Abstract
Background:
Person-centered maternity care (PCMC) is a model that prioritizes respect, dignity, and responsiveness to each woman’s needs, values, and preferences during childbirth. It promotes open communication and personalized care, which is crucial for improving maternal satisfaction and increasing hospital-based deliveries. While recognized as a key element of quality maternal care, the implementation of PCMC varies across different countries. This review aims to assess the pooled mean score and key predictors of PCMC in Ethiopia.
Objectives:
This review aims to assess the pooled mean score and key predictors of PCMC in Ethiopia.
Design:
Systematic review and meta-analysis.
Data sources and methods:
This systematic review and meta-analysis followed the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) 2020 guidelines. A comprehensive search was performed in international databases, and registers including: PubMed, Cochrane Library, Google Scholar,
Results:
Seven studies, involving 3383 women, were included in the review. The pooled mean PCMC score was 56.75% (95% CI: 55.08, 58.41). The highest scores were reported in Oromia (60.2) and Addis Ababa (59.2), while the lowest was in South Gondar (52.3). Key factors influencing PCMC included educational status (β: −2.7, 95% CI: −3.98, −1.45), complications during childbirth (β: −5.34, 95% CI: −7.24, −3.44), and time of delivery (β: −3.10, 95% CI: −4.10, −2.11).
Conclusion:
The pooled mean score of PCMC in Ethiopia is lower than in many other countries. Key determinants include women’s education, complications during childbirth, and the timing of delivery. Addressing these factors is crucial for improving the quality of PCMC in Ethiopia.
PROSPERO registration number:
CRD42024603854.
Introduction
Maternal and neonatal mortality rates (MNMRs) remain unacceptably high in many low- and middle-income countries (LMICs).1,2 In response to this critical issue, the World Health Organization (WHO) has strongly advocated for the delivery of high-quality care throughout pregnancy, childbirth, and the postnatal period as a key strategy to reduce mortality and morbidity in LMICs. 3 Delivering high-quality maternity care requires more than just focusing on clinical components; it must also encompass respectful and dignified care. 4 While the clinical aspects of care are central to reducing high mortality rates, addressing both dimensions is essential for comprehensive improvement.4,5
Person-centered maternity care (PCMC) is a vital element of quality care throughout the pregnancy and childbirth journey; it has been identified as a promising factor in reducing MNMR, and the low utilization of facility-based deliveries. 6 PCMC is a core component of quality maternity care, highlighted in the WHO recommendations for a positive childbirth experience. 7 PCMC focuses on delivering childbirth care that is respectful, responsive, and compassionate.6,8 This approach to care is gaining recognition as a crucial aspect of healthcare quality, particularly in maternity services. 9 Effective PCMC ensures care that respects and responds to the preferences, needs, and values of individual women and their families. 10
The core elements of PCMC include dignified and respectful treatment, effective communication and autonomy, and supportive care. 11 Evidence suggests that higher levels of PCMC are associated with improved maternal and neonatal outcomes. For example, studies have found that women who report better PCMC experiences are significantly less likely to experience maternal morbidity (by 62%) and neonatal morbidity (by 26%). 12 Additionally, receiving high-quality PCMC has been linked to a 61% reduction in neonatal complications compared to those who receive poor PCMC. 13 Despite the acknowledged importance of PCMC, there is extensive evidence of poor implementation worldwide, often seen in the mistreatment of women during childbirth. 14
The person-centered approach is a cost-effective strategy applicable in both developed and less-developed settings, significantly enhancing the quality of maternity care. 15 It prioritizing respectful, responsive, and individualized care tailored to women’s unique needs, it fosters compassionate communication and support. 16 This leads to improved maternal and neonatal outcomes, making it a promising solution for enhancing care across diverse healthcare environments, regardless of available resources. 17 Implementation of PCMC is suboptimal and inequitable globally, particularly in communication and autonomy, mean PCMC scores were generally lower in Africa, moderate in Asia, and higher in the United States. 6 Evidence indicates that the implementation of PCMC in LMICs is inadequate, with average scores for PCMC practices not exceeding 50%. In this region, communication and respect for women’s autonomy are often lacking, underscoring a significant gap in PCMC delivery. Additionally, the quality of PCMC varies based on women’s socioeconomic status and the type of healthcare facility where they give birth, revealing disparities in the provision of dignified and supportive care. 11
In Ethiopia, various individual studies conducted in different regions have reported that the mean score for implementing PCMC ranges from 19.07 out of 39 to 65.8 out of 90.18–20. However, these studies have produced inconsistent results with significant variability, complicating efforts to draw general conclusions at the national level. To address this gap and establish robust evidence for best practices, a systematic review and meta-analysis has been proposed. The objective of this review is to assess and consolidate the available data, ultimately estimating the overall prevalence (mean score) of PCMC and identifying its potential predictors in Ethiopia.
