Abstract
Background:
Intravenous thrombolysis with tenecteplase within 4.5 h after ischemic stroke is noninferior to alteplase. However, it is uncertain whether this is also true in patients last known to be well more than 4.5 h before treatment initiation (last known to be well more than 4.5 h before treatment initiation (LKW > 4.5 h)). We aimed to compare tenecteplase and alteplase in this population using data from two large multicenter registries.
Methods:
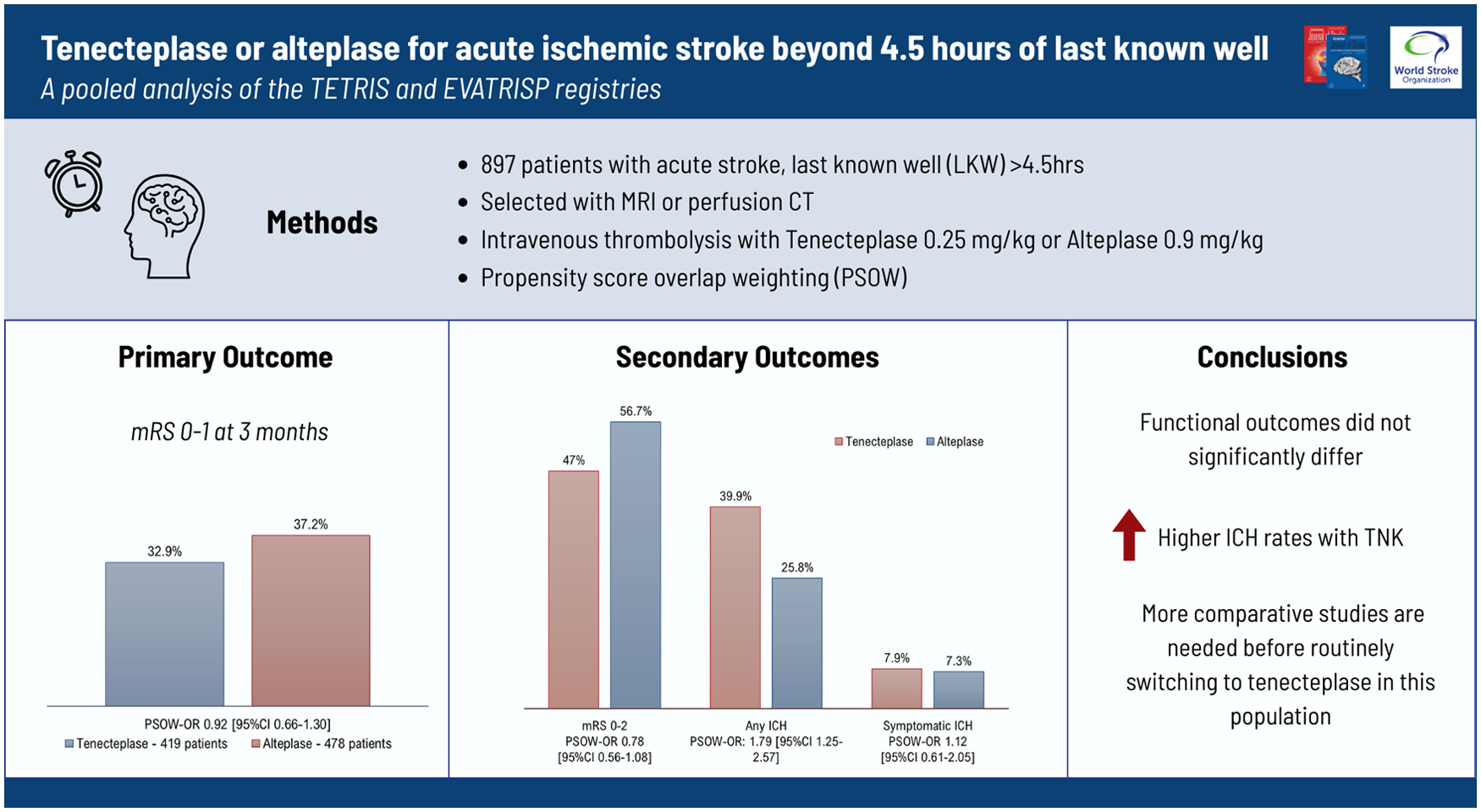
Pooled retrospective analysis of acute stroke patients LKW > 4.5 h treated with tenecteplase 0.25 mg/kg (Tenecteplase Treatment in Ischemic Stroke Registry (TETRIS) registry) or alteplase 0.9 mg/kg (EVATRISP registry plus 4 French centers participating in TETRIS) based on the results of magnetic resonance imaging (MRI) or perfusion computed tomography (CT). Excellent functional outcome at 3 months (modified Rankin Scale (mRS) 0–1) was the primary outcome. Secondary outcomes were mRS 0–2, shift analysis of the mRS, any intracranial hemorrhage (ICH), symptomatic ICH, and death. Propensity-score overlap weighting (PSOW) was used to account for imbalance in baseline characteristics.
Results:
A total of 897 patients (tenecteplase: n = 419; alteplase: n = 478) were included between 2015 and 2024 (mean age: 74 (IQR 64–84); median National Institutes of Health Stroke Scale 11 (6–17) unknown stroke onset in 777 (86.6%) patients). At 3 months, mRS 0–1 was achieved in 138 (32.9%) and 178 (37.2%) patients treated with tenecteplase and alteplase, respectively (crude OR 0.83 (95% confidence interval (CI) 0.63–1.09); PSOW-OR 0.92 (95% CI 0.66–1.30)). Compared with alteplase, tenecteplase was not significantly associated with mRS 0–2 (PSOW-OR 0.78 (95% CI 0.56–1.08)) or better functional outcome over the whole range of the mRS (PSOW-common OR 0.83 (95% CI 0.62–1.11)). Tenecteplase was associated with significantly higher odds of any ICH (PSOW-OR: 1.79 (95% CI 1.25–2.57)), but not symptomatic intracranial hemorrhage (PSOW-OR 1.12 (95% CI 0.61–2.05)).
Conclusions:
The functional outcomes of patients LKW > 4.5 h treated with tenecteplase or alteplase did not significantly differ in this pooled analysis of two observational registries. However, the direction of the associations did not favor tenecteplase over alteplase, and therefore, more comparative studies—ideally randomized—are needed before routinely switching to tenecteplase in this population.
Keywords
Get full access to this article
View all access options for this article.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
