Abstract
Background:
Assessment of intestinal activity and severity of Crohn’s disease (CD) is crucial to guide treatment. In this study, we aimed to investigate the accuracy of spectral computed tomography (CT) in this assessment and make a comparison with conventional CT.
Methods:
A total of 50 patients with ileocolonic CD underwent spectral CT scanning. Conventional CT and spectral CT images were reconstructed. Endoscopic lesions were classified as absent, mild lesions and severe lesions. Qualitative and quantitative findings in CT images were compared in these segments. Logistic regressions were established, based on conventional and spectral CT parameters, to predict intestinal activity and severity. Comparisons were made by receiver operating characteristic (ROC) curve.
Results:
The results showed that bowel wall hyperenhancement, ulcers on CT images, comb sign, bowel wall thickness, normalized iodine concentration (NIC) and slope of HU curve (λHU) increased significantly (p < 0.01) with endoscopic severity. In predicting intestinal activity, spectral CT demonstrated higher accuracy (99.6% versus 94.7%), sensitivity (99.1% versus 93.4%) and specificity (99.9% versus 94.4%) than conventional CT. In predicting intestinal severity, spectral CT also had higher accuracy (96.5% versus 91.9%), sensitivity (96.5% versus 92.1%) and specificity (95.8% versus 89.8%) than conventional CT. Besides, both NIC and λHU correlated significantly with Simple Endoscopic Score for CD (r = 0.833 and r = 0.771; both p < 0.001), but their correlations with C-reactive protein (r = 0.578 and r = 0.513; both p < 0.01) and Harvey–Bradshaw Index (r = 0.545 and r = 0.522; both p < 0.01) were moderate.
Conclusions:
Compared with conventional CT, spectral CT had higher accuracy in detecting intestinal activity and severity of CD, which could be an alternative choice in evaluation of CD.
Introduction
Crohn’s disease (CD) is a chronic relapsing and remitting inflammatory bowel disease with unknown etiology and its incidence is increasing in China [Zhao et al. 2014]. The evaluation of disease extension and activity is crucial and important to make therapeutic strategy [Tong et al. 2013]. This assessment usually depends on endoscopy. However, sometimes, complete examination through endoscopy is difficult to achieve due to stricture in the intestine. Also, the risks of endoscopy, such as perforation and discomfort, should also be considered [Bodily et al. 2006]. Computed tomography (CT) and magnetic resonance imaging (MRI) have become alternative choices to make assessment of the disease. However, MRI is time consuming and suffers from poor accessibility in some countries. However, CT features rapid screening and is widely available [Wu et al. 2014], though, also has its shortcomings. The averaging attenuation effect of polychromatic X-rays in conventional CT reduces the low-contrast spatial resolution between materials [Lv et al. 2011].
Spectral CT, a novel CT scanning mode, has been recently introduced, which could improve lesion detection and enhance image quality. It uses dual-energy X-rays produced by the rapid switching of high and low energy, which produces material-decomposition images (e.g., water- and iodine-based material-decomposition images) and monochromatic spectral images with energy ranging from 40 to 140 keV. The material-decomposition images can be used to estimate, quantitatively, the water and iodine content in lesions and normal tissues [Lv et al. 2011]. Its clinical value has been increasingly investigated, including staging of gastric cancer [Pan et al. 2013], differentiation of thyroid nodules [Li et al. 2012], detection of insulinomas [Lin et al. 2012], and characterization of liver lesions [Lv et al. 2011; Wang et al. 2014].
