Abstract
Conducting large multi-site research within universities highlights inconsistencies between universities in approaches, requirements and responses of research ethics committees. Within the context of a social science research study, we attempted to obtain ethical approval from 101 universities across England to recruit students for a short online survey. We received varied responses from research ethics committees of different universities with the steps to obtaining ethics approval ranging from those that only required proof of approval from our home institution, to universities that facilitated fast-track applications to those that required a full ethics review. Some universities also completely refused. After contacting all 101 universities in England, 60 universities gave clearance to our study. In this article, we present the different approaches universities adopted in response to our application to sample from students in their institution. We consider a number of conceptual and ethical issues pertinent to considering ethics approval for researchers from other universities in England and critically discuss three possible models of ethics governance that would cover all universities in England.
Introduction
Over the past decade, much has been written about the inconveniences and inconsistencies that research ethics committees and ethics governance systems impose on researchers in the medical and social sciences (Abbott and Grady, 2011; Edwards et al., 2004). The failings of the medical research ethics governance systems have been documented exhaustively, and there is overwhelming empirical evidence that medical research ethics committees vary in the kinds of judgement that they make and the processes that they use (Angell et al., 2006; Caulfield et al., 2011; Edwards et al., 2007; Hirshon et al., 2002; Larson et al., 2004; Mansbach et al., 2007; Racine et al., 2010). In this article we provide one small example of this, but we think it is a striking empirical example that shows a similar level of variation across ethics committees in universities in England. We go on to suggest some ways in which the university system might be relevantly different from the more straightforwardly medical context, and some ways in which the variation might be managed.
In the United Kingdom, and partly in response to these complaints and the associated evidence, the National Research Ethics Service (NRES), which governs research conducted on patients in the National Health Service (NHS), has instituted a range of important evolutions in an effort to make the system transparent, robust and consistent in the appropriate way (NREAP, 2014). Research ethics in the NHS of England was formally established in 1991 and followed several transformations in subsequent years. In 2000, the Central Office for Research Ethics was formed, and in 2007 a National Research Ethics Service (NRES) was established to maintain the UK-wide framework for ethical review of research within the NHS. This framework allows for greater harmony between NHS committees and for multi-site projects to go through only one ethics committee. The decisions then apply across all sectors and committees.
In stark contrast, research ethics committees within universities have no overarching governing body or systematic structure that enables coordination and organization. The Tinker and Coomber 2004 report highlighted this lack of procedural agreements for university research ethics and noted the different types of research ethics structures within universities (Tinker and Coomber, 2004). These procedural differences between university research ethics systems can be attributed to the rapid introduction of university research ethics committees (URECs) from the year 2000 and to the fact that universities are their own entities responding to more localized pressures. The rise in number and shape of research governance systems was linked to the fact that funders of research began to threaten funding unless ethical approval was obtained. Research ethics approval for social sciences was also required by funders specifically through the Economic and Social Research Council’s (ESRC) Research Ethics Framework (REF) (now called Framework for Research Ethics, FRE) (ESRC, 2015). Although some guidance is given on how to handle ethical issues, notably by the ESRC, little is provided on the procedural process and on how to handle inter-university research and external researchers.
In what follows we present empirical results of an encounter with higher education (HE) research ethics governance in England through a study which involved an online survey on health behaviours of students across England (101 universities). In the discussion sections, we first consider a range of ethical issues about the governance of research in universities that these data highlight, with particular focus on how inter-university research might be handled. We then go on to present and critically evaluate a number of alternative solutions to this set of issues. Importantly, these issues are more complex and distinct than a first glance at the criticisms and empirical evidence of variation might suggest. In particular, they resist the straightforward comparison from research in the medical setting to the higher education context. While we do encourage the development of an overarching system or agreement about the ethical principles and processes of governance, we do not advocate strongly for one model over another but we do suggest that the range of considerations that we articulate captures the key ethical points involved in decisions about such a system.
