Abstract
This study aimed to observe dynamically the changes of x-ray, histomorphology appearance and serum inflammatory cytokines of cervical degenerative disease in rat models and to discuss the mechanism of cervical degeneration. Sixty Sprague Dawley rats were randomised into test (n = 45) and control (n = 15) groups, which were randomly subdivided into three groups corresponding to 1, 3 and 6 mo post operation. At the corresponding postoperative stage, cervical x-ray films were acquired, and intervertebral disc space and intervertebral foramen size were measured. Some serum inflammatory cytokines from all rats were quantitatively determined. Then, the morphological change in cervical intervertebral disc specimens stained with hematoxylin and eosin was observed. The results were analysed and compared among groups. Compared to the control group, the cervical x-ray and histomorphology appearance of rats in the test group showed varying degrees of degeneration. Furthermore, the serum IL-1β, TNF-α and IL-10 in the test group increased significantly at the corresponding postoperative stage (P < 0.05, P < 0.01 and P < 0.001, respectively) compared to the control group. This model of cervical disc degeneration can accelerate imaging and histological degeneration, but it may be accompanied by changes in serum inflammatory cytokines levels.
Keywords
Introduction
Cervical spondylosis is a common and severe degenerative disease in the middle-aged population, which seriously affects human physical and psychological health and quality of life, and the morbidity of which now shows a trend of affecting younger people. However, the specific pathogenesis remains unclear and might result from multiple factors, among which cervical degeneration is regarded as an important risk factor.1,2 Several scholars have confirmed that disc degeneration is significantly associated with changes in intervertebral inflammatory cytokines. Mern et al. 3 found that intradiscal cytokine imbalance was associated with vertebral disc degeneration. Wuertz et al. 4 considered that the presence of IL-1β, IL-6 and TNF-α would exacerbate disc degeneration. However, what is presently lacking is a study on the role of systemic inflammatory response in the pathogenesis of cervical spondylosis, since previous studies have mainly focused on the relationship between the degenerative disc and intradiscal inflammatory cytokines. Therefore, we established cervical dynamic and static imbalance models in rats and hoped to study the connection between cervical degeneration and systemic inflammatory responses by comparing the serum levels of some inflammatory cytokines between the test and control groups. A reliable animal model of cervical disc degeneration can provide favourable conditions and is a good experimental model for the research of the pathogenesis, development and prevention measures of cervical degenerative disease. The model of cervical disc degeneration induced by imbalanced dynamic and static forces in rats is commonly used in clinical research. However, it does not directly affect the intervertebral disc. Furthermore, the degeneration process is relatively slow, which can simulate well the cervical degeneration process in human beings in that the cervical muscles are weakened due to long-term and persistent strain and irritation experienced in modern life. 5 This study established cervical dynamic and static imbalance models in rats by destroying the cervical muscles and related ligaments. Then, with the aid of imaging, tissue morphology and determination of serum inflammatory cytokines, a dynamic observation and preliminarily exploration was conducted of the mechanism of cervical degeneration.
Materials and methods
Animals
Sixty adult and healthy male Sprague Dawley rats (220–250 g) were randomised into test (n = 45) and control (n = 15) groups, which were randomly subdivided into three groups corresponding to 1, 3 and 6 mo post operation. The test groups included 10, 15 and 20 rats at each corresponding postoperative stage, and the control group had five rats at each time point. This study was carried out in accordance with the recommendations of the Guide for the Care and Use of Laboratory Animals of the National Institutes of Health. The animal use protocol was reviewed and approved by the Institutional Animal Care and Use Committee (IACUC) of Nanjing Medical University.
Model establishment
The modelling method referred to Wang et al. 6 by destroying the cervical muscles and related ligaments. Specific methods were as follows: the rat was shaved on the nape of the neck and disinfected, and a 2–2.5 cm longitudinal incision was made at the midline to cut the skin and subcutaneous tissue. Every muscle layer was fully separated. Superficial muscles – platysma muscle, trapezius and rhomboideus – and deeper muscles – splenius cervicis muscle, Italiciue longissimus capitis, longissimus atlantis, longissimus cervicis, hiocostalis cervicis, semispinalis capitis – were transected successively, and 1.5 cm of each of these muscles were resected to avoid coalescence. Finally, the supraspinous ligament and interspinous ligaments from C2 to C7 were cut off before suturing the skin layers successively. The sutures were not removed and were left to come off naturally. The preparation before surgery and anaesthesia of the rats in the pseudo-surgery (control) group were the same as for the rats in the test group. The skin incision of the rats in the control group was sutured without resecting or cutting any muscle or ligament. Rats were housed in individual cages under normal conditions at 23–25°C and were fed a standard diet. They were given an intramuscular injection of 50,000 IU penicillin sodium to avoid infection after surgery.
Index assessment
X-ray studies
Anterioposterior and lateral x-rays of the rat cervical spine were taken at the corresponding postoperative stages after model establishment. X-rays were taken in the same position fixed after intraperitoneal anaesthesia with ketamine. Anterior, middle and posterior intervertebral space and intervertebral foramen diameters were measured on anterioposterior films and lateral films, respectively. Films were taken using the same molybdenum target x-ray machine (model no. 52420658, DirectView Vita CR; Carestream Health, Rochester, NY) under the same conditions (working potential: 220 V; current: 15 A).
Serum inflammatory cytokines
Serum from all rats was collected intraperitoneally at 4°C, centrifuged at 850 g for 15 min and preserved at –80°C after 1, 3 and 6 mo postoperatively. Serum IL-1β, TNF-α and IL-10 levels were measured using a standard quantitative sandwich ELISA (Groundwork Biotechnology Diagnosticate, San Diego, CA) with a 100 pg/ml detection limit of sensitivity. Serum samples were diluted 1:5 and 1:10 in PBS. All analyses and calibrations were performed in duplicate. Optical densities were determined using an absorbance microplate reader (Elx808™; Bio-Tek Instruments, Winooski, VT) at 450 nm. GraphPad Prism (GraphPad Software, Inc., San Diego, CA) was used to analyse all materials and to depict the standard curve.
Histological and morphological studies
All rats were executed after the experiments finished. Cervical spines were removed and trimmed of adherent tissue, and the complete cervical intervertebral discs from C4 to C6 were removed, fixed in 4% neutral-buffered formalin, decalcified and embedded in paraffin. Four-micron-thick midsagittal sections were cut, and the sections were stained with hematoxylin and eosin, dehydrated, cleared in xylene and sealed with neutral balsam. Histological and morphological studies were performed with a microscope (BX43; Olympus, Tokyo, Japan) to observe the median sagittal plane of each intervertebral disc.
