Abstract
Balloon endoscopy-assisted endoscopic retrograde cholangiopancreatography (BE-ERCP) has become an essential modality for managing pancreaticobiliary diseases in patients with surgically altered anatomy (SAA). This review summarizes the current evidence and technical advances in BE-ERCP, with a focus on insertion strategies tailored to specific reconstructive surgical techniques. Recent developments in short-type balloon endoscopes have improved maneuverability and device compatibility, enabling the widespread use of standard ERCP accessories. In addition, innovative tools, such as highly rotatable sphincterotomes, helical stone retrieval baskets, and newly introduced slim cholangioscopes, have expanded the diagnostic and therapeutic potential of BE-ERCP. Papillary interventions, including endoscopic sphincterotomy, endoscopic papillary balloon dilation (EPBD), large balloon dilation (EPLBD), and combined approaches (ESBD), are discussed with respect to their feasibility and safety in SAA. Furthermore, the clinical efficacy of stone removal and lithotripsy techniques, including peroral cholangioscopy-guided electrohydraulic lithotripsy, is reviewed. Finally, we address the emerging role of interventional endoscopic ultrasound as a complementary or alternative strategy to BE-ERCP. Taken together, this review provides a comprehensive update on current techniques and evolving strategies for endoscopic management of bile duct stones in patients with altered anatomy.
Keywords
Introduction
Endoscopic retrograde cholangiopancreatography (ERCP) is the standard treatment for bile duct stones, offering high success rates and minimal invasiveness in patients with normal gastrointestinal anatomy.1–3 However, in patients with surgically altered anatomy (SAA), such as those who have undergone Roux-en-Y (R-Y) gastric bypass, Billroth II (B-II) gastrectomy, or pancreaticoduodenectomy (PD), standard ERCP becomes technically challenging in these patients, mainly because of the complexity of the reconstructed gastrointestinal tract and the difficulty in reaching the papilla or bilioenteric anastomosis.
Previously, percutaneous transhepatic drainage and surgical treatment were considered the first-line options.4,5 In 2001, double-balloon endoscopy (DBE) was developed for the diagnosis and treatment of small bowel diseases,6,7 and subsequently, balloon endoscopy-assisted ERCP (BE-ERCP) began to be performed for pancreatobiliary interventions in patients with SAA, with numerous reports demonstrating its efficacy.8–12 Furthermore, short-type balloon endoscopes, including DBE and single-balloon endoscopy (SBE), specifically designed for pancreatobiliary interventions, became available.13–16 These scopes offered excellent insertion performance and compatibility with standard ERCP accessories, leading to the establishment of BE-ERCP as the first-line treatment for pancreatobiliary diseases in patients with SAA.1–3
In parallel, therapeutic endoscopic ultrasound (EUS) has gained increasing attention as an alternative or complementary strategy, especially in cases where BE-ERCP is technically unsuccessful or time-prohibitive.17,18
Furthermore, percutaneous transhepatic biliary drainage and surgical bile duct exploration remain important fallback options, particularly for patients with complex anatomy, inaccessible anastomoses, or failed endoscopic interventions.
This review aims to provide a comprehensive overview of bile duct stone removal in patients with SAA, with a primary focus on BE-ERCP techniques and outcomes. In addition, we discuss the evolving role of EUS-guided approaches, percutaneous and surgical alternatives, and highlight current limitations, evidence gaps, and future perspectives in this rapidly developing field.
Reconstruction method in SAA
Surgical treatment for gastrointestinal and pancreatobiliary cancers has led to improved patient prognosis, not only due to advances in surgical techniques but also through enhanced perioperative management, including adjuvant and neoadjuvant chemotherapy. As a result, the frequency of encountering conditions such as bile duct stones, biliary or pancreaticojejunostomy strictures, and malignant biliary obstruction has been increasing in patients with surgically altered gastrointestinal anatomy.
Various reconstruction methods are employed following gastrectomy, including Billroth I (B-I), B-II, R-Y, and double-tract reconstruction. 19 Among these, the R-Y method has become increasingly common in recent years. After PD, several reconstruction techniques are used, such as the Modified Child method, Whipple method, and Cattell method. 20 In B-II and modified Child reconstructions, a Braun anastomosis may be added, which can influence the subsequent endoscopic insertion strategy.
