Abstract
Background:
Urinary incontinence is a growing issue among adult women globally. Limited data exist examining the impact of occupational, environmental, and behavioral factors on urinary incontinence.
Objective:
This quantitative, cross-sectional pilot study examined the workplace behaviors of adult women experiencing urinary incontinence. It was hypothesized that specific jobs and work environments would be associated with increased urinary incontinence and urgency based on identified behaviors and work-related conditions.
Design:
This study is a quantitative, cross-sectional survey.
Methods:
Adult women (18 years and older) with a history of urinary incontinence were recruited from August 2022 to February 2023 to complete a one-time survey consisting of multiple-choice and short answer questions identifying specific workplace behaviors and symptoms of urinary incontinence. Descriptive statistics and data categorization were used to observe outcomes and examine relationships between urinary incontinence and particular professions.
Results:
Urinary incontinence and urgency-related symptoms affected healthcare and business professionals at a higher prevalence. The most commonly reported behaviors across all professions consisted of withholding urine and utilizing absorbance products.
Conclusion:
The results of this study will help guide women’s health practitioners in exploring current workplace behaviors that may contribute to urinary incontinence in adult women. With this knowledge, practitioners can provide meaningful education to employers and employees to prioritize toileting behaviors in the workplace.
Background
Urinary incontinence (UI) is a growing issue among adult women worldwide. Globally, 30%–60% of middle-aged and older women report UI with associated symptoms significantly impacting their overall quality of life. 1 Stress UI is defined as urine leakage occurring with increased intra-abdominal pressure, such as coughing, sneezing, lifting, or straining, often resulting from pelvic floor muscle weakness. In contrast, urge UI occurs when urine leaks following a strong and sudden urge to urinate. 2 Age, menopause, detrusor underactivity, and losing urine with defecation are common risk factors for progressive UI; however, workplace conditions may also contribute. 3 A study by Kim and Kwak 4 reveals a significant association between work environments and UI, suggesting that UI is prevalent among working women. Additional evidence supports that work-related behaviors and poor toileting habits contribute to UI symptoms in specific work environments. 5 Past medical histories, such as obstetric and gynecological events, and psychological conditions, including depression and anxiety, also influence work-related behaviors of adult women as these conditions prelude and assist in developing personal habits. 1 Acquired habits associated with UI affecting the workplace include toileting planning, limiting fluid intake, and diet and exercise lifestyle factors. 6
Previous research has identified that the incidence of UI is explicitly frequent among healthcare workers and military servicewomen.7,8 Such work environments and other work-related external factors often contribute to excessive urine withholding as work inconvenience determines the number of voids during the work day. 7 Chronically withholding urine frequently leads to dysfunctional self-management strategies, such as straining or bearing down to void more quickly to return to work. 1 Women often change their behaviors to accommodate their work schedules. 3 Other work-related behaviors associated with UI have been identified, including withholding urine until returning home, avoiding public restrooms, and hovering over the toilet. After developing these habits and behaviors, urgency, stress UI, monthly UI, and infrequent voiding were significantly associated with workplace restroom limitations. 5
The effect of UI behaviors has progressed beyond the workplace, resulting in women experiencing altered concentration, an inability to complete tasks, and feelings of embarrassment or emotional distress in all contexts of their lives. 1 Although some professions have been identified, others with similar work conditions likely contribute to UI and maladaptive behaviors in adult working women. Therefore, further exploration is needed to determine the workplace behaviors of adult women experiencing UI.