Protocol
The empirical data that we present here was not sought directly as part of a study focused on illustrating variation. The data accidentally emerged as a by-product of a separate research process, so it is unclear, at least, that publishing these findings in an anonymized way requires separate ethics approval (Macdonald, 2010). 1 It arose from the experiences of seeking approval for a distinct project aimed at undergraduate students in England. Our initial study involved recruiting first year undergraduate students for a short online survey which investigated health behaviours in students in England. It contained a few personal questions but no sensitive topics (lifestyle habits in eating and exercise, but no sexual or illegal drugs questions). We applied for ethics approval at our home university with a research protocol which involved recruiting students from all the universities in England. We received ethics approval without needing to modify most of the protocol.
We proceeded to contact individually all university ethics committees (n = 100) featured in the England League Table, to ensure that they were content for us to proceed in recruiting their students. This was not required by our home university, but we had written in our initial ethics applications that we would do so. We felt that it was an appropriate course of action so as to (i) ensure that universities were aware of our research, (ii) obtain recommendations of gatekeepers, and (iii) get institutional endorsement, which would in turn help us have the support of the student unions for dissemination of the survey. We found the contact information of ethics committees on university websites and emailed a standardized message to the secretary of ethics committees. When there was no contact information for ethics committees available, we emailed the registrar or the research office to obtain contact details. In our email to the research ethics committees, we explained that we had obtained full ethics approval from our home university and had understood this to cover recruitment in their university. We further attached our full home ethics application and approval letter and asked whether they were happy for us to proceed with our study. We also asked if they had any recommendations on gatekeepers for recruitment. If we received no answer after three weeks we sent a reminder.
Empirical data
