Abstract
Each year, around 30,000 intercostal chest drains (ICDs) are inserted in the UK, with complications like displacement being a common concern. Various fixation techniques have been proposed to secure ICDs, but there is no consensus on a gold standard. A scoping review was conducted to identify publications describing ICD fixation methods and frequency with which they become dislodged. Three databases were reviewed: MEDLINE from 1946 to 17th October 2024 through the Ovid® website portal, PubMed®, and the Cochrane Central Register of Controlled Trials (CENTRAL). Appropriate search terms and synonyms were applied with Boolean operators and from 5275 identified records 63 were included for review. Nine ICD fixation principles were identified to classify fixation methods: kinking; Poisson-effect (“Roman Sandal”); suture “through” the tube; tube fixation points (cuffs or wings); friction/adhesion (from ties or dressings); external coiling/locking/flattening; internal balloons; internal coiling (pigtails); subcutaneous tunnelling. Many fixation methods combined more than one principle. Although no definitive conclusions on the best fixation method can be drawn from this review, trends suggest that incorporating sutures or using combined techniques, such as sutures paired with dressings, cable ties or balloon catheters, may enhance ICD security. In laboratory conditions, the highest pull force was associated with the modified Jo’berg knot. Further robust studies are needed to compare the effectiveness of different fixation methods superior in terms of displacement rate, but also taking into account pain, skin integrity, wound leakage/infection, or ease of use.
Introduction
A working, well-positioned, intercostal chest drain (ICD) can be precious, particularly in mechanically ventilated, intensive care unit (ICU) patients. ICDs are used to allow drainage of air, blood, pus, or effusion fluid from the pleural space, and they are commonplace in the ICU in the management of trauma, infection and after surgery. Estimates of how often ICDs become partially or completely dislodged vary between 6% and 42% and incidence reportedly increases in ICDs in situ for greater than 24 h.1–5 ICD dislodgement may result in additional radiological investigations and exposure, need for nursing and medical review, re-positioning or re-insertion. As an estimated 30,000 ICDs are inserted every year in the UK, preventing dislodgement is an important consideration.6,7
Furthermore, ICD insertion is associated with significant risk of complications, including misplacement and visceral damage, making them the subject of alerts and guidelines.8,9 Minimising the need for re-insertion has obvious safety implications, as well as being economically advantageous and kinder to the patient.
Many different techniques of ICD fixation have been described but there is no agreed gold standard, and it is unclear if any specific fixation technique is superior at reducing the risk of displacement. Many descriptions of fixation techniques are brief and ambiguous.7,8,10,11 Advanced Trauma Life Support® course (ATLS®) and British Thoracic Society (BTS) guidelines both recommend using sutures, but do not recommend a method of suturing.7,12
The aim of this work is to identify the range of published ICD fixation techniques and evaluate whether any have been demonstrated to be more secure.
Methods
We performed a structured search of MEDLINE, PubMed® and the Cochrane Central Register of Controlled Trials (CENTRAL) from 1946 to 17th October 2024 seeking publications describing fixation techniques or a comparison of the frequency of complications associated with different methods of fixation. Controlled trials (whether randomised or not), observational studies, laboratory studies, editorials, and items of correspondence were all considered for inclusion.
The search was performed and reported according to principles outlined by the Joanna Briggs Institute and the Preferred Reporting Items for Systematic reviews and Meta-Analyses extension for Scoping Reviews (PRISMA-ScR) guideline. 13 The aims and methodology were agreed a priori but not pre-published in the international prospective register of systematic reviews (PROSPERO) which does not accept scoping reviews. In keeping with similar reviews, ethical approval was deemed unnecessary.
English language articles referring to temporary drains placed transcutaneously into the pleural cavity in either adult or paediatric practice were considered, including those placed using Seldinger or blunt dissection techniques, and those placed during surgery. All designs and sizes of ICD were included, and for the purposes of this review, any reference to “small bore” drains was interpreted as a drain size of less than 18 Fr (French gauge) which has a 6 mm outer diameter. Laboratory studies, including live animal, cadaveric, or simulation models, were included if deemed relevant to human practice.
Studies describing drainage systems connecting two body cavities, methods of wound closure rather than drain fixation, or long-term (or outpatient) ICDs were excluded.
The following search terms were used with the appropriate Boolean operators and wildcards to identify articles relating to ICDs: “thoracostomy,” “intercostal,” “pleural,” “chest”; “Seldinger,” “surgical,” “Wayne,” “Fuhrman,” “pigtail”, “tube,” “drain,” “catheter.”
Terms (including wildcards) used to identify different fixation techniques (when combined with the above terms) were: “fixation,” “securement,” “anchor,” “suture,” “stitch,” “adhesive,” “dressing,” “balloon,” “cuff,” “pigtail.”
After de-duplication, titles and abstracts of returned articles were independently screened by two investigators (MB and CW) according to the above a priori eligibility criteria. Where the inclusion of an articles was not clear, it was reviewed and discussed jointly by MB and CW to arrive at a consensus decision. This was required where articles only partially fulfilled the inclusion criteria, for example those that used Foley catheters as chest drains.
For studies deemed eligible for inclusion, the following data were extracted: authors, publication date, journal, title, country of origin, fixation technique, type and frequency of complications (where described), population and clinical setting.