In cases of congenital biliary dilatation or bile duct injury during cholecystectomy, gastric-preserving R-Y reconstruction with hepaticojejunostomy is commonly performed. Although rare in Japan, R-Y gastric bypass is widely used in Western countries as a treatment for obesity. 21
In patients who have undergone B-I, B-II, or R-Y reconstruction following gastrectomy, the target for cannulation remains the native duodenal papilla. By contrast, after PD or gastric-preserving R-Y reconstruction, the target is the choledochojejunostomy site. The insertion techniques differ according to each reconstruction method and are described in the following sections.
Insertion technique
Various types of reconstructive surgical techniques exist, and even within the same reconstruction method, substantial variation in the location and angle of anastomoses can significantly complicate scope insertion during BE-ERCP. In this section, we provide an overview of insertion strategies according to representative types of gastrointestinal reconstruction (Figure 1).

Representative gastrointestinal reconstruction methods and corresponding endoscopic insertion strategies. (a) Modified Child reconstruction with Braun anastomosis after pancreaticoduodenectomy. At the gastrojejunostomy site, the efferent limb should be selected. At the Braun anastomosis, the central lumen among the three—extending straight beyond the suture line—should be chosen. (b) Billroth II reconstruction without Braun anastomosis after distal gastrectomy. Accurate identification and selection of the afferent limb are essential for reaching the papilla. The afferent limb is often fixed in an upwardly retracted position. (c) Roux-en-Y hepaticojejunostomy with gastric preservation. This is the most technically challenging reconstruction, requiring deep intubation with maximal scope shortening and stretching to avoid loop formation and slack in the remnant stomach. (d) Roux-en-Y reconstruction after total gastrectomy. Scope insertion is relatively straightforward, but the approach to the papilla is more critical. A large reverse alpha loop should be formed while avoiding excessive shortening or traction to achieve a favorable retroflexed position.
In patients with B-II or Child reconstruction, 22 the insertion route depends on the presence of a Braun anastomosis. If present, insertion should be performed via the efferent limb, and at the anastomosis, the central lumen (i.e., the lumen continuing straight beyond the suture line) should be selected. If absent, accurate identification of the afferent limb is essential to avoid inadvertent entry into the efferent limb. In such cases, the afferent limb is often fixed in an elevated position to prevent afferent loop syndrome, which complicates insertion and increases the risk of gastrointestinal perforation due to excessive advancement force. 23
In R-Y reconstruction following gastrectomy, insertion itself is not particularly difficult; rather, the approach to the papilla is of greater importance.24,25 By intentionally avoiding scope shortening or stretching and instead forming a large reverse alpha loop during insertion, a favorable retroflex position can often be achieved. Conversely, R-Y reconstruction with gastric preservation presents the greatest challenge for insertion. To avoid slack caused by loop formation within the remnant stomach, deep intubation should be performed with maximal scope shortening and stretching.
Thus, even among patients with R-Y reconstruction, endoscopic insertion techniques must be adapted based on whether gastrectomy has been performed, underscoring the importance of selecting an approach tailored to the specific surgical anatomy.
Devices for balloon endoscopy-assisted ERCP
Balloon endoscopy
Balloon endoscopy is an endoscopic system developed based on a novel insertion technique, in which the intestine is grasped and stabilized or shortened using balloons to enable deep insertion through a long and tortuous postoperative intestinal tract. Currently, two balloon endoscopy systems are available: the double-balloon endoscope from Fujifilm and the single-balloon endoscope from Olympus.
Initially, ERCP in SSA was performed using standard-type scopes designed for small bowel observation8,9; however, their extended length and limited compatibility with therapeutic devices made for standard ERCP procedures even more challenging than today. In 2016, short-type scopes became available for both DBE and SBE systems,26–28 enabling the use of standard ERCP devices due to their appropriate working length and larger accessory channel diameter. To improve insertion performance, DBE is equipped with an “advanced force transmission function” and an “adaptive bending system,” while SBE incorporates “high-force transmission” and “passive bending.”
These standard-type scopes have undergone various improvements in recent years, including enlargement of the accessory channel, enhancement of image quality, incorporation of image-enhanced endoscopy functions, and further advancements in insertion performance. Further refinements are also anticipated in short-type scopes used for pancreatobiliary interventions.
