Abstract
Alcohol is legalized and used for a variety of reasons, including socially or as self-medication for trauma in the absence of accessible and safe supports. Trauma-informed approaches can help address the root causes of alcohol use, as well as the stigma around women’s alcohol use during pregnancy. However, it is unclear how these approaches are used in contexts where pregnant and/or parenting women access care. Our objective was to synthesize existing literature and identify promising trauma-informed approaches to working with pregnant and/or parenting women who use alcohol. A multidisciplinary team of scholars with complementary expertise worked collaboratively to conduct a rigorous scoping review. All screening, extraction, and analysis was independently conducted by at least two authors before any differences were discussed and resolved through team consensus. The Joanna Briggs Institute method was used to map existing evidence from peer-reviewed articles found in PubMed, CINAHL, PsycINFO, Social Work Abstracts, and Web of Science. Data were extracted to describe study demographics, articulate trauma-informed principles in practice, and gather practice recommendations. Thirty-six studies, mostly from the United States and Canada, were included for analysis. Studies reported on findings of trauma-informed practice in different models of care, including live-in treatment centers, case coordination/management, integrated and wraparound supports, and outreach—for pregnant women, mothers, or both. We report on how the following four principles of trauma-informed practices were applied and articulated in the included studies: (1) trauma awareness; (2) safety and trustworthiness; (3) choice, collaboration, and connection; and (4) strengths-based approach and skill building. This review advances and highlights the importance of understanding trauma and applying trauma-informed practice and principles to better support women who use alcohol to reduce the risk of alcohol-exposed pregnancies. Relationships and trust are central to trauma-informed care. Moreover, when applying trauma-informed practices with pregnant and parenting women who use alcohol, we must consider the unique stigma attached to alcohol use.
Keywords
Introduction
To understand the relevance of trauma-informed approaches with women who use(d) alcohol during pregnancy, it is important to situate the role of alcohol in girls’/women’s lives when they are pregnant. Alcohol is an increasingly common substance used by pregnant girls and women in many countries. 1 For example, in Canada, 70%–80% of women of childbearing age drink alcohol and approximately 22%–25% report heavy drinking (defined as four or more drinks on one occasion). 2 The reasons why women drink alcohol while pregnant are highly varied and complex. Reasons range from not knowing they are pregnant and enjoying alcohol as a social norm and lubricant, to coping with compounding realities of trauma, systemic inequities, discrimination, mental health challenges, and violence.1,3–6
Alcohol use during pregnancy is intertwined with social and structural determinants of health, including early childhood experiences of trauma and violence, patriarchy and toxic masculinity, mental health challenges, racism and discrimination, contemporary and historical forms of colonization, as well as the lack of access to supports and services for mental health and/or trauma.7–11 In addition to early childhood experiences of trauma, people experiencing social and health inequities frequently live with elevated health burdens, including preventable injuries and chronic diseases that contribute to an increased likelihood of mental health and substance use challenges.12–14 Moreover, women globally are disproportionately affected by intimate partner and domestic violence, fewer opportunities for employment with liveable wages, inequitable parenting and other caregiving responsibilities, and other forms of gender discrimination.15–17 As a legal and accessible substance, alcohol is commonly used for self-medication and as a coping method. 18
While public and private messages aimed at women consuming alcohol greatly vary by cultural norms, places that endorse and market alcohol to all legal drinking ages, regardless of gender or childbearing years, also shame women who drink alcohol while pregnant for the potential harm it may have on a fetus. If a woman has a child with fetal alcohol spectrum disorder (FASD), a lifelong developmental disability resulting from prenatal alcohol exposure, she often experiences many forms of judgment, assumptions, guilt, fear, and shame.19,20 These judgments, assumptions, guilt, and shame associated with having to disclose or explain prenatal alcohol use usually surface out of concern for children with FASD, and not the mothers themselves—sometimes resulting in having children removed from their mother’s care and placed in foster care, with no clear mandate to support the mother.21–24 Stigma, blame, and shame attached to consuming alcohol during pregnancy for women is a real and significant barrier to accessing support, information, resources, and care for themselves, their child(ren), and their families.25,26
Experiences of trauma and trauma-informed approaches
Some women may drink alcohol to cope with trauma and life challenges. 27 Trauma results from experiences that overwhelm an individual’s coping capacity and can interfere with an individual’s sense of security, safety, and self-efficacy. 28 In an earlier study of 80 women in Washington State who had given birth to children with FASD, 95% of the women had been abused as a child or adult, 80% had a major mental illness, which included 77% being diagnosed with post-traumatic stress disorder, and 72% were unable to reduce their alcohol consumption because of their experiences in abusive relationships. 29 The interconnections between trauma, substance use, discrimination and racism, violence, as well as social, health, and material inequities are inherent and well documented.30–32
Trauma-informed approaches take into account the long-lasting emotional responses from distressing events, both the past and present in all aspects of service delivery. Trauma-informed approaches also respond to the judgmental and accusatory narrative around alcohol use in pregnancy. Furthermore, trauma-informed approaches involve acknowledgment that women may not attend services not because of a lack of interest or desire, but because of specific past experiences of trauma, thus allowing providers to adapt service provision to better support women who experience barriers to substance use and related services.
