Abstract
Background:
Familial hypercholesterolaemia (FH) is a genetic condition that significantly increases cardiovascular disease (CVD) risk, particularly in women. Lipid-lowering therapies (LLTs), such as statins and PCSK9 inhibitors, play a crucial role in reducing low-density lipoprotein cholesterol (LDL-C) and preventing CVD. However, women with FH often face disparities in diagnosis, treatment and outcomes.
Objectives:
To assess the effectiveness of LLT in reducing CVD incidence among women with FH and identify gaps in current treatment practices.
Design:
Systematic review.
Data Sources and Methods:
A comprehensive literature search was conducted in December 2024 across PubMed, EMBASE, Web of Science and CINAHL, guided by the PICO framework. Thirteen studies met the inclusion criteria; six were rated high quality using the Evidence-Based Librarianship tool. Due to heterogeneity in study design and outcomes, a narrative synthesis was performed.
Results:
LLT, particularly statins, consistently reduced LDL-C levels and CVD incidence in women with FH. PCSK9 inhibitors and combination therapies offered additional benefit in high-risk cases. Up to an 80% relative risk reduction was observed in women who initiated early and sustained therapy. However, several studies reported that women were less likely to receive intensive LLT, had a delayed diagnosis and were 32% less likely than men to reach LDL-C targets. Data on premenopausal and menopausal women remain limited.
Conclusion:
LLTs are effective in reducing CVD risk in women with FH, yet treatment disparities persist. Addressing barriers such as adherence, hormonal influences and access to advanced therapies is essential. Personalised, gender-specific strategies are needed to close care gaps and improve outcomes for this high-risk population.
Plain Language Summary
Women with Familial Hypercholesterolemia face an increased risk of heart disease. This review examined how well cholesterol-lowering treatments work for women with FH. It found that while treatments like statins are effective, women often don’t receive them early enough or at high enough doses. More personalised and gender sensitive care may help prevent more heart disease in these women.
Keywords
Introduction
Cardiovascular diseases (CVDs) rank as the top global killer, causing about 17.9 million deaths in 2019. 1 In Europe, CVD remains the leading cause of death, accounting for over 3 million deaths annually. 2 The economic burden is also substantial, with costs attributed to health and long-term care, representing 11% of the EU’s total healthcare spending. 3 Familial hypercholesterolaemia (FH) is a hereditary disorder marked by elevated low-density lipoprotein cholesterol (LDL-C) levels, significantly increasing the risk of CVD. 4 Recent estimates suggest that FH affects approximately 1 in 311 individuals worldwide, making it one of the most common genetic disorders. 5 This prevalence suggests that over 25 million people globally have FH. In Ireland, it is estimated that around 20,000 people have FH, yet only a tiny percentage have received a diagnosis. 6 Despite its prevalence, FH remains widely underdiagnosed, highlighting the critical need for comprehensive screening programmes to facilitate early detection and treatment. 7 Since FH is an irreversible risk factor, prompt detection is essential for initiating appropriate treatment. Although lipid-lowering therapies (LLTs), such as statins and PCSK9 inhibitors, are available, studies indicate that many patients with FH fail to achieve optimal LDL-C reduction. 8 This systematic review (SR) examines the effectiveness of LLT in lowering LDL-C levels in women with FH. It evaluates whether current treatment strategies adequately reduce CVD risk in this population.
Women with FH tend to develop atherosclerotic cardiovascular disease (ASCVD) about 7–20 years later than men with FH. 9 If FH is left untreated, an estimated 30% of women will experience a heart attack by the age of 60 years (versus 8% in the general population), compared to men by the age of 50. 10 CVDs remain the leading cause of death among women, particularly due to FH, which increases this risk.11,12 However, there is a significant gap in knowledge regarding the management of CVD risk in women with FH. Primary care nurses play a crucial role in educating patients about the risk factors for CVD by promoting adherence to LLTs and overseeing their overall cardiovascular health. 13
Monitoring LDL-C levels is essential for diagnosing FH, evaluating treatment effectiveness and maintaining target levels to lower cardiovascular risk. Women with FH should strive for an LDL-C level below 2.6 mmol/L or a minimum reduction of 50% from their baseline levels. 14 Women with FH with high LDL-C levels often experience delays in diagnosis, limited access to lipid-lowering treatments and treatment gaps during pregnancy and breastfeeding. 15 Research indicates that FH remains significantly underdiagnosed in many countries, with disparities in healthcare infrastructure affecting access to screening and treatment.16,4 While some countries, such as the Netherlands and the United Kingdom, have well-established FH screening programmes, others struggle with insufficient resources and awareness, leading to missed diagnoses and suboptimal treatment. In Ireland, the management of FH in primary care settings needs to be improved, with limited access to genetic screening in some regions. 17
A lack of resources can hinder general practitioners’ ability to identify at-risk patients, resulting in inadequate care for those with FH.12,18 The above issues are important to explore, particularly for women who face the dual burden of managing both FH and elevated CVD risk. 19
Despite the established link between FH and CVD, research on the effectiveness of LLT, specifically in women with FH, remains limited. A preliminary search was completed across significant databases, including PubMed, CINAHL, EMBASE, Scopus and Cochrane, which did not identify a completed SR addressing this question. Given the existing knowledge gap, this review is essential to evaluating whether current lipid therapies adequately reduce LDL-C levels and prevent CVD in this high-risk population. This SR aims to inform clinical practice and guide future research on optimising FH management in women by synthesising available evidence.
