Abstract
Chronic inflammation plays a central role in the pathogenesis of chronic obstructive pulmonary disease (COPD). However, there are no effective anti-inflammatory pharmacologic therapies available for COPD so far. Recent evidence suggests that an immunologic mechanism has a role in the pathogenesis of COPD. Macrolides possess anti-inflammatory and immune-modulating effects may be helpful in the treatment of COPD. Several clinical studies have shown that long-term use of macrolides reduces the frequency of COPD exacerbations. However, the subgroups that most effectively respond to long-term treatment of macrolides still need to be determined. The potential adverse events to individuals and the microbial resistance in community populations raises great concern on the long-term use of macrolides. Thus, novel macrolides have anti-inflammatory and immuno-modulating effects, but without antibiotic effects, and are promising as an anti-inflammatory agent for the treatment of COPD. In addition, the combination of macrolides and other anti-inflammatory pharmacologic agents may be a new strategy for the treatment of COPD.
Introduction
Chronic obstructive pulmonary disease (COPD) is associated with enhanced chronic inflammation in the airways and the lung in response to inhaled cigarette smoke and other noxious particles [Global initiative for chronic obstructive lung disease, 2016]. Despite the high morbidity and mortality of COPD (it is projected to be the third-leading cause of death worldwide by 2020), there are no existing therapies that have been shown to effectively prevent the long-term decline in lung function of disease or reduce mortality. The aim of pharmacologic therapy is to reduce COPD symptoms, decrease the frequency and severity of exacerbations, and improve health status and exercise tolerance. The recognition that chronic inflammation plays a central role in the pathogenesis of COPD has led to the widespread use of corticosteroids in the treatment of this disease. However, patients with COPD are poorly responsive to glucocorticoids, even at high doses of inhaled or oral intake, when compared with those with asthma [Barnes, 2003]. Furthermore, treatment with corticosteroids is only recommended for patients with severe and very severe COPD and at high risk of exacerbations in the Global Initiative for Chronic Obstructive Lung Disease (GOLD) 2015 [Global initiative for chronic obstructive lung disease, 2016], indicating the limitation and lagging of traditional anti-inflammatory treatments for COPD. Particularly, there are no anti-inflammatory pharmacologic therapies available in early-stage COPD at present. Thus, it is urgent to identify novel targets and new anti-inflammatory drug therapies for COPD.
There are no effective anti-inflammatory therapies because of the lack of understanding of the cellular and molecular mechanisms associated with the chronic inflammatory processes of COPD. Recently, the observation that an abnormal immune response was involved in the chronic inflammation of COPD suggests that an immunologic mechanism has a role in the pathogenesis of the disease [Cosio et al. 2009]. Thus, some investigators proposed that COPD could be an autoimmune disease triggered by cigarette smoking [Agusti et al. 2003; Taraseviciene-Stewart et al. 2006; Curtis et al. 2007; Lee et al. 2007]. Although there have been reports that using immunoregulators in COPD can decrease the severity and frequency of exacerbations [Collet et al. 1997; Li et al. 2004], relatively little is known about the precise mechanisms involved.
It has long been recognized that 14-membered and 15-membered macrolides possess anti-inflammatory and immune-modulating effects that are independent of their antibiotic activity [Culic et al. 2001; Jaffe and Bush, 2001; Zalewska-Kaszubska and Gorska, 2001; Rubin and Henke, 2004]. The clinical benefits of macrolides in the treatment of diffuse panbronchiolitis encouraged the application of macrolides to a broader range of chronic inflammatory airway diseases such as cystic fibrosis, bronchiectasis and asthma [Nagai et al. 1991; Kudoh et al. 1998; Wolter et al. 2002; Kadota et al. 2003]. Recent literature revealed that the effects of macrolides on preventing COPD exacerbations, but the possible anti-inflammatory mechanisms have not yet been fully elucidated. Here, we review the latest studies regarding long-term macrolide treatment in COPD in order to explore the mechanisms by which macrolides may contribute to the disease and to estimate the clinical benefit and potential harmful effects of these agents.