Results
A total of 4531 records were identified by database searching and underwent title and abstract screening, with 159 articles selected for full-text review and 63 included in the final analysis (Figure 1). Of these, 30 were descriptions of techniques with no associated analysis.14–43 There were 33 studies which examined or compared the efficacy of fixation techniques,2,3,44–74 including 10 laboratory studies, including both simulations and alive and cadaveric animal models44–53; and 23 human clinical studies,2,3,54–74 of which five involved children.65–67,69,73
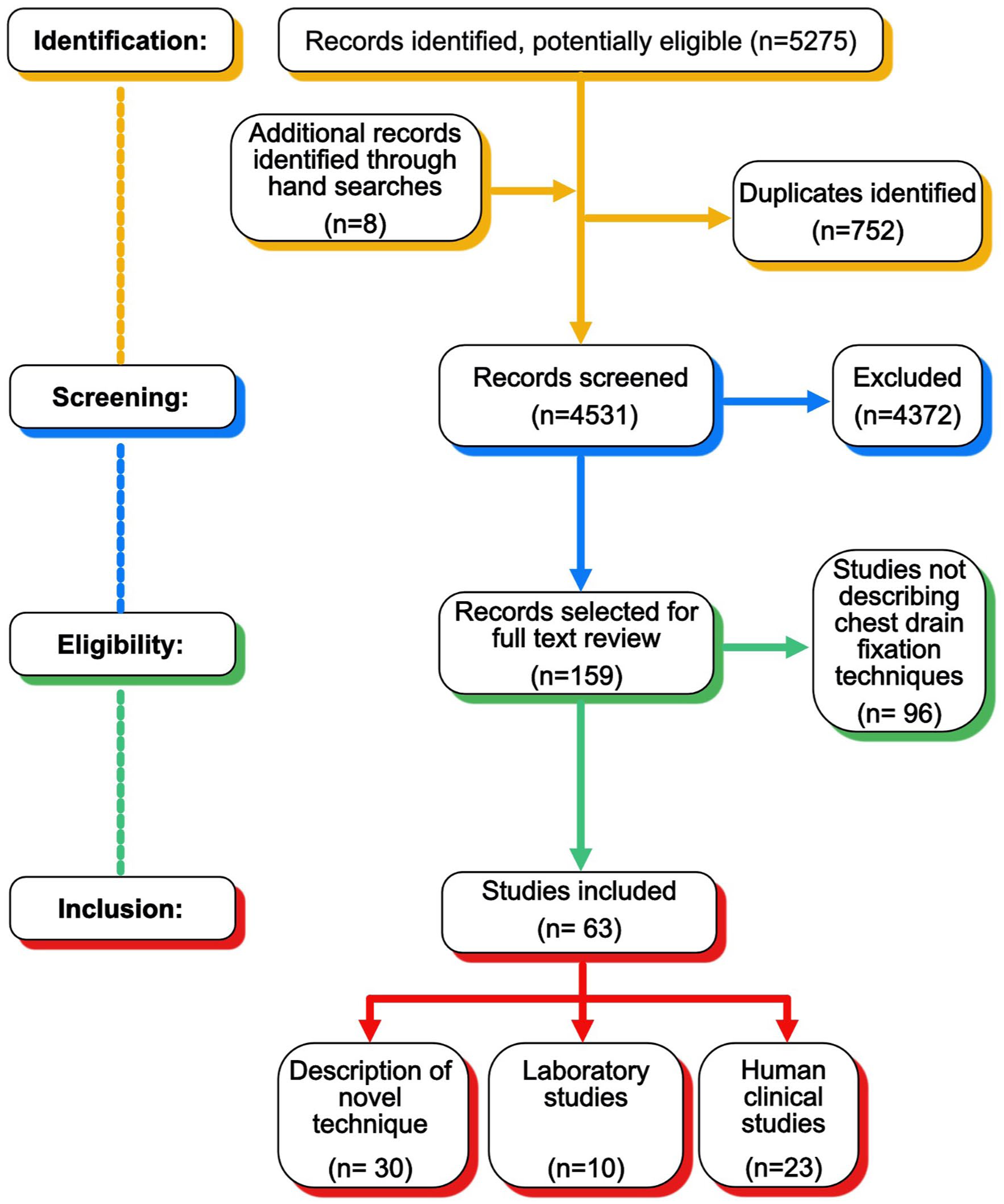
Flow diagram of literature search for intercostal chest drain fixation methods.
Fixation techniques
Thirty articles described one or more ICD fixation techniques (Table 1).14–43 From these articles, nine common principles were identified as a means of classifying methods used to secure ICDs: kinking; Poisson-effect (“Roman Sandal”); suture “through” the tube; tube fixation points (cuffs or wings); friction/adhesion (from ties or dressings); external coiling/locking/flattening; internal balloons; internal coiling (pigtails); subcutaneous tunnelling (Table 2). Several ICD fixation techniques combined several of these principles, and some articles reported using equipment designed for other purposes, such as cable ties and urinary catheters, for ICD fixation.18,31,47,60
Published descriptions of one or more novel techniques for intercostal chest drain fixation.