Methods
Systematic review registration, data sources, and search strategies
This systematic review had designed to estimate the pooled prevalence (mean score) of PCMC and its predictors in Ethiopia. The protocol was registered in the International Prospective Register of Systematic Reviews (PROSPERO), with a registration ID: CRD42024603854. All published articles were searched in major international databases such as PubMed, Cochrane Library, Google Scholar,
Population (CoCoPop) search strategy was used. The CoCoPop framework is a tool used to structure research questions and guide literature searches, particularly in systematic reviews focused on prevalence and observational data. It stands for Condition (the health issue or phenomenon of interest), Context (the setting or environment in which the issue occurs), and Population (the group of people being studied). Conditions: PCMC, context: Ethiopia, population: pregnant/childbearing women. PCMC in Ethiopia is the outcome of interest. The primary outcome was the magnitude of PCMC in Ethiopia. The secondary outcomes were: the predictors of PCMC. The research question is: What is the magnitude of PCMC in Ethiopia? And what are the key predictors of PCMC in Ethiopia. For each selected CoCoPop component, the electronic databases were searched using keywords and the medical subject heading (MeSH) terms. The search terms were combined by the Boolean operators “OR” and “AND” were used to structure the search effectively (Supplemental Material S1).
Eligibility criteria and study selection
This review included studies conducted using cross-sectional, cohort, or case–control designs that reported on the prevalence, magnitude, determinants, associated factors, or predictors of person-, individual-, women-, or patient-centered maternity care specifically using the standardized 30-item PCMC scale developed by Afulani among women who gave birth in health facilities in Ethiopia who gave birth in health facilities. 21 Subsequently All English language published articles in Ethiopia released between January 2016 and November 5, 2025 were retrieved to these systematic reviews and meta-analysis. All identified articles from the databases and search engines were exported to EndNote 20 for management. First, through review of title, abstract and full paper was done by three reviewers (TNK, KAA, and SAG) independently. Any disagreement with the reviewers was settled by discussion and the involvement of a third reviewer as necessary. Subsequently, a full-text analysis of potentially qualifying studies including identification of duplicated records was done. In cases of duplication, only the full-text version of the article was retained for analysis.
Quality assessment and data abstraction
This systematic review and meta-analysis adhered to the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) 2020 checklist (Supplemental Material S2). The Joanna Briggs Institute (JBI) quality assessment tool was employed to evaluate the quality of the included studies. Quality appraisal was performed independently by two reviewers (TNK and KAA) to minimize bias and enhance the reliability and credibility of the findings. Specifically, the JBI critical appraisal checklist for analytical cross-sectional studies consisted of eight clearly defined criteria aimed at assessing methodological and overall quality of the studies. Each criterion provided four distinct options: “yes,” “no,” “unclear,” and “not applicable.” The maximum score achievable with the JBI tool was 8 (based on the sum of “yes” responses). To determine the quality of each study, a good-quality article were the one that fulfills most of the JBI criteria with minimal concerns about bias, confounding, or other methodological issues.22,23 Consequently, to ensure the validity of the systematic review findings, primary studies classified as good quality were included (Supplemental Material S3). Then, two reviewers (TNK and KAA) independently extracted the pertinent data from the selected articles using a standardized data extraction format prepared in Microsoft Excel. The data extraction format included primary author, publication year, study setting, study period, sample size, the mean score of PCMC and mean score of each three components of PCMC (dignity and respect, communication and autonomy, and supportive care) as reported in the primary studies. All primary studies included in this review assessed PCMC using the standardized 30-item PCMC scale developed by Afulani et al. This scale comprises 30 items divided into three domains and is typically scored on a 4-point Likert scale ranging from 0 to 3 per item, yielding a total possible score of 90. All of the included studies reported both the mean total PCMC score out of 90 and the corresponding normalized score on a percentage scale (out of 100%) to facilitate interpretation and comparison. Since the standard reporting format for PCMC is the mean score out of 90, we used this format for analysis. Both overall and domain-specific PCMC mean scores were used to interpret the level of PCMC in each context and enabled a more nuanced synthesis of findings across studies. And the selected predictors of PCMC (adjusted beta coefficient with confidence interval (CI), extracted directly from the multivariable linear regression analyses reported in each of the individual primary studies. These coefficients represent the adjusted associations between the selected predictors and the PCMC score as reported by the original study authors) were taken based on the available articles (Supplemental Material S4). Then it was exported to STATA version 17 (StataCorp LLC, Texas, USA) for analysis.