Trauma-informed practices acknowledge a person’s life experiences and impacts of trauma, avoid re-traumatizing them, and support safety, choice, and control so that an effective and sensitive response can be adopted in practice and service delivery. 33 Four key principles guide trauma-informed approaches including: (1) trauma awareness; (2) safety and trustworthiness; (3) choice, collaboration, and connection; and (4) strengths-based approach and skill building. 34 Being trauma-informed does not necessarily require disclosing or treating trauma; rather, it means working in ways that support healing and acknowledge women’s circumstances without retraumatizing them. 34 Because pregnant women can be especially vulnerable to violence and trauma, 35 trauma-informed practices are vital in supporting women, particularly when helping women to reduce alcohol use in their current pregnancy or in future pregnancies. How trauma-informed practices are being used and experienced, or how impactful they are, in diverse settings where girls and women who use(d) alcohol during pregnancy are accessing programs, services, or supports is not well documented.
This study
In this scoping review, our objective was to synthesize existing literature and identify a range of promising trauma-informed approaches when working with pregnant and/or parenting women who use(d) alcohol. By mapping and examining promising trauma-informed approaches, programs, and initiatives, we aimed to advance and highlight approaches that better support women who use alcohol to reduce the risk of alcohol-exposed pregnancies.
Throughout this article, we use the term substance use instead of terms such as “problematic substance use” and “substance abuse” because not all substance use should be seen as problematic, and “abuse” is a word reserved for harm inflicted on people. In cases where authors reported on women diagnosed with substance use disorder, we did not change the terminology. We deliberately use the term live-in to describe any programs or services that include living accommodations instead of “residential” because of its association with residential schools, educational institutions that many Indigenous children were forced to attend across Canada, the United States, Australia, and Aotearoa (New Zealand), in efforts to colonize Indigenous People. We use the term women to include people of any gender who were pregnant or had given birth, recognizing that authors of analyzed studies used did not define or qualify how they used or understood sex and gender in their research when reporting on girls, females, and women.
Methods
Scoping reviews are useful in providing a broad overview of a topic by mapping and examining emerging evidence. 36 They are effective in clarifying key concepts, examining critical gaps in knowledge, and reporting on types of evidence that address and inform practice. We used the Joanna Briggs Institute’s (JBI) Review Methodology which consisted of five key steps: (1) identifying the research question; (2) identifying relevant peer-reviewed studies; (3) study selection; (4) charting the data; and (5) collating, summarizing, and reporting the results. We followed the Preferred Reporting Items for Systematic Reviews and Meta-Analyses extension for Scoping Reviews (PRISMA-ScR) checklist. 37 See Figure 1 for the PRISMA flow diagram.

PRISMA flow diagram of records.
Search strategy
An initial concept chart was developed using the JBI Population/Concept/Context (PCC) framework to inform the search strategy.39,40 The concept chart was developed by the second author (YA), discussed with three members of the research team (MEMN, LW, and KDH), reviewed by other co-authors and a research librarian (DC). YA identified nine relevant peer-reviewed articles that were essential to the review and DC conducted an analysis of keywords in the titles, abstracts, and the index terms of the relevant articles and refined the concept chart into a search strategy. These relevant articles were retrieved through researching databases for studies that explicitly utilized trauma-informed approaches related to pregnant and/or pregnant women who use(d) alcohol. The subject headings and keywords used are outlined in Supplementary File 1. The keywords included, but were not limited to, pregnancy, substance use, prenatal care, parenting, social determinants of health, stigma, harm reduction, and social support. This strategy was translated into CINAHL (EBSCO), PychINFO, Social Work Abstracts, and Web of Science. The final search of peer-reviewed published literature was run by YA on 19 January 2022 to include results dating back to 2005 when the Canadian guidelines for FASD were first published. When the guidelines were released, there was increased attention to potential harms associated with drinking alcohol during pregnancy and we were interested in analyzing relevant research conducted since that time. 36
Identifying relevant studies
All citations were imported into Covidence, a data screening and extraction software system for reviews. 37 After duplicate articles were removed by the software, the research team members met to discuss inclusion and exclusion criteria to maximize inter-rater reliability. Two reviewers independently screened each title/abstract and full text. Any conflicts at the title/abstract screening stage were reviewed through discussion between LW and YA. Before starting the full-text screening, all reviewers (except DC) pilot screened a sample of five articles outside of Covidence to test for consistency between team members and discussed conflicts until consensus was reached. For full-text screening, conflicts were discussed by the reviewers in conflict or by a small team of three reviewers [YA, MEMN, LW].
