Abstract
In 2023, the Intensive Care Unit at the Dudley Group NHS Foundation Trust became the first in the UK to achieve Gold Standards Framework (GSF) accreditation. This study evaluates the impact of GSF implementation on end-of-life care delivery and associated metrics. Coding of end-of-life care increased from 10.7% to 16.1% and the proportion of deaths recognised as GSF Amber/Red rose from 14.5% to 58.1% with an increased number of referrals to Specialist Palliative Care. GSF accreditation was associated with sustained improvements in key end-of-life care metrics in intensive care, enhancing collaboration with Specialist Palliative Care and supporting more individualised, patient-centred care.
Introduction
Between 15% and 20% of all admissions to intensive care units (ICUs) in the UK die during that hospital admission. 1 In recent years there has been increasing recognition of the role of palliative medicine in intensive care settings, not merely at the point of imminent death, but in parallel with intensive therapy to improve symptom control, communication, decision making, and alignment of care goals. 2
However, no single accepted model or standardised approach exists for how palliative care should be integrated into ICU workflows.3–6 Indeed, reviews repeatedly highlight that, despite theoretical consensus on its importance, how to integrate within practice remains highly heterogenous across settings, and many ICUs lack structured systems to do so.7,8
The Gold Standards Framework (GSF) offers a structured approach to identification, classification (green/amber/red), and planning for patients in their last year of life. 9 The Dudley Group NHS Foundation Trust adopted GSF trust-wide in 2019, enabling consistent coding and prompting of proactive discussions and individualised care plans.
In 2023, our unit achieved the first intensive care-level GSF Quality Hallmark Award in the UK (a mark of independent validation recognised by UK regulators). Given this achievement, it becomes feasible to examine whether the accreditation and associated systemic changes have translated into measurable improvements in the delivery of end-of-life care within our ICU, and the sustainability of this approach.
Through this work, we hope to contribute empirical evidence on the effectiveness of systematic palliative care integration in intensive care and to inform further scale-up or refinement of best practices.
Methods
Retrospective service evaluation using patient electronic records to review all patients who died on intensive care, between 1 January 2021 and 31 December 2024. It was conducted in a 670-bed acute trust with 23 intensive care beds.
Following trust-wide adoption of GSF in 2019, our unit appointed consultant and senior nurse GSF champions who received dedicated training and support from our Specialist Palliative Care team. Building on positive early engagement, work towards GSF accreditation began in 2022, led by these champions with Specialist Palliative Care input. This focussed on staff education and embedding screening and coding into daily multidisciplinary ward rounds. Identified patients have a GSF code recorded in their record, prompting communication, advance care plan discussions and coordinated care from the multidisciplinary team. GSF codes used are GSF Green (last year of life), GSF Amber (last months to weeks of life), and GSF Red (last hours to days of life). Regular audits reviewed data completeness and feedback outcomes, alongside continued staff education on palliative triggers, conducting ACP discussions and coordinating with Specialist Palliative Care services.
Local work towards GSF accreditation began in early 2022, with formal accreditation achieved in 2023; 2021 therefore represents a pre-implementation baseline. For each calendar year, the following variables were collected: Number coded with GSF on electronic patient record, number of deaths on intensive care, patients offered ACP, patients with a recorded preferred place of care (PPOC), patients recognised as dying (GSF Red) who had an individualised plan of care, patients referred to Specialist Palliative Care and direct discharges from the ICU.