Methods
Design
The SR includes various studies, including randomised controlled trials (RCTs), cohort studies and observational studies. These different designs contribute to variability in the quality and reliability of evidence. These studies were searched using the Cochrane Handbook for Systematic Reviews. 20
Aim and research question
This SR examined the impact of LLT on the incidence of CVD among women with FH. The PICO framework assisted in developing the research question and formulating the inclusion and exclusion criteria.
PICO framework
Outcomes measured
Primary outcome
To assess the impact of LLT on the incidence of CVD in women with FH.
Secondary outcomes
Compare the development of CVD with and without therapy
Comparison of the effectiveness of different LLT
Sex-specific differences in LLT outcomes
Adherence to LLT and its influence on CVD risk
Delayed diagnosis and sex difference in FH prevalence
Search strategy
The present SR included studies that met the following criteria.
Inclusion criteria
Studies that include both men and women may be considered if data for women can be extracted separately.
Studies evaluating the effects of LLT by LDL-C measurements and CVD outcomes.
Study design: RCTs, retrospective analyses, observational studies, cohort studies or case–control studies.
Studies published in English.
Exclusion criteria
Research involving children.
Investigations lacking LDL-C reduction and cardiovascular outcome measurements.
Study types include case reports, series, editorials and animal studies.
Search methods
The following electronic databases were searched:
Web of Science (2015 to January 2025)
CINAHL (2015 to January 2025)
PubMed (2015 to January 2025)
EMBASE (2015 to January 2025)
A database search was conducted to identify relevant articles, assess their eligibility and select those that met the predefined inclusion criteria. 21 This search was conducted across four electronic databases: EMBASE, CINAHL, PubMed and Web of Science, all of which are accessible via the RCSI library. These databases were chosen for their extensive coverage of medical and health literature, ensuring a broad selection of relevant studies.22,23 The search employed keywords following the PICO framework and MeSH terms to refine and clarify the search: Familial Hypercholesterolaemia; Lipid Lowering therapies; Women; Cardiovascular Disease; Female; Cardiovascular mortality; Arteriolosclerosis; Cardiovascular disease, incidence, statins, Low-Density Lipoprotein, High Cholesterol, Coronary Heart Disease, Reducing Cholesterol. Boolean operators (‘OR’ and ‘AND’) were used to combine keywords effectively. Filters were applied to refine the search in line with the inclusion criteria. 24 To ensure thoroughness, additional relevant terms were explored using ‘OR’. The most pertinent results were reviewed to identify potential synonyms that could enhance the search. 22 Grey literature was also considered, including government reports, health service documents, theses, dissertations, conference papers and clinical trial registers. Sources such as GreyNet International and OpenGrey were utilised to identify unpublished or non-peer-reviewed studies that might offer supplementary insights.25,26 In addition to database searches, reference lists from studies identified during the initial search were reviewed, which yielded relevant information and data. 27 DynaMed was also consulted to obtain the latest guidelines for managing FH.
Data extraction
A data extraction template was used to input key data relevant to the question. A table was constructed to outline the characteristics of each study (see Table 1). No data transformations were performed. Where datasets were incomplete, values were excluded from synthesis and the issue was noted.
Characteristics of included studies.
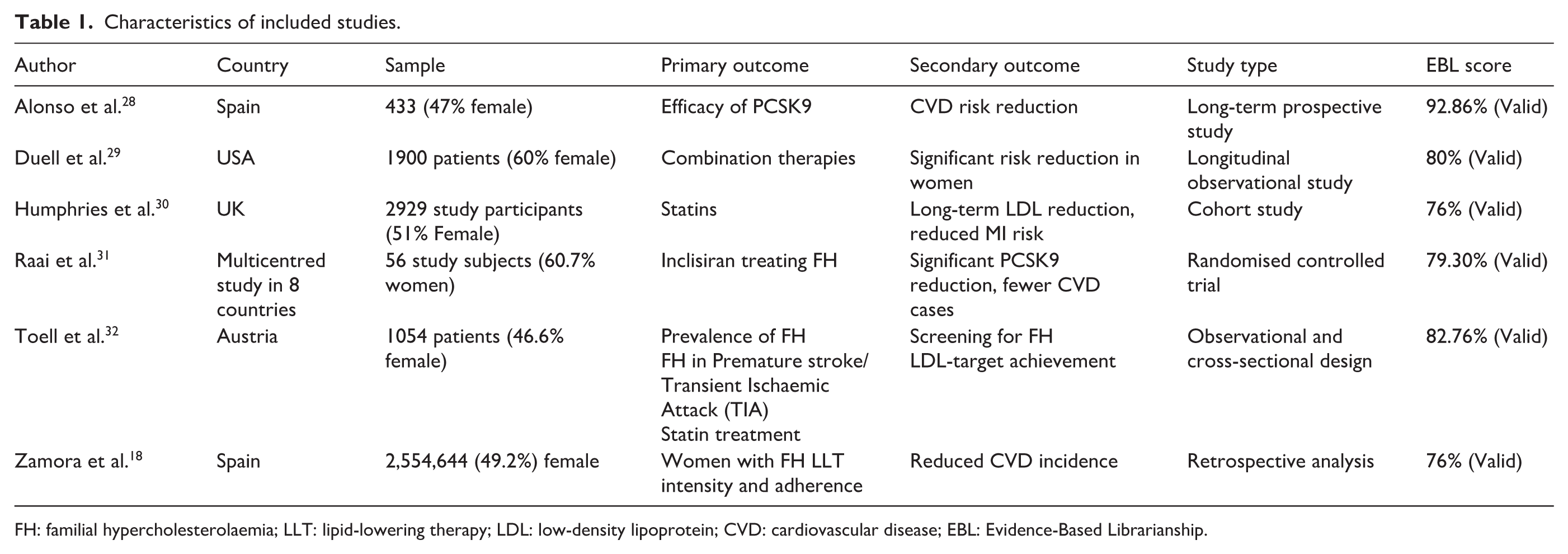
FH: familial hypercholesterolaemia; LLT: lipid-lowering therapy; LDL: low-density lipoprotein; CVD: cardiovascular disease; EBL: Evidence-Based Librarianship.