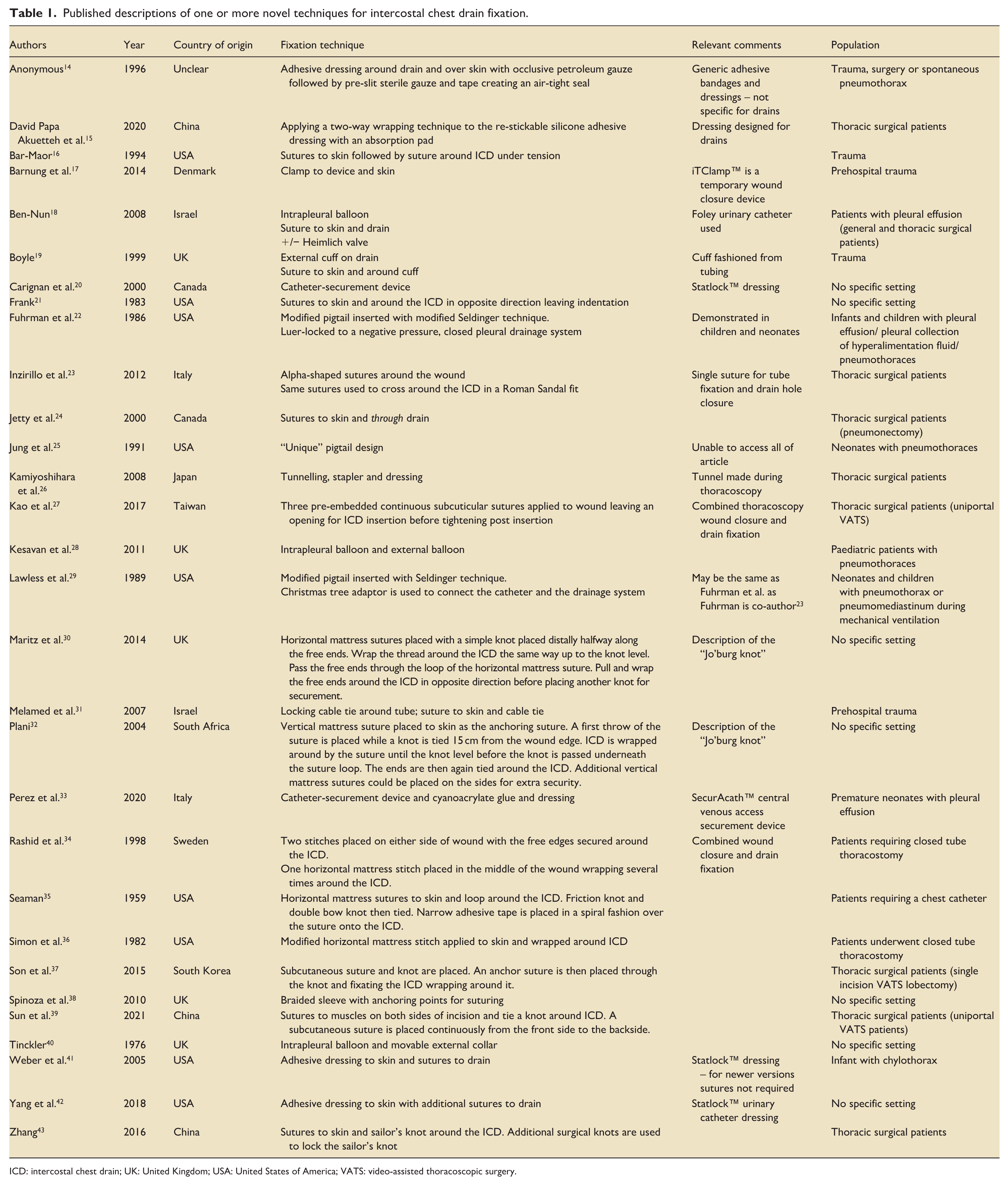
ICD: intercostal chest drain; UK: United Kingdom; USA: United States of America; VATS: video-assisted thoracoscopic surgery.
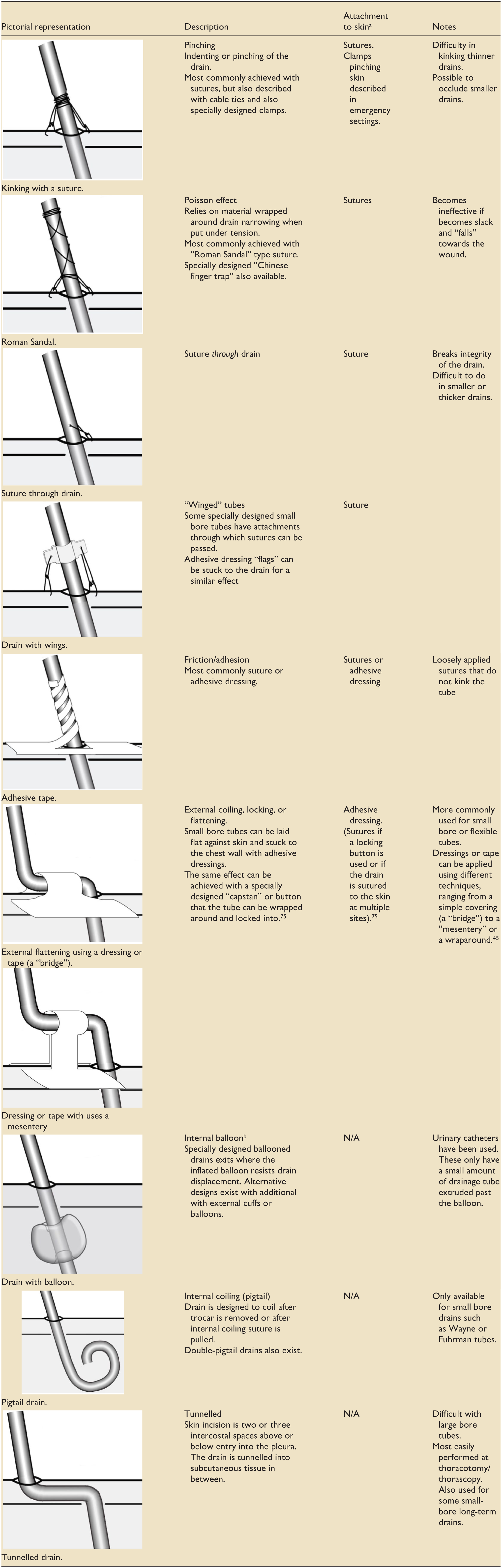
Classification system of intercostal chest drain fixation principles.