Macrolides: the benefit from animal models and research in vitro
It has been well established that macrolides exerted anti-inflammatory effects by attenuated mucus secretion and decreased accumulation of neutrophils and macrophages in the airway through reduced production of proinflammatory cytokines, adhesion molecules and chemokines [Kanoh and Rubin, 2010]. New animal experiments show that the administration of erythromycin can alleviate inflammation in the airway, lung parenchyma, and pulmonary vascular system and protect the destruction of alveoli in a smoking murine model of emphysema [Mikura et al. 2011]. Further study revealed that, compared with rats exposed to cigarette smoke, inflammatory cells (e.g. neutrophils, lymphocytes and macrophages) were significantly decreased in bronchoalveolar lavage fluid from those receiving erythromycin. Meanwhile, the matrix metalloproteinases (e.g. MMP-2, MMP-9) and proinflammatory mediators (e.g. tumor necrosis factor-α, interleukin [IL]-6) are also significantly reduced [Zhou et al. 2012]. In vitro, erythromycin can suppress the activation of transcription factor nuclear factor (NF)-κB and activator protein 1 (AP-1) which induced by hydrogen peroxide in human bronchial epithelial cells. [He et al. 2008]. In addition, erythromycin also has a beneficial effect on the pulmonary vascular remodeling in rats exposed to cigarette smoke. Our latest studies showed that a greater number of T-helper (Th)1/T cytotoxic (Tc)1, Th17/Tc17 cells and a fewer number of regulatory T-cells were found in mice exposed to cigarette smoke or patients with COPD, and this imbalance of T-lymphocyte subsets persisted even after cessation of cigarette smoke exposure [Chu et al. 2011; Zhang et al. 2012; Duan et al. 2013]. However, these abnormal immune responses in mice exposed to cigarette smoke were partly corrected by administered erythromycin [Bai et al. 2012]. These observations suggest the immunomodulatory properties of macrolides.
Compared with patients with asthma, even high doses of glucocorticoids exerted limited anti-inflammatory effects on the patients with COPD, suggesting the corticosteroid resistance of COPD [Barnes, 2003]. This phenomenon may be due to a reduction and inactivity of histone deacetylase 2 (HDAC2) as a result of over expression of NF-κB and phosphoinositide 3-kinase (PI3K) which induced by oxidative and nitrative stress [Ito et al. 2005; Adcock and Barnes, 2008; Barnes, 2013]. In previous studies, we have found that erythromycin was able to reverse the corticosteroid resistance through increasing HDAC-2 protein expression which was impaired by cigarette smoke extract (CSE). These changes were associated with the suppression of NF-κB activity in human macrophages
Macrolides: recent clinical study on the treatment of COPD
Clinical evidences of erythromycin on the treatment of diffuse panbronchiolitis introduced the applications of macrolides in a variety of inflammatory airway diseases [Crosbie and Woodhead, 2009; Spagnolo et al. 2013]. Exacerbation of COPD is an acute event characterized by a worsening of the patient’s respiratory symptoms and relates to an accelerated rate of decline in lung function [Donaldson et al. 2002], dramatically changing the nature of the course of the disease, leading to significant mortality. COPD exacerbations are associated with increased upper and lower airway and systemic inflammation, which suggests the potential effects of macrolides on preventing the exacerbation of COPD. In fact, several recent clinical studies have shown that long-term use of macrolides reduced the frequency of COPD exacerbations and extended the time to the next event (Table 1). Firstly, Seemungal and colleagues [Seemungal et al. 2008] conducted a single-center, randomized, double-blind, placebo-controlled study, in which they administered erythromycin at 250 mg twice daily to 109 patients with moderate-to-severe COPD over 12 months. They found erythromycin treatment was associated with a significant reduction in exacerbations in patients with COPD but there were no statistically differences between the groups in terms of forced expiratory volume in 1 second (FEV1), sputum IL-6, IL-8, myeloperoxidase, serum C-reactive protein, or serum IL-6. Subsequently, He and colleagues confirmed Seemungal’s findings by performing 6 months’ treatment with erythromycin (125 mg, 3 times/day) in 35 COPD patients [He et al. 2010]. The outcome showed not only a reduction in exacerbations in COPD patients who received erythromycin but that this was linked to a decrease in airway inflammation, as shown by a decreased number of neutrophils and neutrophil elastase in the sputum. Since neutrophils are the major inflammatory cell in the airways of patients with COPD, the decrease of neutrophils and neutrophil activity in sputum may be partly responsible for the clinical beneficial effects in patients receiving erythromycin. Pomares and colleagues next investigated the clinical benefits of long-term azithromycin treatment (500 mg, 3 times/week) over 12 months in patients with severe COPD and at least four acute exacerbations per year [Pomares et al. 2011]. Their results revealed that azithromycin therapy significantly decreased the number of acute exacerbations of COPD (2.8 ± 2.5
Summary of random-control studies evaluating the clinical effectiveness of macrolide therapy in COPD.

COPD, chronic obstructive pulmonary disease; ICS, inhaled corticosteroid.