Inclusion criteria were: primary studies published in English between 2005 to 19 January 2022; within Canada, Australia, Aotearoa, United States, South Africa, or the United Kingdom; reported on interventions with pregnant and/or parenting women who use(d) alcohol (alone or with other substances) or whose children have FASD; reported on approaches, programs, tools, supports, or models linked to pregnant or parenting girls/women; and contained evidence of trauma-informed practices. We determined which countries would have the most studies related to women, pregnancy, and alcohol use based on our familiarity with FASD prevention-related bodies of literature. We excluded: discussion, commentary, literature review, or prevalence articles and case reports; interventions that targeted substances that did not focus primarily on alcohol; preconception approaches and programs; articles that had no women-specific population interests, focus, or outcomes; articles focused on foster/adoptive families or parents generally; and articles that focused on health-care providers’ perspectives or perceptions of an intervention. The inclusion and exclusion criteria were determined based on the research team’s previous experience and publications on FASD and women who use(d) substances.18,25,41–43
Data extraction
Data extraction was conducted by five team members [YA, NB, LW, KDW, MEMN] within Covidence. Extraction fields were discussed and finalized through team discussions to map and examine available evidence that would help us identify promising trauma-informed approaches and practices with pregnant and parenting women who use(d) alcohol during pregnancy. We extracted information about the study demographics, the approach or interventions, the results, recommendations, and how trauma-informed practices were applied (see Table 1). After two reviewers independently extracted from each article, MEMN reviewed all extracted information by both reviewers to create a “consensus” response to each extracted field. The consensus extraction fields were exported out of Covidence and into Microsoft Excel for analysis.
List of extraction headings and questions.

Data analysis
Exported data were “cleaned” to have consistent categories and terminology to describe locations (e.g. “Breaking the Cycle treatment program” to “multi-service maternal substance use treatment program in Toronto”), populations studied (e.g. “women accessing Sheway services” to “pregnant and parenting women with substance use, and their children, accessing an interdisciplinary wraparound program”), and study settings (e.g. “residential substance abuse treatment program participants were interviewed about their time in the facility where they stayed for a period of time” to “live-in substance use treatment program where the majority of women were Indigenous, between age 16–31, from rural and/or reservation communities and where people are court mandated to attend the program”). For qualitative descriptions of program or initiative approaches, reported trauma-informed practices, terms used to describe trauma-informed approaches and practices, barriers, outcomes, as well as practice and research recommendations, we thematically open-coded and organized the data. MEMN and YA independently conducted an initial analysis before discussing and reaching consensus on themes. After consensus was reached, MEMN and YA re-analyzed the data before sharing and discussing preliminary themes with other team members. The team discussion on the findings resulted in re-analyzing the trauma-informed practices data using a deductive approach with four trauma-informed principles articulated in the Trauma-Informed Practice Guide, which is widely recognized in Canada: (1) trauma awareness; (2) emphasis on safety and trustworthiness; (3) opportunity for choice, collaboration, and connection; and (4) strengths-based approach and skill building. 34 We chose to organize the findings by principles so that readers could see how trauma-informed practices were operationalized across diverse practice modalities.
Results
Study selection and characteristics
The database searches yielded 7615 unique references after duplicates were removed. After screening all titles and abstracts, 423 articles were retrieved and a total of 37 articles were included for analysis as shown in the PRISMA flow diagram (Figure 1). Two articles reported on the same study so they were analyzed together and represented in Table 2 in the same row,44,45 resulting in 36 included studies.
Summary of analyzed studies.
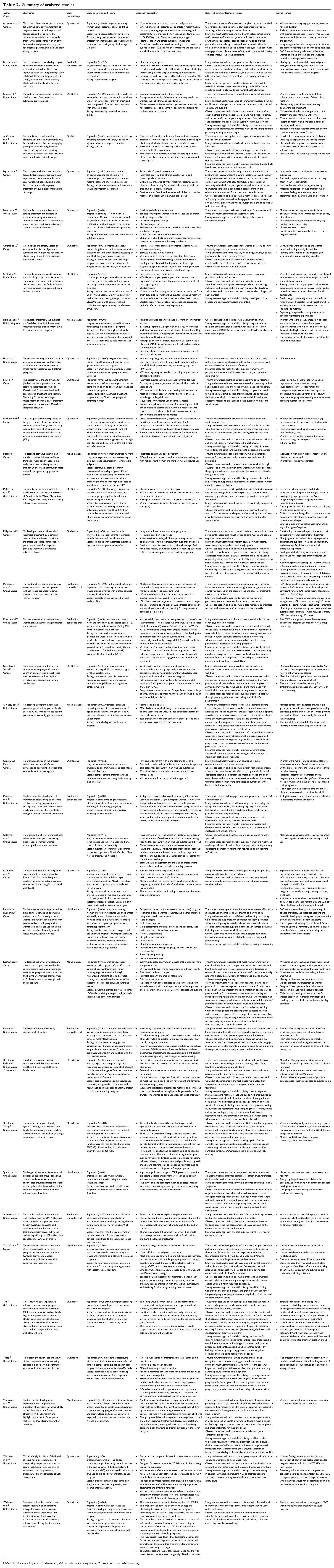
FASD: fetal alcohol spectrum disorder; AA: alcoholics anonymous; MI: motivational interviewing.
