Abstract
Background:
Lithium, a naturally occurring element in drinking water, has demonstrated beneficial effects for stroke in prior research, yet its relationship with stroke risk in the general population remains uncertain.
Aims:
To evaluate the association between environmental lithium exposure and stroke risk.
Methods:
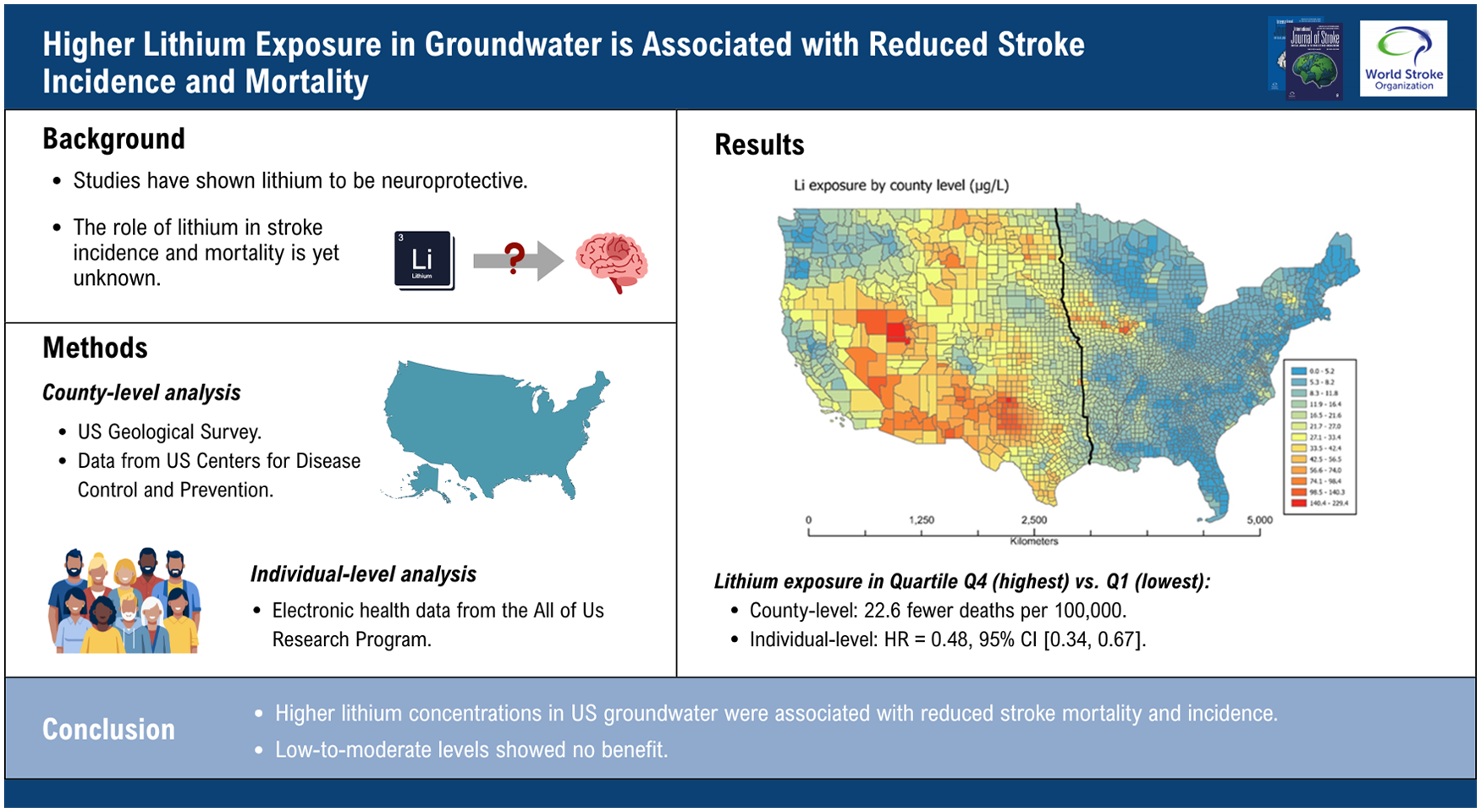
We assessed environmental lithium exposure across the United States using monitoring data of 4700 wells for drinking groundwater from the US Geological Survey. Ecological and individual-level analyses were conducted. Ecological associations between county-level lithium concentration and stroke mortality (2015–2019) were evaluated in 3108 counties using multivariable linear regression adjusted for county-level socioeconomic factors. Individual-level associations were examined in 303,153 adults (⩾35 years old) from the All of Us Research Program with electronic health records followed up through 1 October 2023 using stratified Cox models adjusted for individual-level sociodemographic, behavioral, and clinical factors. Lithium was analyzed per interquartile range (IQR) increase and by quartiles.
Results:
In ecological analysis, each IQR increase in lithium exposure corresponded to 8.2 fewer stroke deaths per 100,000 population (95% confidence interval (CI) = −9.8, −6.5). Compared with the lowest quartile (⩽ 6.6 µg/L), the highest quartile (> 23.3 µg/L) showed 22.6 fewer deaths per 100,000 (95% CI = −27.4, −17.8); middle quartiles were not associated. In All of Us, each IQR increase was associated with a 23% lower incident stroke risk (hazard ratio (HR) = 0.77, 95% CI = 0.66, 0.90). The highest exposure quartile (> 17.7 µg/L) had a 52% lower risk (HR = 0.48, 95% CI = 0.34, 0.67) versus the lowest; the second (HR = 1.23, 95% CI = 0.73, 2.09) and third (HR = 0.92, 95% CI = 0.50, 1.69) quartiles showed non-significant associations. Results were robust to alternate exposure windows and residential stability restrictions.
Conclusion:
Higher naturally occurring lithium concentrations in US groundwater are associated with reduced stroke mortality and incidence, whereas low-to-moderate levels confer no benefit.
Get full access to this article
View all access options for this article.