We experienced a high variability in responses, with very different response times. In total, we were able to reach 89 universities (excluding the home university). Eleven ethics committee were not emailed because we could not obtain contact details. When emailing ethics committees, in some instances we were referred to special sub-committees of specific disciplines, while in others we were referred to a central university ethics committee. From these committees, we received a range of responses: no response, no need for further approval, need for fast-track approval, need for fast-track approval with extra steps, and need for a full review. We also received replies simply stating that the university did not approve this study. Figure 1 presents an overview of the 100 ethics processes, while Table 1 provides the frequency of different types of responses from ethics committees. As portrayed, there is clearly no universal process for dealing with ethics applications which come from external researchers. There was also no consistency across the universities in changes requested or in reasons behind refusals. From the 89 universities we were able to contact, responses from the committees can be classified into three categories: approval, no response or declined. An important number of ethics committees were not reached because of lack of information on how to get in touch.
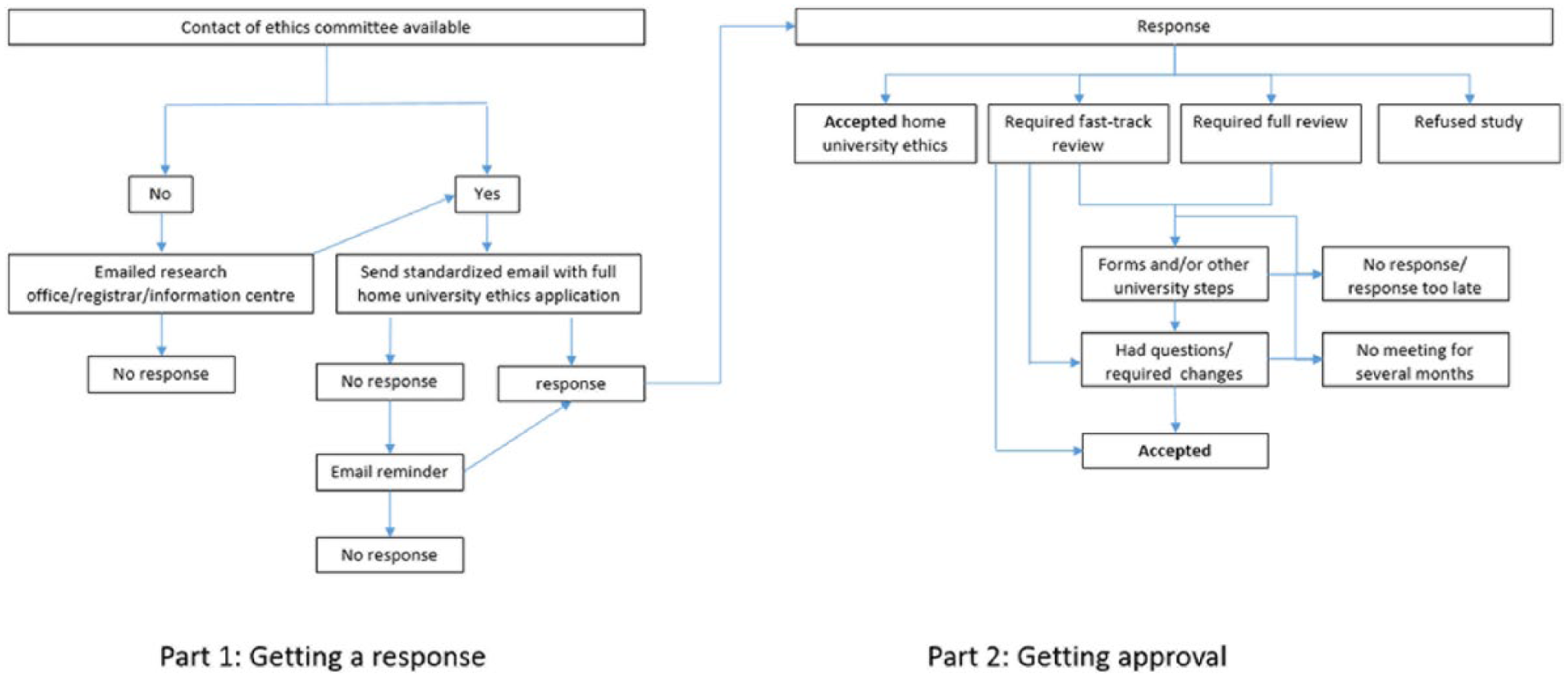
Diagram of the pathways to getting responses from ethics committees in 100 universities in England.
Frequency of type of response from 100 university ethics committees in England.
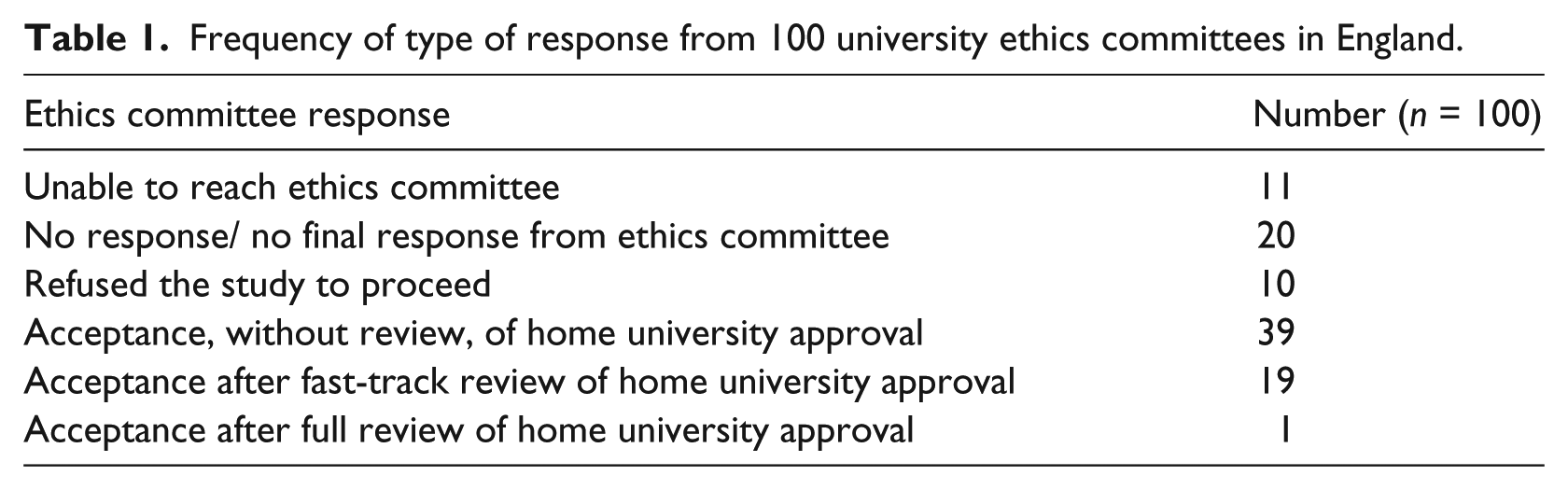

Category 1: Approval (n = 59)
No further approval needed: Committees (n = 39) stated there was no need to seek other university permissions when one already had university ethics approval: ‘Normally, there is no need to obtain additional ethics approval from any sites used for recruitment and data collection once you have been granted ethics approval by an appropriate institutional Research Ethics Committee, in your case the IDREC of the University of Oxford.’
University approval letter issued: Committees (n = 15) provided ethics approval letters with their home institution headed paper, with two universities demanding the recruitment material to clearly state that their university had also approved it: ‘We do request that all external studies make it clear that [name] UREC is aware of the study and the following statement should be inserted in any recruitment letter/emails to [name] students.’
Reference to clear guidelines for external research: Committees (n = 5) stated that there were clear guidelines on the website for external researchers or they emailed us the clear guidelines. These included filling out forms, proving collaboration, proving acceptance of departments for recruitment etc.
Expression of concerns/questions on proposal: Committees (n = 10) emailed concerns/questions of a different nature and targeting different aspects of the protocol, several of which were never mentioned by our home institution or by any other ethics committees.
