Abstract
Multi-system comorbidities are common in patients with multiple sclerosis (PwMS) and significantly influence the disease’s presentation and progression. A comorbidity is defined as an illness other than the specific disease of interest (in this case, MS). Generally, chronic or recurrent conditions are included, while transient conditions such as infection or concussion are excluded. Certain modifiable metabolic diseases in PwMS, such as hypertension, diabetes, dyslipidemia, and modifiable health factors such as smoking, alcohol, and obesity, are also considered part of MS comorbidity in this review, since these are risk factors not only for poor outcomes in MS but also for other vascular comorbidities in PwMS. Cohort studies and clinical trials have reported that comorbidity could have multiple adverse effects on MS. The purpose of this review is to summarize studies investigating modifiable risk factors of comorbidity of MS, as well as multiple body system comorbidities in MS, focusing on the influence these comorbidities have on MS outcomes. We aim to emphasize that the management of MS involves not only disease-modifying therapy, but also requires controlling and preventing modifiable risk factors for comorbidities and appropriate treatment of comorbidities, as these interventions may be equally crucial in improving the prognosis of MS.
Introduction
Multiple sclerosis (MS) is an immune-mediated, disabling disease of the central nervous system with highly heterogeneous outcomes. It is characterized by intermittent, recurrent, and focal episodes of inflammatory demyelination and neurodegeneration, and it is the major cause of nontraumatic neurologic disability in young adults.1,2 There is increasing interest in the comorbidities of MS as more evidence has emerged that comorbidities across multiple body systems are not uncommon in patients with MS (PwMS). 3 However, most of the evidence regarding comorbidities in MS has been obtained from studies in Europe and North America, including population-based studies 4 from Canada, the USA, the UK, Italy, and Sweden; notably, no studies from Africa and very few from Asia were published.
Methodological differences such as different definitions of comorbidities, statistical measures, study group size, and time scales between studies, give rise to heterogeneous findings between published studies. However, according to most large cohort studies or clinical trials, comorbidities are consistently associated with worse MS outcomes and may be partly responsible for the heterogeneity of clinical outcomes in MS. 5 At the level of the individual, comorbidity adversely affects outcomes throughout the disease course in MS, including diagnostic delays from symptom onset, 6 disability at diagnosis, 6 disease activity,7,8 subsequent disease progression, 9 disease-modifying treatment (DMT) choice,10,11 health-related quality of life 12 and even mortality. 13 At the societal level, comorbidity is associated with increased healthcare utilization, work impairment, and costs. However, through what mechanisms these comorbidities affect the outcomes of MS remain unsolved mysteries.
In addition, certain potentially modifiable metabolic comorbidities in MS, such as hypertension, diabetes, dyslipidemia, and modifiable health factors such as smoking, alcohol, and obesity, are risk factors not only for poor outcomes in MS but also for other vascular comorbidities in PwMS. 14 Although health behaviors, 15 such as smoking and alcohol intake, are not included in the classic definitions of comorbidity, these modifiable conditions affect the risks of vascular comorbidities and MS outcomes. Therefore, we considered health behaviors as a part of MS comorbidity in our review. Prevention and modification of these modifiable risk factors provide opportunities to reduce the overall comorbidity burden and improve MS prognosis. Timely identification of these risk factors is paramount to effectively treating MS in clinical practice.
In this review, we summarize studies investigating modifiable risk factors of comorbidity of MS, as well as multiple body system comorbidities in MS, focusing on the influence these comorbidities have on MS outcomes. We aim to emphasize that the management of MS involves not only DMT, but also requires controlling and preventing modifiable risk factors for comorbidities and appropriate treatment of comorbidities, as these interventions may be equally crucial in improving the prognosis of MS.
Methods
A comprehensive literature search was conducted across the PubMed database when preparing for this narrative review to identify relevant studies on MS and its comorbidities/modifiable risk factors. All the related literature published from January 2005 up to March 2025 was reviewed. Furthermore, we manually checked the references of relevant papers and reviews to find any other pertinent articles. We categorized and summarized the findings from all relevant literature and presented the summarized results in spreadsheets.