Publication bias and statistical analysis
The publication bias was assessed using the funnel plot and Egger’s tests with a p-value of less than 0.05 declared as publication bias.24,25 I2 statistic was employed to assess heterogeneity among studies and a p-value less than 0.05 and I2 ⩾70% was used to declare heterogeneity. As a result of moderate heterogeneity, the random effects model was used as a method of analysis to estimate the pooled effect. The effect of selected determinant variables was analyzed using separate categories of meta-analysis. The findings of the meta-analysis were presented using forest plot and adjusted β-value with its 95% CI. Additionally, we performed a sensitivity analysis to assess whether the pooled prevalence estimates were influenced by individual studies.
Results
Study identification and characteristics of included studies
This systematic review and meta-analysis included published studies on PCMC and determinant of PCMC in Ethiopia using international electronic databases. The initial search yielded 4394 articles, both published and unpublished. After removing 126 duplicates, 4268 articles remained for title and abstract screening, which led to the exclusion of 4200 articles. A total of 68 full-text articles were then assessed based on predefined inclusion and exclusion criteria. Of these, 61 were excluded for not addressing the primary outcomes of interest or for not using the appropriate operational definition of PCMC. Many of these studies focused on respectful maternity care, which is a component of PCMC but does not cover the full scope, leading to their exclusion to avoid bias in the PCMC implementation. Additionally, three studies were excluded because they focused on person-centered abortion care rather than childbirth care,26–28 and one study was excluded as it was focused on person-centered ante natal care. 29 One particular study on PCMC was excluded from the meta-analysis because it used a 13-item PCMC scale, differing from the 30-item scale recommended by other studies; this study reported a mean PCMC score of 19.01. 20 Ultimately, seven cross-sectional studies met the criteria and were included in the final quantitative meta-analysis (Figure 1).

Flowchart of study selection for systematic review and metanalysis on PCMC and its predictors among women who gave birth in Ethiopia.
Characteristics of the included studies
All seven studies included in the review were cross-sectional in design, each reporting both the magnitude and determinants of PCMC among women who had given birth. The studies collectively involved 3383 women in Ethiopia between 2020 and 2024. The largest sample size (763) was from a study conducted in South Gondar, Amhara region, whereas the smallest sample (317) came from a study in Dessie, also in the Amhara region.30,31 The studies were conducted across four regions of Ethiopia: four in the Amhara region,30–33 one from Southern Nations, Nationalities and Peoples region (SNNPR), 34 one from Addis Ababa, 19 and the remained one was from Oromia (Table 1). 18
The characteristics of the included studies on PCMC during childbirth and its predictors among women who gave birth in Ethiopia.

PCMC: person-centered maternity care; SNNPR: Southern Nations, Nationalities and Peoples region.
PCMC in Ethiopia
The meta-analysis of the seven studies showed that the pooled mean score of PCMC among women who gave birth in Ethiopia was 57.92 (95% CI: 55.01, 60.83). A random effect model was used because there is moderate heterogeneity (I2 = 66.6%, p = 0.006; Figure 2).

The pooled mean score of person-centered maternity care during childbirth in Ethiopia.
Subgroup analysis
Subgroup analysis of the mean scores of PCMC across different regions in Ethiopia. The finding of the subgroup analysis reveals consistent PCMC scores within Addis Ababa, Oromia, and SNNPR, but significant variability within the Amhara region (I2 = 79.8%). The overall analysis suggests a moderate level of heterogeneity across all studies, but no significant differences between the regional subgroups (p = 0.513; Figure 3).

Findings of the subgroup analysis by study setting on person-centered maternity care during childbirth in Ethiopia.