Statistical methods
Data are presented as the mean ± SD. ANOVA and statistical analysis were performed using GraphPad Prism (GraphPad Software). Levene’s test was used to assess the equality of variances. If variances were equal, a one-way ANOVA was employed to compare mean values among groups. The rank-sum test was performed if the data were not normally distributed or if variances were not equal.
Results
General observation
Forty-five rats in the test groups underwent surgery with no fatalities, and were characterised by head bobbing, twisting and shaking that disappeared after about 1 wk. Seven d after surgery, five rats died and were dissected, in which cervical infection and intestinal tympaniteses were present. No further deaths were observed in either the test or control group post operation.
Radiological findings
There were no significant differences in intervertebral space and intervertebral foramen diameters on the cervical x-rays between the control and test groups at 1 mo post operation (Figure 1). At 3 mo (Figure 2) and 6 mo (Figure 3), the postoperative cervical x-rays in the test group showed a loss of cervical lordosis or cervical retroflection, narrowing of intervertebral foramen and reduced intervertebral disc space compared to the control group. The measurement results of the intervertebral space and intervertebral foramen diameters on the postoperative x-rays are shown in Tables 1–3. Compared to the control group, the test group showed similar intervertebral spaces and intervertebral foramen diameters 1 mo after surgery (P > 0.05), distinctly decreased C4–C5 posterior intervertebral spaces and C5–C6 middle intervertebral spaces 3 mo after surgery (lateral x-ray; P < 0.05) and markedly reduced C2–C3 middle and posterior intervertebral spaces, C3–C4 and C5–C6 posterior intervertebral spaces, C6–C7 anterior and middle intervertebral spaces 6 mo after surgery (lateral x-ray; P < 0.05, P < 0.01 and P < 0.001, respectively), as well as significantly narrowed C4–C5 and C5–C6 intervertebral foramen 6 mo after surgery (P < 0.05 and P < 0.01, respectively). In the test group, intervertebral spaces and intervertebral foramen diameters of rats at 6 mo were obviously narrowed compared to corresponding parameters at 1 mo (P < 0.05 and P < 0.05), but these were not statistically different from corresponding parameters at 3 mo (P > 0.05 and P > 0.05).
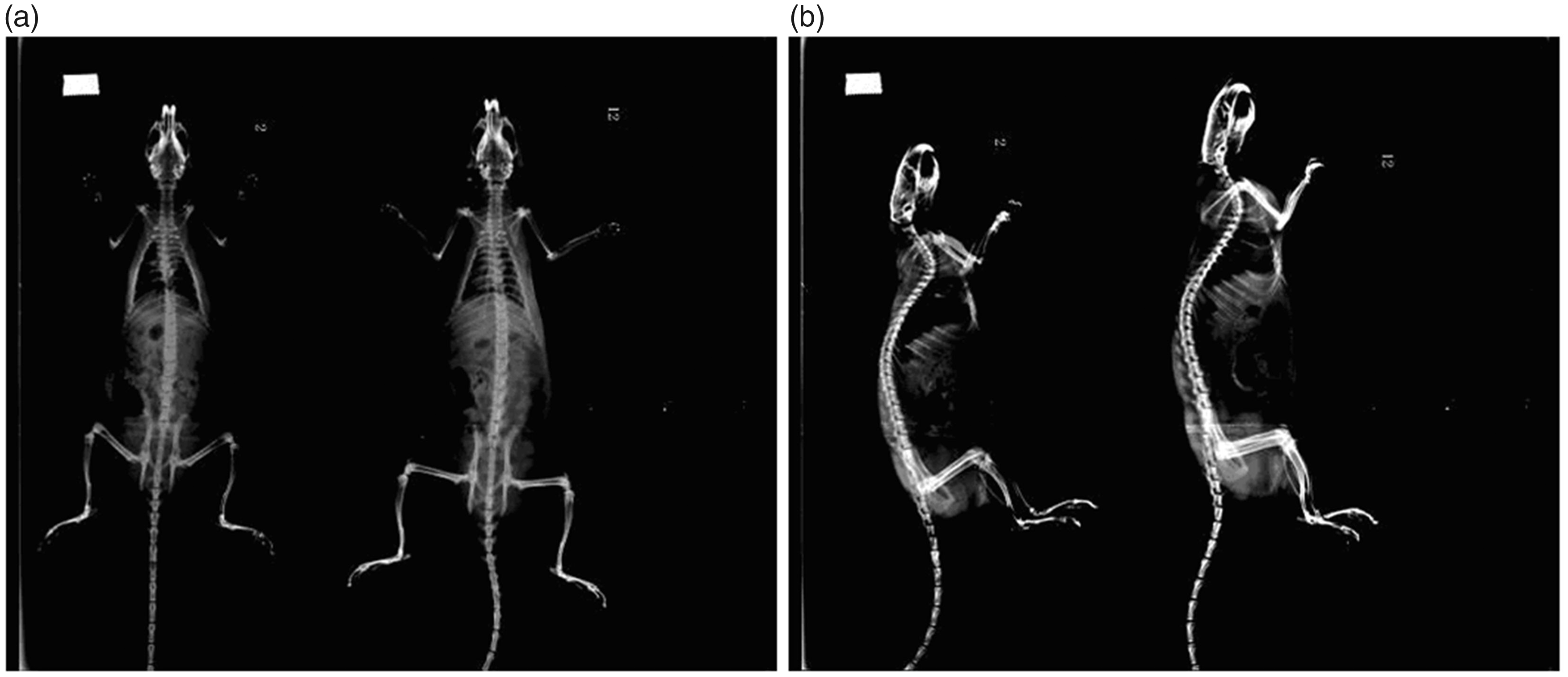
One-mo postoperative anteroposterior and lateral cervical spine x-ray of rats in the test and control groups. (a) One-mo postoperative anteroposterior cervical spine x-ray of rats in the test and control groups. (b) One-mo postoperative lateral cervical spine x-ray of rats in the test and control groups.
