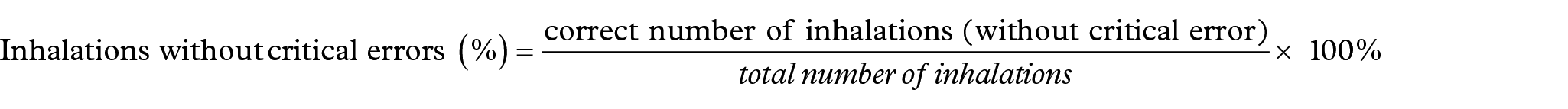Abstract
Background:
Asthma is a chronic condition with a high health and social burden in children. Although many well-studied effective therapies are available, because of suboptimal adherence and inhalation technique, asthma in children remains frequently uncontrolled. It is often assumed that adherence and technique are highly correlated items, but this assumption has not been thoroughly validated.
Objective:
This trial evaluates the correlation between adherence and inhalation technique and the association of patient-related factors with these two important parameters.
Design:
Observational phase I of the IMproving Adherence by Guiding INhalation via Electronic monitoring (IMAGINE) study, a three-phased Randomized Controlled Trial (RCT) in children with uncontrolled asthma.
Methods:
The observational phase I of the IMAGINE study was designed to determine the correlation between adherence and inhalation technique in pediatric subjects with uncontrolled asthma. During this observational study phase, adherence and inhalation technique were measured with a smart add-on device called Respiro© (Amiko, London). Patient-related factors were assessed either at baseline (e.g. characteristics of the patient), or during the study period (e.g. number of emergency room (ER) visits and daily salbutamol intake).
Results:
Of the 34 enrolled subjects, 6–18 years old, suffering from moderate to severe uncontrolled asthma, 32 successfully completed phase I. No significant correlation between adherence and inhalation technique was observed (r = −0.21; p = 0.234). Twenty-one percent of children had both good adherence and good inhalation technique. Children with good adherence had more often ⩾1 ER visits during follow-up, while poor inhalation technique was associated with younger age and lower height at baseline, and a higher daily salbutamol dosage intake and ⩾1 ER admission during follow-up.
Conclusion:
Our findings demonstrated no correlation between therapy adherence and inhalation technique, suggesting that these should be regarded as distinct and frequent pitfalls of inhaled medication use.
We observed that inhalation technique was significantly associated with ER visits, rescue medication use, age, and height, while good adherence correlated with ER visits. Recognizing these factors allows pediatricians to identify risk profiles for poor inhalation technique and poor adherence, enabling more targeted and personalized interventions.
Trial registration: NL-OMON25807.
Keywords
Introduction
Asthma is a common chronic condition in children, characterized by airflow limitation. 1 Despite the availability of a wide range of medications, a significant proportion of children—up to 50%—continue to experience uncontrolled asthma. 2 This imposes a substantial health, economic, and social burden worldwide. 3
Poor adherence to inhaled controller therapy and inadequate inhalation technique are critical challenges that must be addressed when managing uncontrolled asthma in children. 4
Adherence rates in asthma range from 49% to 71% in children, exhibit considerable variability, and tend to decrease during over time. 5 Poor adherence is associated with poor disease control, reduced lung function, increased reliance on oral steroids, and higher hospital readmission rates. 6 Additionally, inhalation technique among children is often suboptimal, with studies reporting that the proportion of children correctly performing all steps of inhaler use ranges from 0% to 55%. A Dutch study found that good adherence to medical therapy, defined as >80% adherence, was associated with significantly better asthma control. 7
The Global Initiative for Asthma (GINA) guidelines recommend evaluating both adherence and inhalation technique before considering step-up therapy, such as targeted biologics. 1
Multiple techniques available for monitoring adherence are available. However, these methods are often unreliable and seem to overestimate therapy adherence rates.6,8 Most commonly used monitoring techniques include patient self-reports and pharmacy prescription records. However, patient self-reporting is prone to recall bias and social desirability bias, leading to overestimating adherence. Pharmacy prescription records provide information on prescription collection, but do not confirm whether the medication is taken as prescribed and in used the correct way. 8 Furthermore, in the short term, pharmacy prescription records may be unreliable due to a large number of doses in each inhaler. Electronic monitors provide an objective assessment of adherence and are considered the gold standard. 9 However, most of the electronic monitors only report whether the inhaler has been used, and they do not assess whether it was used correctly.9,10
In this study, we use a smart add-on device, the Respiro© (Amiko, London). 11 This device records the date and time of inhaler use and evaluates various aspects of inhalation technique.