Incontinence across occupations
The prevalence and severity of UI may vary for adult women based on their profession. Previous studies focused on professions with long work hours, limited restroom availability, and other work-related reasons. Healthcare workers, teachers, industrial workers, and military personnel are some of the few heavily investigated. A study by Kim and Kwak 4 aimed to determine the differences in general, health-related, and occupation-related characteristics and the association between UI and specific occupations. The study showed an overall prevalence of UI among occupations of 7.5%. 4
The requirements of specific jobs may influence the behaviors associated with voiding when necessary. For instance, a study conducted by Pierce, Perry, Gallagher, and Chiarelli found that the patient-first mind-set was reported as the primary behavioral explanation for withholding in the workplace for nurses and midwives. 6 With an understanding of how these individuals think due to their profession, appropriate interventions can be determined to establish awareness of UI. For example, nurses understand UI diagnoses and the importance of bladder health from their education; however, it is essential to keep them updated on the importance of appropriate habits. 2 Along with the work-related aspects, research has aimed to identify reasons for the increased prevalence of UI among working women. O’Shea et al. 8 found service women’s work environments are often compromised by the climate, availability, and cleanliness of bathrooms, as well as the crowding, decreased privacy, safety concerns, limited sanitary items, heavy material of uniforms, and a lack of trust toward their superiors. Finally, Pierce et al. 6 identified that work conditions and the occurrence of UI could potentially result in an increased likelihood of discontinued work, causing an impact on the quality of life of working women.
Environments
The pressures of the work environment and psychological challenges often advance women into the more severe stages of UI. 3 Pierce et al. 6 conclude that nurses’ and midwives’ urinary symptoms and behaviors depend on multiple socio-ecological influences. These factors may include organizational and policy setting, workplace behaviors, personal attributes, and perceived environments. Specifically, patient acuity, staff-to-patient ratios, adequacy of amenities, legal rest breaks, occupational health policy, and social relationships among coworkers can explain behaviors related to urinary symptoms. The clinical areas for this specific population of women included emergency, intensive care units, general and surgical wards, midwifery, and perioperative settings. Alternatively, healthcare workers in an outpatient clinic identified that they had more authority over when they would use the restroom than healthcare workers in different environments. 7 It is essential to examine environmental barriers to adequately address insufficient workplace amenities. Individuals who report restroom limitations at work indicate that unsatisfactory bathroom environments, restricted availability, and employer restrictions contribute to limited restroom usag. 5 As these studies focus on healthcare careers, it is crucial to determine any additional, significant occupational environments contributing to UI symptomology.
Gaps in the literature
Upon reviewing the current literature, there is little evidence connecting the role of specific professions and the direct impact on UI. Further consideration is needed to explore how physically demanding work environments and other jobs influence UI in adult women. 8 Current research demonstrates that specific work-related behaviors warrant further analysis. 9 Furthermore, there is a lack of investigation related to UI’s negative impact on psychosocial health and quality of life. A preliminary study conducted by Hartigan et al. 7 identified the need for further studies to confirm the relationship between work interference association and toileting behaviors that result in undesirable bladder symptoms.
Various studies reveal that UI is more common in working women requiring physically active work than unemployed women displaying a need for further research regarding the specific jobs of women who experience UI. Determining the physical workload for specific behavioral, environmental, and additional relevant factors is essential. Further occupational health initiatives must be implemented to combat these negative influences and avoid continued patterns of neglecting self-care. Overall, research supports the idea that educational and further research efforts are imperative to promote healthy bladder practices in the workplace.
Methodology
This cross-sectional study surveyed adult women (18 years and older) with a history of UI from August 2022 to February 2023 to examine work history, associated environments, and workplace behaviors. Descriptive statistics and data categorization were used to observe potential relationships between the prevalence of UI and specific professions.
Sample
A sample of healthy adult females with a history of UI was recruited from the community through convenience sampling. Participants must be female, 18 years or older, and have a history of UI to be included in the study. Pregnant women, males, females with no history of UI, and women under 18 were excluded. In addition, individuals 12 months or less from post-surgical procedures, including abdominal, obstetric, and gynecological surgeries, were also excluded from the study. The research proposal was submitted and approved by the University of South Alabama’s Institutional Review Board.
