Abstract
Background:
Improved survival from critical illness in recent years has led to an increase in patients with Post Intensive Care Syndrome (PICS). Routine, dedicated, specific and individualised assessment, rehabilitation and follow-up after critical care discharge is recommended but is currently inadequate in the UK. The aim of this study was to explore patients’ and family members’ experiences of a critical care admission, focussing on recovery and rehabilitation.
Methods:
As part of an intervention development programme, a series of iterative focus groups with survivors of critical illness and their family members was held. Parallel groups with staff involved in the care and rehabilitation of critically ill patients were also conducted. Participants mapped out their recovery journey identifying key moments and challenges and shared their recommendations for recovery and rehabilitation. Brokered dialogue was used to enable patient and staff groups to ask and answer questions of each other. Data analysis was completed using reflexive thematic coding.
Results:
Thirty-four participants attended the focus groups, with 28 attending the first two groups discussed in this paper. Using the experiences described by the participants, three overarching themes were identified; fear, helplessness and frustration. Participants also reported both short and longer-term consequences of ICU admission and shared their priorities and advice for recovery and rehabilitation.
Conclusion:
Critical care admission is a traumatic experience for patients and family members. Our data highlights patients’ needs for ongoing, holistic support during a stay in critical care and beyond.
Introduction
Improved survival from critical illness in recent years has led to an increase in patients with chronic cognitive, psychological and physical impairments known as Post Intensive Care Syndrome (PICS).1,2 Multidisciplinary assessment, rehabilitation and follow-up is recommended 3 but not routinely delivered. Despite published NICE guidance on rehabilitation after critical care in 2009, and further quality standards in 2017,4,5 currently less than a third of Intensive Care Unit (ICU) patients in the UK receive dedicated outpatient follow-up 2–3 months after ICU discharge6–8 although the availability of follow-up clinics has improved.4,5 An editorial in the British Medical Journal in 2021 highlighted the lack of adequate post-ICU rehabilitation, emphasising the serious consequences for individuals and associated increased costs to the NHS, particularly from unplanned readmissions. Research to determine the most clinically and cost-effective rehabilitation strategies should be a priority, with collaboration between patients, funders and researchers to identify and address evidence gaps. 8
The UK Guideline for the Provision of Intensive Care Services (GPICSv2.1) 3 highlights that leaving ICU is only the start of a long recovery process which may take months to years, and that there may be considerable residual impact on patients’ morbidity and longevity. Recommendations include monitoring outcomes and recovery progression using measures appropriate for the stage of recovery and individual therapy dependent on local resources. This includes personnel, equipment and finance plus a specialist coordinator to facilitate oversight of the rehabilitation pathway. Delivery of services to these standards, especially after leaving hospital, is improving but still has a long way to go. 9 A national survey in 2021 found that the biggest barriers to delivery of adequate critical illness recovery and follow-up services were lack of funding and availability of sufficient staff. 10
The need to think of alternative strategies to deliver therapeutic interventions such as home-based services and virtual platforms to “ensure maximum inclusivity for patients into rehabilitation programmes” has been considered against the limited availability of resources. 10 However, the need for careful management to prevent issues such as digital poverty and literacy from limiting access should also be considered. Current literature highlights that research into improving post-ICU recovery is essential and is strongly suggestive that the development of accessible, inclusive interventions to aid recovery should be of central prominence.
In response to this, we wanted to explore the patient experience of critical illness and recovery and identify their key issues and concerns, with the ultimate aim of developing and co-producing a patient-centred and relevant intervention to aid recovery. Here we discuss the lived experiences of ICU survivors and their families during and after an admission to critical care. A patient-centred approach was important from the start to help shape the focus of subsequent stages of the project ensuring any resulting intervention would address patients’ needs. This approach is supported by GPICSv2.1 which advocates proactive involvement of patients in setting their rehabilitation plan. 3
Methods
This study used qualitative methods including graphic elicitation of experiences via timelining, 11 further elicitation activities included brokered dialogue 14 and facilitated discussion within focus groups. Ethical approval for this study was obtained from North East-York Research Ethics Committee ref 23/NE/0113.
Recruitment and consent
Participants were recruited through advertisements using local social and professional networks and contacts including the Welsh Intensive Care Society and local ICU follow-up support groups, and nationally using social media (“X”) and
Focus groups
We planned our focus group sample sizes to include four to eight participants sharing the required background (critical illness survivor, family member or healthcare professional) along with two to four members of the research team including trained facilitators and an intensive care consultant. This number was planned to allow each participant sufficient opportunity to express their views, for the facilitators to be able to moderate, seek clarification and further exploration of any differences in views and analyse the transcripts afterwards, as well as allowing for last minute “no shows.” 13 A series of iterative focus groups was planned. Each group was offered multiple times across a combination of in-person and on-line environments to maximise opportunities for attendance and ensure richness and diversity of information shared. Facilitators guided participants through specific activities detailed below and ensured engagement from all. Groups were audio recorded for verbatim transcription. Hand-written notes and observations were also documented by the research team. The researchers facilitating focus groups included a critical care consultant and a research fellow with a background in qualitative research and cognitive behavioural therapy. The team also included non-participatory observers: a final year medical student; a research fellow with a background in pharmacology and a research officer with a psychology background (Figure 1).