Request for changes: Committees (n = 6) had special requests/changes to be made to the advertising material or consent form.
Category 2: No response (n = 20)
No final response given: Committees (n = 6) initially responded, sent applications to fast-track review, but did not confirm approval within 2 months (i.e. before recruitment start date).
No response: Committees (n = 14) never replied, despite a reminder or an initial answer.
Category 3: Declined (n = 10)
Similar studies already being accepted: ‘I am afraid that we must decline your request for access to our students. We do receive many requests for the involvement of our students in research activity and we are therefore obliged to prioritize such requests and consider the impact of multiple requests for participation on our student body.’
Feared impact on university surveys: ‘Your application was found to be ethically sound but, regrettably, was not given management/governance approval because of the danger of reduced engagement by our students with [name] surveys due to questionnaire fatigue.’
Refused to have external researchers recruit their students: ‘Researchers who do not work at [name] cannot apply for nor obtain ethical approval at [name], which is needed in order to conduct research with our students.’
Refused without clarification: ‘The Chair of the University Research Ethics Committee, [name], has refused to provide ethical approval for your study.’
Needed full review and no committees were to be convened before October.
In summary, we received a majority of positive responses from universities. Almost 40 universities reported that ethics approval from one university was overarching and allowed recruitment from other universities. The other universities which approved the study requested a few changes but still provided approval. On the face of it, these universities might be taken to have had confidence in the ethics review processes of another university and were prepared to pass on the final decision about participation to the individual student. This kind of view might lead us to think that these universities and their ethics committees adopt a fairly liberal view of their role: that much of the research conducted in universities, including surveys like this one, does not actually run the risk of inflicting sufficient harm to warrant sanctions or regulations (Dingwall, 2008; Hammersley, 2009; Oakes, 2002; Reed, 2007; Sheehan and Dunn, under review 2 ) and that the decision about participation rests with the students. One concrete policy-related example of this is that several universities have opt-out or opt-in mailing lists or dedicated website pages advertising student recruitment.