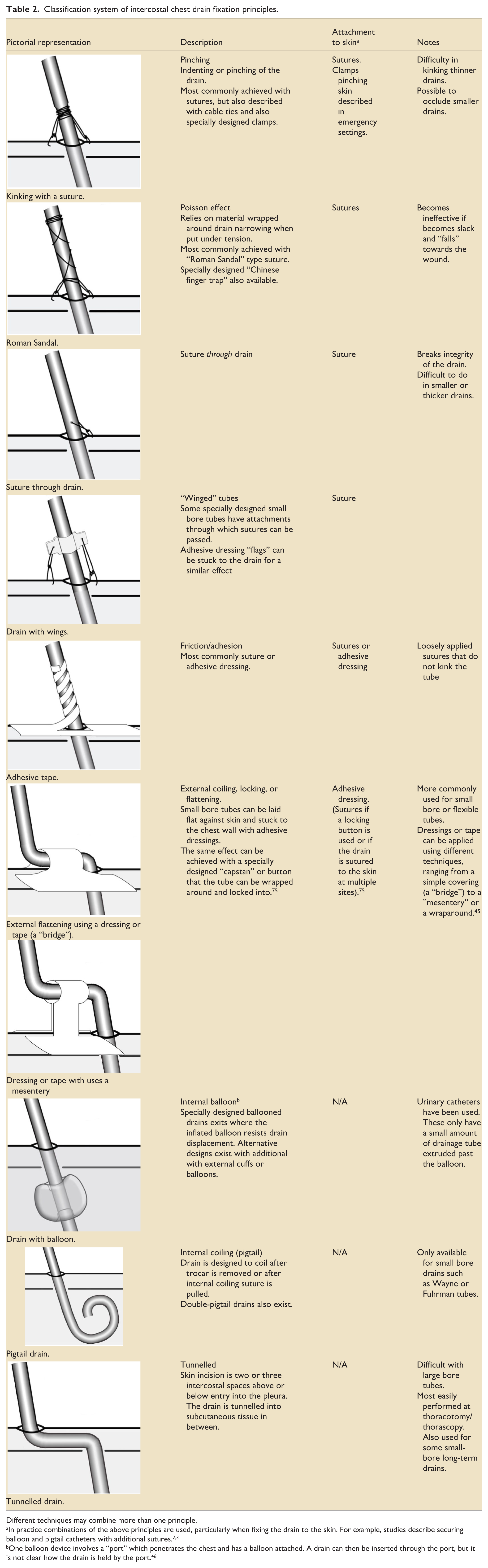
Different techniques may combine more than one principle.
In practice combinations of the above principles are used, particularly when fixing the drain to the skin. For example, studies describe securing balloon and pigtail catheters with additional sutures.2,3
One balloon device involves a “port” which penetrates the chest and has a balloon attached. A drain can then be inserted through the port, but it is not clear how the drain is held by the port. 46
Laboratory studies
Table 3 summarises laboratory and simulation-based studies of ICD fixation techniques.47–54 There was no standardised assessment of the efficacy of different techniques. Some studies compared the absolute risk of displacement, while others measured the length of tubing displaced by force, or the time until complete displacement. Experimental methods involved either a continuously increasing force, repeated pulling events using a predetermined force, or subjective estimates of force. Different fixation techniques withstood peak pull forces (i.e. the force required to dislodge an ICD) ranging from 19 to 180 N (Table 4). For comparison, a previous ergonomics paper has suggested that the average peak pull strength of a sample of young men in a standing position was approximately 150 N. 76
Laboratory studies (including animal or simulation models) analysing different types of intercostal chest drain fixation methods.
