Abstract
Background:
Dose Error Reduction Software (DERS) are downloaded onto Smart Pumps with minimum and maximum infusion rate settings to reduce the risk of medication errors when administering intravenous medicines. There are no current national standards for the application of this technology on Adult Intensive Care Units (ICU), and clinical application and governance of this technology is currently unknown.
Method:
A multicentre, cross-sectional survey was conducted using a self-administered questionnaire to explore practical aspects of Smart Pump containing DERS use, such as whether a DERS library was present, how it was managed, how propofol was administered, what kind of error reporting processes were in place, as well as nursing qualifications and competencies on ICUs in England.
Results:
A response rate of 50.7% (136/268 responses) ICUs units in England was achieved and indicated that 63.2% (86/136 responses) of responding units had a Smart Pump containing a DERS library. Three administration strategies were used, mg/kg/h, mL/h and ‘Other’ (which most responses stated as mg/h) for propofol for continuous sedation in ICU Smart Pump containing DERS libraries. In 68.6% (49/86 responses) of ICUs, DERS use and DERS error rates are not reported through local operational and governance structures. DERS use was significantly associated with units having a Clinical Nurse Educator with a postgraduate education certificate (p = 0.005).
Conclusions:
There are no standardised DERS settings for the anaesthetic agent propofol and inconsistent approaches to Smart Pump containing DERS governance oversight across ICUs in England. Further research is required to understand the clinical significance of identified variability.
Introduction
Medication errors are a leading cause of preventable harm in healthcare settings and are associated with serious adverse sequelae such as patient morbidity and mortality, increased length of stay and substantial healthcare costs. 1 A recent report suggests that in England alone, an estimated 237 million medication errors occur annually, with almost 20% (47.2 million) of these occurring in hospital settings. 2 The same report suggests that although a large proportion of these are low to negligible risk, others carry the potential for significant harm. This is particularly relevant within Adult Intensive Care Units (ICU), where complex and high-risk intravenous medication regimens are highly prevalent 3 and medication errors are five times more likely to occur compared to a non-critical care environment. 4 A study of ICUs across North West England identified that errors in administration of medication were deemed to be the most reported type of medication error and were most likely to cause harm to patients. 5
Dose Error Reduction Software, also referred to as Drug Error Reduction Software,6,7 (DERS) are incorporated onto Smart Pumps with minimum and maximum infusion rate settings to reduce the risk of medication errors when administering intravenous medicines. 8 The extent of use of Smart Pump containing DERS in the United Kingdom is not currently known, 9 however, Smart Pump containing DERS libraries are thought to be used more commonly in critical care areas due to the complexity of the intravenous infusions used. 10
International studies have appraised the effectiveness of Smart Pump containing DERS use11–13 including comparing practices between England and the United States of America (USA). One study noted that the USA had an accurate definition of requirements around infusion device use and therefore patterns of errors were ‘comparable’. In the USA, drug libraries were programmed by manufacturers, whereas in England this is done locally by clinicians. 14 The variability of Smart Pump containing DERS use in England may lead to an inefficient use of the technology and healthcare resources as well as increasing the risk of medication administration errors.
In England, it remains the responsibility of individual organisations to develop their Smart Pump containing DERS libraries, which may result in widespread variation unless national guidance is produced. NHS organisations procure Smart Pumps from different manufacturers, with the ability to configure Smart Pump settings in multiple ways.
The Healthcare Safety Investigation Branch (HSIB), which covers healthcare organisations in England, have previously identified variability of Smart Pump use on ICUs. The HSIB investigated three incidents involving fentanyl administration at three different ICUs, which was published in their report ‘Procurement, usability and adoption of “smart” infusion pumps’. The investigation identified that DERS were developed ‘locally’ and no national guidelines or standards on how to implement the libraries currently exist. 15 HSIB recommended that the Medusa NHS Injectable Medicines Guide (IMG) team lead on addressing this challenge, including developing standardised intravenous infusion concentrations and the configuration of drug libraries. 15 HSIB recommend that each Trust should have a governance process set up to ensure appropriate safety configuration of Smart Pumps, with the final responsibility sitting under the Trust’s Medicines Safety Officer (MSO) or Medicines Committee. 15
Propofol is an anaesthetic agent which is commonly used in ICU for sedation. 16 There are two different concentrations available for sedation in the form of 1% and 2% 17 and can be administered using volumetric and syringe driver Smart Pump devices. 18 As Propofol has attributes such as constant dose titration to target sedation scores and monitoring of patient parameters, it a useful drug to benchmark administration practice across England. The variability of different propofol profiles and formulations across England has not previously been explored.