The refusals, on the other hand, can be taken to reflect a more protective or paternalistic stance on research ethics and the ethics review process. Most refusals can be characterized by the idea that the universities (or in their place, the ethics committee) should protect their students and thus have an important role in deciding what constitutes and causes harm as well as about how much is too much. During our interactions with ethics committees, the ethics committee (or their representative) at several universities seemed to suggest that advertising too many surveys to students caused harm to students in the form of survey fatigue.
Mixed in with these concerns for students was also a privileging of internal over external research. This suggests a kind of protectionism: ensuring that ‘our’ researchers have first or privileged access to ‘our’ students. In a similar vein, several universities did not allow external researchers to apply for ethics approval within that university, thereby only allowing internal researchers to recruit students for their studies. This may be a method for controlling the quality of research conducted on students or to ensure that there is low recruitment fatigue from students and thus enough subjects for internal research.
In total, 60 universities (including our home university) provided clearance for this study, though there was variation in the amount and kind of access (in terms of methods of recruitment) that was granted. The variety of responses from ethics committees, as indicated in Table 1, shows a clear inconsistency in the processes by which university ethics committees handle external research as well as in the content of the decisions made about granting ethics. From the 60 universities, we were only able to recruit from 26, as several universities granted ethics but did not grant recruitment rights or they allowed recruitment only via a certain research website.
Discussion
Our experience, described above, brings with it a number of interesting and important issues about research ethics governance across the higher education system in the UK (and indeed across higher education systems more broadly). In particular, it raises questions about the various kinds of ‘inclinations’ that a university review system might have, particularly when it comes to its assessment of external research or inter- or multi-university research. This is in addition to the perhaps more obvious question about whether or not there should be an overarching system or agreement between universities that harmonizes the processes of review across the system and gives it an appropriate degree of procedural consistency.
In what follows we first consider the general form that these inclinations might take in the university context. This consideration takes the form of an initial set of research ethics frameworks: generalized stances that we might take to research ethics governance in the university context. We then briefly consider the nature of the guidance that exists that makes specific reference to the governance issues surrounding external and inter-university research. In the third part of this discussion section we consider a number of conceptual and ethical issues that are pertinent to this question and about which it is important to be clear. In the final part we bring the discussion together to outline three possible governance university ethics models. We investigate what these might look like and what issues they might face.
Initial research ethics framework
There are several stances that might be taken by research ethics committees on the issue of inter-university governance in higher education. Below, we discuss a range of ethical considerations that are in play in this context. In each case, they are different theoretical stances or outlooks on research which could explain the differences between universities in their processes:
(a) Libertarian-style inclinations: This view is a strong advocate of student choice and the importance of the rights and freedoms of researchers. It is generally sceptical about governance and the extent of the role of ethics committees. Indeed, one approach to the governance process is to be outright resistant – there is no need for ethics review of the kinds of research in question, and there is certainly no general presumption that it is required (Dingwall, 2008; Dyer and Demeritt, 2008; Hamburger, 2004; Hammersley, 2009). We take this latter position to be an untenable one (McGuinness, 2008; Sheehan, 2008; Sheehan and Dunn, under review 2 ). It is also a position that is not currently endorsed in the UK and many other countries. A second more moderate approach along these lines is to concede the need for some, albeit minimal, governance, but where oversight is primarily about the facilitation of consent: it is up to the individual student to decide to participate (Edwards et al., 2004). A view of this sort is likely to be permissive about inter-university research, perhaps trusting the processes of the home institution or checking the details of the consent process before allowing the research.
(b) Paternalist-style inclinations: Through this view, the prevention of harm is crucial. It is concerned (i) that research ethics committees should exist to protect participants and (ii) that they should decide about acceptable levels of harm and risk of harm for potential participants (Garrard and Dawson, 2005; Savulescu et al., 1996). In this respect the ethics committee functions to limit the choices of individuals by preventing certain research from being offered to them. In this context, the committee makes a judgement, on issues such as how much is too much research in terms of spam, survey fatigue, over-research etc. It might also make a judgement about the value of the research itself and so whether it is worth conducting it on their students.