Data analysis and synthesis
This SR employed a narrative synthesis to interpret findings across studies with heterogeneous designs and outcomes. While quantitative data on LDL-C reduction and cardiovascular (CV) event rates were reviewed, the variability in study methods and populations limited the feasibility of a purely statistical synthesis. The narrative approach proved valuable in capturing essential insights that might otherwise be overlooked through quantitative analysis alone. It explored gender-specific themes that are particularly relevant to women with FH. In addition, subgroup patterns were considered to investigate potential modifiers of treatment effects based on age, type of therapy and adherence levels.
Quality appraisal
The quality of the included studies was evaluated with the Evidence-Based Librarianship (EBL) tool, which assessed search results and identified relevant studies to mitigate publication bias. 33 The EBL tool employs a structured scoring system that evaluates studies across four key domains: population, data collection, study design and results analysis. 34 Each domain was assigned a score based on predefined criteria, allowing for an objective assessment of study rigour. The total EBL score was calculated by summing the domain scores. The higher the score, the stronger the quality. Studies above the set threshold were deemed suitable or included, while those with lower scores were excluded. This approach minimised bias, ensuring that only well-conducted studies contributed to the SR, thereby enhancing validity. 33
Results
The SR analysed 743 articles based on the inclusion criteria. A date range of the past 10 years was applied to focus on recent studies. The initial database searches identified 743 articles, which were reduced to 564 after eliminating 179 duplicates. Screening of abstracts led to the exclusion of 311 articles, while a full-text review eliminated 157 for insufficient data on women with FH and 81 that failed to meet the inclusion criteria. Ultimately, 13 studies were adequate and aligned with the inclusion criteria. After using the EBL tool to assess the validity of the studies, six articles were identified as of high quality (see Figure 1 for the PRISMA diagram).