The responsibility of administration of intravenous medications and using Smart Pumps is with nursing staff. There is limited evidence on best practice for training nursing staff, and there are no specific national training guidelines or competencies for using Smart Pumps. 19 However, the Guidelines for the Provision of Intensive Care Services version 2 (GPICSV2) standards for ICUs 20 state that all registered nurses commencing in ICUs must be working towards Step 1 of the National Competency Framework for Adult Nurses in Critical Care (NCF). 21 This competency covers ‘Use medication regimes in practice to titrate medications within prescribed limits’ and ‘Increasing or decreasing the infusion rates as appropriate’. Smart Pump containing DERS has the potential to offer an extra safety layer for administering intravenous infusions through alarming at maximum rates of infusions to reduce the risk of overdose. Therefore, comparing attainment of NCF Step competencies to application of DERS could offer insight into the potential medication risks that ICU patients are exposed to. In addition, the safe use of Smart Pumps containing DERS libraries may also be dependent on the competence and support of end-users. Broader indicators of educational competency and infrastructure (e.g. post-registration nursing qualifications, or presence of Clinical Nurse Educators ((CNEs)) may influence their safe implementation and oversight, warranting exploration of these factors.
The aim of this study was to benchmark the current landscape of DERS use in ICUs in England, with a specific focus on propofol, to understand its national implementation and governance.
Primary objectives
To examine current Smart Pump use across ICUs in England, including how propofol 1% and 2% are administered and how DERS libraries are configured.
To explore how DERS libraries are governed and maintained within individual ICUs.
Secondary objective
To assess how nursing competencies and educational infrastructure related to Smart Pump and DERS use align with national standards (e.g. GPICSV2 and NCF).
Method
Study design
A multicentre, cross-sectional survey was conducted using a self-administered questionnaire.
Setting and population
Each unit was asked to identify one appropriate clinician to complete the survey. This individual either chose to participate or nominated another suitable clinician locally. Eligible respondents were professionals with working knowledge of the intravenous Smart Pumps used in their ICUs and access to the unit’s nursing competencies via the local training matrix. The questionnaire was distributed to all 268 NHS ICUs in England identified on the Intensive Care National Audit & Research Centre’s (ICNARC) Case Mix Programme (CMP). 22
Questionnaire development
To examine how DERS is used in intravenous Smart Pumps across ICUs in England, we developed an online survey using the Qualtrics® platform. The questionnaire mainly included closed-ended questions, though free-text fields were added to allow respondents to elaborate when needed. The authors designed the survey based on their experience working with Smart Pump systems in ICU, and on knowledge of local governance recommendations and national training structures. We included questions to cover practical aspects of Smart Pump containing DERS use, such as whether a library was present, the configuration of settings, how propofol was administered, weight descriptors for dosing, nature of established local auditing and error reporting processes, as well as nursing qualifications and competencies. The survey used built-in logic to display or skip certain questions based on previous responses, keeping the content relevant and streamlined for each participant. A draft was reviewed by a local research team, and changes were made based on feedback regarding layout, clarity and presentation. The questionnaire was piloted at one ICU (which was the research base site) to assess face validity and amendments were made following review. The final questionnaire included 15 questions and took approximately 10–15 min to complete when piloted.
Data collection
A cover letter and survey link were emailed via the National Adult Critical Care Programme (NHS England) to regional Critical Care Specialist Clinical Networks (formerly known as Operational Delivery Networks). 23 These networks promote research amongst their local units, and they forwarded the invitation to a suitable clinician at each local ICU. If multiple clinicians were identified, this was attributed as ‘multi-disciplinary team’ (MDT). The survey was open for 3 months during the data collection period of October 2024 to January 2025. Non-responding units were identified, and their local Specialist Clinical Network was contacted to send two follow-up reminder emails during the data collection period. Additionally, regional networks were contacted with a list of non-responding units (identified through survey monitoring) and asked to prompt participation. Partial responses were included in the analysis. If multiple partial responses were received from 1 unit, the most complete survey was used; if identical in completeness, the first response was used.
Data analysis
Survey data were exported from Qualtrics and analysed using SPSS® (Version 29). Descriptive statistics, including frequencies and percentages, were used to summarise categorical responses related to the presence and governance of Smart Pump containing DERS, propofol administration methods and workforce training and competencies across ICUs. Crosstabulation analyses were performed to explore associations between the presence of Smart Pump containing DERS and educational competencies and qualifications of nurses within units. Statistical significance was assessed using the Pearson Chi-Square Test, and Fisher’s Exact Test was used where expected cell counts were less than 5. A significance threshold of p < 0.05 was applied. Analyses were conducted on valid cases only.