Recently, no studies focus on the application of spectral CT in evaluation of CD. In this study, we aimed to assess the activity of CD with the aid of spectral CT and make a comparison with conventional CT.
Methods
Patients
The Ethics Committee of Renji Hospital affiliated to Shanghai Jiao Tong University School of Medicine approved this study, and written informed consent was obtained from all patients. Methods were carried out in accordance with the approved guidelines. From January 2015 to December 2015, 50 patients with a confirmed diagnosis of ileocolonic CD were prospectively studied. They all underwent ileocolonoscopy and spectral CT scanning. They also had blood samples obtained for analysis of C-reactive protein (CRP) concentration. All of the examinations were conducted within 5 days. Clinical activity of CD patients was assessed using the Harvey–Bradshaw Index (HBI) [Harvey and Bradshaw, 1980].
Endoscopic procedure
Ileocolonoscopy was considered as the reference standard for the evaluation of CD extension and activity. The endoscopy was conducted by two senior gastroenterologists who had more than 10-years’ experience in endoscopy. Patients were asked to undertake bowel cleansing with polyethylene glycol (PEG, Wanhe Inc., Shenzhen, China) solution 4 hours before the examination. The endoscopic severity of CD was evaluated by Simple Endoscopic Score for Crohn’s Disease (SES-CD) [Sostegni et al. 2003]. The variables of SES-CD include presence of ulcers, ulcerated surface, affected surface, presence of narrowings, and number of affected segments. Terminal ileum, ascending colon, transverse colon, descending colon, sigmoid colon and rectum were respectively scored. The endoscopists completed the scoring system immediately after examination. The results were in consensus with each other. Then, they divided each segment into three categories according to the lesion severity: (1) absence of lesion; (2) mild lesions: inflammatory lesions without ulceration, such as edema, erythema or pseudopolyps; (3) severe lesions: superficial or deep ulcers, or accompanied with stenosis or fistula. When more than two lesions existed at a single segment, the classification was made based on the most severe lesion.
Computed tomography examination
Patients fasted for over 8 hours before CT examinations and took 2000 ml solution of PEG for bowel preparation. At 45 minutes before scanning, an additional 1000 ml PEG solution was administered orally to each patient for small bowel distention. Patients who could not tolerate the full volume of luminal contrast were asked to drink 750–1000 ml of the same solution as it was enough to obtain optimal distension. To reduce bowel peristalsis, 20 mg of anisodamine was administered intravenously just before the examination. The spectral CT scanning was performed by multi-phase CT, in spectral-imaging mode, with fast-tube voltage switching between 80 and 140 kVp on adjacent views during a single rotation, which used a Discovery CT750 HD CT scanner (GE Healthcare, Waukesha, Wisconsin). Other scanning parameters were as follows: collimation thickness of 0.625 mm, tube current of 600 mA, rotation speed of 0.6 seconds and helical pitch of 0.983. Patients were injected by iodinated nonionic contrast material (Iopamidol, 370 mg/ml; Shanghai Bracco Sine Pharmaceutical, China) with a rate of 4 ml/second and 1.5 ml/kg of body weight. Single-phase scanning during the enteric phase was performed after a 45-second delay. The CT images were reconstructed by using projection-based material-decomposition software and a standard reconstruction kernel. Three types of images were reconstructed for analysis: conventional polychromatic images obtained at 140 kVp, iodine- and water-based material-decomposition images (Figures 1a and 1b), and monochromatic images obtained at energies ranging from 40 to 140 keV (Figures 1c and 1d).