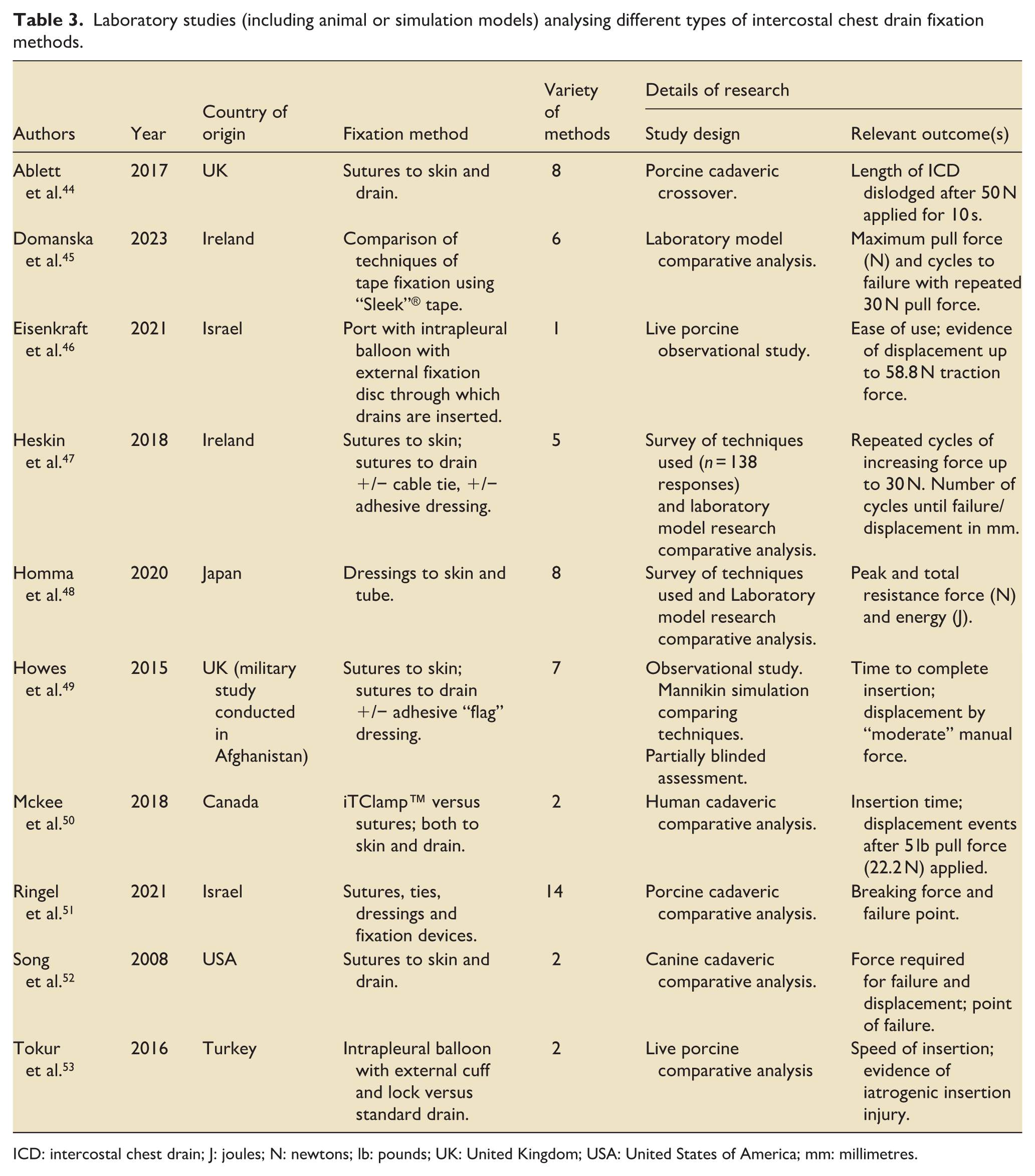
ICD: intercostal chest drain; J: joules; N: newtons; lb: pounds; UK: United Kingdom; USA: United States of America; mm: millimetres.
Comparison of the peak pull forces at which failure occurs with ICD fixation methods.
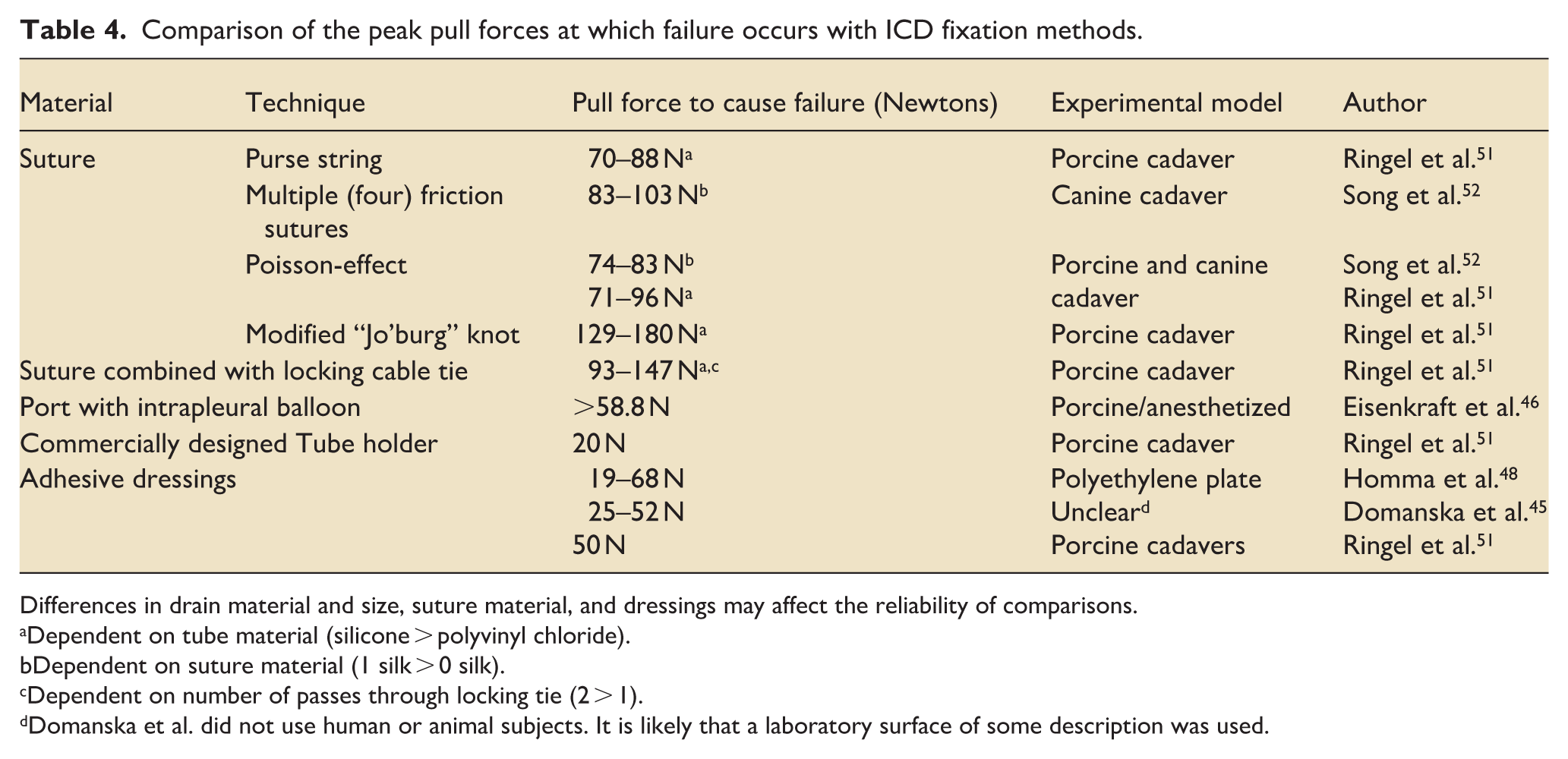
Differences in drain material and size, suture material, and dressings may affect the reliability of comparisons.
Dependent on tube material (silicone > polyvinyl chloride).
Dependent on suture material (1 silk > 0 silk).