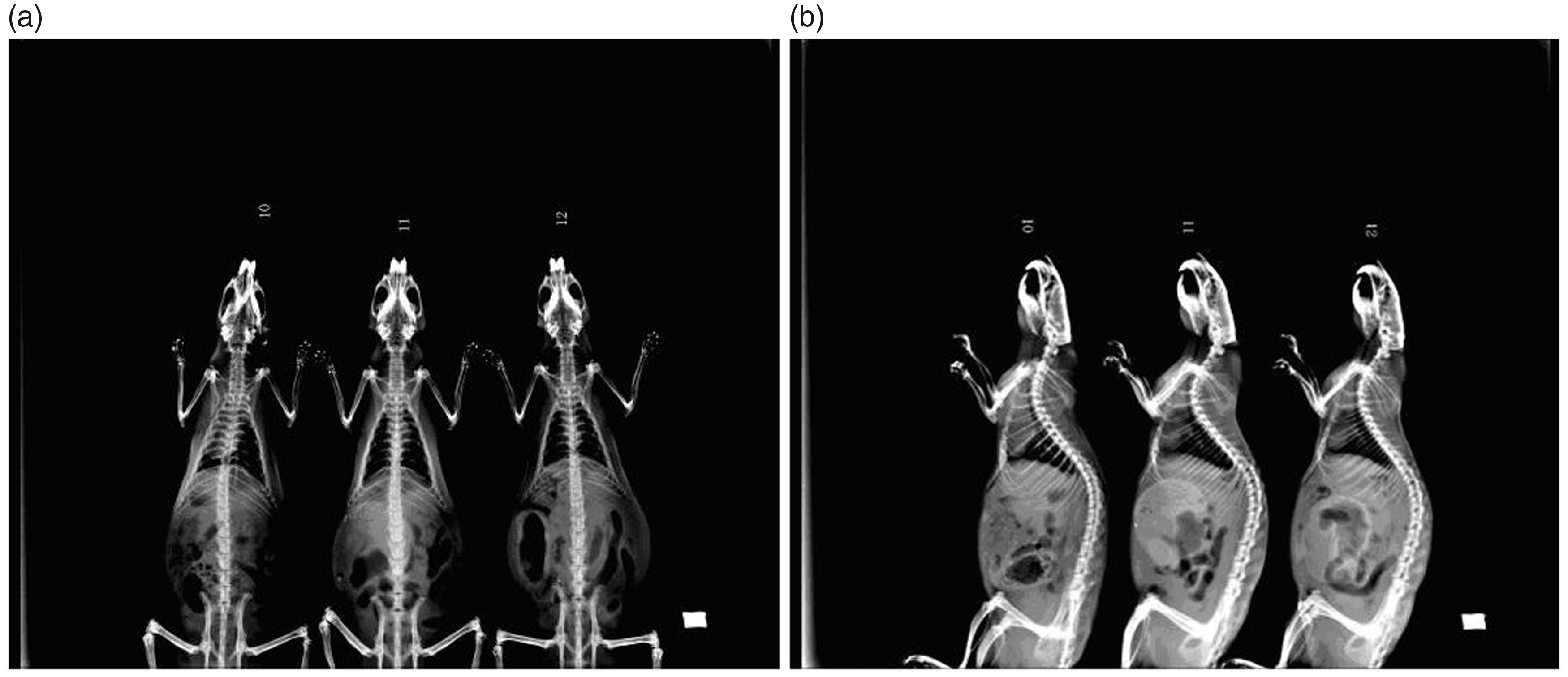
Three-mo postoperative anteroposterior and lateral cervical spine x-ray of rats in the test and control groups. (a) Three-mo postoperative anteroposterior cervical spine x-ray of rats in the test and control groups. (b) Three-mo postoperative lateral cervical spine x-ray of rats in the test and control groups.
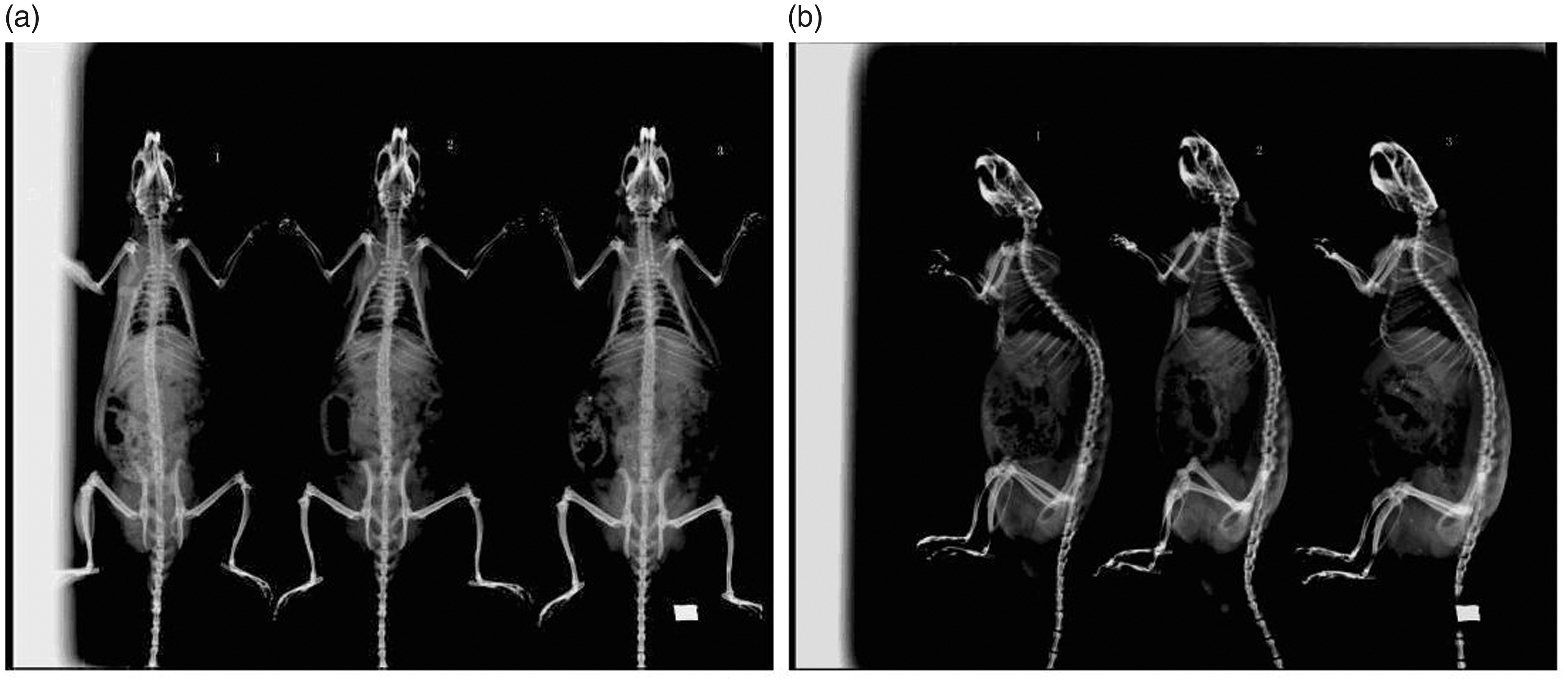
Six-mo postoperative anteroposterior and lateral cervical spine x-ray of rats in the test and control groups. (a) Six-mo postoperative anteroposterior cervical spine x-ray of rats in the test and control groups. (b) Six-mo postoperative lateral cervical spine x-ray of rats in the test and control groups.