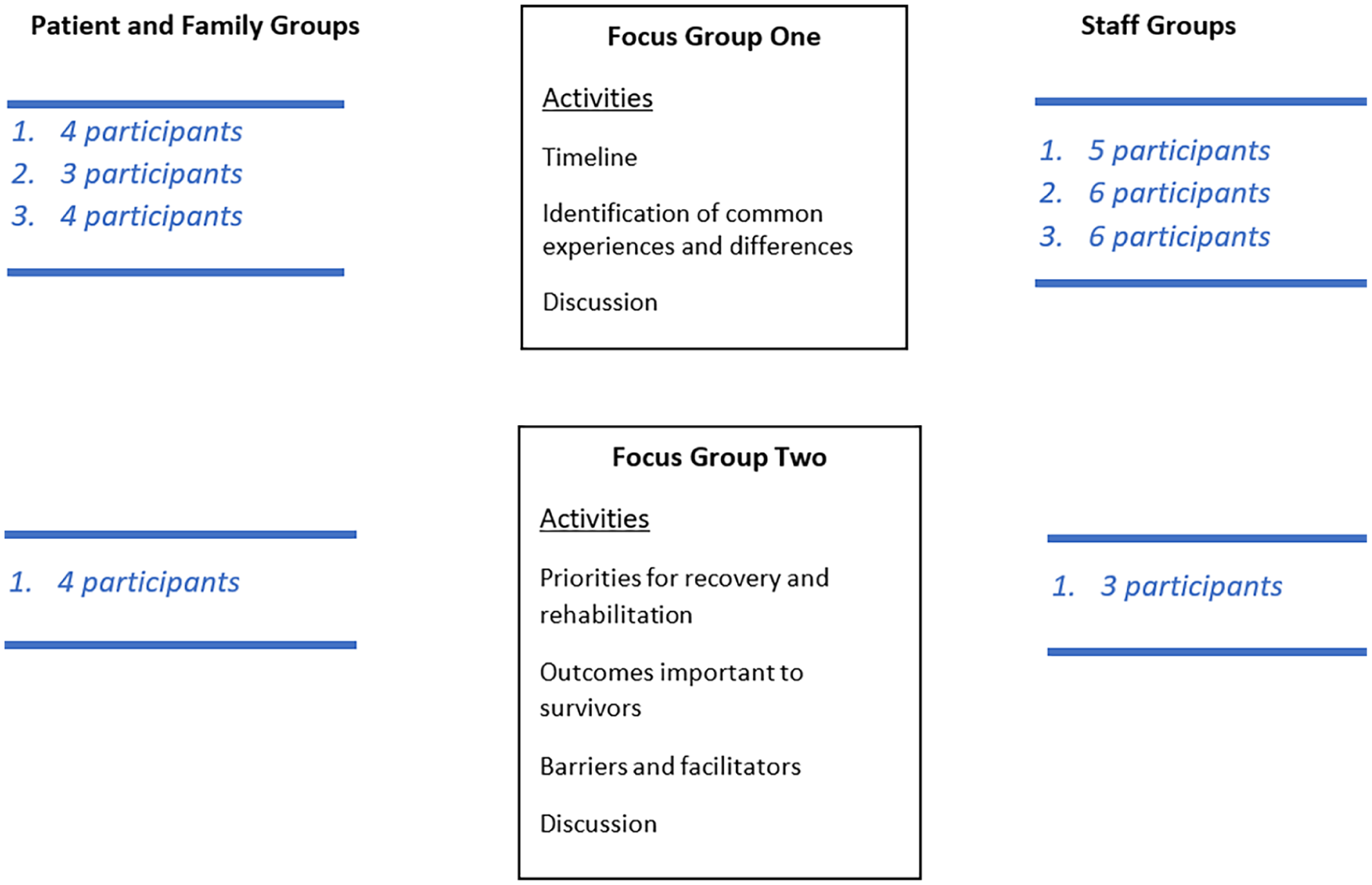
First two focus group activities and participation.
In the first focus group participants were invited to prepare a timeline of their critical illness journey, including key experiences and challenges experienced in relation to their recovery and rehabilitation. Family members were asked to create a timeline of their loved one’s journey from their perspective and staff were asked to make a timeline for a typical patient in their institution. Participants then shared these timelines as a tool for stimulating discussion around the similarities and differences in individuals’ experiences.
In the second focus group, participants were asked to pretend they were going to a desert island and could only take with them: two priorities or activities to support recovery and two priorities or activities to support rehabilitation. We defined recovery as “getting back to (or as close as possible to) quality of life and health status prior to illness” and rehabilitation as “the process of achieving recovery.” Subsequent focus groups involved building on discussions held in previous and parallel focus groups with healthcare professionals.
Brokered dialogue
We used a research method known as “brokered dialogue” which allows communication between parties that may have seemingly divergent views or perspectives and may not otherwise have had the opportunity to discuss these issues. 14 This method was used between the patient/family/carer groups and the staff groups to encourage each group to ask questions of the other and answer questions in return. The brokered dialogue questions were invited at the end of each focus group and presented to the next group, along with any answers to previous questions.