Ethical considerations
Ethics approval was granted by the University of Central Lancashire Committee for Ethics and Integrity (HEALTH 01166) on 26 September 2024. All data were stored securely on a server hosted by the university, in line with the requirements of the UK GDPR and the Data Protection Act 2018. Completion of the questionnaire was voluntary and implied consent. No personally identifiable information was collected, although responses were linked to hospitals.
Results
A response rate of 50.7% (136/268 responses) from ICUs in England was achieved, with 63.2% (86/136) of responding ICUs having a Smart Pump containing DERS library (Table 1).
Propofol administration practices.
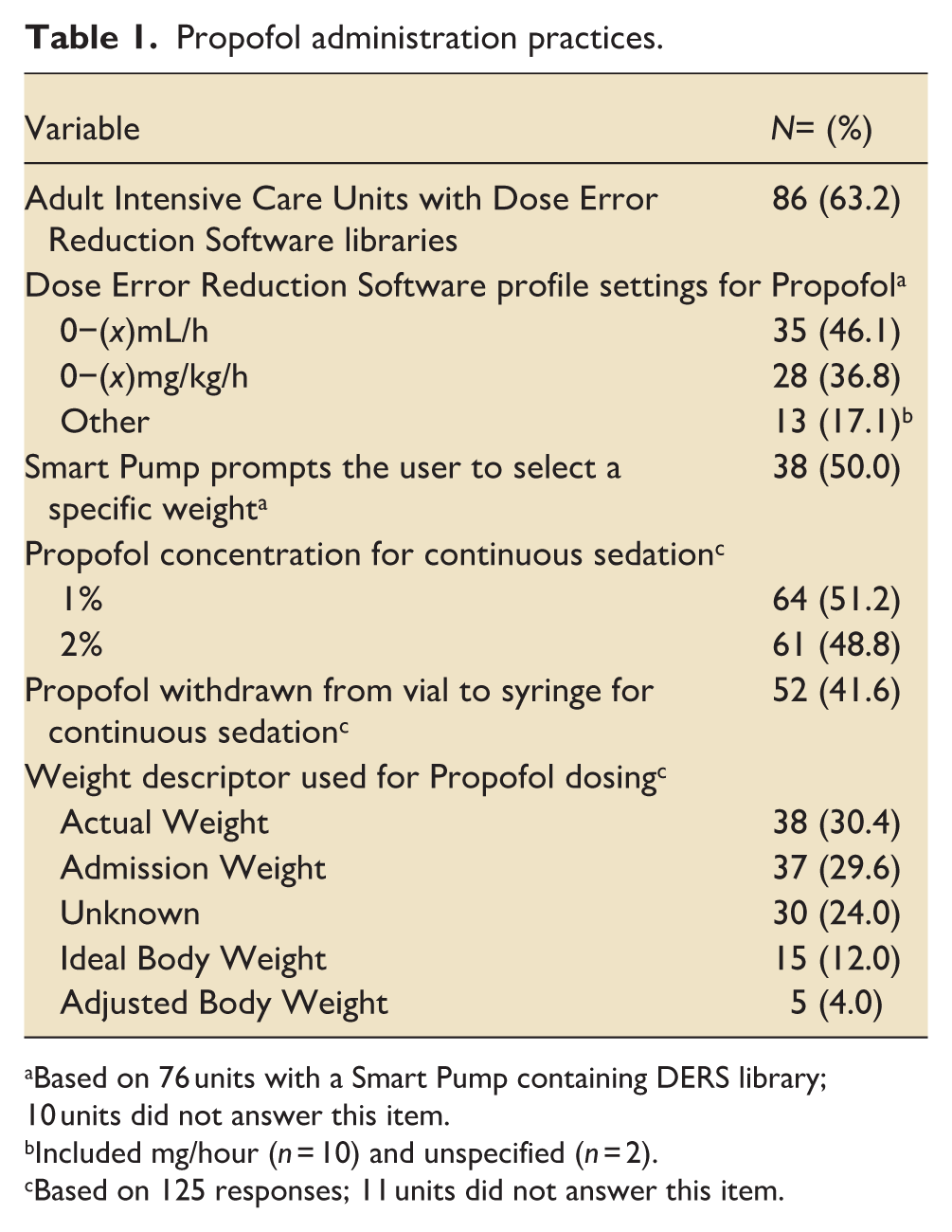
Based on 76 units with a Smart Pump containing DERS library; 10 units did not answer this item.
Included mg/hour (n = 10) and unspecified (n = 2).
Based on 125 responses; 11 units did not answer this item.