Definition of comorbidity in MS
Comorbidity is defined as the total burden of illness other than the specific disease of interest (in this case, MS). To focus the number of conditions examined, we concentrated our definition of comorbidity on chronic or recurrent conditions, rather than transient conditions such as infection. 16 Complications that arise from MS, such as neurogenic bladder, are also excluded because the mechanisms by which they originate relate to the disease of interest. Health behaviors are not included in classic definitions of comorbidity. However, behaviors such as alcohol intake, smoking, and low levels of physical activity have independent effects on the risk of vascular comorbidities and the outcomes of MS. Therefore, we considered health behaviors as comorbidity risk factors rather than simple confounders. 15
Mechanism of comorbidity in MS
The prevalence of comorbidity gradually increases year by year with the progression of multiple sclerosis and the increasing age of patients.17,18 Several general mechanisms may explain the coexistence of comorbidity and MS. Conditions may co-occur due to chance, or may be uncovered as a result of tighter screening tests before or subsequent to MS diagnosis and treatments (“surveillance hypothesis”). 19 However, the co-occurrence of disease may also relate to underlying disease-related mechanisms:
1.
2.
3.
4.
The prevalence and incidence of comorbidity in MS
The reported prevalence and incidence of comorbidity in MS vary widely, depending on the study population and the type and number of conditions considered. Based on meta-analysis, the five most prevalent comorbidities seen in MS are depression (23.7%), anxiety (21.9%), hypertension (18.6%), hyperlipidemia (10.9%), and chronic lung disease (10.0%). 