Dependent on number of passes through locking tie (2 > 1).
Domanska et al. did not use human or animal subjects. It is likely that a laboratory surface of some description was used.
Suturing techniques appeared to withstand the highest forces, with the modified “Jo’burg” technique being highly resistant to displacement, resisting forces up to 180 N (Newtons). 51 The modified “Jo’burg” technique is a hybrid technique that combines elements of both pinching and Poisson effects (Figure 2).
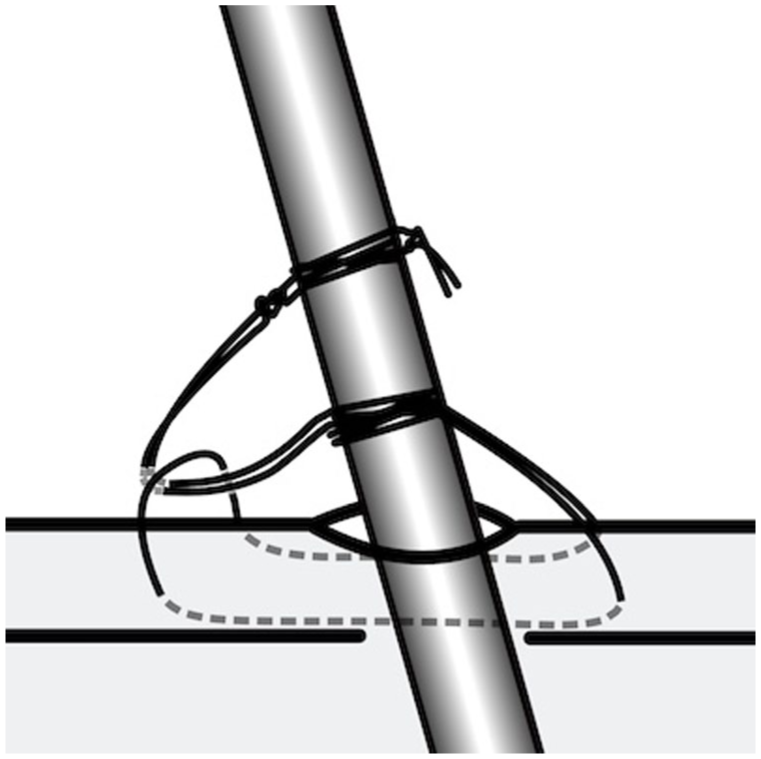
Modified Jo’burg knot suture fixation technique.