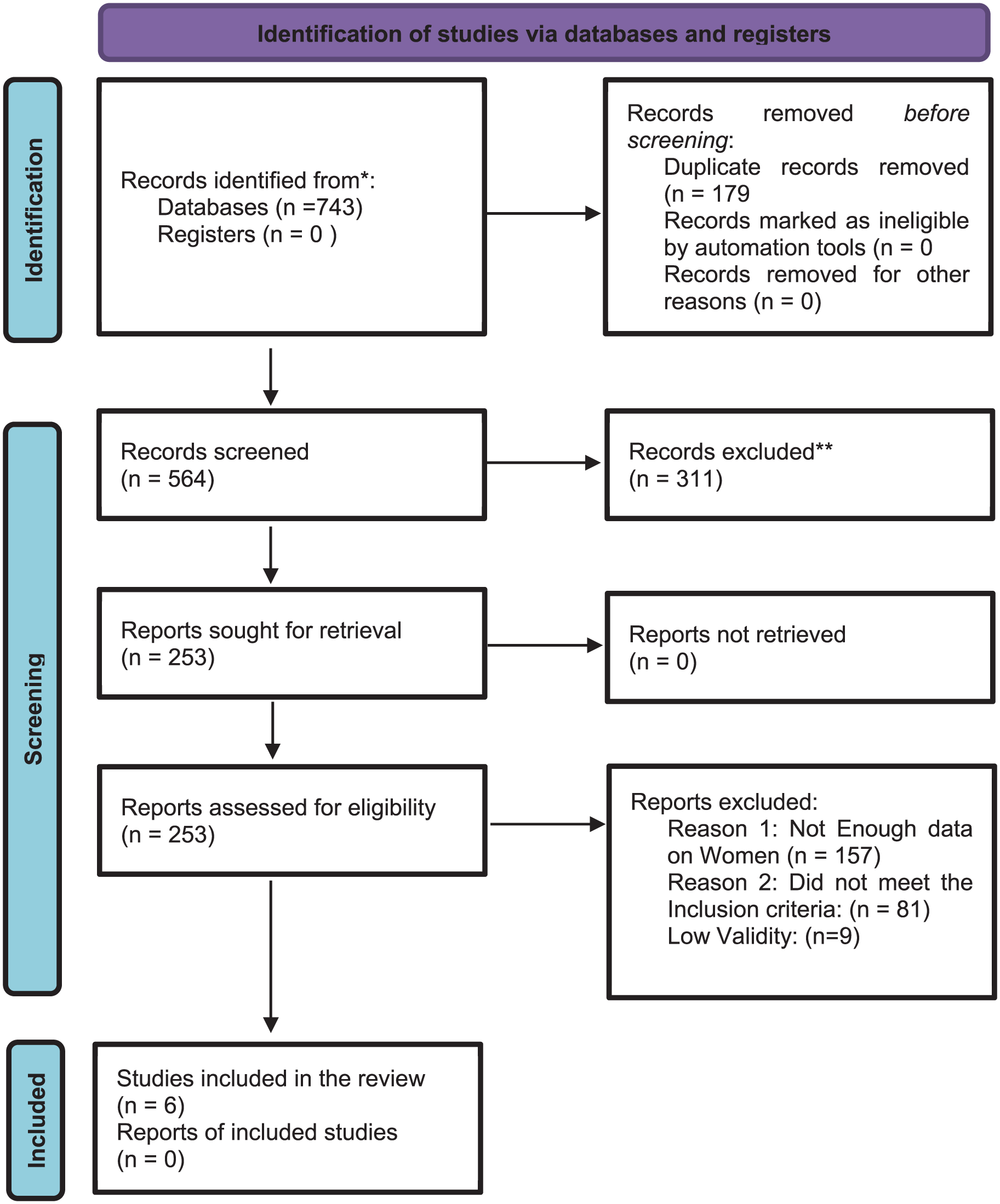
PRISMA 2020 flow diagram.
Study designs
Each of these studies used different methodologies to explore various aspects of LLT and CVD outcomes, providing a comprehensive understanding of the topic from different research perspectives. These studies generally followed quantitative methods, focusing on clinical outcomes like LDL-C reduction, CVD risk and treatment adherence. For example, three studies utilised observational designs.14,32,36 while two conducted longitudinal cohort studies to evaluate treatment effectiveness over time.29,30 One study utilised an RCT, offering experimental evidence on the efficacy of LLT. 31 None of the included studies used qualitative methods, focusing on quantitative data trends and measurable treatment outcomes.
Geographical location
Six studies met the inclusion criteria for various countries worldwide. The studies are conducted in the United States, 29 Spain,14,18 United Kingdom, 30 Austria 32 and multiple countries. 31 This global diversity offers valuable insights into the varying approaches to managing FH across different healthcare systems and populations.
Participants and sample size
Study participants were adult patients who were diagnosed with FH. Many studies included sub-data on women with FH and their response to LLT. The focus on assessing CVD risk and the impact of specific treatments is a common theme in most studies. The review analysed data from six high-quality studies included in this review, encompassing a total of 2,561,016 participants, providing a broad representation of FH populations. The smallest study, 31 included 56 participants, whereas the largest 18 analysed 2,554,644 individuals. The table below provides insights into female participants included in each study, as seen in Table 2.
Female study participants.

A detailed overview of the studies in Table 3, which includes participant demographics, FH subtype, LLTs used, dose regimens, treatment durations, follow-up periods and reported outcomes such as LDL-C reduction, target achievement and CVD mortality reduction.
Summary of study characteristics, treatment regimens and outcomes in women with familial hypercholesterolaemia.