3 Some comorbidities occur more commonly in PwMS than in the general population, particularly mood disorders, cardiovascular disease, and some of the comorbid autoimmune conditions. 3 A large population-based study from four Canadian provinces using data from 23,382 incident MS cases and 116,638 age-, sex-, and geographically matched controls reported that the most prevalent comorbidity in PwMS was depression (19.1%), followed by hypertension (15.2%), while in the matched controls the prevalence of these two comorbidities were only 9.38% and 12.9% respectively. 27 Although psoriasis (7.74%) and thyroid disease (6.44%) were the most prevalent comorbid autoimmune diseases reported in the MS population, most studies report no statistically significant difference in prevalence when compared to the general population. Inflammatory bowel disease is the only autoimmune disease consistently reported to be more common in the MS population (0.56% vs 0.30% in the general population). 27 Summaries of comorbidities across multiple body systems reported to be associated with MS are provided in Tables 1–6 and Figure 1.14,18,27–38
Risk factors of adverse health behaviors that have been reported to be associated with MS.

MS, multiple sclerosis; RLS, restless legs syndrome.
Metabolic syndrome comorbidities that have been reported to be associated with MS.

DM, diabetes mellitus; MS, multiple sclerosis.
Vascular comorbidities that have been reported to be associated with MS.
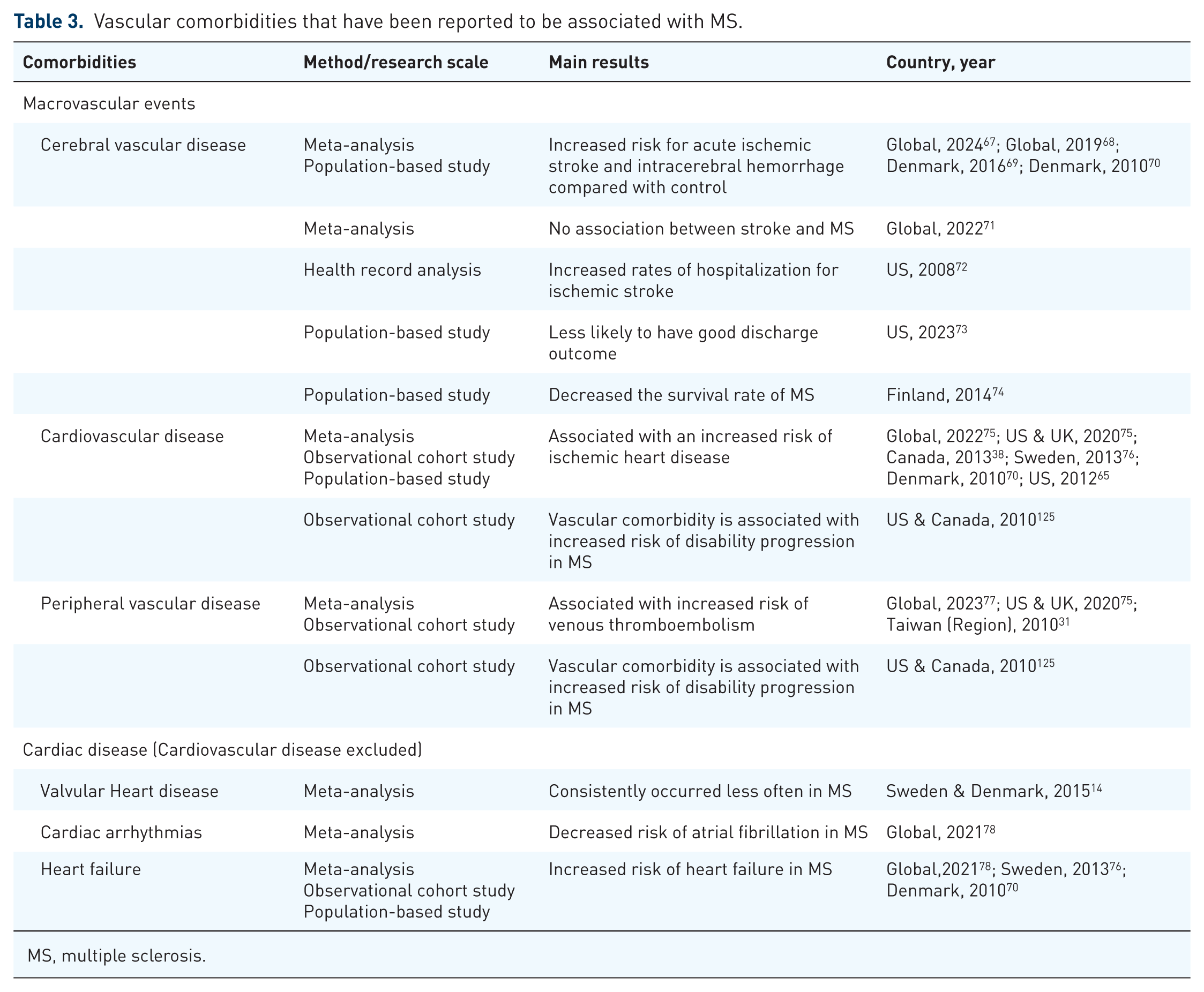
MS, multiple sclerosis.
Comorbidities (Psychiatric and Neurologic disease) have been reported to be associated with MS.
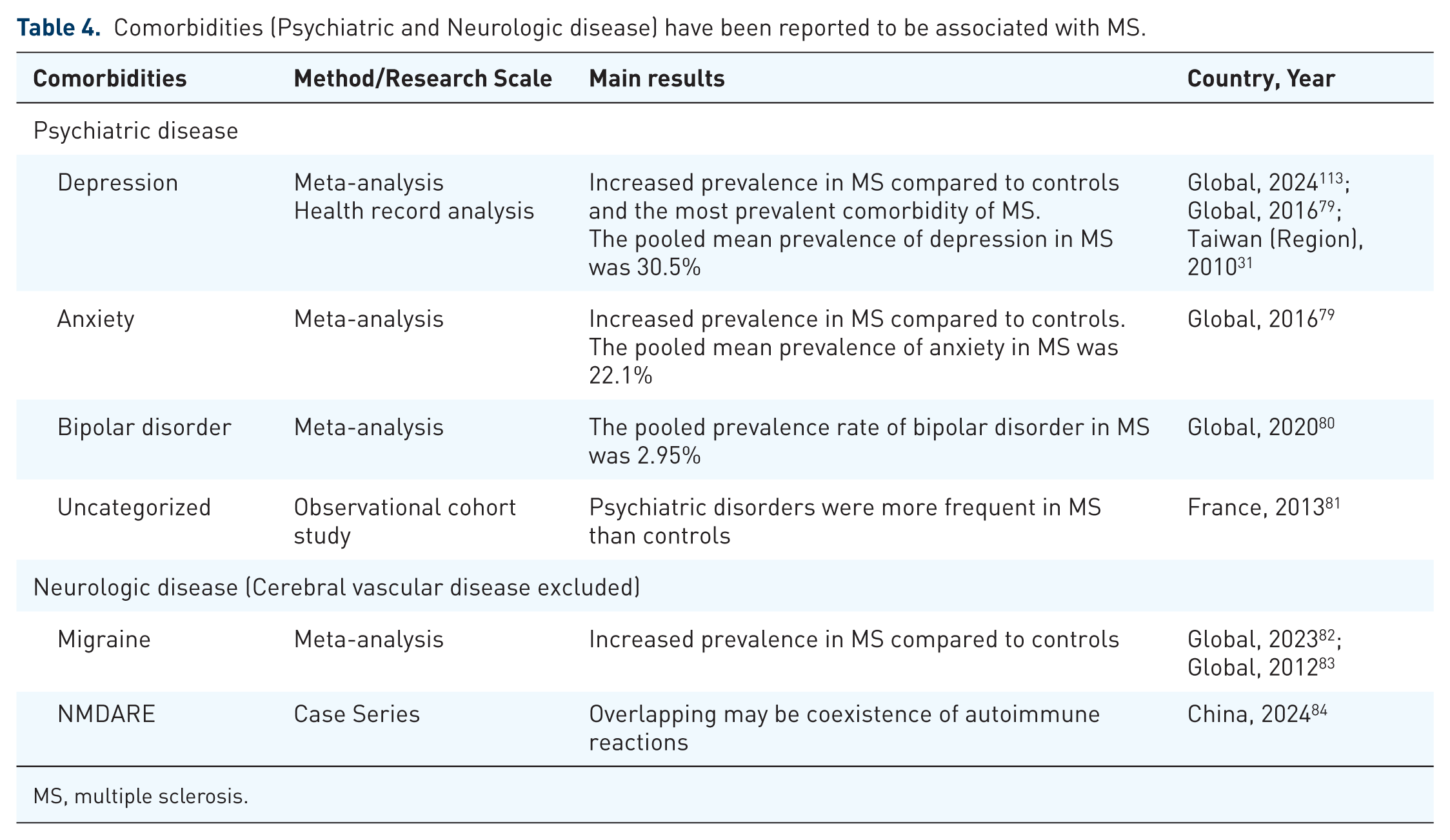
MS, multiple sclerosis.