Although commonly used suturing techniques that rely on the Poisson-effect (“Roman Sandal”) appeared to perform well in laboratory studies, some studies suggested that it was prone to becoming loose with the wrappings slipping down the tube.49,51 Heskin et al. found that the Poisson-effect was made more effective by the addition of cable ties or adhesive dressings to prevent slippage. 47 Combination techniques performed favourably in some studies, however the only force measurements were those from Ringel et al. involving cable tie and suture combination – these performed well (approximately 100–150 N), although not as well as the modified “Jo’burg” knot. 51 Adhesive dressings did not perform as well in laboratory studies with displacement forces ranging from 19 to 68 N.45,48,51
Studies in humans
There were 23 studies that identified that examined ICD fixation in humans (Table 5).2,3,54–74 Four studies described combined techniques of wound closure and drain fixation in patients undergoing thoracoscopic surgery.54,56,59,71 They were among several studies addressing skin discomfort or injury/healing as the outcomes of primary interest.57,58,60,62,74
Human clinical studies analysing or comparing different types of intercostal chest drain fixation methods.
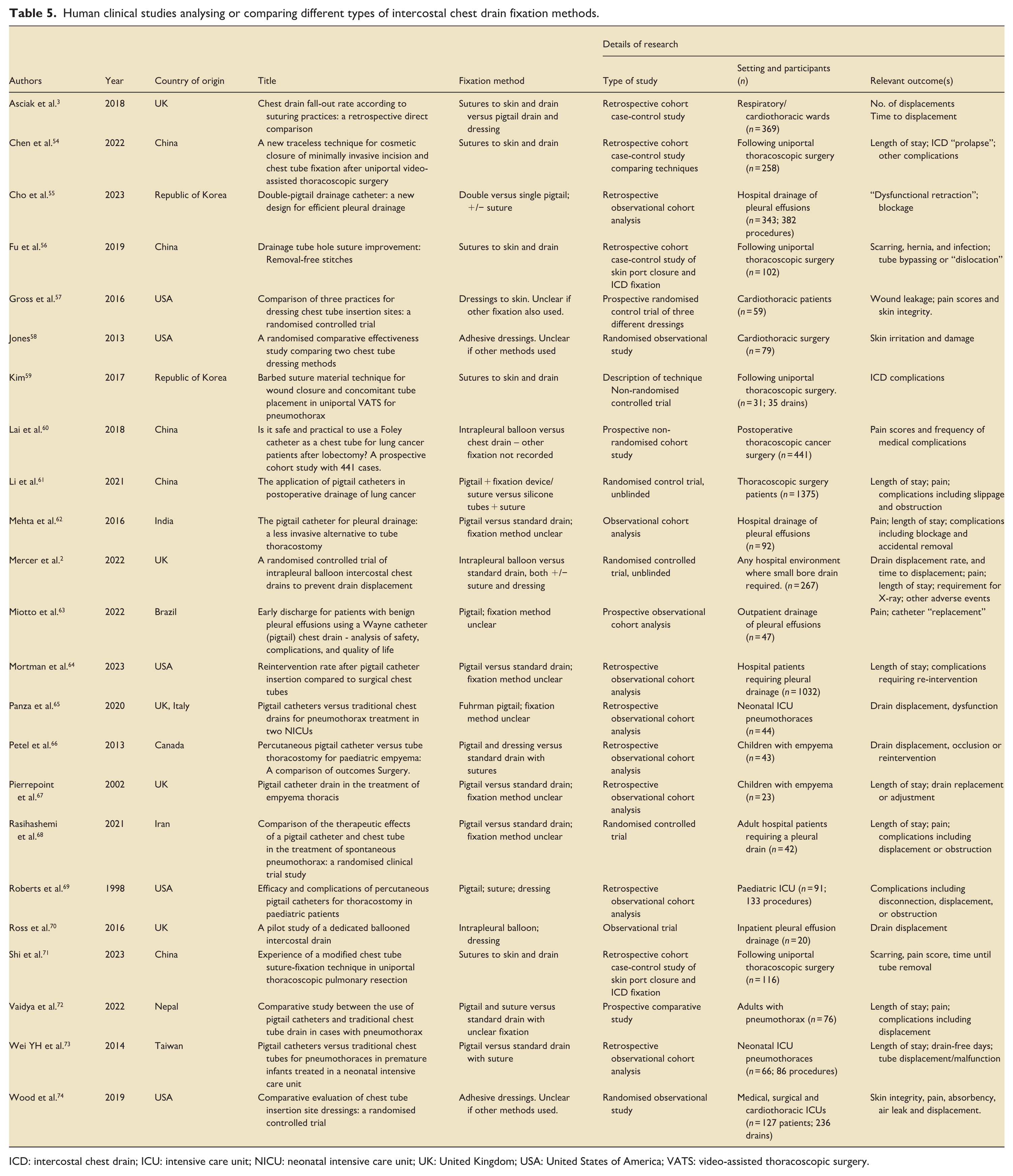
ICD: intercostal chest drain; ICU: intensive care unit; NICU: neonatal intensive care unit; UK: United Kingdom; USA: United States of America; VATS: video-assisted thoracoscopic surgery.