The majority of studies were conducted in the United States (n = 22)44–66 and Canada (n = 13),66–79 with one study in the United Kingdom. 80 Seventeen studies were conducted in live-in and/or outpatient treatment centers;46,47,49,51,52,54,56–58,61,63,64,66,68,70,73,76 six studies described their program, service, or intervention to be in non-medical settings offering case coordination, integrated or comprehensive supports from multiple sectors, or wraparound programs where a wide range of programs and services were provided in one location;44,45,69,75,77,78,81 four were based in a medical clinic as the single point of access or the entry point for women to be connected with an intervention or additional supports;47,55,62,69,73 four were home-based or part of an outreach program;48,56,60,64 and one was unclear. 53 While 14 studies included mothers only,44,45,47,49,52,53,56,58,59,63,64,66,70,74,76 14 included pregnant women and mothers,46,54,55,57,60,63,67,68,71,72,75,77–79 and nine were with pregnant women only.48,50,51,54,61,62,69,73,80 Table 2 details summary information for each included study.
The authors of many studies spoke of barriers to care, such as childcare, transportation, and location of programs. Even in the context of studies about programs, services, and interventions that aimed to reach and support pregnant and/or parenting women with substance use, four studies reported on stigma and/or fear of losing custody of their children as barriers to seeking care.54,71,75
Terms and concepts used to describe trauma-informed approaches and practices
Authors used various terms and phrases to describe trauma-informed approaches and practices in the absence of using the explicit term “trauma-informed.” These terms and phrases included: relational, judgment-free, supportive, emotionally safe, culturally safe/responsive, harm reduction, holistic, women-centered, strengths-based, individualized, self-determination, and wraparound.
Authors often also described programs and services as being integrated, comprehensive, one-stop, single access, or wraparound. However, it was not always clear how these terms were operationalized or understood, nor were they necessarily comparable. For example, Breaking the Cycle 67 and two family medicine clinics 69 were both described as “integrated care” programs for pregnant women using substances. While Breaking the Cycle is a program that collaborated with nine agencies including child protection, substance use treatment, corrections and probation, health, and child mental health and development, 67 the family medicine clinics offered primary care from physicians, nurse practitioners, midwives, and obstetricians, as well as a substance use counselor and psychiatrist. 69 Both aforementioned examples offered an integrated program; (1) Breaking the Cycle addressed both primary and social determinants of health, whereas (2) the family medicine clinics addressed integrated primary care services. In short, terms and descriptions of programs, services, and interventions, as well as trauma-informed approaches and practices, varied greatly across articles.
Thematic findings
The thematic findings were organized by the four trauma-informed principles, highlighting how each principle is practiced across multiple settings and contexts, as well as the reported outcomes. We organized the findings in this way to present grouped examples of how trauma-informed principles were put into practice across the varied settings, geographies, and populations included in this scoping review.
Trauma awareness
Trauma awareness refers to learning and understanding what trauma includes, how it can impact individuals and groups, how people cope, and recognizes the importance of accounting for trauma when supporting people, without requiring individuals to recount their traumas. 34 A number of studies indicated that staff understood, recognized, and accounted for the complexities of trauma for women, and sometimes children.44,52,53,62,64,67,68,70,76–79 While only one study explicitly stated that staff were trained in complex trauma and trauma-informed care, 60 Tarasoff et al. 75 noted that the 12 integrated treatment programs being studied embraced a trauma-informed philosophy in the ways programs were delivered as well as how staff worked with pregnant and parenting women by considering client histories and experiences of trauma in their program delivery. Hser et al. 57 drew attention to how women are more likely to have coexisting complexities related to gender-specific social determinants of health when thinking about trauma. McCarron et al. 58 recognized that in the context of Indigenous women, program developers and staff must recognize the historical and intergenerational trauma experienced by individuals, families, and their collective communities.