Analysis
Focus group recordings were transcribed verbatim and subject to a process of cleaning to ensure accuracy and for the removal and/ or alteration of potentially identifying personal information. Notes from facilitators and observers were typed and collated. Transcripts and observational notes were subject to reflexive thematic analysis 15 using both manual coding and NVivo software. Patterns and themes identified were compared and discussed within the research team. Reflexive thematic analysis aligns well with an interpretivist epistemology and our focus on constructing an understanding that acknowledges the subjective and lived experiences of all stakeholders in this study. In co-designing a new health intervention, a realist approach was deemed most appropriate to explore context specific mechanisms, outcomes and gain an understanding of what works, for whom and when. 16
Findings
Focus group one ran six times and focus group two ran twice, with 28 participants in total (See Tables 1 and 2 below for details of participants). Some participants chose to attend both focus groups (six in total; three patients and three staff). All focus groups began with introductions of those present, where many participants offered a brief overview of their experience of critical care, sharing the underlying reasons for critical care admission. Following this, the timeline activity was used as the initial stimulation to explore in more depth, the participant’s experience of critical care admission. The sharing of these stories was clearly highly emotive for those talking about their own health, but also for those sharing stories of observing a loved one in this environment. For some family members, it was clear that discussion of the impact of the critical care admission on the family/ relationship was not something they had engaged with previously and many admitted actively avoiding discussion to prevent further upset on both sides.
Background of focus group participants.
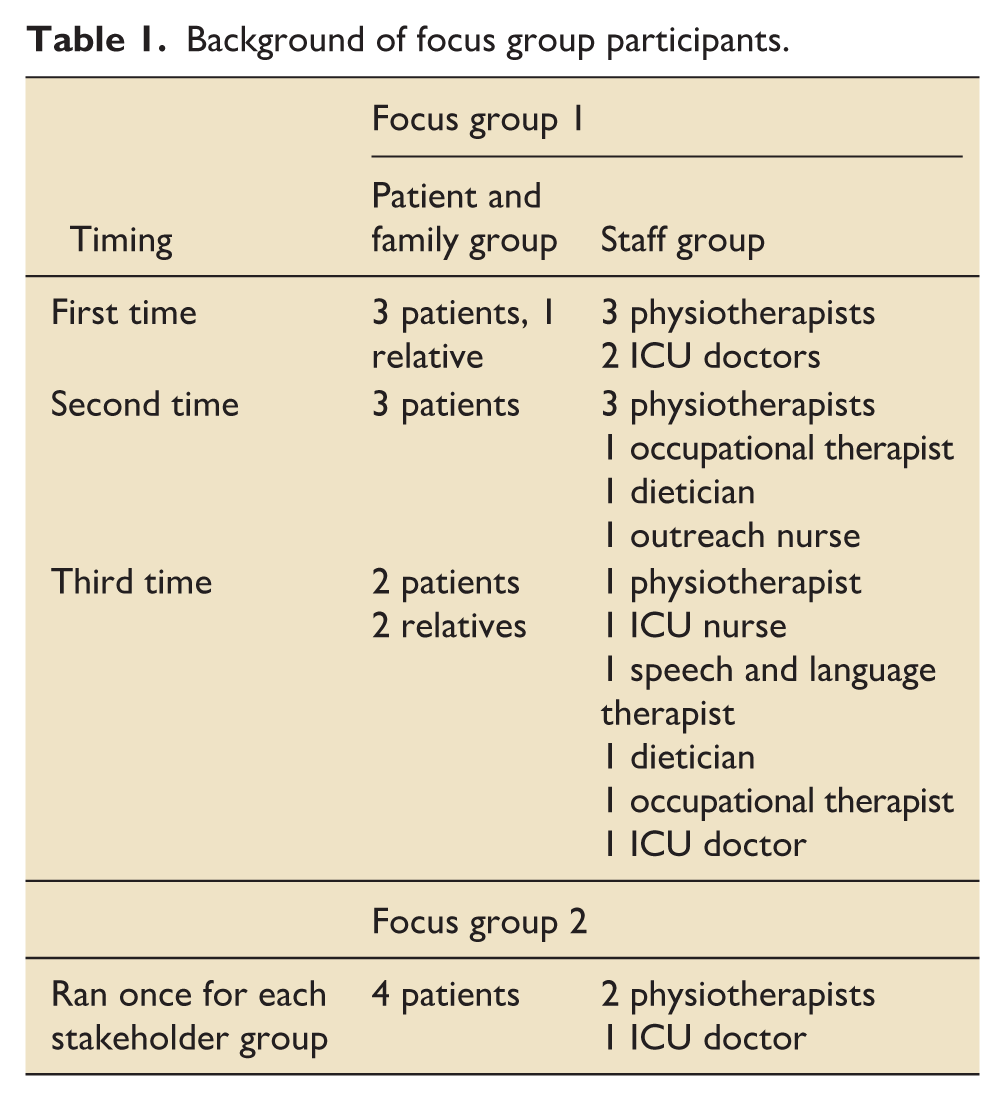
Further details of focus group participants.