Marked bowel wall hyperenhancement in ascending and descending colon (arrows) in a 30-year-old female with Crohn’s disease.
Computed tomography image analysis
Two experienced radiologists reviewed conventional polychromatic images, iodine- and water- based material-decomposition images and monochromatic images. They had consensus with each other. They were blind to patient information, location of lesions and results of endoscopy. Six segments used in endoscopic analysis were also applied in CT analysis. Bowel wall hyperenhancement (defined as segmental hyperenhancement of all, or part of the bowel wall, greater than that of the adjacent bowel wall), bowel wall thickness (mm), mucosal ulceration (defined as deep depressions in the mucosal surface), enlarged (>1 cm) regional mesenteric lymph nodes and comb sign (defined as regional dilation of the vasa recta) were assessed in conventional CT mode.
The spectral CT images were analyzed by GSI Viewer software 4.4 (GE Healthcare, Waukesha, Wisconsin). Circular or elliptical regions of interest (ROIs) were placed on the iodine-based material-decomposition images and encompassed as much of the high-enhancing areas of the lesions as possible. To ensure consistency, three consecutive slices were measured and the average values were calculated. The measured iodine concentration divided by iodine concentration in the artery was the normalized iodine concentration (NIC), which was used with the aim of minimizing differences in patients, scanning times, and iodine concentrations. Slope of HU curve (λHU), which represented X-ray attenuation coefficient at different energy levels, was calculated using the following formula [Li et al. 2012; Wu et al. 2014]:
Statistics
SPSS 18.0 software for windows was used to analyze the data. Comparisons for qualitative CT findings were measured by chi-square test. Comparisons for quantitative measures were tested using analysis of variance (ANOVA) followed by the Bonferroni post hoc test. Logistic regression was used to find which parameter had independent value to predict intestinal activity (both mild and severe lesions) and intestinal severity, respectively. Receiver-operating characteristic (ROC) curve was used to evaluate the accuracy of the regression model. Both parameters in conventional CT mode and spectral CT mode were used to establish the regression equation and comparisons were also made. Threshold value, area under receiver-operating characteristic (AUROC) curve, accuracy, sensitivity, specificity, positive and negative predictive value (PPV, NPV) and positive and negative likelihood ratios (LR+, LR−) were calculated. Correlations of NIC and λHU with SES-CD, CRP concentration and HBI were measured by Spearman’s rank correlation. p < 0.05 was considered statistically significant in all reported p values.
Results
The characteristics of the 50 patients
A total of 50 patients with ileocolonic CD were included in our study. The detailed information of these patients is listed in Table 1. There were 23 females and 27 males. Of these, 17 patients were in clinical remission (HBI ⩽ 4), and 33 patients had active disease (HBI > 4). Complete ileocolonoscopy was achieved in 47 patients. The reason for failure was due to severe stenosis (n = 3). Consequently, a total of 282 bowel segments were evaluated under endoscopy. Of them, 176 segments were absent from lesion, 38 segments had mild lesions and 68 segments had severe lesions. All colonic segments reached an adequate distension for CT analysis and the acquired images were in good quality. Tolerance of CT examination was mostly positive.
Clinical and biological characteristics of the 50 patients.