Instrument
The survey instrument was developed using the Qualtrics system. Questions included demographic information, work history, work environments, and habits/behaviors associated with toileting. Questions were posed in multiple-choice and short answer formats to gain contextual information from participants. The survey was disseminated to participants through QR code links and paper-based copies to promote access.
Participants from outpatient therapy clinics, physician offices, and within the community, including community centers and assisted living facilities, and on campus at the University of South Alabama, were invited to complete the survey. Printed flyers with the QR code and copies of the survey were posted in these areas and made available to increase accessibility for all participants. The online version of the survey was created using Qualtrics. Survey questions gathered demographic characteristics and information regarding participants’ work history, conditions, and work environments. Additional questions modified from the International Continence Impact Questionnaire Short Form (ICIQ-SF) aimed to gather information regarding habits/behaviors associated with toileting. Questions were asked in multiple-choice and short response formats to gain contextual information relevant to our research question.
Procedure
Cross-sectional survey research examined adult women’s previous and current workplace behaviors with UI. Individuals were recruited for the study through convenience sampling by distributing and posting flyers with QR codes to the Qualtrics survey to physician offices, outpatient care centers, senior community centers, and assisted living facilities within the Mobile and Baldwin County areas of South Alabama. Paper surveys were also readily available for those who desired them. The individual chose whether or not to participate in the survey. Participation in the survey required approximately two to five minutes. Survey responses were collected, numbered, and quantified. Online survey responses were collected in the Qualtrics system and exported to Excel, while paper survey responses were manually inputted. Descriptive statistics and data categorization were used to track, observe, and document trends. Job categories were created based on broad classification between various sectors based on distinct roles and responsibilities. For example, health professionals included those professionals treating or serving a patient population, business professionals included all executives with desk jobs, educators were grouped for participation in the classroom, and the outliers were placed in a separate group for analysis purposes.
Results
Upon completion of the data collection period, a table of the represented occupations and demographics was developed to understand the sample population better (see Table 1). Represented jobs included professionals from various fields, such as health care, business, education, and others, for a total of 41 participants (see Figure 1). Trends and themes were noted across each professional group regarding symptoms, job functions, work demands, and behaviors (see Table 2).
Participant demographics.

Note. N = 41; *one participant indicated identifying as both White and Asian/Pacific Islander.

Occupations reported across participants.
Frequency of symptoms experienced by participants within job categories.

Note. N = 41; All participants were females.
Healthcare
Participants working in healthcare made up 31.7% of the study population. The professions included nurses, dental hygienists, a physical therapist (PT), an occupational therapist (OT), a speech-language pathologist (SLP), a physician assistant (PA), and a counselor. A total of eight participants within this group reported current symptoms of UI, seven reported ongoing urgency, and two reported other symptoms such as pelvic pain and urgency stress. Job functions of these healthcare professionals consisted of sitting, standing, or walking for long hours uninterrupted. Most participants (7/13) indicated patient care as their job function, with (4/13) patient or client-first employer expectations. Participants reported minimal, poor, or somewhat flexible ability to leave their job posts (4/13), followed by an inability to leave once patient or client care has started (3/13). One participant mentioned that leaving the job post is highly discouraged or frowned upon. The job functions and demands of the indicated professions may relate to unique behaviors associated with urination. These behaviors consisted of the use of absorbance products (8/13), hovering over the toilet (6/13), withholding or delayed urination (6/13), restricting fluids (5/13), premature urination (4/13), a place preference for urination (3/13), and straining during voiding (1/13).
Business
Participants within the business category made up 26.8% of the study population. The professions included within this category are attorneys, legal secretaries, administrative assistants, project managers, bookkeepers, and employees in human resources, accounting, and veteran affairs. Nine participants reported current symptoms of UI, ten reported ongoing urgency, and two reported other symptoms, such as incomplete emptying and pelvic organ prolapse. Most participants in this category said their job functions involved some form of sedentary behavior, such as desk work or computer work (6/11). When further exploring work demands, it was commonly reported that time demands were flexible (6/11) with opportunities for breaks “anytime” or “as much as needed.” On the contrary, some individuals reported high productivity demands, employee expectations, or inconvenience (4/11) as limitations to taking breaks while working. In terms of behaviors, withholding/delayed urination (8/11) was the most commonly reported among the participants, followed by straining during voiding (6/11) to void more quickly, restricting fluids (6/11), premature urination (4/11), use of absorbance products (4/11), and hovering over the toilet (4/11).