Results
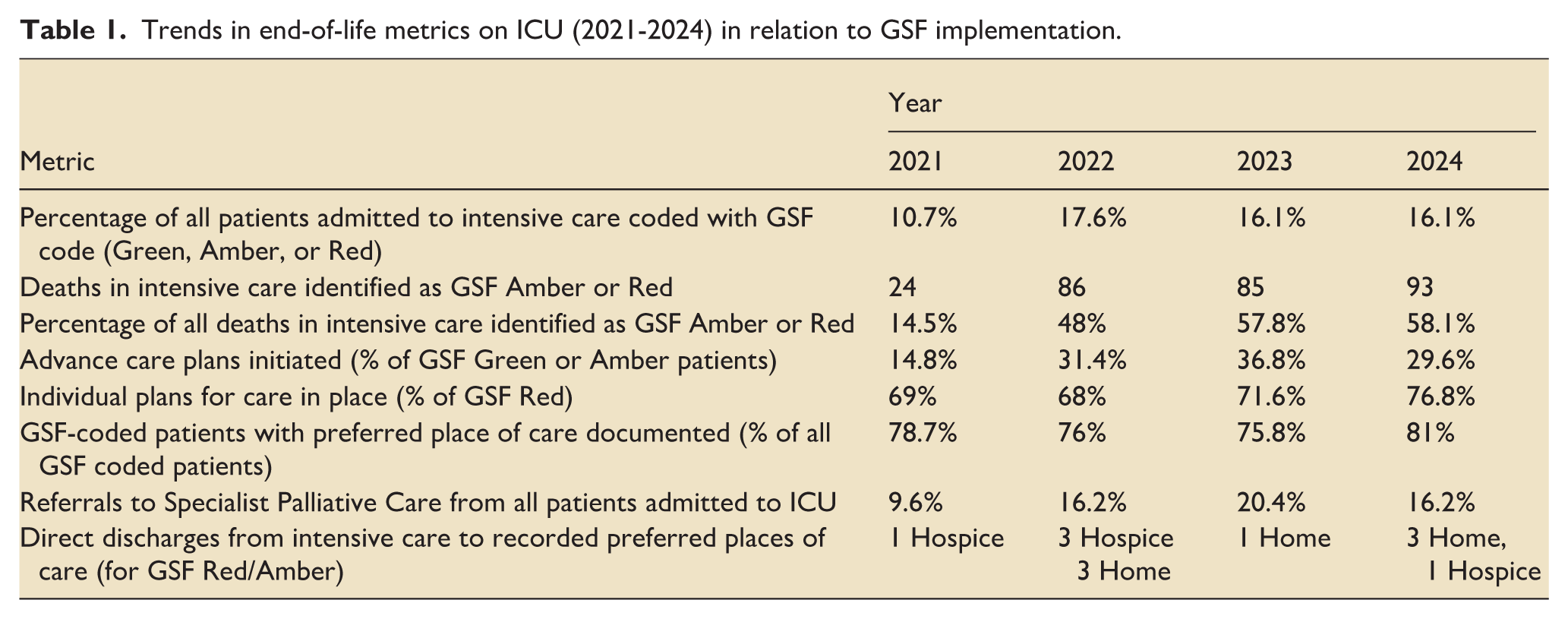
Table 1 summarises key end-of-life metrics on our ICU between 2021 and 2024. Local work towards GSF accreditation started in 2022 and was achieved in 2023. Percentages are calculated using the denominator specified in each row.
Trends in end-of-life metrics on ICU (2021-2024) in relation to GSF implementation.
GSF recognition and coding
The proportion of ICU patients with a GSF code increased from 10.7% in 2021 to 17.6% in 2022, and this improvement was sustained over subsequent years. The proportion of ICU deaths recognised as GSF Amber or Red rose from 14.5% in 2021 to 58.1% in 2024, reflecting improved recognition of patients approaching the end-of-life and greater confidence in initiating prognostic discussions.
Advance care planning (ACP) and communication
The proportion of patients offered an ACP increased, despite recognised barriers to introducing ACP in ICU. 10 For those patients who are recognised as dying (GSF Red), there has also been a sustained increase in the use of individualised plans of care for the dying person.
Preferred place of care (PPOC) and discharge
Recording of a preferred place of care remained consistently high throughout. Direct palliative discharges from ICU for patients identified as GSF Red also increased, showing growth in the familiarity of supporting patients to transition directly from an intensive care environment to their chosen care setting.
Specialist Palliative Care (SPC) involvement
Referrals to Specialist Palliative Care also increased, which demonstrates improved collaborative working and recognition of when to seek Specialist Palliative Care input for patients.
Sustainability
Since implementation, there have been sustained improvements which may reflect the impact of embedding the framework into daily practices.
This analysis is limited by reliance on documentation accuracy and may underestimate informal discussions not recorded in the electronic record.
Conclusion
The GSF offers a structured and sustainable method for integrating end-of-life care principles within an intensive care environment. Through systematic identification, coding, and planning, our ICU demonstrated sustained improvements in recognising patients with end-of-life needs, facilitating advance care planning, and documenting individualised care plans.
The framework has enhanced collaboration with Specialist Palliative Care teams enabling more patients to achieve transitions to their preferred place of care, including direct discharges home. Building on baseline work with local GSF champions, GSF accreditation supported education, engagement, and knowledge, with strong leadership from ICU medical and nursing leads together with support from Specialist Palliative Care teams. This approach supported the team in addressing recognised challenges in intensive care, including prognostic uncertainty, staff confidence, and care planning. These improvements have been maintained beyond the initial accreditation phase, suggesting meaningful cultural and behavioural change within the unit.
Future work should explore staff perceptions of the framework’s impact, barriers to universal adoption, and whether improved documentation and planning translate into measurable differences in patient and family experiences at the end-of-life.
Footnotes
Ethical considerations
Ethical approval was not required for this work as it was a retrospective service evaluation using anonymised patient data collected as part of routine clinical care, in accordance with local hospital policies and national guidelines.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