A total of 13 studies involved pigtail ICDs.3,55,61–69,72,73 Five such studies were conducted on children (where body size often necessitates small diameter ICDs and where external methods of skin fixation other than dressings are challenging).65–67,69,73 Mortman et al. one of the largest retrospective studies, indicated a significantly higher incidence of displacement with pigtail drains compared with surgical ICDs. 64 Double pigtail drains may have a lower displacement rate compared with standard pigtails. 55
Mercer et al. investigated a custom-made ICD with an integral balloon and identified a lower incidence of drain displacement compared with standard 12Fr ICDs, but also a minor increase in adverse events including difficult or painful removal. 2 Two further studies also compared how well balloons secured tubes, but these involved the use of Foley urinary catheters as ICDs, a practice that would be considered off-label usage in many countries.18,60
Discussion
In this scoping review we classified ICD fixation systems using nine principles and have reported a wide variety of laboratory and human studies assessing the comparative performance of fixation techniques that employ those principles. Unfortunately, between-study methodologic and reporting heterogeneity means definitive conclusions on the superiority of any one fixation technique cannot be offered. The type and size of the ICD tube, the suture material and size, the use of any dressings, and the experience of the health practitioner are also likely to play a part.49,51,52 Given the paucity of definitive evidence, it is perhaps unsurprising that ATLS® and BTS guidelines, arguably the most relevant, do not advocate any specific fixation technique.3,12
The literature does, however, allow some conclusions to be drawn. Porcine cadaveric research suggests that the modified “Jo’burg” technique is very resistant to displacement, resisting forces up to 180 N. 51 Our review also suggests that combining different methods of securement, for example combining adhesive dressing with sutures, or suturing pigtail, small bore Seldinger, and balloon drains, may be more successful at preventing dislodgement than single techniques alone.2,3,47 In fact, BTS guidelines recommend that small bore or pigtail ICDs are sutured alongside any other fixation method, based in part on the results of Asciak et al.3,7
Another BTS recommendation is that any adhesive dressings should involve a “mesentery” or “omental tag” (see Table 2, dressing or tape with uses a mesentery). 10 The paper by Domanska et al. would seem to cast doubt on this suggestion as it found that a higher force was required to dislodge a drain with a “bridge” covering (see Table 2, external flattening using a dressing or tape (a “bridge”)) than those with a mesentery. 45 However, insofar as comparison between studies is possible, our scoping review finds that that adhesive dressings appear less effective than sutures in preventing ICD dislodgement (Table 4).
Some fixation techniques may have limited applicability. Although a large proportion of included studies involve pigtail drains, their use remains contentious for several indications. 64 Another example, tunnelling, is typically only feasible for large bore drains inserted during surgical wound closure. In contrast, certain techniques may provide added benefits in specific circumstances. For example, balloon-tipped urinary catheters have been deliberately used to tamponade bleeding intercostal vessels. 77 Some intraoperative techniques combine chest drain fixation with wound closure aiming for improved cosmetic results.
The re-purposing of medical equipment as ICDs, including central venous, Bonnano, and urinary catheters, was described in several papers that were excluded at the screening stage. Off-label use of equipment not designed for chest drainage is discouraged as it leaves health organisations and professionals liable in the event of adverse reactions. 78 In spite of this, we chose to include two references to Foley catheters in our review due to the size of the cohorts examined, and the potential requirement for non-standard approaches to ICDs in low-resource settings.18,60
One of the strengths of this study is that it had very broad search criteria which meant a wide range of methodologies were reviewed. These included living and cadaveric, human and animal models. By way of contrast, a weakness of this study is that it was not possible to synthesise all of the available results into definitive recommendations on fixation technique. Only 15 studies compared frequency of dislodgement, but often this was as a secondary outcome with methodology that was poorly described and involved small numbers of participants.2,3,54–56,61,62,66–69,72–74 Another weakness of this study is that it has not been possible to identify the frequency with which different fixation techniques are encountered in the ICU setting or in other clinical scenarios. The largest audit of UK ICDs did not record which techniques were used, only that “accidental dislodgement of chest drains should be avoided by adequate fixation.” 4
We also recognise that bland dislodgement rates are only one aspect of what might make one fixation method better or worse than any other. Consideration of insertion time, expertise required, cost, patient experience (including pain), skin integrity, and wound leakage (including subcutaneous emphysema and wound infection) should all be considered important. Many of these factors were outcome measures in several of the studies we reviewed.2,56–58,60–63,71,74 Future research should combine examinations of the security of different fixation methods with the other outcomes described above.
Conclusions
Despite the recognised problems associated with of ICD fixation failure, research in this field has been sporadic and inconsistent. This review has attempted to summarise existing research to inform current practice and future research needs. Individual expert practitioners with established ICD fixation techniques acceptable to their institution and patients should be reticent to alter practice based solely on this review of the literature. However, we can cautiously suggest that it was possible to identify certain trends. For example, the more secure ICD fixation techniques identified in this scoping review appear to be those involving sutures or sutures combined with cable ties or adhesive dressings. Of the suture techniques for which evidence was available, those which indented the chest drain were more successful than those that did not, whilst in a laboratory setting the highest identified pull force identified was associated with the modified Jo’berg knot.
Footnotes
Author contributions
Study design, planning, conduct: CW, MB, DWH. Writing, and revision of manuscript: all authors.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study/project is funded by the NIHR - i4i Product Development Awards (PDA) - Breakaway Chest Drain Valve (Reference: NIHR204562). The views expressed are those of the author(s) and not necessarily those of the NIHR or the Department of Health and Social Care.
Declaration of conflicting interests
The authors declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: MB receives an annual honorarium for work with Quotient Sciences.
The other authors have no interests to declare.