Previous studies have identified multiple patient-related factors associated with either therapy adherence or inhalation technique. However, these studies have primarily relied on patient-reported adherence, self-reported inhalation technique, or physician-observed assessments in clinical settings.12 –14 Furthermore, the relationship between therapy adherence and inhalation technique remains poorly understood. In many healthcare settings, it is commonly assumed that adherence and technique are closely correlated, but this assumption has not been thoroughly validated. Clinicians often hypothesize that poor inhalation technique contributes to poor adherence, either through underuse or overuse of inhalation medication. Some studies suggest that incorrect inhaler technique may be an unintentional factor contributing to poor adherence. 15 To address this issue effectively, it is crucial for healthcare professionals to better understand the relationship between adherence, inhalation technique, and asthma control.
By using the smart add-on device in a home setting, we expect to obtain a more representative assessment of the interrelationship between patient-related factors, therapy adherence, and inhaler technique errors.
The IMproving Adherence by Guiding INhalation via Electronic monitoring (IMAGINE) Study investigates therapy adherence and inhalation technique in children with uncontrolled asthma as well as their relationship with patient-related factors and clinical outcomes. While literature and clinical practice do not consistently align on this topic, it is often assumed that adherence and inhalation technique are closely linked in asthma management. In the observational phase (Phase I) of this study, we hypothesized that adherence and inhalation technique are not directly related. Additionally, we aimed to identify specific parameters in children that serve as risk factors for poor or good adherence and inhalation technique.
Methods
This study was part of the three-phase IMAGINE study 16 (see Figure 1). This manuscript reports on the observational phase I. The STROBE guideline was followed (Strengthening the Reporting of Observational Studies in Epidemiology; see Supplemental Appendix A). 17 and registered with the Clinical Trials Registry Platform (NL-OMON25807). 18 Recruitment took place from October 2019 through October 2023.

Overview of the three phases including the parameters which will be assessed. T0 is the start of phase I, T1 is the end of phase I and start of phase II (study visit), etc.
Study population
We asked outpatient children from a large teaching hospital in Enschede, The Netherlands, and diagnosed with uncontrolled moderate to severe asthma, to participate in the IMAGINE study. We considered their asthma uncontrolled based on the (childhood) asthma control test (c-)ACT score lower than 20 (see Supplemental Appendices A and B), and/or lung function reversibility on short acting bronchodilator of at least 12%. Reversibility was defined as percentage change from prebronchodilator to postbronchodilator in the absolute value of FEV1. 19
Inclusion and exclusion criteria
All participants were between 6 and 18 years old and had uncontrolled moderate to severe asthma. They were outpatients at a large teaching hospital in the Netherlands. Asthma was classified as uncontrolled if the (childhood) Asthma Control Test (c-)ACT score was below 20 and/or if lung function showed a reversibility of at least 12% following short-acting bronchodilator administration. Moderate to severe asthma was diagnosed by a pediatric pulmonologist based on the clinical need for daily controller medication to prevent frequent symptoms and/or exacerbations.
The Respiro© device had to be compatible with the participants’ controller medication, which was feasible for the Nexthaler©. A switch from a metered-dose inhaler to a dry powder inhaler was permitted, provided that the medication remained unchanged. Before study enrolment, participants were required to use this dry powder inhaler for at least 1 month.
Children, or their parents (if the child was under 12 years old), had to be proficient in Dutch to participate. Exclusion criteria included children with chronic pulmonary conditions or other disorders that could potentially affect lung function.
Study design
This is an observational study, phase I of the IMAGINE study, a three-phase RCT in children with uncontrolled asthma. During the baseline visit participants filled in the (c)ACT questionnaire, demographic data were collected, and they were provided with the Respiro© (Amiko, London) and a handheld spirometer (AirNext©, NuvoAir, Stockholm, Sweden). The Respiro© was only used for monitoring adherence and inhalation technique, and subjects received no feedback during phase I of the study that lasted for 4 weeks. With the handheld spirometer, reversibility was measured during the baseline visit. Subjects were asked to withhold from their bronchodilator medication for 12–24 h before the measurement. Salbutamol 200 µg was used as bronchodilator, administered without valved holding chamber, with nose clip. Subjects measured spirometry bi-weekly at home. For this spirometry at home, subjects received an extensive education from the researcher during the first visit. At every study visit, reversibility was measured under supervision and the (c-)ACT questionnaire was completed.