The primary difference between the EI-580T and the SIF-H290S lies in the number of balloons; however, the position of the device channel also differs (Table 1). 29 In the EI-580T, the catheter exits in the 5 o’clock direction, allowing the catheter tip to point toward 11 o’clock—this design is optimized to align with the bile duct axis when the papilla is positioned at 6 o’clock. By contrast, the SIF-H290S has its device channel at the 8 o’clock position, requiring the operator to adjust the papilla to a position between 8 and 12 o’clock, and to fine-tune the catheter angle accordingly for successful biliary cannulation based on the specific case (Figure 2). 24
Parameter of balloon endoscopies.


Endoscopic view and device channel orientation in balloon-assisted endoscopy. (a) In double-balloon endoscopy using the EI-580BT (Fujifilm Co., Tokyo, Japan), the device channel exits at the 5 o’clock position, allowing the catheter tip to naturally orient toward 11 o’clock. This facilitates alignment with the bile duct axis when the papilla is at 6 o’clock. (b) In single-balloon endoscopy using the SIF-H290S (Olympus Co., Tokyo, Japan), the device channel is at the 8 o’clock position. The operator must adjust the papilla to between 8 and 12 o’clock and fine-tune the catheter angle to achieve successful biliary cannulation, depending on the anatomical situation.
Accessory devices for biliary stone management
In biliary access and bile duct stone treatment, in addition to guidewires, catheters, and sphincterotomes, a variety of devices are required, including dilators (balloon/mechanical/drill types), stone retrieval balloons, baskets, and a mechanical lithotripter. In BE-ERCP, scope maneuverability limitations and the lack of an elevator necessitate the appropriate selection of devices to ensure safe and efficient stone extraction.
Short-type BAE allows the use of standard ERCP accessories. For difficult cannulation, devices such as steerable cannulas (Swing Tip; Olympus Co., Tokyo, Japan/KC226; Zeon Medical, Tokyo, Japan)30–32 and the high-rotatability sphincterotome (Seeking Tome ZERO; MTW Endoskopie, Wesel, Germany/ENGETSU; KANEKA Medix, Osaka, Japan) facilitate optimal axis alignment .33–37 The pancreatic duct guidewire technique can be stabilized using the uneven catheter. 38
During endoscopic sphincterotomy (EST), the altered scope orientation often causes the sphincterotome to face away from the oral protrusion (Figure 3). The novel highly rotatable sphincterotome (ENGETSU), with excellent rotatability, enables precise blade positioning and is gaining attention.36,37 Among balloon dilators, REN (KANEKA Medix)—with its tapered tip—provides high penetration in tight intrahepatic or anastomotic strictures. In endoscopic papillary balloon dilation (EPBD), balloon slippage is problematic, and waist-shaped nonslip balloons have been reported to be effective in BE-ERCP. 39 Drill dilators, originally developed for interventional EUS, 40 are also useful in BE-ERCP for tight or angulated strictures. 41 For stone retrieval, helical eight-wire baskets (VorticCatchV; Olympus Co./RASEN2; KANEKA Medix) offer superior grip and rotation, and are effective regardless of SAA.

Blade direction during endoscopic sphincterotomy with conventional and balloon endoscopy. (a) With a side-viewing duodenoscope and conventional sphincterotome in normal anatomy, the blade naturally aligns with the papillary oral protrusion due to the direction of endoscope bending. (b) In balloon endoscopy-assisted ERCP for altered anatomy, using a conventional sphincterotome, the blade often misaligns with the desired incision direction due to endoscope bending, frequently pointing opposite to the papillary oral protrusion.
Unlike standard ERCP scopes, device usage is limited due to restrictions in scope length and working channel diameter. With mechanical lithotripters, non-guidewire-assisted models can be employed as in standard ERCP; however, the selection of guidewire-compatible models remains limited (Trapezoid; Boston Scientific, MA, USA/LithoCrushV; Olympus Co.).
Previously, due to limitations in working channel diameter, the use of mother–baby cholangioscopes during BE-ERCP was not feasible. However, with the recent introduction of the slim peroral cholangioscope (POCS; eyeMax 9Fr (≒ϕ3.2 mm); Micro-Tech Endoscopy, Nanjing, China), it has become possible to use cholangioscopy through the working channel of balloon endoscopes (ϕ3.2 mm). This advancement has also enabled the application of POCS-guided lithotripsy, including electrohydraulic and laser systems, thereby expanding therapeutic options in patients with SAA.