Results of anteroposterior intervertebral disc space measurements.
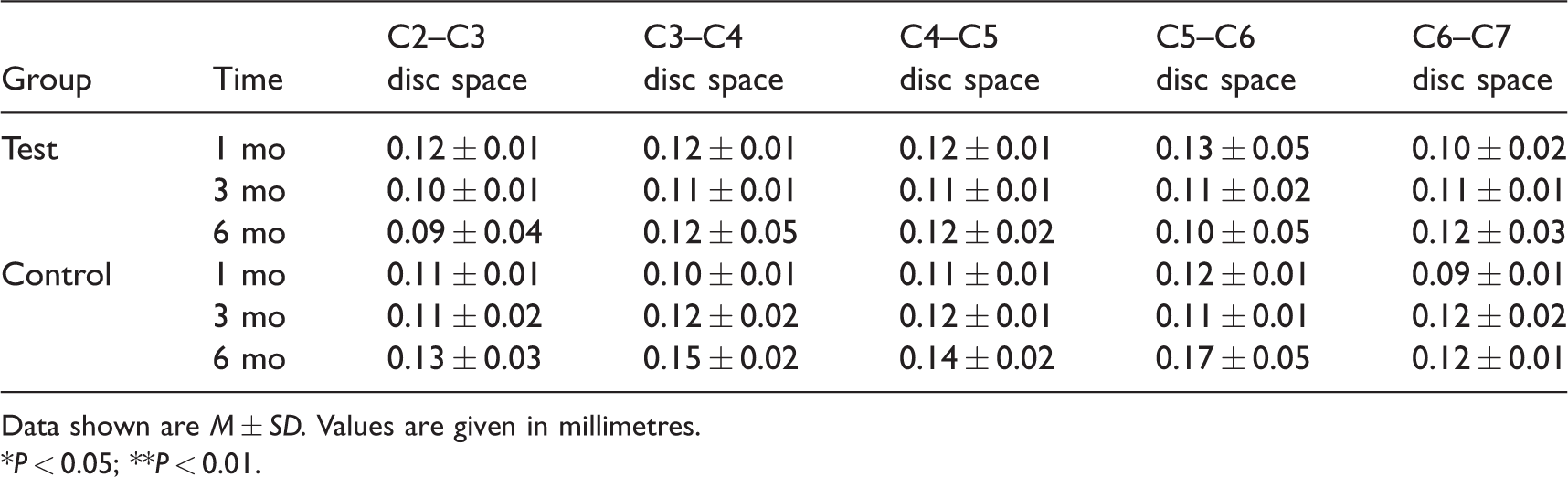
Data shown are M ± SD. Values are given in millimetres.
*P < 0.05; **P < 0.01.
Results of lateral intervertebral disc space measurements.
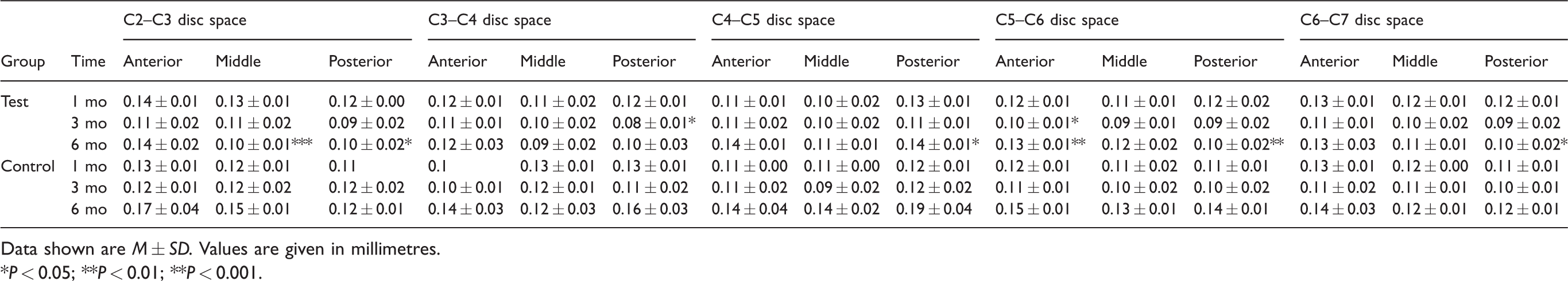
Data shown are M ± SD. Values are given in millimetres.
*P < 0.05; **P < 0.01; **P < 0.001.
Results of lateral intervertebral foramen diameter measurements.
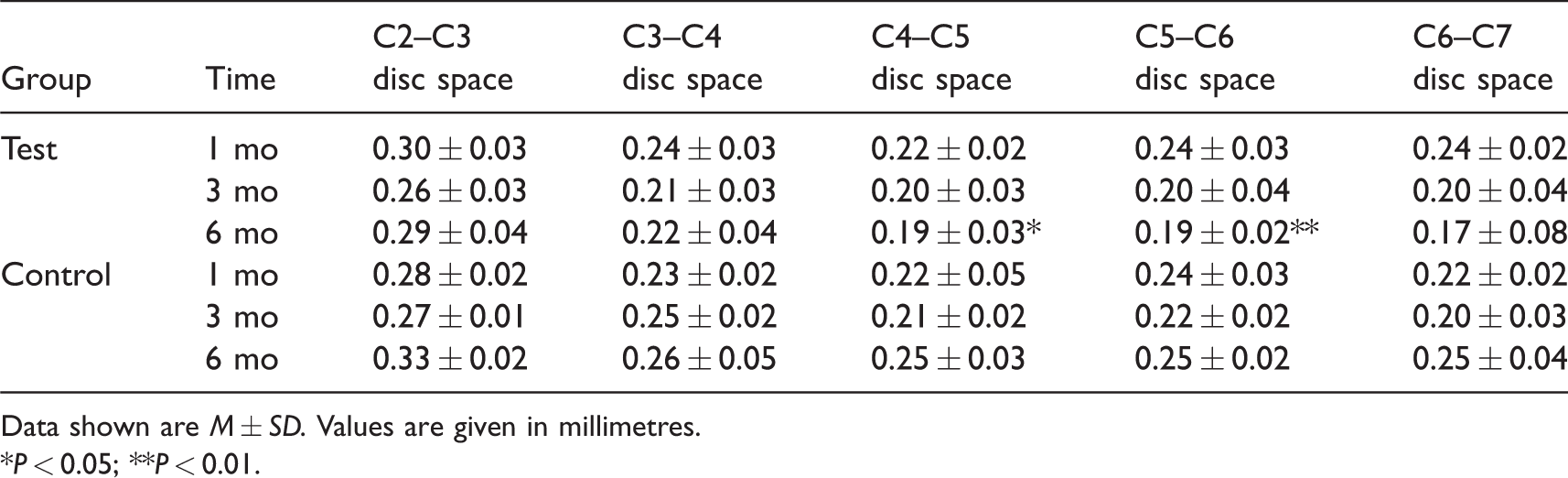
Data shown are M ± SD. Values are given in millimetres.