Questions raised from macrolide treatment of COPD
Some patients with COPD are prone to suffer frequent and severe exacerbations while other patients are not. This subgroup of patients are now recognized as having a distinct and important phenotype of COPD [Han et al. 2010]. Results from the studies of Albert and colleagues and Uzun and colleagues demonstrated that the maintenance of azithromycin treatment showed the most benefit in patients with COPD who exhibited the phenotype for frequent exacerbations. This observation raised the question of the kind of patients with COPD that are more likely to benefit from the use of long-term macrolide therapy [Albert et al. 2011; Uzun et al. 2014]. Consequently, Han and colleagues [Han et al. 2014] carried out a secondary analysis of this large randomized trial to identify the subgroups to most effectively respond to long-term treatment of azithromycin. They noted that azithromycin is more effective in older patients and patients ranked in milder GOLD stages, especially in those requiring both antibiotic and steroid treatment, but there was no difference in efficacy by sex, history of chronic bronchitis, oxygen use, or concomitant COPD therapy. The relatively little effect among current smokers suggested that azithromycin should be cautiously administrated in this subpopulation. Interestingly, their results demonstrated an increased treatment response for patients at milder GOLD stages. Since this subpopulation accounts for a large part of COPD, this finding may provide evidence for pharmacological intervention with macrolides in the early stages of COPD. In COPD patients with stable neutrophilic bronchitis, Simpson and colleagues found that the addition of azithromycin 250 mg daily for 12 weeks to standard respiratory medications resulted in a trend for a reduction of severe exacerbations experienced and in the markers of neutrophilic airway inflammation [Simpson et al. 2014]. Even though the causal relationship between the anti-exacerbation effect of azithromycin on COPD and an anti-neutrophilic mechanism was unverified, it is reasonable to conclude that the patients with stable neutrophilic bronchitis would be the subgroup which would benefit from the long-term macrolide therapy.
Bronchiectasis coexisting in patients with COPD is identified with increasing use of computed tomography in the assessment of patients with COPD. This radiological change is associated with longer exacerbations and increased mortality, which suggests the clinical importance of coexisting bronchiectasis in COPD [Patel et al. 2004; Martinez-Garcia et al. 2013]. Although the treatment strategies recommended in GOLD 2015 are the usual COPD therapies combined with conventional lines for bronchiectasis [Global initiative for chronic obstructive lung disease, 2016], there are still controversies in the best regimen and lack of pharmacologic agents for this subpopulation of COPD. A growing body of evidence has shown the clinical beneficial effects of long-term macrolide therapy on non-CF bronchiectasis patients. The latest evidence from three randomized, double-blind, placebo-controlled trials, which demonstrated significant reductions on pulmonary exacerbations and better quality of life among non-CF bronchiectasis patients treated with long-term, low-dose macrolide therapy (azithromycin or erythromycin), further confirmed the notion that macrolide maintenance treatment provided clinical benefit in non-CF bronchiectasis [Wong et al. 2012; Altenburg et al. 2013; Serisier et al. 2013]. Therefore, patients with COPD coexisting with bronchiectasis might be a potential population to benefit from maintenance macrolide therapy. Nevertheless, the most suitable population for long-term macrolide treatment and the time the agent should be administered remains uncertain.
It seems that maintenance treatment with erythromycin, azithromycin and clarithromycin all achieved clinical benefits in patients with COPD, so a question remains on the kind of macrolides that should be prescribed. Over the past decades, the progressive introduction of long-acting macrolides, particularly azithromycin, but also clarithromycin, resulted in substantial and sustained increases in macrolide resistance in the community [Karlowsky et al. 2009; Serisier, 2013]. Although erythromycin is the only drug isolated from nature, and has long been used in the treatment for diffuse panbronchiolitis (DPB), it seems to be better tolerated and displays a lower risk of induction of macrolide resistance than azithromycin and other macrolides. In light of this, erythromycin may be a more appropriate and responsible alternative than azithromycin or clarithromycin for patients with COPD.
Concerns about long-term use of macrolides
Despite the beneficial effects of reducing exacerbation of COPD, an agreement on the concerns about the potential adverse events of long-term macrolide use in COPD has not been reached. The common adverse effects in long-term use of macrolides included gastrointestinal intolerance, impairment of liver function and hearing impairment. Uzun and colleagues reported that approximately one-fifth of patients in the azithromycin group complained of diarrhea [Uzun et al. 2014]. Compared with those receiving placebo, a higher rate of hearing impairment in participants receiving azithromycin was found in the study by Albert and colleagues (25%
The greatest concern regarding the wide use of maintenance macrolide therapy in COPD is microbial resistance in community populations [Serisier, 2013]. There is little information available on the clinical consequences of macrolide resistance to individuals. In the study by Albert and colleagues, they found the rate of nasopharyngeal colonization with pathogens resistant to macrolides was 81% in the azithromycin group during the course of the study when they were not colonized with selected respiratory pathogens at the time of enrollment [Albert et al. 2011]. This was twice as high as the placebo group (41%). Similarly, long-term, low-dose macrolide therapy significantly increased the proportion of macrolide-resistant respiratory pathogens in non-CF bronchiectasis patients [Wong et al. 2012; Altenburg et al. 2013; Serisier et al. 2013]. Given the greater patient population of COPD, the maintain use of macrolide treatment in this population may greatly affect population macrolide resistance in the community.