In standard-type endoscopes, further limitations arise due to the scope length, restricting the available options for devices such as guidewires (Revowave RWUA-2555I; PIOLAX Inc., Yokohama, Japan), sphincterotomes (MTW disposable papillotome 9913021051; MTW Endoskopie), retrieval balloons (Zeon balloon catheter for biliary stone removal 133-127-3; Zeon Medical Co., Japan/Multi-3V Plus B-V233V-A, Olympus Co.), and mechanical lithotripters (Zemex crusher catheter LBGT-7425S; Zeon Medical Co.). In addition, the use of removable, integrated plastic biliary stents and metal stents is not feasible.
Clinical outcomes of BE-ERCP
With the widespread adoption of BE-ERCP, this technique has been extensively utilized for the management of pancreatobiliary diseases in patients with SAA. Numerous studies have been conducted to date, progressively elucidating its therapeutic outcomes.
DB-ERCP and SB-ERCP
DBE and SBE differ in the number of balloons, the position of the device channel, and device performance. These differences can affect scope insertion, biliary cannulation, the success rates of therapeutic interventions, and the incidence of adverse events.
A meta-analysis in 2021, 15 including 24 studies with a total of 1523 DB-ERCP cases, reported a scope insertion success rate of 90% (95% CI: 84–94) and a therapeutic success rate of 93% (95% CI: 88–97). The overall adverse event rate was 4% (95% CI: 3–6). A meta-analysis in 2021, 42 including 21 studies with a total of 1227 SB-ERCP cases, reported a scope insertion success rate of 86.6% (95% CI: 82.4–90.3), a biliary cannulation success rate of 90% (95% CI: 87.1–92.5), and a therapeutic success rate of 75.8% (95% CI: 71.0–80.3). The overall adverse event rate was 6.6% (95% CI: 5.3–8.2).
In summary, DBE and SBE each have distinct advantages and limitations. DBE generally provides superior pleating, stability, and therapeutic success, whereas SBE is less costly, technically simpler, and less preparation (e.g., no balloon attachment).43,44 Thus, scope selection should be tailored to the patient’s anatomy and the procedural goals. Ultimately, it is desirable to establish standardized techniques that maximize the unique advantages of both platforms, based on a thorough understanding of their respective characteristics. 29
Endoscopic papillary procedures: EST, EPBD, and EPLBD
Appropriate papillary intervention is crucial for the safe and effective removal of bile duct stones. Available techniques include EST, 45 EPBD, 46 and endoscopic papillary large balloon dilation (EPLBD). 47 EST is generally the most commonly performed procedure; however, in patients at high risk for bleeding or perforation, EPBD is often considered as an alternative. Comparative studies between EST and EPBD have demonstrated equivalent short-term complete stone removal rates. 48 Moreover, EPBD is associated with better preservation of sphincter function, resulting in significantly lower long-term recurrence rates of bile duct stones and cholecystitis. 49 Nonetheless, early adverse events, particularly post-ERCP pancreatitis, are significantly more frequent in the EPBD group. 50
In addition, endoscopic sphincterotomy followed by balloon dilation has been shown to reduce bleeding risk by limiting the extent of the sphincterotomy incision while still ensuring sufficient papillary opening for stone removal.51,52 This combined approach may also enhance stone clearance rates and reduce the need for mechanical lithotripsy (ML).
In patients with SAA, EST is technically challenging due to the absence of an elevator and the difficulty in orienting the sphincterotome blade toward the oral protrusion (Figure 4). In a randomized controlled trial comparing EST and EPBD in patients with B-II reconstruction, 53 no significant differences were observed in procedural time, ML use, or early adverse events between the two groups; however, post-ERCP bleeding was significantly more common in the EST group. Recently, the development of highly rotatable sphincterotomes has enabled precise and rapid adjustment of the cutting direction, even in cases with altered anatomy (Figure 4). These devices are expected to facilitate safer and more efficient EST during BE-ERCP.