*P < 0.05; **P < 0.01.
Serum inflammatory cytokines
IL-1β levels in the control group at 1, 3 and 6 mo postoperatively were 97.76 ± 13.33, 112.69 ± 33.35 and 99.78 ± 13.44 pg/ml, respectively, and 266.69 ± 85.33, 211.22 ± 49.23 and 143.71 ± 38.58 pg/ml, respectively, in the experimental group. Compared to the control group, the serum IL-1β in the experimental group increased significantly at 1 and 3 mo following surgery (P < 0.05 and P < 0.05), but there was no statistical difference at 6 mo (P > 0.05; Figure 4).
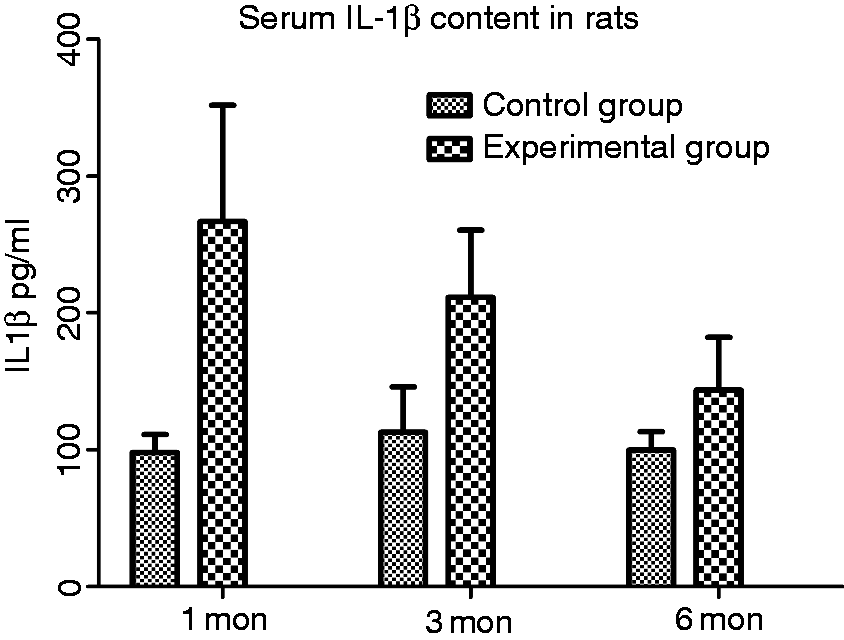
Level of serum IL-1β in the control and test groups.
TNF-α levels in the control group at 1, 3 and 6 mo postoperatively were 79.55 ± 7.64, 74.54 ± 2.23 and 79.60 ± 11.76 pg/ml, respectively, and 147.15 ± 26.12, 144.39 ± 29.45 and 101.59 ± 16.19, respectively, in the experimental group. There were significant differences in the serum TNF-α levels between the experimental group and the control group at 1 and 3 mo following surgery (P < 0.01 and P < 0.01), but no significant difference was seen at 6 mo (P > 0.05; Figure 5).
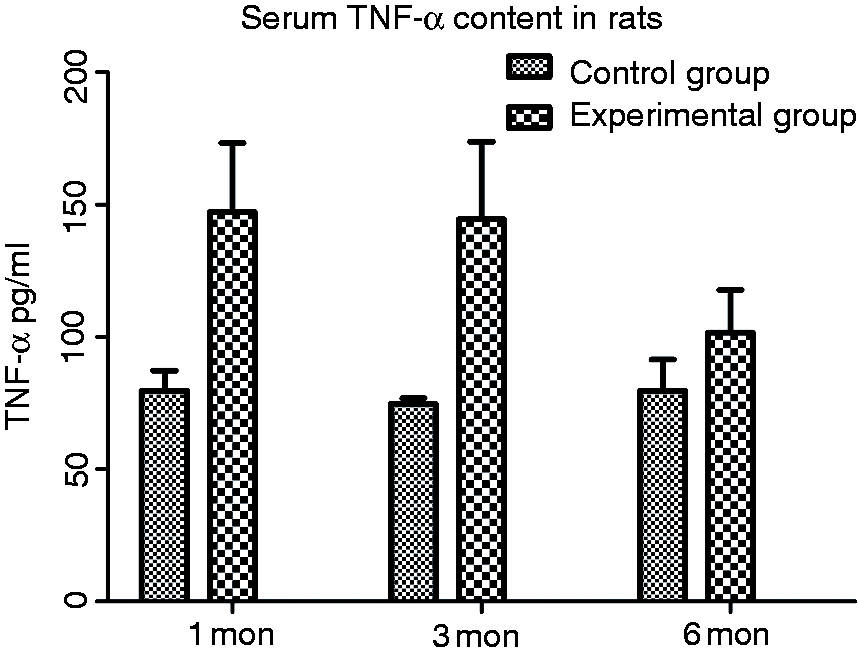
Level of serum TNF-α in the control and test groups.
IL-10 levels in the control group at 1, 3 and 6 mo postoperatively were 59.81 ± 3.68, 64.60 ± 0.96 and 59.82 ± 13.11 pg/ml, respectively, and 94.65 ± 9.37, 111.73 ± 10.42 and 69.93 ± 9.69 pg/ml, respectively, in the experimental group. IL-10 levels in the experimental group significantly increased at 1 and 3 mo following surgery (P < 0.001 and P < 0.001) but not at 6 mo (P > 0.05) compared to the control group (Figure 6).