Education
Participants working in education-related occupations made up 17% of the study population. These individuals were either currently or previously employed as professors or grade-school teachers. A total of five participants reported current symptoms of UI, and four participants reported urgency. No other symptoms in this group were reported. The job functions of educators in the study consisted of prolonged sitting or standing and frequent positional changes. Regarding work demands, most participants (5/7) reported limited flexibility to leave their job posts and employer expectations centered on the well-being of their students (4/7). These job functions and demands have resulted in the accumulation of unique behaviors affecting urination. Participants reported holding/delaying urination as the most common behavior (6/7), followed by the use of absorbance products (4/7) and hovering over the toilet (3/7). Restricting fluids (2/7), premature urination (1/7), and straining during voiding (1/7) were the least reported behaviors for this group.
Other
Participants in the “other” category made up 24.4% of the study population. The jobs within this category included homemakers, retired individuals, a cashier, and a landscaper. A total of nine participants reported current UI, and five participants reported urgency. No other symptoms were reported. Multiple job functions and work demands were reported due to the miscellaneous nature of this group of participants. Therefore, responses did not reveal any relevant categories. Participants reported the use of absorbance products as the most common behavior (5/10), followed by restricting fluids (3/10) and hovering over the toilet (3/10). Holding/delaying urination (2/10) and premature urination (1/10) were the least reported behaviors for this group.
Consistent symptoms across job categories
Ongoing UI and urgency were reported across all job categories. Thirty-one participants identified ongoing episodes of UI, and 26 participants reported persistent symptoms of urgency. In comparison, four participants reported other symptoms such as pelvic pain, urgency stress, incomplete emptying, and pelvic organ prolapse. Healthcare and business professionals are most affected by current UI and urgency-related symptoms. Trends of limited flexibility and high employer expectations have potentially contributed to acquiring compensatory behaviors to manage toileting needs. The most common behaviors reported across all groups are withholding urine (22) and utilizing absorbance products to absorb leaking urine (21 participants).
Discussion
Forty-one adult women with a history of UI completed a survey identifying their work history, conditions, habits, and behaviors associated with toileting in the work environment. This research examined the relationship between UI and specific jobs. The findings revealed the greatest number of participants with a history of UI were healthcare workers, followed by business professionals, totaling 31.7% and 26.8%, respectively. The remaining participants were from other worker roles, including education, homemakers, and several outlying jobs (Figure 1). While the number of participants is low, it is worth noting that these data add to the previous research identifying that the incidence of UI is explicitly frequent among healthcare workers (7) and remains common among working women. 4 Understanding and acknowledging the frequency of UI among these professions and working women, in general, are essential for promoting workplace inclusivity, implementing supportive policies, and fostering a culture that prioritizes the well-being of individuals managing such conditions. Without these considerations and the implementation of appropriate policy, the idea that the occurrence of UI could potentially result in an increased likelihood of discontinued work, causing an impact on the quality of life of working women, is validated. 6
This research also examined the relationship between UI and specific workplace behaviors (Figure 2). The most common behavior reported among healthcare workers was using absorbent products, hovering over the toilet, and then withholding or delaying urination. In comparison, the business professionals reported withholding and delayed urination as the most common work-related behavior, followed by straining during voiding to void more quickly and restricting fluids. However, this group of workers also reported using absorbent products and hovering over the toilet in fewer numbers. The participants working in education reported withholding or delaying urination as the most common behavior, followed by using absorbance products and hovering over the toilet. The remaining participants reported using absorbance products as the most common behavior, followed by restricting fluids and hovering over the toilet. Observing these reported trends, it is noteworthy that the three most consistent behaviors across all participants and job categories are withholding or delaying urination, using absorbent products, and hovering over the toilet. All such behaviors have been previously identified to have a cumulative effect on bladder health (1) and contribute to UI prevalence. 5 It must also be considered that these behaviors can potentially disrupt daily tasks and job responsibilities as the employee’s focus shifts to a constant concern about leakage, discomfort from withholding urine, and altered toileting habits that may be particularly problematic in jobs that require sustained focus and concentration.
