in a rapid and selective shutdown of tumor vasculature via destruction of endothelial cells [Chaplin et al. 1996]. In an analogous, but unique manner to the TKIs described above, these agents interrupt tumor blood flow, depriving the tumor of necessary nutrients and oxygen [Siemann et al. 2004, Tozer et al. 2005]. In addition, VDAs have the added ability to target established blood vessels and are not limited to inhibition of new vessel formation, targeting genetically stable cell populations and potentially decreasing the chances of acquired drug resistance [Lippert, 2007]. One of the best-studied agents within this class is combretastatin A-4 phosphate (CA4P), a synthetic, phosphorylated prodrug of the natural product combretastatin A-4 (CA4) [Bilenker et al. 2005]. This drug functions by binding β-tubulin subunits, preventing microtubule formation resulting in cytoskeletal changes within endothelial cells [Salmon and Siemann, 2006]. The anti-vascular effects of CA4P have been demonstrated in both in vitro and in vivo models, and appear to be the result of endothelial damage, leading to increased vascular resistance, reduced tumor blood flow and central tumor necrosis [Bilenker et al. 2005; Salmon and Siemann, 2006]. Furthermore, in mouse models, CA4P has been shown to act synergistically with 5-fluorouracil, cisplatin and carboplatin [El-Zayat et al. 1993; Bilenker et al. 2005].
The most extensively studied VDA in the treatment of cervical cancer is the investigational anticancer drug 5,6-dimethylxanthenone-4-acetic acid (DMXAA) [Zhou et al. 2002]. This drug was developed by the Auckland Cancer Society Research Centre (ACSRC) and has recently completed phase I studies in New Zealand and the UK under the direction of the Cancer Research Campaign’s Phase I/II Clinical Trials Committee. The effects of DMXAA include induction of cytokines, tumor necrosis factor (TNF-α), serotonin and nitric oxide (NO). In a phase I trial exploring DMXAA in the treatment of several solid tumors, DMXAA (22 mg/kg by intravenous infusion over 20 min) resulted in a partial response in 1 patient with metastatic cervical squamous carcinoma. Given the clinical and preclinical data, 6 separate VDAs have been synthesized and are in various stages of phase I and II clinical trials exploring their efficacy in patients with solid tumors [Lippert, 2007]. As with other novel agents, a unique AE profile exists amongst VDA and includes cardiovascular disease and tumor pain [Cai et al. 2011].
Conclusion
Publication of GOG protocol 240, which detailed an OS advantage with the addition of bevacizumab to cytotoxic chemotherapy, is practice changing and represents the first and only study within the gynecologic cancer arena exhibiting an OS advantage with addition of a targeted anti-angiogenic agent. The significance of this 3.7 month improvement in OS is most clear when placed in context of prior clinical trials in this setting. Unlike patients with advanced stage ovarian or mBC, where salvage therapy commonly translates into partial or complete response, patients with metastatic or recurrent cervical cancer have failed to show any meaningful response to multimodal therapy in prior studies. With these results, and an evolution in the molecular therapy of this disease, it is anticipated that patients with previous poor prognosis cervical cancer may achieve durable and meaningful remission improving quality of life.
As our understanding of the tumor microenvironment evolves and the contribution of the angiogenic switch is further delineated, novel therapeutic paradigms are likely to emerge. More recently, immune modulation has gained interest in the treatment of cervical cancer and combined therapy targeting tumor vasculature, while enhancing the body’s innate response to this immunogenic malignancy may translate into improved survival outcomes. It is a scientific priority to continue to develop phase II/III clinical trials in an effort to provide this vulnerable population with effective therapeutic options.
Footnotes
Funding
The research was supported by a National Cancer Institute T32 Training Grant awarded to the Division of Gynecologic Oncology at the University of California, Irvine.
Conflict of interest statement
K.S.T discloses that he has served as a consultant for Genentech/Roche and his institution has been awarded a research grant from Genentech for contracted research.