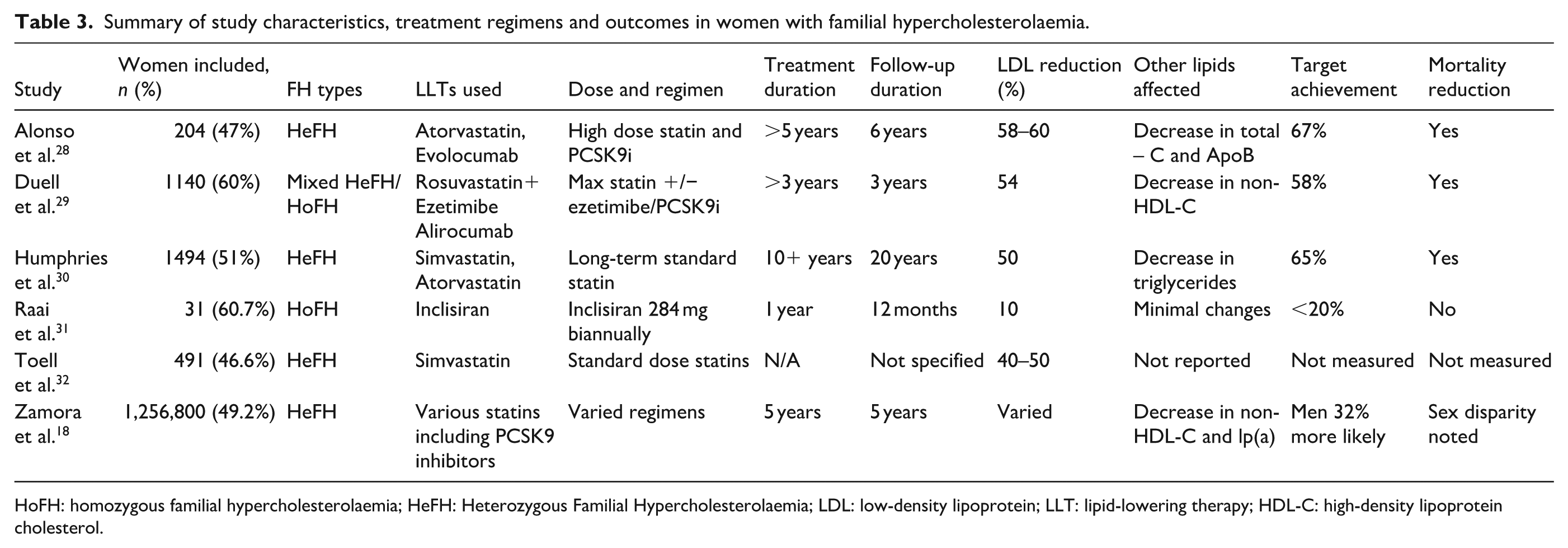

HoFH: homozygous familial hypercholesterolaemia; HeFH: Heterozygous Familial Hypercholesterolaemia; LDL: low-density lipoprotein; LLT: lipid-lowering therapy; HDL-C: high-density lipoprotein cholesterol.
As illustrated in Table 3, high-intensity statins and PCSK9 inhibitors were the most commonly used LLTs, with reported LDL-C reductions ranging from 50% to over 60% in several studies.14,29 Despite therapeutic efficacy, LDL-C target achievement remained suboptimal in some studies, particularly among women with HoFH. 31 Treatment duration and follow-up varied considerably, which may have contributed to the heterogeneity of outcomes. Notably, three studies14,29,30 reported a clear association between LLT use and reduced CVD mortality among female FH patients.
Primary outcomes
Women with FH derive substantial CVD risk reductions from LLT. Statins-based treatment dramatically lowers coronary risk in women with FH compared to historical outcomes without therapy. Untreated FH carries a very high lifetime risk, with approximately 30% of women with FH experiencing a coronary event by the age of 60. 18 The included studies indicate that women initiating LLT before CVD onset achieved a 76% relative risk reduction in coronary events. The types of outcomes reported across these studies, such as CVD incidence, mortality and LLT effectiveness, are summarised in Table 4.
Outcomes measured.
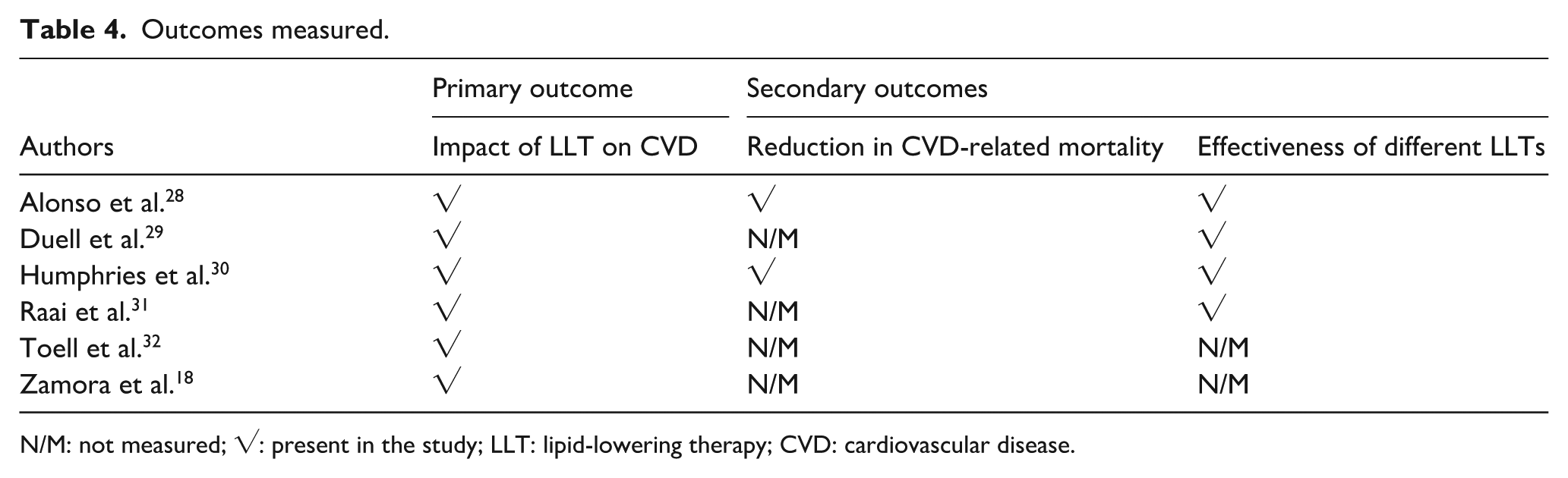
N/M: not measured; √: present in the study; LLT: lipid-lowering therapy; CVD: cardiovascular disease.