Safety and trustworthiness
Safety and trustworthiness refers to the physical/environmental, emotional, and cultural safety required for people to develop trustworthy relationships and engage in healing. 34 A sense of safety was fostered when program and service staff were consistently non-judgmental, welcoming, and respectful with women accessing supports.47,54,55,60,69,70,72,75,77–79 Andrews et al. 67 reported that when organizational staff, at all levels, fostered a culture of safety and trust between staff, clients, managers, and with other community agencies, clients noticed. By modeling how to create safe spaces, have empathy, show care and compassion, and be reliable and consistent, not only did the sense of safety and trustworthiness increase in programs and services, but it was also foundational to building, teaching, and supporting healthy and sustainable relationships.51,66,67,76 In programs that offered outreach/outpatient supports that worked around women’s needs by meeting in the evenings, on weekends, and/or at home offered a layer of safety for women.56,63,64,75,81
While many of the studies focused on settings solely supporting pregnant and parenting women, one study compared women-only to mixed-gender treatment programs and found that women-only supports and interventions improved levels of completion and long-term outcomes associated with substance use, in addition to having women-only staff. 57 Similarly, several studies with Indigenous women and/or in Indigenous communities highlighted the importance of having cultural programming, Indigenous staff, and cultural safety practices when fostering a sense of safety and trust.48,58,81
Safety was fostered through helping women form healthy relationships, find safe housing, manage systems navigation, and be (re-)connected to their children through including children or child minding in programming. 77 Wraparound and single access programs and/or programs with case coordinators/workers that assisted women to advocate and navigate multiple and complex systems of care helped women feel safer and trust staff and programs.48,72,73,77,78 Specifically, having trusted staff and organizational support for women engaged with the child welfare system, many of whom may have initially feared child welfare involvement, helped women to feel safer.63,75,77,78
Choice, collaboration, and connection
Creating opportunities for choice and self-determination, connections between people in relational ways that foster trust, and collaboration across all relevant levels and systems of care are all included in this principle. 34 Most studies were focused on approaches, programs, or services that included choice, ranging from voluntary live-in treatment centers to motivational enhancement therapy where women chose their own attainable goals to work toward. Several studies highlighted how individualized care, choice, and collaborative planning with staff supports were highly effective in addressing substance use, mental health issues, and parenting—in sustainable and motivating ways.52,56,59,60,68–70,72–75,77–79 An example where choice was highly effective was offering to meet women in their own homes or a place that women felt comfortable, rather than coming into an office. 48
Central to collaboration and connection is the concept of relationships. The quality and emphasis on relationships and relational approaches plays a key role in many approaches, programs, and services. When relationships between staff and pregnant or parenting women were strong, women reported feeling a sense of belonging, community, safety, support, and hope.52,78,79,81 Relationships between women, through peer connections and support, featured prominently in several studies, reporting the added benefit of strong support networks continuing to exist after a program had ended.53,59,60,71,81 Some programs focused on supporting women based on their existing networks of people and supports, with sustainability beyond the intervention in mind.56,64 Initiatives that helped connect women with educational and job opportunities also served as protective factors for substance use and mental health.44,45,54,70,72
Similar to the safety- and trust-related findings, when staff worked in collaborative ways with pregnant or parenting women and their children, other staff within the organization, and with staff of other agencies, women were more likely to experience success and confidence in attaining their goals.51,52,55,67,69,76,79 When programs for parenting women not only included programming for their children, but also attended to strengthening the mother–child relationships, women reported more success and confidence in parenting, confidence in reducing or stopping their substance use, and improved mental wellness.49,76–78,81
Strengths-based approach and skill building
A strengths-based approach refers to recognizing, appreciating, and building on the capacities, abilities, and resources of individuals. Skill building refers to developing and promoting strategies, skills, and knowledge that help individuals to cope, manage, and thrive. 34 Programs that were flexible around women’s lived realities (e.g. missing an appointment or being late, childcare and transportation needs, or lack of safe housing) and did not penalize women often also took approaches to working with women’s strengths and recognizing when they were ready to make positive changes.44,49,59,62,64,70 In one study, the authors reported that counselors saw women beyond their substance use, and women had dignity to counter common feelings of shame and distrust. 77 Numerous studies reported on successful outcomes from motivational interviewing or motivational enhancement therapy in which women worked with counselors to identify their strengths, resources, and motivations to set individualized goals.50,51,60–62,68,72,74,80
Skill building was most commonly evident in curriculum-based interventions;49,65 training on managing and coping with substance use, mental health, and wellness strategies;44,45,48,49,53,60,70,72 parenting skills and mentorship;47,49,52,53,65,71,72,74,75 self-care workshops; educational, vocational, and life skills courses;54,57,64,75 and child birth.44,45,69 Similarly, some initiatives trained and supported parents in communication and obtaining access to other systems of care.56,64
Reported outcomes linked to trauma-informed approaches and practices