Sensitivity analysis
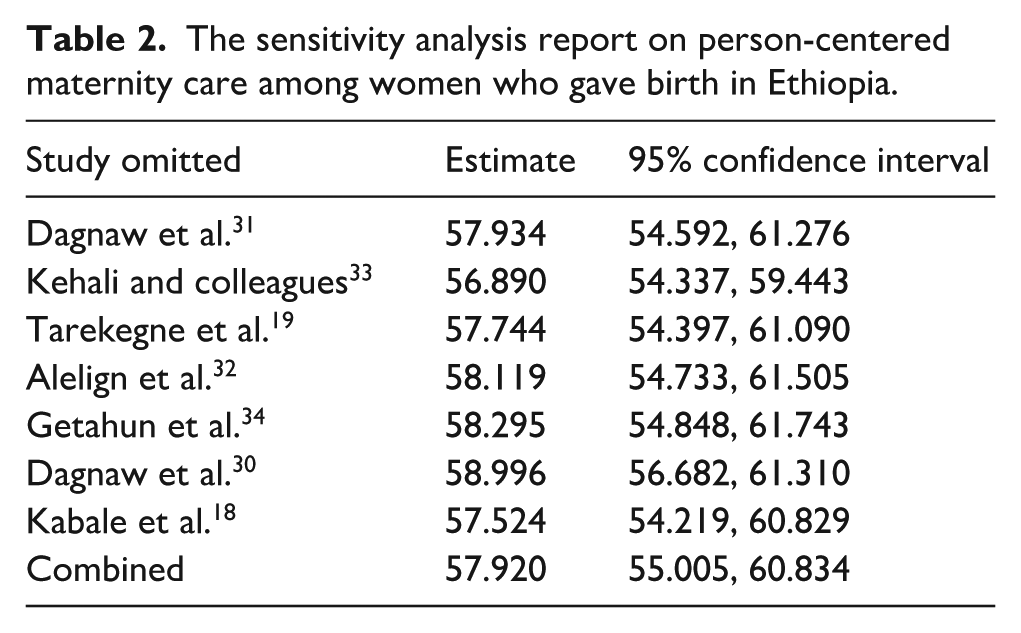
The sensitivity analysis revealed that no single study exerted undue influence on the overall estimate of PCMC prevalence among Ethiopian women. The pooled estimate remained stable, with values close to the overall combined estimate of 57.92%, regardless of which study was excluded. The CI for each omitted study also showed consistency, ranging from approximately 54.2%–61.8%. The estimates varied slightly, from a low of 57.52% when Kabale et al. was excluded, to a high of 58.99% when Dagnaw et al. was excluded. This analysis confirms that the pooled PCMC prevalence estimate of 57.92% is robust and stable. Excluding any one study did not cause significant fluctuations in the overall estimate, with the revised values staying within a narrow range (57.52%–58.99%). Therefore, the meta-analysis results of this studies are reliable and not overly influenced by any individual study, supporting the validity of the pooled PCMC prevalence estimate in Ethiopia (Table 2 and Figure 4).
The sensitivity analysis report on person-centered maternity care among women who gave birth in Ethiopia.

Leave-one-out sensitivity analysis plot of person-centered maternity care during childbirth in Ethiopia.
Publication bias
A funnel plot and Egger’s test were used to assess potential publication bias in this meta-analysis. While the funnel plot appears slightly asymmetric upon visual inspection, the statistical results from Egger’s test indicate no significant publication bias, with a p-value of 0.164. Therefore, the systematic review and meta-analysis do not show evidence of significant publication bias. The slight asymmetry in the funnel plot is likely due to the small number of studies included in the meta-analysis, rather than actual publication bias (Figure 5).

Funnel plot assessing publication bias for person-centered maternity care during childbirth in Ethiopia.
Distribution of the PCMC subscale in Ethiopia
PCMC is assessed using three major subscales: dignity and respect (6 items, maximum score of 18), communication and autonomy (9 items, maximum score of 27), and supportive care (15 items, maximum score of 45), giving a total of 30 items and a maximum score of 90. This review found that, in Ethiopia, supportive care is provided less effectively compared to the other two subscales, indicating a gap in the implementation of comprehensive PCMC.
Dignity and respect
The mean score for implementing dignity and respect during childbirth in Ethiopia is 13.78 out of 18. This score reflects the overall level of attention and priority given to ensuring that women are treated with dignity and respect throughout the childbirth process in the country. The practice of maintaining dignity and respect during childbirth is critical to promoting a positive birth experience, as it encompasses the recognition of a woman’s autonomy, cultural preferences, and personal needs (Figure 6).