(c) Protectionist-style inclinations: The third kind of view that is pertinent to the university context relates to the reality of competition between universities, both for research profiles and for access to students as research subjects. It might lead to thoughts such as: ‘our students are for us to conduct research on’; ‘we want to make it harder for other universities to conduct research that will benefit them’. This competition can seem to be somewhat unsavoury in the context of an education system. That is, the idea that universities are exclusionary and protective of their own standing at the expense of research might seem to run counter to the ideals of education and the value of knowledge. However, without sustained argument it would be inappropriate to dismiss these as genuine considerations. The reality of universities in a market context is likely to impinge on educational ideals at some point.
This view might also include non-trivial ideas of loyalty and solidarity. The idea that particular higher education institutions conduct their work in particular ways, encapsulating distinctive values and thereby attracting and developing certain values and interests is one that has definite merit and is one that might legitimately bring with it protectionist inclinations. On this view, a university could and perhaps should be sceptical about inter-university research and might most often refuse external ethics applications or make the process of applying very strenuous.
Universities or ethics panels may follow or adopt one of these inclinations that influences the approval of research within their institution, in particular when it comes from external sources, especially other universities. Of course, these inclinations are unlikely to be explicitly articulated or in any way a conscious part of the process. They might vary from individual to individual within the ethics review process at a given university. Our experience, detailed above, suggests very loosely that most universities in England may lean towards libertarian-style inclinations, but it is clear that there are definite discrepancies among universities and some, in this case, found it appropriate to respond in something more like a paternalistic or protectionist manner.
Guidance
General guidance for university research ethics committees has been published by research councils and the Association of Research Ethics Committees. The frameworks discuss the roles of individual ethics committees and principles of governance but do not directly incorporate policies or strong recommendations with regard to external or multi-site university research (AREC, 2013; ESRC, 2015). Within ESRC-funded projects, research deemed collaborative may decide to have joint projects reviewed only by one research ethics committee and still satisfy the ESRC minimum requirements. This guidance, however, does not guarantee that each university would not still request individual ethics application to their university. Beyond this guidance, which only applies to a small portion of social science research, the guidance for multi-site research within universities is not apparent.
General considerations on inter-university research
There are a number of specific issues and distinctions that are worth considering as they make a difference to how we might think about various models for addressing these issues in practice:
(a) Inter-university, external research and research on another university’s students: There are a number of important distinctions to be drawn between the kinds of research that might be conducted involving multiple universities or involving researchers from multiple universities. We are clearly, for example, not considering here the processes by which collaborations between universities are subject to ethics review. We might suggest that the key kind of research that is of interest here is inter-university research: where researchers from one university embark on a large-scale project with multiple university sites and where the student population, either as a whole or partially, forms the potential research participants. Here the idea is, perhaps paradigmatically, to study the population of students (or the members of universities generally) qua students. Our study discussed above falls into this category.
Relatedly, we might distinguish this from multi-university research, which could be a broader category meant to include research which involves a range of different university sites but which is not necessarily conducted by university researchers – perhaps marketing research aimed at undergraduates. In this kind of case, we might think that the processes of review should be different from those that apply when the researchers come from ‘inside’ the university system. Similar considerations might apply for international researchers.
Third, we might distinguish research which is conducted from outside the home university setting but which targets students not in virtue of their being students but, say, in virtue of their being consumers of a certain sort. The idea here is that the student or university membership is being accessed but not in their capacity as students or members of a university. Questions about the harms associated with over-research are interesting in this case. It is hard to see who could oversee the effects of such research on the university population.
The final kind of research that is worth distinguishing here is where a university researcher has a specific interest in studying students or university members from another specific university or range of universities. For example, a researcher from a university in the south of the UK might be interesting in studying student populations in the north for historical or regional geographical reasons. A different example might be a researcher who wants to study the effects of a particular local incident on the student population. In both cases the research interest of the external researcher is specifically focused on the university or universities in question.