DERS profile settings varied, with mL/h limits being most common (46.1%), followed by mg/kg/h limits (36.8%) and other settings (17.1%), with most ‘other’ settings being reported as mg/h (Table 1). Half of Smart Pumps prompted users to select specific weight descriptors when starting an infusion. Propofol concentrations were used in similar proportions for continuous sedation (51.2% used 1%, 48.8% used 2%), with the majority of propofol infusions administered directly from vials (58.4%) rather than withdrawn into syringes. Weight descriptors used for propofol dosing showed considerable variability, with actual weight (30.4%) and admission weight (29.6%) being most common, though 24.0% of units reported unknown weight descriptor used (Table 1).
Approximately two-thirds of units with Smart Pumps had a named clinician responsible for review and maintenance of libraries (64.0%), with pharmacists (36.4%) and medical consultants (30.9%) being the most assigned roles (Table 2). Local DERS use and error auditing at ICU governance and operational level was in place in less than one-third of units (31.4%) with Smart Pumps.
Implementation and governance of dose error reduction software.
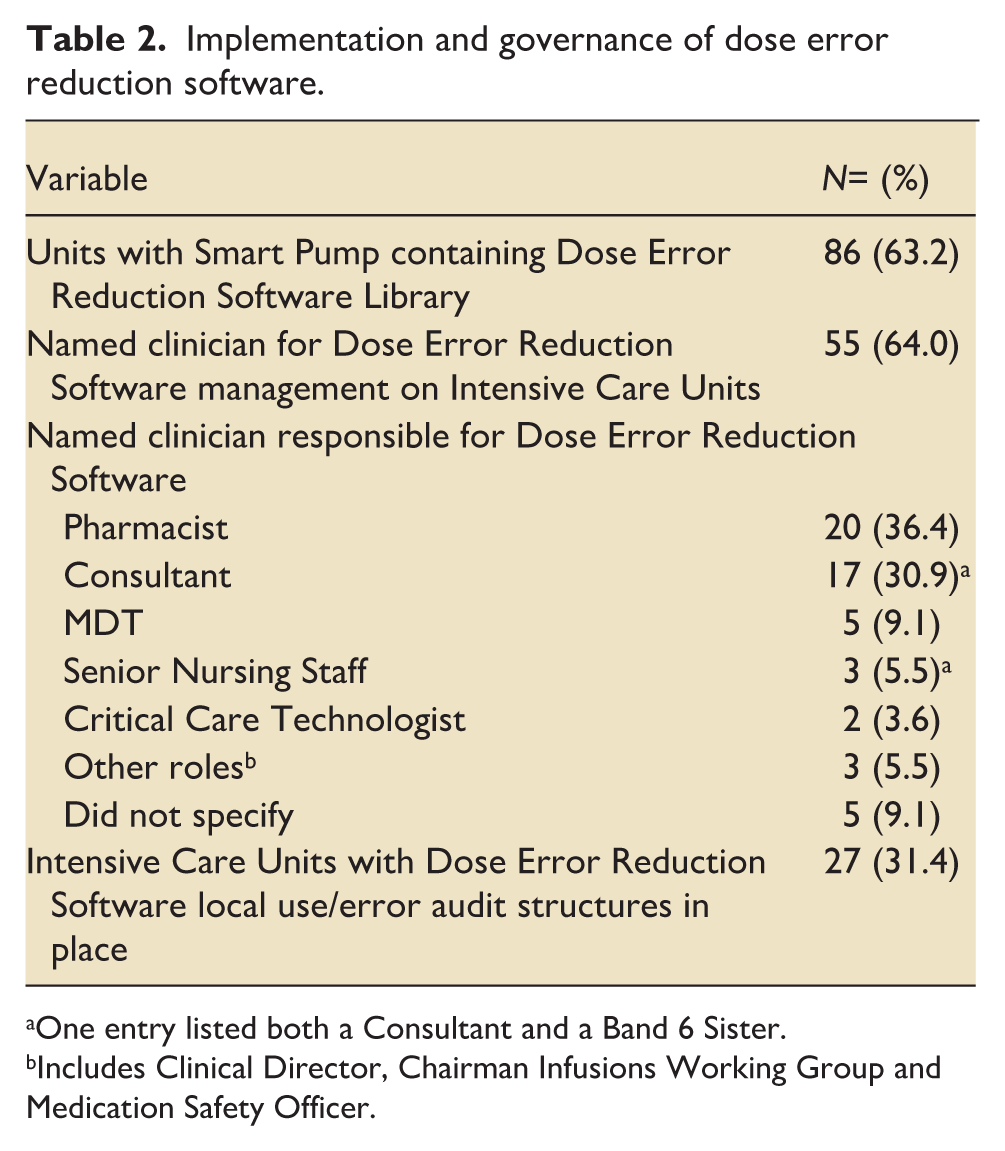

One entry listed both a Consultant and a Band 6 Sister.