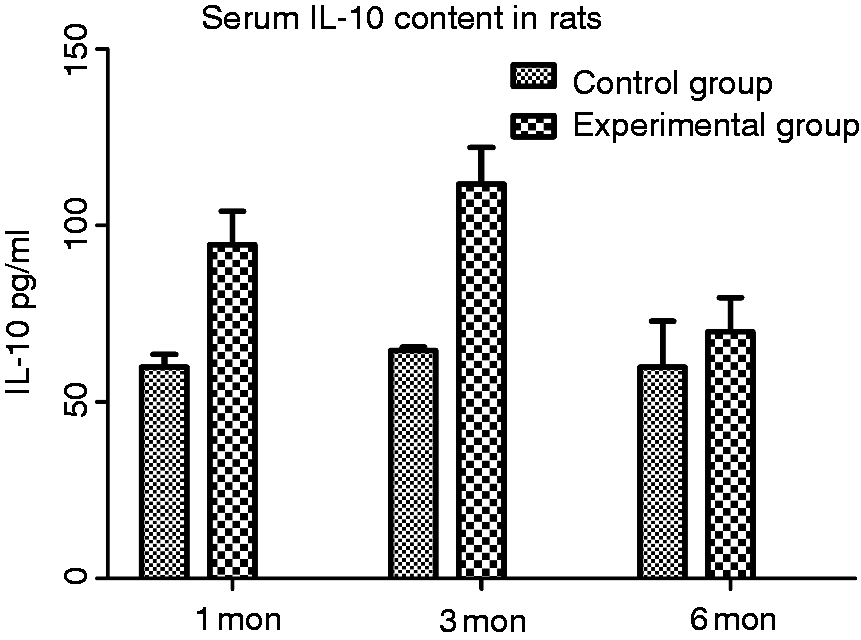
Level of serum IL-10 in the control and test groups.
Histological and morphological findings
The structure of the cervical intervertebral disc tissue of rats in the control group (Figure 7a) was essentially normal at the corresponding postoperative stage: all control discs constituted a rounded nucleus pulposus with some chordoid tissue mostly stellar shaped and evenly distributed in them, well-organised collagen lamellas and a well-defined border between the annulus fibrosus and nucleus pulposus, without cell degeneration, necrosis or proliferation of granulation tissue. Histological evidence of different degrees of cervical disc degeneration was seen in all test groups at each time point post operation. The morphological changes in the cervical intervertebral disc in the test group at 1 mo post operation (Figure 7b) were most seriously degenerated: denaturing of the outer layer of fibrous tissue, thickening, with proliferation of peripheral blood vessels near the nucleus pulposus. Most of the specimens showed that the nucleus pulposus was reduced or even replaced by the fibre or cartilage tissue. To a certain extent, the degree of cervical intervertebral disc degeneration at 3 mo (Figure 7c) decreased compared to at 1 mo. The proliferation of vascular tissue, annulus fibrosus and cartilage cells were still visible, and the degeneration of nucleus pulposus was seen in a few samples. The most moderate morphological degeneration of disc was seen at 6 mo (Figure 7d). No obvious degeneration of the nucleus pulposus was found in any specimens. However, proliferation of vascular tissue, annulus fibrosus and cartilage cells was still present.
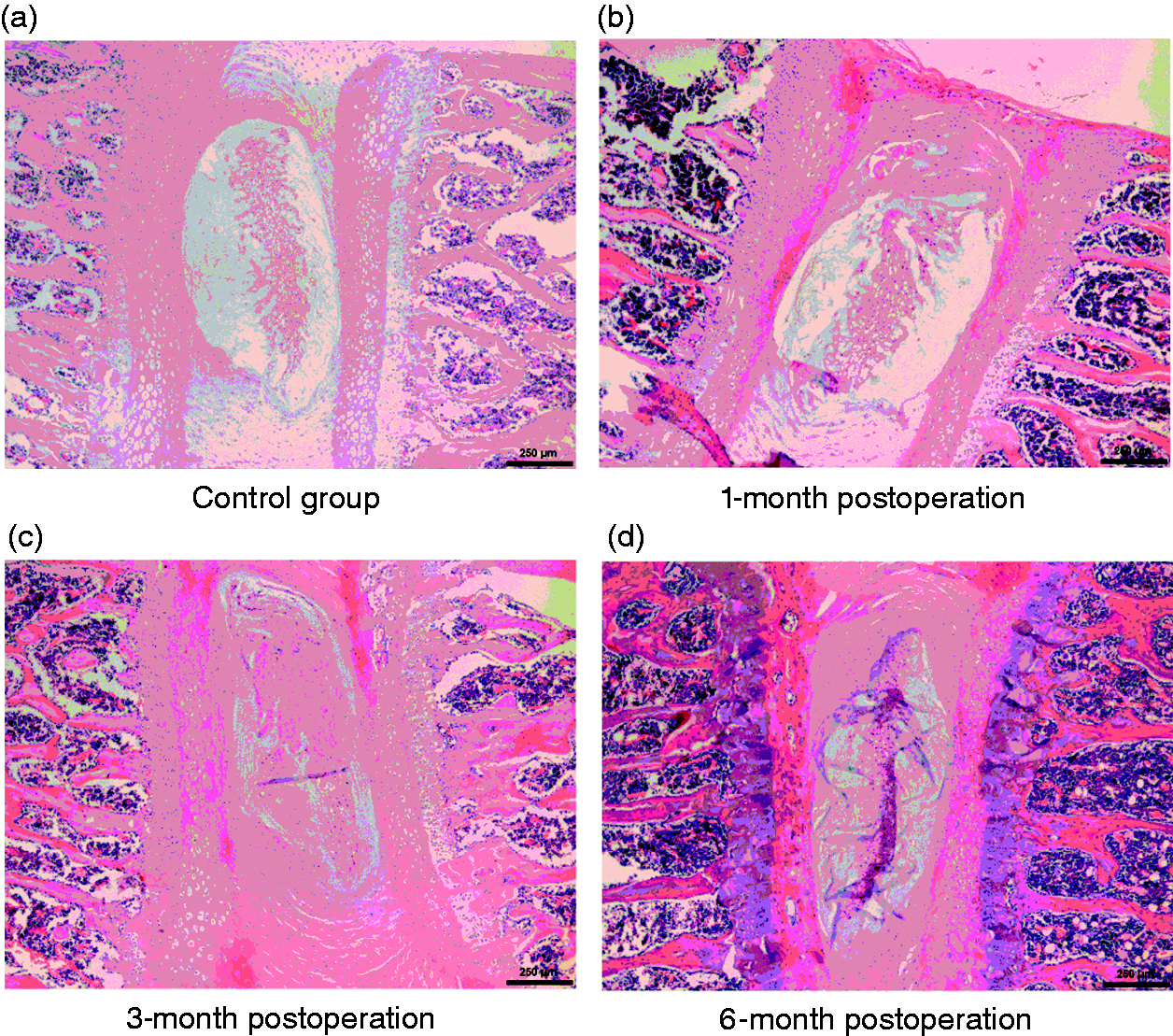
Histological and morphological findings of rats in the test and control groups.