The pooled mean score of dignified and respectful care during childbirth in Ethiopia.
Communication and autonomy
The mean score for the implementation of communication and autonomy during childbirth in Ethiopia is 15.68 out of 27. This score indicates the extent to which women are involved in decision-making and whether they experience clear, respectful communication during childbirth. Improving communication and autonomy can also foster trust in the healthcare system and promote more positive experiences for women giving birth (Figure 7).

The pooled mean score of communication and autonomy during childbirth care in Ethiopia.
Supportive care
The mean score for implementing supportive care during childbirth in Ethiopia is 26.27 out of 45. This score reflects the level of support that women receive during labor and delivery, including emotional, physical, and informational support. Supportive care would contribute to a more positive birth experience, improved maternal and neonatal outcomes, and greater satisfaction with the care provided. It could also help in building trust in healthcare services, encouraging women to seek professional care during childbirth and ensuring that their needs are met in a respectful and supportive manner (Figure 8).
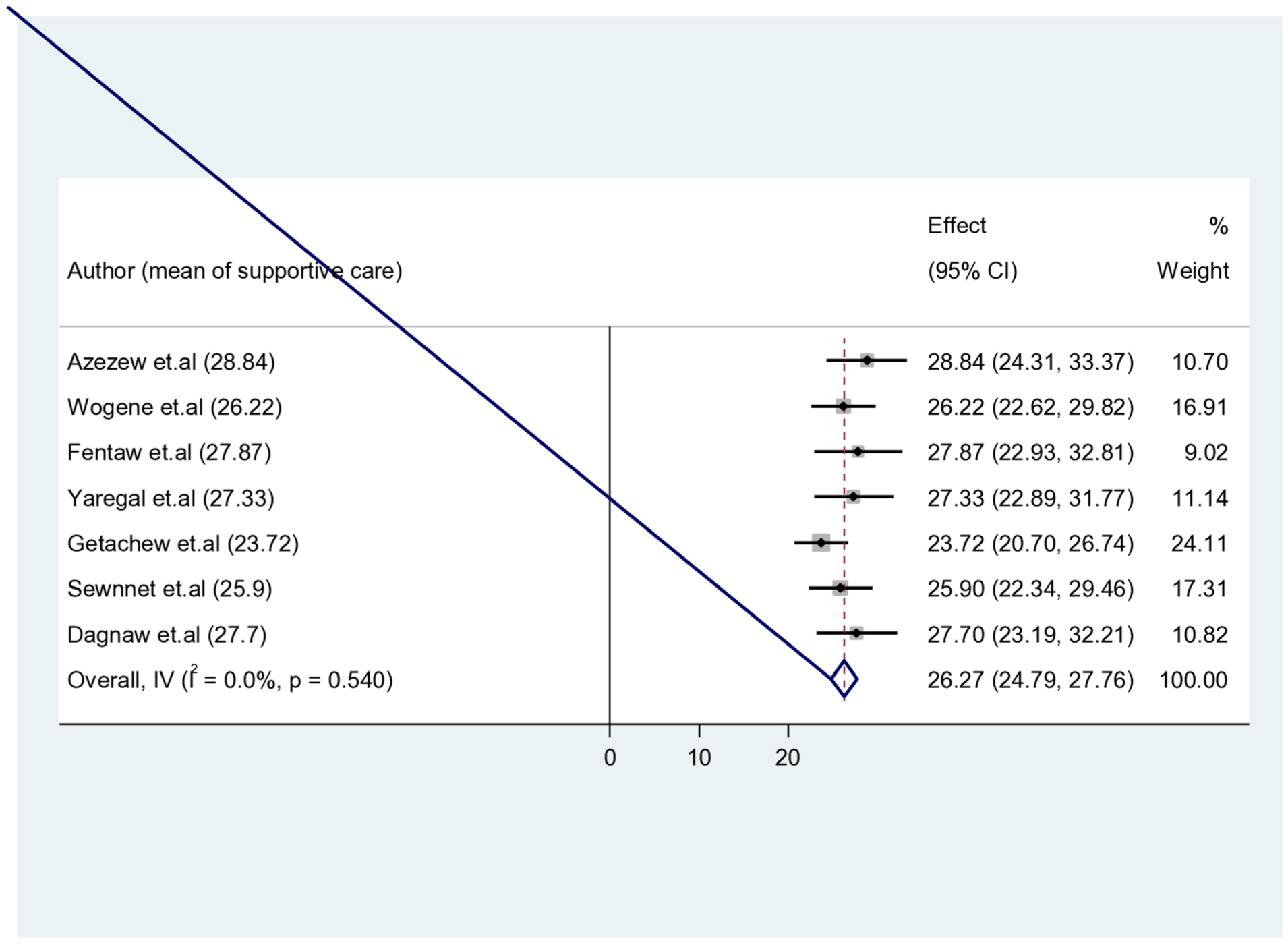
The pooled mean score of supportive care during childbirth in Ethiopia.