Comorbidities (autoimmune, gastrointestinal, hematology, renal disease) have been reported to be associated with MS.

GERD, Gastroesophageal reflux disease; MS, multiple sclerosis; PwMS, patients with multiple sclerosis; RA, rheumatoid arthritis; SLE, systemic lupus erythematosus; UC, ulcerative colitis.
Comorbidities (pulmonary disease, dermatology disease, musculoskeletal disorder visual disorders and neoplasms) that have been reported to be associated with MS.

COPD, chronic obstructive pulmonary disease; HR, hazard ratio; MS, multiple sclerosis.

Comorbidities and the prevalence of different comorbidities in multiple sclerosis.
The pattern of comorbidity in different groups of PwMS
Comorbidity at different stages of MS
Many studies have reported that comorbidities are common in PwMS before, at, and after diagnosis. At least some of the prodromal symptoms and diagnoses seen prior to MS diagnosis likely relate to comorbid illness. A nested case-control study including 10,204 incident MS cases and 39,448 matched controls reported MS patients had a significantly higher risk of depression, anxiety, insomnia, gastric, intestinal, and urinary disturbances even 10 years before MS diagnosis. 105
At the time of MS diagnosis, many studies report that the comorbidity burden is already high.106,107 When compared to age-, sex-, and geographically matched controls, the prevalence of hypertension, diabetes, heart disease, chronic lung disease, epilepsy, fibromyalgia, inflammatory bowel disease, depression, anxiety, bipolar disorder, and schizophrenia was reported as more common in the MS population at MS diagnosis. 27 A study of 8983 American participants in the NARCOMS registry 108 reported that 35.0% of participants had at least one physical comorbidity at MS diagnosis, of whom 53.6% had one comorbidity, 24.6% had two, and 21.8% three or more. Therefore, clinicians need to be aware of the presence of comorbidities at the diagnosis of a first demyelinating event and treat the patient holistically. 18
The prevalence of specific comorbidities increases after MS onset or diagnosis. Comorbidities with the highest change in prevalence post-symptom onset were reported to be depression (+26.9%), anxiety (+23.1%), hypertension (+21.9%), osteoarthritis (+17.1%), high cholesterol (+16.3%), eye diseases (+11.6%), osteoporosis (+10.9%), and cancer (+10.3%). 18 This accumulation of comorbidities seems to be greater than that expected with normal aging, and the mechanisms mentioned above may explain this change. 18 Behavioral changes seen in some PwMS may accelerate the accumulation of certain comorbidities. For example, physical activity may drop in the context of neurological illness, which may contribute to an increased risk of vascular comorbidities and osteoporosis. Second, the use of DMTs in PwMS may indirectly cause certain comorbidities, as mentioned above.