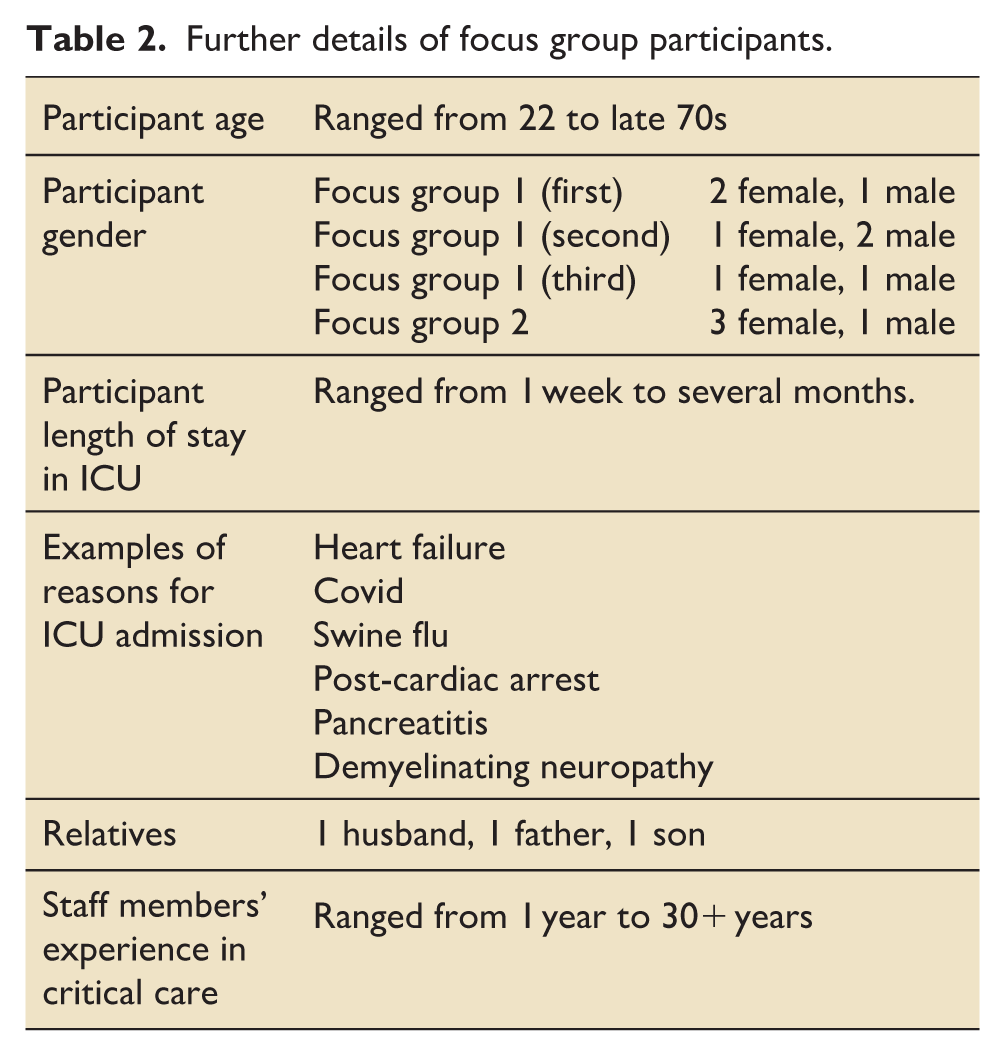
“
Timelines
There was a remarkable similarity between the timelines produced, regardless of the background of the participant (patient, relative or staff member). Key significant timepoints marked on the timelines included: initial admission; period of acute illness and associated interventions such as invasive ventilation or tracheostomy; stepdown to ward and eventual discharge home. Many participants also added challenges such as delirium and low mood as well as milestones such as sitting on the edge of the bed, vocalising, standing and taking first steps.
Themes
Three overarching themes were developed from the data collected in the timelines and discussions; (1) helplessness associated with vulnerability and reliance on others; (2) fear and anxiety as a result of physical incapacity affecting motivation, mood and sleep; and (3) frustration associated with adjustment to a new reality and perception of lack of support or understanding from others.
Theme 1: Helplessness associated with vulnerability and reliance on others
Theme 1 describes the experience of helplessness associated with a critical care admission. This theme applied to patients and their family members and was recognised by staff members. A number of associated subthemes were identified.
Subtheme 1.1: Loss of independence - “an adult baby.”
Most patients and family members found the need for total reliance on staff challenging, ultimately leading to a feeling of helplessness in their overall situation and low mood. The majority of patients in the focus groups had been independent and generally healthy prior to their critical illness and the sudden transition to dependence on others for every basic need was very challenging to experience and accept. Survivors commented that staff made this easier by maintaining dignity and professionalism and getting to know them as a person.
I was too weak, the muscle wastage. I couldn’t really move my arms at all. I described myself as an adult baby. I was unable to talk, communicate. I was unable to move. I was unable to eat solids, I had the NG tube. I was bathed in bed. I was toileted and cleaned in bed. I could do nothing for myself.
Subtheme 1.2: Delirium - “more real than anything else I’d been through.”
For many patients, the delirium was more real than reality and they struggled to differentiate between their delirious memories and what actually happened. This led to a feeling of helplessness for a number of the patients and their family members. Years after their ICU admission, some patients still recall the delirious episodes with incredible clarity and question the validity of their memories, leading to further feelings of helplessness, self-doubt and vulnerability.
I have plenty of memories of horrific terrifying nightmares but no true memories. When I woke from the coma the nightmares carried forward because they were more real to me than the world I was now awake in.
Subtheme 1.3: ward stepdown - “I couldn’t reach my buzzer and I just cried for an hour.”
Transfer from critical care to a general hospital ward appeared on all patient and family members’ timelines as a major stressful event accompanied by a feeling of a loss of control and helplessness. It was very common to feel that this move had happened “too soon” and patients and families alike felt that the ward environment was less safe and supportive than ICU.
I felt abandoned and felt as though I’d left ICU too soon, as though they’ve got you to a stage where you’re stable to them but you weren’t. . .I certainly didn’t feel safe on the ward.
This issue was also identified on staff timelines, who acknowledge that it is a big shock for patients when they move to a ward but that it is difficult to prepare them for this as people don’t understand how it will feel until it actually happens.