In each of these cases there appear to be different considerations that are relevant to the ways in which universities both individually and as a group ought to approach the processes that are in place for the ethics review of these kinds of research.
(b) The value of inter-university research: It is believed that the initial participation rate for 17–30-year-olds (i.e. proportion of 17–30-year-olds who attend university) at UK Higher Education Institutions is 47 percent (HESA, 2015). The approximate UK student population is over 2.2 million, indicating that a large proportion of individuals within the UK between the ages of 17–30 are in universities (BIS, 2015). This student population is an important part of the society on which to conduct research as their views and opinions matter, especially given the role that they will play in the development of academia and society in the future. Further, university students are in early adulthood where behaviours are fostered. It is important to better understand their needs and behaviours in order to provide adequate support for their development into healthy adults. They represent a wide diversity of backgrounds, physiological and psychological states, thus providing low-selection-bias samples for studies. Students are not the only subjects of interest within universities; similarly, those employed by universities across the UK represent a population worthwhile investigating within inter-university research as similar work environments across 100 sites provide ideal research comparative groups.
Overall, universities and their members are a vital part of our society and its future. Without research conducted on these institutions, their constituent populations and their functioning, we will be in no position to maintain and improve them.
(c) Medical context versus university context: Are there any reasons for thinking that the university context is relevantly different from the medical or NHS one? That is, are there any reasons for thinking that there should not be any sort of overarching approach to the way in which research is reviewed in the UK? It is important to note that we assume that there is reason to have ethics governance of research for non-medical research that is conducted in universities (Sheehan and Dunn, under review 2 ). This is in spite of the literature calling this into question in various ways (Dingwall, 2008; Dyer and Demeritt, 2008; Hammersley, 2009; Librett and Perrone, 2010; Reed, 2007; Richardson and McMullan, 2007). At a general level, the medical and university context are considerably different in terms of available resources, possible types of research and the overall quantity of research conducted. They also may differ in the amount of research that requires multi-site/multi-institution. It may, for example, be that research that is conducted across universities is more readily conducted in a collaborative way by involving researchers from each of the relevant institutions. The medical context has alternative means of accessing the population where there are universal databases for contacting patients as opposed to closed student enrolment lists. They thus require well-structured systems such as those in place in the USA and UK whereby one ethics committee review is sufficient.
Overall, there may be differences of scale, investment, attention and perhaps, at least, perceptions of risk involved in research in the purely medical context as compared to that of universities. These differences might give rise to greater political impetus for change and control, but it is hard to see these differences doing all of the work in maintaining sharp distinction in the approach to research ethics governance (Sheehan and Dunn, under review 2 ).
Three models of ethics governance
Having presented the details of our experiences with university RECs across the UK and initially considered a range of different stances that these RECs have taken and might take, we now present three models of ethics governance that might be used to structure an overall position on inter-university research in the UK. Each of the models suggested below are simple initial outlines. They are loosely based on strategies that have been adopted elsewhere and would require very different kinds of commitment on the part of those universities who are party to the agreement. We do not claim that these three models exhaust the possibilities, but we do think that they represent a reasonable starting point:
(a) Multiple research ethics committees: This model is based on the idea that one decision is made by an appropriately constituted committee which permits access to all ‘member’ universities. It is based on the idea of a multicentre research ethics committee (MREC) which was put in place in the NHS/COREC in 1997 (Al-Shahi, 2005). Essentially, MRECs are committees that are established for the sole purpose of reviewing inter-university or multi-university research. In this scenario, universities would sign up to the process and constitution for an over-arching decision-making agreement whereby when one committee is providing ethical clearance it is sufficient to recruit all the students mentioned in the protocol. Universities would need to work together to agree on the details of which research would count as falling within the remit of the MREC, but the distinction drawn above might be relevant. In order to facilitate recruitment, student unions, departments or the registries could be involved in advertising research recruitment.