Promising macrolide treatments for COPD
To overcome the potential effect of traditional long-term macrolide therapy on the development of antimicrobial resistance in the community, several novel macrolides, which have anti-inflammatory and immuno-modulating effects but without antibiotic effects, are under development (Table 2). A novel class of nonantibiotic 14-membered macrolide derivatives of azithromycin with anti-inflammatory and immune-modulatory effects, CSY0073, was reported to correct the inflammation-driven immune dysfunction in models of inflammatory bowel diseases and arthritis [Mencarelli et al. 2011]. Furthermore, CSY0073 also can attenuate lung inflammation induced by lipopolysaccharide challenge in mice. Balloy and colleagues reported that CSY0073 diminished the production of proinflammatory cytokines by macrophages exposed to
Candidates of novel macrolides for the treatment of COPD.
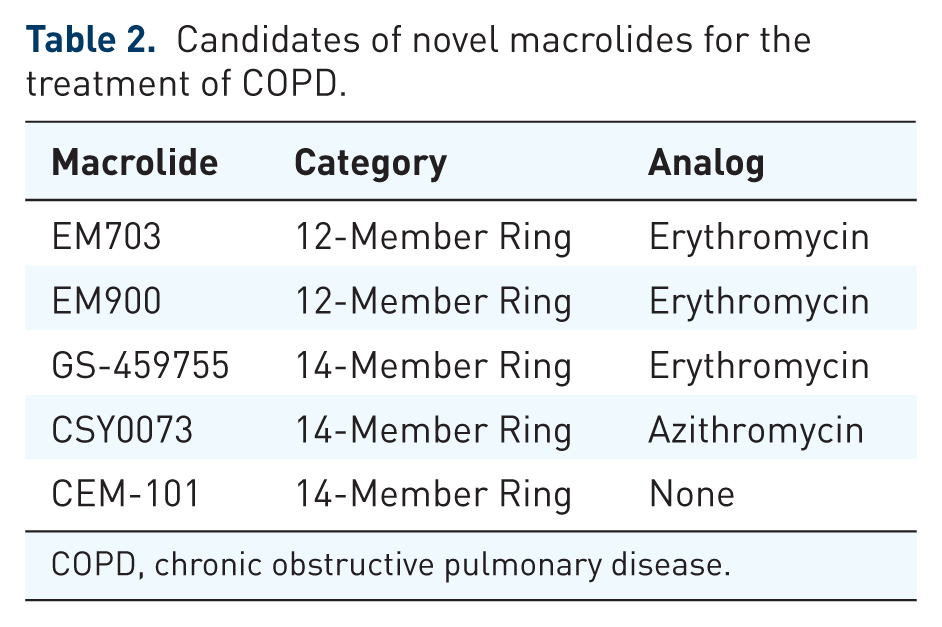
COPD, chronic obstructive pulmonary disease.
In view of the special anti-inflammatory properties of macrolides, the combination of macrolides and other anti-inflammatory pharmacologic agents may be a new strategy for the treatment of COPD. Recently, our study demonstrated that the combination of erythromycin and dexamethasone improved corticosteroid sensitivity through inhibiting the PI3K-δ/Akt pathway and enhancing glucocorticoid receptor α expression. Furthermore, the combination of erythromycin and dexamethasone markedly reduced the production of IL-8 by peripheral blood mononuclear cells of COPD patients and U937 cells exposed to CSE [Sun et al. 2015]. Therefore, combining macrolides with corticosteroids might enhance the anti-inflammatory effects of steroids in the treatment of COPD.
In addition to the direct anti-inflammatory activities, macrolides have the potential to influence the adaptive immune response by modulating the function of many immune cells. Our latest study found that under the stimulation of CSE, erythromycin dramatically down-regulated the expression of the co-stimulatory molecule CD40 on dendritic cells
Conclusion
Evidence from
Footnotes
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Conflict of interest statement
The authors declare that there is no conflict of interest.