Subtheme 1.4: Motivation - “Focus on the today, maybe tomorrow.”
There was also a feeling of determination to overcome this feeling of helplessness, described by a number of participants and the subtheme of motivation came up repeatedly in all focus groups, particularly with regard to goal-setting on the ward and after leaving hospital. Many participants recognised this self-motivation as being key to their subsequent progress and recovery.
Every day I would be doing some exercises..I kept a log of my walking and it was only, it’s really in the end it’s to show that you’re making progress.
Staff members described their delight and satisfaction when they managed to encourage and channel a patient’s motivation into clinical progress and wondered how they could better identify when a patient is reaching this stage and help to promote these feelings. However, there was also a recognition that some patients do not appear to feel this motivation and remain passive and helpless, which is a challenge to manage.
Subtheme 1.5: Staff support - “They made me feel safe and valued.”
All patients and family members described the positive impact of the ICU staff, especially the nurses. This was particularly relevant to the theme of helplessness as patients frequently recalled their dependence on staff for basic support such as moving, feeding, washing, toileting and helping with communication and they appreciated being treated with respect and dignity. Many also described valuing staff for their companionship and feeling the bedside nurse was their advocate. The word “family” was used by a number of participants when describing the staff who helped look after them (“
They normalised the things that were really embarrassing.
Theme 2: Fear and anxiety as a result of physical incapacity affecting motivation, mood and sleep
Theme 2 explores the concept of the fear that both patients and their family members associated with a critical care admission, often causing distress for years after. A number of associated subthemes were identified.
Subtheme 2.1: Difficulty breathing/air hunger - “Continually suffocating.”
This was a common and powerful memory that people still found distressing to recall, often years later. Recollections were vivid, describing the feeling of not being able to breathe or communicate but still being able to think clearly, feeling like dying would be a relief and welcoming the decision for invasive ventilation as the struggle to breathe would be at an end.
It’s just like a packet of air underwater, you have to grab like that, the bubbles, just to sustain you.
Subtheme 2.2: Realisation of illness severity - “I was very emotional.”
While patients’ family members were well aware of how unwell their loved ones were, the patients themselves took time to catch up and understand this and many found that this realisation had a detrimental effect on their mood and motivation. At a time when the family members could see some progress and were starting to have hope of recovery, their fear was reducing whilst the patients were struggling to come to terms with everything that had happened and their fear of relapse or death was escalating.
I didn’t want to exist. I didn’t want to be trapped in this body. I was in so much pain. The reality of everything just hit and you’re saying what just happened?
Subtheme 2.3: Sleep - “I thought I wouldn’t wake up again.”
Problems with sleep were commonly reported throughout every stage of the journey and continued as a long-term issue for many participants. Most patients however described the issues regarding sleep in relation to overwhelming feelings of fear.
Utter exhaustion, utter, utter exhaustion but just completely unable to sleep. It was almost as though my body was too scared to switch off.
Theme 3: Frustration associated with adjustment to a new reality and perception of lack of support or understanding from others
The third theme describes the feelings of frustration that were common in many of the participants. As they progressed through their physical rehabilitation, they felt their brains needed more stimulation and they felt there was insufficient support to help with the adjustment back to life at home and the lifelong impact of an episode of critical illness. A number of associated subthemes were identified.
Subtheme 3.1: Boredom - “There was no entertainment really to motivate your mind.”
Patients overwhelmingly identified boredom as one of the key experiences of critical illness recovery, especially after ward stepdown when people were often still unable to do anything independently but no longer had a critical care nurse always by their side and had to wait their turn for attention and support.
You’re just left, sometimes you’re just left with a telly or a radio and your own thoughts. What, how do you stimulate people’s brains as well to keep them active as well as the body?
Subtheme 3.2: Going home - “It all felt really sudden.”
This was another stressful time leading to feelings of frustration identified on all timelines and in focus group discussions. Similar to ward stepdown, this time was recognised by staff members as being very challenging for patients and families as they realise their “new reality” on returning to their home environment. Experiences of support and follow up after hospital discharge varied with time and location as different hospitals offer very different services, with more support available in recent years compared with 5+ years ago. Patients admitted during the Covid-19 pandemic frequently described little to no follow-up support for some time after discharge. However, despite the differences in support experienced, the feelings of shock, unpreparedness, abandonment and struggling to cope were almost identical.
There was very much a feeling of abandonment and that’s not a criticism of the hospital or that team at all. That’s more about the NHS and the system we have.
Subtheme 3.3: Lasting effects - “It’s there all the time.”
The focus group data supported the theory that critical illness should be considered a lifelong diagnosis. 2 Most participants had not been able to return to the life they had prior to their illness, many describing the major financial and social impact of being unable to work. There was also a psychological impact of awareness of one’s own mortality, the slow progress to recovery and frustration at others not understanding their experiences. Comparisons were made to survival from cancer or heart attacks where it was felt there is more public awareness.
It’s a lifelong diagnosis, it’s a change in the whole rest of your life, things are never going to be the same again.
Priorities/activities for recovery and rehabilitation
Focus group two explored participants’ priorities for rehabilitation and recovery and asked them to share wisdom and advice they would give to others. There was a high level of agreement between all of the participants, with almost identical advice from the patient and staff groups. This advice included setting realistic goals, having things to look forward to, prioritising sleep and mental health, living in the moment, pacing, being kind to yourself, and expecting good days and bad days. After all of the distressing experiences and emotions reported in the first focus groups, this one was unexpectedly very positive. All of the patients were more than a year from their experience of critical illness and perhaps this time had allowed reflection on the things that helped them to survive and recover and their advice for others was kind, practical and often humorous.