Comorbidity in different sexes of MS
Sex-specific differences in the prevalence of both overall burden and specific comorbidities have been studied in recent years. Some studies reported that compared to female PwMS, comorbidities were more frequent in male PwMS. Based on a study of 8983 MS patients from the NARCOMS registry, being male was reported to be associated with the risk of comorbidity (females vs males, odds ratio (OR) 0.77; 95% CI (confidence interval), 0.69–0.87). 106 Different patterns of comorbidities between sexes have also been reported. For example, the prevalence of hypertension was disproportionately higher in men than women with MS Based on a population-based study, 27 21.5% of male PwMS and 14.2% of female PwMS had hypertension, while this percentage in the age-, sex-, and geographically matched population was similar in both sexes (14.5% in male vs 12.3% in female controls). Hence, relative to the matched populations, the prevalence of hypertension was 48% higher for men with MS and 16% higher for women with MS. In contrast, the prevalence of chronic lung disease has been described as more frequent in female patients. In the same population-based study, 13.5% of female MS patients had chronic lung disease, compared to 9.74% of female matched population, with similar proportions between male PwMS (9.90%) and male matched population (8.21%). However, the difference in MS comorbidity across biological sexes and socio-cultural genders remains an unresolved issue and requires more attention and further investigation in future studies.
When screening for MS complications in clinical practice, it is therefore important to consider not only the risk factors for comorbid disease and the background population prevalence but also the specific comorbidities that are increased in MS patients of different sexes.
Comorbidity in different ages of MS
Significant advances have been made in recent years, both in the treatment of MS and in the comorbidities associated with aging. Consequently, the life expectancy of PwMS almost equals that of the general population,109,110 and this has drawn more attention from researchers to the comorbidities in elderly MS patients. As in the general population, old age is accompanied by a greater risk of developing other health disorders.
The prevalence of metabolic syndromes, such as hypertension, hyperlipidemia, and diabetes, increases in older age groups and may be directly connected to cognitive impairment in MS. Cardiovascular diseases are believed to be the most common cause of death in people over 65 years of age, and prevalence increases significantly after the age of 50 years. 111 In addition, autoimmune diseases, such as rheumatoid arthritis or giant cell arteritis, and autoantibodies, such as antinuclear antibodies, are common findings in elderly people. 112
However, unlike the above comorbidities, anxiety and alcohol abuse were reported in some studies to be statistically significantly less likely among older age groups.113,114 Other studies also mentioned that older age is associated with a lower prevalence of depression and milder symptoms. 115 Due to the differential prevalence of comorbidities in different age groups, MS specialists should place greater emphasis on carefully screening for such age-related comorbidities in older adults with MS. When necessary, they should promptly refer patients with certain comorbidities to appropriate specialists for specialized treatment and regular follow-up. This is an important component of the holistic management of MS patients.
Comorbidity in different ethnic groups of MS
So far, the vast majority of global research on MS comorbidity has been conducted in Europe and North America, with high-quality epidemiological studies emerging from countries such as Canada, Italy, the United States, Sweden, and the United Kingdom. However, due to the scarcity of relevant publications from Africa and Asia, and the fact that even within Europe and North America, high-quality studies are largely concentrated in limited regions rather than being nationwide and population-based, it remains challenging to conduct globally comparative research on ethnic-specific MS comorbidities. More extensive and diverse ethnic studies are needed in the future, particularly high-quality research on MS comorbidities from Africa and Asia.
The effect of comorbidity on MS
Comorbidities have an adverse influence on outcome throughout the disease course in PwMS, from MS diagnosis to the end of life. At the individual level, comorbidity is associated with postponed diagnosis, increased severity of disability at diagnosis, higher relapse rates, earlier disability progression, worse MRI outcome, lower health-related quality of life, more complicated DMT decisions, and even increased mortality5,6,116,117 At the health system’s and society’s level, comorbidity is associated with increased healthcare costs, healthcare utilization, and reduced employment. 5
Comorbidity postpones the diagnosis of MS
Comorbidity may present very early in the MS disease course at diagnosis, and preexisting comorbidity may obscure the MS diagnosis. 6 Several studies reported that comorbidity was associated with MS diagnostic delay. Using the NARCOMS registry, Marrie and her team did a study that included 8,983 MS participants with physical and mental comorbidities. It found that the presence of comorbidities and associated adverse health behaviors may both be associated with diagnostic delay. The mean (SD) diagnostic delay in the study sample was 7.03 (7.4) years. 6 After multivariable adjustment for demographic and clinical characteristics, the diagnostic delay increased if vascular, autoimmune, musculoskeletal, gastrointestinal, visual, and mental comorbidities were present. Another nationwide population-based Danish study reached a conclusion consistent with Marrie’s findings; However, it reported a mean (SD) diagnostic delay of 3.96 (4.79) years, which differs somewhat from the previous study. They also identified that PwMS who suffered from cerebrovascular, cardiovascular, and pulmonary disease, as well as DM and malignancies, had statistically significant longer diagnostic delays for MS. 116
The reasons for this diagnostic delay associated with comorbidities are unknown, but there are several possible explanations6,116: First, preexisting diseases or adverse effects of their treatments may conceal new symptoms and negatively affect access to care. The patient tends to attribute new symptoms to the known disease that the patient has already been diagnosed. Second, the doctor attributes the new symptoms and signs to the preexisting disease. Third, the diagnostic test results may be complicated by preexisting disease and interpreted incorrectly. For example, preexisting diabetic neuropathy could present with sensory symptoms that overshadow sensory symptoms related to as-yet undiagnosed MS. These findings suggest that practitioners treating patients with chronic diseases should not attribute new neurologic signs or symptoms to preexisting diseases without careful consideration.