Includes Clinical Director, Chairman Infusions Working Group and Medication Safety Officer.
Just over half of units had ⩾50% of nursing staff with post-registration award in intensive care (52.9%; Table 3). Most units had dedicated supernumerary CNE (73.5%), most of whom had post-registration intensive care awards (82.4%). Regarding Step 1 NCF competency requirements, around half of responses indicated that 0%–20% of their nursing workforce still required sign-off (Table 3).
Intensive care units nursing staff profile and competencies.
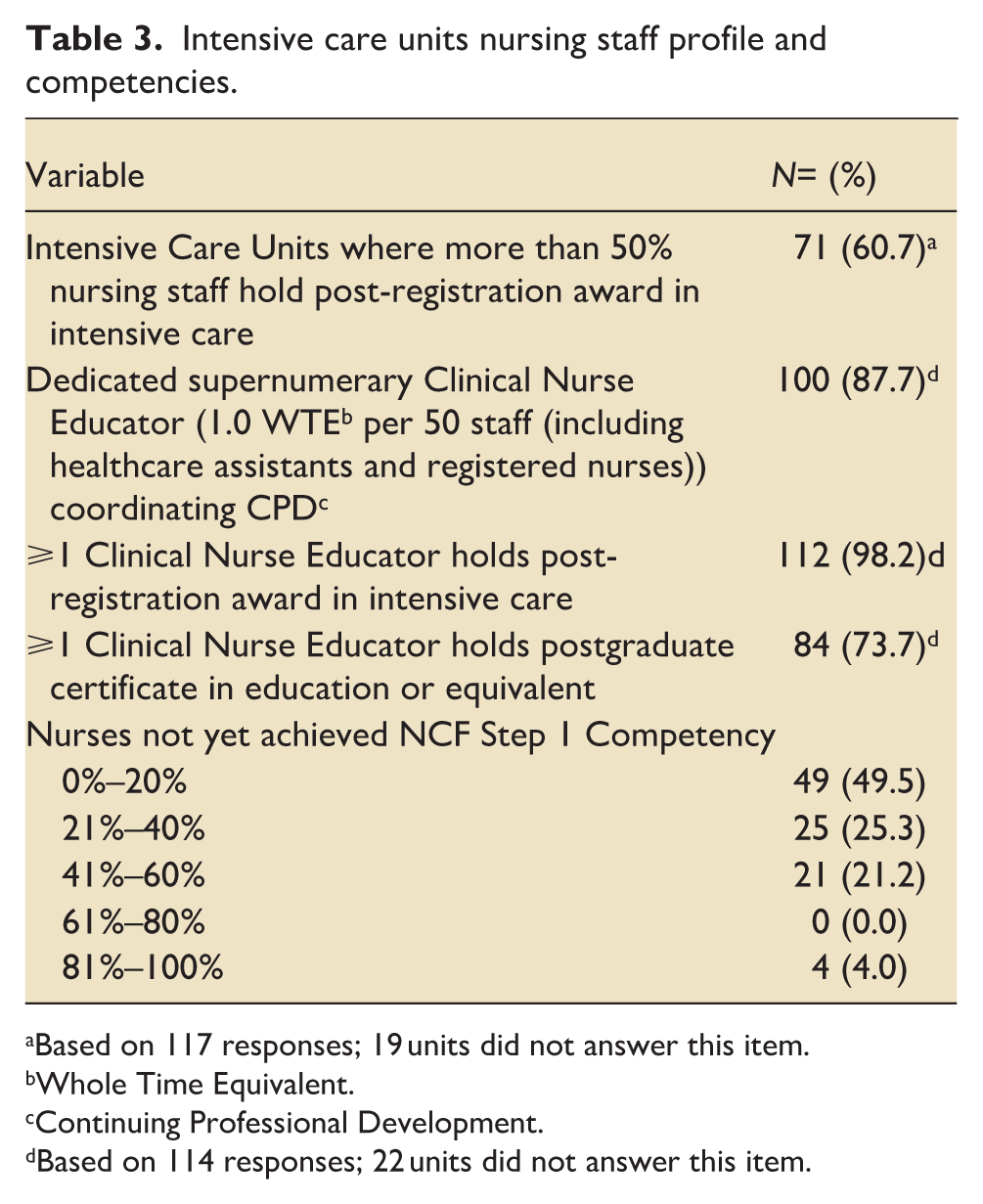
Based on 117 responses; 19 units did not answer this item.
Whole Time Equivalent.
Continuing Professional Development.
Based on 114 responses; 22 units did not answer this item.