Reported outcomes associated with trauma-informed principles were linked to multiple approaches and practices not easily attributed to a single approach or practice. Initiatives that embedded trauma-informed principles throughout their programming, ways of engaging with women, and training their staff, reported reduced mental health symptoms, decreased substance use, and improved and sometimes long-term support networks.44,45,59–61,64,69–74,76,81 Women who accessed supports reported how the initiatives improved protective factors for substance use and mental health issues, such as increased hope, confidence, skills, strategies, and motivation for a better life.53–55,60,69,72,74,77–79,81 The authors of one study reported that women in a trauma-informed integrated treatment program felt like they were treated as a “whole person” and were not made to feel ashamed, as they often felt. 70 Other authors reported on how programming helped women link their past trauma with their current context which, in turn, helped reduce stigma, guilt, and shame that women had been feeling.47,65
In programs and initiatives that took a relational approach with pregnant or parenting women using substances, including alcohol, women were more likely to feel welcomed and cared for, complete a program, improve their circumstances and well-being, and establish sustainable social networks.47,55,58,59,67,69,70,73,75,77,79 The authors of several studies demonstrated that peer support programs facilitated sustainable benefits to the women and often times their children.52,55,58,71,79 The authors of three studies reported that having Indigenous staff and culturally specific care for and with Indigenous women improved the level of access, trust, and well-being of the women and their families.48,58,78
Several positive outcomes were identified in programs that (1) allowed parenting women to bring their children, (2) recognized the importance of nurturing relationships between women and their children, (3) offered parenting skills training and mentorship, and/or (4) offered support to mothers navigating the child welfare system. The women in these programs experienced improved parenting confidence,47,65 increased access to needed supports,52,57,72 reduced substance use, 64 and increased likelihood of keeping custody of their children.54,64,77,78
Practice recommendations from the literature
Most authors made recommendations for practice at the system, organizational, and/or program/intervention levels based on their study findings. We thematically organized recommendations related to trauma-informed practices by system, organizational, and program levels (see Table 3). At the systems level, the authors of multiple studies recommended and endorsed integrated, coordinated, and comprehensive approaches that include working with women, their children, and sometimes families to support them in relevant areas that may include mental health, child welfare, housing, intimate partner violence, and justice.46,59,63,65,68,70–72,76–78 Furthermore, women’s most basic needs need to be addressed at the systems level before trying to address substance use and mental health issues.44,71
Trauma-informed related practice recommendations.

At the organizational level, some authors recommended increased and coordinated efforts to reach women as soon as they are pregnant,68,71 and a handful of authors recommended relational approaches be used and modeled at all levels within and between organizations.64,67 Multiple authors recommend long-term support networks within communities that will help foster connections and relationships.45,67,77–79 Primary care networks need to be a good entry point for specialized services for women with substance use challenges, and primary care providers need to be trained around available networks for pregnant and parenting women with substance use challenges.73,79
At the program level, many recommendations were made including tailoring programming around women’s realities;58,70,77,78 investing in peer support and mentorships that last longer than programs;55,69,73,79 offering home visiting where possible to foster cultural safety; 48 removing childcare and transportation barriers;72,79 attending to relationships between staff and women 66 and mother–child dyads;64,67 using motivational interviewing/enhancement therapy;53,58 including parenting skills and planning that includes children and relevant family systems;52,79 and including family therapy as an option.56,64
Discussion
The aim of this study was to synthesize peer-reviewed research regarding how trauma-informed approaches can be used and are helpful for pregnant and parenting women, specifically those using alcohol. As such, we recognize how alcohol use and mothering are uniquely positioned, stigmatized, and represented in public discourse. In the following sections, we briefly discuss how: (1) relationships and trust are central to trauma-informed care; (2) how alcohol differs from other substances in applying trauma-informed care, but also how the trauma-informed approaches and practices in the context of populations are not well-represented in the literature; and (3) how trauma-informed care is an inherent part of culturally safe practices.
Relationships and trust above all else
Trauma-informed approaches that show the most promise with reducing or preventing alcohol use later in pregnancy or in future pregnancy/pregnancies can be found across systems, organizational, and program levels. The most common trauma-informed approach described across all articles was that of a relational approach. A relational approach is designed to be reparative of past negative, overwhelming, unsafe relationships and to provide the opportunity to build trust and connection. Relationships and trust served as the foundation for addressing stigma and breaking down barriers to care for women who use(d) substances, including alcohol. Without relationships and trust at several intersecting levels, including between women, between women and staff, between staff, and within/across support networks, programs and interventions would not be as effective. While most studies did not report on the involvement of women’s partners, women in programs that prioritized principles of choice, collaboration, and connection may have included partners in activities such as counseling or parenting classes.