Comorbidity influences disability at MS diagnosis
Preexisting comorbidity also affects the severity of disability at MS diagnosis. Specific comorbidities that were reported to be associated with increased severity of disability at diagnosis mainly included obesity, vascular, musculoskeletal, and mental comorbidities. 6 Other comorbidities, such as gastrointestinal and autoimmune disease, were not associated with the severity of disability at diagnosis. Marrie et al. did a study based on the NARCOMS Registry and used Patient Determined Disease Steps (PDDS) to measure the degree of disability at MS diagnosis. The study found that an increasing number of comorbidities was associated with a greater degree of disability at diagnosis. 6
There are several possible reasons for this association: first, attribution of MS symptoms and signs to a preexisting comorbidity delays the MS diagnosis and consequently leads to more severe disability at diagnosis. 116 Second, combinations of different chronic comorbidities may lead to similar disability and result in reduced mobility or balance at MS diagnosis. 6 Third, different comorbidities may have interactions pathophysiologically and could increase the disability. 6 For example, autoimmune diseases such as systemic lupus erythematosus (SLE) with increased peripheral inflammation and elevated cytokines are associated with disability of MS at onset.
Comorbidity is associated with increased MS relapse rate
The association between comorbidity and the risk of relapse has been evaluated in several studies. The presence of multiple comorbidities has been associated with more relapses regardless of DMT use,7,117,118 and a higher comorbidity burden (3 or more conditions) is additionally associated with increased relapse rate (Hazard Ratio (HR), 1.45; 95% CI, 1.00–2.08).7,118 Kaarina et al. 7 recruited 885 relapsing-onset MS patients from four Canadian MS clinics in a prospective multicenter cohort study. They reported participants with ⩾3 baseline comorbidities (relative to none) had a higher relapse rate over the subsequent 2 years.
In particular, migraine was found to be associated with increased relapse rate (HR, 1.38; 95% CI, 1.01–1.89), and this result was independent of the effects of age and sex.119,120 A potential biological explanation for this is reverse causation, in that MS relapse mediates the release of vasoactive amines, including bradykinin and adenosine triphosphate, which lead to migraine attack. 119 Second, it may be that the release of inflammatory and vasoactive compounds during a migraine can also trigger MS relapses. 121 Third, there may be confusion between symptoms relating to migraine and those relating to MS.
Several other comorbidities have also been reported to be associated with MS relapses. For example, psychiatric disorders were proven to be associated with an increased hazard of relapse (HR, 1.07; 95% CI, 1.02–1.14) compared with no psychiatric disorders in a meta-analysis study based on 16,794 MS patients. 120 Hyperlipidemia was also reported to be associated with increased MS relapse rate in a cohort study based on four Canadian MS clinics. 7 There were also some small-scale studies reported that rheumatoid arthritis, anemia, and asthma were associated with increased risk of relapse. 122 However, the causal relationships between these comorbidities and MS relapses remain to be confirmed by larger, population-based studies or systematic reviews.
Therefore, for MS patients with comorbidities, a comprehensive evaluation of the comorbidity profile is important for predicting the patient’s disease activity and provides guidance in formulating a personalized DMT plan.