Discussion
Establishment of cervical dynamic and static imbalance models in rats
With the rapid change in the way of working and living in modern life, the pathogenic factors of cervical spondylosis also tend to diversify. More and more scholars have deemed that the diseased cervical muscles and ligament play an important role in the early stage of cervical degeneration. It is important to study the aetiology and mechanism of cervical spondylosis by establishing unstable cervical spine models with experimental animals. So far, the commonly used models of cervical spine degeneration include the acupuncture intervertebral disc model, 7 spontaneous models, 8 bipedal rat models 9 and others. The imbalance of cervical dynamic and static forces induced by destruction of the cervical muscles and related ligaments, of which the degeneration process is relatively slow, can simulate well the cervical intervertebral disc degeneration process in human beings, in which the cervical muscles are weakened as a result of long-term work and study with the head bowed in modern life, as a ‘spontaneous’ degeneration model. 10
The mechanical system that maintains cervical stability includes static and dynamic systems. The static system consists of vertebrae, adnexa and the intervertebral disc and attached ligament. The dynamic system is regulated and controlled by the cervical muscles, which serves as the basis and prerequisite of spinal stability. 11 Some studies12,13 have deemed that dynamic imbalance normally occurs in the early stages of cervical degenerative disease. First, exogenous pathogenic factors directly or indirectly influence the cervical dynamic system, that is, cervical muscles are weakened due to long-term and persistent strain and irritation. Then, dynamic imbalance results in an imbalanced static system that comprises the cervical vertebral body, ligaments and intervertebral disc, followed by biomechanical imbalance of the cervical spine, cervical instability and cervical intervertebral disc degeneration, which lead to annulus fibrosus corruption, nucleus pulposus extrusion, vertebral body collapse, intervertebral disc space and intervertebral foramen stenosis. Consequently, complicated symptoms are present due to mechanical compression of the cervical nerve root, blood vessels and spinal cord from the intervertebral disc and osteophytes. We assessed the changes in intervertebral space and intervertebral foramen diameter on x-ray films of the cervical spine to reflect the degree of cervical degeneration objectively. The results revealed that the appearance of cervical degeneration on x-rays at 3 and 6 mo postoperatively was significantly different in the test group compared to the control group. The results confirmed that we successfully established a reproducible experimental model of cervical dynamic and static imbalance in rats.
We then dynamically observed the morphological changes of the cervical intervertebral disc tissue in order to confirm the above opinion. The results indicated that the histology of the disc tissue of rats in the control group was essentially normal, while the test groups at each time point demonstrated different degrees of histological degeneration compared to the control group: denaturating of the outer layer of the fibrous tissue, thickening, with proliferation of peripheral blood vessels near the nucleus pulposus. Part of the specimens showed that the nucleus pulposus was reduced or even replaced by the fibre or cartilage tissue. Disc tissue is normally avascular. However, did the appearance of capillaries in some parts of the disc specimens in the test groups indicate aging or tissue degeneration? Tolonen et al.14–16 found that disc herniation tissue contained vascular ingrowth. The viewpoint that neovascularisation in the intervertebral disc also plays an important role in cervical degeneration has been widely accepted by some scholars. Some studies17,18 have shown that mutual promotion of the expression of hypoxia-inducible factor-1α and cyclooxygenase-2 occurred in the formation of capillaries during lumbar intervertebral disc degeneration. Lee et al. 19 proposed that IL-1β and TNF-α could stimulate the gene expression of vascular endothelial growth factor (VEGF) of nucleus pulposus cells, thus promoting the proliferation of vascular endothelial cells and further vascularity. Our other studies20,21 found periodic mechanical stress-promoted chondrocyte proliferation and formation of new blood vessels which confirmed our conjecture further.
Significance of IL-1β, TNF-α and IL-10 in the process of cervical degeneration
Disc degeneration is considered the earliest and pre-essential pathological and physiological change for cervical spondylosis. With advances in research on cervical spondylosis, more and more scholars have realised that the deterioration of cervical degeneration is revealed not only by the morphological change, but also by the biochemical imbalance of the internal milieu of the cervical disc. Some studies22,23 have confirmed that a variety of inflammatory cytokines and chemical mediators have been discovered in the disc herniation tissue. However, there has been no relevant research concerning the role of systemic inflammatory response during the occurrence and development of cervical spondylosis. In our preliminary clinical follow-up survey, we found that serum IL-6 of patients with lumbar disc herniation was significantly higher than in the control group, while levels significantly decreased and symptoms subsided after 2 wk absolute bed rest. Thus, we hypothesised that it is not only local inflammatory reactions but also systemic inflammatory responses that play a significant role in the degenerative process of cervical spondylosis. Equally, we found that the serum levels of IL-1β, TNF-α and IL-10 in the test group were statistically higher than those in the control group, which was consistent with the above conjecture.
Cytokines are glycoproteins produced by a variety of cells and secreted into the extracellular fluid, involved in the immune response and inflammatory regulation. IL-1β 24 is thought to be the most important cytokine, with strong pro-inflammatory activity by stimulating the production of multiple pro-inflammatory mediators such as cytokines, chemokines and matrix metalloproteinases. In addition, IL-1β can promote oxidative stress and accelerate the degradation of the extracellular matrix, inducing cell senescence apoptosis, thereby accelerating disc degeneration. One study proposed that the level of TNF-α 25 was closely related to the patient’s cervical pain, which could facilitate neurovascular ingrowth via increased production of VEGF. At the same time, it directly injured the vascular endothelial cells and led to high expression of thrombomodulin, promoting the endothelial cells to secrete IL-1β and finally causing the capillary permeability increase. A histological study showed that disc herniation tissue contains vascular ingrowth, while TNF-α could induce thrombosis and damage the vascular barrier. Consequently, TNF-α in nucleus pulposus tissue may enter the blood circulation, leading to higher levels of TNF-α in the peripheral blood, which could indirectly reflect the local inflammatory reaction in herniation tissue. IL-10 26 mainly exerts an anti-inflammatory action which may be increased as a result of the tight coupling of the pro-inflammatory arm of the local disk disease process with an anti-inflammatory regulatory arm of the response, which is necessary to prevent excessive stimulation and tissue destruction. Li et al. 27 discovered that either TGF-β or IL-10 alone suppressed the expression of inflammatory cytokines. Furthermore, their combined use produced a higher level of inhibition of TNF-α and IL-1β than either TGF-β or IL-10 alone. So, we speculated that IL-10 might be involved in one anti-degeneration mechanism in the cervical degeneration process.