Features and clinical application of the novel sphincterotome (ENGETSU™). This sphincterotome has high rotational performance and dual-action capability. (a) Pull mode extends the blade. (b) Push mode loosens the blade. These functions can be combined to orient the blade in any direction. (c, d) In BE-ERCP for patients with altered anatomy, the blade initially points opposite to the papillary oral protrusion due to scope flexion. By rotating the tip and extending the blade, the blade was successfully aligned with the bile duct axis, enabling biliary cannulation.
For large bile duct stones, EPLBD is often performed to achieve wide dilation, in addition to the use of ML to fragment stones within the bile duct. In cases with surgically altered gastrointestinal anatomy, several studies have reported favorable outcomes of EPLBD, with complete stone removal rates ranging from 96.7% to 100%.54–56 However, the safety profile of EPLBD without preceding EST remains uncertain, as there have been reports of severe acute pancreatitis associated with this approach. 57
Devices for stone removal
Balloon catheters and basket catheters are widely used for stone extraction. While balloon catheters carry no risk of stone impaction, basket catheters are considered to exert a stronger pulling force by directly grasping the stones. Previous comparative studies and guidelines have indicated that both devices offer comparable efficacy and safety.2,3 Therefore, the choice of device should be based on factors such as stone size and number, endoscope maneuverability, and the risk of impaction. In cases involving small stones or a pocket-like configuration of the distal bile duct, both balloon and basket catheters may fail to engage the stones effectively. However, a recently introduced rotatable eight-wire helical basket has shown utility in the removal of small stones,58–61 and future prospective trials or comparative studies against balloon catheters are anticipated.
Peroral cholangioscopy-guided electrohydraulic lithotripsy
For large bile duct stones, treatment typically involves EPLBD followed by mechanical lithotripsy (EML), with stone extraction using a balloon or basket. Recently, however, electrohydraulic lithotripsy (EHL) under POCS has gained attention. In a prospective randomized controlled trial 62 comparing POCS-guided EHL with conventional therapy (Endoscopic mechanical lithotripsy; EML, balloon, or basket) for stones ⩾10 mm in patients with normal anatomy, the stone clearance rate was significantly higher in the POCS-EHL group (93% vs 67%, p = 0.009), despite a longer mean procedure time (120.7 ± 40 min vs 81.2 ± 49.3 min, p = 0.0008), and the adverse event rates were comparable. Furthermore, a network meta-analysis 63 involving 19 RCTs, 2752 patients comparing treatment strategies for large bile duct stones (>10 mm) demonstrated that POCS-EHL had the highest efficacy among all modalities. Given the high cost of POCS-EHL, it is recommended to select between EST + EPLBD, which is more cost-effective and also yields favorable outcomes, and POCS-EHL based on the clinical context.
As the development of the eyeMax 9Fr, which can be used in conjunction with BAE (Figure 5), increasing reports have demonstrated the utility of BE-POCS and BE-POCS-EHL for the diagnosis and treatment of biliary and pancreatic diseases in patients with SAA.64–67 Further accumulation of clinical cases and prospective comparative studies is warranted.
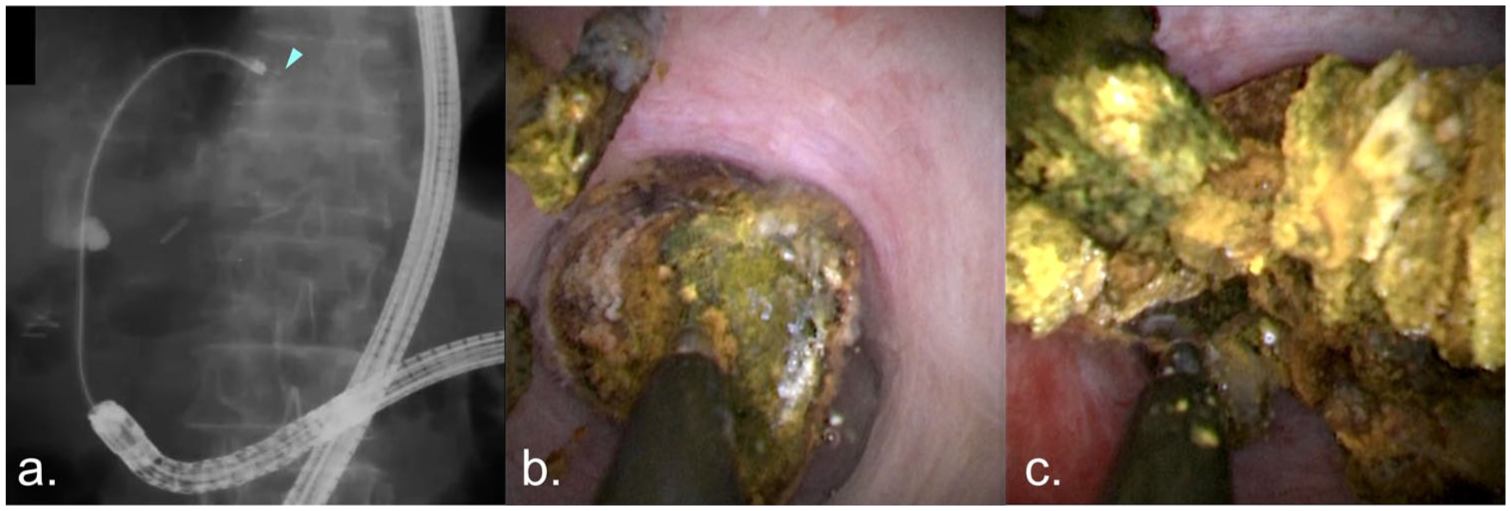