Relationships and trust are essential to creating “safe spaces” for people to be, in the literal environmental sense, as well as in the emotional, spiritual, and cultural senses.83,84 In contexts where relationships and trust are an implicit part of the organizational culture and program, it stands that women and their children will not only feel safer, but will also be witness to and can be authentically mentored in developing healthier relationships with themselves and others. Some practitioners and researchers argue that there are three relationships to tend to when mothers who use(d) substances during and after pregnancy seek substance use treatment/support: (1) the mother, (2) the child(ren), and (3) the mother–child(ren) dyad.75,85,86 Children of mothers who use substances may also experience forms of trauma and greatly benefit from engaging in and seeing healthy relationships. Moreover, if mother–child relationships are supported, modeled, and strengthened, there will be decreased levels of stress and unresolved trauma that would otherwise trigger substance use in the future.87–89
Studies in our review included pregnant and parenting women who use(d) alcohol, or alcohol and other substances, live with trauma, and accessed a support/service or initiative. However, there is very little research on pregnant or parenting women who are not accessing substance use–related supports or services, and/or who belong to middle and upper socio-economic classes where alcohol dependency is more hidden and women are not under social or child welfare surveillance.90–94 More specifically, we are referring to white middle and upper class women, as it is well-documented in the countries that we include in this review that racialized women are subject to more surveillance, policing, trauma, and stigmatizing stereotypes.95,96
Alcohol in comparison to other substances
The licit nature of alcohol as a socially acceptable, legal, affordable, and accessible substance makes it different from most other substances used by pregnant and parenting women coping with trauma. However, the teratogenic effects of alcohol have the most impact on fetal development when consumed during pregnancy, as compared with other commonly used substances.95,97 The public image of women who consume alcohol and substances during pregnancy is influenced by popular media and news coverage that presents them in a negative manner,43,98 sometimes framing drinking during pregnancy as criminal behavior that must be policed.84,99 Mothers who use alcohol are generally portrayed as being willful and responsible for their situations, rather than seeing the alcohol use as a coping behavior, and the systems in place around women are less likely to be blamed or held accountable. 84
In relation to FASD awareness and education, media frequently tout FASD as “100% preventable” and someone is to blame (namely, the mother), entirely ignoring the broader societal and systemic inequities and injustices that were/are at play in ways that are harder to pinpoint. Girls and women with unrecognized forms of intergenerational trauma live with an increased risk of mental health and other chronic physical health challenges, and polysubstance use is a normalized coping strategy.8,100,101 Another unrecognized area of concern is girls and women who are prenatally exposed to alcohol themselves and living with the effects of unrecognized and undiagnosed FASD, in addition to trauma. In other words, substance use and mental health supports, programs, services, and interventions are rarely developed, planned, and implemented with an intergenerational trauma and FASD-informed lens.102–104
Linking trauma-informed practices with cultural safety
Cultural safety is a term that is most widely used in the health delivery contexts where power imbalances exist between those who provide care and those who receive it, most relevant in contexts where Indigenous Peoples and/or racialized people are accessing care within colonial and Eurocentric colonial countries.105–107 It requires care providers to be critically self-aware, reflexive, and culturally humble; for cultural safety to be realized, only the people receiving the care can determine whether or not the care is culturally safe. 105 Only seven of the analyzed studies made reference to concepts of cultural relevance, cultural competency, or cultural safety in their approaches to working with pregnant or parenting women.48,58,71,74,78,79,81 In countries and regions where societal hegemonic power is reflected in the staff providing care, and people receiving power are subject to racial and cultural discrimination by dominant groups in their society, the importance of cultural safety is often overlooked.
It is unclear whether studied programs, services, and interventions did not seriously consider cultural safety, whether research participants were not prompted to think about the cultural safety of the studied intervention/approach, or whether the authors of the study did not report on related findings in their article. In the context of pregnant or parenting women who are Indigenous and/or racialized in countries where people in positions of power are predominantly white and represent colonial and racist systems, often sub- or unconscious colonial and racist ways of thinking and doing that perpetuate harm persist, making the implementation of relational approaches and building trust harder. Research on trauma-informed approaches must include and examine how cultural safety is being addressed within the staff complement, training, and environment when working with Indigenous and/or racialized pregnant and parenting women, and how cultural safety in these contexts serves the needs of the non-dominant group (e.g. those from unrepresented and marginalized or racialized groups) instead of upholding safety for dominant groups (e.g. white people).
Strengths and limitations
There were four key strengths of our scoping review. First, our review helps to paint the landscape of trauma-informed practices within a dearth of literature about pregnant and parenting women who use alcohol. While there are studies that (1) explore modalities of substance use treatment for pregnant and parenting women who use alcohol and (2) point to trauma-informed practice as best practice, there is limited research that bridges the two and explores how the principles of trauma-informed practice are operationalized for them to effectively and uniquely support women. Second, our review was inclusive of studies that were diverse in methodology, discipline, and terminology. Third, this scoping review offers a comprehensive overview of research in an area that is understudied, despite its consideration as best practice. Fourth, the composition of our team offered a rigorous and robust scoping review search strategy and protocol. Our team included a research librarian to test and develop a search strategy drawing on inter- and multidisciplinary bodies of literature that extended beyond health, as well as members with content expertise in alcohol and (pregnant) women, trauma-informed practice and its key principles, and FASD. Our team is well positioned to mobilize the findings, conduct further research, and engage with diverse stakeholders to improve the well-being of individuals, families, and communities where alcohol is present through trauma-informed approaches and practices that support girls’ and women’s health and wellness.
Limitations of this study include the geographies represented in the findings, namely the United States and Canada; using a search strategy built around concepts and language related to FASD prevention, trauma-informed, and substance use fields; and excluding gray literature such as organizational or program evaluation reports. Consequently, it is possible that relevant sources were missed in our review. We also chose to thematically organize and analyze evidence of trauma-informed approaches based on four pre-determined and broadly defined principles of trauma awareness, emphasis on safety and trustworthiness, opportunity for choice, collaboration, and connection, and strengths-based approach and skill building. In doing so, the results may not neatly align with differing trauma-informed principles adopted by others.