The immunology theory 28 in disc pathophysiology which was first proposed by Naylar et al. 29 has received increasing attention in recent years. Some scholars support the concept of immune-mediated mechanisms in disc pathophysiology, believing that the nucleus pulposus was the largest tissue devoid of blood vessels encircled by the annulus fibrosus and cartilaginous plate, and that the herniation tissues may act as auto-Ags stimulating the body’s immune system to engender auto-Abs and/or autosensitised lymphocytes, resulting in abnormity of humoral immunity and/or cellular immunity. Cytokines such as IL-1β, TNF-α and IL-10 may play certain regulation roles in this process.30,31
Interestingly, we found that the histological cervical disc at 1 mo degenerated most seriously, while the degenerative trend gradually reduced from 3 to 6 mo post surgery. Similarly, the levels of IL-1β, IL-10 and TNF-α at 6 mo in the test group dropped compared to levels at 3 and 1 mo postoperatively, which was inconsistent with our previous conjecture. This may be due to the fact that the neck muscles of rats in the test group gradually healed (Figure 8) after establishing the model at 1 mo, resulting in the cervical dynamic and static imbalance of rats gradually recovering to a certain extent, and also simultaneously slowed down the process of degeneration of the cervical spine, which confirmed that cervical instability could accelerate cervical degeneration from the opposite angle.
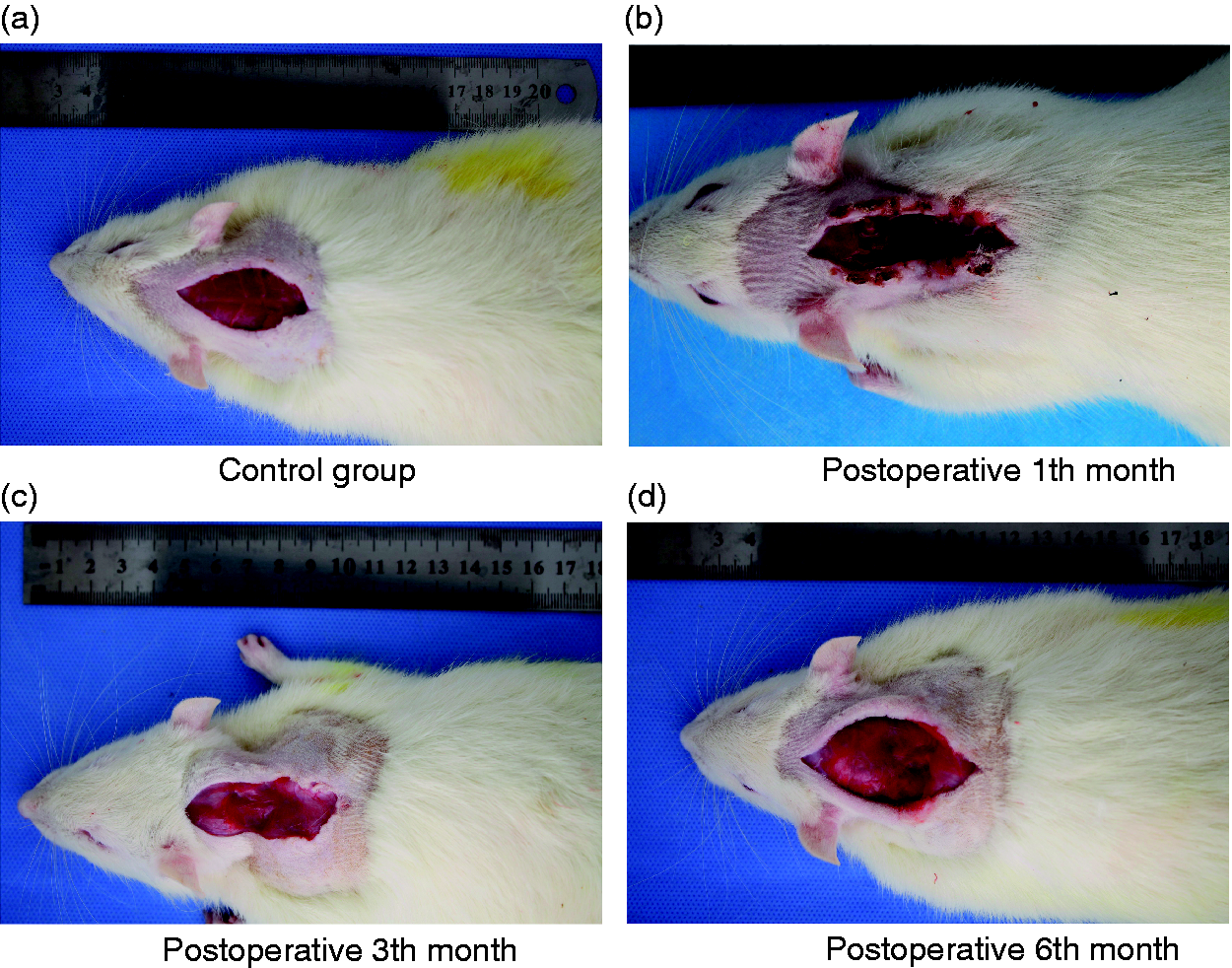
Healing of cervical muscle in rats in the test group at different time points.
In conclusion, our results suggest that a cervical dynamic and static imbalance model can simulate the degenerative process of the cervical spine to a certain extent, accompanied at the same time by changes in serum inflammatory cytokine levels. However, given the complexity of human disc degeneration, no animal model can perfectly mimic the entire pathophysiological process. Therefore, further research and better animal models for the pathogenesis of cervical spondylosis are still needed to confirm the above conclusion.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship and/or publication of this article: This work was supported by The Project of Invigorating Health Care Through Science, Technology and Education (Jiangsu Provincial Medical Youth Talent), Changzhou City High Level Health Personnel Training Project (Grant No. 2016CZBJ029), Changzhou International Scientific and Technological Cooperation Project (Grant No. CZ20170021), Jiangsu Postdoctoral Research supported project (Grant No. 1701001A) and Jiangsu Province ‘Six Talents Peak’ Project (Grant No. WSW-186).