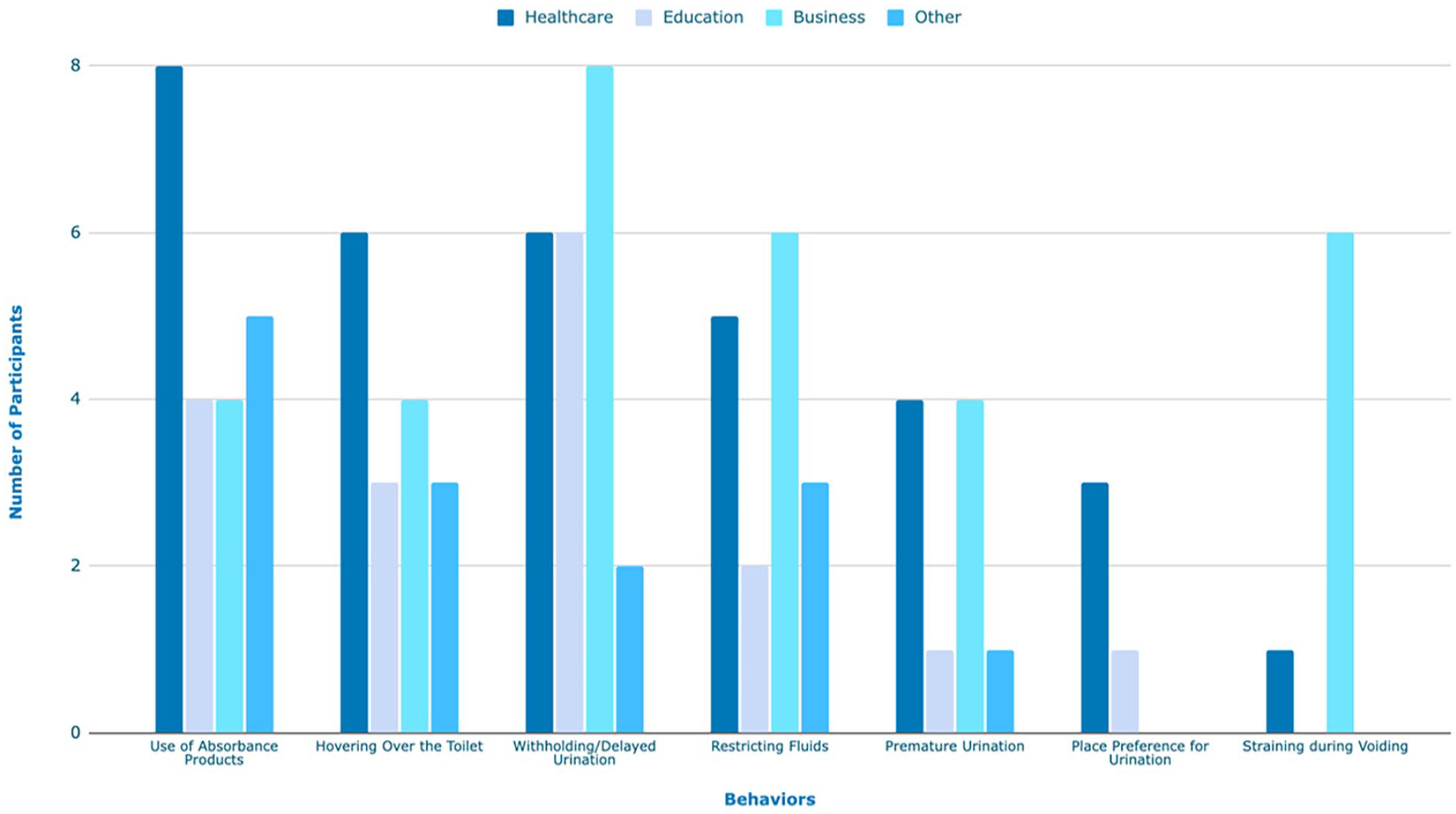
Behaviors reported across occupations.