A limitation of this model is that universities would give up some sovereignty as they could not limit specific research from being conducted (e.g. on the basis of their researchers already conducting a similar study) or limit the sites at which university research is conducted.
(b) No external researchers: A second model begins with the premise that universities should be closed to external researchers. URECs would therefore only consider research by those in their university. Should researchers from one university really need to recruit students in another university, they would have to establish a collaboration with researchers in the external university. The clear advantages of this model are that it acknowledges both the paternalist and protectionist inclinations of universities. Neither of these is necessarily problematic, and both are plausibly taken to reflect the reality of the university system in the UK. That is, it seems reasonable for universities as educational institutions to take the welfare of their members seriously and, in this respect, to seek to protect or at least maintain the ability to protect their interests. Second, it is clear that the reality of the university system is one of competition. This is competition for students and for funding that is driven at least in part by research and research productivity. In this context and the pressure on universities to be independently viable institutions, it makes good sense to simply prevent the competition from using the university’s resources for their own gain.
This model is limited in a number of respects, however, particularly if our concerns are broader than the individual university. Inter- and multi-university research is significantly hampered by the workload for individual researchers, the very real possibility of inconsistencies between ethics committees, and correspondingly fewer large-scale projects, owing to the difficulty of the task. Our experience detailed above provides clear evidence of these limitations.
(c) Individual research ethics committees with site-specific assessment/gate-keeper: The third model is very similar to the system that is currently in place in the NHS (NRES): each proposal is reviewed once by the REC at one university. This need not be the home university but it is likely that researchers would turn first to their institution for review. Universities would sign on to a system where one ethics approval is sufficient for all universities. The overall requirements of such a system on individual committees would need to be fairly robust in order to assure signatories to the agreement that the standards of review across the system were adequate. That is, the system would need to avoid the concern that ethics review in one university was more robust, more thorough and ‘more difficult’ than in another. As with the current NRES system, this would likely require a standardized set of application forms, and minimum requirements for membership and for the processes of review.
The model could be adjusted to involve some ‘site-specific’ consideration whereby each home institution could make limited local judgements about practicalities etc. but not full ethical assessment. (Notice that this could also be an adaptation of the first model.) This review would be lower-key and individual universities might be only permitted to refuse researchers due to site-specific issues such as over-research or lack of infrastructure for certain research.
The clear limitation of this model is the amount of coordinating bureaucracy that the system would require. The system would need to be managed and overseen, and in this respect it would require funding. Perhaps most of all such a system would require the agreement of a substantial majority of universities in the UK if it were to be feasible.
Conclusion
In this article, we have highlighted the variation between university ethics research committees within one country. From our experience universities seem to approach research ethics from different inclinations, and these have impacts on the options for inter-university research. Indeed, through our empirical study, we found that out of 101 universities in England, we received ethics approval from 60 universities. We obtained 10 refusals and 20 no-replies across different stages. Our study also showed procedural inconsistencies between committees. Recruitment for large-scale projects from multi-sites looks difficult and not standardized.
In this article, we have explored a number of issues that might arise in the context of university research ethics governance. We have presented and evaluated a number of alternative solutions to this set of issues. In particular, we noticed that they resist the straightforward comparison from research in the medical setting to the higher education context. While we do broadly favour the development of an overarching system or agreement about the ethical principles and processes of governance, we do not advocate strongly for one model over another, but we do suggest that the range of considerations that we articulate captures the key ethical points involved in decisions about such a system. The arguments and suggestions in this article are intended to begin a discussion rather than to conclusively close it.
Footnotes
Acknowledgements
Claudia Vadeboncoeur is grateful for support from the Clarendon Fund, the Nuffield Department of Population Health and Wolfson College. Mark Sheehan is grateful for the support of the Oxford NIHR Biomedical Research Centre, UK.
Conflict of interest
The authors declare that there is no conflict of interest.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
