Abstract
Background:
Randomized trials have demonstrated that early anticoagulation after acute atrial fibrillation-associated ischemic stroke is safe and non-inferior to delayed initiation. Whether anticoagulation should be delayed in people with larger infarcts is uncertain.
Aims:
To investigate whether ischemic stroke infarct volume, measured precisely by segmentation, modifies the treatment effect of early anticoagulation with a direct oral anticoagulant (DOAC).
Methods:
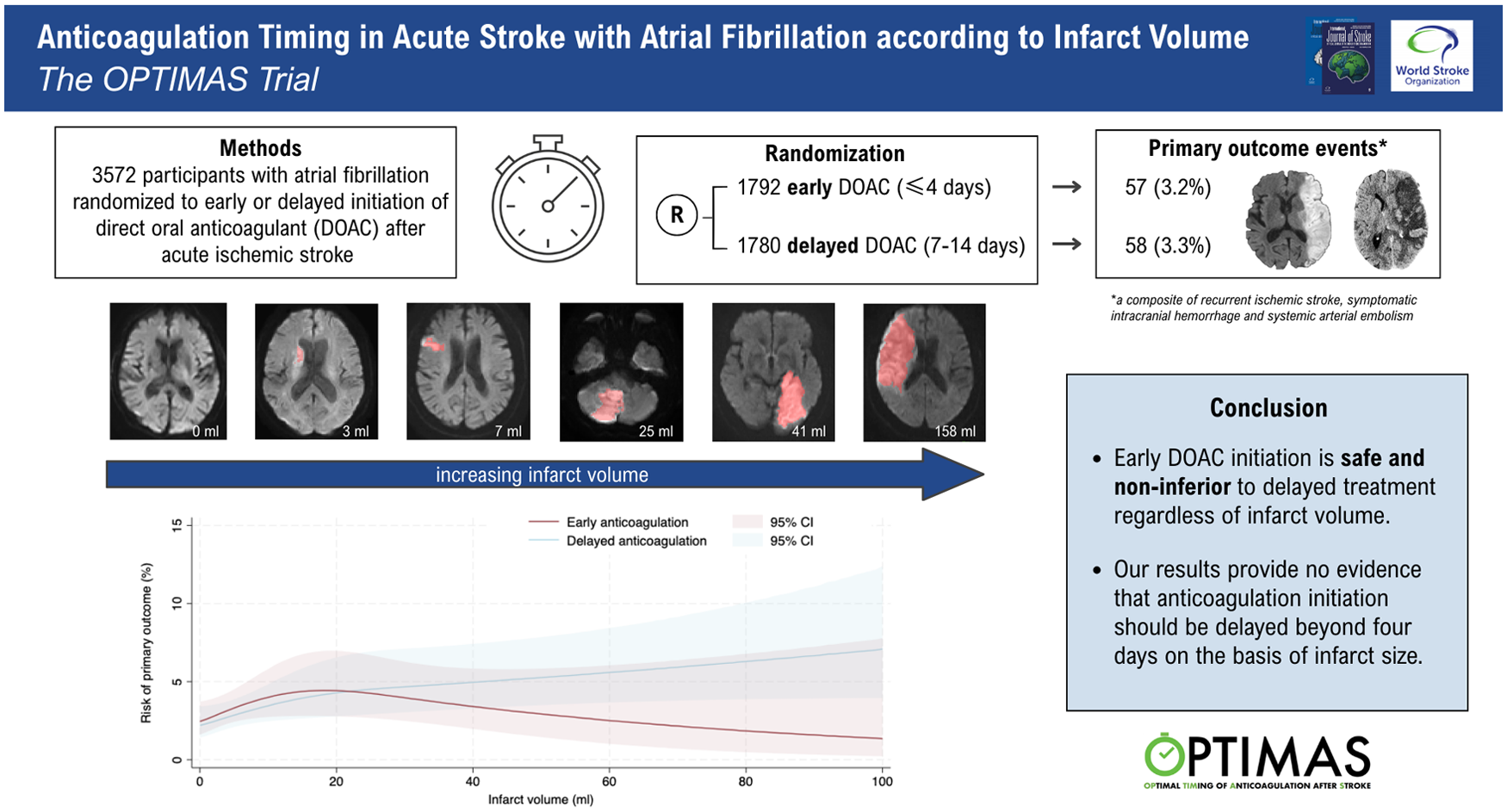
We did a prespecified secondary analysis of OPTIMAS (NCT: 03759938), a randomized, parallel-group, open-label trial with blinded outcome assessment which randomized people with acute ischemic stroke and atrial fibrillation to early initiation of any licensed DOAC, within 4 days of onset, or delayed initiation 7–14 days from onset. The primary outcome was a composite of recurrent ischemic stroke, symptomatic intracranial hemorrhage (ICH), and systemic arterial embolism within 90 days. A central neuroimaging laboratory determined infarct volume using diffusion-weighted magnetic resonance imaging (MRI) using a validated deep learning segmentation model; on computed tomography (CT), infarcts were segmented manually. We modeled infarct volume as a continuous variable using restricted cubic splines and tested for an interaction with treatment allocation in mixed effects logistic regression.
Results:
We included 3572 participants (mean age = 78 ± 10 years, 45% female), 98.6% of the main trial population. The effect of early versus delayed anticoagulation did not vary with infarct volume (pinteraction = 0.18). Rates of the primary outcome were 17/568 (3.0%) and 12/599 (2.0%) for early versus delayed initiation with infarcts of 0–5 mL; 6/220 (2.7%) and 11/229 (4.8%) with infarcts of 5–10 mL; 13/258 (4.6%) and 10/283 (3.5%) with infarcts of 10–25 mL; 6/145 (4.1%) and 8/145 (5.5%) with infarcts of 25–50 mL; 1/93 (1.1%) and 7/94 (7.4%) with infarcts of >50 mL; and 14/481 (2.9%) and 10/430 (2.2%) in participants with no infarct visible on clinically acquired brain imaging. Corresponding odds ratios and 95% confidence intervals were 1.52 (0.71–3.20), 0.55 (0.20–1.51), 1.29 (0.55–3.00), 0.74 (0.25–2.21), 0.13 (0.02–1.11), and 1.25 (0.55–2.86), respectively. There were no increased rates of symptomatic ICH with respect to anticoagulation timing for those with large infarcts (>25 mL); there were 3/238 (1.3%) events in the early group and 5/239 (2.1%) in the delayed group.
Conclusion:
The treatment effect of early anticoagulation with a DOAC in acute ischemic stroke associated with atrial fibrillation was not modified by infarct volume. Adverse outcomes were not increased with early anticoagulation in people with larger infarcts. Our results provide no evidence that anticoagulation initiation should be delayed beyond 4 days on the basis of infarct size.
Keywords
Get full access to this article
View all access options for this article.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