IQR, interquartile range; 5-ASA, 5-acetylsalicylic acid; TNF, tumor necrosis factor; CRP, C-reactive protein; SES-CD, Simple Endoscopic Score for Crohn’s disease.
Qualitative computed tomography image analysis
The major qualitative findings are listed in Table 2. The comparison of intestinal segments with absent, mild and severe lesions demonstrated a progressive and significant increase in bowel wall hyperenhancement, ulcers on CT images and comb sign. Bowel wall hyperenhancement was detected in 98.5% of severe lesions, which was significantly higher than that in mild lesions (86.8%) and endoscopically normal segment (4.5%). Ulcers at CT images were observed in 70.6% of severe lesions, while they were only detected in 15.8% of mild lesions and 2.8% of endoscopically normal segments. The presence of comb sign had higher occurrence in severe lesions (55.8%) when compared with mild lesions (31.6%) and endoscopically normal segments (6.8%). Enlarged lymph nodes had higher occurrence in severe lesions (41.2%) and mild lesions (28.9%) than that in endoscopically normal segments (5.1%). However, no significant difference was observed between mild and severe lesions (p = 0.294).
Differences of qualitative findings in conventional computed tomography (CT) images by chi-square test according to endoscopic severity.

p values for comparisons between endoscopically normal segments and mild lesions.
p values for comparisons between mild lesions and severe lesions.
Quantitative computed tomography image analysis
Quantitative parameters such as bowel wall thickness, NIC and λHU were also associated with endoscopic severity (Figure 2). The bowel wall thickness in mild lesions was significantly greater than that in endoscopically normal segments (4.62 ± 2.33 mm versus 1.83 ± 0.64 mm; p < 0.001). The bowel wall thickness in severe lesions was also significantly greater than that in mild lesions (7.18 ± 2.94 mm versus 4.62 ± 2.33 mm; p < 0.001). There were significant differences in NIC between endoscopically normal segments and mild lesions (0.16 ± 0.04 mg/ml versus 0.33 ± 0.08 mg/ml; p = 0.002), and between severe lesions and mild lesions (0.44 ± 0.06 mg/ml versus 0.33 ± 0.08 mg/ml; p < 0.001). The λHU increased significantly in mild lesions when compared with endoscopically normal segments (2.95 ± 0.53 versus 1.4 ± 0.43; p < 0.001), and was also significantly higher in severe lesions than in mild lesions (4.1 ± 0.67 versus 2.95 ± 0.53; p < 0.001). The example of λHU is shown in Figure 3.

Boxplots of quantitative parameters.

The graph depicts the changes of the HU curve in endoscopically normal segments, mild lesions and severe lesions.
Predictive parameters for activity and severity of Crohn’s disease
Parameters in conventional CT and spectral CT were used to make logistic regressions to predict intestinal activity and severity. The accuracy of prediction was compared using the ROC curve.
In conventional CT mode, bowel wall hyperenhancement, bowel wall thickness, ulcers on CT images, comb sign and enlarged lymph nodes were included as independent variables. In prediction of intestinal activity, bowel wall hyperenhancement and bowel wall thickness were independent predictors, both p < 0.001 (Table 3). The regression equation was:

Independent parameters of conventional computed tomography (CT) to predict intestinal activity and severity.

OR, odds ratio; CI, confidence interval; CT, computed tomography.
The threshold value was 0.351. The area under ROC curve was 0.978, with accuracy of 94.7%, sensitivity of 93.4%, specificity of 94.4%, PPV of 90.9% and NPV of 95.9%. In prediction of intestinal severity, bowel wall hyperen-hancement (p < 0.001), bowel wall thickness (p < 0.001) and ulcers at CT images (p < 0.001) were independent predictors (Table 3). The regression equation was:
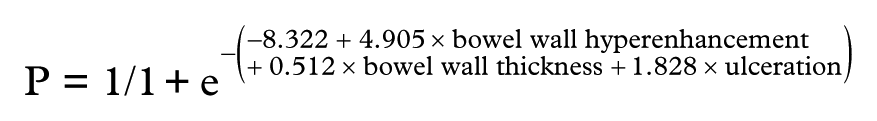
The threshold value was 0.338. The area under ROC curve was 0.971, with accuracy of 91.9%, sensitivity of 92.1%, specificity of 89.8%, PPV of 74.1% and NPV of 97.3%.
In spectral CT mode, NIC and λHU were included as independent variables. In prediction of intestinal activity, both NIC (p = 0.009) and λHU (p = 0.016) were independent predictors (Table 4). The regression equation was:

Independent parameters of spectral computed tomography (CT) to predict intestinal activity and severity.

OR, odds ratio; CI, confidence interval; NIC, normalized iodine concentration; λHU, slope of the HU curve.
The threshold value was 0.497. The area under ROC curve was 0.999, with accuracy of 99.6%, sensitivity of 99.1%, specificity of 99.9%, PPV of 99.8% and NPV of 99.5%. In prediction of intestinal severity, NIC (p = 0.001) and λHU (p < 0.001) were also independent predictors (Table 4). The regression equation was:

The threshold value was 0.332.The area under ROC curve was 0.991, with accuracy of 96.5%, sensitivity of 96.5%, specificity of 95.8%, PPV of 87.9% and NPV of 98.9%.
The results showed that compared with conventional CT mode, the regression equation produced by parameters in spectral CT had higher accuracy, sensitivity, specificity, PPV and NPV in prediction of both intestinal activity and severity (Table 5 and Figures 4 and 5).
Comparisons of logistic regressions based on conventional and spectral computed tomography (CT) to predict intestinal activity and severity.

CT, computed tomography; AUROC, area under receiver-operating characteristic curve; PPV, positive predictive value; NPV, negative predictive value; LR+, likelihood-ratio positive; LR−, likelihood-ratio negative.