Crosstabulation analyses were conducted on valid cases to explore whether the presence of a Smart Pump containing DERS was associated with nursing staff qualifications and educational infrastructure within ICUs. One statistically significant association was identified: units with a Smart Pump containing DERS were more likely to have a Clinical Nurse Educator (CNE) holding a postgraduate certificate in education or equivalent (χ² = 7.87, p = 0.005). No other significant associations were found (Table 4).
Associations between ICUs with Smart Pumps containing DERS and nursing profile/competencies.
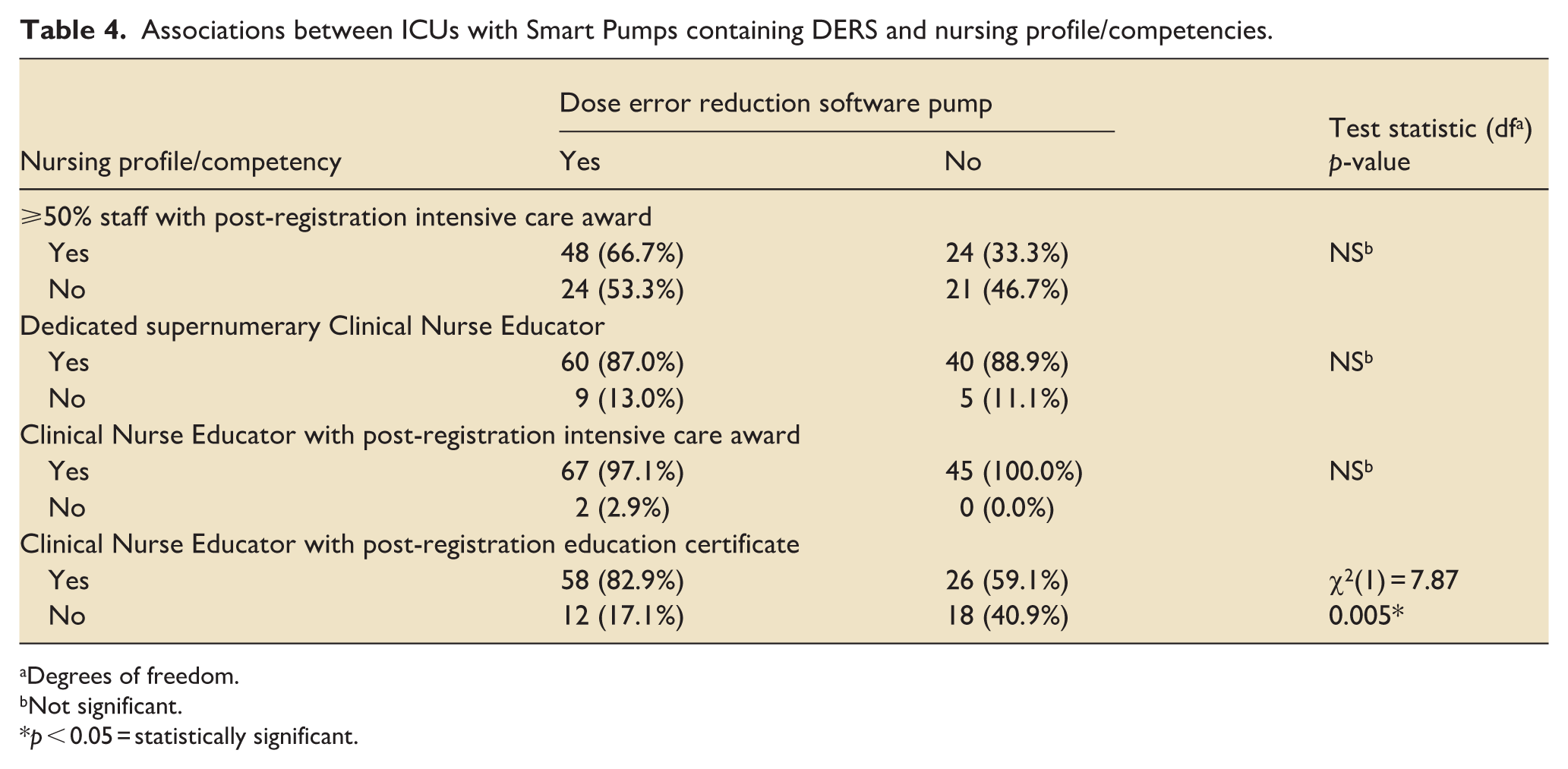
Degrees of freedom.
Not significant.
p < 0.05 = statistically significant.