Data from the SAFEHEART registry demonstrated that PCSK9 inhibitors significantly reduced LDL-C levels by approximately 58%–60%, with about 67% of patients achieving LDL-C targets, correlating with a significant reduction in the incidence of cardiovascular events. 14 Combination therapies involving statins and PCSK9 inhibitors are highly effective in modifying long-term risk. Conversely, the efficacy of inclisiran appeared limited in individuals with homozygous FH (HoFH), showing minimal LDL-C reduction and limited improvement in CVD risk. 31
The Simon Broome registry, summarised by Humphries et al., 30 reported decreased coronary heart disease mortality among women receiving LLT, especially long-term statin therapy; however, increased mortality persisted in patients with severe FH despite treatment. The CASCADE FH registry data revealed that high-intensity statins and combination therapy regimens led to more significant LDL-C reductions and fewer CV events. 12 A sex-specific disparity was identified in one study, with women being 32% less likely to achieve LDL-C targets compared to men, primarily due to lower adherence and delayed diagnosis. 18 Additionally, untreated women with FH experienced ASCVD events around 20 years earlier than untreated men with FH. 32
Secondary outcomes
A consistent pattern emerged across the included studies, which showed that women who received LLT, particularly high-intensity statins and PCSK9 inhibitors, experienced substantially lower rates of adverse CV outcomes than those who remained untreated or under-treated. Patients receiving LLT, particularly those on a PCSK9 inhibitor, showed a significant reduction in LDL-C levels, with a median drop of 58 mg/dL.14,29 In contrast, untreated women with FH faced a nearly sixfold increase in major adverse cardiovascular events, especially among those with pre-existing ASCVD.29,30,18
Several studies included in this review indicated that women who initiated treatment early and achieved sustained LDL-C reduction experienced a lower incidence of coronary events compared to their untreated counterparts.29,30,18 These findings are consistent with the outcomes reported across the studies as detailed in Table 3.
Comparison of the effectiveness of different LLTs
Statins remain the first-line treatment for women with FH, reducing LDL-C by approximately 50%. High-intensity statin therapy alone was associated with 40%–80% relative risk reduction in CV events.29,30 Where statins were insufficient, adjunct therapies such as ezetimibe and PCSK9 inhibitors contributed to additional LDL-C reductions. Duell et al. 29 observed a 15%–25% LDL-C reduction with ezetimibe, especially in secondary prevention contexts. PCSK9 inhibitors achieved 54%–61% LDL-C reduction, mainly when used in conjunction with maximised statin and ezetimibe therapy. 14 SAFEHEART registry data showed that 67% of patients on PCSK9 inhibitors reached LDL-C targets. In contrast, inclisiran showed minimal LDL-C reduction in patients with HoFH. However, the SR also revealed limitations in therapeutic response, particularly in patients with HoFH, likely due to impaired LDL receptor function. 31 A summary of the comparative effectiveness of these therapies in terms of LDL-C and CVD event reduction is provided in Table 5.
Comparison of LDL-C and CVD event reductions by the LLTs.

FH: familial hypercholesterolaemia; LDL-C: low-density lipoprotein cholesterol; CVD: cardiovascular disease; HoFH: homozygous familial hypercholesterolaemia.
Sex-specific differences in LLT outcomes
Real-world data show that women often receive lower treatment intensities, experience delayed therapy initiation and have a lower likelihood of attaining recommended LDL-C targets.29,18 Women were approximately 32% less likely than men to reach LDL-C targets. 18 Factors such as provider decision-making, pregnancy-related concerns and healthcare access differences were identified as contributing to the underutilisation of optimal therapy in female FH patients, as seen in Figure 2.
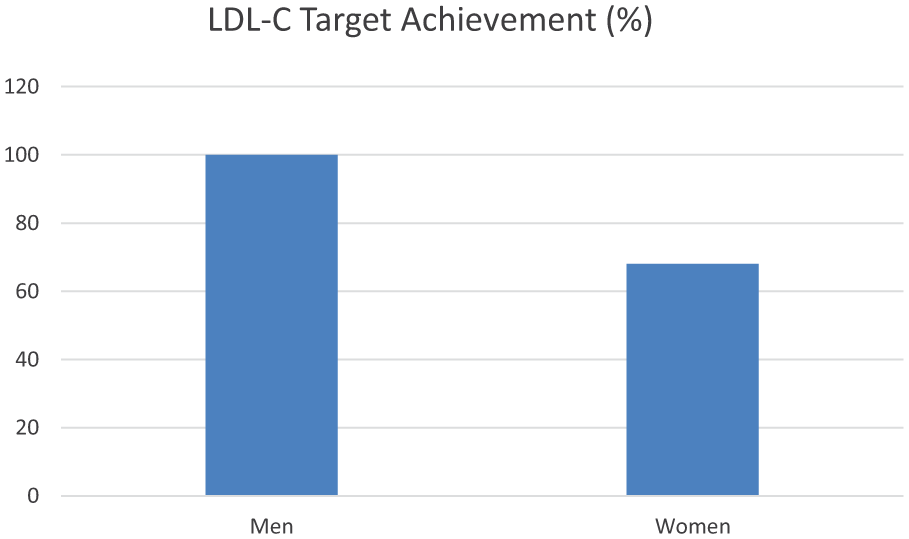
Sex-specific differences in LDL-C target achievement among FH patients.