Receiver-operating characteristic curves of conventional computed tomography (CT) and spectral CT to predict intestinal activity (a) and severity (b) under endoscopy.

A 25-year-old male with Crohn’s disease.
Correlation between parameters in spectral computed tomography and clinical markers
Global values of NIC and λHU were calculated by adding their values in ileum, ascending, transverse and descending colon, sigmoid colon and rectum. We then evaluated their correlations with SES-CD, CRP and HBI. Both NIC (r = 0.833; p < 0.001) and λHU (r = 0.771; p < 0.001) had significant correlation with SES-CD. Segmental SES-CD, segmental NIC (r = 0.86; p < 0.001) and λHU (r = 0.812; p < 0.001) also had significant correlations with it. NIC correlated significantly but moderately with CRP (r = 0.578; p < 0.01). λHU also had a moderate correlation with CRP (r = 0.513; p < 0.01). Both NIC (r = 0.545; p < 0.01) and λHU (r = 0.522; p < 0.01) correlated moderately with HBI.
Discussion
The primary characteristic of CD lesion is its skip pattern. The applications of CT and MRI have a key role in the assessment of CD. Compared with CT, MRI is less available and time consuming. However, conventional CT uses polychromatic X-rays, which could result in beam-hardening artifacts and averaging attenuation effects [Boll et al. 2010]. Beam hardening caused by the preferential absorption can shift the attenuation of a material in the scanning field of view within a patient, or between patients. Because of beam-hardening artifacts, attenuation values are sometimes unreliable for verification of small lesions [Lv et al. 2011]. Recently, spectral CT, a new CT scanning mode, could switch rapidly between high and low energy. It enables the creation of monochromatic spectral images at energy levels ranging from 40 to 140 keV. Besides, the detector of spectral CT features energy-sensitive photon-counting abilities, which allows the classification of detected X-ray photons into energy bins. By recognizing tissue- and material-specific energy distributions, the creation of selective material-decomposition images could be achieved [Boll et al. 2010; Lv et al. 2011]. Water and iodine are often selected as the basis material-decomposition pair, because their atomic numbers cover the range of atomic numbers for materials generally found in medical imaging and those of soft tissue. The monochromatic image depicts how the imaged object would look if the X-ray source produced only X-ray photons at a single energy. Therefore, spectral CT could reduce the beam-hardening artifacts and averaging attenuation effects commonly seen in the conventional CT scan [Pan et al. 2013; Yu et al. 2013]. Also, the radiation output of the spectral CT scanner, in terms of volume CT dose index, was between 16 and 18 mGy, which was comparable with 14–17 mGy for conventional CT enterography. Therefore, spectral CT improved the accuracy of evaluating intestinal activity and severity without increasing radiation dose. Besides, compared with first-generation, the new generation of spectral CT features lower lose of radiation (0.15 mGy), which could also acquire good image quality in diagnosis of pulmonary disease [Newell et al. 2015]. It will open up new diagnostic and research opportunities in CT phenotyping.
In our study, we classified bowel segments into three categories, namely, endoscopically normal segment, mild lesions and severe lesions according to endoscopic examinations. Qualitative findings, such as bowel wall hyperenhancement, ulcers on CT images and comb sign progressively increased with endoscopic severity. Colombel and colleagues and Tong colleagues also found that bowel wall hyperenhancement significantly correlated with endoscopic severity [Colombel et al. 2006; Tong et al. 2013]. Meyers and McGuire regarded tortuosity and dilatation of the ileal vessels as ‘vascular jejunization of the ileum’ or the ‘comb sign,’ suggesting the occurrence of this finding in patients with CD [Meyers and McGuire, 1995]. Colombel and colleagues also indicated that the presence of the ‘comb sign’ was associated with endoscopic severity [Colombel et al. 2006]. In terms of enlarged lymph nodes, there was a significant difference between lesions and normal mucosa. But, the difference did not exist between mild and severe lesions.