Goal-setting - “Don’t expect to be able to do what you used to do straight away.”
Most patients mentioned that they set themselves goals. Many differentiated between their goals for recovery and rehabilitation, with the recovery goals being more long-term. For example, one patient wanted to be able to walk his daughter down the aisle at her wedding. Goals for rehabilitation were reported as being more quickly attainable, such as taking a couple of steps further each day. One patient described this as “
All of the patients emphasised that goals should be realistic and achievable and many mentioned that it was helpful to have a visual record of their targets and achievements, such as a diary or a whiteboard or poster by their bed.
Almost every patient recalled how helpful staff had been during their rehabilitation journey, particularly the physiotherapy teams: The physiotherapists were critical for recovery and you know they were amazing and you know I connected with them. I could turn what they were saying into action.
The staff focus group members also recognised the importance of setting a range of targets, and that this should be guided by the patient. However, they pointed out that “it’s not one size fits all” and that every patient requires a slightly different approach.
Ask the patients how to support and motivate them because rehabilitation isn’t a pill and we can’t prescribe it for them. It’s something they have to engage in. ICU physiotherapist (20 years experience)
Prioritisation of mental health - “Be kind to yourself.”
Almost all of the patients and staff mentioned the toll that critical illness and rehabilitation takes on mental health. They felt that a lot of patients fell into the trap of pushing themselves too hard during their recovery and feeling very low and disappointed if they were not making progress as quickly as they hoped. They offered a lot of advice around being kind to yourself, acknowledging your feelings and seeking support (“
Patients and staff all commented on the fact that the journey to recovery is rarely straightforward and felt that people should be prepared for this at the beginning and reassured that it is normal to have ups and downs.
One bad day doesn’t mean you’re having a relapse. We all have bad days. It doesn’t mean that you failed
The final activity in this focus group was a fun challenge where participants were asked to pick a “luxury item” and a piece of music to help with recovery and rehabilitation. Luxury items chosen included devices for entertainment and communication such as tablets and mobile phones and comfort items such as cuddly toys and pets (see Table 3 for further detail). This exercise resulted in amusement and laughter within the groups and stimulated a lot of discussion. Songs suggested were all high energy motivational tracks.
“Luxury items” to help with recovery and rehabilitation.

Brokered dialogue
The brokered dialogue summarised the key points from each focus group to the next group and encouraged questions and comments. This stimulated interesting discussion within and between the focus groups. It was interesting to note that the questions asked by the patient groups addressed important and serious topics including decision making on treatment cessation or escalation, how staff would feel if it was their family member unwell, and is survival considered a positive outcome at any cost? Patients also wanted to remind staff to remember they are people not just patients.
How can I understand why I survived? - “Why me? Why not me?”
Many patients reported that their families had been told they may not survive, and some were aware of other patients in ICU with them who had died. A number of our patients mentioned survivor’s guilt, feeling guilty that they had survived when others had not. Some also felt guilty because they felt they were not grateful enough for their survival and still struggled with physical and psychological symptoms including low mood. They felt a need to understand why decisions had been made to continue treating them when treatment was stopped for other patients.
To the doctors deciding my fate, thank you for not pulling the plug, but why didn’t you?
This question resulted in a lot of discussion amongst the staff groups about how decisions are made, and whether intensive care is more art than science. The response to the patient groups explained that treatment decisions in ICU are complex and are approached on an individual case basis using all available information about that patient and their condition and involving a wide multidisciplinary team.
Toxic positivity - “they’re all celebrating the success and actually your motivation just goes right down the other way.”
There were several conversations around this theme. Patients felt that staff were very focussed on patient survival and asked the staff groups whether they viewed survival as wholly positive despite the cost? They wanted to know that the teams looking after them take into account what is in the best interests of the patient and what would be acceptable to them in terms of quality of life going forward.
Patients and families made it clear that they wanted information at every stage of their journey that was accurate, relevant and pragmatic, but also noted that pacing of information was important as they couldn’t take in much information at a time without becoming overwhelmed or forgetting key points.
Information-wise, when I got home I had this burning desire to find out what happened to me. What is ARDS, what is ECMO, what is pulmonary fibrosis?
The staff groups took these questions and comments very seriously and the issue of “toxic positivity” was discussed at length with many staff members reporting back that they had reflected and changed their own practice as a result of these conversations. There was a recognition that every patient is different and some respond better to hard facts and keeping expectations realistic whereas others need more help with positive encouragement to motivate themselves.
Compassion - “The person in the bed is a human first and a patient second.”
Although most of the patients felt that the staff, particularly nursing staff, had made them feel safe and valued and maintained their dignity as much as possible, some reported negative experiences including feeling like a burden, embarrassment during intimate care and overhearing distressing conversations around the bed space. They asked for the staff groups to be reminded that their patients are human beings. The staff groups found this difficult to hear, as they all felt that they prioritised patient dignity and always behaved compassionately. However, after some discussion, there was a recognition that too much empathy can be upsetting and could interfere with professionals’ ability to do their job well.
We need to dissociate a little bit when patients are very unwell as a protective mechanism otherwise you’d probably go home every day and cry. Critical care dietician (>15 years experience).