Predictors of PCMC in Ethiopia
This meta-analysis identified three significant factors that are strongly associated with PCMC in Ethiopia. These factors include the time of delivery (day or night), the educational status of the women, and complications during the childbirth process.
Time of delivery
Women who gave birth at night in Ethiopia had significantly lower PCMC scores compared to those who delivered during the day. On average, their scores were 3.10 points lower on the 90-point PCMC scale (adjusted β value of −3.10, 95% CI: −4.10, −2.11). This significant difference highlights a disparity in the quality of maternity care based on the time of delivery. Improving PCMC for night-time deliveries requires targeted interventions, such as ensuring adequate staffing levels, providing additional support during night shifts, and training staff to maintain high-quality, patient-centered care at all times (Figure 9).

Relationship between time of delivery and person-centered maternity care during childbirth in Ethiopia.
Educational status of the women
Women without formal education in Ethiopia had significantly lower PCMC scores than those with formal compared to women with formal education. On average, their PCMC scores were 2.70 points lower on the 90-point scale (adjusted β value of −2.7, 95% CI: −3.98, −1.45). This suggests a significant disparity in the quality of maternity care based on a woman’s educational status. Addressing this disparity requires focused interventions, such as health education programs that empower women with information about their maternity care rights and options, as well as training healthcare providers to offer equitable, respectful care regardless of a woman’s educational background (Figure 10).

Relationship between educational status of women and person-centered maternity care during childbirth in Ethiopia.
Complication during the childbirth process
Women who experienced complications during childbirth, either affecting themselves or their newborns, had significantly lower PCMC scores compared to those without complications. On average, their PCMC scores were 5.34 points lower on the 90-point scale (adjusted β value of −5.34, 95% CI: −7.24, −3.44). This significant difference highlights how the presence of complications can negatively impact the quality of care received. By improving the balance between clinical care and person-centered care during complications, the healthcare system can ensure that women receive holistic care that addresses both their medical and emotional needs, ultimately improving their childbirth experience and outcomes (Figure 11).

Relationship between complications during the childbirth process and person-centered maternity care during childbirth in Ethiopia.
Discussion
This systematic review and meta-analysis found that the pooled mean score of PCMC in Ethiopia is 57.92 (95% CI: 55.01, 60.83). This result aligns with similar studies conducted in other LMICs, such as a peri-urban setting in Kenya (58.2 out of 90), India (54), and Nigeria (55.13).11,36,37 The consistency of these findings across diverse geographic regions suggests that there are shared challenges in implementing PCMC in resource-constrained settings.
However, the pooled mean score for PCMC in Ethiopia (57.92) is higher than scores reported in studies conducted in rural Kenya (24.2 out of 39), 38 Ghana (46.5 out of 90), Sierra Leone (38.2 out of 90), 6 and Massachusetts, United States (47.80 out of 90). 9 These differences may be attributed to variations in sociodemographic characteristics and contextual factors that affect the implementation of PCMC. In the case of Kenya, the study was conducted in a rural setting where women may have limited awareness of their reproductive rights during childbirth. This lack of knowledge can hinder their ability to demand or expect PCMC, as they may not fully understand what constitutes respectful and supportive care. Additionally, rural healthcare facilities often face more significant resource constraints, further limiting the delivery of high-quality, person-centered care. In the study from the United States, the focus was solely on primipara women (first-time mothers), a population that may have different needs and expectations compared to multiparous women. First-time mothers may have less experience with the healthcare system and may not advocate for themselves as confidently, potentially affecting their ability to receive PCMC. Additionally, the stress and uncertainty of a first childbirth experience could influence the quality of care they perceive, even in a high-resource setting like Massachusetts. These contextual differences may explain why the review found a higher mean score of PCMC in Ethiopia compared to these other regions.