Conclusions and implications for future practice, policy, and research
While the concept of trauma-informed principles, approaches, and practices are incorporated into a variety of settings that support pregnant or parenting women who use(d) substances, there is a dearth of studies in this field. The most promising practices involve organizational staff that use a collaborative and relational approach to providing integrated and comprehensive supports where women feel welcomed, free of judgment, seen, and treated as a “whole” person. Effective supports for pregnant and parenting women using substances including alcohol must foster a sense of safety, which requires trauma-informed training, education, and policies for the people responsible for programs, supports, and services.
Based on the findings of our review, cultural safety training and approaches should be integrated into practice. Trauma-informed, sex- and gender-based, and culturally relevant policies must be developed or amended, and implemented, to remove unnecessary barriers and stigma for pregnant and parenting women who seek support to reduce the number of people who must navigate challenges associated with substance use and FASD. Further research is warranted evaluating the long-term outcomes of trauma-informed approaches, programs, and services; critically examining how systems and their policies play a role in enabling common traumas linked to substance use during pregnancy; understanding the women who do not access supports and services; and studying substance use programs and initiatives that address intergenerational trauma and parents who are living with FASD.
Research Data
sj-docx-1-whe-10.1177_17455057221148304 – Supplemental material for Supporting pregnant and parenting women who use alcohol during pregnancy: A scoping review of trauma-informed approaches
Supplemental material, sj-docx-1-whe-10.1177_17455057221148304 for Supporting pregnant and parenting women who use alcohol during pregnancy: A scoping review of trauma-informed approaches by Melody E Morton Ninomiya, Yasmeen Almomani, Katharine Dunbar Winsor, Nicole Burns, Kelly D Harding, Megan Ropson, Debbie Chaves and Lindsay Wolfson in Women’s Health
Supplemental Material
sj-docx-2-whe-10.1177_17455057221148304 – Supplemental material for Supporting pregnant and parenting women who use alcohol during pregnancy: A scoping review of trauma-informed approaches
Supplemental material, sj-docx-2-whe-10.1177_17455057221148304 for Supporting pregnant and parenting women who use alcohol during pregnancy: A scoping review of trauma-informed approaches by Melody E Morton Ninomiya, Yasmeen Almomani, Katharine Dunbar Winsor, Nicole Burns, Kelly D Harding, Megan Ropson, Debbie Chaves and Lindsay Wolfson in Women’s Health
Supplemental Material
sj-docx-3-whe-10.1177_17455057221148304 – Supplemental material for Supporting pregnant and parenting women who use alcohol during pregnancy: A scoping review of trauma-informed approaches
Supplemental material, sj-docx-3-whe-10.1177_17455057221148304 for Supporting pregnant and parenting women who use alcohol during pregnancy: A scoping review of trauma-informed approaches by Melody E Morton Ninomiya, Yasmeen Almomani, Katharine Dunbar Winsor, Nicole Burns, Kelly D Harding, Megan Ropson, Debbie Chaves and Lindsay Wolfson in Women’s Health
Supplemental Material
sj-docx-4-whe-10.1177_17455057221148304 – Supplemental material for Supporting pregnant and parenting women who use alcohol during pregnancy: A scoping review of trauma-informed approaches
Supplemental material, sj-docx-4-whe-10.1177_17455057221148304 for Supporting pregnant and parenting women who use alcohol during pregnancy: A scoping review of trauma-informed approaches by Melody E Morton Ninomiya, Yasmeen Almomani, Katharine Dunbar Winsor, Nicole Burns, Kelly D Harding, Megan Ropson, Debbie Chaves and Lindsay Wolfson in Women’s Health
Supplemental Material
sj-docx-5-whe-10.1177_17455057221148304 – Supplemental material for Supporting pregnant and parenting women who use alcohol during pregnancy: A scoping review of trauma-informed approaches
Supplemental material, sj-docx-5-whe-10.1177_17455057221148304 for Supporting pregnant and parenting women who use alcohol during pregnancy: A scoping review of trauma-informed approaches by Melody E Morton Ninomiya, Yasmeen Almomani, Katharine Dunbar Winsor, Nicole Burns, Kelly D Harding, Megan Ropson, Debbie Chaves and Lindsay Wolfson in Women’s Health
Supplemental Material
sj-docx-6-whe-10.1177_17455057221148304 – Supplemental material for Supporting pregnant and parenting women who use alcohol during pregnancy: A scoping review of trauma-informed approaches
Supplemental material, sj-docx-6-whe-10.1177_17455057221148304 for Supporting pregnant and parenting women who use alcohol during pregnancy: A scoping review of trauma-informed approaches by Melody E Morton Ninomiya, Yasmeen Almomani, Katharine Dunbar Winsor, Nicole Burns, Kelly D Harding, Megan Ropson, Debbie Chaves and Lindsay Wolfson in Women’s Health
Footnotes
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