In regard to quantitative findings, bowel wall thickness also increased with the endoscopic severity, which was consistent with a previous study [Tong et al. 2013]. We also tried to make quantitative analysis in spectral CT mode. Knowing how a substance behaves at two different energies can provide information about tissue composition beyond that obtainable with single-energy techniques [Coursey et al. 2010]. Spectral CT is capable of extracting quantitative information about the elemental and molecular composition of tissue and contrast materials based on their attenuation properties. The iodine concentration in lesions derived from the iodine-based material-decomposition images is quantitative, and thus might be a useful parameter [Boll et al. 2010; Lv et al. 2011]. In our study, we found NIC increased with endoscopic severity. NIC was significantly higher in severe lesions than in mild lesions. There was also a significant difference between mild lesions and endoscopically normal segments. HU curves could be automatically generated for given ROIs, describing the dynamic change of measured CT Hounsfield units of ROIs against increasing keV values within the range of 40–140 keV. Each tissue has its own characteristic curve [Li et al. 2012]. Wang and colleagues reported that the λHU could be used to differentiate among hemangioma, hepatocellular carcinoma, metastasis and simple cysts [Wang et al. 2014]. In our study, we found that the λHU paralleled with endoscopic severity. The λHU significantly increased in severe lesions when compared with mild lesions, and was also significantly higher in mild lesions than in endoscopically normal segments.
Detecting intestinal activity and severity is critical, because the presence or persistence of ulcerative lesions is relevant to disease course and surgical requirements [Allez et al. 2002]. So, we decided to use parameters in conventional CT and spectral CT to establish logistic regressions and to see which mode was better in predicting intestinal activity and severity. In predicting intestinal activity, bowel wall hyperenhancement and bowel wall thickness were independent predictors in conventional CT mode. Both NIC and λHU were independent predictors in spectral CT mode. Compared with conventional CT, accuracy, sensitivity and specificity in spectral CT mode increased from 94.7% to 99.6%, 93.4% to 99.1% and 94.4% to 99.9%, respectively. In predicting intestinal severity and bowel wall hyperenhancement, bowel wall thickness and ulcers on CT images were independent predictors in conventional CT mode. Also, both NIC and λHU were independent predictors in spectral CT mode. Spectral CT featured greater accuracy (96.5% versus 91.9%), sensitivity (96.5% versus 92.1%) and specificity (95.8% versus 89.8%) than those in conventional CT mode, as well. As a result, quantitative measurement in spectral CT mode could produce satisfactory results and detect severe lesions in endoscopy more precisely.
Our study found significant correlation between NIC, λHU and SES-CD. It further proved that these two quantitative parameters could be used as alternative parameters to assess endoscopic severity. CRP is not a specific biomarker to monitor CD activity. It correlates moderately well with clinical, endoscopic, histologic, and radiographic disease activity [Papay et al. 2013]. In our study, we also found CPR correlated moderately with NIC and λHU. NIC and λHU demonstrated moderate correlations with HBI. The moderate correlations we observed were most likely due to the HBI result depending on several other variables in the scoring system.
There are some limitations of this study. First, this investigation reflects our preliminary experience with a relatively small number of patients. Further clinical trials need to prove our results. Another limitation is the lack of validation of the results in an independent cohort. Third, this study was focused on the use of quantitative information generated by using CT spectral imaging. In the future, qualitative assessment of iodine- and water-based images could be added to evaluate their clinical value. Additionally, the changes of parameters in spectral mode in response to the treatment should be investigated in future. Last but not least, the selection of size and placement of the ROIs were arbitrary. Measurement deviation of NIC and λHU cannot be absolutely avoided.
In conclusion, spectral CT had good performance in evaluation of CD activity. Compared with conventional CT, the administration of spectral CT could be an alternative choice to endoscopy in the assessment of CD.
Footnotes
Acknowledgements
Jiang Chen Peng and Qi Feng contributed equally to this article.
Funding
This work was supported by the National Science Foundation of China (grant numbers 81470820 and 81370508).
Conflict of interest statement
None of the authors has any potential conflicts of interest related to this article to declare and the results of this report have been produced, analyzed, and interpreted without any outside participation.