Comorbidity has adverse influence on MS disability progression
Different comorbidities have been found to be associated with disability and disease progression in PwMS. Obesity at MS onset was reported to be associated with an increased risk to reach an EDSS of 3 after 6 years, after adjustment for sex, age, smoking, and comorbidities (HR 1.84; 95% CI 1.29–2.61). 66 A more interesting study reported that obesity is associated not only with disability progression as reflected by the EDSS but also with cognitive disability worsening (HR 1.51; 95% CI 1.09–2.09). 123 The level of disability in those who reported dyslipidemia (HR 1.05; 95% CI 0.07–2.02) was reported to be significantly higher compared to those who did not report this comorbidity. 122 Restless legs syndrome (OR: 0.98; 95% CI, 0.97–0.99) has also been reported to be associated with faster MS disability progression. 124
In recent years, the comorbidity that has received the most attention is vascular disease. The presence of two or more cardiometabolic conditions, such as hyperlipidemia, ischemic heart disease, and cerebrovascular conditions, was associated with a more rapid progression of disability.120,125 Patients with one or more vascular comorbidities at the time of their diagnosis of MS had more than 1.5 times increased risk of needing a cane to walk. 125 MS patients with vascular comorbidities progressed to an EDSS of 6 on average 6 years sooner than those who never had a vascular comorbidity. These significant associations between vascular disease and disability progression in MS may be explained by the fact that increased peripheral inflammation in vascular diseases may accelerate neurodegeneration and brain atrophy.126,127 Alternatively, both may impact disability outcomes via impaired neuronal resilience.
In a multicenter cohort study of 3166 individuals with incident MS, Zhang et al. also confirmed that comorbidities are associated with an apparent increase in MS disability progression. Interestingly, they found that with each additional comorbidity, there was a mean increase in the EDSS score of 0.18. 9 Thus, approximately having one comorbidity confers an increase in disability as large as 2 years of expected progression over time.
In addition to physical and mental comorbidities, certain adverse health behaviors also increase the risk of disability progression. Smoking has been associated with reaching key disability milestones and the conversion from RRMS and SPMS across multiple studies. A UK cohort study of 895 people with MS reported that the risk of reaching an EDSS score of 4.0 and 6.0 was higher in those who had a history of smoking than in those who never smoked. Besides, ex-smokers had a significantly lower risk of reaching an EDSS score of 4.0 and an EDSS score of 6.0 than current smokers. 128 A study of 728 smokers from the Swedish National MS Registry estimated the time to conversion from RRMS to SPMS. They demonstrated that each additional year of smoking after diagnosis accelerated the time to conversion to SPMS by 4.7%. The median age at conversion to SPMS was 48 years in those who continued to smoke versus 56 years in those who quit. 129
So far, the mechanism of this association between comorbidity and disability progression is not known. The studies published still cannot confirm whether treating comorbidities can mitigate the impact of these comorbidities on MS disability progression. However, monitoring comorbidity is generally crucial for assessing the prognosis of MS and treating MS holistically.
Comorbidity influences treatment decisions of PwMS
The number of comorbidities was reported to be associated with a time-dependent reduction in the likelihood of initiating a DMT. A one-unit increase in the number of comorbidities may lead to 10% reduction in the likelihood of initiating a DMT (HR 0.90; 95% CI 0.84–0.96) at 1 year from the index date. Patients with ischemic heart disease (IHD) had a lower likelihood of initiating a DMT compared to those without IHD (HR 0.72; 95% CI 0.59–0.87). A retrospective cohort study based on 12,922 older adults (over 60 years) with MS found that congestive heart failure (OR 0.69; 95% CI 0.49–0.99), pulmonary circulation disorder (OR 0.52; 95% CI 0.31–0.87), chronic pulmonary disease (OR 0.72; 95% CI 0.57–0.90), gastrointestinal disorders (OR 0.63; 95% CI 0.42–0.96), cancer/lymphoma (OR 0.66; 95% CI 0.51–0.86), and rheumatoid arthritis/collagen-related disorders (OR 0.75; 95% CI 0.58–0.97), were reported to decrease the likelihood of being prescribed a DMT.10,130 Possible reasons include diagnostic delay due to comorbidity, 6 comorbidities leading to DMT contraindications, hesitation to initiate DMT due to multidrug burden, and comorbidity-related risk-benefit imbalance.
Comorbidities may also influence the choice of DMT. For example, the presence of cardiovascular diseases may be an important contraindication when prescribing sphingosine-1-phosphate (S1P) receptor-targeted agents (e.g., fingolimod).
Some comorbidities have been observed to increase the risk of adverse events significantly. A study based on population-based health administrative data in British Columbia, Canada, reported that treatment with IFN-β was associated with a 1.8-fold increase in the risk of stroke, a 1.6-fold increase in the risk of migraine, and a 1.3-fold increase in depression and hematologic abnormalities. 7 Moreover, diabetes is proven to increase the risk of macular edema associated with fingolimod. 131 At the same time, MS patients with migraine may have more difficulty tolerating specific disease-modifying treatments due to worsening headache profiles. 132
A preexisting comorbidity may have an impact on DMT adherence, persistence, and tolerability and thus be associated with a higher risk of switching from the first DMT. 133 For example, comorbid depression is already recognized to reduce adherence to DMTs based on analyses of data obtained from 686 persons with MS. 134
In summary, comorbidities not only affect MS disease itself but also affect DMT decisions, including the choice of whether to initiate DMT, the specific choice and switching of treatment, as well as the efficacy, safety, adherence, and tolerability of DMT. Therefore, assessing comorbidities in PwMS can help guide appropriate personalized treatment approaches.