Primary and secondary objectives
The primary outcome for this observational part of the IMAGINE study was the correlation between therapy adherence and inhalation technique. Therefore, to measure adherence, date and time of inhalation were registered. For measuring the inhalation technique, the orientation of the device during inhalation, peak flow, the duration of the inhalation, the total volume, and opening and closing of the device were registered by the Respiro©. 16
Subjects were considered to be fully adherent if they took as many inhalations each day as prescribed. Therefore, adherence can be calculated by actual medication intake divided by the prescribed intake per day.
Good adherence was defined as taking 75%–125% of all prescribed inhalations. The non-adherent group consists of both under-users, people taking <75% of all prescribed inhalations, and over-users, people taking >125% of all prescribed inhalations. 20
Furthermore, inhalation technique was assessed through two critical errors: peak inspiratory flow <30 L/min 21 and inhalation duration <1 s. 22 Orientation was considered a non-critical error, where orientation is regarded poor if the device deviates more than 45 degrees from the optimal position. Opening and closing of the inhaler were also assessed; the Respiro© device only activates with correct opening of the device.
Inhalation technique was calculated as a percentage of correct inhalations, by dividing the number of inhalations performed correctly without any critical errors, by the number of inhalations performed in total. Good inhalation technique was defined as taking ⩾80% of inhalations without critical errors.
The secondary outcomes for this observational part of the study were patient factors, associated with poor adherence and/or incorrect inhalation technique. The studied factors that were measured at baseline included weight, height, gender, age, number of siblings, educational status, living environment, smoking behavior of parents, sports, baseline lung function, and baseline (c) ACT-score. Other factors (hospital admissions, number of emergency room visits, and number of no-shows) were measured during the active study participation, and prescription refill rates of asthma medication were calculated from pharmacy records from participants’ local pharmacy.13,14,23 –25
The Respiro©
The Respiro© device analyzes vibration patterns associated with inhaler use, enabling the identification of critical inhalation errors such as insufficient peak inspiratory flow, inadequate inhalation duration, and incorrect inhaler orientation. The device utilizes an accelerometer to estimate inhalation flow and detect inhaler orientation.
The accelerometer measures acceleration forces, which determine orientation relative to gravity. In the case of Respiro©, the accelerometer detects changes in motion and position, allowing the system to assess the inhaler’s orientation during use. Additionally, the same sensor captures small vibrations and movements associated with inhalation, facilitating the estimation of inhalation flow.
For further details, refer to the schematic illustration of the Respiro© device in Supplemental Appendix D.
Sample size calculation
The sample size calculation of 68 children for the IMAGINE study has been reported in detail in the protocol article. 16 Since this was an assessment based on limited literature, we included an interim analysis after 34 subjects in the protocol, with stopping rules for effectiveness and futility. 26 The study was stopped for futility after the interim analysis. Therefore, data of 34 subjects are included in the current analysis.
Statistical analysis
Baseline characteristics are displayed as means with standard deviations (SDs) or medians with interquartile range (IQR) for continuous variables depending on the distribution of the variable; categorical variables are displayed as number with corresponding percentages. To determine whether there is a relation between therapy adherence and inhalation technique, a scatterplot was made and the Spearman Rho correlation test was performed. To determine patient-related factors associated with poor adherence and/or incorrect inhalation techniques, univariate analyses were performed, as appropriate, using an unpaired T-test, Mann Whitney U test, or Fisher Exact test, and Relative risks were calculated with descriptive cross-tabulation. Due to the small number of children within each category, no multivariate analysis was carried out. Statistical analysis was carried out using the IBM SPSS statistical package (IBM Corp, Armonk, NY, USA, version 29).
Results
Baseline characteristics
A total of 62 children were screened for inclusion. The flowchart in Figure 2 describes the inclusion of the study population. Table 1 shows the demographic parameters of the total study population in the first column. The group had a mean age of 11.7 (±2.7) years, and there were more male (72%) than female children included in this study. From their registered comedication, we found that 67% of the population used nasal corticosteroids and 45% used salbutamol, with a median dosage of 200 mg (IQR 0–700 mg). The included children participated in 68% of the cases in additional sports activities next to physical education from school. Parents of 37% of the included children have a smoking habit. All children used Foster Nexthaler© as their standard inhaler for controller medication.

Flowchart of study population.
Overview of patient characteristics for adherence (good and non) and inhalation techniques (poor and good).

Physical education.