Discussion
This benchmarking survey examined the landscape of Smart Pump use, DERS settings used and nursing competencies in 50.7% of responding ICUs in England. Wide variation was found in relation to the use of Smart Pumps, propofol administration, local governance processes regarding their use and the attainment of nursing competencies aligned with national standards. These inconsistencies may pose risks to patient safety and highlight the need for a nationally coordinated approach.
DERS libraries in ICUs across England
Our findings demonstrate that across ICUs in England, over 63.0% of responding units have Smart Pumps containing DERS libraries. Therefore, patients admitted to units without Smart Pumps containing DERS libraries have inequitable access to systems designed to prevent medication errors, particularly when administering high-risk drugs such as propofol. An analysis of DERS databases in England has previously concluded that DERS has potentially prevented serious harm or death to over 100 patients in two NHS organisations alone over 12 months, however stated that more research is required to understand if DERS solely mitigated this risk. 24
Propofol and DERS
Propofol is a commonly administered anaesthetic agent used in ICUs to provide sedation in mechanically ventilated adult patients. Our survey has highlighted the lack of consensus on dosing weight descriptors of propofol as a continuous infusion. Actual body weight (ABW) dosing has been used for non-obese patients 25 however, in obese patients the use of ideal body weight (IBW) or adjusted body weight (AdjBW) is preferred.26,27 Our survey demonstrated that admission and actual weight are the most used weight descriptors for dosing propofol, but a proportion of responders were unsure which weight to use and selected ‘Unknown’. In addition, half of the units had Smart Pumps advising end-users on which weight to input if using a weight-based setting. This suggests that ICU patients may be at risk of inaccurate dosing (including overdosing) on weight-based drugs if the wrong weight descriptor is selected when starting an infusion using Smart Pumps containing DERS, and these will alarm at different rates when exceeding the maximum dose. Estimated weights should be avoided on ICU due to risk of inaccurate reporting.28,29 However, this survey did not explore the use of estimated weight when administering propofol. Our survey found that most Smart Pump containing DERS profiles for propofol administration do not consider the weight based minimum and maximum rates as mg/h and mL/h settings are more predominant in England compared to mg/kg/h settings. This suggests that limits are not individually calculated for each patient, and a consensus maximum rate is adopted before a Smart Pump alerts end-users that a potentially excessive rate is being administered. This would therefore require an end-user to manually calculate the maximum infusion rate for a patient, unless other clinical decision support tools are available to the end-user. Doses of propofol which exceed 4 mg/kg/h for greater than 48 h have been associated with increased risk of PRIS (Propofol-related Infusion Syndrome) 30 and PRIS has an associated mortality rate of 36.8%. 31 Therefore, this study highlights an opportunity to standardise DERS settings to administer weight-based medications to enable individualised maximum doses to be calculated by the pump, reduce potential human calculation error and improve patient safety.
A recent retrospective observational study has also highlighted discrepancies with documented amounts of propofol given on an ICU when reviewing electronic patient record documentation and scrutinising infusion pump records. In 4.0% of these patients, a Smart Pump identified that doses which may put patients at risk of PRIS had been administered due to documentation of additional bolus doses administered. 32 This has implications for practice with the potential for ensuring the safe administration of high-risk drugs using DERS in ICU and future developments of Smart Pump interoperability with electronic prescription charts.
There is an increasing focus on reduction in carbon emissions and sustainability practices on ICU. 33 Propofol has been identified as a sedative agent with a low carbon footprint 34 although there are environmental challenges with its disposal. 35 Two intravenous infusion pump devices that are commonly used for propofol are a syringe driver and a volumetric pump. We found that most units do not withdraw propofol into a syringe for administration, which uses fewer plastic syringes. This is an opportunity to standardise administration methodology by administering directly from the vial, 36 however, practical issues such as transferring patients need to be considered as syringe pumps may be preferable in this instance.
Governance of DERS in ICU
We found that approximately two-thirds of units with Smart Pump containing DERS have a named clinician with responsibility for reviewing and maintaining libraries. Several members of the MDT have been cited as the named clinicians with the responsibility of reviewing and maintaining DERS libraries. Interestingly, recommendations for implementing DERS suggest that MSOs and Medicines Device Safety Officers (MDSOs) should have oversight of these libraries with input and collaboration with local expertise. 37 This survey identified that this group accounted for 4.08% of roles with the main roles including Consultants (38.74%) and Pharmacists (40.81%). Previous scoping exercises have identified an MDT approach to setup and implementation. However, following implementation, pharmacists assume responsibility for DERS libraries 38 although it is important to note that this group are not typically the end-users for these devices. Therefore, pharmacists alone may not be the appropriate group for investigating errors using DERS.