The questions and comments from the staff groups to the patient groups were all around the theme of how to improve the patient experience and were well received by the patient groups, with clear and specific answers. Please see Table 4 for examples.
Summary of key questions and answers during brokered dialogue between patient and staff focus groups.
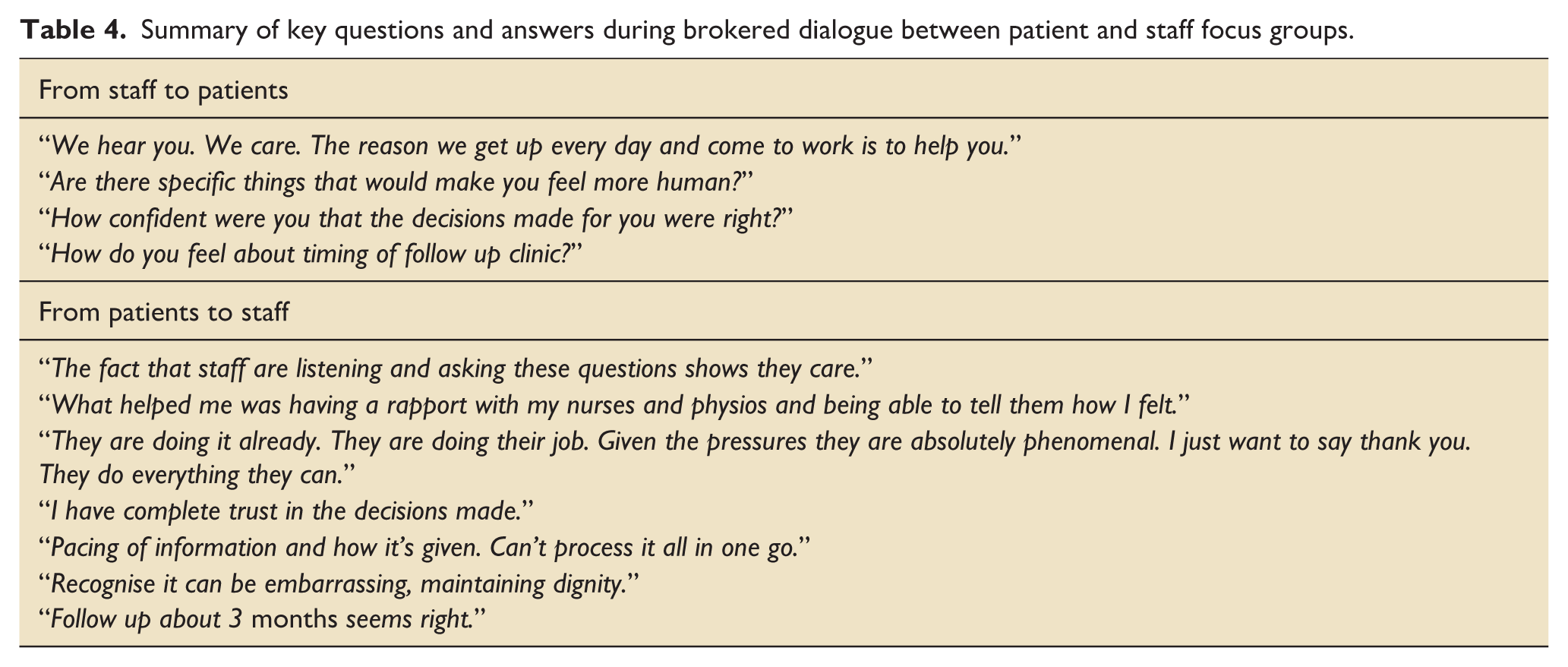
Reflexivity
Throughout the focus groups and during data analysis, the research team tried to maintain awareness of their own backgrounds, experiences and beliefs and how this could influence the data collection and interpretation. One team member had lived experience of a family member going through an ICU admission, one is a doctor working in critical care and all had some background and understanding of psychology. The nature of the challenges communicated by participants were largely unsurprising to the intensive care consultant. However, some elements of the experiences shared were unexpected and troubling. For example, participants’ vivid descriptions and clear memories of breathlessness and delirium were distressing and thought provoking. Communication of experiences and descriptions from the patients and families to the participants in the staff groups elicited different responses depending on the staff roles. For example, those involved in follow-up clinics were familiar with many of the issues faced, as they are regularly reported by their patients. Critical care outreach staff and physiotherapists were not surprised by the problems reported on ward stepdown, whereas this was less well recognised by staff mainly based on the intensive care unit. Communication of the common and more unexpected challenges faced by those experiencing critical illness to those professionals caring for them and involved in their recovery, has the potential for changes to practice, ensuring the patient remains centred in care pathways. In fact, many of the participants in the staff focus groups reported that they had immediately changed their practice in response to the issues discussed in the groups. For example: trying to better prepare patients for stepdown to the ward; giving and repeating information at each step of the pathway; agreeing common short and longer-term goals for rehabilitation and displaying them at the patient bedside.
One particular example, shared by our participants, where practice can be easily amended relates to the stepdown of patients from critical care to other areas of the hospital. Healthcare staff generally view stepdown from critical care to a ward or discharge home as a success criterion, but patients described feelings of abandonment, boredom, fear, inability to sleep, struggling to understand how unwell they had been and adjusting to their new reality. It is important that as care providers, we recognise that our patients may be going through these challenges and allow them the time and empathy they need and not dismiss their feelings with “toxic positivity,” as raised in the brokered dialogue.