The median therapy adherence for all subjects was 77% (IQR 34–96). In total, 16 children were categorized as adherent (50%) and 16 as non-adherent (50%); 1 of these 16 was qualified non-adherent because of overuse (>125%). The median percentage of inhalations without critical errors (inhalation technique) for all children was 83% (IQR 60–100). Seventeen subjects (53%) were categorized with a good inhalation technique and 15 (47%) with a poor inhalation technique.
Correlation between inhalation technique and therapy adherence
Spearman’s Rho correlation test showed a non-significant negative correlation coefficient of −0.21 (p = 0.234), between inhalation technique and therapy adherence (Figure 3). Only seven children (21%) are both adherent and have a good inhalation technique (upper right quarter of the figure).

Scatterplot showing the correlation between adherence and inhalation technique, with reference lines separating good and poor scores.
Factors associated with adherence and inhalation technique
Table 1 shows the distribution of the patient-related factors in the groups, based on adherence and inhalation technique and their significance.
The category one or more ER admissions was significantly higher in the adherent versus non-adherent group; adherent children are 11 times more often admitted to the ER (RR = 11; 95% CI 1.60–75.5) during follow-up. A higher age and height at baseline were significantly related to a good inhalation technique, while higher salbutamol dosage and ER admissions during follow-up were significantly related to a poor inhalation technique. Finally, children with a poor inhalation technique have a 3.4 (95% CI 1.12–10.3) times higher probability of one or more ER admissions during follow-up, compared to those with a good inhalation technique. Other patient parameters did not show a significant association with either adherence of inhalation technique.
Discussion
In this phase of the IMAGINE study, we found no correlation between therapy adherence and inhalation technique in children aged 6–18 years using the Respiro™ add-on device. These results highlight the importance of considering adherence and inhalation technique as distinct pitfalls in asthma therapy. Furthermore, we identified significant correlations between factors such as height and age with a good inhalation technique. Poor inhalation technique was associated with a higher frequency of emergency room (ER) visits and increased salbutamol use, while good adherence was also linked to one or more ER visits.
Given the lack of correlation between adherence and inhalation technique, these two aspects of inhaled medication use should be regarded as independent factors requiring different intervention strategies. In this study, we showed that only 21% of the children are both adherent and using a good inhalation technique. This low percentage emphasizes the importance of repeated instructions and close supervision to optimize asthma management in children with uncontrolled disease according to GINA guidelines. 1 Healthcare professionals, including pharmacists, can play a crucial role in addressing these challenges. We anticipate that the use of eHealth technologies and smart devices could improve inhalation technique by providing real-time feedback to both children and their caregivers. When younger children struggle to achieve correct technique, pediatricians and pharmacists should consider alternative delivery methods, such as spacers, to optimize inhalation therapy.
Our study identified patient-related factors associated with therapy adherence and inhalation technique. In the adherent group, ER visits were significantly more frequent. Children with good inhalation technique were generally older and taller, whereas those with poor inhalation technique had significantly higher salbutamol use and more frequent ER visits. These findings have clinical implications, offering healthcare workers valuable insight into the management of inhalation therapy. Interestingly, the finding of a significant association between ER visits and adherence is contrasts to previous studies, which have reported that good adherence to therapy reduces the risk of exacerbations.6,14 At first glance, this finding may appear contradictory, but it is plausible that children become more adherent following an ER visit due to increased illness awareness. Another possible explanation is that children with more severe or uncontrolled asthma—who experience frequent exacerbations and ER visits—are more reliant on their medication. Both scenarios suggest that an increased engagement with treatment could lead to improved adherence. 27
Conversely, we observed that children with a poor inhalation technique were more likely to have one or more ER visits. If the inhalation technique is inadequate, the inhaled medication may not effectively reach its target areas in the lungs, contributing to poor disease control despite adequate adherence. This finding underscores the importance of focusing on inhalation technique in both acute and follow-up care. Additionally, hospital-based instruction does not always translate to correct inhaler use at home. 28 Therefore, we have to consider integrating digital apps and add-on devices on the inhaler providing ongoing guidance in a home setting, offering feedback directly to children or their caregivers.
Children age and height, likely correlated, were significant predictors of good inhalation technique. Previous research suggests that the quality of inhaler use improves with age and experience. 29 The ability of following instructions, whether verbal or digital, is important in the asthma management, making age a key determinant of inhalation technique. This emphasizes the importance of strict supervision for the younger children throughout the entire inhalation procedure, with active involvement of parents and, where appropriate, digital health tools for real-time feedback. Pharmacy staff, in particular, can play a key by providing frequent instruction to children and caregivers during medication dispensing. In contrast, adherence did not exhibit the same trend, likely due to the more direct role of parents in ensuring timely medication use.