Comorbidity influences quality of life in PwMS
The impact of comorbidity on quality of life in PwMS has been studied in several large cohorts. An increasing amount of evidence suggests that comorbidities could decrease quality of life.12,135 The association of comorbidity and health-related quality of life (HRQoL) was investigated with 8983 participants in the NARCOMS registry. 135 After adjustment for sociodemographic and clinical factors, physical HRQoL decreased as the number of comorbidities increased. A study based on 949 MS patients from four MS clinics across Canada even quantified the impact of comorbidities on quality of life to the extent that an increase of one physical comorbidity corresponded to a decrease of 0.05 points on the Health Utilities Index Mark 3 (HUI3) global utility score. As differences of 0.03 or greater in HUI3 global utility scores are considered clinically important, 136 screening and treatment for comorbidities is significant for improving the quality of life in PwMS. 12
Several specific physical comorbidities have been identified to have an adverse impact on the quality of life in MS. Patients with musculoskeletal and respiratory conditions were reported to have poorer physical HRQoL compared to patients without those disorders. 137 Meanwhile, poorer mental HRQoL was also found in patients with headaches and urinary and digestive tract problems. 137 Except for the direct influence of physical comorbidity on quality of life, physical comorbidity also indirectly worsens the symptoms of depression and fatigue, both of which are important determinants of HRQoL for MS patients. 12
Consequently, as a complement to treatments, interventions targeting amenable comorbidities may result in meaningful improvements in HRQoL of PwMS.
Comorbidity is associated with increased premature mortality
Many studies in North America and Europe have observed that comorbidity is associated with a greater mortality rate among PwMS.13,138–140 The survival remained shorter in the MS population than in the general population. A population-based study identified 5797 MS patients and 28,807 controls matched on sex, year of birth, and region and found that MS was associated with a 2-fold increased risk of death. 13 Comorbidity was believed to be associated with increased mortality risk, and there was a dose effect of preexisting comorbidities on mortality. A study based on the UK Clinical Practice Research Datalink used the Charlson comorbidity index (CCI) to estimate the burden of comorbidity in PwMS. Their results showed that the 5-year all-cause mortality rates in patients with MS were 3.67%, 8.22% and 12.45% for patients with CCI scores of 0, 1, and ⩾2 at the index date, respectively. 107
Several comorbidities, including cardiovascular comorbidity, psychiatric comorbidity, diabetes comorbidity, and lung comorbidity, were consistently found to be associated with increased mortality in MS in several nationwide population-based studies focusing on the effect of comorbidity on mortality in MS.13,116,139,140 Other comorbidities that have been reported to have an influence on the mortality of MS also included cancer comorbidity 116 and cerebrovascular comorbidity, 116 but do not include autoimmune disease, gastrointestinal disease, or musculoskeletal disease. 141 The above impact of comorbidity may partially explain the conclusion, drawn by studies from Denmark and other regions of the world, that the MS population has 10 years shorter life expectancy than the general population.141,142
Conclusion
Over the past few decades, comorbidities of MS have received increasing attention from clinicians caring for people with MS. Comorbidities increase the complexity of patient management and have health, social, and economic consequences for people with MS. Understanding the effects of comorbidities may lead to changes in the disease treatment choice and target, as shown in the national hypertension guidelines that the target blood pressure and the selection of antihypertensive therapy depend on the presence of comorbidities such as diabetes or chronic renal disease. 143 Therefore, routine screening for comorbidity risk factors, as well as chronic comorbidities, should be an important aspect in MS clinical practice. When treating MS patients, the control of modifiable risk factors for comorbidities, treatment of comorbidities, prehabilitation, and rehabilitation are as important as MS-specific DMTs.
To date, there are considerable variations in the outcome data among many published studies on comorbidities. Furthermore, numerous topics related to comorbidities, such as differences across different ethnicities, different age groups, and gender-diverse groups, have yet to receive sufficient attention and in-depth research. Studies based on high-quality disease registries and administrative databases covering an entire population to identify and understand the comorbidities and their risk factors are keys to individualized MS treatment and could further improve outcomes for PwMS in the future.