Moreover, previous research has demonstrated the emotional toll of UI should not be underestimated, as many women may experience embarrassment, shame, and anxiety in the workplace and all contexts of their lives. 1 This emotional burden can contribute to stress and a decline in mental well-being, further impacting job performance and job satisfaction, potentially resulting in an increased likelihood of discontinued work and an impact on the quality of life of working women. 6
At the onset of this study, it was hypothesized that specific jobs and work environments would be associated with an increased prevalence of UI and urgency symptoms based on identified behaviors and work-related conditions. Due to the limited number of recruited participants, it is difficult to conclude that UI is prevalent among specific professions. However, the collected data and observations lend to the validity of previous research identifying the prevalence of UI among healthcare workers (7) and that specific work-related behaviors exist across professions, warranting further analysis. 9 Finally, this study adds to the literature linking the relationship between workplace behaviors that result in undesirable bladder symptoms and compromised quality of life. 7
Limitations
The limited number of recruited participants was the most limiting factor of this study. This limited number could have been due to multiple reasons, including time, interest, and the decreased desire to discuss intimate personal hygiene topics. Furthermore, convenience sampling lacked diversity within the participant pool, including occupation and race. It is also important to note that the sample may not fully represent the broader population despite every effort to maximize recruitment. This study serves as a pilot for future research as it demonstrates a small sample of the population through convenient sampling. It is recommended a power analysis and a sample size be determined in the future to best represent the population as a whole. Another noted potential limitation was some participants likely did not understand the medical terminology used to describe symptoms, which could have caused misunderstandings when reporting symptoms. Strategies such as further education to gain the interest and confidence of participants, utilizing methods outside of convenience sampling, and clearly defining symptoms to participants would result in more robust methodologies for future research.
Conclusion
Although reported jobs vary in terms of roles, job functions, and work demands, a significant number of adult women are experiencing UI. This increasing incidence indicates a relationship between the work environment and the accumulation of behaviors contributing to the development and progression of incontinence.
This study will prove beneficial as practitioners can use the results to review current workplace behaviors that may contribute to the occurrence of UI in adult women. Specifically, it is essential to determine the most prevalent professions associated with UI based on these reported behavioral and environmental factors. The knowledge obtained can be used to develop community occupational health initiatives to reduce UI occurrence in adult women. Education should be implemented in various workplace environments to avoid undesirable bladder symptoms resulting from toileting patterns and behaviors.
These results establish that all Women’s Health practitioners must provide workplace education to promote healthy toileting practices. Adult women need specific strategies to manage their self-care efficiently while at work. Women’s Health practitioners can provide meaningful education to employers and employees to prioritize pelvic health and decrease the number of women affected by UI through preventive practices.
Supplemental Material
sj-docx-1-whe-10.1177_17455057241249865 – Supplemental material for Examining workplace behaviors in adult women with urinary incontinence: A pilot study
Supplemental material, sj-docx-1-whe-10.1177_17455057241249865 for Examining workplace behaviors in adult women with urinary incontinence: A pilot study by Catherine Brock, Samantha Elliott, Sarah Miller, Riley Polomsky, Brooke Shoemaker and Megan Sullivan in Women’s Health
Footnotes
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