(a) DB-POCS-EHL was performed for the fragmentation of the intrahepatic duct (IHD) stones (arrowhead: the tip of the EHL probe; Autolith Touch, Boston Scientific, MA, USA). (b, c) Utilizing the stable scope maneuverability provided by DB-assist, POCS achieved superior visualization and enhanced operability, enabling the efficient fragmentation of IHD stones with EHL.
BE-ERCP and interventional EUS
Currently, BE-ERCP has spread worldwide and is generally used as the first-line treatment for pancreatobiliary diseases in patients with SAA, regardless of complexity. Interventional EUS is typically performed only when BE-ERCP fails. 29 However, with recent advances in devices and techniques for interventional EUS, there is a growing view that EUS-guided interventions may be a more favorable first-line option due to their shorter procedure time and higher success rates in patients with surgically reconstructed anatomy. 68
In a multicenter retrospective comparative study of biliary drainage for biliary obstruction in patients with SAA, BE-ERCP was associated with advantages such as shorter hospitalization and fewer adverse events. However, EUS-guided biliary drainage (EUS-BD) demonstrated a significantly shorter procedure time and a higher rate of successful biliary drainage. 69 In a retrospective multicenter study of treatment for common bile duct stones in R-Y gastrectomy, although the technical success rates were comparable, BE-ERCP was shown to be a safer approach with fewer required sessions, despite a longer procedure time. Notably, among patients in whom biliary access was achieved, the rate of complete stone clearance was significantly higher in the BE-ERCP group.
These findings suggest that EUS-BD may be preferable when prompt biliary drainage is required, whereas BE-ERCP may be more appropriate when the goal is complete stone removal with fewer procedures and greater safety. 70
Conclusion
BE-ERCP has emerged as the first-line approach for managing bile duct stones in patients with SAA, owing to its high success rates and compatibility with standard ERCP techniques. Short-type balloon endoscopes have significantly improved procedural feasibility by enabling the use of conventional accessories and enhancing maneuverability. Various insertion strategies tailored to surgical reconstruction type, combined with the use of novel devices such as highly rotatable sphincterotomes and slim cholangioscopes, have further expanded the therapeutic scope of BE-ERCP.
Despite its efficacy, BE-ERCP is not without challenges, particularly in cases with R-Y reconstructions or complex anastomoses. In such scenarios, interventional EUS techniques have emerged as viable alternatives, offering shorter procedural times and comparable or superior drainage outcomes. However, BE-ERCP retains an advantage in achieving complete stone clearance with fewer sessions and a favorable safety profile.
Recent advancements in device design, including the development of drill dilators, nonslip dilation balloons, and eyeMax-compatible cholangioscopes, continue to refine the safety and efficacy of BE-ERCP. Future directions should emphasize prospective, comparative studies between BE-ERCP and EUS-guided interventions, as well as the development of standardized algorithms based on anatomical reconstruction and procedural goals.
In conclusion, BE-ERCP remains a cornerstone in the endoscopic management of bile duct stones in altered anatomy, and ongoing innovation will further enhance its clinical utility.