Furthermore, this survey has identified that over 64.0% of DERS libraries are not locally scrutinised by auditing usage and error rates through operational or governance structures. This suggests that opportunities to develop libraries with end-user input are not realised, which has previously been highlighted. 39 In addition, there is a need for automated high quality error reports when reviewing incidents to improve medication safety, as the value and frequency of voluntary reporting may offer little benefit 40 and previous retrospective DERS severity analysis has demonstrated intravenous medication administration risk reduction. 24 ICU is a clinical specialty which has thrived on sharing practice and quality improvement initiatives, and the benefits of leading the way with sharing and developing DERS libraries have the potential to ensure standardisation and improved medication safety for patients. Further research into the governance of DERS is required to identify risk and improvement opportunities.
Nursing workforce and DERS
The nursing workforce in ICU has changed significantly over the last 10 years. Many experienced critical care nursing staff have left the profession, which has been exacerbated due to the COVID-19 pandemic, alongside an influx of international nursing staff that require more support and supervision. 41 It is important to note that experience does not necessarily correlate with competence, therefore this survey has reviewed the provision of Step competencies. 42 This survey has identified that dedicated supernumerary Clinical Nurse Educators are present in most units to train this workforce.
This study explored nursing competencies in GPICSV2 to identify if there is any correlation with Smart Pump operational use and governance on ICU. We only identified one significant association between the presence of a Smart Pump containing DERS and having a Clinical Nurse Educator with a postgraduate certificate in education, although this result is likely to be coincidental and may be an indicator of unit size and advanced therapy provided in larger units. Notwithstanding, the inclusion of nursing workforce variables was still considered worthwhile. Studies examining Smart Pump implementation and impact on medication errors have suggested the need for initial and refresher education and training of end users of Smart Pumps, 6 alongside the role of clinical staff engagement and education in adopting and using DERS libraries safely. 10 Although there was an absence of strong associations between nursing variables, it is still possible that nursing workforce factors shape how these systems are embedded and sustained. A more robust approach for reviewing Smart Pumps on ICU as a complex system should be undertaken using the Systems Engineering Initiative for Patient Safety (SEIPS) model in future research. 43
Strengths and limitations
Our survey had a good response rate across England. We have identified inconsistencies with Smart Pump containing DERS governance and application in ICU which has highlighted different research opportunities as a result of this survey. We ensured that appropriate clinicians completed the survey with expertise in this area; however, there may be response bias due to self-reporting.
Our survey did not explore dosing weights for different patient populations, such as dosing propofol in obese patients. We did not ascertain whether prescribing units were the same as administration Smart Pump units for propofol. Furthermore, the clinical significance of exceeding the maximum rate on a Smart Pump and the risk of developing PRIS is unknown.
Our survey did not investigate other high risk intravenous medications, such as opioid infusions, inotropes and vasopressors which would have further strengthened the study results.
In addition, we did not explore the relationship between the named clinicians and MSOs, MDSOs and Patient Safety Specialists. Whilst the role of clinician with Smart Pump oversight on ICU was requested, it may not account for the overall organisational governance structure as we focused on one specific clinical area.
Finally, we did not explore the training competencies and requirements and for DERS at different units.
Conclusion
This benchmarking survey has identified that there is a lack of standardised DERS settings for the anaesthetic agent propofol and inconsistent approaches to Smart Pump containing DERS governance oversight across ICUs in England. We have not identified any significant correlation between nursing competencies and educational infrastructure and DERS implementation on ICU. Further research is required to understand the clinical significance of the variability we have identified.
Footnotes
Acknowledgements
The authors would like to thank all the participants who agreed to take part in this study, as well as the national and regional ICU specialist clinical networks for facilitating roll out across England. The authors would like to also thank Dr Nick Truman (East Lancashire Hospitals NHS Trust (ELHT)), Dr Matt Smith (ELHT), Dr Natasha Lawes (ELHT), Dr Alison McLoughlin (ELHT), Emma Massey (ELHT), Millie Costley (ELHT), Deborah Sutton (ELHT), Yvonne McKean (ELHT), Christine Minnis (Lancashire Teaching Hospitals NHS Foundation Trust), Dr Adam Sutherland (University of Bradford), Michelle Randall (ELHT), Samantha Eccles (University of Central Lancashire) and the Lancashire and South Cumbria Critical Care and Major Trauma Specialised Services Clinical Network for their support in protocol development.
Author note
The views expressed in this report are those of the authors/contributors, and not necessarily those of the National Institute for Health Research or the Applied Research Collaboration North West Coast.
Funding
The authors disclosed receipt of the following financial support for the research, authorship and/or publication of this article: This research is supported by the National Institute for Health Research Applied Research Collaboration North West Coast.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