Adherence to LLT and its influence on CVD risk
Studies consistently reported lower medication adherence rates in women compared to men, with a direct impact on LDL-C reduction and CVD event prevention. 18 Barriers included socioeconomic factors, psychological concerns and adverse effects such as myalgias and statin intolerance.
Delayed diagnosis and sex difference in FH prevalence
Women with FH were often diagnosed later than men, particularly following stroke or Transient Ischaemic Attack (TIA) events. 32 This delay resulted in a more prolonged exposure to elevated LDL-C levels and a higher incidence of premature ASCVD, 18 as shown in Figure 3.

Incidence of ASCVD events by age: Treated versus untreated women with FH.
Data presented in Figure 3 illustrate that untreated women with FH had an ASCVD incidence of approximately 30% by the age of 60. In contrast, those receiving LLT had substantially lower event rates (12%) by the same age.14,30,32 This represents a 60% relative risk reduction, emphasising the life-prolonging potential of early and intensive LLT in women.
Results of quality appraisal
The EBL scores for these studies ranged from 76% to 92.86%, indicating methodological rigour. The majority of the studies achieved high EBL scores (above 75%), demonstrating methodological rigour and the inclusion of relevant and reliable data. The studies had a variety of designs, including long-term prospective studies, longitudinal observational studies, randomised control trials, cohort studies and retrospective analyses. Each study provided valuable insight into the impact of LLT in reducing CVD risk in individuals with FH, as shown in Table 6.
Study validity.

Discussion
This SR shows that LLT, especially statins and PCSK9 inhibitors, significantly lower CVD incidence among women with FH. The reviewed studies consistently reported notable decreases in LDL-C, achieving about a 50% reduction, with PCSK9 inhibitors providing an additional 60% reduction when used with other treatments.30,37 Observational evidence indicates that women who receive early and ongoing LLT can experience up to an 80% relative risk reduction in CVD events compared to those who remain untreated.10,14,37,38 The review also highlighted gender differences in treatment practices and outcomes. Research by Duell et al. 29 and Zamora et al. 18 indicates that women with FH receive less intensive LLTs and are less likely to meet LDL-C targets than men. Later diagnoses and lower adherence rates among women further intensify this disparity. The studies highlight obstacles including worries about fertility and pregnancy, restricted healthcare access and socio-cultural influences such as caregiving roles.22,39 Statins were shown to decrease major vascular events by approximately 20% per millimoles per litre LDL-C reduction in men and about 16% in women.12,37,40,41 Likewise, PCSK9 inhibitor trials included in this review demonstrated consistent risk reductions for both men and women, reinforcing their value as monotherapy and adjunctive therapy in high-risk groups.11,14
New treatments, such as inclisiran, show potential for effective long-term LDL-C management, particularly due to their biannual administration, which could enhance patient adherence. Nonetheless, those with HoFH showed limited effectiveness, indicating a need for personalised treatment strategies. 31 This SR highlights that women with FH who receive proper treatment experience relative reductions in CVD similar to those of men. However, treatment disparities in the real world continue to obstruct optimal outcomes. These disparities stem from factors like clinical decision-making, the absence of sex-specific guidelines and practical challenges, including medication costs and limited access to specialised care.39,42,43 However, despite the established efficacy of these treatments, evidence reveals that women with FH frequently do not fully benefit from available therapies due to systematic undertreatment and unique barriers. Studies from Europe and the United States consistently report that women are prescribed less intensive LLT and are significantly less likely to achieve lipid targets than men.36,38,44 Reasons cited included outdated beliefs about female CVD risk, safety concerns related to reproductive health and clinical misperception of risk urgency. 18 The result is prolonged cumulative LDL-C exposure and increased atherosclerotic burden, often becoming clinically apparent in later life. 30
Importantly, the included studies affirm that adequately treated women with FH derive comparable lifetime benefits from LLT. Although risk reduction appears less pronounced in premenopausal women, the shift of risk following menopause underscores the necessity for early initiation and long-term therapy maintenance. 29 The review and supporting literature suggest that sex-based differences in adherence, access and risk perception contribute more to outcome discrepancies than pharmacologic efficacy. Barriers such as the expense of advanced treatments like PCSK9 inhibitors and inclisiran, as well as gaps in insurance coverage in various countries and interruptions in care, disproportionately affect women. This is due to life-course factors, such as pregnancy and limited access to specialists in this field. 11
Recent real-world data further support the efficacy of LLTs in women with FH. A study by Bosco et al., 45 which included 49% female participants, demonstrated that inclisiran effectively reduces LDL-C in hypercholesterolaemic individuals in routine clinical practice. This strengthens the generalisability of LLT effectiveness to real-world female populations. Despite the benefits, treatment disparities persist. Statin intolerance, which disproportionately affects women, may partly explain lower adherence and intensity of LLR in this group. Casula et al. 24 highlighted a higher prevalence of statin intolerance among hypercholesterolaemic women compared to men, suggesting a need for better-tailored therapeutic strategies. Moreover, emerging evidence suggests that biological differences may influence pharmacogenetic responses. A study by Bosco et al. 46 investigated sex-specific genetic variants associated with poor statin adherence, particularly among women. These findings underscore the importance of considering genetic and sex-specific factors in optimising long-term LLT adherence and CVD outcomes in women with FH.