The findings of this review show that the pooled mean score for PCMC implementation in Ethiopia (57.92) is lower than the global range (60%–90% out of 100) 6 as well as lower than studies conducted in urban areas of Kenya (60.9% out of 100) 11 and Ghana (66.8% out of 100). 38 Several factors may contribute to this difference, including variations in sociodemographic characteristics and disparities in the healthcare systems between Ethiopia and other regions. Another possible reason for the lower score in Ethiopia could be the variation in the implementation of healthcare policies and guidelines aimed at improving maternal care. Countries with better PCMC scores may have more advanced policies or stronger enforcement of standards for respectful maternity care, contributing to higher levels of care and patient satisfaction.
The finding of this review found that women without formal education tended to have lower PCMC scores compared to those with formal education. This is consistent with similar findings from a study conducted in Kenya.21,35 One possible explanation for this disparity is that women who lack formal education may be less aware of their rights during childbirth. As a result, they may not feel empowered to ask healthcare providers about the procedures being performed during labor and delivery. This lack of communication and advocacy could lead to lower-quality, less personalized care for women without formal education, as they may not actively engage in decisions or express their preferences during childbirth. Consequently, healthcare providers may offer less PCMC to these women compared to their more educated counterparts. This highlights the need for improved education and empowerment programs for all women, particularly those with limited formal education, to ensure they are informed and confident in asserting their rights during childbirth.
The results of this review showed that women who gave birth during the night had PCMC scores that were significantly lower than those who delivered during day time. This finding is in line with a study conducted in Kenya. 21 The possible explanation for this difference is that fewer healthcare providers are available during night shifts, creating a mismatch between the number of patients and the available staff. Additionally, since a significant proportion of deliveries occur at night, the workload on the limited staff is disproportionately high, leading to compromised care. 39 This lack of adequate staffing and resources may contribute to the lower quality of PCMC provided to women during night deliveries. Such findings highlight the importance of ensuring adequate staffing and resources during all hours, particularly at night, to maintain the quality of care and ensure that every woman receives respectful, supportive, and individualized care, regardless of when she gives birth.
Women who experienced complications during pregnancy and childbirth were significantly less likely to receive PCMC compared to those with smooth pregnancies and deliveries. This finding aligns with studies conducted in Kenya, Ghana, and other LMICs.35,38,40–42 The possible explanation is that women with complicated deliveries and poor birth outcomes may feel disappointed or distressed, which can hinder open communication with healthcare providers. This breakdown in communication can negatively impact the delivery of person-centered care, as the emotional and psychological needs of these women may not be adequately addressed during the birthing process. Furthermore, the focus on managing medical complications might lead providers to prioritize clinical interventions over compassionate, respectful, and individualized care, further contributing to lower PCMC scores among this group. Perceived lower PCMC scores could be influenced by the emotional response to a negative or traumatic birth experience, even if the actual care provided was technically appropriate and responsive. In such cases, lower PCMC scores might not necessarily reflect poor-quality care, but rather a mismatch between expectations and outcomes, or a lack of emotional closure. Ensuring emotional support and open dialog during such critical moments is essential to maintaining person-centered care, even in high-pressure situations.
Limitation of the review
One key limitation of this systematic review and meta-analysis on PCMC is the small number of the included studies, with only seven studies drawn from four regions of the country. This limited sample size may weaken the comprehensiveness of the findings, as it fails to capture potential variations in PCMC practices across other regions. Consequently, the results may not fully represent the national picture, reducing the generalizability of the conclusions. Expanding future research to include a wider range of regions would provide a more accurate assessment of PCMC across the country, enabling a deeper understanding of the factors affecting its implementation. Additionally, although all included primary studies employed probability sampling techniques primarily simple random and systematic sampling, there remains a potential risk of selection bias, which may affect the representativeness of the study populations. Furthermore, the measurement of PCMC in the included primary studies relied exclusively on self-reported data, which is inherently prone to response bias. Women may not accurately recall all aspects of their birth experiences, or they may hesitate to report negative experiences due to fear of judgment or social desirability bias. This limitation should be considered when interpreting the findings, and future research may benefit from complementing self-report measures with qualitative methods or direct observations to enhance validity.