Discussion
Our findings showed that there are many common experiences during critical illness and recovery, with patients, staff and families all highlighting the same key timepoints, including ward stepdown and discharge home as particularly challenging. Themes identified from focus groups included feelings of helplessness, anxiety and frustration. Priorities and advice for recovery and rehabilitation again showed a lot of overlap between the patient and staff groups and emphasised the importance of setting short and longer-terms goals that are realistic and achievable, promoting self-care and recognition that there will be good and bad days. The patient group did not shy away from difficult topics in the brokered dialogue, asking staff why they had survived, how decisions were made about them and challenging staff to remember their compassion and avoid unhelpful and unwelcome positivity.
People are admitted to critical care for a myriad of clinical indications, with each individual experiencing the process as a unique set of circumstances. Despite these individual experiences, we found that there was a remarkable degree of overlap in specific aspects of participants timelines and the challenges they faced during recovery from critical illness. This indicates that there are common elements to the experience of critical illness, which may warrant deeper consideration from healthcare professionals involved in the care of people admitted to critical care. An awareness of these issues and how our patients may be feeling at key points during their recovery should help us to be more considerate in our interactions and planning our care and communication to suit each individual’s needs and requirements.
Timelines
Other studies using interviews with critical care survivors and their families have described similar milestones on the patient journey and identified specific support requirements for each phase of recovery to minimise negative outcomes. 17 The Faculty of Intensive Care Medicine (FICM) Life after Critical Illness guide (2021) starts with an overview of the current scope of critical illness recovery practices starting in the ICU and again, the key points are the same as we found from our focus groups, with emphasis on the importance of information giving and goal-setting throughout. 9
Themes
The key themes of helplessness, fear and frustration that we identified have not been described explicitly in previous studies but similar emotions have been recognised. A Swedish study 18 interviewed 12 ICU survivors and found that recovery from critical illness was “a long struggle” with survivors describing a desire not to be dependent on others, increased emotional sensitivity and fear of becoming unwell again. Similar to our findings, participants in this study found that unpleasant and unreal memories still affected them negatively after their physical recovery. As in our study, they also expressed gratitude to staff. 18
Two studies in the United States have also interviewed patients and caregivers and found that they reported the experience of recovery from critical illness to be “scary, traumatic and lonely” 19 with “ongoing anxiety and worry.” 20 Like our participants, patients and families in these studies were also clear in their desire for information, particularly “more realistic and detailed prognostication regarding recovery.” 19
Interviews with family members of ICU survivors found that they felt they had “insufficient time to transition from a family visitor to the active caregiver role” when their loved one was discharged from hospital and often felt “overwhelmed and underprepared.” 20 It is well recognised that an ICU admission can severely impact family members’ mental health, with one study following up survivors and their family members finding that symptoms of anxiety, depression and post-traumatic stress disorder (PTSD) in family members were worse than those reported by the ICU survivors. 21
Strengths and limitations
Offering face to face and online opportunities for focus group participation widened access to include participants from a wide geographical area and from a variety of backgrounds including those who struggle to leave the house. Repeating the first focus group six times allowed a large number of participants to tell their stories ensuring the themes developed were more likely to be representative of these stakeholder groups.
However, we are aware that patients, families and staff that choose to volunteer to participate in focus groups and tell their stories are those that are motivated to make a difference. The patients who participated had recovered enough that they were able to join a group and concentrate on speaking and listening for up to 2 h. They were also psychologically ready to talk about their experiences. Patients not in a position to do this would have self-excluded from these focus groups and we have not heard their perspectives. Opinions and advice on recovery from critical illness have been received from those motivated to join these groups to help others, and these individuals may also have had more self-motivation during their own recovery. Caution should therefore be used in applying their advice to other patients who may not be appreciative or responsive to this approach, for example detailed information giving and shared goal-setting. Staff members joined the focus groups in their own free time outside work so again, their experiences and opinions likely represent the more altruistic and motivated perspective, or those with fewer commitments who were in a position to provide this time.
It is important to note that although there were many similarities between patient perspectives, there were also some significant differences. In the similar words of one patient and two staff members, “
In summary, these focus groups have been extremely informative and provide a rich data set from which we can learn a lot about our patients and ourselves. The descriptions of the lived experience of critical care admission described here provide important insights into how patients experience the recovery journey, which will enable improvements in the service we deliver to attain and maintain the highest quality standards for our patients. We should all aim to adhere to the FICM guidance for patient care during and after critical illness but how else can we use our findings to improve the care we provide? The next phase of this research study has continued with some of the focus groups participants forming a patient steering group. The specific aim of this next phase was to co-develop an intervention to address some of the issues identified by patients. Although the presence of more staff members with specific training to provide appropriate information to prepare for moves to the ward or home, help with reassurance, relaxation and avoidance of boredom would be ideal, staff numbers and NHS finances do not currently allow for this. Therefore, a virtual reality intervention has been developed with specific and tailored content providing information, distraction and relaxation according to the priorities identified in the focus groups and supported by the patient steering group. This intervention is currently being assessed in a feasibility trial, which will be reported soon (ISRTCN 88854487).
Footnotes
Acknowledgements
We would like to thank all of our focus group participants for giving their time and sharing their experiences and opinions with us.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Funding for this study was provided by Health and Care Research Wales (Research for Patient and Public Benefit) RfPPB-21-1870(P).
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