The review emphasises the urgent need to close the women’s FH care gap. Clinicians are advised to initiate high-intensity statin therapy as early as possible in female patients, reflecting current guidelines that emphasise the importance of early lipid control to prevent vascular damage.29,30,42 PCSK9 inhibitors also provide an effective alternative or adjunctive treatment for women who cannot reach LDL targets or experience statin intolerance.14,42,44
Limitations
This review identified several limitations. Due to considerable heterogeneity in study design, participant populations, interventions, measured outcomes and reporting standards, a meta-synthesis was not feasible. As such, a narrative synthesis was used to integrate findings. The included studies varied in sample size, treatment types, follow-up durations and population subgroups, making direct statistical pooling inappropriate. These studies highlight the transformative impact of LLTs on reducing the burden of cardiovascular procedures and events, providing clear guidance for future clinical practice. Key messages include the timely initiation of therapy, optimal use of combination therapies and the implementation of sustained long-term prevention strategies, ultimately improving patient outcomes and reducing healthcare system burdens.38,44 A notable limitation of this review is the reliance on predominantly observational data, given the scarcity of explicit RCTs focused on women with FH. Although the consistency of evidence strongly supports LDL-C reduction benefits, the precise magnitude of risk reduction in women with FH depends heavily on observational estimates, which could be influenced by biases such as healthy adherence effects of residual confounders. Nevertheless, consistent findings across multiple observational cohorts, including the Simon Broome Register, CASCADE-FH and the Spanish registry, provide substantial credibility to these conclusions.14,29,30 This review did not formally assess reporting bias or certainty of evidence using tools such as the GRADE framework, which may limit the strength of inferences drawn from observational data.
Future research and implications for practice
Future research should focus on conducting high-quality, sex-specific RCTs to evaluate the efficacy and safety of LLTs in women with FH. These trials should explore the impact of hormonal status (e.g. menopause, pregnancy), adherence challenges and pharmacodynamic differences in treatment response. More granular, sex-disaggregated data are needed across all phases of research to support precision medicine approaches to FH management. There is also a need to develop and test target interventions that address adherence barriers unique to women, such as effective management, reproductive considerations and caregiver burden. Health services research should investigate models of care that integrate CVD risk screening into routine reproductive and primary care settings. For clinical practice, these findings reinforce the urgency of initiating LLT early in women and sustaining treatment throughout the life course. Clinicians should adopt a proactive approach to address treatment hesitance, provide education about CVD risk in women and ensure equitable access to advanced therapies. Enhanced guidelines implementation and multidisciplinary management models involving lipid specialists, primary care providers and women’s health practitioners will likely improve outcomes for this high-risk population.
Conclusion
This SR highlights that women with FH face a significantly elevated risk of CVD, effectively mitigated by appropriate LLT, such as statins, ezetimibe, PCSK9 inhibitors and inclisiran. These therapies significantly reduce LDL-C and dramatically lower the incidence of cardiovascular events when optimally applied. However, persistent underdiagnosis, undertreatment and adherence challenges influenced by misconceptions, pregnancy concerns and healthcare biases create a substantial gender gap in outcomes. Addressing these barriers through early FH identification in women, aggressive guideline-driven therapy initiation, effective pregnancy management and equitable access to advanced treatments is essential. Prioritising these areas enables healthcare providers to maximise the therapeutic potential of LLTs, significantly lowering CVD risk in women with FH and ultimately aligning their cardiovascular outcomes.
Footnotes
Acknowledgements
We thank Dr Linda Nugent, for her guidance, expertise and constructive feedback at every stage of this review; RCSI for providing access to the necessary resources and databases that made this research possible; librarians, Brefini and Patrick, for their assistance in developing and refining the search strategy and accessing relevant literature; our family, Robert and Casey, for their constant encouragement and understanding throughout this research project. Finally, our sincere thanks to the IGPNEA and Mizen Medical Practice for their support.
Ethical considerations
Not applicable.
Consent to participate
Not applicable.
Consent for publication
Not applicable.
Author contributions
The author conceptualised the study, conducted the literature search, data analysis and drafted the manuscript. LN provided methodological guidance, critical review and editorial input. All authors read and approved the final manuscript.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data availability statement
Not applicable.