Conclusion
The mean score of PCMC in Ethiopia is lower compared to many studies conducted in other regions. Key factors contributing to this include women’s educational status, complications during childbirth, and the time of delivery, particularly at night. These factors have been consistently supported by various studies as significant contributors to the lower levels of PCMC. To address these challenges, it is essential to prioritize the improvement of respectful, dignified, and women-centered care in maternity services. We recommend that stakeholders, including policymakers, healthcare institutions, and community leaders, take steps to enhance the training and support for healthcare providers to fully implement PCMC practices. Additionally, empowering women to actively participate in decision-making during their childbirth process is crucial to fostering a more collaborative and respectful care environment. By addressing these areas, Ethiopia can improve the quality of maternal care and ensure better health outcomes for women.
Supplemental Material
sj-docx-1-whe-10.1177_17455057251392349 – Supplemental material for Person-centered maternity care during childbirth and its predictors in Ethiopia: Systematic review and meta-analysis
Supplemental material, sj-docx-1-whe-10.1177_17455057251392349 for Person-centered maternity care during childbirth and its predictors in Ethiopia: Systematic review and meta-analysis by Tirusew Nigussie Kebede, Kidist Ayalew Abebe, Leweyehu Alemaw Mengstie, Moges Sisay Chekole, Sewunnet Azezew Getahun, Tebabere Moltot Kitaw, Birhan Tsegaw Taye and Solomon Hailemeskel Beshah in Women's Health
Supplemental Material
sj-docx-2-whe-10.1177_17455057251392349 – Supplemental material for Person-centered maternity care during childbirth and its predictors in Ethiopia: Systematic review and meta-analysis
Supplemental material, sj-docx-2-whe-10.1177_17455057251392349 for Person-centered maternity care during childbirth and its predictors in Ethiopia: Systematic review and meta-analysis by Tirusew Nigussie Kebede, Kidist Ayalew Abebe, Leweyehu Alemaw Mengstie, Moges Sisay Chekole, Sewunnet Azezew Getahun, Tebabere Moltot Kitaw, Birhan Tsegaw Taye and Solomon Hailemeskel Beshah in Women's Health
Supplemental Material
sj-docx-3-whe-10.1177_17455057251392349 – Supplemental material for Person-centered maternity care during childbirth and its predictors in Ethiopia: Systematic review and meta-analysis
Supplemental material, sj-docx-3-whe-10.1177_17455057251392349 for Person-centered maternity care during childbirth and its predictors in Ethiopia: Systematic review and meta-analysis by Tirusew Nigussie Kebede, Kidist Ayalew Abebe, Leweyehu Alemaw Mengstie, Moges Sisay Chekole, Sewunnet Azezew Getahun, Tebabere Moltot Kitaw, Birhan Tsegaw Taye and Solomon Hailemeskel Beshah in Women's Health
Supplemental Material
sj-xlsx-4-whe-10.1177_17455057251392349 – Supplemental material for Person-centered maternity care during childbirth and its predictors in Ethiopia: Systematic review and meta-analysis
Supplemental material, sj-xlsx-4-whe-10.1177_17455057251392349 for Person-centered maternity care during childbirth and its predictors in Ethiopia: Systematic review and meta-analysis by Tirusew Nigussie Kebede, Kidist Ayalew Abebe, Leweyehu Alemaw Mengstie, Moges Sisay Chekole, Sewunnet Azezew Getahun, Tebabere Moltot Kitaw, Birhan Tsegaw Taye and Solomon Hailemeskel Beshah in Women's Health
Footnotes
Acknowledgements
We would like to express our sincere gratitude to Asrat Woldeyes Health Science Campus, Debre Berhan University for providing us with the time and institutional support (unlimited internet access) to conduct this systematic review and meta-analysis. We also extend our appreciation to the authors of the primary studies included in this review, particularly those who contributed to the development and application of the PCMC framework. Their valuable work laid the foundation for our analysis and significantly contributed to the advancement of evidence-based maternal healthcare practices.
Ethical considerations
Not applicable.
Consent to participate
Not applicable.
Consent for publication
Not applicable.
Author contributions
All authors were involved in reviewing and editing the manuscript and approved the final version for submission.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data availability statement
All data generated or analyzed during this systematic review and meta-analysis are fully included within the manuscript and Supplemental Material.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