Additionally, we found that taking increased doses of salbutamol as a rescue medication was associated with poor inhalation technique. Children with a poor inhalation technique likely receive lower bioavailable doses, leading them to dispense more rescue therapy to compensate. Thus, monitoring salbutamol dispensing at pharmacies could serve as a valuable starting point for identifying children with a poor inhalation technique.
A key strength of this study is the continuous use of the smart Respiro© add-on device throughout study period, ensuring that our results in this study were representative for the use of inhalers in a home setting.
However, this study has certain limitations. The relatively small sample size may limit the generalizability of our findings. Additionally, synchronization errors between the add-on device and the mobile application may have resulted in some inhalations not being registered, potentially leading to an underestimation of adherence. Furthermore, it is possible that children with a good inhalation technique required lower adherence levels if their prescribed dose exceeded their actual needs. It is also important to acknowledge that additional factors influence inhaler effectiveness, such as pre-inhalation exhalation and post-inhalation breath-holding, which were not extensively assessed in this study. Finally, participants were aware that their adherence and inhalation technique were being monitored, which may have influenced their behavior, leading to improved adherence and technique a phenomenon similar to the Hawthorne effect.30,31
Conclusion
Data from this limited sample size demonstrated no correlation between therapy adherence and inhalation technique. This finding suggests that these two factors should be considered as distinct aspects of inhaled medication use and that both represent independent and frequent challenges in therapy for asthma in children. This is further highlighted by the observation that in daily practice that, in routine clinical practice, only 21% of children exhibit both adequate inhalation technique and good adherence.
Our analysis showed that the inhalation technique is significantly associated with ER visits, rescue medication use, age, and height, while good adherence correlates with ER visits. Understanding these associations enables pediatricians to identify risk profiles for poor inhalation technique and adherence, allowing for more targeted interventions. Ensuring that children not only take their medication consistently but also use the correct inhalation technique is critical. This process should involve parental supervision, pharmacist support, and, where appropriate, digital health technologies to provide real-time guidance and feedback.
Supplemental Material
sj-docx-1-tar-10.1177_17534666251346363 – Supplemental material for The correlation between the level of therapy adherence and inhalation technique in children with uncontrolled asthma using a smart inhaler: the IMAGINE study
Supplemental material, sj-docx-1-tar-10.1177_17534666251346363 for The correlation between the level of therapy adherence and inhalation technique in children with uncontrolled asthma using a smart inhaler: the IMAGINE study by Esther Sportel, Boony Thio, Kris Movig, Job van der Palen and Marjolein Brusse in Therapeutic Advances in Respiratory Disease
Supplemental Material
sj-pdf-2-tar-10.1177_17534666251346363 – Supplemental material for The correlation between the level of therapy adherence and inhalation technique in children with uncontrolled asthma using a smart inhaler: the IMAGINE study
Supplemental material, sj-pdf-2-tar-10.1177_17534666251346363 for The correlation between the level of therapy adherence and inhalation technique in children with uncontrolled asthma using a smart inhaler: the IMAGINE study by Esther Sportel, Boony Thio, Kris Movig, Job van der Palen and Marjolein Brusse in Therapeutic Advances in Respiratory Disease
Supplemental Material
sj-pdf-3-tar-10.1177_17534666251346363 – Supplemental material for The correlation between the level of therapy adherence and inhalation technique in children with uncontrolled asthma using a smart inhaler: the IMAGINE study
Supplemental material, sj-pdf-3-tar-10.1177_17534666251346363 for The correlation between the level of therapy adherence and inhalation technique in children with uncontrolled asthma using a smart inhaler: the IMAGINE study by Esther Sportel, Boony Thio, Kris Movig, Job van der Palen and Marjolein Brusse in Therapeutic Advances in Respiratory Disease
Supplemental Material
sj-pptx-4-tar-10.1177_17534666251346363 – Supplemental material for The correlation between the level of therapy adherence and inhalation technique in children with uncontrolled asthma using a smart inhaler: the IMAGINE study
Supplemental material, sj-pptx-4-tar-10.1177_17534666251346363 for The correlation between the level of therapy adherence and inhalation technique in children with uncontrolled asthma using a smart inhaler: the IMAGINE study by Esther Sportel, Boony Thio, Kris Movig, Job van der Palen and Marjolein Brusse in Therapeutic Advances in Respiratory Disease
Footnotes
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.